Abstract
Introduction:
Cannulation is an essential part of haemodialysis with arteriovenous access. Patients’ experiences of cannulation for haemodialysis are problematic but poorly understood. This review aims to synthesise findings related to patients’ experiences of cannulation for haemodialysis from qualitative studies, providing a fuller description of this phenomenon.
Methods:
Eligibility criteria defined the inclusion of studies with a population of patients with end-stage kidney disease on haemodialysis. The phenomena of interest was findings related to patients’ experiences of cannulation for haemodialysis and the context was both in-centre and home haemodialysis. MedLine, CINAHL, EMBASE, EMCARE, BNI, PsycInfo and PubMed were last searched between 20/05/2019 and 23/05/2019. The quality of studies was assessed using the using Joanna Briggs Critical Appraisal Checklist for Qualitative Research. Meta-aggregation was used to synthesise findings and CERQual to assess the strength of accumulated findings.
Results:
This review included 26 studies. The subject of included studies covered cannulation, pain, experiences of vascular access, experiences of haemodialysis and a research priority setting exercise. From these studies, three themes were meta-aggregated: (1) Cannulation for haemodialysis is an unpleasant, abnormal and unique procedure associated with pain, abnormal appearance, vulnerability and dependency. (2) The necessity of cannulation for haemodialysis emphasises the unpleasantness of the procedure. Success had multiple meanings for patients and patients worry about whether the needle insertion will be successful. (3) Patients survive unpleasant, necessary and repetitive cannulation by learning to tolerate cannulation and exerting control over the procedure. Feeling safe can help them tolerate cannulation better and the cannulator can invoke feeling safe. However, some patients still avoid cannulation, due to its unpleasantness.
Conclusions:
Cannulation is a pervasive procedure that impacts on patients’ experiences of haemodialysis. This review illuminates further patients’ experiences of cannulation for haemodialysis, indicating how improvements can be made to cannulation.
Registration:
PROSPERO (CRD42019134583).
Introduction
Haemodialysis is a life-sustaining treatment for patients with end-stage kidney disease. An essential part of haemodialysis and a continuing challenge, is providing adequate vascular access (VA). 1 Recommendations about the type of VA used for haemodialysis are becoming more nuanced, promoting inclusion of patient choice and likelihood of success as considerations in this decision. 2 However, arteriovenous (AV) access continues to be recommended as the best option for the majority of haemodialysis patients.1–3 AV access continues to be associated with reduced mortality and better patency than central venous catheters (CVC) 4 and better patient experience.5,6 Thus, efforts are still needed to reduce barriers to AV access use, optimising outcomes and patients’ experiences, promoting AV access as a viable choice.
AV access for haemodialysis requires insertion of two needles at the start of each treatment, also known as cannulation. This is needed for each treatment, meaning thrice weekly haemodialysis requires 312 cannulations a year. Despite its frequency, cannulation for haemodialysis remains difficult for patients to tolerate. It is associated with pain, anxiety, vulnerability, fear and worry.7–10 In the UK, an annual survey of renal patients repeatedly identifies cannulation as the third poorest scoring area for patient experience.11–13 Fear of cannulation of AV access can also lead to patients avoiding AV access for haemodialysis, choosing to use a CVC.14,15 Therefore, an in-depth understanding of patients’ experiences of cannulation is valuable to guide recommendations for improvements.
Several reviews illuminate patients’ experiences of cannulation for haemodialysis. A systematic review of patients’ experiences of VA highlights fear of cannulation. However, as this focusses on broader VA experience, it does not explore cannulation in depth. 7 A scoping review of qualitative and quantitative studies identifies common problems with cannulation including pain, inability to cannulate, clinical complications and fear. 16 However, this does not provide detailed description or synthesis of findings. Four individual qualitative studies examine patients’ experiences of cannulation for haemodialysis in sub-populations8,17 or parts of cannulation,9,18 but provide no full description of this phenomenon. Therefore, we aimed to explore patients’ experiences of cannulation of AV access for haemodialysis.
Methods
Study design
We decided to explore this phenomenon using a qualitative systematic review. A synthesis of qualitative studies that explore experiences of cannulation, VA and haemodialysis would enable findings from different studies to be drawn together, providing a fuller, in-depth description of patients’ experiences of cannulation for haemodialysis, increasing understanding and focusing guidance on how to improve cannulation for haemodialysis. The protocol was developed using PRISMA-P 19 and ENTREQ, 20 and registered on PROSPERO (CRD42019134583) prior to starting the review.
Review question
The review question was developed using the P (population), I (phenomena of Interest), Co (Context) formation for qualitative systematic reviews 21 :
‘What are adults with end-stage kidney disease undergoing haemodialysis (P), experiences of cannulation of AV access (I), when undergoing haemodialysis in both in-centre and home settings (Co)?’
Studies were included if they generated findings directly related to the phenomenon, even if this was not the study focus. Inclusion and exclusion criteria (Table 1) maintained focus on everyday cannulation for haemodialysis, rather than less usual cannulation procedures which may generate unique findings. Non-English articles were translated for data extraction.
Inclusion and exclusion criteria for studies.

Data extraction
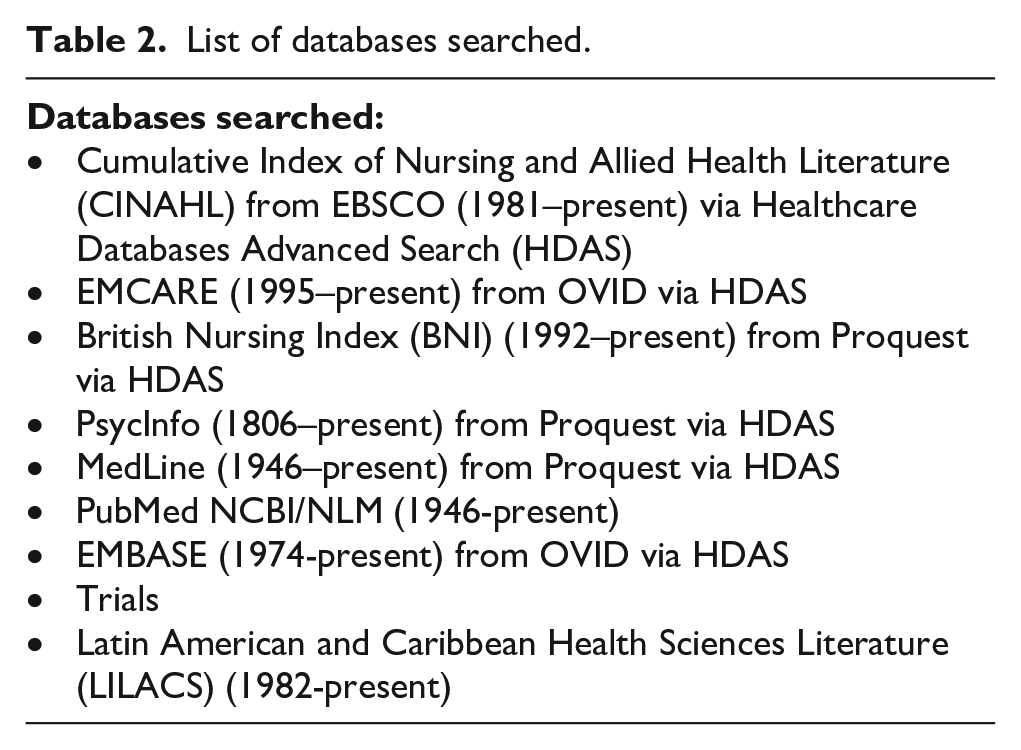
The search strategy was developed using the PICo, with examination of keywords used in 15 relevant articles, to prompt search terms (Supplemental Material 1). Databases were searched between 20/05/2019 and 23/05/2019 (Table 2, Supplemental Material 2), against pre-set criteria. Reference lists of included articles and articles with a systematic literature search were searched for further sources, ensuring a comprehensive search of qualitative research which can be difficult to identify.20,21 A bespoke data extraction form was designed and piloted. Following the pilot, minor changes were made. Data extracted from each study included the study population, the type of cannulation used, methods used, conclusions and limitations. Any findings related to cannulation for haemodialysis were extracted, including verbatim quotes from the study article describing the finding and related participant quotes. The final data extraction form is available in Supplemental Material 3. No studies were excluded due to their quality, though quality was assessed using Joanna Briggs Critical Appraisal Checklist for Qualitative Research. 22 Screening of articles, data extraction and assessment of quality of articles were completed by two authors independently. Disagreement between co-authors was discussed and, when required, adjudicated by a third author.
List of databases searched.
Synthesis of findings
Meta-aggregation was used to synthesise findings. 23 Meta-aggregation enables a broad exploration of a topic, with a complete search strategy. 23 It provides a comprehensive base to explore a poorly understood topic. The meta-aggregation of findings was implemented through a number of stages:
(1) Each extracted finding was given an inductive category to describe what this finding illuminated about the phenomenon. Where appropriate, different findings were allocated into the same category.
(2) All findings and categories were shared and discussed at a group co-author meeting, where all co-authors were present. During this discussion, co-authors were able to add their own interpretation of findings, which was then discussed. This led to changes in categories and how they were described.
(3) Together, two co-authors (CF and HB) assimilated categories into synthesised findings, which are described as themes and sub-themes. This assimilation was regularly reviewed in meetings together.
(4) Once both co-authors agreed the themes and sub-themes, these were circulated to all other co-authors for comments, with minor adjustments made.
(5) CF and HB discussed the final themes and sub-themes, identifying the relationship between them. A diagram was produced to describe this, which was reviewed and agreed by all co-authors.
The final analysis became more interpretative than is traditionally produced by meta-aggregation. 23 However, this level of interpretation became necessary due the diversity and breadth of findings across studies, that were shaped by heterogeneous research questions. Once the analysis was complete, a CERQual assessment of accumulated findings 24 was completed by two co-authors.
To maintain trustworthiness, the primary author (who spent 20 years working as a haemodialysis nurse regularly performing cannulation) maintained a diary throughout to promote reflexivity. 25 As described by Fischer, 25 the primary author did not completely bracket her previous experience of the phenomenon, but used the reflexive diary to recognise her assumptions that could bias the analysis. Throughout the study, these assumptions were openly discussed with co-authors to minimise any inappropriate influence. However, her experience was used to form the categories, themes and sub-themes, whilst ensuring these remained focused on the extracted findings from studies.
Results
The results of the screening process are summarised in the PRISMA flow diagram (Figure 1). During full text screening, one potential inclusion (a dissertation in Portuguese) was excluded due to excessive translation costs. However, the study in this dissertation was included through a published article. 18
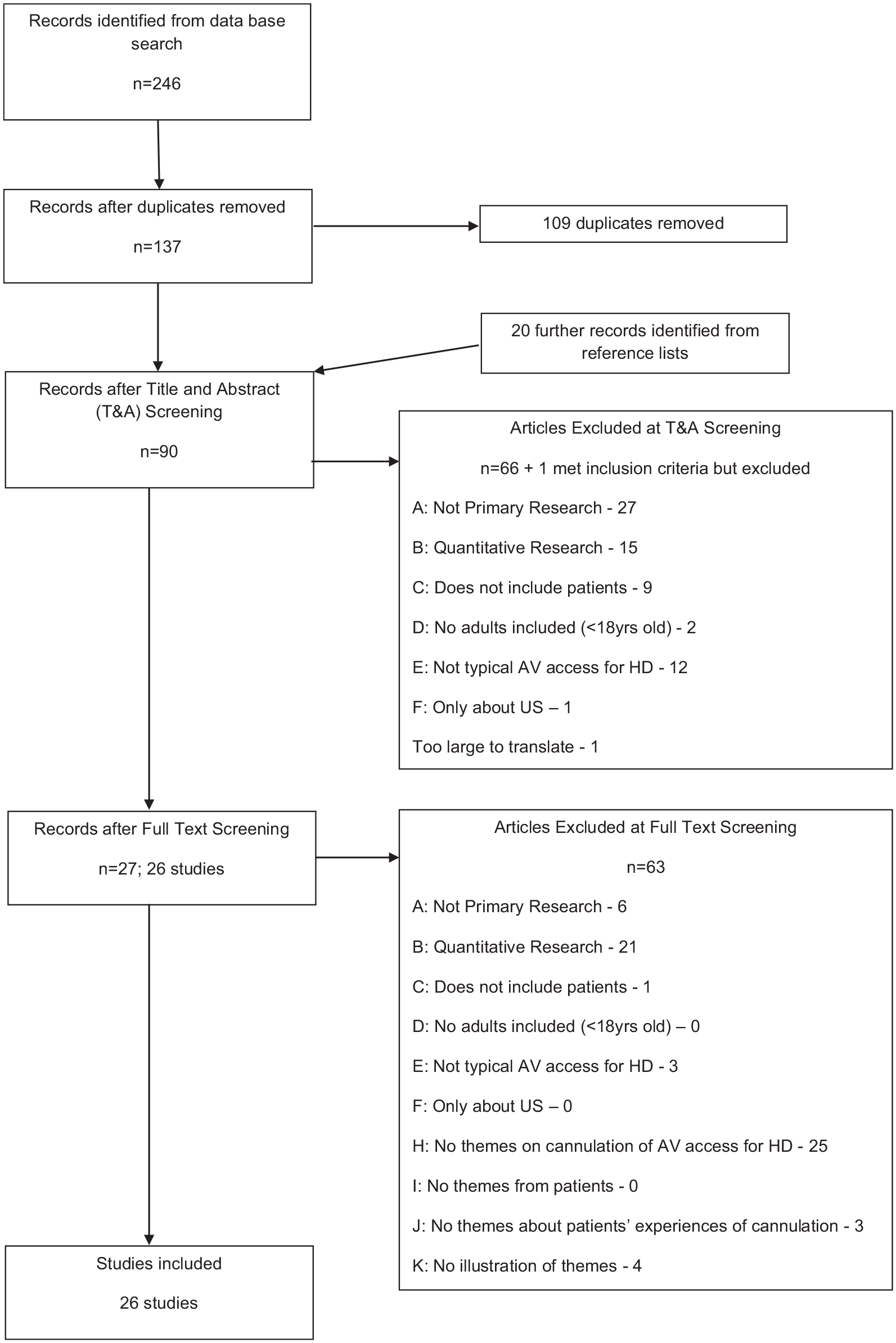
PRISMA flow Diagram.
Table 3 provides a description of the included studies. Only four studies were directly about cannulation.8,9,17,18 Other studies were about pain,26,27 experiences of VA for haemodialysis,14,28–33 experiences of in-centre and home haemodialysis34–46 and research priority setting. 47 Studies were conducted across five continents, but despite this diversity in study location themes extracted did not seem to vary due to culture, with the exception of one study, which developed themes linked to religion in a Thai culture. 27
Description of included studies.
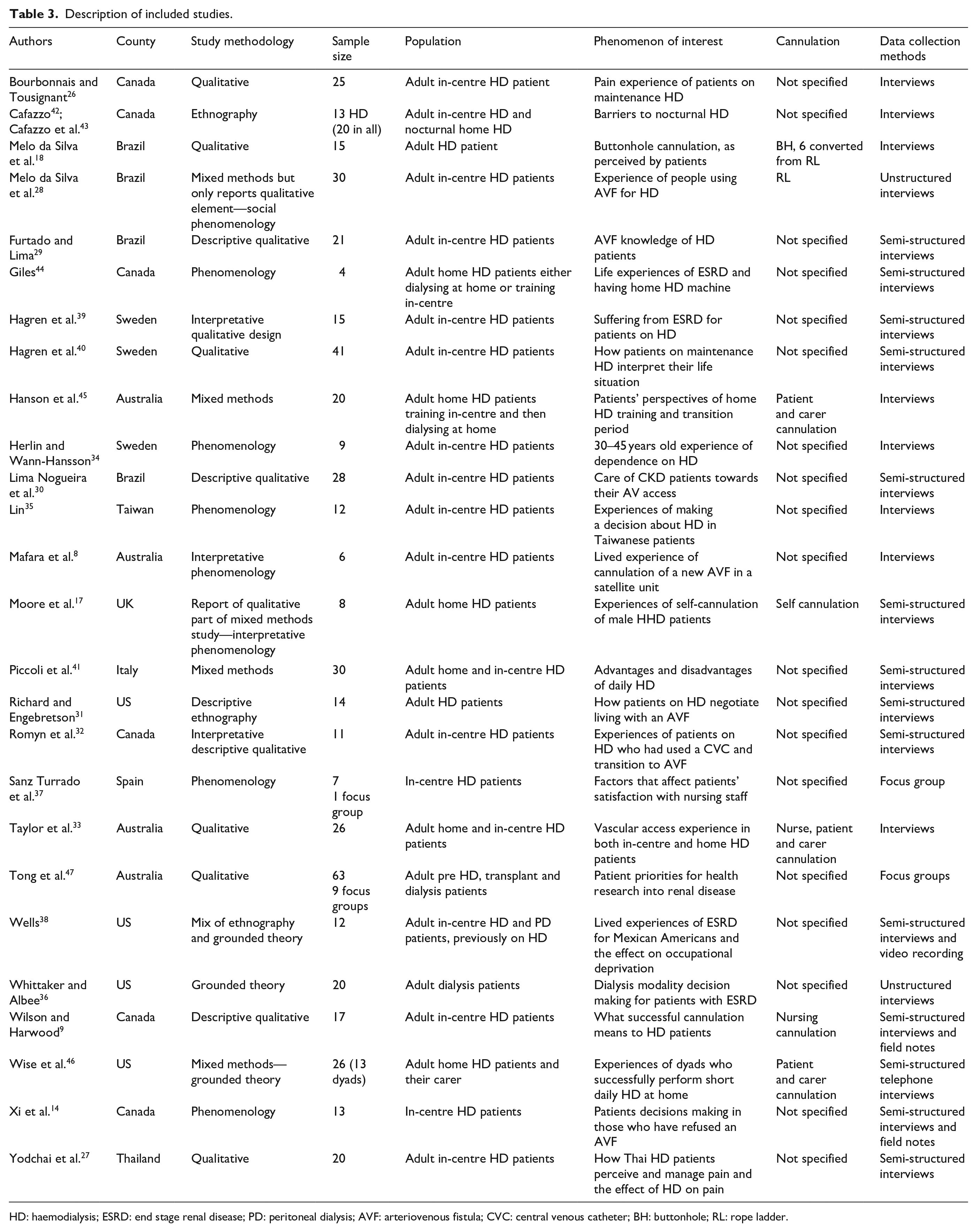
HD: haemodialysis; ESRD: end stage renal disease; PD: peritoneal dialysis; AVF: arteriovenous fistula; CVC: central venous catheter; BH: buttonhole; RL: rope ladder.
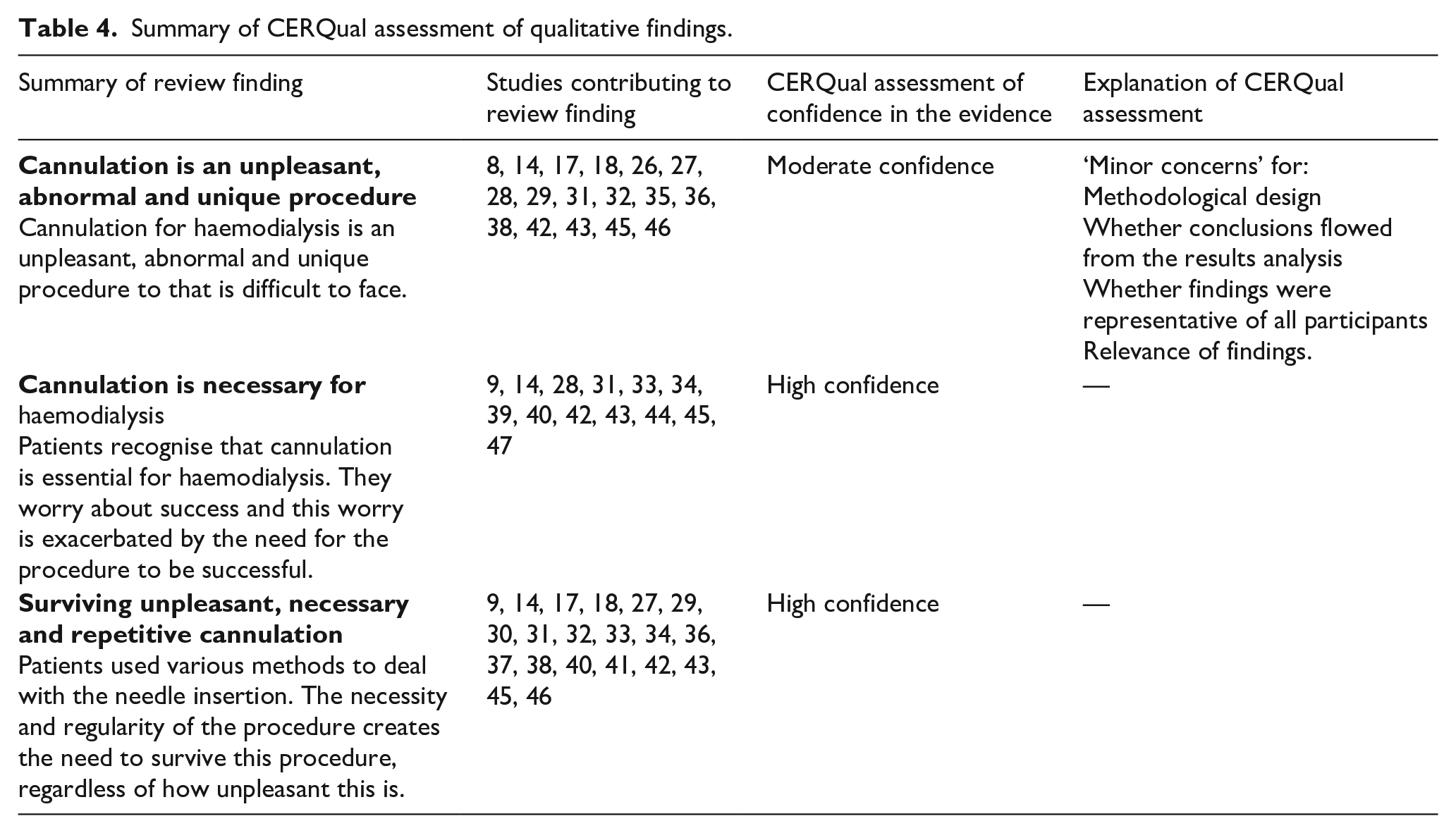
The quality of studies varied (Supplemental Material 4). Most studies displayed congruity between the research methodology and the research question (present in 25/26 studies), methods used to collect data (24/26), data analysis (20/26) and interpretation of results (20/26). The most frequent limitations identified were a lack of: a stated philosophical perspective (absent in 16/26), statement locating the researcher (22/26) and the influence of the researcher on the research (22/26). This may be due to journal requirements rather than being absent in the study itself. The results of the CERQual assessment are shown in Table 4. The remainder of the results describes the synthesis of extracted findings from studies that describe patients’ experiences of cannulation for haemodialysis.
Summary of CERQual assessment of qualitative findings.
Patients’ experiences of cannulation
We identified 3 themes and 10 sub-themes to describe patients’ experiences of cannulation for haemodialysis (Figure 2). Each theme interacts with the others, influencing and altering the impact of each. Therefore, cannulation experience is one holistic entity, with three overlapping and influencing themes. Cannulation is part of the haemodialysis process and as such difficult to separate from this, thus happens within this wider context. Key quotes extracted from studies, to illustrate each theme and sub-theme, are indicated by italics within the text, with detailed quotes provided in Supplemental Material 5.
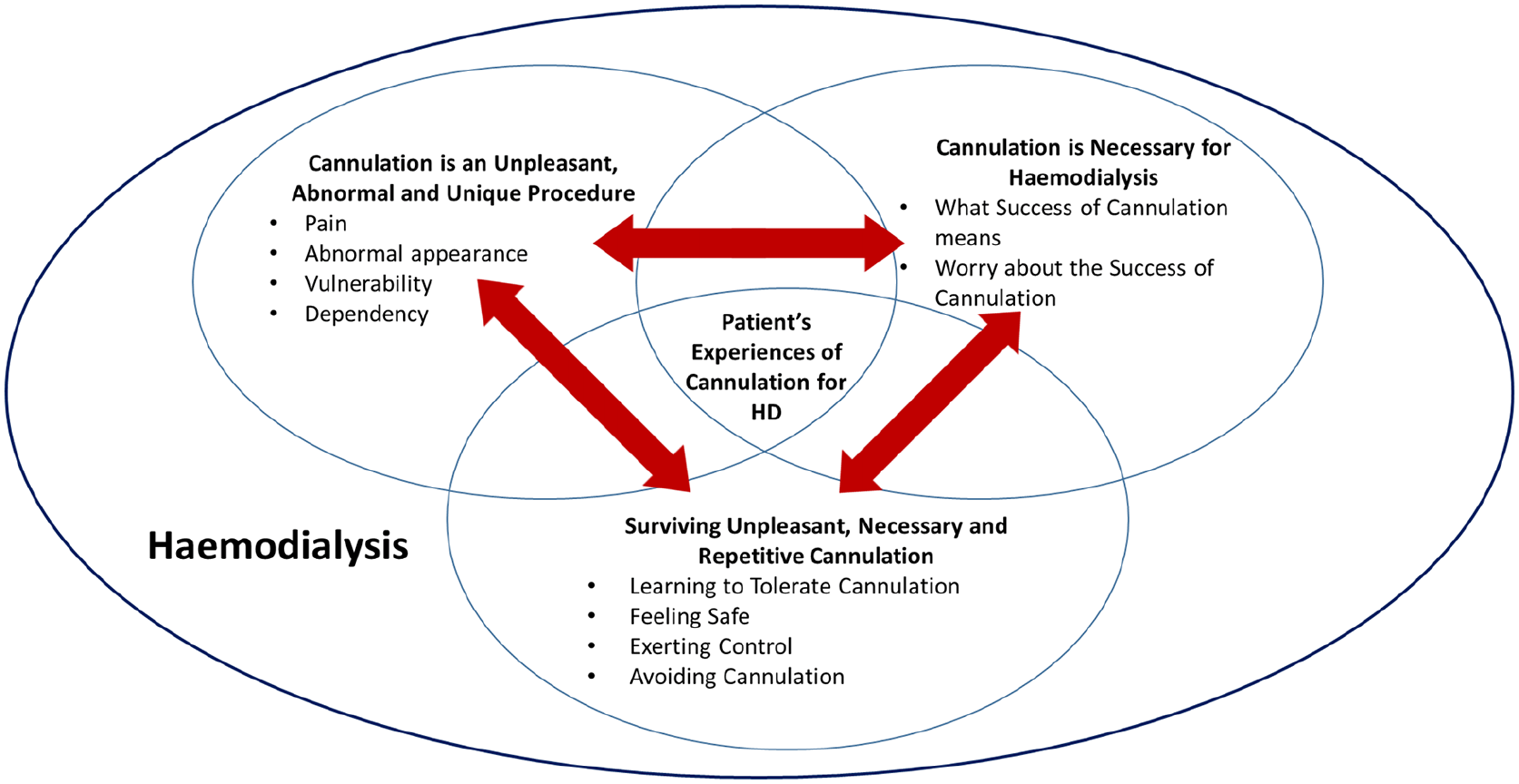
Patients’ experiences of cannulation for haemodialysis.
Theme 1: Cannulation is an unpleasant, abnormal and unique procedure
Cannulation creates unpleasant feelings and is not a normal procedure for patients to experience regularly: ‘Cannulation is not normal, sticking a needle in. But my life depends on it. . . . Every time I get the needle ready I hear the music from Jaws’. 45 Cannulation for haemodialysis is associated with pain, concern about the abnormal appearance of the arteriovenous access, vulnerability and dependency. The context of regular haemodialysis makes this a unique procedure that is not similar to other one-off cannulation events.
Patients also worried about the
The cannulation procedure itself induced feelings of
Some patients felt the cannulation procedure created
Theme 2: Cannulation is necessary for haemodialysis
Patients recognised that cannulation is essential for haemodialysis: ‘I come here to live. That’s the short story. So whatever happens to me, thinking I am not going to like those needles put in, that is a fact’. 9 The cannulation and arteriovenous access ‘keeps me alive. If it wasn’t for it, I wouldn’t be here’. . . 28 This link with a life-sustaining treatment changes what success means and leads to worry about whether it will be successful.
Due to its link with haemodialysis, a life-sustaining procedure, patients
Theme 3: Surviving unpleasant necessary and repetitive cannulation
The necessity and regularity of cannulation created a need to survive the procedure regardless of its unpleasantness: ‘. . .I was very scared the first time, but now I can take it [needle insertion]’. 27 This theme illuminates how patients manage this unpleasant procedure not just once, but on a frequent and regular basis.
Patients often
Some patients
Finally, not all patients were able to cope with the unpleasantness of cannulation, leading to some
Discussion
This review aims to explore patients’ experiences of cannulation for haemodialysis, developing an in-depth description of this experience. Synthesising findings from multiple studies broadens what we already know from current studies into one cohesive description. Using qualitative findings to do this, maintains the focus on what patients’ feel and experience, rather than imposing healthcare professionals’ assumptions and preconceptions. If we can develop greater understanding of this phenomenon, this will focus improvements in cannulation.
Our findings start to illuminate how patients feel about cannulation for haemodialysis. It is an unpleasant, abnormal and unique procedure that is difficult to face. However, despite its unpleasantness, the necessity of successful cannulation for haemodialysis introduces extra emphasis on the procedure, creating worry about the success of the cannulation and whether multiple needle attempts will be needed. This necessity also drives a need to survive this unpleasant, repetitive procedure. Patients learn to tolerate the needle insertion and attempt to exert control over the procedure as a means to survive this. Feeling safe makes the cannulation easier to tolerate. Despite this, the procedure often remains unpleasant. Which can lead to patients avoiding needle insertions. Whilst we previously knew that cannulation was associated with challenges, this aggregation of findings starts to fully describe the trauma cannulation causes to patients, how the link to a life sustaining treatment exacerbates this and how patients survive this unpleasant procedure on a regular basis.
Our analysis has identified that cannulation is an inherent part of haemodialysis and VA use. The issue of cannulation is not only evident in studies that specifically explore cannulation, but is also highlighted in studies that explore experiences of VA14,28–33 and haemodialysis.34–46 Casey et al’s 7 systematic review identified ‘fear of cannulation’ as part of patients’ experiences of VA for haemodialysis and a key area of concern. Whilst studies have found there was better patient satisfaction with AV fistulae in comparison to AV grafts and CVCs, patients with AV access were more likely to be bothered by symptoms associated with cannulation, namely the appearance of their access, pain, bruising and swelling.5,6 Since completion of our systematic review, Kuo et al. 48 have completed a qualitative study exploring what patients believe to be a ‘bad run’ for haemodialysis. Again, cannulation was highlighted as one of four main issues for haemodialysis patients, alongside cramps, ‘crashing’ and clotting. The consistency with which cannulation is highlighted in studies examining haemodialysis and VA experience indicates the pervasive nature of this issue.
The necessity of cannulation and its link to receiving a life-sustaining treatment appears to have a significant impact on patients, causing them to have a heavy burden of worry about whether cannulation will be successful. Despite its importance to patients, miscannulation continues to occur frequently49–51 and is often accepted as a part of haemodialysis. Whilst preventing miscannulation is the optimal solution, it is unlikely that it can be avoided completely. Therefore, better strategies are also needed to support patients through miscannulation.
Whilst patients may learn to survive unpleasant, necessary and repetitive cannulation for haemodialysis, this does not necessarily mean cannulation improves but that they learn to tolerate cannulation out of necessity for survival. Feeling safe can make cannulation easier to tolerate, with the cannulator, environment and cannulation technique influencing this. Whilst there is broad acceptance that cannulation varies with different cannulators, there is a paucity of studies exploring how we can reduce this variation and promote ‘good’ cannulators. Harwood et al. 52 conducted a qualitative study with nurses, to identify what led to successful cannulation. They found this went beyond just technical skill, including patient-centred care, teamwork and self-awareness of the cannulator. Our review reflects this, where the attitude and communication of the cannulator can improve or adversely affect the patients’ experiences. Training of cannulators is one area where canulation can be improved, 7 however consideration needs to be given not just to technical skill but also the social interaction during cannulation. The environment also plays a part in patients feeling safe, which was a theme in Wilson and Harwood 9 study. This identified that a calm, relaxed environment improved patients’ experiences of cannulation, whereas a chaotic environment had the opposite effect. Haemodialysis units are often busy, with adherence to schedules often leading to a pressured work environment. Cannulators, but also managers who influence nursing schedules and workloads, should aspire to create a calm haemodialysis unit that makes patients feel safe to undergo cannulation and survive its unpleasantness. The cannulation technique used also appears to affect whether patients feel safe. This was particularly evident in one included study that explored buttonhole cannulation, where patients appeared to felt safer with this technique. 18 However, there were no studies exploring any other cannulation techniques. Therefore, it is difficult to determine whether buttonhole technique leads to a better cannulation experience. Quantitative studies have compared buttonhole to other cannulation techniques, using pain scores to measure patients’ experiences of cannulation. A meta-analysis found that whilst observational studies indicated a significant reduction in pain with buttonhole cannulation, this was not replicated in randomised controlled trials. 53 Whilst there are no firm conclusions about how pain is affected by cannulation techniques, our review demonstrates that pain does not solely describe patients’ experiences of cannulation, with many other factors influencing this. Therefore, further research is needed into how cannulation techniques influence patients’ experiences of cannulation, including pain but also measuring other aspects of patients’ experiences.
Control also appeared to improve patients’ experiences of cannulation. Four studies included in our review specifically explored home haemodialysis,42–46 generating themes around self-cannulation, with two further studies exploring self-cannulation.17,33 Whilst it is tempting to believe that self-cannulation will improve cannulation experience for many patients and should be promoted, our review indicates that self-cannulation is also difficult to achieve. It is unlikely to be a viable solution for all haemodialysis patients. However, control during cannulation is also evident in non-self-cannulation. 31 Controlling who cannulates you or where they cannulate could be a form of gaining control over the procedure. Whilst it is good to promote self-cannulation, when it is not possible, we need to think beyond self-cannulation, considering how the dynamic between the cannulator and canulatee can promote the patient feeling in control.
A strength of our review is that we have included articles in any language, encompassing a breadth of cultural backgrounds. As with all systematic reviews, the strength of findings is limited by the quality of studies included. We did not exclude any studies due to quality, to enable exploration of the breadth of findings available. This means we have included studies of varying quality. However, the CERQual assessment (Table 4) indicates high confidence in our findings, with moderate confidence in the first theme, ‘Cannulation is an unpleasant, abnormal and unique procedure’. The moderate confidence in the first theme indicates a lack of richness in understanding of the unpleasantness of cannulation. Throughout studies, there appears to be an assumption that everyone knows this unpleasantness exists, limiting the depth with which it is explored. Further research needs to really explore how canulation is unpleasant for patients and what this means to them.
In conclusion, this systematic review illuminates patients’ experiences of cannulation for haemodialysis. The synthesis of qualitative findings provides a richness and depth of understanding of this phenomenon, which would not be possible to achieve through an examination of quantitative studies. Canulation is a pervasive procedure that impacts on patients’ experiences of haemodialysis. The unpleasantness of the cannulation procedure for haemodialysis patients is evident and includes issues related to pain, abnormal appearance, vulnerability and dependency. However, we still need further understanding of this unpleasantness. The necessity of cannulation for haemodialysis emphasises the unpleasantness of the procedure, leading to worry about whether it will be successful. Worry about unsuccessful cannulation is an issue for patients, but the frequency of this event means there needs to be exploration of how we minimise this but also how we support patients through this event. Patients learn to survive repetitive cannulation, where feeling safe and in control can improve their experiences. This indicates cannulation is not just a technical skill, but also a social process. Cannulators and haemodialysis environments need to make patients feel safe and in control. Cannulation techniques may also influence these aspects, but further research is needed to determine how. Whilst this review has helped further develop our understanding about patients’ experiences of cannulation for haemodialysis, there is still much to understand about this phenomenon, to continue to improve this for haemodialysis patients.
Supplemental Material
sj-pdf-1-jva-10.1177_10.1177_11297298211067630 – Supplemental material for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review
Supplemental material, sj-pdf-1-jva-10.1177_10.1177_11297298211067630 for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review by Catherine Fielding, Louise Bramley, Carol Stalker, Sarah Brand, Suzanne Toft and Heather Buchanan in The Journal of Vascular Access
Supplemental Material
sj-pdf-2-jva-10.1177_10.1177_11297298211067630 – Supplemental material for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review
Supplemental material, sj-pdf-2-jva-10.1177_10.1177_11297298211067630 for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review by Catherine Fielding, Louise Bramley, Carol Stalker, Sarah Brand, Suzanne Toft and Heather Buchanan in The Journal of Vascular Access
Supplemental Material
sj-pdf-3-jva-10.1177_10.1177_11297298211067630 – Supplemental material for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review
Supplemental material, sj-pdf-3-jva-10.1177_10.1177_11297298211067630 for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review by Catherine Fielding, Louise Bramley, Carol Stalker, Sarah Brand, Suzanne Toft and Heather Buchanan in The Journal of Vascular Access
Supplemental Material
sj-pdf-4-jva-10.1177_10.1177_11297298211067630 – Supplemental material for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review
Supplemental material, sj-pdf-4-jva-10.1177_10.1177_11297298211067630 for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review by Catherine Fielding, Louise Bramley, Carol Stalker, Sarah Brand, Suzanne Toft and Heather Buchanan in The Journal of Vascular Access
Supplemental Material
sj-pdf-5-jva-10.1177_10.1177_11297298211067630 – Supplemental material for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review
Supplemental material, sj-pdf-5-jva-10.1177_10.1177_11297298211067630 for Patients’ experiences of cannulation of arteriovenous access for haemodialysis: A qualitative systematic review by Catherine Fielding, Louise Bramley, Carol Stalker, Sarah Brand, Suzanne Toft and Heather Buchanan in The Journal of Vascular Access
Footnotes
Acknowledgements
We would like to acknowledge Professor Nicholas Selby, Professor Paula Ormandy and Professor Maarten Taal for their mentorship of the lead author throughout completion of this study, on occasions providing advice that affected the content and conduct of this systematic review. Thank you to the NIHR who have funded Catherine Fielding (ICA-CDRF-2018-04-5T2-003), Louise Bramley and Sarah Brand during this project.
Author contributions
All authors have contributed to the systematic review and manuscript as follows:
• Catherine Fielding: Development of the protocol, literature search, screening of articles, data extraction, assessment of quality of articles, data synthesis, CERQual assessment, drafting of manuscript.
• Dr. Louise Bramley: Development of the protocol, data extraction, assessment of quality of articles, data synthesis, review of manuscript.
• Dr. Carol Stalker: Development of the protocol, data extraction, assessment of quality of articles, data synthesis, review of manuscript.
• Dr. Sarah Brand: Development of the protocol, data extraction, assessment of quality of articles, data synthesis, review of manuscript.
• Suzanne Toft: Development of the protocol, literature search, screening of articles, review of manuscript.
• Dr. Heather Buchanan: Development of the protocol, screening of articles, data extraction, assessment of quality of articles, data synthesis, CERQual assessment, drafting of manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval is not required as this is a systematic review.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Catherine Fielding, Clinical Doctoral Research Fellow (ICA-CDRF-2018-04-5T2-003) is funded by Health Education England (HEE)/National Institute for Health Research (NIHR) for this research project. The views expressed in this publication are those of the author(s) and not necessarily those of the NIHR, NHS or the UK Department of Health and Social Care. Dr. Louise Bramley and Dr. Sarah Brand are both National Institute for Health Research (NIHR) Senior Nurse and Midwife Research Leaders. The views expressed in this article are those of the author(s) and not necessarily those of the NIHR, or the Department of Health and Social Care.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
