Abstract
Unsafe abortion remains one of the leading causes of maternal mortality in sub-Sahara Africa, with relatively poor access to quality postabortion care (PAC) services. This study evaluated the quantity and distribution as well as the utilization of PAC services in Burkina Faso, Cote d’Ivoire, and Guinea. We conducted a secondary data analysis using the most recent EmONC surveys in the 3 countries between 2016 and 2017. We used PAC signal functions approach to assess facilities’ capacity to provide basic PAC at both primary and referral level of care and comprehensive PAC at the referral level. We illustrated population coverage of PAC services based on the WHO benchmark, and then assessed the utilization of PAC services. Basic PAC capacity at primary level was low (36.6%), ranging from 16.2% in Burkina Faso to 36% in Cote d’Ivoire. About 82.0% of hospitals could provide comprehensive PAC. There were disparities in the geographical distribution of PAC services at both national and subnational levels. Abortion complications represented 16.2% of all obstetric emergencies, and uptake of PAC modern contraceptive was low (37.1%) in all countries. There is a need to focus on access to PAC at the primary level of care in the 3 countries.
Keywords
Background
Despite a significant decline in the abortion rate worldwide since 1994, unsafe abortion remains one of the leading causes of death and illness for women and girls, particularly in sub-Sahara Africa (SSA), where abortion is legally restricted in most countries. 1 According to the World Health Organization (WHO) classification of abortion safety, only 1 in 4 abortions in Africa was safe. 1 In this context, West Africa is one of the 4 regions of the continent where an estimated 44% or more of abortions are classified as least safe, with a high risk of adverse health outcomes associated with unsafe abortion. 2 Furthermore, these complications can potentially have serious consequences for women’s health and economic well-being and result in a high cost burden on public health systems.3,4
Most countries in SSA, like many others in the world, have recognized the problem of unsafe abortion as a public health problem at the Cairo International Conference on Population and Development (ICPD) in 1994, 5 and later considered access to safe abortion care through the Maputo protocol as a woman’s right. 6 This recognition resulted in the commitment of the countries that health systems have the responsibility to ensure that abortion is safe in circumstances where it is legally indicated and ensure that postabortion care (PAC) is part of national reproductive health programs and services to reduce deaths to unsafe abortion.
The PAC model was developed to address the harmful health consequences of unsafe abortion, providing essential emergency care to women who are present at health facilities with complications from unsafe or incomplete abortions. 7 PAC has been implemented in many countries, even those with restrictive abortion laws, to address the complications associated with unsafe abortion. The PAC model has been shown to be an acceptable way to improve services provided to women in need without violating local norms or legal restrictions on abortion provision. The model lists 3 essential components: (I) emergency treatment for complications of spontaneous or induced abortion; (II) postabortion family planning counseling and services; and (III) linkage between emergency care for induced abortion and other reproductive health services, such as treatment of sexually transmitted diseases.7,8 The availability of adequate PAC infrastructure and service provision that would allow equitable access and use of quality services by beneficiaries is key to the success of the PAC model. 9 Evidence showed that although access to care among women with unsafe abortion complications has expanded in SSA since 1994 ICPD, the availability of PAC services is still low in SSA.10 -12 In a recent combined facility and household survey in Côte d’Ivoire and Nigeria, Bell et al 13 reported insufficient availability, readiness, and accessibility of PAC services, as well as social inequalities in access to these services in both countries. However, few studies on PAC availability evaluated the geographical distribution along with the amount of services, and most of these studies focused on countries in East and Southern Africa.11,14,15 Moreover, little is known about the utilization of PAC services in SSA, especially for West African countries. 12
The present study aims to fill the knowledge gap on the availability of PAC services and their use in Burkina Faso, Cote d’Ivoire, and Guinea. All 3 countries are located in West Africa and have very poor reproductive health performance, with maternal mortality and unsafe abortion rates among the highest in the world.1,16 Therefore, providing quality PAC is crucial to achieving the maternal health goals of the Sustainable Development Goals (SDGs) by 2030.
Building on previous research that used the signal functions approach to assess abortion and PAC services availability,10,11,14,17 we used nationally representative health facilities data from the evaluation of emergency obstetric and neonatal care (EmONC), of which the PAC is one of the essential components, to specifically assess first the availability of PAC services in and between the 3 countries, and then to determine the use of PAC services by women with abortion-related complications. This will not only fill the scientific evidence gap, but will also provide an updated state of the health system capacity to provide PAC and point out the urgent needs related to access and quality of PAC, to be addressed by policymakers and governments, and also support the implementation of relevant PAC interventions in SSA.
Methods
Study design and settings
We conducted a secondary data analysis of EmONC surveys data from Burkina Faso, Cote d’Ivoire, and Guinea. These SSA countries were chosen based on the criteria of a recent EmONC survey conducted, Burkina Faso in 2016, 18 Côte d’Ivoire, 19 and Guinea in 2017. 20 We received authorization from respective countries’ Ministries of Health to use the data.
Like many other African countries, the health system in all 3 countries is pyramidal in type, with an administrative side and a care delivery side. Public health facilities are organized into 3 levels that provide primary, secondary, and tertiary care. The first level of care in Burkina Faso consists of 2 sublevels, with primary health facilities that can refer to district hospitals. The private health sector, essentially present in large cities or economic centers, fits into the different levels of the health pyramid.
Sociodemographic and maternal health indicators are summarized in Table 1 for the 3 countries: mortality rates are very high for the 3 countries, with high fertility rates and low use of contraceptives. Abortion in the 3 countries is highly restricted and permitted only when the mother’s life is at risk or in cases of rape or incest. In Burkina Faso, safe abortion is also allowed in cases of severe fetal malformation.
Reproductive health indicators in the 3 countries.

Source: Burkina Faso (National general population and housing census 2009 21 ), Demographic and Health Survey (Burkina Faso 2015 22 ); Cote d’Ivoire (National general population and housing census 2014, 23 Multiple Indicator Cluster Survey 2016 24 ) and Guinea (National general population and housing census 2014, 25 Multiple Indicator Cluster Survey 2018 26 ).
Data source
EmONC assessments were performed in all health facilities that provided deliveries. The evaluation used modified tools based on the Columbia University Averting Maternal Death and Disability (AMDD) Program Needs Assessment Toolkit to document the availability of infrastructure, equipment, drugs, supplies, and human resources for all EmONC services and service delivery, including PAC. 27 The questionnaire used for data collection was standardized and validated at a regional workshop in Abuja in 2016 and at each country level.
For population coverage by PAC services, we considered the data sources for the population used in each country, available on the respective EmONC databases and reports.18 -20 Data on subnational regions correspond to regional health divisions in force in each country at the time of data collection of the EmONC survey.
Study Population and Sample
The study population consisted of public and private health facilities that offer PAC in delivery services. We considered all health facilities included in each country’s EmONC needs evaluation database. EmONC needs assessment surveys are national cross-sectional hospital-based studies that use a representative sampling method. The most recent survey database was considered for each of the included countries. The sample size of health facilities varies from country to country, but is nationally representative.
In Burkina Faso, the EmONC survey included 422 health facilities selected from public and private health facilities at all levels of the health pyramid. The sample comprised 351 primary care facilities and 71 hospitals that were included exhaustively. Data were collected from 26 September to 24 October 2016.
A comprehensive survey of all public facilities with at least 2 qualified health workers who could provide care to women and new-borns was carried out in Côte d’Ivoire from November to December 2017. A total of 438 health facilities at all levels of care were included in the sample, of which 418 were actually visited.
In Guinea, the survey covered 229 of the 230 health facilities identified by the mapping carried out in 2015 to provide emergency obstetric and neonatal care, including 174 primary care facilities and 56 hospitals. The target health facilities were public and private and performed deliveries in 2016 and 2017. These include the Ignace Deen National Hospital maternity ward, regional and prefectural hospitals, health centers, improved health centers, and private and faith-based hospitals. Data collection was carried out from 25 to 27 October 2017 in Conakry and from 30 October to 20 November 2017 in the rest of the country.
Study variables
We used the indicators for availability and utilization proposed by Healy et al 17 and then adapted to PAC by Campbell et al. 14 We only retained indicators that could be assessed on the basis of the information related to PAC available in the EmONC data. Thus, the availability of PAC services is measured through 2 indicators: (1) the amount of PAC services available, defined as the number of facilities providing basic and comprehensive PAC, and (2) the distribution of PAC facilities that represents the number of facilities providing basic and comprehensive PAC in subnational areas. The use of PAC services is assessed through 3 indicators: (1) the proportion of women treated for abortion-related complications, (2) the proportion of women treated for serious abortion complications, and (3) the proportion of women who obtain postabortion contraception. The WHO defines serious abortion complications as those that can quickly become life-threatening if not treated immediately and include shock, severe vaginal bleeding, intraabdominal injury, and sepsis. 9 The definitions of each indicator and the measurement recommendations are given in Appendix A.
Two aggregate indicators were created to assess the capacity of the health system to provide basic or comprehensive PAC (Appendix B), based on the signal function approach already described in previous studies.10,11,14
The level of care of the facilities was categorized into 2 categories based on the structure of the health system in each country: the primary level of care that grouped all the facilities at the first level; in Burkina Faso, this concerns only the first sub-level of care. The level of care referral grouped all higher levels of care in the different countries. All facilities should be able to provide basic PAC, while comprehensive PAC that require greater ability to address the most severe complications are expected at the referral level of care.
Statistical analysis
To estimate the availability of PAC services in each country, we first calculated the number of facilities that could provide basic PAC among primary-level facilities and the proportion of referral facilities that could provide comprehensive PAC. The results were presented as proportions of facilities for each category of capability per country.
We then evaluated the distribution of PAC services for each health region in the 3 countries applying the WHO recommended number of basic and comprehensive service delivery points by population size (5 facilities per 500 000 population with at least 1 providing comprehensive care for EmONC). 28 We then represented the coverage of the PAC through geographical maps for each country; The health regions were classified into 4 groups with equal amplitude using QGIS software, version 3.4.6-Madeira.
Proportions were used to assess the utilization of PAC services by women at the facility level.
All statistical analyses were performed on Stata version 15.0.
Ethical considerations
This research used preanonymized quantitative datasets, for which ethical approval was given at the time of data collection. The protocol for this study was submitted and approved by the Burkina Faso Health Research Ethics Committee (N°2020-02-033). Permissions to access and analyze data were requested and obtained from each country’s maternal and child health department before starting the study.
Results
Characteristics of health facilities in the 3 countries
A total of 1063 health facilities were included in this analysis: 422 in Burkina Faso, 412 in Cote d’Ivoire, and 229 in Guinea). The characteristics of the facilities are described in Table 2. There were 902 facilities (84.8%) at the first level of care, where the facilities were expected to provide basic PAC services. Most of the facilities in this sample were public (95.3%), while 3.1% were private. Seven out of 10 facilities (70.7%) were located in rural areas. More than 3 quarters of the health facilities had potential basic EmONC capacity (78.5%).
Characteristics of the facilities.

Figure 1 shows the proportion of facilities by PAC capacity per level of care and per country. Slightly more than a third of the health facilities in the 3 countries (36.6%, n = 330) could provide basic postabortion care (36.6%, n = 330) at the first level of care, ranging from 27.0% in Guinea, 37.8% in Cote d’Ivoire to 42.8% in Burkina Faso. At the referral level of care, both the basic and comprehensive capacity of the PAC was evaluated. Approximately 82.0% (n = 132) of the hospitals could provide a comprehensive PAC, ranging from 75.0% in Burkina Faso, 65.6% in Guinea, to only 42.0% in Cote d’Ivoire. The capacity to provide basic PAC at the referral level ranged from 16.2% in Burkina Faso to 36% in Cote d’Ivoire.
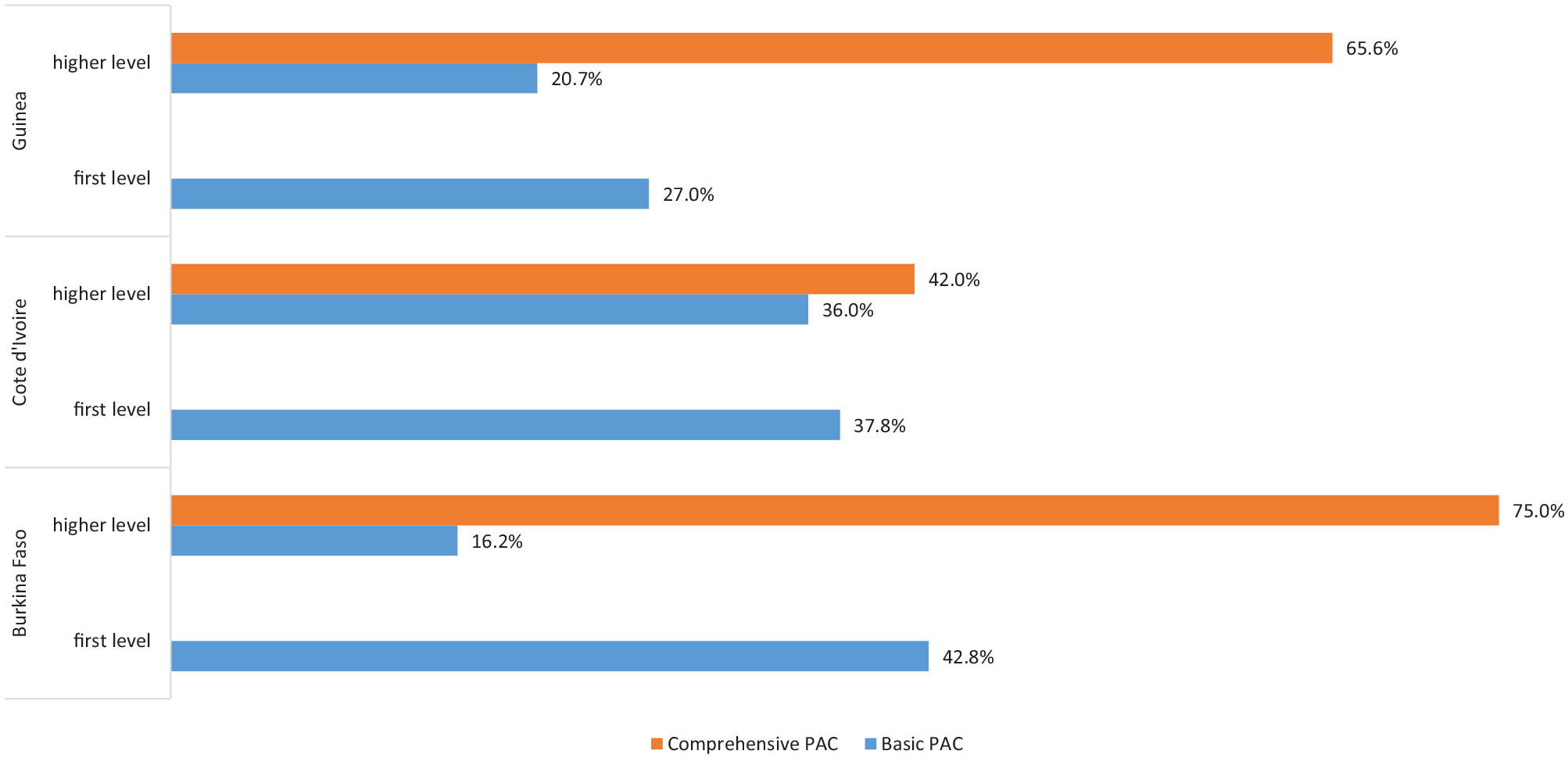
Proportion of facilities with basic and comprehensive capacity of PAC, per level of care and country (Burkina Faso n = 422, Cote d’Ivoire n = 412, Guinea n = 229) 2016 to 2017.
Figure 2 shows the geographical distribution of basic PAC services in each country. Ten regions (24.4%) of the 41 met the 3 countries’ recommended benchmark for basic PAC provision. In Burkina Faso, with 13 health regions, the distribution of basic PAC services between regions ranged from 61.5% to 187.5%. Three health regions (the Cascades, Central Plateau, and Sud-Ouest) of the 13 (23.1%) met the recommended levels. The number of health regions in Côte d’Ivoire was 20 in 2017. The distribution of basic PAC per region in the country ranged from 20.0% to 160.0%, with 6 regions (Agneby-Tiassa-Me, Hambol, Indenie Duablin, Kabadougou-Bafing-Folon, N’zi-Ifou, Worodougou-Bere) of 20 (30.0%) that met the recommended target. In the 8 health regions of Guinea, the distribution of basic PAC per region ranged from 9.1% to 129.4%; Only 1 region (Nzerekore) met the recommended level (12.5%).
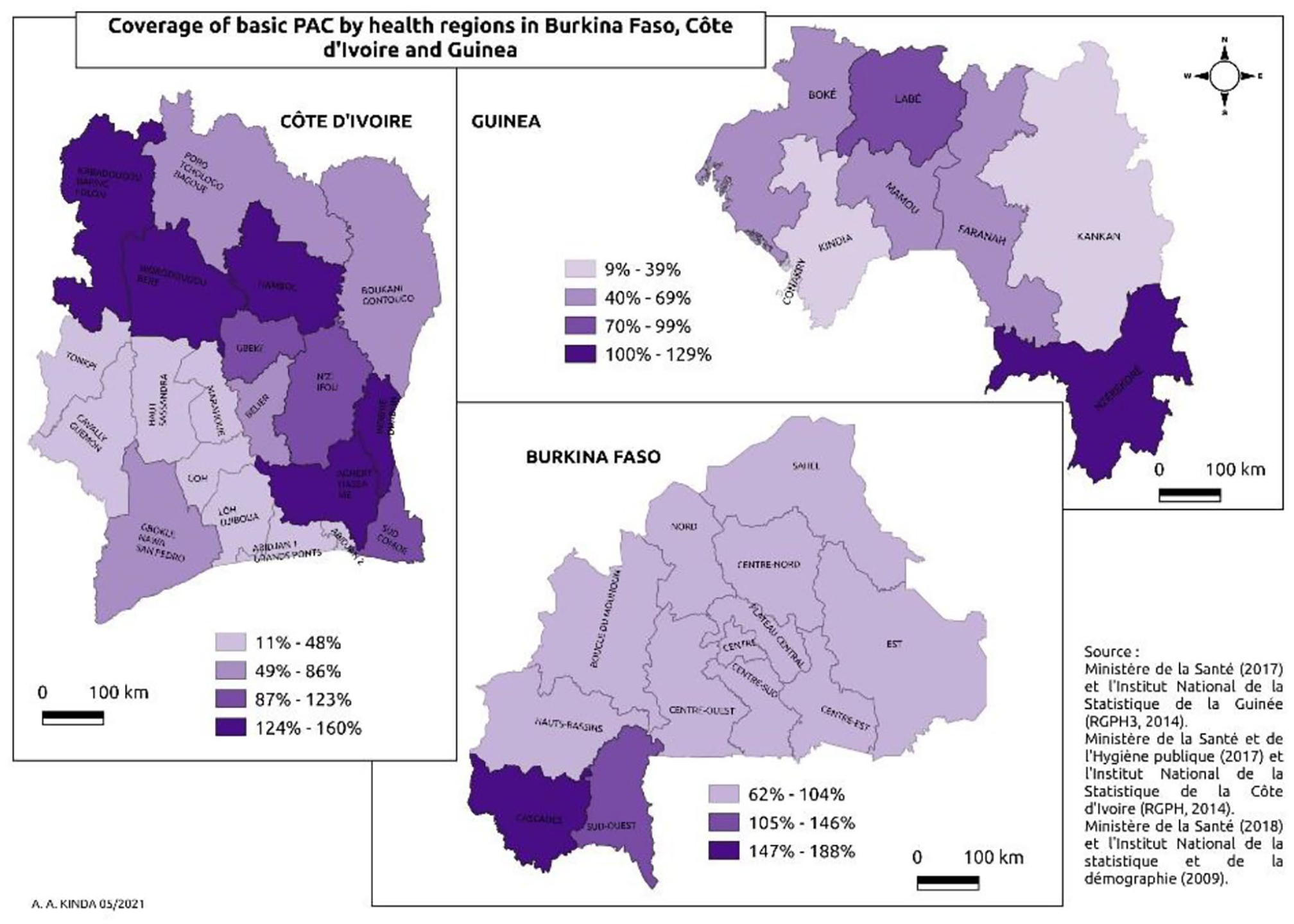
Distribution of basic PAC services in Burkina Faso, Cote d’Ivoire, and Guinea.
For the distribution of basic PAC services, many health regions with smaller population sizes generally had the highest percentages, regardless of the country and except for some health regions (Gôh, Lôh-Djiboua, Marahoue, and Tonkpi in Cote d’Ivoire and Nzerekore in Guinea) (Supplemental Table 1).
The distribution of comprehensive PAC services within countries is presented in Figure 3. In general, 78.0% of the regions met the recommended levels of population coverage by PAC services. There does not appear to be any particular pattern in the distribution of comprehensive coverage of PAC services by population size. In Burkina Faso, this distribution ranged from 50.0% to 200.0%; Only 1 region (Cascades), which had the lowest population, did not meet the benchmark requirements (7.7%). Performances of the comprehensive distribution of PAC services in Côte d’Ivoire start from 33.3% to 200.0% (Hambol, Indenie Duablin, Kabadougou-Bafing-Folon, Worodougou-Bere). Twelve regions (60%) met the recommended level, while 1 health region (Tonkpi) did not have any facility with this capacity. Some regions with low population sizes met the recommended levels (Belier, Gôh, Hambol, Indenie-Duablin, Kabadougou-Bafing-Folon, Nzi-Ifou, Comoe, Worodougou-Bere). In contrast, more populous health regions did not meet the targets (Abidjan 1 and 2, Poro-Tchologo, Gbokle-Nawa-San Pedro, and Tonkpi). All 8 health regions in Guinea met the recommended level of comprehensive PAC services, most of them far exceeding the target; the highest performance observed was 350.0% (Boké).

Distribution of comprehensive PAC services in Burkina Faso, Cote d’Ivoire, and Guinea.
In all countries, the health regions where the largest city, usually the capital of the country, is located did not meet the coverage target for basic services (Centre (80.8%) in Burkina Faso, Abidjan 1 (39.1%) and 2 (38.7%) in Cote d’Ivoire and Conakry (33.3%) in Guinea) and comprehensive PAC services in Cote d’Ivoire (Abidjan 1 (40.0%) and 2 (66.7%)).
The proportion of facilities that met the benchmark target varied within the health region of each country (Supplemental Table 1).
Utilization of PAC services
In total, 219 248 direct obstetric complications occurred in the 3 countries during the reporting period of the surveys accounted. A total of 35 417 (16.2%) abortion-related complications were reported for the same period.
The utilization of PAC services was estimated using 3 indicators (Table 3). The first indicator of the utilization of the PAC service refers to the proportion of women treated for abortion complications. Approximately 16.2% of the women received for an obstetric emergency had an abortion complication. The highest proportion was achieved in Cote d’Ivoire (26.0%).
Use of PAC services by women with abortion-related complications.

Abbreviation: -, information not available.
The proportion of women treated for serious abortion complications represented the second indicator of the utilization of evaluated PAC services. Of all abortion-related complications received in the facilities, 12.9% had a life-threatening complication. Most of them were found in referral level facilities (13.2%). Abortion complications represented 11.8% of obstetric emergencies at the primary level. Guinea had the highest percentage of severe abortion complications received in health facilities (34.5%).
The third indicator measured the proportion of women who received postabortion contraception services. In general, only 37.1% of women treated for an abortion complication obtained modern family planning after abortion. While in Burkina Faso, the proportion of women who received modern contraception after abortion was higher at the referral level (54.7%), in Cote d’Ivoire, this proportion was higher among those who benefitted from basic PAC (50.9%). This indicator could not be estimated from Guinea EmONC data.
Discussion
This study analyzed the availability and utilization of PAC services in Burkina Faso, Cote d’Ivoire, and Guinea, using EmONC surveys. The findings showed variability in the availability of PAC services at both the national and the subnational levels. Overall, the availability of basic PAC was low at the primary level of care in all 3 countries. Only Guinea met the target for availability for comprehensive PAC services in all regions. Abortion complications remain a significant cause of obstetric emergencies (16.2%); approximately 12.9% of these complications were very severe. Postabortion modern contraceptive uptake among women seeking PAC was also generally low (37.1%) in the 3 countries.
The findings of our study are consistent with previous reports reporting the availability of PAC services in SSA countries that generally reported the low availability of basic PAC. Therefore, in West Africa, in Senegal in 2015, the percentage of basic PAC available was only 53% at the primary level of care, 10 while Bell et al 13 in 2021 found that approximately 1 in 3 facilities in Nigeria and 36.9% in Côte d’Ivoire could provide basic PAC at the same level of care. The same findings were reported in other SSA countries (Kenya (15%) in 2010 and Tanzania (28%) in 2014-15 in East Africa 10 and Zimbabwe (21%) in 2016 11 ) and in other low- and middle-income countries. 29 These findings may be due to the fact that, in general, postabortion care, although a component of basic EmONC, is usually only offered at a referral level of care, despite the fact that primary care health centers are considered the entry point and the most accessible facilities in health systems, especially in rural areas.
Generally, comprehensive PAC services are provided at the referral level of care, usually located in urban areas and may also have more structural capacities in terms of equipment, supplies, and staffing. 9 However, the capability to provide comprehensive abortion appears higher in our results than previously reported. Therefore, only 10% of referral facilities in Zimbabwe 11 and 55% of various countries in SSA could provide comprehensive PAC. 10 However, our findings are consistent with studies on EmONC availability. 30 As there is no significant gap between the evaluation periods of the health systems, this variability may reflect the actual capacity of each country’s health system to provide PAC.
The findings also illustrated the unequal national distribution of each type of PAC services in each country, rapidly giving a broad view of inequities within and between countries by showing how widely or smaller health services are dispersed. The high availability of comprehensive PAC in most regions of the 3 countries could be explained by an underestimate of the need for PAC in the proposed benchmark.11,14 Other studies also raised some concerns about the relevance of the use of this benchmark. Among these, the relevance of considering information on the entire population rather than focusing on women of childbearing age and the lack of an explicit measure of accessibility that would truly reflect the physical distance or travel time between the service delivery point and the user were therefore questioned. 31 However, accessibility to services has multiple dimensions and good availability with adequate geographical coverage alone is not sufficient to guarantee improvement in health indicators. 32 In fact, the financial accessibility and acceptability of health services are important dimensions to consider, especially for a subject as sensitive as induced abortion. In fact, the strong stigma surrounding abortion means that even when services exist, people do not always use them when needed.12,33
Combining measures of availability and utilization of PAC services could allow us to better understand the causes of poor performance of a health system. The proportions of abortion-related complications among women seeking care found in this study suggest that unsafe abortion is a public health problem in the 3 countries that needs to be seriously addressed through relevant and effective interventions. Evidence has shown that postabortion family planning is a high-impact practice that results in greater adoption of family planning when provided proactively at the same time and location where a woman receives facility-based PAC. 8 However, the adoption of family planning according to our findings among women seeking care is still low, despite a very high capacity to provide contraceptive methods in the 3 countries. This is in line with the results of most studies in SSA.11,14,29,34,35
This study presents some limitations. Using data from EmONC surveys that are limited to health facilities that offer delivery services, we were confronted with some limits already described by studies that have used a similar approach10,11,14,17: hospitals that provide postabortion care do not offer delivery services. Furthermore, the information collected is generally related to general hospital services, but is not specific to the organization of PAC services and the degree of integration of services such as PAC family planning. Therefore, we approximated the ability to provide PAC signal functions based on delivery indicators. In addition, private facilities could have been underestimated in this analysis, due to the type of sampling in each country, though representative. Finally, another limitation of our study, which is also inherent in the type of methodology used, is the lack of information on the sociodemographic characteristics of women presenting abortion complications, which did not allow an analysis of the factors influencing the utilization of PAC services.
However, despite these limitations, this study allowed comparison of the availability and utilization of PAC services using recent and nationally representative data obtained through a comprehensive and standardized method for the evaluation of health facilities. This is important in these countries that have similar health system organization and abortion regulations, and where health system information on PAC services is scarce. Bell et al 13 in their study in 2021, which used an innovative approach that combined population data with hospital data, provided recent and up-to-date information on both the availability and the accessibility and equity of PAC services in Cote d’Ivoire. Our findings provide additional illustrated information on the adequate distribution of both basic and comprehensive PAC services throughout the country. Additionally, data on the use of services not only assess the need for PAC, but can also serve as a baseline for measuring progress in the provision of quality PAC services through the evolution of service utilization indicators in Cote d’Ivoire, while comparing this performance to countries in the subregion where unsafe abortion also remains one of the main causes of maternal mortality. The results obtained could serve for decision making on further improvements in public health programs and policies related to postabortion. Improving the availability of PAC services at the primary level would avoid delays and inequity in access to care, as evidence reported that poor rural women may have more abortion-related complications. 1 In addition to the availability of services, it is also necessary to ensure that the care provided is consistent with the quality of care recommendations, especially with regard to postabortion family planning services.
Conclusion
This study provides evidence on the availability and use of postabortion care services in 3 West African countries where access to abortion care is restricted. The results highlighted disparities in the availability of PAC between countries and within subregions in the same country, as well as missed opportunities such as improving the adoption of PAC family planning. There is a need to focus on access to postabortion care at the primary level and to ensure that women seeking care for an abortion complication receive evidence-based care according to recommended standards of care. Monitoring the trends in the progress of indicators for PAC use is important for the effectiveness of interventions.
Supplemental Material
sj-docx-1-his-10.1177_11786329221092625 – Supplemental material for Availability and Utilization of Postabortion Care Services in Burkina Faso, Côte d’Ivoire, and Guinea: A Secondary Analysis of Emergency Obstetric and Neonatal Care Needs Assessments (EmONC)
Supplemental material, sj-docx-1-his-10.1177_11786329221092625 for Availability and Utilization of Postabortion Care Services in Burkina Faso, Côte d’Ivoire, and Guinea: A Secondary Analysis of Emergency Obstetric and Neonatal Care Needs Assessments (EmONC) by Rachidatou Compaore, Adja Mariam Ouedraogo, Adama Baguiya, Denise Olga Kpebo, Sidikiba Sidibe and Seni Kouanda in Health Services Insights
Footnotes
Appendix
Signal functions for basic and comprehensive post abortion care.

| PAC functions expected for all facilities | |
|---|---|
| 1. Removal of retained products of conception 2. Administration of parenteral antibiotics 3. Administration of parenteral uterotonics 4. Administration of intravenous fluids 5. Provision of at least 1 modern, short acting contraceptive method |
|
| PAC functions expected at primary health care level facilities: Basic PAC capability | PAC functions expected at referral level facilities: Comprehensive PAC capability |
| 1. Communication means with referral facilities 2. Transportation means for referral 3. Availability of qualified staff for normal delivery, on duty or on call 24 h/7 d |
1. Capability for blood transfusion administration 2. Capability for cesarean section 3. Provision of at least 1 long-lasting family planning method 4. Availability of qualified staff for cesarean section, on duty or on call 24 h/7 d |
Acknowledgements
RC received funding from the HRP Alliance, part of the UNDP-UNFPA-UNICEF-WHO-World Bank Special Programme of Research, Development and Research Training in Human Reproduction (HRP), a cosponsored program executed by the World Health Organization (WHO), to complete her studies. This article represents the views of the named authors only and does not represent the views of the World Health Organization. RC thanks AAK and OT for their support in conducting this analysis.
Author Contributions
RC conceptualized and wrote the first draft of the manuscript. SK, AMO, and AB substantially contributed to the study methodology and data analysis and critically reviewed the first draft. AMO, AB, DOK, SS, and SK critically reviewed the subsequent drafts of the manuscript. All authors read and approved the final manuscript and agreed to the submission.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
