Abstract
Background
Hypertension is a major health problem with serious medical and financial consequences. Experimental studies in animals and clinical studies in humans have demonstrated that acupuncture can reduce blood pressure significantly in hypertensive patients. The objective was to assess the effect of acupuncture on blood pressure in hypertensive patients treated at a complementary medicine clinic.
Methods
Blood pressure values measured before and following acupuncture were recorded from the charts of hypertensive patients who came to the clinic for treatment of other problems. The therapy used was the Kiiko Matsumoto technique for blood pressure imbalance.
Results
Twenty-nine patients were studied (18 [62%] women). The mean age was 58.5 ± 16.3 years. Systolic blood pressure dropped significantly as a result of the treatment and there was a non-significant trend to reduced diastolic pressure. Weekly acupuncture therapy led to a continuous reduction in systolic blood pressure.
Conclusions
Acupuncture has a beneficial effect on hypertension, particularly on systolic pressure. Further studies with larger study groups for longer periods of time can confirm this observation and contribute to our understanding of combination therapy with acupuncture and conventional medications for hypertension.
Background
Public interest in and demand for complementary medicine services have increased in recent years in Israel (Kitai et al. 1998; Shmueli and Shuval, 2004) and throughout the Western world (Eisenberg et al. 1993; Zollman and Vickers, 1999; MacLennan et al. 1996; Garaghan, 1994; Shekelle et al. 2005). Complementary medicine includes several therapeutic methods, all aimed at improving the patient's health and quality of life (Leibovici, 1996). This form of healing is complementary, rather than an alternative to conventional medicine.
A nationwide telephone survey that was conducted in the U.S.A. (Eisenberg et al. 1993) showed that 34% of 1,539 participants had used complementary medicine in the previous year. In 1990, residents of the United States paid about 425 million visits to complementary practitioners (compared with 338 million visits to primary care physicians in the same period). Total expenditures by Americans for non-conventional medicine were estimated for that year to be 13.7 billion dollars (Eisenberg et al. 1993). The popularity of complementary medicine in Israel is reflected in the opening of complementary medicine clinics by the health funds. Clalit Health Services runs about 40 clinics for complementary medicine throughout the country.
In a study conducted among patients treated in the Clalit Health Services’ complementary medicine clinic in Beer-Sheva, Israel we found that acupuncture and shiatsu massage therapy were the preferred treatments (61% of all treatments provided in the clinic). The most common reason for treatment was musculoskeletal conditions (47%) (Soffer et al. 2001).
Acupuncture is a Chinese method of treatment whose roots extend back 2,500 years or more. Acupuncture releases chemicals such as endorphins and enkephalins that can inhibit pain and generate a feeling of relaxation (Bianchi et al. 1991).
Practitioners trained in Oriental medicine believe that a vital energy called “chi” circulates in the body through 12 main pathways called meridians. Each meridian is named after a particular organ or “official,” but the term actually relates to the energetic function more than the structure or anatomy of the organ. There are both surface and internal projections for each meridian. The surface projections contain sites called acupuncture points. Oriental medicine practitioners insert needles into these points to influence the body's chi to restore health (Tierney et al. 2003).
Published reports have indicated that acupuncture has a beneficial effect on blood pressure in studies of laboratory animals (Lee and Kim, 1994; Zhou et al. 1993) and humans (Kalish et al. 2004; Sainani, 2003; Guo and Ni, 2003; Chiu et al. 1997; Smith, 1992). The aim of the present study was to assess the effect of acupuncture on blood pressure in hypertensive patients undergoing treatment in a complementary medicine clinic.
Methods
Setting
The Complementary Medicine Clinic of Clalit Health Services in Beer-Sheva treats about 3,000 patients who receive about 15,000 treatments annually. The therapy offered includes acupuncture, reflexology, shiatsu massage therapy, homeopathy, chiropractics, Feldenkreiss, biofeedback, naturopathy, herbal medicine, medical hypnosis, Bach flowers and more.
A physician examines every patient who comes to the clinic and recommends an appropriate therapy. Certified practitioners who have undergone appropriate training and supervision provide the treatment. Approximately 25% of the practitioners are medical doctors. The treatments are not included in the national basket of health services, so patients are required to pay for them.
Study Population
The study population was comprised of 29 hypertensive patients who received acupuncture therapy for reasons unrelated to their hypertension, but were also receiving medication for hypertension at the time.
Acupuncture
Each patient received 5–7 acupuncture treatments for their particular medical problem, weekly on the same day and at the same hour. One of the methods used was the Kiiko Matsumoto acupuncture technique for blood pressure imbalance, a Japanese acupuncture technique that is based on abdominal diagnosis (Matsumato and Birch, 1988). At each session needles were inserted regularly into all of the seven main points:
Sp. 6–strengthens the kidneys, especially kidney yin and essential hypertension due to kidney yin insufficiency.
Sp. 9–regulates and strengthens the spleen, hypertension due to dampness
Pc. 8–regulates the heart
Pc. 3–regulates the heart and expands and relaxes the chest
Pc. 5–regulates and strengthens the heart and relaxes the chest
Pc. 6–regulates and strengthens the heart and regulates the vessels
Pc. 4–regulates the heart for rheumatic heart disease, chest pain and palpitations
Acupuncture is carried out with needles (needles CE-02, size 0.2 x 30, Acumed, China). The patients remain with the needles inserted for 25 minutes. The same practitioner (NW) treated all study patients. Blood pressure measurements taken prior to and following therapy were recorded retrospectively from the patients’ charts. All measurements were done with digital blood pressure equipment (Omeron model MX3, Omeron, Japan). Blood pressure was measured in each participant before and after each treatment at a minimum of 5 consecutive weekly sessions. Throughout acupuncture therapy the patients continued to take their regular hypertension medications. We asked the study patients to report any changes in their medical treatment. None reported any such changes. We did not ask them about lifestyle changes.
Statistical Analysis
Paired t-tests were used to compare mean blood pressure values before and after each treatment. ANOVA for repeated measurements by the General Linear Model (GLM) was used to analyze the cumulative effect of acupuncture on blood pressure. Statistical significance was set at p < 0.05, throughout.
Results
Blood pressure was measured in 29 patients, 18 women (62%). The mean age was 58.5 ± 16.3 years. Blood pressure was measured for all 29 participants before and after the first five treatment sessions. At session 6 the blood pressure was measured in 23 patients and at session 7 in 20 patients. Systolic pressure was more beneficially affected than diastolic pressure by acupuncture. The mean systolic and diastolic pressures before and after each acupuncture session are shown in Tables 1 and 2, respectively.
Mean systolic blood pressure before and after each treatment session (mean ± SD).
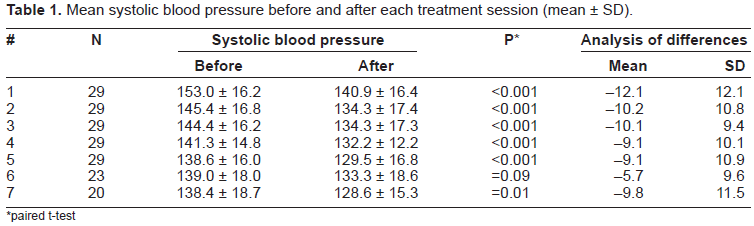
paired t-test
Mean diastolic blood pressure before and after each treatment session (mean ± SD).
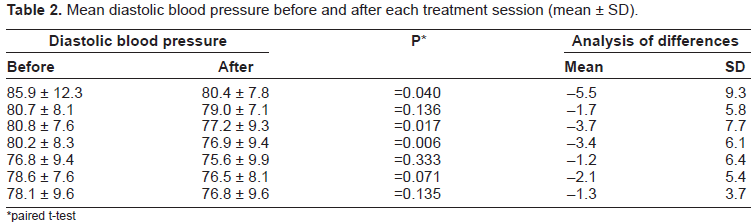
paired t-test
The mean systolic blood pressure before the first treatment session was 153.0 ± 16.2 compared with 128.6 ± 15.3 after the seventh session. The mean diastolic blood pressure before the first treatment session was 85.9 ± 12.3 compared with 76.8 ± 9.6 after the seventh session.
Figure. 1 shows the results of ANOVA for repeated measurements performed to assess the effect of treatment over time (number of treatments). A reduction in blood pressure was observed as follows: 1) systolic pressure before treatment (p < 0.001), 2) systolic pressure after treatment (p = 0.018), 3) diastolic pressure before treatment (p = 0.35), 4) diastolic pressure after treatment (p = 0.018).
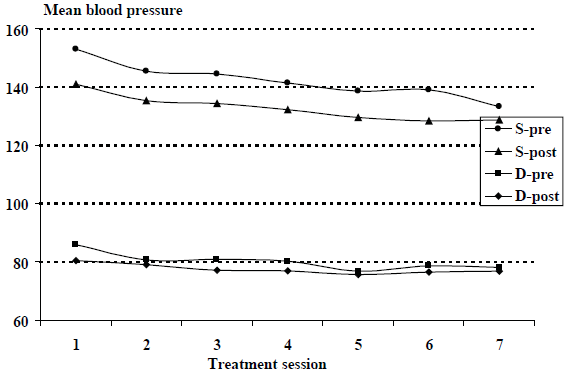
Mean systolic and diastolic blood pressure by treatment session. S-pre = systolic pressure before treatment; S-post = systolic pressure after treatment; D-pre = diastolic pressure before treatment; D-post = diastolic pressure after treatment.
Discussion
Hypertension is a major health problem with serious medical and financial consequences. Experimental studies in animals and clinical studies in humans have demonstrated that acupuncture can exert significant effects on the cardiovascular system and provide effective therapy for a variety of cardiovascular ailments (Smith, 1992). In the present study we found that systolic blood pressure was more beneficially affected than diastolic blood pressure by acupuncture therapy. Guo and Ni (Guo and Ni, 2003) reported similar findings. They also noted that acupuncture does not affect normotensive individuals.
It appears that acupuncture at defined points affects blood pressure through the rennin-angiotensin system. Acupuncture was placed on the Shih-Hsuan (Sipseon EX-UE-11) of two-kidney one clip hypertensive rats. Both the systolic blood pressure and the plasma renin activity decreased significantly after the acupuncture therapy. In the sham-operated and control rats the procedure did not lead to any significant changes (Lee and Kim, 1994). The results of that research suggest that the suppressive hemodynamic effect of acupuncture on the EX-UE-11 may be related to changes in plasma renin activity.
In the present study acupuncture was performed on hypertensive patients who received the therapy for other unrelated medical problems, but were also being treated for hypertension. Acupuncture was provided together with regular medical therapy and not in its place. It is possible that the referral to complementary medicine itself may have led the patients to take their medications more regularly or to change their lifestyles, e.g. by eat properly. However, these aspects could not be evaluated in the present study.
There are methodological limitations to this study. The study group was small, but despite this we found a significant reduction in systolic blood pressure in the short run. We do not know if this effect would have been maintained in the long run. In addition, the same practitioner who did the acupuncture therapy measured the blood pressure, which could lead to bias. This chance of bias is reduced by the fact that the measurements were taken with electronic blood pressure equipment and the exact results were recorded in the patient's chart. Also, for this study the blood pressure measurements were collected retrospectively from the patients’ charts reducing the danger of bias even further.
The study group is highly selected in that it was comprised of patients who sought this type of private treatment and were able to pay for it.
There was no control group in this study. A possible control group would have been patients undergoing sham acupuncture. In studies of acupuncture in the treatment of pain the investigators stated that although sham acupuncture may be as effective as real acupuncture, experimentally induced acute pain studies in animals and humans have consistently shown that real point stimulation is far superior to sham (Tierney et al. 2003). These conflicting findings have prevented sham acupuncture from being widely accepted as an appropriate control. The 1998 NIH Consensus Statement on Acupuncture recommendations for research focus on finding such a control (Tierney et al. 2003).
We believe that further studies with larger patients groups, a longer study period, and appropriate controls will confirm the observation that systolic blood pressure is lowered by acupuncture and may shed more light on its effect on diastolic blood pressure. Such studies could contribute to our understanding of combination therapy with acupuncture and conventional medications. Such combined therapy might reduce the rate of adverse effects from drugs and improve the use of economic resources dedicated to the treatment of hypertension.
Footnotes
Acknowledgement
The first five authors make equal contributions to this paper.
The author(s) declare that they have no conflicts of interest.
