Abstract
Background:
The onset of the COVID-19 pandemic has contributed to increased stress among healthcare professionals. Among these healthcare providers are Ontario pharmacists, who are facing new and pre-existing challenges and new stressors since the pandemic.
Objectives:
This study aimed to understand the stressors and lessons learned by Ontario pharmacists during the pandemic through their lived experiences.
Methods:
In this descriptive qualitative study, we conducted semi-structured one-on-one interviews with Ontario pharmacists virtually to learn about their stressors and lessons learned during the pandemic. Interviews were transcribed verbatim, then analyzed using thematic analysis
Findings:
We reached data saturation after 15 interviews and identified 5 main themes: (1) Communication/miscommunication with the public and other care providers; (2) high workload due to staff shortage and low appreciation/acknowledgement; (3) mismatch in market demand and supply; (4) informational gaps pertaining to the COVID-19 pandemic along with rapid protocol changes; and (5) lessons learned to improve the future of pharmacy practice in Ontario.
Discussion:
Our study helped us gain a better understanding of the stressors pharmacists faced, their contributions, and the opportunities that arose due to the pandemic.
Conclusion:
Drawing on these experiences, this study provides recommendations to improve pharmacy practice and increase preparedness for future emergencies.
Introduction
The challenges brought by the COVID-19 pandemic increased stress, anxiety, and other mental health consequences for healthcare professionals, including pharmacists, which contributed to high rates of burnout.1 -4 Results from a national survey on pharmacists during the pandemic showed higher levels of burnout due to new pressures such as reduced staffing, increased hours, and insufficient medication supply. 5 Notably, the psychological impact was not introduced by the pandemic; rather, it was exacerbated, as these pressures are not new in pharmacy. Specifically, pharmacists are often overlooked members of the healthcare system, which was evident during the pandemic.
Pharmacists experienced an increased workload dealing with their traditional duties and COVID-related tasks. 6 The traditional duties of pharmacists required greater efforts as the pandemic increased the complexity of their typical delivery of care. For example, they experienced an influx of patients and worked longer hours. Despite the challenges brought by the pandemic, pharmacists implemented novel strategies to optimize the delivery and accessibility of services to patients and played a vital role in the prevention and treatment of COVID-19.6,7 Furthermore, due to the limited access to physician care, pharmacists played a crucial role in helping patients with chronic diseases manage their health. 8 Additionally, most Ontario pharmacies became primary sites for COVID-19 testing and vaccination and dispensation of COVID-19 therapeutics (eg, Paxlovid).
Despite the availability of some national data on the stressors of pharmacists during the pandemic, 8 province-focused evidence remains scant. Furthermore, determining pharmacist-focused strategies to improve service provision among Canadian pharmacists is still not well explored. Identifying the stressors and providing recommendations for the future of pharmacy is crucial to strengthen the noted issues and strain on the current pharmacy industry. 1 Gaining insight into these variables is necessary as it impacts the pharmacists, the patients, and the healthcare system.
The purpose of this descriptive qualitative study was to identify and understand the stressors of working during the pandemic and explore future opportunities in the field of pharmacy based on the lessons learned drawn from their experiences. Specifically, by gaining insight into their experiences, this study sought to establish sustainable and effective methods to improve pharmacy service delivery.
Methods
We conducted one-on-one interviews with Ontario pharmacists. We obtained REB approval from the University of Guelph Research Ethics Board (20-06-044). Participants were recruited through a partnership with OnPharm, a provincial association of 350 community pharmacies, who helped disseminate our study’s information to their members. Additionally, participants were recruited through a snowballing technique, as participants were encouraged to share the study with their colleagues. Eligible participants were registered Ontario pharmacists who worked through the first 2 waves of the pandemic, from January 2020 to March 2021. Interested participants directly contacted the supervising researcher (BG). Informed consent was obtained in writing and verbally before each interview. Participants received a $25.00 gift card as a token of appreciation.
Interviews were conducted virtually through Cisco Webex®9 or by phone. The researcher (BG) used a semi-structured interview script to conduct the interviews (Supplemental Appendix A). Participants were initially asked about demographic information (gender, age, and relationship status) and the characteristics of their pharmacy (area of practice and services offered). Next, they were asked to describe the stressors that arose from the first and second waves, how they dealt with them, and if they had any lessons learned for future emergencies to reduce stressors and improve service delivery. Member checking was applied regularly during the interviews to ensure the validity of the information. 10
The audio-recorded interviews were transcribed verbatim into text. The coder (ZZ) reviewed all the transcriptions while listening to the audio to ensure the accuracy of the transcripts and to de-identify the transcripts, followed by reading the transcripts 2 additional times. This method allowed the researchers to familiarize themselves with the data further. 11
Braun and Clarke’s 11 steps of thematic analysis were applied as a structured approach to developing codes and themes. Following the familiarization phase, BG and ZZ inductively coded the data using Quirkos software. 12 Each researcher read through the transcripts highlighting important notes such as the similarities and differences across the data. Based on these patterns, initial codes were generated, and the transcripts were reviewed again, with the codes being applied as appropriate. Next, codes with similar content were combined and merged to form themes. After their independent analysis, both researchers met to review and finalize their themes. Finally, these themes were iteratively reviewed to ensure their relevance to the broader theme.
Findings
We reached data saturation after interviewing 15 participants. The average interview length was 43 minutes. Six participants identified as women and 9 as men. Their age ranged between 26 and 48 (M = 34). Eight pharmacists held management or ownership positions. Thirteen participants worked in an independent community setting, and 2 worked in a chain setting. Participants were from various locations across Ontario, including the northeastern, central, southeastern, and southwestern regions (Table 1).
Participant demographic information.

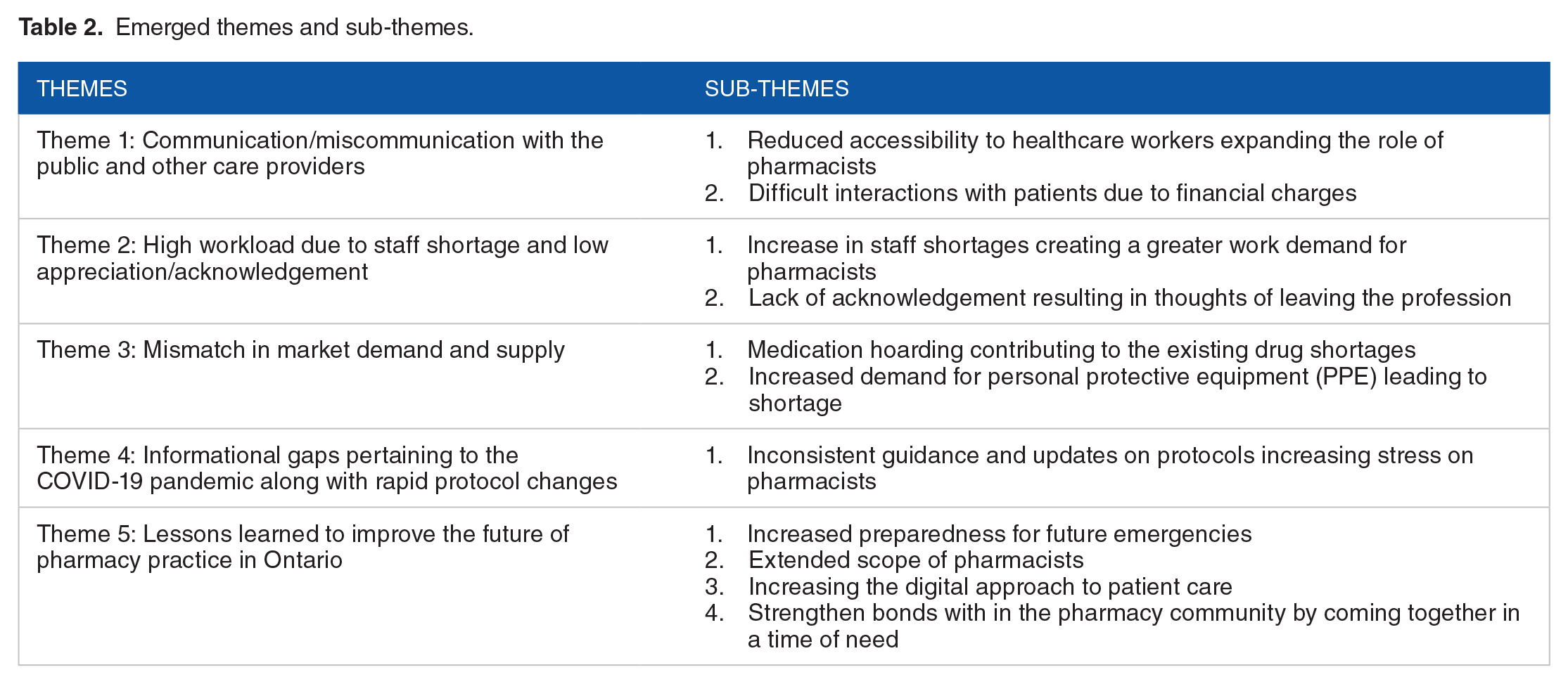
We identified 5 main themes: (1) Communication/miscommunication with the public and other care providers; (2) high workload due to staff shortage and low appreciation/acknowledgement; (3) mismatch in market demand and supply; (4) Informational gaps pertaining to the COVID-19 pandemic along with rapid protocol changes; and (5) lessons learned to improve the future of pharmacy practice in Ontario (Table 2). Please see Figure 1, which depicts the 4 stressor-related themes and their consequences.
Emerged themes and sub-themes.

Thematic map of the identified stressor themes (excluding theme 5) and their interconnectedness. The 4 dark blue rectangles represent the identified stressor themes contributing to pharmacists’ experience during the pandemic. The lighter rectangles represent the subthemes. The solid line delineates the connection between the theme and subthemes. The dotted lines represent the connected implications across themes and subthemes based on the participants’ experiences.
Theme 1: Communication/miscommunication with the public and other care providers
Our results revealed the transition of other HCP working remotely reduced their accessibility creating communication challenges (Table 3). Pharmacists stress increased as they struggled to communicate with physicians. This required pharmacists to “essentially play quarterback,” (P13) ensuring patients were receiving quality care. Being at the forefront, participants found themselves as a primary site of care for assessing and triaging patients’ symptoms. They indicated that they were “harassed” (P13) by some patients for medications and had to “chase down doctors for prescriptions” (P13).
Theme 1 and subthemes with selected excerpts.

Second, participants voiced concerns regarding the economic changes straining the patient-pharmacist relationship. Specifically, due to the high demand for personal protective equipment (PPE) early in the pandemic, manufacturers increased costs, translating to increased prices for consumers, leading to patient dissatisfaction. This was of particular concern because at the time, the media was cautioning the public about “price gougers.” Therefore, some pharmacists reported they discontinued selling PPE or sold it at or below cost. Dissatisfaction with costs also occurred because of policy changes made due to medication shortages. Pharmacists reported that they could not dispense more than 30 days of certain types of medication, resulting in patients paying the dispensing fees more times than expected. Finally, patients not wearing masks felt unwelcome by pharmacists.
Theme 2: High workload due to staff shortage and low appreciation/acknowledgement
Our results indicate the pandemic exacerbated the on-going staffing issues in pharmacies (Table 4). Participants reported increased stress as they completed “2 to 3 times” (P4) the amount of work due to staff shortage. Reportedly, the rise in COVID-19 cases has instilled fear among pharmacy workers, leaving workplaces shorthanded. Additionally, pharmacies were understaffed on short notice as per public health self-isolation guidelines. Pharmacists explained that the introduction of the Canada Emergency Response Benefit, a temporary benefit that provided financial support to Canadians affected by COVID-19, provided employees with the option to stay home and receive the benefit instead of working in a high-risk environment. Moreover, the implementation of delivery services also required additional staff and time from pharmacists. Adjusting to the increased turnover rate required them to fulfill the duties of other roles, thus working longer hours with minimal breaks, resulting in burnout.
Theme 2 and subthemes with selected excerpts.

Participants reported feeling unappreciated by the public. As they felt their role has been overlooked for years, some participants were not surprised by the lack of appreciation they received. Pharmacists had to acquire their own PPE and were not prioritized to receive the vaccine compared to other healthcare workers. Participants expressed they felt the burden of other professionals being “placed on [their] shoulders,” (P7) and despite the inherent risk of working in a pharmacy setting, they were not shown gratitude. This resulted in a few participants sharing their thoughts about leaving the profession (n = 4).
Theme 3: Mismatch in market demand and supply
Participants shared concerns regarding drug shortage, which intensified during the pandemic because of medication hoarding (Table 5). Reportedly, during the beginning of the pandemic, patients began stockpiling medications creating a backlog of vital medications. This period was recalled as “living in a nightmare” (P3). Some participants expressed the 30-day supply mandate being beneficial in ensuring an equitable distribution of resources. However, it brought on additional administrative stressors like increased paperwork. Participants also explained that relying on international suppliers for medication has contributed to the shortage of drugs, which is reportedly a pre-existing issue.
Theme 3 and subthemes with selected excerpts.

Our findings indicate the shortages were not limited to medication. Simple instruments such as thermometers were also unavailable. The fear of contracting COVID-19 was heightened among pharmacists as they could not secure PPE to protect themselves in high-risk environments. Some reported taking “extreme” measures to remain safe such as making their own hand sanitizers and finding alternatives for masks.
Theme 4: Informational gaps pertaining to the COVID-19 pandemic along with rapid protocol changes
Our results revealed that because Ontario pharmacists were among the patient-facing healthcare providers (HCP) in the early stages of the pandemic, they faced criticism due to factors outside their control (Table 6). First, the initial uncertainty of the pandemic required participants to intuitively create health and safety guidelines due to perceived untimely guidance from official sources. Consequently, they expressed frustration as they believed these gaps made them appear incompetent in front of patients. For instance, at times, participants reported health information was simultaneously disseminated to pharmacists and the public. Therefore, pharmacists who missed the news announcements reported being informed of updated practices by the public rather than their professional organizations or regulatory bodies.
Theme 4 with selected excerpts.

Theme 5: Lessons learned to improve the future of pharmacy practice in Ontario
Participants advised that Ontario should focus on increasing preparedness in future emergencies based on lessons learned during the pandemic (Table 7). Specifically, they cautioned that outsourcing raw materials from overseas is not advisable. Rather, having local manufacturers can help reduce the chances of facing drug shortages. Participants explained that commonly used generic medications could easily be manufactured locally. Similarly, they recommended domestic PPE production to prevent future supply shortages and their associated stressors. Finally, a participant expressed that despite the previous Severe Acute Respiratory Syndrome (SARS) epidemic, there was limited preparedness for a pandemic. Therefore, increasing preparedness should be crucial so that Ontario is well-equipped to tackle future pandemics.
Theme 5 and subthemes with selected excerpts.
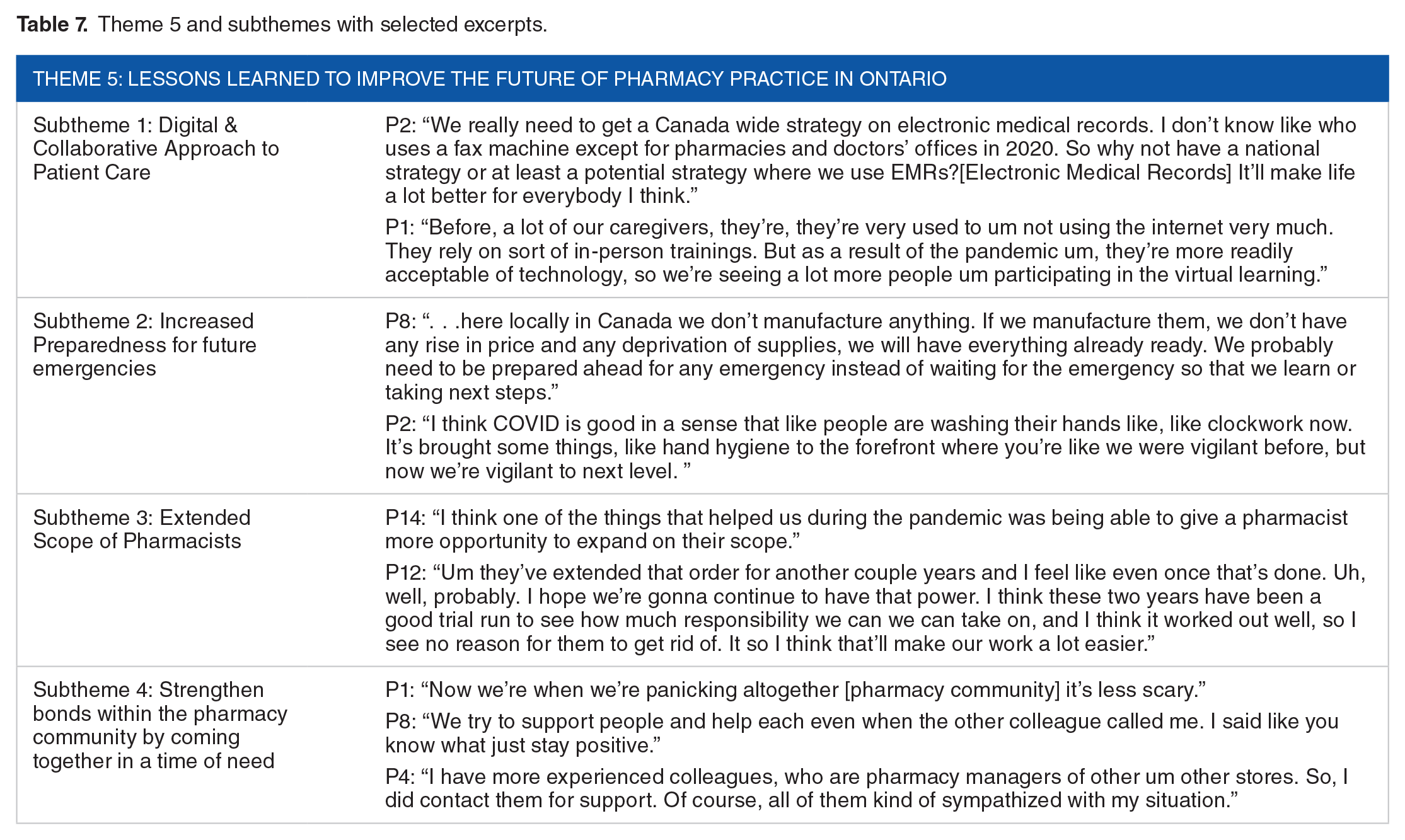
Additionally, participants’ responses showed evidence of the importance of improved safety measures because of the pandemic. The fear of COVID-19 has encouraged pharmacists to be more vigilant about regular sanitation practices that will remain in place after the pandemic. For example, participants reported that handwashing is “like clockwork now.” (P2) Also, plexiglass barriers became permanent fixtures in pharmacies, as they provide safety from other illnesses besides COVID-19.
Participants expressed the pandemic provided Ontario pharmacists with the opportunity to demonstrate they are prepared and willing to practice to the full extent of their knowledge when the healthcare system demands it for the sake of their patients. They noted in some respects, Ontario is more restrictive than other provinces in terms of their scope. Altogether, participants stated this increased authority alleviated some stress by allowing them to use their professional judgment rather than solely relying on primary HCP. Another positive outlook reported was the increased use of technology for educational and streamlining services for clients. Participants explained that in the absence of in-person seminars, they resorted to online platforms, which reportedly improved participation.
Participants explained the pandemic helped strengthen their bonds within the pharmacy community. Community pharmacists mentioned that local pharmacies helped each other when faced with drug or supply shortages. Reportedly, participants found ease in knowing that everyone was together and tackling the pandemic in unity. Additionally, pharmacists took on the role of giving back to the community. One participant mentioned that to avoid accusations of price-gouging, they donated all the profit from the PPE sales to local charities.
Participants reflected on the difficulty communicating with healthcare professionals and emphasized the importance of implementing a streamlined, digital approach to patient care. They explained that utilizing a “universal” electronic medical record would allow for effective communication between all providers involved in the patient’s circle of care. As reported, the current system of using fax machines, while secure, is outdated and inefficient. Alternatively, an approach toward digital healthcare could “make the lives of healthcare workers easier” (P10), especially for those working remotely. Finally, regarding the communication issues that arose, participants proposed having readily available structured guidelines established for pharmacists to adapt to in their practice to reduce stress.
Discussion
This study identified and expanded the understanding of the stressors faced by Ontario pharmacists, along with practical lessons learned to improve service provision. Miscommunication, high workload due to staff shortage and limited acknowledgement, mismatch in market demand and supply, and sudden changes in protocols were among the stressors Ontario pharmacists faced during the pandemic. While these results are unique and distinct, their consequences are intricate. For instance, pharmacists faced communication challenges with their patients. Some of these communication challenges were due to rapid protocol changes along with a mismatch in demand and market supply. This highlights the complexity of the findings, which require careful consideration from a policy perspective.
Drawing on the results, it is evident that several issues faced during the pandemic were pre-existing, and the pandemic intensified them. Staff shortages, increased workload, lack of acknowledgement and drug shortages are on-going stressors faced by pharmacists. The pandemic introduced additional stressors such as communication barriers, PPE shortage, negative perception of pharmacists by the public, and the fear of COVID-19. The findings of our study are consistent with other studies conducted in this area, in which pharmacists identified similar major challenges (medication shortages and patient expectations) and future outcomes for the field of pharmacy.8,13
Our results revealed the sudden onset of the pandemic left pharmacists vulnerable to scrutiny with situations outside their control. For instance, due to the fear of being described as price-gouging, participants reported discontinuing selling PPE or selling them at a loss. These consequences are unsurprising as there is a negative correlation between reputation and price-gouging behaviours. 14 Nevertheless, retail pharmacists were at a disadvantage given the increased costs by the manufacturers due to scarcity while the public, including the media attributed the price increase to price-gouging. Furthermore, failing to receive clear information related to protocol changes in a timely manner was a contributing stressor to Ontario pharmacists, which added to the scrutiny by the public. This finding was consistent with an Australian qualitative study where the pharmacists felt frustrated because of unclear messaging around protocol changes. 15
Participants reported more stress during the pandemic caused by increased work demand and longer hours due to staff shortages. Staff shortage is a concern across various healthcare sectors across the world, including Canada.16 -18 For instance, a recent survey by the Canadian Pharmacists Association found over 50% of participants experience some degree of burnout and staff shortage. 19 Similarly, a study assessing pharmacists’ working conditions reported areas of concern, including inadequate break times, insufficient time to complete tasks, and reduced staffing. 20 Participants expressed feelings of burnout, “[I was] losing sleep, uh probably destroying my health” (P7), because of working long hours, with minimal breaks, to keep the pharmacy afloat. Additionally, they reported that having proper staffing would have been beneficial as it would help distribute the workload.
Despite their efforts, pharmacists reported feeling under appreciated by the public. These feelings are not isolated in the pharmacy community. Specifically, other healthcare workers, such as medical laboratory professionals whose work is often “behind-the-scenes,” experienced little recognition as well. 16 Inadequate appreciation of the healthcare sector contributes to the poor well-being of healthcare workers. 21 Our study found that the lack of recognition combined with the increased workload has introduced thoughts of leaving the profession, implying that pharmacists have been, to some degree, dissatisfied with the working conditions during the pandemic, which is a predictor of intention to leave the profession. 22
The pandemic intensified a long-existing drug shortage issue faced by Canada. Participants emphasized that the drug shortage led to extended time retrieving medication for patients, and if unsuccessful, they needed to offer alternative treatments. Unsurprisingly, this shortage caused disruptions to patient care, workflow, and increased costs for alternative medications. 23 Moreover, with countries like China and India producing almost 80% of the raw ingredients, disruptions to the supply chain early in the pandemic exacerbated the drug shortage. 24 Participants described those outsourcing vital medications as detrimental, and the pandemic emphasized the need to move to local production. To combat the supply chain disruptions, pharmacists were legally restricted to dispensing medication for a 30-day supply only. 25 While this mandate could have led to some backlash (eg, additional dispensing fees) it was effective in overcoming the shortage of medication. Accordingly, shortening the limit supply, especially for vital medications, could provide some relief until other solutions are considered. However, our study emphasizes the need for proper protocol and guidelines to be disseminated to pharmacists prior to any changes to ensure that pharmacists are competent in advising the public.
The 2003 SARS epidemic emphasized the need for changes to be made to the public health and healthcare systems to respond to infectious diseases effectively. 26 However, our findings indicate that despite the lessons learned from that epidemic, the healthcare system remained unprepared. Unsurprisingly, the stressors emerging from the uncertainty of the pandemic, combined with awaiting health guidelines, negatively impacted pharmacists. To that end, having established safety guidelines for airborne viruses would have been more ideal rather than awaiting to examine the severity of the pandemic. 27
While our results revealed several challenges that Ontario pharmacists are facing, it also revealed opportunities that arose from the pandemic. In addition to reporting of improved sanitization practices, our results highlighted the capability and potential of pharmacists within healthcare and their positive influence on their communities despite their lack of recognition. This is an essential finding with favorable implications if pharmacists are utilized adequately.
Limitations
While this undertaking provides important future implications for the field of pharmacy in Ontario, some limitations are worthy of mentioning. First is the inherent limitation in qualitative methodologies where it is difficult to generalize the results. Given the scarcity of information on Ontario pharmacists during the pandemic, a qualitative approach was necessary as a preliminary step to inductively collect information about their stressors and lessons learned. Moreover, as this study was conducted during a relatively stressful time for pharmacists, we were unable to control for pharmacists based on additional obligations (eg, owner and manager) or geographical locations. Notwithstanding these limitations, we reached data saturation rather quickly where participants expressed similar stressors and opportunities, irrespective of additional job roles or geographical locations. Future studies should build on this study in larger scale studies to further examine potential correlates of stress such as job role, pharmacy type, geographical location, and population density.
Recommendations
The results from this study emphasize the need to address the growing crisis of staff shortages in pharmacies. The increased workload and poor working conditions are contributing to feelings of burnout. Thus, there is a need to optimize the workflow in pharmacies, which can be done by ensuring pharmacies are appropriately staffed so the workload can be distributed amongst the staff. Utilizing pharmacy technicians to assist in providing advanced services could reduce pharmacists’ workload and allow them more time to provide clinical services. 19 Additionally, adequate clerical staffing in pharmacies will relieve pharmacists of the burden of having to perform tasks such as faxing or requesting follow-up requests and allow them to allocate this time to patient care. Sharing the tasks amongst staff would allow for scheduled breaks, which is known to help workers’ mental well-being, increase work engagement and reduce errors. 19
Our findings are consistent with existing literature regarding the drug shortage in Ontario. 24 More research is required to examine the current drug shortage in Ontario. For instance, the American Society of Health-System Pharmacists recommended implementing a drug-product shortage team who would be responsible for developing protocols when facing drug shortages. 28 Similar initiatives in Ontario could help reduce drug shortage-related stressors on pharmacists and pharmacy owners in the province by having readily available solutions in face of supply challenges. Additionally, the drug supply relies heavily on the availability of raw ingredients, and thus any barrier to acquiring the raw material will ultimately result in a shortage. 28 Stockpiling may not be a feasible approach considering the shelf-life expectancy of certain drugs. However, evidence suggests that Canada has the technology to produce its own drugs. 29
With high stress levels, the lack of appreciation for pharmacists is a long-standing issue that needs to be addressed. 30 Emphasizing the importance of their role in patient care is necessary for pharmacists to continue to deliver optimal care through their services. 31 This is of utmost importance as meaningful recognition is linked to increased morale and reduced burnout. 32 Furthermore, our results indicated a perceived negative perception of pharmacists by the public. Therefore, emphasizing their role in patient care and appreciating their efforts is of utmost importance to reduce any loss of reputation.
Recognizing pharmacists’ contribution to patient care reinforces advocacy for Ontario pharmacists to be granted authority to work to their full potential with proper compensation. For instance, Alberta has given pharmacists full prescriptive authority to initiate or manage treatment, inject drugs, and order or interpret laboratory test results. 33 The impact of the high numbers of COVID-19 cases led to physician burnout leaving Ontario with a physician shortage. 34 Thus, recognizing the favorable implications on the healthcare system, we recommend policymakers to re-examine Ontario pharmacists’ scope of practice. In doing so, it would be ideal to further integrate pharmacists within the Canadian healthcare system. 35
The introduction of the government’s proposal to expand pharmacists’ scope to assess minor ailments as of January 2023 is promising. 36 This expansion builds on the momentum from the pandemic, where pharmacists became a primary site of care, providing patients with greater access to care. Integrating them into the assessment and treatment process will help improve their sense of inclusion and emphasize the importance of their role as valuable members of the circle of care. However, as pharmacists continue to relieve the burden of the healthcare system, it is crucial to also examine their workload pay structure, as increasing their job role without proper consideration of their current duties or adequate pay would be unjust and would merely worsen a pre-existing issue. Moreover, equitable compensation for tasks common across professions is important.
We also recommend exploring a universal electronic medical record that could be used securely between HCP to improve continuity of care. While fax machines are secure, the stress of the pandemic highlighted their downfalls when primary HCP worked remotely. The implementation of such a model should integrate features from existing models in other provinces, to provide more comprehensive medical records, increasing efficiency and improving patient outcomes.
Though the stress faced by pharmacists during the pandemic is irreversible, it is essential they are provided with the support and resources needed to promote employee wellness. A study assessing pharmacists’ burnout found that the lack of awareness of resources contributed to burnout. 37 Finally, implementing disaster management courses within pharmacy school curriculums can help increase preparedness and be beneficial knowledge for pharmacists to consider in future emergencies. By reflecting on the lived experiences of pharmacists during this pandemic, it is evident that these changes are necessary to improve preparedness in light of future pandemics.
Conclusion
This study’s goals were to provide recommendations to improve pharmacy practice and increase preparedness for future emergencies. Drawing on their experiences, our study identified key themes emphasizing the negative impact on the perception of pharmacists by the public, experiencing increased workload while feeling unappreciated, difficulty acquiring inventory, emerging opportunities because of the pandemic, and recommendations for the future of pharmacy. While some experiences are long-standing in the field of pharmacy, the pandemic has exacerbated the stressors faced by pharmacists contributing to increased stress and poor working conditions. We believe the suggested recommendations of changes to workflow, expanding their scope of practice with proper compensation, improving preparedness, and acknowledging the importance of their role in patient care are expected to reduce the stressors faced by pharmacists. Ideally, the implementation of these changes would improve the working conditions of pharmacists in Ontario, provide pharmacists support and contribute to advancing the profession of pharmacy. In the event of a future pandemic, the findings of this study can play a crucial role in improving the lives of pharmacists by proposing necessary solutions that should be implemented.
Supplemental Material
sj-docx-1-his-10.1177_11786329231169937 – Supplemental material for Behind the Counter: Exploring Pharmacists’ Stressors and Lessons Learned During the Pandemic in Ontario, Canada
Supplemental material, sj-docx-1-his-10.1177_11786329231169937 for Behind the Counter: Exploring Pharmacists’ Stressors and Lessons Learned During the Pandemic in Ontario, Canada by Zoha Zahoor, Andrew Papadopoulos, Behdin Nowrouzi-Kia, Patty Ibrahim, Mina Tadrous and Basem Gohar in Health Services Insights
Footnotes
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Canadian Institutes of Health Research (CIHR; EG7-179466)
Declaration Of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
