Abstract
Background:
A growing number of recent literatures have attempted to document the factors related to drug use in different contexts, but limited studies analyzed the factors related to patient’s severity level.
Objective:
We aimed to examine the correlates of behavioral, environmental, socioeconomic, geographic factors, and severe drug addiction.
Methods:
We used a sample of 6790 people who use drugs (PWUD) from rehabilitation centers during 2019 to 2020 in Indonesia. Data were obtained from Drugs Rehabilitation Information System (SIRENA) by the Indonesian National Narcotics Agency (BNN) during 2019 to 2020. SIRENA used the adapted version of WHO’s Addiction Severity Index (ASI), which assesses patient’s addiction severity level and relevant factors. A composite of the ASI factors is classified as “poor” or “serious” if its score is 4 or higher. The data was analyzed using logistic regression model to estimate correlations of severe drug addiction.
Results:
We found a high prevalence (65.08%) of our sample reported having severe drug addiction, which needed intervention and support. Poor psychiatric condition (OR = 4.02, CI: 2.97-5.44), serious work-related issue (OR = 2.10, 1.75-2.51), poor medical condition (OR = 2.01, 1.32-3.06), and serious family and social problems (OR = 2.56, 2.15-3.05) were significantly associated with severe drug addiction. Male users had higher odds of severe drug addiction (OR = 1.81, 1.55-2.20), compared to female counterparts. Patients in urban areas had higher odds of severe drug addiction (OR = 1.19, 1.1-1.3) than those in rural. Those in less developed regions (eg, Sumatera, Kalimantan, and Sulawesi) had higher odds of severe drug addiction (OR = 2.33, 1.9-2.9), compared to those in the most developed region (eg, Java and Bali).
Conclusion:
This evidence can help policymakers in refining the harm reduction policies in Indonesia and other countries with similar settings.
Introduction
Drug use is a growing public health problem in low-income and middle-income countries (LMICs). The United Nations Office on Drugs and Crime (UNODC) estimated that in 2030, the population at most risk of drug use will increase by 43% in LMICs. 1 Drug use was responsible for 585 000 premature deaths in LMICs, of which 167 000 deaths were due to overdoses with 59% are below 50 years old. 2 Moreover, 31.8 million (1.3%) of Disability-Adjusted Life Years (DALYs) were attributed to drug use in 2016, 3 which threatened countries’ productivity and resulted in economic burden (eg, crime cost, health cost, and productivity cost) in LMICs. 4
Indonesia is one of the LMICs currently battling with the increasing issue of drug use. The country has witnessed an increase in the drug use rate, from 1.80% in 2018 to 2.40% in 2019. 5 As Indonesia is currently experiencing increasing number of productive population, efforts toward tackling public health problems including drug use can ensure reaping the demographic dividend. 6 The country has implemented various programs to prevent and reduce drug use, which are considered as the strictest drug use laws in Southeast Asia including the “shoot-on-sight” policy, imprisonment, and rehabilitation programs. 7 While the efficacy of the programs might be determined by factors related to the drug addiction,8,9 there is very limited evidence related to the this issue in Indonesia. Hence, evidence to better understand such factors is crucial to shape a more well-targeted anti-drug policies in the country.
Previous studies have provided some evidence on the factors related to drug use and addiction in different contexts. Those studies concluded that different psychosocial stressors and social environmental factors are associated with drug use behavior.10 -15 Furthermore, populations living in certain places like urban or highly-populated areas possess higher risks of drug use as they have easier access to public entertainment places, drugstores, and transportation facilities. 16 However, evidence on factors associated with the patient’s severity level is limited. As one of the main goals of substance use treatment, understanding factors related to addiction severity level could help refine harm reduction policies and improve treatment in rehabilitation centers across the country and other LMICs with similar settings.
Understanding the factors driving an addiction’s severity level will help to identify the different harm reduction programs needed by individuals as varied by the contributing factors. In terms of harm reduction policies, different substance type requires different treatment. 17 In addition, many factors such as gender-stigmatization, lack of family’s and friends’ supports, as well as psychosocial to logistical barriers have prevented individuals in accessing harm reduction programs.18,19 Thus, our study aims to examine the associations between a range of behavioral, environmental, socioeconomic, and geographic factors and severe drug addiction in Indonesia. Given the country has the strictest drug use laws in Southeast Asia, our findings will provide insights into preventive actions for relevant stakeholders in a larger global context.
Methods
Data and sample
This is a cross-sectional study to examine socioeconomic, geographic, and behavioral correlates of severe drug addiction in Indonesia. We used facility-level data from Drugs Rehabilitation Information System (Sistem Informasi Rehabilitasi Narkoba [SIRENA]) owned by the National Narcotics Agency (Badan Narkotika Nasional [BNN]) from 2019 to early 2020 (just before the COVID-19 pandemic began in the country). The data provide assessment of 6790 patients in rehabilitation centers under BNN throughout the country. The subject in the data is the patients being admitted to the rehabilitation center owned by BNN. All incoming patients need to undergo a medical checkup. Admitted patients are limited to those with non-severe physical and mental illness based on the result of medical checkup. Patients who have severe physical or mental illness are considered ineligible to be included in the rehabilitation treatment sessions and therefore are excluded from the addiction severity assessment.
The assessment form was adapted from the Addiction Severity Index (ASI) by the World Health Organization, which assesses PWUD substance addiction severity level and relevant factors. The BNN used the original ASI version from the fifth edition of ASI by McLellan et al 20 which is directly translated into Bahasa Indonesia. BNN recruits assessor/counselors to conduct in-depth interviews to assess all incoming patients using the ASI form prior to their admission to the center. All assessor/counselors have received trainings prior to conducting the assessment to ensure quality data. The assessment score also helps to determine the type of rehabilitative services received. There are 2 services offered, for example, outpatient and inpatient services. In both types of services, patients will receive counseling sessions, symptomatic treatment, and basic health checkups. Specifically for inpatient services, patients will receive therapeutic community facilities, and family support groups. In addition, vocational training is available for inpatient post-rehabilitation.
In addition to general information data, the assessment collected several information to measure the severity of addiction including severity of substance use, psychiatric condition, work-related issue, medical condition, and family/social problems. For each item, a patient gave a score from 0 to 9: score 0-1 means no considerable problem and no intervention needed; score 2-3 means there is a bit of problem but no intervention/support needed; score 4-5 means there is a moderate problem and some intervention/support needed; score 6-7 means there is a serious problem and intervention/support needed; score 8-9 means there is a serious problem and intervention/support really needed. The score assessment will be given based on the assessor observation on the patient’s physical and psychological conditions in times of rehabilitation. For our analysis, we followed the BNN ASI definition: severe drug addiction and poor/serious issues as having an assessment score 4 or higher (moderate problem and some intervention/support needed). Moreover, we included age, sex, marital status, and educational levels, urban location, and region (Sumatera, Java, Kalimantan, Sulawesi, and the Eastern region [including Nusa Tenggara, Maluku, and Papua]) as control variables.
Empirical strategy
In terms of data analysis, we employed a logistic regression to estimate the correlates of severe drug addiction using the equation below.
Results
At the beginning of the discussion, we will provide a concise overview of our study’s main findings, including sample characteristics, behavioral and environmental assessments, and the outcome variable in Table 1. In terms of sample characteristics (panel a), the majority of the sample (67%) were not married and were mostly male (89.2%). A larger percentage of our participants attended primary and secondary schools, 44.8% and 46.7%, respectively. Then, most of our participants (65.7%) lived in urban areas. By region, Sumatra and Java, we had a higher percentage of our participants, 37.2% and 25.9%, respectively. Regarding behavioral and environmental assessment (panel b), a higher percentage of our participants, 16.0% and 18.4%, reported serious work-related and family and social problems, respectively. In terms of the outcome variable (panel c), 65.1% of our sample reported having a severe drug addiction, which needed intervention and support. For more detailed information, please refer to Table 1.
Sample characteristics.
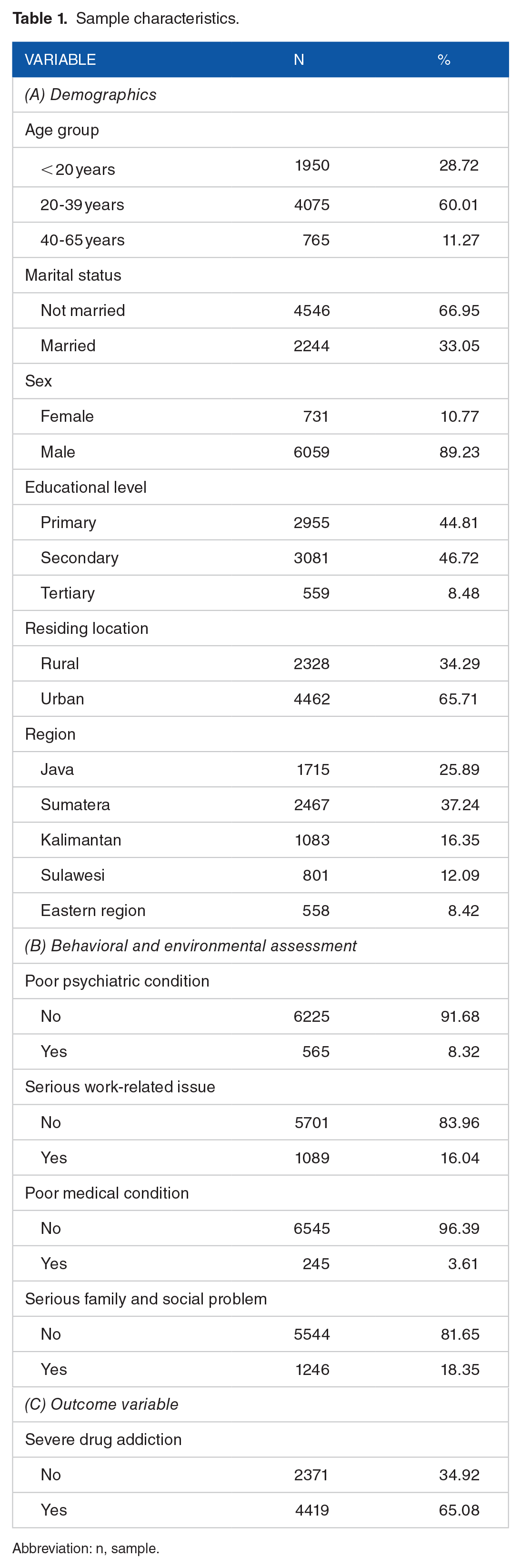
Abbreviation: n, sample.
Regarding the first regression result, the correlates of severe drug addiction for all and by type of substance are shown in Table 2. We found that poor psychiatric condition, serious work-related issue, poor medical condition, and serious family and social problems are significantly associated with severe drug addiction. Among the 4 factors, we found that poor psychiatric condition has the strongest association—patients with poor psychiatric conditions were 4 times more likely to have severe drug addiction to any type of substance (OR = 4.0, 95% CI:3.0-5.4). The other factors such as having serious work-related issue, poor medical condition, and serious family and social problems were 2.1 (95% CI: 1.8-2.5), 2.0 (CI: 1.3-3.1), and 2.5 (CI: 2.2-3.0) time higher odds of severe drug addiction, respectively. In terms of sociodemographic characteristics, we found that age, sex, location, and region are significantly associated with severe drug addiction. Older age group was associated with higher odds of severe drug addiction with significant odds on those aged 20 to 39 years (OR = 1.3, CI: 1.2-1.6) compared to aged 20 years or under. Male patients were 1.8 (CI: 1.5-2.2) times more likely to have severe drug addiction than female patients. Patients in urban areas were 1.2 (CI: 1.1-1.3) times more likely to have severe drug addiction than those in rural areas. By region, those in Sumatera, Kalimantan, and Sulawesi were 1.7 (CI: 1.5-2.0), 1.9 (CI: 1.6-2.3), and 2.3 (CI: 1.9-2.9) times more likely to have severe drug addiction, compared to those in the Java region
Correlates of severe drug addiction for all and by substance type in Indonesia 2019-2020.

Abbreviations: N, sample; OR, odds ratio; CI, confidence interval; Ref, reference group.
P < .05. **P < .01.
By type of substance, the majority of our sample used stimulant (63.3% of total sample in this analysis). The rest of sample used depressant (22.9%) and hallucinogen (13.8%). In terms of the associations, the patterning is similar for stimulant and hallucinogen, which shows the strongest associations between severe drug addiction and poor psychiatric condition (OR = 4.8 [CI: 3.1-7.5] for stimulant and OR = 5.5 [CI: 2.6-11.6] for hallucinogen). For depressant, the strongest associations were between serious family and social problems and severe drug addiction. In terms of sociodemographic characteristics, the patterning is relatively similar with the analysis using all substances, although some associations were not statistically significant. However, it is worth noting that the associations by urban/rural were flipped. Patients in urban areas were more likely to have severe addiction to stimulant (OR = 1.6, CI: 1.3-1.8) while, in contrast, those in rural areas were more likely to have severe addition to depressant (OR = 0.7, CI: 0.5-0.9).
In the subsequent regression results, the correlates of severe drug addiction by urban/rural and sex are shown in Table 3. By urban/rural, the associations between the 4 behavioral and environmental assessments and severe drug addiction were consistently stronger in patients living in rural areas, compared to those in urban areas. For instance, the associations between poor psychiatric condition and severe drug addiction were OR = 4.8 (CI: 2.8-8.2) and OR = 3.0 (CI: 2.1-4.4) in rural and urban, respectively. Similarly, the associations between serious work-related issue and severe drug addiction were OR = 3.1 (CI: 2.3-4.4) and OR = 1.8 (CI: 1.4-2.3) in rural and urban, respectively. By sex, the associations between the 4 behavioral and environmental assessments and severe drug addiction were relatively stronger in male than female patients, except for serious work-related issue. For instance, the associations between poor psychiatric condition and severe drug addiction were OR = 4.7 (CI: 3.3-6.6) and OR = 2.3 (CI: 1.1-4.9) among males and females, respectively. In contrast, the associations between serious work-related issue and severe drug addiction were OR = 2.1 (CI: 1.7-2.5) and OR = 2.7 (CI: 1.7-4.3) among males and females, respectively.
Correlates of severe drug addiction by location and sex in Indonesia 2019-2020.
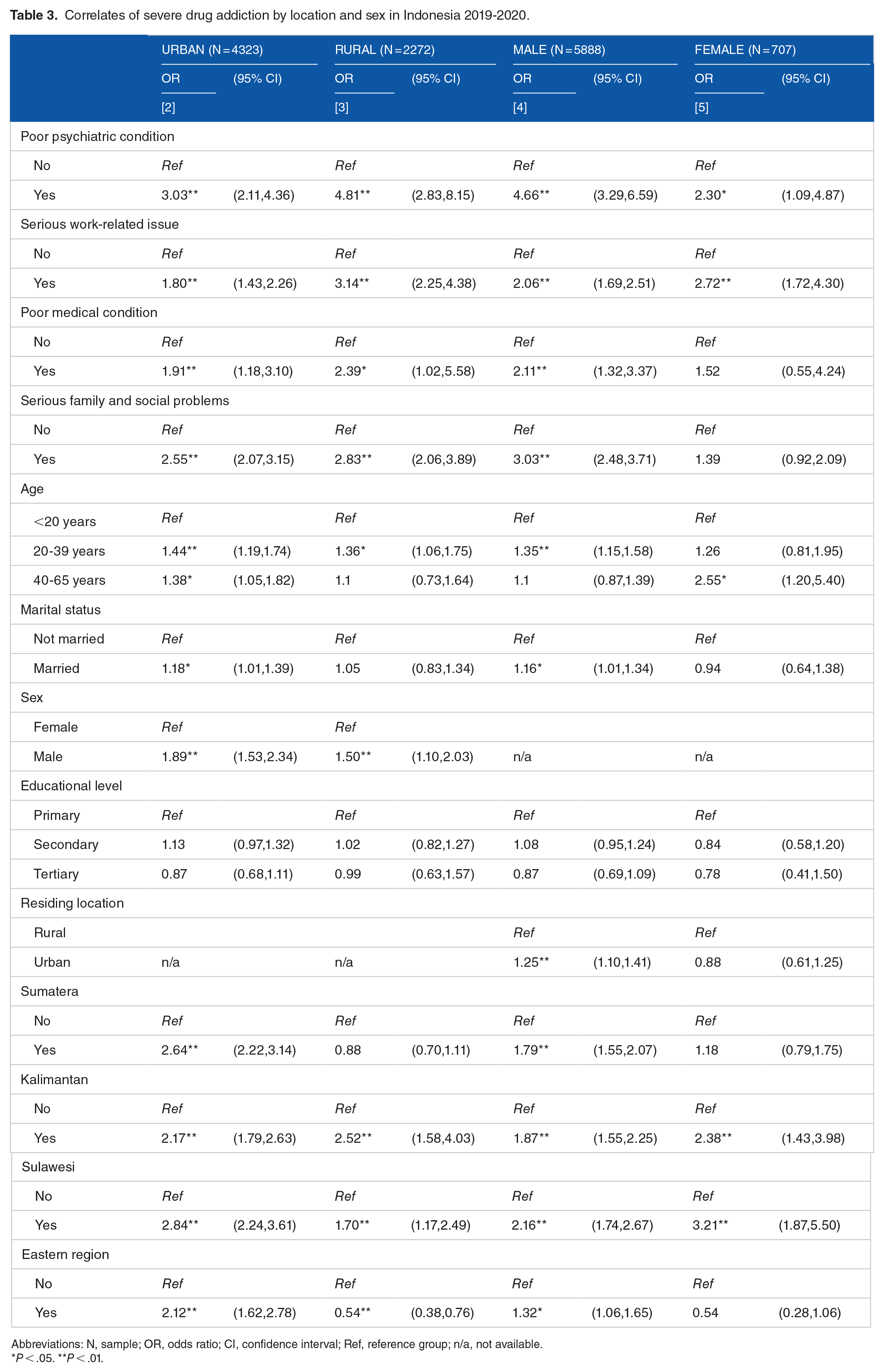
Abbreviations: N, sample; OR, odds ratio; CI, confidence interval; Ref, reference group; n/a, not available.
P < .05. **P < .01.
Furthermore, the last analysis reveals the correlations of severe drug addiction based on regional factors shown in Table 4. The associations between the 4 behavioral and environmental assessments and severe drug addiction were mixed by region. For instance, the associations between poor psychiatric condition and severe drug addiction were strongest in Sumatera (OR = 5.2 [CI: 2.4-10.9]) and weakest in Sulawesi (OR = 2.9 [CI: 1.2-7.0). The associations between serious work-related issue and severe drug addiction were strongest in Kalimantan (OR = 3.2 [CI: 1.9-5.3]) and weakest in Java (OR = 1.7 [CI: 1.3-2.4). The associations between poor medical condition and severe drug addiction were strongest in Java (OR = 2.7 [CI: 1.4-5.4]) and weakest in Sulawesi (OR = 1.0 [CI: 0.3-3.8], not significant). The associations between serious family and social problems and severe drug addiction were strongest in the Eastern region (OR = 3.3 [CI: 1.8-6.1]) and weakest in Kalimantan (OR = 2.0 [CI: 1.3-3.2]).
Correlates of severe drug addiction by region in Indonesia 2019-2020.
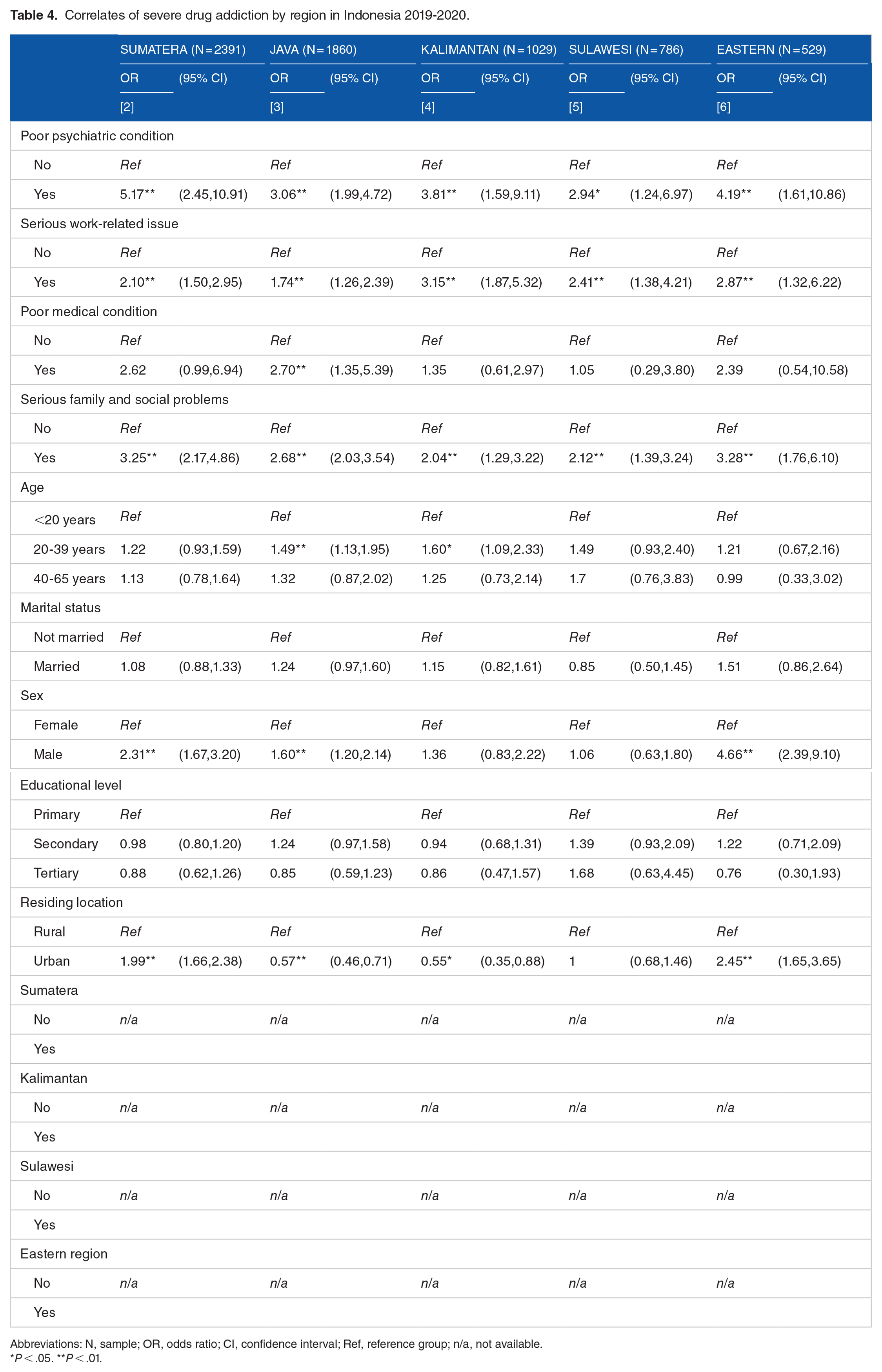
Abbreviations: N, sample; OR, odds ratio; CI, confidence interval; Ref, reference group; n/a, not available.
P < .05. **P < .01.
Discussion
In our study, we used a sample of 6790 PWUD from rehabilitation centers during 2019 to 2020 in Indonesia. A high number of 65.1% of our sample reported having severe drug addiction, which needed intervention and support. We found that factors such as poor psychiatric condition, serious work-related issue, poor medical condition, and serious family and social problems are significantly associated with severe drug addiction. We also found that socioeconomic factors (eg, age and sex) and geographic factors (eg, urban/rural and region) are significantly associated with severe drug addiction.
We found that poor psychiatric condition has the strongest association with patients having poor psychiatric conditions who were 4 times more likely to have severe drug addiction. This aligns with evidence from other settings. A study of 3079 participants in the United Kingdom concluded that problem substance use was common amongst those with severe mental health problems. 21 A meta-analysis of 22 epidemiological surveys showed the strongest associations were for drug use and major depression (OR 3.8). 22
In terms of sociodemographic factors, we found that sex is significantly associated with severe drug addiction. Male users had 1.8 times higher odds of severe drug addiction, compared to female counterparts. This finding aligns with previous studies which showed that males were more likely to have drug problems.21,22 However, this may be due to potential drug use-related stigma by gender. A literature review of 75 studies showed that women who use drugs experienced greater levels of stigma, 23 which may prevent them to seek treatment including at rehabilitation centers.
In terms of geographic factors, we found that urban location and region were significantly associated with severe drug addiction. Patients in urban areas had 1.2 times higher odds of severe drug addiction than those residing in rural areas. Also, we found that patients in Sumatera, Kalimantan, and Sulawesi had up to 2.3 times higher odds of severe drug addiction, compared to those in the Java region. The higher odds of drug addiction in urban areas is in line with theoretical evidence from other studies. The characteristics of urban environments such as higher discrepancies in income distribution and higher exposure to threatening conditions that may lead to mental issues, lower collective efficacy and higher residential segregation that may result in less controlled deviant behaviors, higher population density that increase “contagiousness” in drug misuse, and better transportation access that increase mobility of illicit drugs, are estimated to contribute to higher incidence of drug use. 24 This finding may imply an institutional barrier in seeking for treatment as most of treatment centers (both private and public) are centralized in urban areas. The barriers in accessing the treatment centers in urban areas may result in lack of rural patients captured in the sample. Since Java is the most developed region in Indonesia, the higher drug addiction in regions outside Java may stem from the inequal distribution of available services to information and treatment in less-developed areas. Lack of institution’s availability or difficulties to access nearest treatment centers have also been found as barriers from seeking harm reduction treatment programs in other countries.25 -28
The findings in this study have important implications for policymakers in refining the harm reduction policy in Indonesia and other countries with similar settings. Firstly, compared to other countries in South-East Asia, mental health services and systems in Indonesia remain underdeveloped especially due to lack of professional mental health practitioners and inadequate financial investment. 29 For patients with poor initial psychiatric condition, psychological intervention will be needed during the harm reduction programs. Therefore, strengthening the country’s mental health system and awareness is recommended. Secondly, gender stigmatization among PWUD may prevent patients from seeking treatment in drug rehabilitation centers. To address the issue, the frontliners and practitioners of the harm reduction programs will need to be adequately trained. Finally, the last implication concerns the spread and coverage of the harm reduction programs. Increasing the breadth of the current programs will be required in reaching remote and vulnerable patients.
To our knowledge, this is the first study in LMICs using a relatively large number of PWUD at rehabilitation facilities to assess behavioral, environmental, socioeconomic, and geographic correlates of severe drug addiction. However, our study has at least 2 limitations. First, given the cross-sectional nature of our data, our findings only showed correlation, not causation. For instance, we found a strong association between poor psychiatric condition and severe drug addiction. The pathway could be either poor psychiatric condition cause severe drug addiction or the other way around. Second, while our samples were relatively nationally representative with data obtained from rehabilitation centers across the country, nearly 90% of our samples were males. Thus, our findings may not be generalizable to both males and females and further study with a larger sample of female PWUD may be needed.
Conclusion
This study found a significant association between factors such as poor psychiatric condition, serious work-related issue, poor medical condition, and serious family and social problems to severe drug addiction. We also found that socioeconomic factors (eg, age and sex) and geographic factors (eg, urban/rural and region) are significantly associated with severe drug addiction. This evidence supports improvement in harm reduction policies in Indonesia and other countries with similar settings. Also, our findings highlight the need to strengthening the country’s mental health system and population awareness.
Footnotes
Acknowledgements
The authors would like to thank Universitas Indonesia for providing the grant to conduct research through the International Indexed Publication Grant (Hibah Publikasi Terindeks Internasional/PUTI Q1) with grant number: NKB-363/UN2.RST/HKP.05.00/2022.
Author Contributions
WD contributed to project conceptualization, monitoring all stages of the project, and proofread the manuscript; AA and AB contributed to conceptualization, data collection, and proofread the manuscript; NA prepare and proofread the manuscript, DK contributed to the project conceptualization; YBAP editing the format of final manuscript. All authors agree with the manuscript.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Universitas Indonesia through International Indexed Publication Grant (Hibah Publikasi Terindeks Internasional/ PUTI Q1). Grant Number: NKB-363/UN2.RST/HKP.05.00/2022.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.

