Abstract
Spirituality seems to be an important cultural factor for African American women when thinking about their health. It is, however, not clear how spiritual health locus of control (SLOC) impacts health-related outcomes in the context of health message processing models, such as the Extended Parallel Process and the Risk Perception Attitude framework. Using a survey of African American and Caucasian women in the context of breast cancer, the role of SLOC and its interactions with perceived efficacy and risk was examined on four health outcomes–-message acceptance, talking about breast cancer, information seeking, and behavioral intentions. For African American women, SLOC had a positive impact for talking about breast cancer through an interaction with risk and efficacy such that women high in both SLOC and perceived efficacy, but low in perceived risk were more likely to talk about breast cancer than when efficacy was low. However, high SLOC exacerbated the negative effects of efficacy on talking about breast cancer regardless of the risk level for Caucasian women. SLOC also had a positive influence on attending to breast cancer information in the media for African American women. SLOC played no role in attending to breast cancer information for Caucasian women. Interestingly, SLOC played no role for African American women on behavioral intentions, however, it worked to decrease behavioral intentions for Caucasian women when risk was high.
There are significant differences in breast cancer death rates among different racial groups, and these differences have increased over the last decade. According to American Cancer Society (ACS, 2006), breast cancer results in the second highest mortality rate of all cancer types among women. When all ages are considered, Caucasian women have a higher incidence of breast cancer than African American women. However, the survival rate is lower among African American women than among Caucasian women (ACS, 2006). This disparity exists despite reports that the level of breast cancer screening is equal between the two groups (NCI, 2005). Further, the gap in mortality rates has not improved for African American women over the last decade (U.S. Cancer Statistics Working Group, 2006). The reasons for racial disparity in breast cancer mortality are likely complex, and several factors may play a role in the disparity among mortality rates, such as the quality of breast cancer treatment, differences in information seeking, as well as social/cultural factors that may affect communication between patients and health care providers.
Researchers have tried to find reasons why breast cancer outcomes seem to vary, in part, as a function of race (Hughes, Lerman & Lustbader, 1996). Numerous studies have reported that prevailing attitudes of pessimism and fatalism regarding cancer among African Americans are significant barriers to process cancer prevention messages and to further participate in cancer prevention (ACS, 1981; ACS, 1989; Cardwell & Collier, 1981; Denniston, 1981; Freeman, 1989; Guillory, 1987; Hall & Bell, 1985; Michielutte & Diseker, 1982; Price, Desmond & Wallace, 1988; USDHHS, 1987). Powe (1996), for example, reported that cancer fatalism was a major inhibitor to participation in cancer screening among African Americans. Some researchers emphasized spirituality and religion in understanding African American women's attitude and belief toward breast cancer (Clarke-Tasker, 1993; Phillips, Cohen & Moses, 1999). Clarke-Tasker (1993), for example, noted that historically, religion and spirituality have played a crucial role in the lives of African American. Jennings (1996) reported that African American women may believe that breast cancer screening is futile in the face of God's will because God can still inflict breast cancer upon them. This line of research implies that African American women may process breast cancer prevention messages differently from Caucasian women. Fatalism, spirituality, and religion seem to influence how African American women process breast cancer prevention messages.
Recently, research has moved away from fatalistic beliefs and toward health locus of control. Beliefs about what controls a person's health (health locus of control) are associated with breast cancer screening behaviors. For African American women, an important dimension of health locus of control is spiritual–-the belief that God has control over health. Holt, Clark, Kreuter, & Rubio (2003) found that spiritual health locus of control (SLOC) is comprised of active (God empowers individual) and passive (God has control) sub-dimensions. It is, however, not clear how these variables can be explained in the context of health message processing theories such as the Extended Parallel Process Model (EPPM, Witte, 1992) and the Risk Perception Attitude framework (RPA, Rimal & Real, 2003).
Inspired by the EPPM model and the RPA framework, the purpose of the current study is to compare and test whether African American women and Caucasian women process breast cancer prevention messages differently. More specifically, we attempt to explore how SLOC may interact with perceived efficacy and perceived risk, and how that interaction influences the likelihood of accepting media message recommendations, communicating with others about breast cancer, seeking more information about breast cancer, and self-protection behaviors (e.g. getting a mammogram).
By empirically testing the role of cultural (SLOC) and ethnic (race) factors in message processing in the context of health communication models, the findings of this research will significantly contribute to developing effective breast cancer prevention messages targeting different ethnic groups.
The Extended Parallel Process Model(EPPM)
Fear appeals have long been employed in various health campaigns to motivate people to perform adaptive behaviors. In breast cancer prevention campaigns, for example, it has been reported that fear appeal messages affect accessibility of attitudes toward the threat and adaptive behaviors that, in turn, lead to behavioral intentions to perform breast self-examinations (Roskos-Ewoldsen, Yu, & Rhodes, 2004). While most fear appeal models focused on explaining the process associated with message acceptance, Witte (1992) suggested that it is critical to explore both the process that may facilitate message acceptance and the process that may lead to message avoidance. Drawn from Leventhal's danger-control/fear-control framework (Leventhal, Watts, & Pagano, 1967) and Rogers’ (1975) Protection Motivation Theory (PMT), Witte (1992) proposed the EPPM in which she identified specific conditions leading to message acceptance and rejection processes from key constructs: threat, efficacy, and fear. There are three key arguments in the EPPM. First, there is a difference between fear and threat such that fear and threat generate different outcomes. Second, fear is the key to understanding the message rejection processes. Lastly, the interactions between threat and efficacy are the primary determinants of message outcomes (i.e. acceptance or rejection).
More specifically, Witte (1992) explained that an individual is involved in two appraisals when they are exposed to fear appeal messages. First, individuals evaluate the perceived threat in the message. If the appraisal of threat produces moderate to high perceived threat, then fear is generated (Easterling & Leventhal, 1989; Lang, 1984). Consequently, individuals are motivated to begin the second evaluation–-an appraisal of the efficacy of the recommended response. When the perceived threat is low, however, individuals will ignore the message and thus, there is no need to evaluate efficacy. When both perceived threat and efficacy are high, the processing moves to the danger control by thinking of ways to avert the threat. When perceived threat is high but perceived efficacy is low, fear control processes are initiated. The fear elicited from a significant threat in a message becomes intensified when individuals believe that they cannot effectively deter the threat. This will motivate individuals to cope with their fear by engaging in maladaptive responses, thus leading to message avoidance or rejection.
In summary, perceived threat determines the intensity of the reaction to the messages, whereas perceived efficacy determines the nature of the reaction (i.e. danger control, fear control, Witte, 1992, p. 338). Drawn from the EPPM model, Rimal and Real (2003) proposed the RPA framework, in which they formulated four specific audience segments (i.e. responsive, avoidance, proactive, indifference) as a function of perceived risk and efficacy.
The Risk Perception Attitude Framework(RPA)
Drawn from the EPPM, the RPA framework (Rimal & Real, 2003) suggests that the effect of perceived risk on health behaviors will be moderated by people's efficacy beliefs. One of the differences made in the RPA compared to the EPPM is audience segmentation. Audience segmentation in health campaigns is critical, argue Rimal and Real, in that messages can be designed specifically for the needs of the target audience. Rimal and Real (2003) formulated four attitudinal groups based on individuals’ perceived risk and efficacy beliefs. The first group is the responsive group. Individuals with a responsive attitude have high perceived risk and high efficacy beliefs. They are likely to be most motivated to engage in self-protective behavior. The second group is the avoidance group. Here, individuals have high risk perceptions and low efficacy beliefs and are characterized by an avoidance attitude. The third is the proactive group. Here, people have low risk perceptions but high efficacy beliefs and are characterized by a proactive attitude. Individuals in this group are motivated by their desire to maintain their health or to remain disease free. The fourth group is the indifferent group. Here, people have low perceived risk and low efficacy beliefs. People in this group do not believe they are vulnerable, and therefore, they are the least likely to be motivated in process health-related information.
Rimal and Real (2003) reported that the responsive group (efficacy beliefs high, perceived risk high) showed healthier outcomes than the avoidance group (efficacy beliefs low, perceived risk high); and the proactive group (efficacy beliefs high, perceived risk low) reported healthier outcomes than the indifference group (efficacy beliefs low, perceived risk low). In sum, given a particular level of perceived risk, those with higher efficacy beliefs are likely to show more positive health outcomes than those with lower efficacy beliefs.
Sloc, Perceived Threat, Perceived efficacy
Research findings suggest that African Americans may believe that illness such as breast cancer is closely related to their failure to live according to God's will. African American women, therefore, may believe that harmony or disharmony with God influences their breast cancer (Phillips et al. 1999, p. 569). The influence of SLOC may be a potential facilitator or barrier to breast cancer prevention message processing.
However, there are, to our knowledge, few studies that explain how spiritual beliefs about one's health may influence perceived threat and efficacy. Does SLOC of African American women increase their perceived efficacy while decreasing their perceived threat? Or does SLOC decrease African American women's perceived efficacy while increasing perceived threat? Does SLOC work differently for African American women than for Caucasian women? There is a dearth of research that explains how African American women's SLOC may interact with perceived threat and efficacy and further, how the interactions may lead to message avoidance or acceptance.
The research questions addressed in the current study ask, in a breast cancer context, how ethnic (race) and cultural (SLOC) factors interact with perceived risk and efficacy beliefs represented in the four specific segments in the RPA framework. How do these relationships influence health outcomes, such as talking about breast cancer, acceptance of breast cancer information, seeking information about breast cancer, and the intentions to engage in breast cancer detection behaviors?
Method
A survey was conducted in conjunction with another CDC-funded research project on African American newspapers. Because of this, eleven cities with fairly large black populations served as the sampling frame. These cities were Dallas, Houston, Chicago, Detroit, Baltimore, Milwaukee, Nashville, Buffalo, Richmond, Kansas City, and Jacksonville. The number of completed surveys was 446 (240 Caucasian women; 206 African American women).
The response rate was 50%. The survey was in the field from February through June 2004, rotating through the sampled cities during this time. See Appendix A for technical details of the survey.
Criterion Variables
Message acceptance
Message acceptance was measured as the response to the following two items: Now I want you to recall the last time you saw or heard about the breast cancer in the media: The information convinced me; I learned a lot about breast cancer from the information. Respondents were asked to respond on a 7-point scale, where 1 = strongly disagree and 7 = strongly agree. A composite index was computed separately for the African American (r = 0.49, p < 0.01) and the Caucasian samples (r = 0.55, p < 0.01).
Talking about Breast cancer
Talking about breast cancer was measured as the response to the following two items: I talk about breast cancer with my friends; I talk about breast cancer with my family. Respondents were asked to respond on a 7-point scale, where 1 = strongly disagree and 7 = strongly agree. The mean was computed separately for the African American (r = 0.61, p < 0.01) and the Caucasian samples (r = 0.53, p < 0.01).
Information Seeking
Respondents were asked to rate how often they paid attention to breast cancer information in four media: television, radio, newspapers, and magazines on a 4-point scale were 1 = not at all and 4 = a lot. The mean was computed separately for the African American (alpha = 0.77) and the Caucasian samples (alpha = 0.75).
Behavioral Intention
Respondents were asked to report via yes/no responses if they had ever conducted a breast self-examination, if they ever had a mammogram, if they planned to have a mammogram in the future and if they planned to have a mammogram in the next 6 months. The items were summed to create a 0–4 scale, where the higher the number, the more behaviors the participants reported.
Predictor Variables
Spiritual Health Locus of Control(Sloc)
The SLOC measure was adopted from Holt et al. (2003). They found that SLOC was a two dimensional concept, where one dimension reflected an active belief in God's role in health, and where the other dimension reflected a passive belief in God's role in health. As with Holt et al. the active dimension was measured as the response to two items: If I lead a good spiritual life, I will stay healthy; If I stay healthy, it is because I am right with God. The passive dimension was measured as the response to two items: I rely on God to keep me in good health; Through my faith in God, I can stay healthy. Respondents were asked to respond on a 7-point scale, where 1 = strongly disagree and 7 = strongly agree.
Although SLOC was conceived of having two dimensions in prior research, our factor analysis showed that these four items loaded on one factor (Eigenvalue = 3.02, 75.54% variance explained). Further the factor loadings of the four items ranged from 0.844–0.901. Therefore we opted to create a single composite index for SLOC by averaging across the four items (African American sample alpha = 0.80; Caucasian sample alpha = 0.89). Admittedly, we lose the dimensionality of the concept, but we gain measurement precision as well as a clearer analytic interpretation of how SLOC interacts with efficacy and risk on our outcome measures.
Perceived Efficacy
Perceived efficacy was measured as the response to the following four items: I avoid some behaviors because they may cause breast cancer; There are many things I can do to avoid breast cancer; I follow some behaviors because they may prevent breast cancer; I avoid some places because exposure might cause breast cancer. The first and fourth items were reversed so that a higher value on all four items reflected higher perceived efficacy. Respondents were asked to respond on a 7-point scale, where 1 = strongly disagree and 7 = strongly agree. The mean was computed separately for the African American sample (alpha = 0.67) and for the Caucasian sample (alpha = 0.59).
Perceived Risk
Perceived risk was measured as the response to the following three items: How likely do you think it is that you will get breast cancer? (1 = very unlikely; 5 = very likely), I never think that I might have breast cancer (scaled flipped; 1 = strongly disagree; 7 = strongly agree). The items were standardized, then the mean was computed separately for the African American sample (r = 0.32, p < 0.01) and for the Caucasian sample (r = 0.30, p < 0.01).
Control Variables
Three control variables were measured, age, education, and income, and were measured in standard survey questions. See Appendix B for demographic statistics.
Results
The three predictor variables of interest–-SLOC, efficacy, and risk–-were dichotomized for each sample of African American and Caucasian women by splitting each variable at its median. This strategy was employed to aid in the interpretation of two- and three-way interactions. A series of three-way ANCOVA tests was conducted to explore the differentiated effects of spirituality on four criterion variables between African American and Caucasian women: message acceptance, talking about breast cancer, information seeking, and getting a mammogram. Each ANCOVA model was a 2 (SLOC) x 2 (efficacy) x 2 (risk) test on each of the four criterion variables, with age, education, and income serving as controls. Each ANCOVA was run separately for African American women and Caucasian women.
Effects on Message acceptance
Results from neither African American nor Caucasian women demonstrated any significant relationship with message acceptance. Among African American women, no main effect was significant (SLOC, F(1,158) = 2.48, p = 0.12; efficacy, F(1,158) = 0.19, p = 0.67; risk, F(1,158) = 0.24, p = 0.63). While the three-way interaction on message acceptance approached significance (F(1,158) = 2.95, p = 0.09), two-way interactions were not significant (SLOC x efficacy, F(1,158) = 0.26, p = 0.61; SLOC x risk, F(1,158) = 3.14, p = 0.08; efficacy x risk: F(1,158) = 0.12, p = 0.74). Among Caucasian American women, the main effects (SLOC, F(1,178) = 0.45, p = 0.50; efficacy, F(1,178) = 0.141, p = 0.71; risk, F(1,178) = 0.00, p = 0.99), the two-way interactions (SLOC x efficacy, F(1, 178) = 0.14, p = 0.71; SLOC x risk, F(1,178) = 0.13, p = 0.72; efficacy x risk, F(1,178) = 0.45, p = 0.50), and the three-way interaction (SLOC x efficacy x risk, F(1,178) = 0.02, p = 0.89) were not significant, either.
Effects on Talking about Breast cancer
The results from two three-way ANCOVAs revealed quite different paths through which SLOC affected the extent to which African American and Caucasian women talked about breast cancer. Among African American women, the three-way interaction between SLOC, efficacy, and risk was significant, F(1,167) = 4.27, p = 0.04, η 2 = 0.027. Table 1 shows that African American women with high SLOC who felt highly efficacious and less risky talked most about breast cancer (M = 5.49, SD = 1.80). However, women with low SLOC who had low efficacy and low risk beliefs talked less about breast cancer. No main effects of SLOC (F(1,167) = 0.84, p = 0.36), efficacy (F(1,167) = 0.75, p = 0.39), and risk (F(1,167) = 1.55, p = 0.22) were significant. None of the two-way interactions were significant: SLOC x efficacy (F(1,167) = 0.92, p = 0.34), SLOC x risk (F(1,167) = 1.45, p = 0.23), and efficacy x risk (F(1,167) = 1.76, p = 0.19).
Interaction between SLOC, efficacy, and risk on talking about breast cancer: African American women.
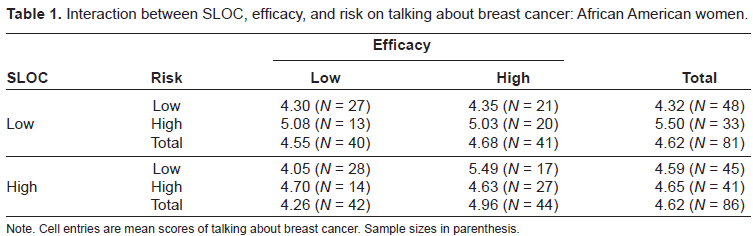
Note. Cell entries are mean scores of talking about breast cancer. Sample sizes in parenthesis.
Meanwhile, Caucasian women of high efficacy were marginally more talkative about breast cancer than those of low efficacy, F(1,186) = 2.80, p = 0.10. The other predictor variables (SLOC, F(1,186) = 0.01, p = 0.92; risk, F(1,186) = 1.96, p = 0.16) did not produce any significant main effects. With respect to the interaction terms, SLOC x efficacy was significant, F(1,186) = 5.18, p = 0.02, η 2 = 0.029.
Table 2 shows how SLOC interacted with efficacy among Caucasian women for talking about breast cancer. When SLOC was low, there was no mean difference between the high- and low efficacy groups. However, when SLOC was high, high efficacy beliefs produced marginally more talking (M = 4.63) while low efficacy beliefs produced less (M = 3.66). The interaction between SLOC and risk approached significance (F(1,186) = 3.12, p = 0.08), while others–-efficacy x risk (F(1,186) = 0.02, p = 0.88) and SLOC x efficacy x risk (F(1,186) = 0.15, p = 0.70)–-were not significant.
Interaction between SLOC and efficacy on talking about breast cancer: Caucasian women.
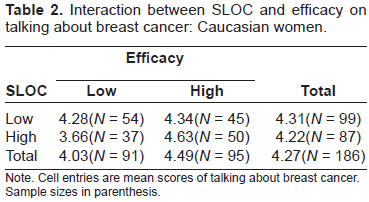
Note. Cell entries are mean scores of talking about breast cancer. Sample sizes in parenthesis.
Effects on Information seeking
Different predictor variables appeared to make African American and Caucasian women seek breast cancer information. The results from African American women indicated that only SLOC had a significant effect on paying attention to breast cancer information in the media, F(1,167) = 5.88, p = 0.02, η 2 = 0.036. Women high in SLOC (M = 3.00, SD = 0.84) tended to seek more information than women low in SLOC (M = 2.72, SD = 0.78). The effect of risk was marginal (F(1,167) = 2.76, p = 0.10), and the others were not significant: efficacy (F(1,167) = 1.65, p = 0.20), SLOC x efficacy (F(1,167) = 2.67, p = 0.11), SLOC x risk (F(1,167) = 0.12, p = 0.73), efficacy x risk (F(1,167) = 0.17, p = 0.68), and SLOC x efficacy x risk (F(1,167) = 2.64, p = 0.11). Among Caucasian women, the effect of efficacy was significant, F(1,186) = 4.03, p = 0.05, η 2 = 0.022. The attention level of the high efficacy group (M = 2.77, SD = 0.67) was higher than the low efficacy group (M = 2.52, SD = 0.79). Risk also had a marginal effect (F(1,186) = 3.10, p = 0.08) among Caucasian women. There were no other significant effects: SLOC (F(1,186) = 0.01, p = 0.92), SLOC x efficacy (F(1,186) = 0.00, p = 0.99), SLOC x risk (F(1,186) = 0.13, p = 0.72), efficacy x risk (F(1,186) = 0.08, p = 0.79), and SLOC x efficacy x risk (F(1,186) = 0.03, p = 0.87).
Effects on Behavioral intentions
Differences between African American and Caucasian women were also detected in predictor variables for behavioral intentions. Among African American women, the interaction between efficacy and risk produced a significant effect, F(1,167) = 8.59, p < 0.001, η 2 = 0.052. As shown in Table 3, the mean decreased from 3.58 (SD = 0.53) for the low efficacy group to 3.18 (SD = 0.98) for the high efficacy group when risk was perceived to be low. In contrast, the mean increased from 3.41 (SD = 0.84) for the low efficacy group to 3.70 (SD = 0.62) for the high efficacy group when perceived risk was high. The rest of independent variables were found not to have significant effects on behavioral intentions: SLOC ((1,167) F = 1.51, p = 0.22), efficacy (F(1,167) = 0.24, p = 0.62), risk (F(1,167) = 2.37, p = 0.13), SLOC x efficacy (F(1,167) = 0.01, p = 0.91), SLOC x risk (F(1,167) = 2.59, p = 0.11), and SLOC x efficacy x risk (F(1,167) = 0.99, p = 0.32).
Interaction between efficacy and risk on behavioral intentions: African American women
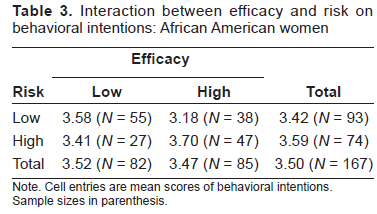
Note. Cell entries are mean scores of behavioral intentions. Sample sizes in parenthesis.
Among Caucasian American women, the main effect of SLOC was significant, F(1,186) = 4.31, p = 0.04, η 2 = 0.024. The women low in SLOC (M = 3.54, SD = 0.73) were more likely to engage in detection behavior than women high in SLOC (M = 3.21, SD = 0.86). Efficacy was also found to have a significant effect on behavioral intentions, F(1,186) = 4.52, p = 0.04, η 2 = 0.025. The high efficacy group (M = 3.52, SD = 0.68) was more likely to engage in detection behavior than the low efficacy group (M = 3.24, SD = 0.91). The effect of risk was not significant (F(1,186) = 0.18, p = 0.67). For the interaction effects, SLOC x risk had a significant effect on behavioral intentions (F(1,186) = 3.80, p = 0.05; Table 4), where low SLOC women with high risk perceptions were the most likely to engage in detection behavior, while high SLOC women with high risk perceptions were the least likely to engage in detection behavior. The other interactions were not significant: SLOC x efficacy (F(1,186) = 0.31, p = 0.58), efficacy x risk (F(1,186) = 1.50, p = 0.22), and SLOC x efficacy x risk (F(1,186) = 0.01, p = 0.95).
Interaction between SLOC and risk on behavioral intentions: Caucasian women.
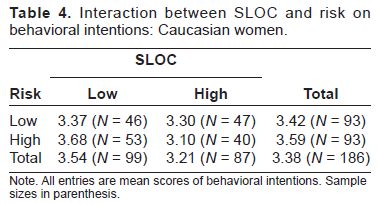
Note. All entries are mean scores of behavioral intentions. Sample sizes in parenthesis.
Discussion
The current study attempted to test a model of the process associated with how African American and Caucasian women process breast cancer information. A survey was conducted across eleven cities in which African American and Caucasian women were asked to report on their levels of spiritual health locus of control, their perceived risk and efficacy attitudes about breast cancer, and their level of talking about breast cancer, information seeking, message acceptance, and behavioral intentions to perform breast self-examinations and to get mammograms. The relationships between SLOC and risk and efficacy attitudes were of particular interest in this study, especially how those relationships differed between African American and Caucasian women.
For African American women, SLOC had a positive impact for talking about breast cancer. SLOC interacted with risk and efficacy such that high SLOC women with high efficacy and low risk were more likely to talk about breast cancer than when efficacy was low. However, high SLOC exacerbated the negative effects of efficacy on talking about breast cancer regardless of the risk level for Caucasian women.
This finding is contrary to the previous studies that argued the negative effects of SLOC on African American women's health behaviors (Underwood, 1992). Our findings can be explained by two ways. First, according to Hughes et al. (1996), the spiritual orientation of African Americans has a significant impact on their mode of coping (e.g. stress, risk, etc.) in that it leads African American women to positively re-appraise their situations. When referring to this argument, our findings suggest that despite their realization of a certain level of risk, those African American women whose SLOC was high seemed to re-appraise their situation and to engage more with breast cancer information, either through media or through interpersonal discussion. Welton and colleagues (1996) also found that their participants rating high on God control tried to seek emotional support and practical advice from others (p. 22) when facing a difficult situation.
Another way to look at this result comes from Hathaway and Pargament (1991). They suggested that there are three types of coping that are related to the interpretations of the relationship of God and self: 1) the self is passive and responsibility for coping is placed under God's control; 2) God is passive while the self is active; and 3) both God and the self are active, working together to deal with the stressor. When referring to this way of explanation, previous studies may focus on the first interpretation of the perception of God and self (i.e. passive self and coping is under God's control), thus reporting the negative effect of spirituality on health behaviors. In concert with Holt et al.'s (2003) conceptualization of SLOC, our study suggests that African American women in our sample likely perceived both God and the self as active. This perception seems to encourage African American women to seek more information and to talk about breast cancer in order to seek emotional support and helpful advice.
Interestingly, SLOC played no role for African American women on behavioral intentions. Instead risk and efficacy interacted so that those with high levels of each were most likely to engage in detection behaviors. However, SLOC worked to decrease behavioral intentions for Caucasian women when risk was high.
The significance of our study are several. First, theoretically, we incorporated a cultural factor–-SLOC–-into a health communication model and empirically tested the role of SLOC in African American women's message processes. By embracing cultural and ethnic factors, our study contributes to developing a more holistic health message processing model to better understand processes associated with health message rejection and acceptance when targeting diverse ethnic groups. From a practical standpoint, our results indicate that when a breast cancer prevention message is designed for African American women, health communicators should consider how to “positively” utilize the role of SLOC in African American women's health message processing. Further, our African American sample reported to respond to breast cancer detection behaviors in ways in which current message processing models (EPPM and RPA) predict.
As with all research, this study has its limitations. The reliabilities of certain variables are lower than we would like. This could be due to several factors. First, the survey was in the field for longer than is usually the case. This situation was mandated by the original purpose of the research, which was to sample cities in which other CDC-funded projects were occurring. Also, while there was an attempt to utilize items used in prior health communication research, especially in measuring perceived efficacy and risk, we were not altogether successful.
Future research should continue to examine the role SLOC plays in both African American and Caucasian samples on other health outcomes and in other health contexts. One suggestion would be to examine how SLOC works with efficacy and risk beliefs on threat-induced fear. Prior literature suggests that spirituality may affect a person's level of fear with respect to health-related messages, but at this point, it is not clear how.
Footnotes
Acknowledgements
This study was funded by the Health Communication Research Center (HCRC) at the University of Missouri-Columbia through a grant from Centers for Disease Control and Prevention. Cancer Prevention Programs Number U57/CCU723093-01
Appendix A
Appendix B
Sample Demographic descriptive statistics.
1.
Of the 483 completed interviews, six surveys were conducted to female residents that did not meet the age requirement of the study. Of the 476 surveys, 240 were Caucasian women, and 206 were African American women. In addition, 15 were Latino/Hispanic, 4 Asian/Pacific Islanders, 5 American Indian, 2 others, and 4 refused to identify their ethnicity.
2.
Majority of the Ineligible numbers were residential households that did not meet the age requirement (2,433). Other ineligibles included those of (1) there was no adult available, (2) there were no permanent residents, (3) group homes, (4) cell phone, (5) pay phone, and etc.
3.
Communication barriers are defined as those that could not be communicated in English, are hearing impaired, and etc.
4.
Ring-no-answers are defined as the phone numbers in which no one answered to any of the eight attempts made during the period when the project was implemented.
5.
Callbacks are defined as the numbers in which someone answered during the project implementation period but a callback was scheduled because the selected person was not available.
