Abstract
Background:
Mammography use and its predictors among older women require further study.
Objectives:
Mammography use and its relationship to demographic characteristics, health care access, and breast cancer risk factors in women ages 60 to 85 in the United States were examined.
Design:
US Health and Retirement Study 2014 dataset was examined.
Methods:
A descriptive study using secondary data was analyzed for use of mammography screening and its predictors in women ages 60 to 85 in United States.
Results:
In total, 5177 (73.4%) of respondents reported mammography use. Mammography use was higher among older women who were married, nonsmokers, alcohol drinkers, engaged in vigorous exercise, and had dental visits.
Conclusion:
Women ages 60+ in the US HRS dataset revealed continued mammography screening into later years (73.4%), and mammography use was higher among older women who had healthy lifestyles and habits. Insights for health care providers and systems are to recommend mammography use for women age 60 to 85 years are provided. This US study can be used to inform future research and policy regarding breast cancer screening among older women.
Introduction
Background
The world’s population is aging, a process by which the age structure shifts toward older ages. 1 The number of older adults, defined as persons ages above 60, had exceeded one billion worldwide in 2020, and is projected to double by 2050, moving from 12% to 22% in proportion of the total population. 2
Breast cancer is the second most common cancer and the second most common cause of cancer death in the United States. 3 Early detection of breast cancer through mammography screening is accepted as the best preventive practice to decrease the need for extensive breast cancer treatment and improves the chances for survival, and leads to better prognosis, and recovery. 4 During the 25-year period from 1975 to 2000, 25% of cumulative breast cancer deaths have been averted through screening. 5 Researchers have found that mammography use for older women ⩾70 years comprise a small portion of the total screening examinations. However, older women represent a significant portion of all patients diagnosed with screen detected cancers with most tumors, and a majority of older women were in good to excellent health.6,7
Mammography guidelines and insurance coverage
US guidelines and methods for routine mammography screening and cost vary depending on the professional organization and as related to insurance coverage or provider recommendation. 7 Health insurance coverage and structure in the United States for mammography coverage is provided through a hybrid of public and private insurance.8,9 In the past 5 years, mammography guidelines have evolved to address middle and older age groups and risk levels more precisely. Mammography guidelines still vary by organization but generally recommend screening through age 74, with individualized decisions for older women based on health, life expectancy, and risk. The US Preventive Services Task Force advises biennial screening for women ages 40 to 74 and stopping at 75 due to insufficient evidence of benefit beyond that age. 3 Similarly, the American College of Physicians recommends stopping screening for average-risk women aged 75+ or those with a life expectancy of 10 years or less. 9 The American Cancer Society suggests annual mammograms for women 45 to 54, with the option of biennial screening starting at 55 if in good health. 10 Similarly, the American College of Radiology recommends individualized screening after age 55 based on life expectancy, health status, and willingness to pursue treatment. 11
The cost of a mammogram screening for patients can range from 0 to more than 300 USD 7 and should also consider cost benefits for screening older women. Annual mammography was not found to be cost-effective for older women. However, biennial mammography screening to age 80 years was cost-effective. 12 These researchers report that women considering screening beyond 75 years should weigh the potential harms of overdiagnosis versus the potential benefit of dying from breast cancer. For healthy older women with little or no comorbidity risks, extending biennial screening mammography to 80 years is associated with modest costs for the health benefits gained; however, extending beyond 80 was not cost-effective. Extending annual mammography beyond age 75 was associated with higher burdens of overdiagnosis compared with biennial mammography. 13
Mammography use and predictors
In the United States among women ages 50 to 74, 76.4% received a mammogram within the past 2 years nearing the Healthy People 2030 target of 77.1% of women being up to date in screening. However, health disparities persist with 68.3% versus 79.6% of women below 200% and above 200% of the federal poverty level, respectively, having had a mammogram. 14 Having comorbid diseases, 15 lower socioeconomic status,11 -19 lower education, 20 limited health care access,18,20 recent immigrant status,21,22 and having 3 or more children 17 have been found to be associated with lower mammography use. Regarding socioeconomic status, individual and neighborhood-level measures that include income and education level, employment status, food insecurity, and overcrowding have been found in numerous studies to influence breast cancer screening.18,19 Mammography use has been found to be positively associated with receipt of preventive services,15,20 higher self-rated health-related quality of life, 22 having diabetes, 20 being married,21,23,24 older age,15,24 and black race. 17 On the other hand, a study among Turkish women aged 40 to 69 found that those who rated their general health as “very good” were least likely to obtain regular mammography possibly reflecting more concerns about cancer. 20
Emerging literature covers factors related to mammography use among older women (age 60-85) and the extent that they are receiving mammography. Socioeconomic and health status has been found to be associated with mammography compliance among older women.25,26,27 Higher likelihood of mammography has been found to be associated with regular access to health care,26,27 excellent health,25,28 not smoking,28,29 and not having depression. 22 Frequent hospitalizations, 21 comorbidities, 21 and functional limitations or disability28 -30 were found to be barriers associated with lower mammography use among older women. Educational attainment, age, receipt of flu vaccination, and history of benign breast biopsy were also independently associated with being screened beyond age of 75 years. 31
The National Health Interview Surveys have examined mammography screening and factors associated with mammography use with life expectancy in years, and self-reported good to excellent health was found both to be strongly associated with mammography use in older women.7,31 Using Medicare and Breast Cancer Surveillance Consortium data, women ages 66 to 75 who had less than a high school education were found to be non-adherent to mammography. 15 An analysis of 2014 and 2016 HRS and 2013 Health Care and Nutrition Study datasets found that food insecurity was a barrier for screening, and the likelihood of receiving mammography was higher for women ages 50 to 74 with greater educational attainment and higher household income.6,26, Medicare data was used to examine mammography among women ages 64 to 74 in Texas and found rural and racial disparities in mammography use. 27
The HRS dataset has been used to examine mammography for women aged 50 years and older. Most of these studies examined a variety of prevention behaviors that include mammography and associated the behaviors with one predictor outcome, for example, cognitive impairment, multi-morbidity, life satisfaction, resilience. Two HRS studies examined cognitive impairment with “prevention behaviors” that include mammography and found that those age 50 and older who reported cognitive impairment were less likely to obtain mammography.32,33 In a different study that examined women who were diagnosed with Alzheimer’s disease and related dementia (ADRD), overall those with ADRD were more likely to receive a mammogram. 34 Using the HRS, women aged 50 and older with higher life satisfaction were more likely to received mammography screening. 35 Another HRS study found that high mastery was associated with a greater likelihood of receiving a mammogram. 36 Multi-morbidity was found to be negatively associated with mammography among women aged 52 years and older. 37
Mammography discontinuation
Research has also been conducted on the extent of mammography discontinuation among older women. However, there is little evidence available to make a recommendation for or against continuing breast screening beyond age 75 years. 38 Many older women who meet the criteria for discontinuing mammography continue to receive it.39,40 Decisions to stop mammography were not found to be associated with older age or life expectancy.39,41 Studies have found an association between the extent of cancer worry or perceived risk and continued mammography among older women39,42
Decisions to discontinue screening only based on age are not recommended. 1 Clinicians should consider life expectancy estimates to inform cancer screening of older adults so that clinicians can speak with their older patients including recommendations for mammography. 41 Tailored communication strategies for clinicians should be used for older patients so that they can make better-informed screening decisions. 1 A sample of women age 65 and older recommended that their physicians provide them with specific information from their health history on why screening should discontinue, but not incorporate life expectancy in that discussion, and leave the screening decision up to the older patient. 43 Ultimately both clinicians and older women experience tensions in using life expectancy to recommend or continue mammography, respectively. For example, clinicians report operational barriers, uncertainly, and hesitation around the use of life expectancy. 41
Purpose of study
The purpose of this study is to identify demographic, health care utilization, and health-promoting lifestyle behaviors as predictors of mammography use among older women ages 60 to 85 using the US Health and Retirement Study 2014 dataset. To our knowledge, examining multilevel predictors of mammography instead of one area, that is, cognitive impairment, multi-morbidity, resiliency, has not been conducted using the HRS. International studies have examined multilevel predicators of mammography for older women using their country’s harmonized datasets from the Global Gateway to Aging project of which the HRS participates. For example, a recent Longitudinal Aging Study of India (LASI) examined demographic, behavioral, and clinical factors related to mammography of older women. 44 This study carries out similar methodology to the recent LASI study using respective US HRS. Findings will enhance the understanding and knowledge of mammography use among older women in the United States as well as inform future research and policy regarding breast cancer screening among older women.
Methods
This is a descriptive study of a secondary data examining mammography use and its predictors among older women using the HRS 2014 data. This study was approved by the University of Hawaii Human Studies Program #2021-00289.
Study populations and setting
A nationally representative dataset was used for the analyses: HRS. HRS is a longitudinal panel study of a representative population sample of adults ages 50 and above conducted by the Survey Research Center at the University of Michigan. Since the HRS is a publicly available dataset used as the data source for this study, we did not consent participants as this was done through the HRS itself at the University of Michigan. The HRS is a study that surveys a representative sample of more than 20 000 Americans since 1992. Because this study analyzed secondary data already collected for HRS, our study also did not involve validation and administration of the HRS questionnaire. Questionnaires may be found on the Global Gateway to Aging website.
The initial HRS cohort, recruited in 1992, consisted of persons born 1931-1941 between ages of 51 and 61 as well their spouses of any age. The HRS has since recruited new cohorts of ages 51 to 56 and their spouses. Currently, the HRS replenishes the longitudinal cohort every 6 years to maintain the study sample at approximately 20 000 participants interviewed every 2 years. Between 1992 and 2016, 43 478 individuals have been interviewed. A strength of the HRS is the detailed economic and health information to enhance our understanding of aging in the United States. The HRS is supported by the National Institute on Aging and the Social Security Administration.
Measurements
Selection of variables
Variables were identified from the initial HRS dataset based on 2 criteria: availability in the HRS dataset and those found to predict mammography use in the literature. This resulted in a list of 15 variables for analysis. The final step before statistical analysis was re-coding the variables. All but 2 (age and self-reported health) in the final list of variables underwent re-coding. Variables that were selected for the analysis from the domains were potential predictors of mammography screening for women 60+.
Description of predictor and outcome variables
Predictor (independent) variables initially included sociodemographic, health status, breast cancer risk factors, and health care access and utilization. Sociodemographic—age, marital status, employment, and education were measured by age group = 5 categories (60-64, 65-69, 70-74, 75-79, and 80-84), married = dichotomous (having a spouse/not having a spouse), work for pay = dichotomous (yes/no), degree = 4 categories (less than high school, high school, AA/junior college, BA/university+). Health status—incorporated self-reported health, behavior risk factors, health conditions. Self-reported health—reported current health was measured by a 5-point scale. Behavioral risk factors such as smoking status, drinking alcoholic beverages, and exercise were analyzed with categories and subcategories such as smoking now: dichotomous (yes/no) questions and values—smoking: no and yes; ever drunk: dichotomous (no, yes), vigorous exercise: 3 categories (at least 1 time/week, <1 time/week, rarely/never). Health conditions—breast cancer risk factors included assessment of diseases/disorders such as ever had condition—dichotomous responses (yes/no); emotional, nervous, or psychiatric problems, arthritis, cancer, diabetes. Health care access and utilization incorporated—doctor and dental visits were analyzed by doctor visit in 2 years: dichotomous (no, yes); dental visit in past 2 years: dichotomous (no, yes). Outcome: 1 survey question on mammography.
Data analysis
The frequencies of predictor variables were calculated using unweighted analyses. All other analyses employed methods for complex survey data analysis using the complex sampling variables provided by the HRS studies. The proportions of women obtaining a mammography were estimated with 95% confidence interval (CI).
Regression models with obtaining a mammography in the past 2 years as a binary outcome used negative binomial regression. Negative binomial regression like Poisson regression has an advantage over logistic regression in that relative risks (RRs) are accurately estimated when the outcome is not rare, as is the case with mammography. 45 Odds ratios from logistic regression can substantially overestimate RRs. 46
Differences in mammography screening by some participant characteristics could result from confounding by other characteristics (ie, differences in screening by levels of self-reported health might be confounded by age). Multivariable and Poisson regression models should help remove such confounding.
The possible predictors of mammography were analyzed using backward selection. We followed the approach described by the book by Heeringa et al titled Applied Survey Data Analysis. The book is an authoritative text on statistical analysis of complex survey data. The authors describe the history of the selection approach, details for implementation, and a worked example with explanations. 47 Variables for selection are chosen based on theory and initial univariable analysis. From step-to-step, the least significant variable was dropped until all remaining variables were statistically significant (P < .05). In other words, all the predictor variables were examined and only those independently significant were retained in the final model. The manuscript reports the results for variables retained in the final model after the backward selection procedure. The final model used reference coding to make the results easily interpretable. As an example, “being unmarried” was chosen as the reference category for marital status.
Results
Demographic characteristics
There was a declining trend of respondents among age groups at the oldest ages with only 22% of those interviewed being above the age 75 years (Table 1). Fifty-eight percent were married, 11% smoked cigarettes, and 38% consumed alcoholic beverages. Forty-two percent of the women engaged in vigorous exercise less than once a week to at least once a week. Seventy-seven percent had a dental visit within 2 years. Seventy-six percent reported good, very good, or excellent health (see Table 1).
Numbers and percentages of women from the United States Health and Retirement Study and percent obtaining mammography by demographic and behavioral characteristics (n = 7082).

Mammography use
Overall reported mammography use was 73.4% (N = 5177) in the US HRS. Highest percentage of mammography use was women who never engaged in vigorous exercise (82.2%), had a dental visit in the last 2 years (81.4%), consumed alcohol (80.6%), self-reported very good health (81.2%), and self-reported excellent health (79.3%) (see Table 1).
Predictors of mammography
The unweighted frequencies and weighted percentages for variables excluded by the backward selection procedure are as follows: diabetes (2005, 28.4%), arthritis (4784, 67.6%), cancer (1100, 25.6%), psychological problems (79, 1.1%), doctor visits previous 2 years (4672, 66.2%), working (4686, 33.7%), highest degree (none (1230, 17.4%) and high school (4226, 60.0%), 926. 13/1%), 700, (9.9%).
All comparisons in the multivariable models were statistically significant at P < .05 except for self-reported health and vigorous exercise less than once per week (Table 2). Those in 65- to 85-year age group categories had 8% to 13% higher screening rates compared with women ages 60 to 64 (P = .001-.009). Married women obtained mammograms 5% more often than unmarried women (P = .032). Nonsmokers were 12% more likely to obtain a mammogram than smokers (P = .002). Women who drank alcoholic beverages were 5% more likely to be screened than women who did not (P = .029). Women who engaged in vigorous exercise at least once a week obtained mammography screening 7% (P = .005) more than women who exercised less than once per week, and women who engaged in vigorous exercise less than once per week obtained mammography 5% more often compared with women who never exercised, although this is not statistically significant (P = .056). Women who saw a dentist in the past 2 years were 33% more likely to obtain mammography screening than women who did not, and this was the strongest predictor of mammography screening (P < .000).
Relative proportions of women from the US Health and Retirement Study who received a mammography in the past 2 years by demographic and behavioral characteristics (n = 5177).
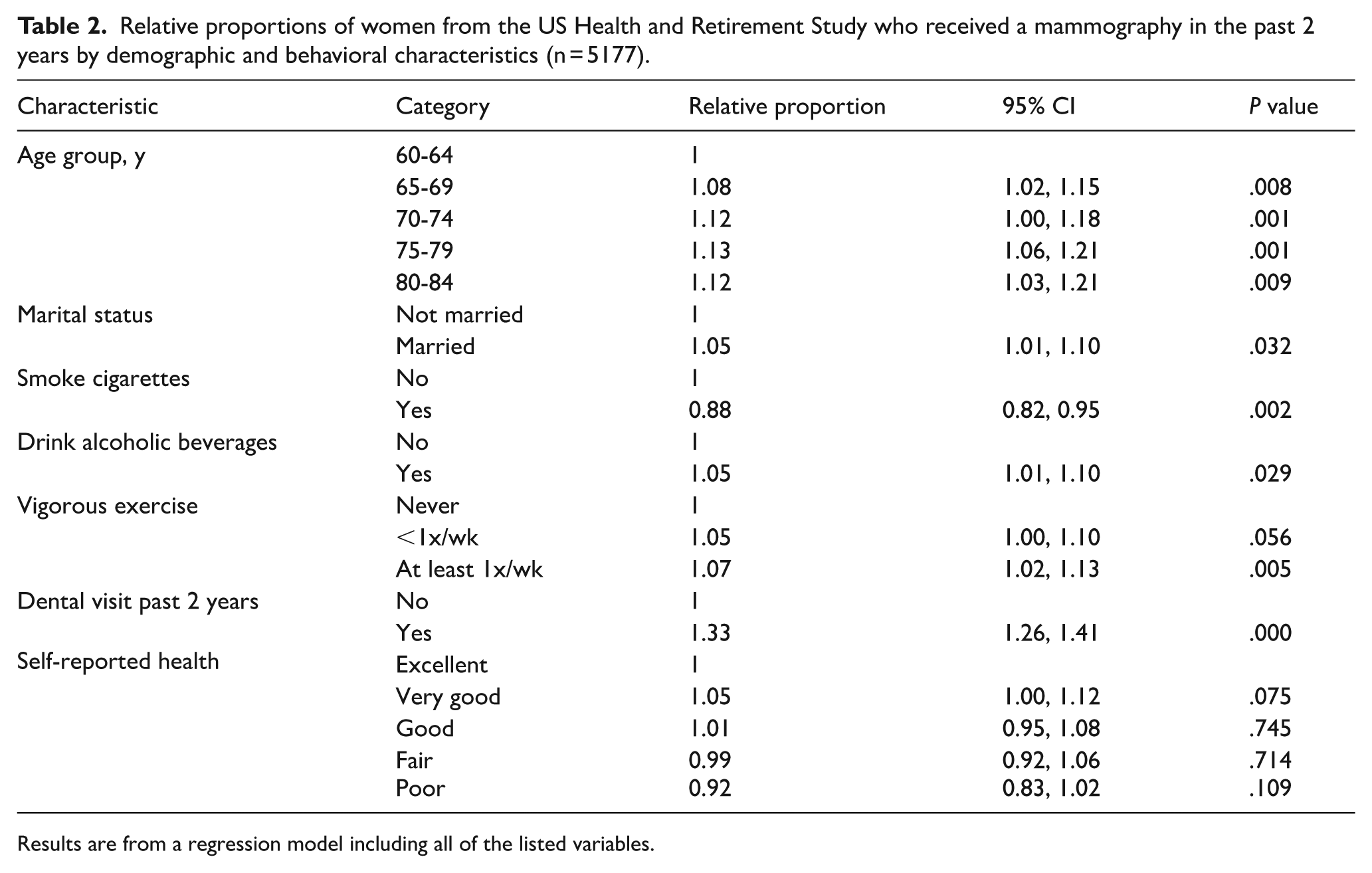
Results are from a regression model including all of the listed variables.
Discussion
Mammography use increased with age among those 69 to 79 years in the US HRS sample. Increased mammography use with age may be due in part to diagnostic reasons. Guidelines recommend that women continue mammography screening until at least 74 years of age. More than 50% of new invasive breast cancer in the United States is diagnosed in women ages 65 years and older. 28 The population of older women will increase due to increasing life expectancy as well as the rise of absolute number of breast cancer cases in older women. 48 Previous studies have found that older women who perceived cancer risk and do not take life expectancy in consideration continued mammography even if they no longer fit the guidelines.39,42
Evidenced-based guidelines for clinicians and their older patients are sparse particularly for older women and thus hard to quantify screening effectiveness and cost. It is difficult to accurately assess screening risks and benefits, and may have a greater risk of overdiagnosis. 1 Considerations for clinicians to recommend continuation or discontinuation of screening for breast cancer in older women include life expectancy, health conditions, comorbidities, and quality of life. Older women are underrepresented in cancer trials resulting in limited evidence to guide screening practice, that is, decisions to continue or discontinue, in this subpopulation. In addition, a clinician’s recommendation for screening may be a strong predictor of screening independent of life expectancy. 31
US women ages 60+ who reported engaging in health promotion behaviors were associated with mammography use. They were married, nonsmokers, drank alcoholic beverages, had higher engagement of exercise, and had regular dental visits. These findings add to the growing literature on lifestyle prevention among older women associated with mammography use. Factors found to predict mammography use among older women in this study align with the healthy behaviors associated with willingness to receive disease prevention service and may serve as a proxy for woman’s predisposition for additional preventive screenings which may be a path for preventing mortality due to other causes. 49 The results of this study point to areas for further investigation in this area.
Regular dental visits predicted mammography use. This aligns with studies that have found that regular dental visits are a health-promoting behavior also associated with other health-promoting behavior. 50 This finding adds to the body of knowledge of types of preventive health care services contributes to health promotion behaviors, especially among older women.
Recommendations
Research recommendations include examining other variables identified in the emerging literature on factors associated with mammography use for older women, and these variables warrant further study. Functional limitations,28,30 comorbidities, 11 food insecurity, 22 and lower education 15 have been found as barriers in mammography screening among older women. Self-reported health was not predictive of mammography use among older women in the HRS survey which was not consistent with Demb et al. 28 More studies should further validate existing findings many of which focus on one topical area as related to mammography such as the HRS studies and begin to elucidate a conceptual model from emerging findings of the multilevel factors that predict screening. Lifestyle behavior factors such as smoking, drinking alcoholic beverages, and exercise were categorized as dichotomous variables, but future studies should refine the subcategories so the results are contextually defined. Finally, future clinical breast cancer screening trials need to include older women ⩾75 years and older.7,42
Prevention practice approaches to address mammography use among older women are recommended. Although the dataset used in this study did not include having a primary care provider, access to and use of primary care providers should also be examined in future studies. Regular dental visits predicted mammography use among older women in this study, which may address use of primary care and its association with screening.
In the United States, 75% of nurse practitioners (NPs) are active in the primary care setting, and the Affordable Care Act has placed additional importance on primary care in the United States. Limited access to primary care, along with women subjectively only seeking diagnostic mammography because of low copay, negatively impacts the use of preventive and routine mammography. Clinician recommendations are an important influence in the patients’ decisions to stop mammography screening. Future intervention studies may include understanding how clinicians can better inform older women that stopping screening may be an option and to how to address concerns of older women are needed. 42 Indeed, individuals who frequently interact with the health care system and providers would more than likely adhere to mammography screening. 20
For older women, education to either consider continuing or discontinuing mammography has been ongoing. Results from this study examining multilevel factors associated with mammography use of women ages 60 to 85 in United States uncovered the complex intersectionality of demographic, health care access, and health behavior variables. Thus, system changes in primary care delivery, such as providing communication training for providers about mammography for older women, can enhance ongoing education efforts. These changes can help encourage older women to get screened for breast cancer, while also prompting others to consider whether they should continue screening as they age. The numbers of primary care providers that include NPs and primary care (family medicine) physicians should also be increased to broaden the provision of tailored prevention services including mammography. Barry found that increasing the supply of Ob-Gyns increases odds of both mammography recommendation receipt and mammography utilization. 51 These findings suggest a need for engagement between patient, provider, and organizational stakeholders to further apply evidence-based practice strategies to address mammography use in older women in the United States. 41
Health care system innovations can encourage individual mammography uptake among older women given the complex sociocultural and demographic factors found to date related to mammography and its benefits based on age and life expectancy. Because changing individual behavior to obtain mammography is complex, policy incentives can also foster mammography uptake. For example, in the United States, encouraging providers to deliver or refer mammography according to guidelines and patients’ needs is critical as quality indicators to meet a target of mammography services.
Limitations
Based on the emerging literature and the study findings, mammography screening use among older women is complex and requires further research. A variety of variables were not able to be examined as they were not available in the dataset or did not end up in the multivariate model because only those independently significant were retained in the final model. The dataset examined was for 2014 only, and mammography trends among older women may have changed with the growing attention on considering continue mammography or not.
Conclusion
The older adult population in the United States continues to grow with women living well into their 80s and beyond. This study used the US HRS to examine mammography use and multilevel predictors of women ages 60 and older. Results from this study examining factors associated with mammography use among older women use in United States uncovered the complex intersectionality of demographic, health care access, and health behavior variables.
A research focus on the patterns of mammography use among older women including its predictors and issues on the extent this preventive behavior should continue. System changes in primary care delivery can enhance education efforts to get women in the United States to get screened for breast cancer. Continued patient education to encourage mammography use according to guidelines and incentivizing and training primary care providers to tailor their screening guidelines are recommended for healthy aging of women 60 years and older.
Footnotes
Acknowledgements
None
Ethical considerations
This study was approved by the University of Hawaii Human Studies Program #2021-00289.
Consent for publication
Not applicable
Author contributions
Angela Sy: Conceptualization, Investigation, Methodology, Project administration, Supervision, Writing—original draft, Writing—review & editing.
Merle Kataoka-Yahiro: Conceptualization, Funding acquisition, Investigation, Resources, Supervision, Writing—review & editing.
James Davis: Data curation, Formal analysis, Funding acquisition, Resources, Software, Writing—original draft.
Sarah Pirani: Investigation, Project administration, Writing—original draft, Writing—review & editing.
Yumiko Kinoshita: Funding acquisition, Investigation, Resources, Writing—review & editing.
Nahoko Harada: Investigation, Writing—original draft, Writing—review & editing.
Maki Kanaoka: Writing—review & editing.
Mami Miyazono: Writing—review & editing
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by grants KAKENHI 19K22764 and the University of Hawaii at Manoa School of Nursing and Dental Hygiene Research Seed Funds for Statistical support. In addition, the study was partially supported by the National Institutes of Health (NIH) U54GM138062 National Institute of General Medical Sciences and U54MD007601, National Institutes of Minority Health and Health Disparities. The content is solely the responsibility of the authors and does not necessarily represent the official views of NIH.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
