Abstract
The number of elderly patients initiating hemodialysis (HD) increased considerably over the past decade. Arteriovenous fistulas (AVFs) are the preferred vascular access (VA) type in most HD patients. Choice of VA for older hemodialysis patients presents a challenge. The higher incidence of comorbidities, longer AVF maturation times, risk of primary failure, risk of patency loss, and shorter life expectancy are important factors to consider. In this review we provide a comprehensive analysis on maturation rates, primary failure, patency, and mortality regarding vascular access in patients older than 75 years of age.
Keywords
Introduction
With the population aging, the burden of age-related chronic conditions, including kidney failure, is increasing globally. 1 According to the latest U.S. Renal Data System the prevalence of end-stage renal disease (ESRD) increased to a new high of 2242 cases per million people in 2018. The number of elderly patients initiating dialysis increased considerably over the past decade, with the highest increase in prevalence among patients older than 65 years.2,3
A functional vascular access (VA) is vital to achieve an appropriate dialysis dose in patients with ESRD. 4 Also, the complications related to VA are strongly related with the morbidity and mortality of patients. The arteriovenous fistula (AVF) is strongly recommended as the preferred VA by current clinical practice guidelines, based on the best long-term outcomes, lowest mortality, and lowest health care costs of AVF compared with arteriovenous graft (AVG) and central venous catheter (CVC).5 –8
Nevertheless, in the elderly, the higher incidence of comorbidities, such as peripheral vascular disease, diabetes mellitus and hypertension, longer AVF maturation times and risk of primary failure, risk of primary and secondary patency loss, and shorter life expectancy are important factors to consider when we think if Fistula-First Initiative is appropriate approach.3,7 –9
According to the 2019 KDOQI VA guidelines, the vascular access plan should be focused on an individualized patient-centered approach, prioritizing the patient’s preference and goals.6,10,11 To date, there are no guidelines concerning VA specifically tailored for elderly patients. In the past decade, several studies have focused on VA and patient outcomes in this population.
In this review, we provide a literature review of existing data concerning VA creation in elderly patients undergoing HD, identify risk factors for failure of vascular access and strategies to improve VA outcomes in this population.
Methods
For this narrative review, we conducted the following literature searches in October 2021 through the PubMed search engine with the MeSH terms: (1) elderly, vascular access, dialysis; (2) elderly, arteriovenous fistula, outcomes; (3) elderly, arteriovenous graft, outcomes; (4) elderly, central venous catheter, outcomes; (5) octogenarians, vascular access, dialysis, outcomes.
Inclusion criteria were articles published in English after the year 2008 up to 31st of October 2021, of adult hemodialysis patients older than 75 years of age, evaluating patient characteristics, and VA and patient outcomes.
Maturation failure or primary failure was defined as an AV inadequate for successful needle cannulation after placement. Primary patency was defined as the period from VA placement until the first intervention to preserve or restore blood flow, first VA failure, or study end, whichever occurred first. Secondary patency was defined as the period from VA placement until VA abandonment for any cause, regardless of the number of subsequent interventions.12,13 Statistical analysis was not performed.
We will now consider the literature with regards to primary failure, patency outcomes, and mortality.
Primary failure in elderly patients
Older age has been associated with primary failure of AVFs.14,15 In a retrospective study of 20,360 patients, the rate of AVF failure increases by 1% for every year above 67 years. 16 The higher prevalence of peripheral vascular disease and diabetes mellitus are important factors which contribute to AVF failure in elderly patients. 17
The rates of primary failure in elderly patients have been contradictory in studies performed over the last two decades, ranging from 16% to 40%.18 –20 More recently, two large retrospective studies reported primary failure rates of 22.1% and 27%, in patients older than 75 years.21,22 The unfavorable results reported by Diandra et al. 23 of a primary failure of 72% in 47 AVFs performed in octogenarians reflect the small sample and high prevalence of diabetes in this population. Indeed, Werner-Gibbings et al. 20 documented a primary failure rate of 16% in 77 octogenarians of whom only 30% had diabetes (Table 1).
Vascular access outcomes in elderly patients.
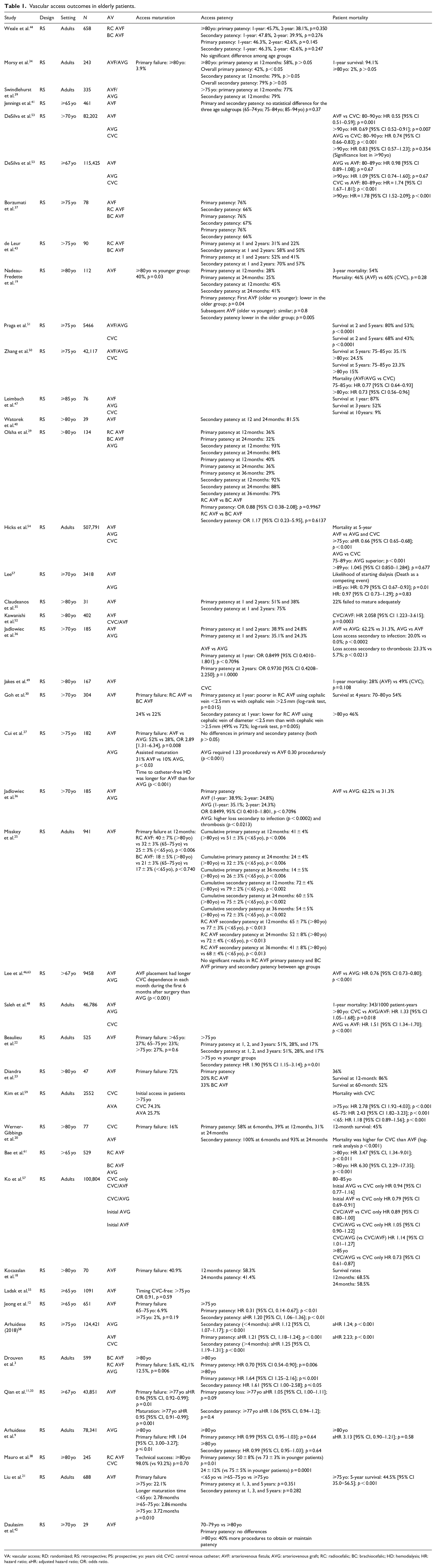
VA: vascular access; RD: randomized; RS: retrospective; PS: prospective; yo: years old; CVC: central venous catheter; AVF: arteriovenous fistula; AVG: arteriovenous graft; RC: radiocefalic; BC: brachiocefalic; HD: hemodialysis; HR: hazard ratio; aHR: adjusted hazard ratio; OR: odds ratio.
Variations in the outcomes of primary failure have also been reported in different AV locations. Primary failure rates have been reportedly higher on distal locations in several studies.3,24 Drouven et al. 3 reported primary failure rates of 42.1% in radiocefalic and only 5,6% rate in brachiocephalic AVFs (p = 0.006) in a cohort of 599 octogenarians. In a retrospective cohort of 563 patients with a median age of 75.9 ± 4.7 years, the primary success of forearm AVFs was 76% versus 94% in proximal AVFs (p = 0.007). 24 Similarly, Misskey et al. 25 described 40 ± 7% versus 18 ± 5% primary failure rates of radiocefalic and brachiocefalic AVFs in patients older than 80 years. Interestingly, in this study, age had an impact on primary failure of distal AVFs (primary failure of 40 ± 7% in >80 years versus 32 ± 3% in 65–75 years versus 25 ± 3% in <65 years, p < 0.006), however, no significant difference was found among different age groups for brachiocefalic AVFs (p < 0.470). 25 A meta-analysis of 13 studies reported a pooled effect in favor of elbow AVF creation in elderly patients. 26
There are data suggesting that AVGs are a reasonable first-line choice for access in selected elderly patients, with reports of higher primary failure rate for AVFs than for AVGs. Cui et al. compared the outcomes for 138 fistulas and 44 grafts that were placed in patients older than 75 years and reported a superiority of AVGs over AVFs in terms of primary failure (OR 2.89 [95% CI 1.31–6.34]; p = 0.008). Additionally, time to catheter-free dialysis was longer for fistulas than for grafts (p < 0.001). 27 Drouven et al. 3 also found significantly lower rates of primary failure in AVGs compared with AVFs (p = 0.006).
Ultrasound mapping has been shown to decrease the rates of AVF primary failure. 28 In a retrospective study of 134 octogenarian patients, 88% of new access created were AVFs placed only if vein size was of at least 3 mm on the ultrasound evaluation, AVF placement was successful in most patients. 29 Goh et al. 30 found that immediate failure of AVFs was similar despite vein diameter, although primary and secondary patency were longer for veins with >2.5 mm in diameter. A proper vascular assessment of elderly patients allows for a better VA planning, by choosing to place a VA with higher likelihood of maturation success.
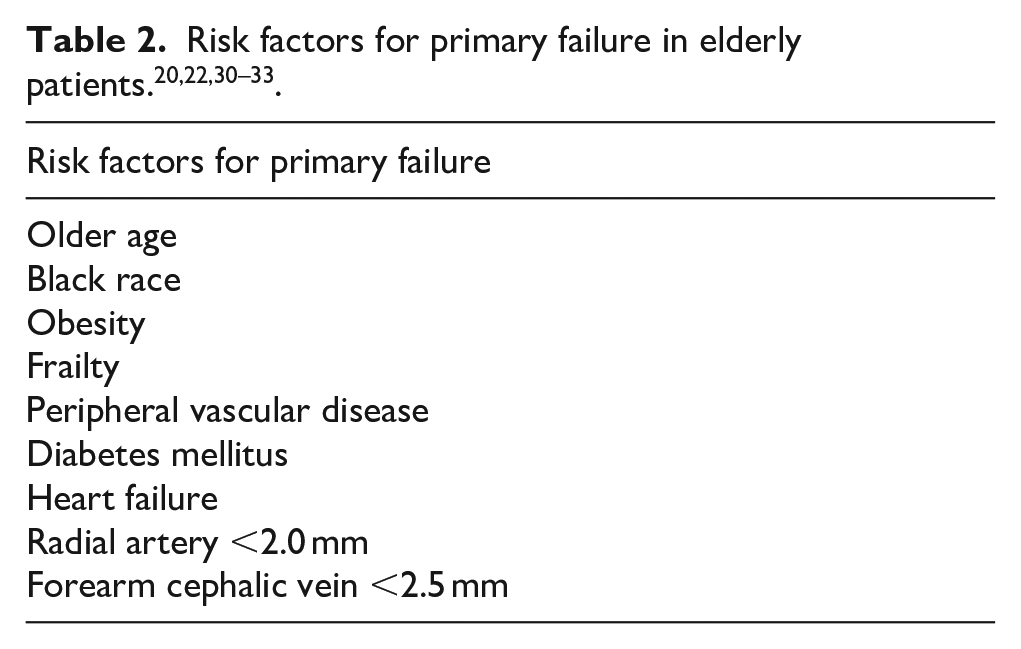
Risk factors for primary failure
Several factors have been identified to influence the likelihood of primary failure. Age over 65 years, female gender, black race, obesity, frailty, vein diameter, comorbidities such as diabetes, peripheral vascular disease, heart failure have been reported to contribute to higher rates of primary failure.31,32 (Table 2) Therefore, age per se should not preclude placement of AVFs but warrants adequate evaluation prior to access placement.
Having a risk predictor model of primary failure could assist decision making for VA placement and improve patient outcomes. Lok et al. 14 developed a risk equation for AVF primary failure, from a retrospective cohort of 422 hemodialysis adults, which incorporated patient age ⩾65, white race, and history of peripheral vascular disease and coronary artery disease. Although this risk equation achieved good predictive accuracy and external validation, in elderly patients the results were not promising. 33 A more adequate model with strong predictors for primary failure remains to be determined to better serve clinical evaluation in this population.
Patency loss in elderly patients
The reported rates of primary patency range from 40% to 70% at 1 year of follow up.18,20,25,34 –37 Primary patency reduces over time, ranging from 20% to 40% at 2 years of follow-up.18,20,22,25,36,38 In our review few studies analyzed primary patency beyond 2 years, probably because mortality in this population is significantly high after that. Indeed, at 3 years of follow-up, Beaulieu and Misskey reported low primary patency rates of 17% and 14 ± 5%, respectively.22,25
As for secondary patency, studies have reported rates ranging from 50% to 80%.34,35,37,39,40 A large retrospective study in 2017, reported a high secondary patency at 1 year of 72 ± 4% in patients older than 80 years. 25 On the other hand, Nadeau-Fredette et al. 19 reported a secondary patency at 1 year as low as 45% in 112 patients older than 80 years. Secondary patency reduces with time and rates have been reported to vary between 20%–80%. Werner-Gibbings and Olsha attributed the high secondary patency rates of their cohorts, 93% and 88% at 2 years of follow-up, respectively, to preoperative planning and aggressive monitoring and maintenance.20,29
The different classifications by age, comorbidities, different definitions of patency, individual practice patterns, and different locations of AV placement contribute to the wide range of reported patency rates for AVFs and AVGs in the elderly (Table 1).
The comparison of patency rates in the elderly versus younger patients has provided inconsistent results. Indeed, recent studies report that age does not significantly alter the rates of primary and secondary patency.11,21,41,42 A retrospective study of 688 patients found that, among three age groups (<65, ⩾65–75, and ⩾75 years), those with ⩾75 years had no different chances of 1-, 3-, and 5-year primary and secondary patency. 21 Qian et al. 11 reported similar results in a large retrospective study with 43,851 hemodialysis patients assembled from the US Renal Data System. As compared with those aged 67 to <77 years, patients older than 77 years had comparable AVF primary (aHR 1.05 [95% CI 1.00–1.11]; p = 0.09) and secondary patency loss (aHR 1.06 [95% CI 0.94–1.2]; p = 0.4). Although these studies reported similar patency rates, some drawbacks were reported compared to younger groups, namely worst AVF maturation and higher rate of procedures to obtain or maintain patency.
Still, not all studies have reported similar primary and secondary patency rates in the elderly and younger patients. In a large retrospective study with 941 patients, Misskey et al. reported a lower cumulative primary and secondary patency rates (p = 0.006 and <0.002) among patients aged >80 years compared with those <65 years. On this study coronary disease, female sex, previous ipsilateral or bilateral catheters, radiocefalic configuration, and age >65 years were associated with secondary patency loss. 25
Several authors argue that the brachiocefalic AVF should be considered before radiocefalic AVF in HD access in elderly patients because of a longer intervention-free and thrombosis-free interval time. Indeed, several retrospective studies reported better primary patency rates in brachiocefalic AVF compared with radiocefalic AVF.3,23,43 Goh et al. 30 stated the importance of cephalic vein size used in the construction of the radiocephalic fistula and associated worst primary and secondary patency rates in elderly patients in whom the vein had a diameter of <2.5 mm. Misskey et al. 25 also reported shorter secondary patency in radiocefalic AVF in octogenarian patients compared with patients younger than 65 years (p < 0.013). In contrast, Olsha et al. 29 and Weale et al. 44 studies reported no statistical difference between radiocefalic and braquiocefalic AVF in patients older than 80 years. Thus, the decision of VA location should rely on careful patient evaluation prior to VA surgery.
Currently, autogenous arteriovenous fistulae are considered the gold standard in hemodialysis access for end-stage renal disease patients.8,14 AVFs are still preferred to AVGs because once they are successfully used for dialysis, AVFs have superior secondary patency, require less frequent interventions to maintain their patency, and incur fewer infections. Despite no significant differences in the primary and secondary patency between AVGs and AVFs, the reported that the time to catheter-free dialysis was longer for AVF than for AVG (p < 0.001), and the rate of assisted maturation was higher for AVF compared to AVG (31% vs 10%) in elderly patients. 27 Farrington and Lee 10 found that CVC dependence during the 6 months after surgery was longer in AVF compared with AVGs (p < 0.001). The maturation time could become a limitation in elderly patients especially if the life expectancy is short. Hall et al. evaluated cost-effectiveness of AVF placement after dialysis initiation in older adults ESRD aged ⩾65 years as a function of age and life expectancy. For patients with 85–89 years of age, in the lowest life expectancy quartile, AVF placement had the lower probability of cost-effectiveness than AVG placement and CVC use. 45
Still, some disadvantages have also been reported on the use of AVGs in elderly patients. Drouven et al. 3 reported that AVG had reduced primary (HR 1.64 [95% CI 1.25–2.16]; p < 0.001) and secondary patency rates (HR 1.61 [95% CI 1.00–2.56]; p < 0.05). Higher vascular access loss secondary to infection and thrombosis in AVGs were also reported in elderly patients. 36 Additionally, lower all-cause infection–related hospitalization rate (RR 0.93 [95% CI 0.87–0.99], p = 0.01) in AVFs compared to AVGs have also been reported. 46 Though, the higher rate of infections associated with AVGs might be lessened by the higher rate of infections associated with CVCs during the longer maturation time associated with AVFs.
Vascular access and mortality in elderly patients
A review of the literature reveals mortality rates of 40%–50% in ESRD patients after 3–5 years, in patients older than 75 years.21,23,30,47 In a retrospective study of 688 ESRD patients older than 75 years, the survival rate was of 44.5% at 5 years follow-up. 21 Most studies describe poor outcomes in terms of mortality and access-related infections with the use of CVC in elderly patients compared to AVF and AVG.37,48 –55
Arhuidese et al. 56 published a large retrospective study with 124,421 patients older 75 years and reported highest mortality rates in CVC group compared to AVF group (aHR 2.23; p < 0.001). Also, a study of 100,804 patients reported increasingly higher mortality risk in octogenarians with CVC only compared to those who had pre-emptive or converted to AVF or AVG. 58 Furthermore, starting HD with a CVC has been associated with higher mortality in older patients, compared to younger patients (HR 2.78 vs HR 1.18; p < 0.001). 59 The same results being reported in patients older than 90 years.53,60 Therefore, there appears to be a significant association between CVC at HD start and mortality even in older patients.
Several recent studies also suggest a survival benefit of AVF over AVGs in the elderly population.36,48,54 In a study of 529 patients older than 80 years, AVG was significantly associated with all-cause mortality when compared to AVF (HR 6.30 [95% CI 2.29–17.35]; p < 0.001). 61 Ko et al. 58 reported equally unfavorable results in octogenarians who initiated HD by a CVC, as those who converted to AVGs had higher mortality than those who converted to AVF (HR 1.14 [95% CI 1.01–1.27]). Whether mortality is directly associated with the vascular access or is influenced by patient characteristics which dictate the choice and placement of vascular access is not clear. Brown et al. 62 report that patient factors affecting AVF placement, might explain up to two-thirds of the mortality benefit observed in AVF patients in a cohort of 115,425 patients older than 67 years. This highlights the importance of careful patient assessment before vascular access creation.
To summarize the results: the risk of primary failure of distal AVFs is high, therefore proximal AVFs of AVGs should be the preferred VA; ultrasound mapping should be performed to identify and select forearm veins with at least 2.5 mm in diameter to improve maturation rates; AVFs have the higher patency rates and require less interventions to assist maturation while AVGs have shorter catheter dependence time; there is a significant association between CVC at HD start and mortality in elderly patients although mortality is not directly associated with the CVC but most likely results from patient factors.
Limitations and strengths
In the last two decades, numerous studies were performed concerning the selection of the optimal vascular access in elderly patients undergoing HD. The analysis of outcomes was limited by the lack of randomized trials, lack of standardized definitions of elderly, and lack of standardized definitions of patency. As such, analysis of data was mainly based on multiple retrospective observational studies, with different classifications by age and different locations of AV placement with some conflicting results which is why no consensus has been achieved on preferred vascular access and location.
Nonetheless, this review provides a comprehensive analysis on maturation rates, primary failure, patency, and mortality regarding vascular access in elderly patients which we defined as patients older than 75 years of age, in whom decision-making might be more challenging given the higher level of frailty, higher number of comorbidities and lower life expectancy.
Future research areas
There is an urgent need to identify patients with a higher chance of VA maturation and higher patency. The high number of comorbidities and frailty of the elderly represent a challenge for decision making related to vascular access management, since the beneficial aspects of AVF or AVG placement may never be achieved. This is particularly relevant in the first year of dialysis where mortality is higher (30%–50%) in elderly patients. 63 The prediction of patients with higher risk of mortality within the first months or first year would be useful in determining which patients would benefit from AVF or AVG placement.
The use of percutaneous techniques to create AVFs have been performed in elderly patients with excellent patency rates. These AVFs are created at the elbow using proximal radial/ulnar artery as the inflow which improves maturation rates and reduces hand ischemia and heart failure risk. Most likely, these procedures will gain popularity in following years, and the results in this specific population are highly anticipated. 64
Attention should be paid to the selection of an appropriate vascular access, such as AVF versus AVG, or even CVC maintenance in patients with limited life expectancy and/or with high number of comorbidities or frailty, the number of interventions associated with access patency, and length of time for successful HD. 65
Additionally, identifying individual patient preferences and its impact on quality of life should also be taken into account in this population. Interestingly, a survey of 10 patients reported that most patients preferred a CVC rather than AVF or AVG due to interventions associated with AV access failure and dislike of needles, even if associated with mortality. 66 Another survey reported that patients were minimally engaged in decisions regarding VA creation. 67 Indeed, little emphasis has been given to patients’ will to pursue an AV creation, although it is known that repetitive interventions lead to less quality of life. 66 Caregivers should consider a patient-centered approach to VA creation and should engage patients in the decisions. The patient-centered approach aims to select the right VA for the right patient at the right time. This should integrate patients’ preferences, the likelihood of AVF maturation, prior AV creation and estimated life expectancy. 68
Conclusion
Age should not be the sole determinant on the choice of vascular access. Given that CVCs are consistently associated with higher mortality rates, older patients should be considered for arteriovenous access placement. Proximal AVFs are the most appropriate VA in elderly patients with less comorbidities and longer life expectancy. Also, ultrasound vascular mapping can provide useful information for VA placement with higher maturation rates. In patients with higher risk for AVF primary failure, AVGs are a reasonable first-line choice for VA with greater primary success and reduced catheter times. Nonetheless, CVCs may be a viable option for patients with higher frailty scores and minimal life expectancy as to improve quality of life.
Vascular access planning in elderly patients should take into account comorbidities, functional status, vascular ultrasound mapping, maturation time, costs and life expectancy.
Footnotes
Author contributions
TY drafted the manuscript, JG made substantial contributions to the study concept and was involved in drafting the manuscript and critical revised it before submission, JG contributed to the literature research, RF and ER were involved in revising the manuscript critically for intellectual content.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.