Abstract
Background and Aim
Both thalassemia and carnitine deficiency represent independent causes of erythropoietin resistance, and thus anemia, in uremic patients. We evaluated the unknown long-term effects of L-carnitine administration in β-thalassemic on chronic hemodialysis.
Methods
We studied twelve subjects (M = 8; F = 4) affected by β-thalassemia minor (β-thal; HbA2 level = 6.6 ± 0.6%) and forty non-thalassemic subjects (M = 24; F = 16) as controls (C), on chronic hemodialysis treatment. Patients and controls were at target hemoglobin levels (11–12g/dl) prior to the study and underwent to i.v. L-carnitine administration for a one year period-time.
Results
Groups were comparable for age, gender, serum levels of hemoglobin (Hb), iron, ferritine, PTH and aluminum, transferrin saturation, and dialysis modalities. During the study both groups showed significant Hb increase and erythropoietin (EPO) decrease; as a difference, such changes emerged at the 3rd month in C but at the 8th month in β-thal. At start, during the dialysis session the erythrocyte MCV reduced in C but not in β-thal (65.3 ± 3.2 to 65.5 ± 3.2 fl; NS); along carnitine administration period, however, MCV during dialysis decreased also in β-thal, starting since the 9th month of treatment.
Conclusion
This study provides evidence of the lowering of EPO resistance in β-thalassemia patients on hemodialysis due to long-term carnitine administration. Thus, prolonged carnitine supplementation should be suggested to patients on dialysis affected by β-thalassemia with poorly responsive anemia, or requiring large doses of erythropoietin.
Introduction
Anemia is very common in chronic dialysis patients and it is related to relative erythropoietin deficiency, to blood losses from both gastrointestinal tract and dialysis filter or lines, and to blood drawings for laboratory tests (1–4). Also, reduced levels of hemopoiesis compounds (iron, folic acid, vitamin B12) and reduced erythrocytes life are major contributors to anemia in dialysis (1–4). In addition, carnitine deficiency represents an independent cause of erythropoietin resistance in uremic patients. Indeed, the lack of an efficient carnitine pathway in uremia further reduces the erythrocyte half-life and the erythropoietin effectiveness (5–8); likely, the impairment of carnitine metabolism in uremia induces the worsening of erythrocyte membrane functioning (9–10). It has been demonstrated that carnitine administration in dialysis patients improves the management of anemia and reduces the erythropoietin resistance (11–12).
β-thalassemia minor (β-thal) represents a not rare cause of erythropoietin resistance in uremia in several regions, such as Mediterranean areas, but worldwide due to migrations. Indeed, in patients with β-thal on chronic dialysis, higher erythropoietin doses are needed to correct anemia, even if all the major known factors that contribute to erythropoietin resistance are corrected (13–15). The impact of carnitine deficiency on erythropoietin resistance in β-thalassemic patients on hemodialysis, however, has never been explored. Thus, the aim of this study was to evaluate the long-term effect of L-carnitine administration on the erythropoietin resistance in β-thalassemic patients on chronic hemodialysis.
Methods
Patients
Patients were included into the study on the basis of the following criteria: adult age; chronic hemodialysis treatment at a trice weekly schedule; β-thalassemia minor; stable hemoglobin (Hb) levels within the target levels (11–12g/dl) obtained by high erythropoietin (EPO) dosages. We studied β-thalassemia minor hemodialysis patients (β-thal) which were previously treated during a one-year period by progressively higher EPO doses to reach the Hb target; the control of anemia was then prolonged for a further additional one-year time (16). Diagnosis of β-thal was made on the basis of the HbA2 level (>3.5%). In order to evaluate the response of thalassemic patients to carnitine, we also studied as controls a group of hemodialyzed patients without thalassemia (C). All subjects gave their informed consent to the study.
Study design
Prior to study, we performed a six-month run-in period in order to verify the stability of Hb levels (coefficient of variation <3%). After the run-in, L-carnitine was administered at the end of each of the three HD session of the week, at the dose of 2 g for each hemodialysis session, along a 1 year period-time both in C and β-thal-m groups. Thereafter, a six months wash-out period was performed. During the study, iron gluconate was administered i.v. once a week, at the end of the third HD session of the week, to patients with iron deficiency (serum ferritin <100 mg/dl or transferrin saturation [TSAT] <20%), to keep both TSAT above 20% and serum ferritine between 100 and 500 mg/dL. Also folate and vitamin B12 were regularly administered to all patients.
Anemia was evaluated monthly, prior to the second dialysis of the week (16), by drowning blood samples from the arterial line prior to the infusion of saline or heparin and before starting the blood pump. Blood samples were also obtained at three month intervals at the end of dialysis, after 5 minutes stop-flow (blood pump rate 50 mL/min and no dialysate flow), for estimation of dialysis dose. At the end of each dialysis session, dry body weight (BW) was measured and the effective EPO dose administered was reported into the chart.
Hematocrit (Ht), hemoglobin, mean corpuscular volume (MCV) and red blood cells count were detected monthly. Serum levels of urea nitrogen (SUN), parathyroid hormone (PTH), aluminum, iron, ferritine, transferrine and TSAT%, were evaluated every three months.
Analytical determinations
Urea nitrogen was measured using an autoanalyzer (Olympus AU 400, Olympus Italia, Segrate-Milano, Italy). Hemoglobin, red blood cells, erythrocyte volume and hematocrit were measured by a blood cell counter (Cell-Dyn 3500 R, Abbot Diagnostics, Germany). PTH, plasma iron, transferrine and ferritine were evaluated with standard technique. Aluminum was determined by atomic absorbiment (17, 18).
Statistical analysis
Values are reported as mean ±SD. ANOVA for repeated measures and Newman-Keuls post-hoc test was applied for intra-group repeated measures comparison. Unpaired t-test was used for inter-group comparison. A p value <0.05 was considered statistically significant.
Results
We studied twelve subjects (M = 8; F = 4) affected by β-thalassemia minor (β-thal; HbA2 level = 6.6 ± 0.6 %) and forty non-thalassemic subjects (M = 24; F = 16) as control (C). In the β-thal and C groups the renal disease respectively was: primary glomerulonephritis in 6 and 12 patients, hypertensive nephrosclerosis in 3 and 11 subjects, diabetic nephropathy in 3 and 9 subjects, and unknown in 8 controls. No patient suffered of hepatic dysfunction.
Patients were on chronic thrice weekly bicarbonate hemodialysis; the vascular access was always native arterovenous fistula. A total of 5/12 β-thal and 22/40 C subjects used ACE-inhibitors. All patients received β-recombinant EPO at a thrice weekly schedule; the drug was administered intravenously through the inflow needle the end of each HD session.
Patients and controls were comparable for gender, age, dialysis age and dose, nutrition, hemoglobin and iron status (Table 1). Also serum levels of PTH (187 ± 98 and 205 ± 78 pg/ml; NS) and aluminum (38 ± 16 and 45 ± 12 mcg/ml; NS) did not differ between thalassemic and controls. During the study period, body weight, and dialysis both dose and UF rate, were stable in the two groups (Table 2).
Baseline characteristics of thalassemic and control subjects.
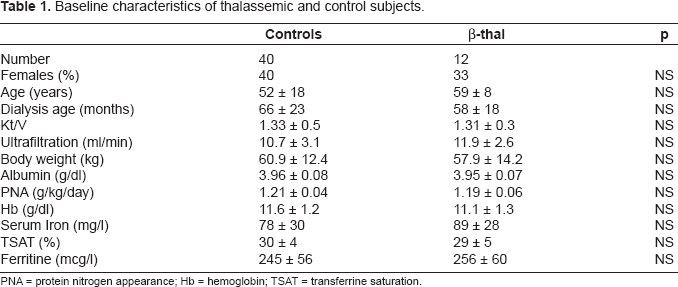
PNA = protein nitrogen appearance; Hb = hemoglobin; TSAT = transferrine saturation.
Body weight (BW), dialysis ultrafiltration (UF) and Kt/V during the study period in Controls (C) and β-thal (T) groups.
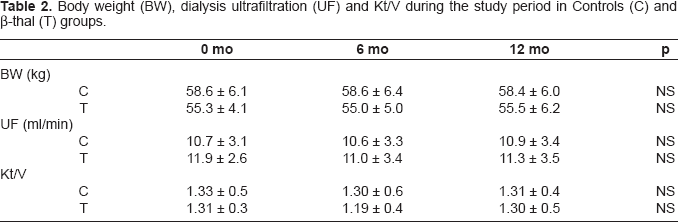
Figure 1 shows the behavior of both hemoglobin and EPO dosage in β-thal (1A) and C (1B) during L-carnitine administration. C showed significant both Hb increase and EPO dose decline since the third month during the study; β-thal group evidenced similar changes in Hb and EPO, but they were evident after 8 months of carnitine administration. At start, EPO dose was 280 and 100 UI/kg/week in β-thal and C groups, respectively; at the maximum response to EPO during the study (12th month) the EPO dose was 170 and 60 UI/kg/week in β-thal and C (stable since the 3rd-6th month) groups, respectively; thus, during carnitine administration, EPO dose decreased by the maximum of 39% in β-thal and 40% in control patients.
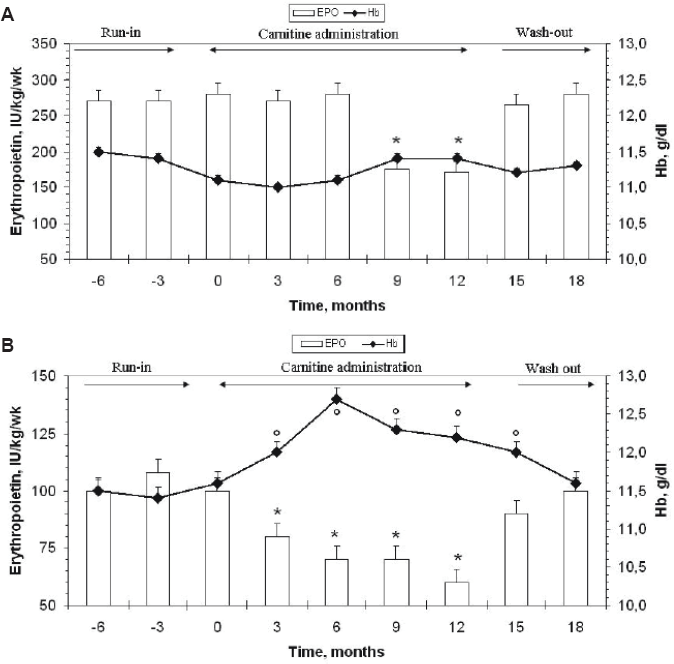
Serum hemoglobin levels and amount of EPO DOSE in β-thal (1A) and Controls (1B) subjects, prior, during and after Carnitine administration. (1A) EPO: * = p < 0.05 vs -6, -3, 0, 3, 6, 15 and 18 months; (1B) EPO: * = p < 0.05 vs -6, -3, 0, 15 and 18 months; HB: ° p < 0.05 vs -6, -3, 0 and 18 months.
Of interest, because of the intra to extracellular water shift due to the hemoconcentration determined by the ultrafiltration during the dialysis procedure, the erythrocyte MCV reduced at the end of dialysis as compared to pre-dialysis values in C, but not in β-thal; in this latter, at the start of the study, the post-dialysis MCV resulted slightly increased (65.3 ± 3.2 to 65.5 ± 3.2 fl; NS) (Figure 2). During the carnitine administration period, however, the intradialysis MCV reduced also in β-thal since the 9th month of treatment; conversely, since the first month of the recovery period after carnitine stop, the MCV in β-thal resumed to increase during dialysis.
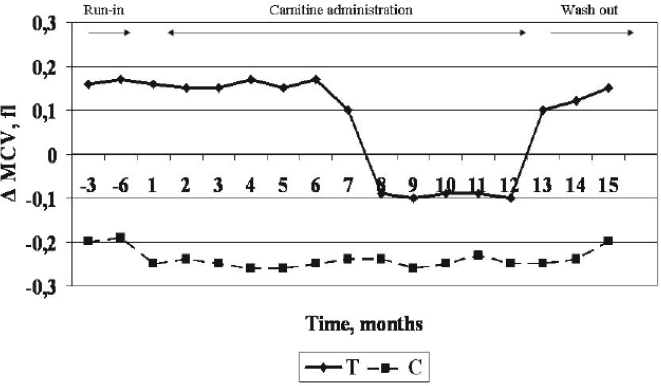
Intra dialysis MCV changes (pre minus post dialysis values) in β-thal and Controls at start, during and after Carnitine administration.
Discussion
There are compelling indicators of carnitine deficiency in chronic dialysis patients as a result of low dietary intakes and increased losses during the dialysis procedure. Koistra first described a relationship between carnitine and anemia in uremia; indeed, he reported that ESRD patients with severe anemia requiring erythropoietin had lower carnitine levels than patients who had less severe or no anemia (19). Matsamura showed a significant inverse correlation between the EPO dose required to maintain target hematocrit in dialysis and both total and free carnitine serum levels (20). All together, these data suggest that carnitine deficiency may contribute to the need for greater EPO doses in anemic, uremic patients (12, 21–25).
This is the first study investigating the effect of long-term carnitine supplementation on EPO resistance in patients on chronic hemodialysis affected by β-thalassemia. The study evidences the lowering of EPO need in β-thal by mean of 39% after 1 year carnitine administration, as compared to a 40% reduction that occurred in non thalassemic patients after 3–6 months; such EPO reduction was associated with stable hemoglobin levels within the target and was reversible after carnitine discontinuation.
A large body of evidences show that MCV results reduced during the hemodialysis due to the intravascular, and consequently intra-cellular, water removal (26–29); such erythrocyte capability is strictly dependent on the cell membrane elasticity (27–28). Our data evidenced a reduction of MCV during the hemodialysis session in the control group, but not in β-thal subjects, possibly due to the rigidity of red blood cell membrane. In β-thal patients the erythrocyte recovered such intra-dialysis capability to reduce cell volume after 8 months of carnitine treatment and again losted such a capacity 4 weeks after stopping the drug administration. Such an erythrocyte behavior is possibly related to the improvement of cell-membrane elasticity during carnitine treatment. Indeed, several authors suggested that in hemodialysis patients without β-thal the effectiveness of carnitine is related to the increasing of erythrocyte stability (30). Furthermore, it was showed in uremic rats that in vivo administration of carnitine increases the osmotic erythrocyte resistance, due to the increase of erythrocyte membrane Na+ – K+ pump activity (13–14, 31–32). Thus, our data may suggest that carnitine administration possibly induces the improvement of erythrocyte deformability in β-thal uremic patients, likely as in non thalassemic uremics; however, such effect is obtained only after a longtime treatment. It can be hypothesized that in β-thal on dialysis only the long-term carnitine administration improves the strictness of RBC, and conversely enhances the cell half-life. Indeed, other Authors showed that abnormalities in RBC deformability improves after carnitine administration, which is also responsible for hematocrit increase and EPO dose reduction (33). In this study, the EPO dose reduced from 280 to 170 UI/kg/day (-39%) at the 12th month of treatment in thal, and all patients were responders (EPO reduction range: -29 to -45%). In the control group the EPO dose decreases from 100 to 60 UI/kg/day (-40%) at the 3rd month of carnitine treatment.
Two groups of expert evaluated the efficacy of carnitine in the treatment of anemia in dialysis patients. The American Association of Kidney Patients Consensus Group concluded there is a definite role for carnitine in dialysis patients, particularly for certain conditions that do not adequately respond to the standard therapy (34). A trial supplementation period may be indicated to exclude carnitine deficiency as a cause of EPO resistance in selected patients (34). More recently, the NKF/DOQI Clinical Practice Guidelines for Nutrition in Chronic Renal Failure reported that the most promising of the proposed applications for carnitine in dialysis patients is in the treatment of EPO resistant anemia (35). It has been suggested that a 4-month trial of carnitine was reasonable in selected patients with anemia and/or very large EPO requirements and should be of adequate duration to reliably assess the response to carnitine.
Recently, Handelman based on the analysis of a database of the registered carnitine trials, concluded that carnitine benefits are not real and, consequently, the dialysis administration of carnitine is not justified (36). However, several authors, either before Handelman observation (11–13, 19–25), or even more recently (38), showed the positive effects of carnitine in patients on chronic hemodialysis. Our study adds new inside in this field, evidencing for the first time the effects of long carnitine administration also in β-thalassemic patients in chronic dialysis.
In summary, carnitine administration has been shown to be effective in many patients for the adjunctive treatment of anemia associated with chronic kidney disease. This study suggests that a very long-term carnitine administration should be useful also in uremic patients on chronic dialysis affected by β-thalassemia on target hemoglobin, by reducing the doses of erythropoietin needed to manage the anemia.
