Abstract
Background
Population-based data about utilization of complementary and alternative medicine (CAM) among those with chronic conditions is lacking.
Objective
To describe whether CAM use by California adults with cancer and other chronic conditions reflects condition-specific patterns or a general tendency to use CAM modalities.
Methods
Interviews of 9,187 respondents including all participants with cancer from a prior representative survey of California households, and a stratified sample of all other respondents. Almost 74% of the respondents reported at least one chronic health problem.
Results
Use of all forms of CAM among those with chronic health problems is high. Those with a diagnosis of cancer are more likely to use prayer, dietary supplements, and support groups, and less likely to use CAM providers and special diets. Overall, individuals diagnosed with most chronic problems use a similar set of CAM modalities. Demographic correlates of CAM use differ in their impact and vary according to what type of CAM is being used.
Conclusions
Clinicians should be aware that while a diagnosis of cancer is associated with a greater use of some forms of CAM, overall patterns of CAM use are similar to those with most other chronic problems.
Background
The extensive use of complementary and alternative medicine (CAM) in the United States and Europe is now recognized. Although some studies have found the overall use of CAM to be more modest (1), most research finds between 40–45% of the adult population uses some form of CAM each year (2)(5). Our knowledge about the use of CAM among the chronically ill is primarily based on studies conducted in practice settings, or among self-selected and convenience samples (6). The lack of population-based data on those with chronic conditions leaves the validity of these findings in question. For example, among women with breast cancer, recent reports of any CAM use have varied from under 30% to almost 70% (7)–(11). Such discrepant findings are typical of reports on current CAM use for many chronic conditions: asthma 6%–42% (12), (13), diabetes 8%–57% (14), (15), (16), depression 5%–57% (17), (18), (19), arthritis 25%–90% (20)(26), and cardiovascular disease 64%–85% (27), (28).
Prior studies make clear that having a chronic condition is an important factor associated with CAM use. But it is unclear if different chronic conditions are associated with an increased use of all or most CAM modalities, or if particular conditions are associated with the use of specific CAM modalities. For example, because cancer is serious, frequently fatal, and often not responsive to treatment, individuals with a diagnosis of cancer might be expected to use CAM more often than those suffering from other chronic problems. The goal of this research is to describe the extent to which CAM use among adults in California with cancer and other chronic conditions is best understood in terms of condition specific patterns, as opposed to a general tendency to use a common array of CAM modalities.
Methods
The data for this study are from a follow-up survey to the 2001 California Health Interview Survey (CHIS 2001), a random-digit-dial telephone survey (N = 55,428) drawn to be representative of California's non-institutionalized household population. Despite an overall weighted response rate of 37.7% (screener completion rate: 59.2%, interview completion rate: 63.7%), the weighted CHIS 2001 sample was representative of California's diverse population in terms of its similarity to the census for age, sex, race/ethnicity, and rural-urban residence (29).
The sampling frame for the California Health Interview Complementary and Alternative Medicine Supplement (CHIS CAM) was constructed from the approximately 80% of CHIS 2001 respondents who were willing to be re-contacted. In order to ensure sufficient participation of individuals with cancer, a specific focus of the research, the sample included all CHIS 2001 respondents who reported a diagnosis of cancer (excluding non-melanoma skin cancers) and a random sample, stratified by race and ethnicity, of remaining CHIS 2001 respondents who did not report having cancer. In order to ensure sufficient racial/ethnic diversity, 100% of Pacific Islanders, Native Americans/Alaska Natives, Asians, African-Americans, and those reporting a multiracial identity who did not have cancer were included, as well as 59% of the Latinos and 13% of the whites. The over-sampling of respondents with cancer means that the sample is not representative of the California population. However, the sample is diverse and appropriate for testing the association of socio-demographic factors and CAM use. The telephone interviews were conducted in English, Spanish, Korean, Cantonese and Mandarin between January 30th, 2003 and April 27th, 2003. The completed sample contains 9,187 respondents, of which 1844 reported a diagnosis of cancer in either CHIS 2001 or during the period between the two studies. The overall unadjusted response rate was 56%, and varied by race/ethnicity, with a rate of about 66% for whites and rates just below 50% for both African Americans and Latinos and just above 50% for Asian-Americans. The primary reason for non-response was difficulty in locating the original CHIS 2001 respondents. This was caused by the two-year gap between CHIS 2001 and CHIS-CAM, as well as the lack of detailed information for re-contacting respondents. The net response rate i.e., the number of completed interviews divided by the number of eligible contacts was 77.3%.
Interview
As there is no standard definition of CAM, we selected specific CAM modalities for inclusion on the basis of their prevalence in prior studies as well as for their ability to encompass the five types of CAM modalities described by the National Center for Complementary and Alternative Medicine (27). We collected information regarding the use of 11 CAM providers (chiropractors, massage therapists, acupuncturists and other practitioners of TCM, osteopaths, curanderos, naturopaths, homeopaths, Native American healers, Ayurvedic practitioners, and Reiki practitioners), special diets for treating or preventing illness (open-ended), and 30 dietary and herbal supplements exclusive of multivitamins (listed in Table 2), 4 mind-body techniques (imagery/guided imagery, meditation, hypnosis/self-hypnosis, biofeedback), self-directed prayer, and support groups (open-ended). Use of a special diet was assessed by asking if the respondent had “changed the food you eat or gone on a special diet in order to help deal with cancer/an illness or to help stay healthy.” While not all positive responses to this item may indicate CAM use, dietary changes are an important CAM modality, and have commonly been assessed by similar ambiguous questions. The use of self-directed prayer was assessed by asking if the respondent had “ever prayed specifically for the purpose of your own health?”
Age is grouped into four categories: 20–35, 36–50, 51–64, and 65+. The racial/ethnic categories are mutually exclusive with Latino treated as a “race/ethnic” category, along with non-Latino white, non-Latino African American and American Indian/Alaskan Native. Asian/Pacific Islander includes those who classified themselves as Chinese, Filipino, Japanese, Korean, South Asian, Vietnamese, Cambodian, Native Hawaiian and Other Pacific Islander. Respondents reporting more than one race/ethnicity were assigned to the one they said they identified with most. If they did not have a category with which they most identified, they were coded as “other.” Income is measured as the proportion of household income (0–99%, 100–199%, 200–299%, >300%) relative to the Federal Poverty Level (FPL) for 2001 when data for CHIS 2001 were collected. Education is based on the highest number of years of schooling received (0–11 yrs., 12 yrs./h.s..grad, 13–15 yrs., 16 or more yrs.) Residential status (urban, suburban, rural) was based on the population density of the respondent's zip code.
Respondents were also asked if they “now have” any of the following chronic conditions: asthma, any other lung or breathing problem, chronic obstructive pulmonary disease, arthritis or rheumatism, back or neck problems, stroke (ever had), diabetes, high blood pressure or hypertension, or depression or anxiety disorder. If a respondent was unsure about his/her status with regard to one of these conditions, s/he was asked “Has a doctor or other health professional told you that you have [chronic condition]? As one goal of the study is to examine the use of CAM among those with cancer as opposed to other chronic conditions, the respondents are grouped into those who had cancer, regardless of whether or not they had any other chronic condition(s), those who reported having each of the other chronic conditions (asthma, etc.) regardless of whether they had any other chronic condition(s) except cancer, and those who reported having no chronic conditions. For purposes of analysis respondents who reported “lung problems” and “chronic obstructive pulmonary disease” were combined into one group, as were those who reported either “heart disease” or “stroke” (“cardiovascular problems”), “arthritis” and “back or neck problems” (“musculoskeletal problems”), and “anxiety” and “depression” (“mood disorders”). The survey procedures and instruments used in both CHIS 2001 and CHIS CAM were approved by the Institutional Review Board of the University of California, Los Angeles.
The primary outcome variables are: 1) the (adjusted) percentage of respondents who reported visiting specified CAM providers, or any of these practitioners during the 12 months prior to being interviewed; 2) the (adjusted) percentage of respondents who reported utilizing specified CAM techniques (regular use of two or more dietary/herbal supplements in addition to a multi-vitamin, mind-body techniques, support groups during the 12 months prior to being interviewed; 3) the (weighted) percentages of respondents who reported ever praying specifically for their own health, and 4) using a special diet to deal with or prevent an illness.
Statistical Methods
Data were weighted to compensate for the differential probability of selection for each sampled unit, reduce biases arising from the selected characteristics of the respondents, and adjust, insofar as possible, for under coverage in the sampling frame and surveyed respondents. The weighting of the CHIS CAM data was initially based on the final weights for CHIS 2001 which included adjustments for non-response weighted to the 2000 Census in order that estimates are representative of California's non-institutionalized population. These weights were then adjusted for language eligibility, willingness to participate in follow-up studies, and both sub-sampling and non-response by stratum (age, gender, cancer status, race/ethnicity, rural-urban residence) in CHIS CAM.
Analyses reported here consist of weighted frequency estimates of previous CAM use. Crude (unadjusted) comparisons of these estimates using differences in proportions with 95% confidence intervals (CI) and adjusted odds ratios with 95% confidence intervals in multivariable models are also shown. Logistic regression using sampling weights based on the Taylor Series Method (as used in SUDAAN) was used to examine the relation of socio-demographic factors and health status with various types of CAM use.
Results
Selected characteristics of the entire CHIS-CAM sample and sub-groups of these respondents reporting specific chronic conditions are shown in Table 1. As expected, respondents not reporting a chronic condition were more likely to be younger than those who did report chronic problems. Latinos were also less likely to report chronic conditions and whites more likely to do so. Income, education, and urban-rural residence appear to be unrelated to chronic conditions in our sample. Respondents reporting a cancer diagnosis were diverse. However, whites are over-represented and Latinos are under-represented relative to the state's population. Among those with cancer, about one third (356 = 32.5%) reported being diagnosed within three years prior to the interview; about one fifth (474 = 22.2%) reported having breast cancer, and one sixth (241 = 16.3%) reported prostate cancer (data not included in Table 1.) Over 90% reported that their cancer is/was “treated by a specialist.”
Sample Characteristics and Health Condition (Unweighted N, Weighted %).
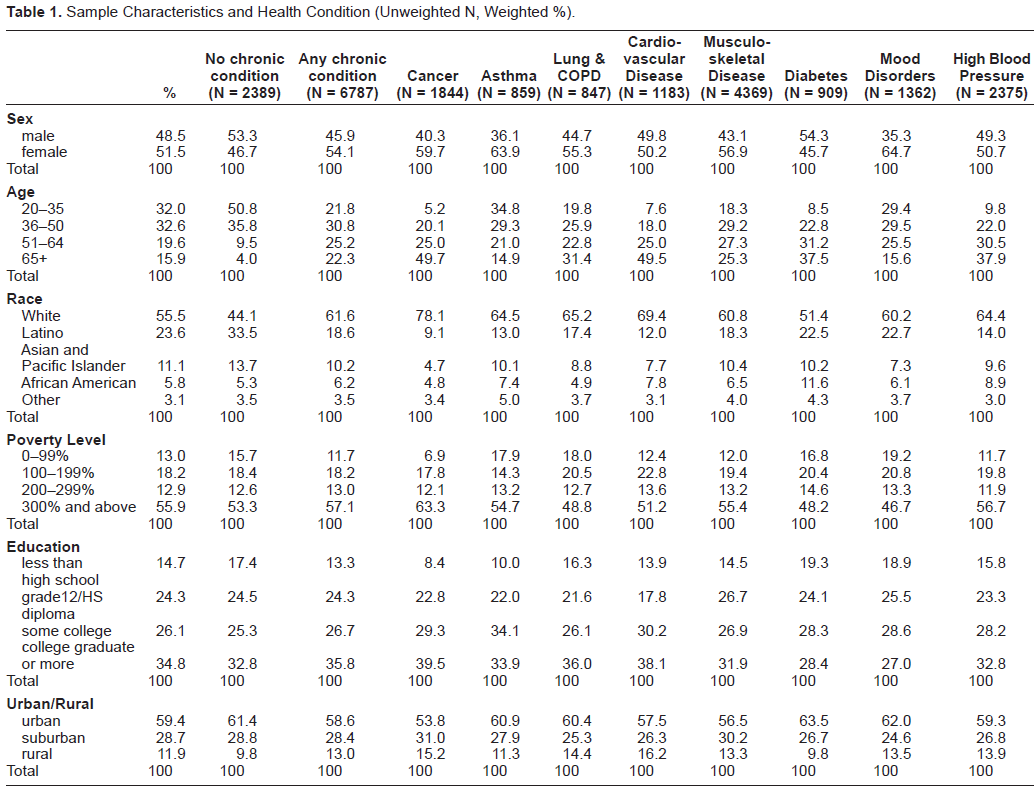
Table 2 shows the absolute number of respondents who used each type of CAM provider and other CAM modalities over the past 12 months prior to the interview, along with the weighted proportion of the respondents with no chronic condition, any chronic condition, and each specific condition who reported using these same CAM providers and other CAM modalities. CAM providers used by less then 2% of the sample (osteopaths, homeopaths, curanderos, naturopaths, Native American healers, Ayurvedic healers, Reiki practitioners) were combined into an “other provider” category. Having any of the chronic conditions is associated with increased utilization for every indicator of CAM use. The table also compares CAM utilization among those reporting a specific condition with utilization among those reporting all other chronic conditions except the specific condition being compared. For example, compared to those with any of the other conditions, respondents with cancer reported being less likely to have visited a massage therapist, used multiple providers, or used a special diet, while being more likely to have used dietary supplements, prayed for their own health and participated in a support group. Those reporting cardiovascular problems were less likely to use CAM providers, particularly massage therapists, and more likely to pray for their health, while those with musuloskeletal conditions were more likely to use providers, especially chiropractors and massage therapists, as well as take dietary supplements. Diabetics report using fewer providers and dietary supplements, along with greater use of special diets and self-directed prayer. Individuals with mood disorders were notable in being more likely to report using most types of CAM, while respondents with high blood pressure were generally less likely to report the use of CAM providers and mind-body techniques. The CAM modalities used by respondents reporting pulmonary problems were difficult to distinguish from those used by respondents with other chronic problems.
Use of Select CAM Providers and Techniques within the past 12 months by Specific Health Condition (Unweighted N, Weighted %).
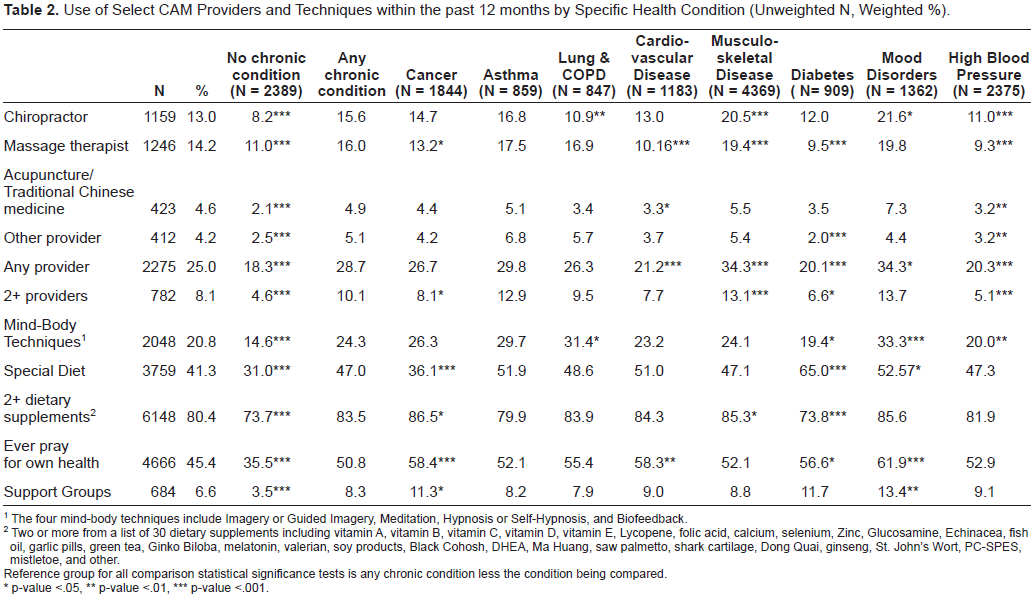
The four mind-body techniques include Imagery or Guided Imagery, Meditation, Hypnosis or Self-Hypnosis, and Biofeedback.
Two or more from a list of 30 dietary supplements including vitamin A, vitamin B, vitamin C, vitamin D, vitamin E, Lycopene, folic acid, calcium, selenium, Zinc, Glucosamine, Echinacea, fish oil, garlic pills, green tea, Ginko Biloba, melatonin, valerian, soy products, Black Cohosh, DHEA, Ma Huang, saw palmetto, shark cartilage, Dong Quai, ginseng, St. John's Wort, PC-SPES, mistletoe, and other.
Reference group for all comparison statistical significance tests is any chronic condition less the condition being compared.
p-value <.05,
p-value <.01,
p-value <.001.
Table 3 shows the relation of selected socio-demographic factors to the use of any CAM provider over the past 12 months for respondents reporting no chronic conditions, cancer, and seven other chronic problems (weighted percentages, adjusted odds ratios, 95%CIs). The odds ratios are adjusted to show the impact of the variable in question on the use of a specific type of CAM while controlling for the effect of all other variables in the model.
Use of Any CAM Provider within the past 12 months by Specific Health Condition and Select Demographic Variables (Weighted %, Adjusted Odds Ratios * , 95% Confidence Intervals).

Adjusted Odds Ratios from a Multiple Logistic Regression, with use of Any CAM Provider within the past 12 months as the dependent variable and sex, age, race, poverty level, education, urban/rural, and insurance status as independent variables.
In the unadjusted analysis being female is associated with greater use of CAM providers for every chronic condition except asthma, diabetes, and high blood pressure. However, with the exception of musculoskeletal problems, the multivariable model does not indicate a clear relation of gender to CAM provider use.
For most conditions, the oldest respondents (65+ yrs.) are less likely to use CAM providers. However, for those under 65 years, the association of use and age varies considerably by condition. For example, among those with either cancer, the frequency of use drops consistently with age, while for those with asthma, diabetes, mood disorders, high blood pressure or musculoskeletal problems the rate first goes down with age, then rises, and then declines.
The relation of CAM use and racial/ethnic group identity also varies by the presence of specific chronic conditions. Latinos report the clearest pattern, with consistent low unadjusted rates of utilization of CAM providers among those with most chronic conditions, including cancer. African-Americans also report low levels of CAM provider use, although the differences are not as clear in the multivariate model. Asian/Pacific Islanders with specific chronic conditions report CAM provider use at about the same level or greater than among whites, while reporting lower provider use for those not reporting any chronic condition.
The relation of family income to the use of CAM providers does not follow a clear trend. Income and provider use are unassociated among those reporting cancer, asthma, other lung conditions, and cardiovascular problems, while they are related among those reporting musculoskeletal problems, diabetes, mood disorders, and high blood pressure.
There is a clear and strong relation with those who have not graduated from high school showing less utilization of CAM providers. Among respondents with chronic conditions, education has the greatest impact among those with lung, cardiovascular, and musculoskeletal conditions. This association is not evident among those with cancer. Urban, as opposed to suburban or rural residence, does not appear to be a determinant of CAM use. Respondents with cancer are more likely to see a CAM provider if they are uninsured. But, the impact of insurance status in the multivariate model is not clear.
Discussion
Confidence in the findings of this study is limited by a relatively high non-response rate in the original CHIS2001 survey, the potential for respondent's self-assessments of specific diagnoses to be unreliable, the possibility that some CAM users who experienced positive outcomes may be more likely to participate in a study of this sort than CAM users with negative outcomes, and the difficulty of conducting a follow-up survey by phone in an area with high geographic mobility. Still, we believe that the findings presented are among the most representative ever collected of California's diverse population of individuals who suffer from chronic conditions. Our results indicate that clinicians should be aware that a diagnosis of any chronic condition is strongly associated with substantially greater utilization of every type of CAM. The extent to which CAM use among those with a particular condition differs from use among those with other chronic conditions is variable. In the case of asthma, none of the eleven measures of CAM use we examined greatly differs from the level of use found among those reporting any of the other conditions. In the case of diabetes, the level of utilization differs on eight of the eleven measures. Respondents with cancer report differences on six of the measures.
It is also clear that different conditions are, to some degree, associated with the use of different CAM modalities. Musculoskeletal problems are associated with the use of chiropractors and massage therapists, cancer with greater use of support groups, self-directed prayer, and dietary supplements, and diabetes with more use of special diets. In addition, our results indicate the impact of socio-demographic factors, such as gender, age, and race/ethnicity, on condition-specific CAM provider use among the chronically ill is somewhat distinct from what has been found in clinic-based research. For example, being female does not have a strong impact on the use of most provider based CAM. Age and race/ethnicity have a complex relation with CAM use among the chronically ill, although Latinos do report a generally low level of utilization. The use of CAM providers among both Asians-Americans and African Americans varies by which specific chronic conditions are reported. The variable impact that current health insurance coverage has on CAM provider use may reflect the very restricted coverage for CAM under most insurance plans, as well as the possibility that CAM is substituted for conventional care for some, but not all, chronic conditions. Level of education is the single most consistent predictor of CAM use across groups with different chronic conditions.
Despite the variation noted above, each type of CAM is used extensively among those with every chronic condition. For example, the use of multiple dietary supplements is essentially ubiquitous, regardless of condition. Respondents reporting mood disorders are more likely to use a wide array of approaches, supporting the notion that such individuals have a general disposition toward the use of health services and interventions (30), (31), (32). While some conditions, such as diabetes and high blood pressure, seem to be associated with relatively lower overall use of CAM, absolute levels of use are still quite high. Clinicians should be aware that while specific conditions are associated with the use of particular CAM modalities, the use of most forms of CAM is common among all those with chronic conditions, including cancer. Similarly, while some types of patients with chronic conditions are more likely to use certain types of CAM, the clinical implications of these differences should not be overestimated.
