Abstract
This study assessed the prevalence, reasons, and factors associated with refraining from seeking needed health care among the Sámi population in Sweden. Using data from a 2021 health survey, 3,658 individuals participated. Descriptive and regression analyses were applied to summarize the data and determine the magnitude of associations between independent variables and refraining from health care. Results showed 19.9% of participants refrained from seeking needed health care. Common reasons included lack of time (25%), problem resolution (16%), long wait times (16%), and uncertainty about where to seek care (13%). Factors associated with the higher prevalence of refraining included being a woman, being under 65, having lower income, experiencing economic stress, belonging to a forest reindeer herding community, and residing outside Sámi homelands. Interventions should be designed to address healthcare access inequities among vulnerable Sámi subgroups. Further research is needed to understand these disparities and reasons for refraining from care in non-pandemic contexts.
Introduction
Swedish healthcare policy is characterized by a strong commitment to ensuring equitable access to health services based on need (Lundberg, 2018; Schneider et al., 2017). Despite these efforts, inequalities in access persist among various socio-demographic groups, including those based on gender, socio-economic status, place of residence, migrant and ethnic minority status, and across regions (Janlöv et al., 2023; Kommissionen för jämlik hälsa, 2017; The Public Health Agency of Sweden, 2024). Of Sweden’s five national minorities, the Sámi people are the only Indigenous group. While scattered all over Sweden, most live in Sápmi, the historical homeland of the Sámi, covering the northern areas of Norway, Sweden, Finland, and the Kola peninsula in Russia. Sámi traditional livelihoods include fishing, hunting, reindeer herding, and small-scale farming, but today most Sámi are working within the wage economy alongside the Swedish majority population (Swedish Institute [SI], 2024). Although demographic records are lacking due to the absence of official ethnicity registration, estimates suggest a total Sámi population of approximately 100,000, with at least 20,000 residing in Sweden (SI, 2024). Despite the status of Sámi as Indigenous, Swedish healthcare policy does not mention the Sámi or clarify what that recognition means in the healthcare context; for example, the Sámi are left without the right to speak their language during healthcare encounters (Hunt, 2007).
Globally, racial and ethnic minorities, along with rural and low-income populations, persistently encounter suboptimal health outcomes (Anderson et al., 2016). This is often due to the impact of institutionalized racism and structural poverty, which hinder their ability to access and receive high-quality health care (Gee & Ford, 2011). Numerous studies have revealed that Indigenous populations in North America, Australia, and New Zealand consistently experience significantly lower access to and utilization of health care (Marrone, 2007; Nader et al., 2017; Tiwari et al., 2018). A historical overview of the access to health care of the Māori revealed that New Zealand’s predominantly universal health system failed to deliver equal services to them because of the inability to accommodate cultural and ethnic differences [17]. Similarly, research involving First Nations, Inuit, and Métis in Canada has shed light on the impact of colonial legacy and exposure to culturally unsafe care on patients’ engagement with diabetes management (Jacklin et al., 2017). Huot et al. (2019) identified four distinct themes related to access to care within the health systems of the Circumpolar North, including (1) environmental challenges such as geographical distance and accessibility, weather and seasonal conditions, and limited transportation options and high costs; (2) provider-related barriers such as staff shortages, high turnover, and lack of training and expertise; (3) cultural and linguistic differences between healthcare providers and recipients leading to communication gaps, discrimination, and dissatisfaction; and (4) health system-related factors such as the fragmented management/disjointed coordination of health services, insufficient information flow between management and staff, and financial constraints (Huot et al., 2019). A review from circumpolar countries found that the concepts of cultural safety and cultural competence were widely discussed in the Canadian literature, but not in Greenland, Nordic countries, or Russia. The lack of attention to culturally safe care for Sámi and Greenlandic Inuit was somewhat surprising to the authors, considering Nordic countries’ concern for the welfare of their citizens (Lavoie et al., 2022). This could be partly explained by the notable gap in research concerning healthcare-seeking behaviour and utilization among the Sámi population in general and in Sweden particularly (Stoor, 2016).
Research in Norway has revealed that Sámi-speaking Sámi are less satisfied with their general practitioners compared with other Sámi (Nystad et al., 2008). Studies have further identified a lack of healthcare services adapted to Sámi language and cultural needs, leaving Sámi patients’ needs unfulfilled (Engnes et al., 2022; Mehus et al., 2019).
Meanwhile, a 2007 study from Sweden found that Sámi men and women involved in reindeer herding reported significantly less trust in primary health care and mental health services than a non-Sámi control group. This distrust was hypothesized to have resulted from historical discrimination and societal marginalization, as well as structural deficiencies within the healthcare system, such as healthcare personnel lacking the necessary knowledge and understanding to offer equitable services to their Sámi patients (Daerga et al., 2012). These inequalities are likely to be exacerbated during public health emergencies, such as the coronavirus disease (COVID-19) pandemic, which was declared by the World Health Organization (WHO) in March 2020 and ended in May 2023 (WHO, 2023). The disproportionate impact of COVID-19 on ethnic minorities worldwide further highlighted the persistent health inequities in access and treatment within communities (Peterson et al., 2023; Pickering et al., 2023).
Access to timely healthcare services is a critical determinant of health, and refraining from seeking needed care represents a major public health concern, as it may result in delayed diagnoses, poorer health outcomes, and increased long-term healthcare costs (Loppie & Wien, 2022). Research in Sápmi has largely compared Sámi and non-Sámi populations, with little focus on heterogeneity within the Sámi community. Thus, the aims of this study were to assess the prevalence of refraining from seeking health care despite needs among the Sámi in Sweden, to identify the reasons for the refraining, and to uncover their associated factors in 2021.
Methods
Study design
The SámiHET survey is a population-based health study conducted among the Sámi population in Sweden, on behalf of the Sámi Parliament in Sweden. Inaugurated in 1993, the Sámediggi (Sámi parliament) is a Swedish governmental authority within the area of Sámi culture and reindeer herding, as well as a nationally elected body with 31 parliamentarians, representing the Sámi people in Sweden.
The SámiHET study was implemented following the Norwegian guidelines for Sámi health research, including acquiring the collective consent of the Sámi people in Sweden (Kvernmo et al., 2018). Representatives from the parliament were regularly consulted throughout the study’s design and implementation. The research was developed and carried out by a culturally diverse team of Sámi and non-Sámi scholars from various disciplines. While our positionality likely shaped the study’s conception, design, and interpretations presented in this article, the group is grounded in long-standing, reciprocal relationships with the Sámi community. The main results have been presented and discussed with both the Sámi Parliament and other Sámi stakeholders.
Participants
Due to the non-inclusion of Sámi identity information in the Swedish population registers, three existing administrative registers were utilized to establish a Sámi population frame (Stoor & San Sebastián, 2022). Individuals aged 18 to 84 years and listed in any of the following registries were included in the total sampling frame: (1) the Sámi electoral roll, (2) the reindeer mark registers, and (3) those with reindeer herding as a source of income within the “labour statistics based on administrative sources” register.
A total of 9,249 individuals were identified and sent an invitation to participate in the study. Out of these, 3,779 answered the survey, resulting in a participation rate of 40.9%. However, 121 persons did not unequivocally self-identify as Sámi and were, therefore, excluded from further analysis. Thus, the analytical sample of the SámiHET study comprised a total of 3,658 individuals. Data collection took place from February to May 2021. Additional details about the study design can be found in a previous publication (Stoor & San Sebastián, 2022).
Questionnaire
The 2021 SámiHET survey consisted of 81 primary questions that covered topics such as Sámi identity and language, discrimination, demographic characteristics, lifestyle, general, mental and oral health, and access to or utilization of healthcare services. Individual questionnaires were linked to register data using the personal identity number by Statistics Sweden, allowing the inclusion of register data on age, civil status, education, and income. Sámi stakeholders were consulted regarding the questionnaire design, and a group of Sámi volunteers pilot-tested it in November 2020.
Variables
The outcome variable was defined as “refraining from health care”, which refers to situations where individuals choose not to seek medical or dental care even when they believe they need it. This was determined by the question: “Have you felt the need for medical care during the last 3 months but refrained from seeking it? Respondents were given two options to choose from: ‘Yes’ or ‘No’.” Those who answered “Yes, but the problem was solved” to a follow-up question on reasons were also classified as non-refraining, since they no longer needed to seek care.
The independent variables were categorized into three groups: socio-demographic, socio-economic, and culture-related factors, based on the literature and data availability (Lee & You, 2021; Splinter et al., 2021; WHO, 2010). Socio-demographic factors included six variables. Registered sex included men and women, while self-reported sexual orientation identity was dichotomized into heterosexual and other. Age was stratified into four groups (18–29, 30–44, 45–64, and 65–84 years), per the Public Health Agency of Sweden’s standard practice. Self-reported living arrangement was differentiated into living with others and living alone, and place of residence was categorized into four regions: Norrbotten, Västerbotten, Jämtland Härjedalen, and other (representing the rest of the country). A rurality variable was included based on the official classification of Sweden’s 290 municipalities (Swedish Association of Local Authorities and Regions, 2017), which considers each municipality’s population size, proximity to urban areas, and commuting patterns to urban areas. “Large city” was defined as a municipality with >200,000 inhabitants (Stockholm, Gothenburg, or Malmö) or a municipality which is close to a large city and is functionally connected to a large city by a high commuting frequency (>40% of the population); “medium-sized city” included a medium-sized municipality of >50,000 inhabitants, with at least 40,000 residing in the largest urban area, or a commuting or non-commuting municipality close to a medium-sized municipality; and “small town or rural area” were municipalities not meeting the criteria for either of the other two groups.
This study also included four socio-economic variables: (1) level of education, categorized as low (compulsory; 9 years of schooling), medium (10–12 years of schooling), and high (postgraduate; >12 years of schooling) according to Statistics Sweden’s classification; (2) employment status, determined by the question “Are you currently employed?” with yes/no answer options; (3) individual disposable income, defined as the remaining amount for consumption or savings after taxes, divided into quintiles (with quintile 1 representing the highest income); and (4) economic stress, which was assessed with the following question: “During the last 12 months, have you ever had difficulty managing regular expenses for food, rent, bills, and so on? The response options were ‘no’, ‘yes, once’, and ‘yes, more than once’.”
Two self-reported questions related to the Sámi cultural context were further included in the study, as cultural factors can affect health beliefs and health-seeking behaviour. First, Sámi language proficiency was dichotomized into fluent and non-fluent speakers and second, if they belonged to a Sámi reindeer herding community (RHC), with response alternatives including mountain, forest, concession communities, or none. Reindeer herding is a traditional Sámi livelihood in Sweden. Swedish legislation demands it to be organised in samebyar (communities). Sámi RHCs are a form of economic association, wherein its members are entitled to own reindeer and practice reindeer husbandry. Each RHC has a specified grazing area for their reindeers and a maximum number of reindeers to be kept.
To explore the reasons for refraining/not visiting health care, respondents who reported refraining from seeking care were asked: “What was the reason or reasons for not seeking medical care?” Respondents could select multiple answers from the following options: (1) symptoms resolved on their own, (2) long wait times, (3) could not get an appointment quickly enough, (4) negative experiences from previous visits, (5) economic reasons, (6) lack of time, (7) did not know where to go, and (8) other reasons.
Data analysis
The frequencies of the independent variables and the outcome of the sample together with the reasons for refraining were first calculated. Thereafter, prevalence ratios (PRs) were used to summarize the magnitude of association between the independent variables and refraining from health care with their 95% confidence interval (CI) for inferential purposes. All statistically significant variables in the crude models were included in a multivariable regression model. Multicollinearity among the independent variables was assessed with the variance inflation factor (VIF), with a VIF value of less than 5 indicating low multicollinearity. An individual weight for each respondent was calculated by Statistics Sweden based on the total frame population and the following background variables: sex, age, education, income, and the register from which the participant was included in the study. This was done to ensure that the results could be reported for the whole frame population and not just the respondents. Sampling weighting was thus applied in all analyses conducted, using Stata 14 software.
Ethics
This study received approval from the Swedish Ethical Review Authority (Dnr 2020-04803, Ö 70 2020/3.1) and adherence to the Ethical Guidelines for Sámi Health Research was ensured (Kvernmo et al., 2018). The letter of invitation, which was available in Swedish as well as in North, Lule, and South Sámi languages, explained the purpose of the study and the implications of participation. Participants provided their consent by returning their filled-out questionnaires by mail or using an online portal.
Results
Participants’ characteristics
The total sample consisted of an equal proportion of men and women, with the vast majority identifying as heterosexual. The mean age was 53.7 years, and only one in five lived alone. Geographically, almost half resided in the Norrbotten region, followed by a quarter in Västerbotten. Most participants lived in small towns in rural areas, with only 1 in 10 living in big cities. Almost a quarter of the participants (23.7%) had a high level of education, only 3% claimed to be unemployed, and 14% reported economic difficulties. Six out of 10 participants did not belong to an RHC, but almost a third belonged to a mountain RHC. Most respondents (77.1%) were not fluent in the Sámi language. Details of the sample characteristics are displayed in Table 1.
Characteristics of the total sample, SámiHET 2021.

Reported reasons for refraining from seeking health care
The total prevalence of refraining was 19.9%. A substantial proportion of respondents (40%) refrained from seeking care for reasons not captured by the listed options. A quarter of the participants (25%) reported refraining due to lack of time, with an equal proportion regardless of sex. Approximately 16% refrained because the problem resolved and due to long wait times, with a higher proportion among men than women, while 13% refrained because they did not know where to go, with the proportion of women double than that of men. Only 5% mentioned economic reasons or delayed appointment times as motives for refraining, with a slightly higher proportion among men than women. The shares of reasons for refraining are illustrated in Figure 1.
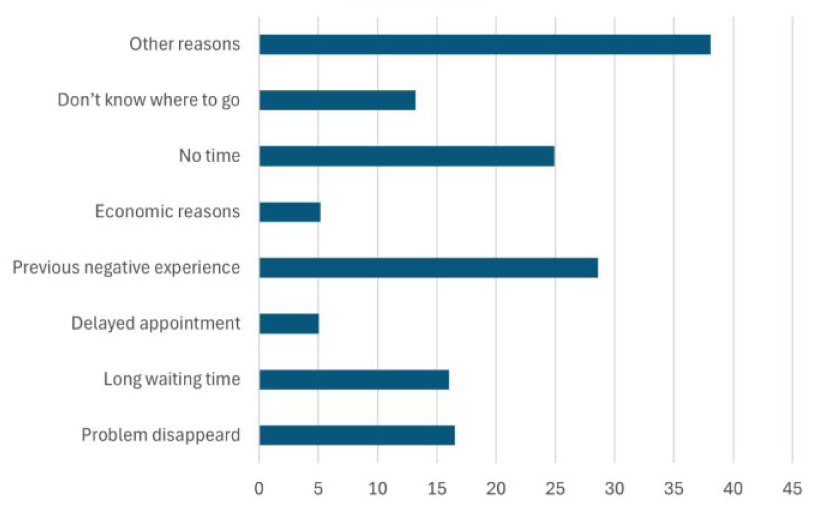
Shares (%) of reasons for refraining.
Determinants of refraining from healthcare refraining among the Sámi in Sweden
Our bivariable analyses revealed significant associations between refraining from health care and several factors, including gender, sexual orientation, age, region of residence, income, difficulties to make ends meet, belonging to a Sámi RHC, and being fluent in the Sámi language. However, after adjusting (a), the prevalence of refraining remained significantly higher among women (aPR: 1.26, 95% CI: 1.09–1.46), among all age groups in years, 45–64 (aPR: 1.91, 95% CI: 1.52–2.40), 30–44 (aPR: 2.17, 95% CI: 1.72–2.74), and 18–29 (aPR: 1.76, 95% CI: 1.34–2.32), compared with the reference elderly, and among those residing in other regions outside Sápmi (aPR: 1.23, 95% CI: 1.03–1.47). Regarding socio-economic status, all income groups and having difficulties making ends meet once (aPR: 1.41, 95% CI: 1.12–1.78) or several times (aPR: 1.81, 95% CI: 1.49–2.21) were statistically significantly associated with refraining. In addition, those belonging to a forest Sámi RHC (aPR: 1.31, 95% CI: 1.03–1.67) reported a higher prevalence of refraining (Table 2).
Prevalence of refraining from health care and crude and adjusted regression estimations based on the prevalence ratio (PR) and their 95% confidence interval (CI).
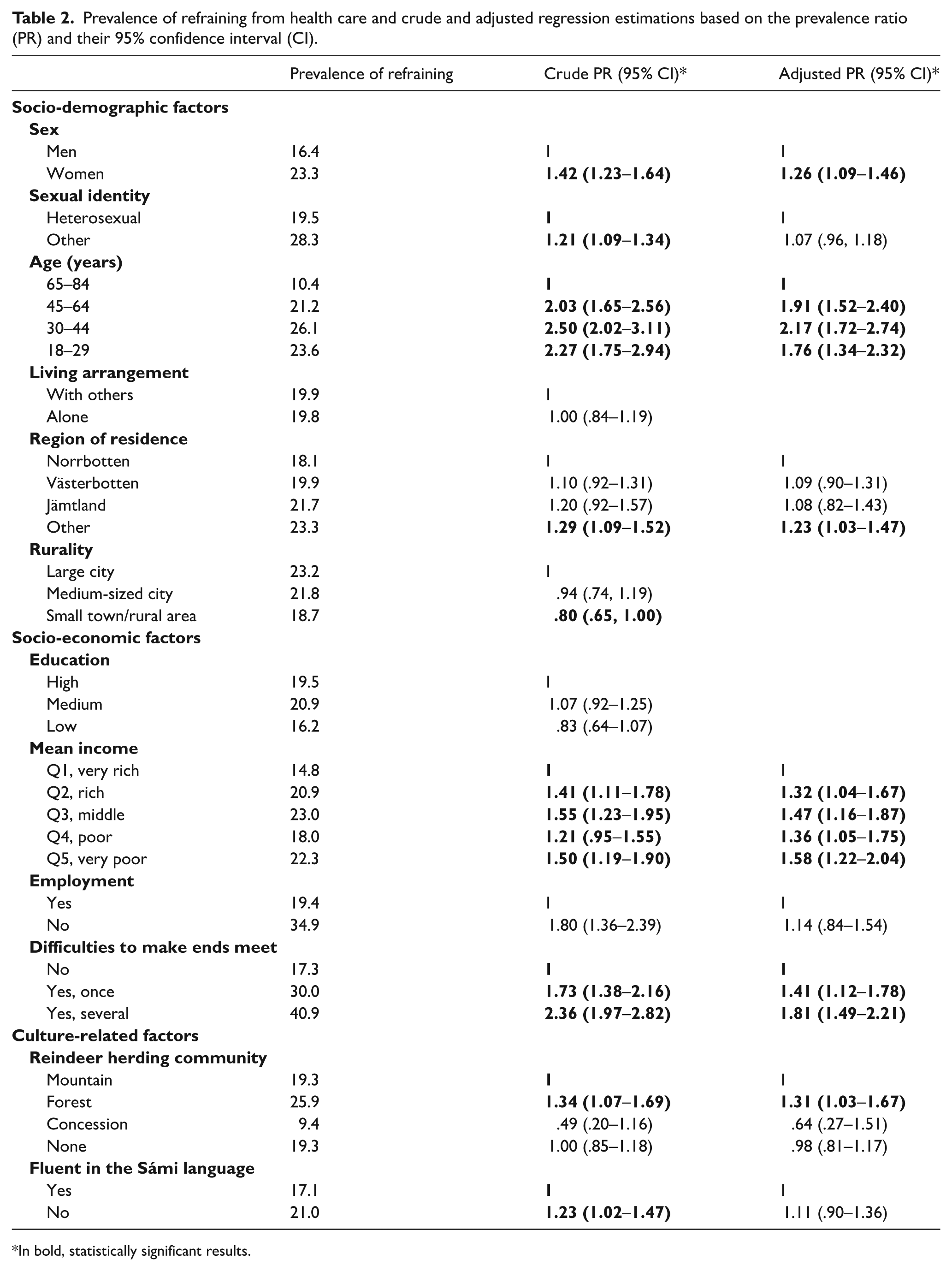
In bold, statistically significant results.
Discussion
This study revealed that one in five Sámi participants refrained from seeking health care during the last 3 months, despite their needs, in 2021. While 4 in 10 refrained for reasons not listed, the most frequently cited reasons for refraining included lack of time, the problem being resolved, long wait times, and uncertainty about where to seek care. Being a woman, under the age of 65 years, having a low income, experiencing economic stress, belonging to a forest RHC, and residing outside the Sámi homelands were associated with a higher prevalence of refraining.
Prevalence of refraining from seeking needed care
Our findings indicate a significantly higher prevalence of refraining among the Sámi from seeking health care despite perceived needs over the past 3 months, compared with a general Swedish population study (3%) conducted in 2012 (Molarius et al., 2014). Studies on Indigenous populations commonly show significantly lower access to and utilization of healthcare services when compared to their countrymen (Marrone, 2007; Nader et al., 2017; Tiwari et al., 2018). For instance, the 2018–2019 National Aboriginal and Torres Strait Islander Health Survey (NATSIHS) reported a higher refraining rate (30%) among Indigenous Australians (Australian Institute of Health and Welfare & National Indigenous Australians Agency, 2023). The observed differences in refraining rates between our study and the Australian survey could be attributed to the specific historical, social, and health system contexts but also to the different study periods (before vs. during the pandemic).
Reasons for refraining from seeking needed care
Four in 10 in this study refrained seeking health care for reasons beyond those listed, which warrants further investigation. This may suggest a possible impact of the COVID-19 pandemic on health-seeking behaviour, as our study was conducted during the pandemic’s second year. This has been shown in another context where healthcare utilization decreased by about one-third during the pandemic, as many people avoided seeking care due to fears of contracting COVID-19 (Moynihan et al., 2021; Vander Woude et al., 2023).
The most frequently reported reason for refraining from seeking health care was lack of time (25%). A plausible explanation is that Sámi prioritized work or other activities over their health or that the health need was not severe enough to warrant seeking care. A similar result was observed in the 2017–2018 NATSIHS study; however, as previously mentioned, comparisons are challenging due to the different study contexts and periods (no pandemic vs. pandemic situation in our study) (Australian Institute of Health and Welfare & National Indigenous Australians Agency, 2023). Other reasons mentioned included the problem being resolved (16%) or long wait times (16%). The latter has also been reported in a previous national Swedish study, where long wait times or the unavailability of services at the required time were cited (18%) as main reasons for not seeking health care (Westin et al., 2004). Once again, the different study periods make comparisons difficult.
Nevertheless, unlike our study (5%), nearly one-third (34%) of respondents in the NATSIHS study and one in five respondents in previous Swedish studies mentioned cost/economic reasons as a barrier to accessing health care (Elofsson et al., 1998; Westin et al., 2004). The low share of respondents citing economic reasons is positive and may indicate that an inability to pay out-of-pocket is a small concern in this context.
Our results further revealed that 13% of participants refrained from seeking needed care because they did not know where to go. This may indicate the difficulty or inability to navigate the healthcare system or the unavailability of services in remote geographical areas. For instance, the digital development in Swedish health care is contributing to a “digital health divide” due to the varying abilities of individuals to access and use available digital technologies (Bywall et al., 2024). Moreover, living in a rural location has been identified as a barrier to accessing adequate health care for communities, regardless of race (Chan et al., 2006; Huot et al., 2019; Marrone, 2007). Rural health facilities often struggle with understaffing and face challenges in attracting health providers to live and work in remote communities. This problem particularly affects Indigenous peoples, as the majority tend to live in relatively rural areas (Australian Institute of Health and Welfare & National Indigenous Australians Agency, 2023; Marrone, 2007; Yangzom, 2023).
Risk factors of refraining from seeking health care despite needs
Several socio-demographic and economic factors were associated with refraining. The higher prevalence among women aligns with patterns observed in other studies conducted in Sweden and elsewhere (Corscadden et al., 2018; Elofsson et al., 1998; Wamala et al., 2007; Westin et al., 2004). The authors have attributed the differences in help-seeking behaviours between men and women to both biological processes and biosocial mechanisms. Among these, the gender care gap—referring to inequalities in housework, division of chores, and caregiving responsibilities—plays a significant role in shaping individuals’ perceptions, attitudes, and behaviours regarding healthcare utilization (Kitterød, 2016; Springer et al., 2012). The association is, however, complex. While a recent study in Northern Sweden found that women had lower trust in the health system compared with men (Baroudi et al., 2022), no differences in confidence in primary health care and mental health services between men and women in the reindeer herding Sámi population have been reported (Daerga et al., 2012).
The prevalence of refraining from seeking health care among working-age/younger individuals (18–64 years) was more than double that of the oldest group (65–84 years). Explanations may include working-age Sámi prioritizing work, family, or other needs over their health. In addition, the 2016 Commonwealth Fund International Health Policy (CFIHP) Survey of Adults showed that in most of the 11 countries surveyed, people aged 65 and older were less likely to encounter multiple barriers to accessing primary care than younger adults (Corscadden et al., 2018). This finding likely suggests that older adults are more knowledgeable and familiar with the use of primary healthcare services than younger individuals (Tillmann et al., 2021).
Unsurprisingly, individuals with low-income levels and those experiencing economic stress were more likely to refrain from seeking health care compared with their reference groups. Income level and economic stress are well-documented determinants of healthcare access within the general population (Corscadden et al., 2018; Gerdtham & Sundberg, 1998; Häger Glenngård & Borg, 2019; Molarius et al., 2014). The 2016 CFIHP Survey revealed that individuals with below-average incomes were significantly more likely to experience access barriers than those with above-average incomes in nearly all surveyed countries, including Sweden (Corscadden et al., 2018). In addition, a Swedish study found that higher-income groups visit doctors more frequently, while lower-income groups tend to stay in hospital longer due to delays in seeking medical attention, leading to more severe conditions (Gerdtham & Sundberg, 1998).
Conversely, it was surprising to observe a higher prevalence of refraining among Sámi residing outside the Sámi homelands, which mostly included large urban areas like Stockholm and Gothenburg. While this may reflect a lack of attention to the cultural needs of Sámi patients in urban settings (Lavoie et al., 2022), perhaps the COVID-19 pandemic affected Swedish regions and communities differently, which may have led to different patterns of health care seeking in northern and southern regions during the pandemic. While previous findings suggest Sámi-speaking Sámi report lower satisfaction with general practitioners compared with Sámi who do not speak their language (Nystad et al., 2008), being fluent in a Sámi language was not a risk factor in this study. However, complex socio-cultural processes might affect relevant behavioural patterns, beyond the supply and demand of healthcare services in the Sámi language. For example, Sámi language proficiency may be an indicator of strong affiliation to Sámi cultural values, which have been described as celebrating stoicism and self-sufficiency (Stoor et al., 2019). Finally, the increased risk of refraining from health care among members of forest Sámi communities compared with others may reflect a different prioritization due to structural reindeer husbandry stressors and, or, or both, a reduced capacity to attend to one’s own health needs in these communities. More research is needed to shed light on this issue.
Limitations
Caution is advised when interpreting these results since the patterns of refraining from seeking health care during the COVID-19 pandemic likely differed from those before and after the pandemic. In addition, due to the cross-sectional design of this study, the findings should not be used to infer causal relationships. Although the outcome variable pertains to the preceding 3 months, the self-reported nature of the questionnaire could have introduced recall bias. In addition, the study relied on three administrative registers for identifying the frame population, excluding Sámi individuals not included in these registers. Although the relatively low response rate (≈ 41%) was comparable to a similar Swedish public health survey conducted at the same time (response rate ≈ 44%), it may still have introduced selection bias, likely resulting in under-estimation of healthcare refraining. Moreover, the finding that approximately 40% of respondents refrained from seeking care for reasons not listed in the survey is noteworthy. This may suggest a mismatch between the survey design and the lived realities of the Sámi population, underscoring the need for qualitative studies. Finally, a more structural perspective on factors limiting access to health care would have been valuable. However, our analysis was constrained by the data available in the SamiHET survey. Since such information was not accessible, we were unable to address these aspects directly. By applying sampling weights, we were able to mitigate non-response bias in several key groups (young, men, the less educated, and those with low income). As a result, we believe that these results provide the most representative estimates of healthcare refraining among Sámi to date, while also highlighting the need for future research to assess their relevance beyond the pandemic context.
Conclusion
This study revealed that one in five Sámi individuals in Sweden refrained from seeking health care during the last 3 months, despite their needs, in 2021 and that 4 in 10 participants refrained from seeking health care for reasons not captured by the listed options. Women, younger age groups, individuals with low- to middle-income levels, those experiencing economic stress, those living outside the Sámi homelands, and those belonging to a forest RHC refrained from seeking health care to a greater extent than their counterparts. These findings underscore the need for culturally safe health care as defined by the Sámi themselves, along with formal recognition in Swedish healthcare policy of the status of Sámi’s status as Indigenous and its implications. They also highlight that achieving health equity among the Sámi in Sweden requires targeted interventions to address inequities in healthcare access among vulnerable subgroups. This includes promoting gender equality, improving socio-economic conditions of the most vulnerable, and ensuring culturally safe, community-led care that is tailored to Sámi needs. Further research is warranted to explore the observed disparities and the reasons for refraining from seeking care, using qualitative methods to gain deeper insights into the barriers faced by the Sámi. In addition, longitudinal studies could help clarify the causal relationships between socio-demographic factors and healthcare utilization.
Footnotes
Acknowledgements
The authors would like to thank the participants of the SámiHET survey; ollu giitu! They also wish to thank Sámediggi (Sámi Parliament) for commissioning the SámiHET study, the Public Health Agency of Sweden for collaboration, and the Statistics Sweden for their assistance with data collection. We also extend our heartfelt thanks to the Public Health Agency of Sweden, the Swedish Research Council, and the Faculty of Medicine at Umeå University for their funding support.
Authors’ note
Ethical considerations
This study received approval from the Swedish Ethical Review Authority (Dnr 2020-04803, Ö 70 2020/3.1) and adherence to the Ethical Guidelines for Sámi Health Research was ensured (Kvernmo et al., 2018). The letter of invitation, which was available in Swedish as well as in North, Lule, and South Sámi languages, explained the purpose of the study and the implications of participation.
Consent to participate
Participants provided their consent by returning their filled-out questionnaires by mail or using an online portal.
Author contributions
MSS and JP contributed to the study’s conception, design, and data collection. MSS performed the data analysis. FKNK drafted the article. All authors reviewed the article’s intellectual content and approved the final version.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and publication of this article: This work was mostly funded by the Public Health Agency of Sweden with contributions from the Swedish Research Council (grant 2020-01779) and the Strategic Funding from the Faculty of Medicine at Umeå University, Sweden (grant FS 2.1.6-339-20).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and publication of this article.
Data availability statement
The data sets analysed in this study are not publicly available due to Swedish legal restrictions on personal data and the current ethical approval. However, they can be accessed upon reasonable request and after obtaining the necessary permissions.
