Abstract
Purpose
We aimed to evaluate conjunctival impression cytology (CIC) findings, tear parameters, and ocular surface in early-stage Parkinson's patients and compare the results with the control group.
Methods
This cross-sectional comparative study included 49 early-stage Parkinson's Disease (PD) patients and 45 healthy individuals as a control group. Clinical staging of Parkinson's patients was performed according to the Hoehn-Yahr Scale. Those with stages 1 and 2 were defined as early-stage PD. Ocular surface disease index (OSDI) questionnaire, tear breakup time (TBUT), Schirmer test, and CIC were applied to the patient and control groups.
Results
There was no significant difference between the two groups in terms of mean age and gender (p = 0.606, p = 0.357, respectively). Schirmer test and TBUT results in the PD group were significantly lower compared to the control group (p < 0.001, p < 0.001). Meanwhile, the OSDI score and CIC stage of the PD group were significantly higher than that of the control group (p < 0.001, p < 0.001).
Conclusions
In early-stage PD, decreased TBUT and Schirmer test values, conjunctival goblet cell loss, and squamous metaplasia development indicate that the ocular surface is affected. Early diagnosis of dry eye in Parkinson's patients is important for preventing complications such as ocular surface damage and visual disturbances.
Introductıon
Parkinson's disease (PD) is an idiopathic neurodegenerative disorder of the nervous system, characterized by tremor and bradykinesia. It is a slowly progressive, chronic disease that typically begins between the ages of 50 and 60 but can also occur in younger patients. 1 The primary pathological mechanism underlying PD is the loss of melanin-containing dopaminergic neurons in the pars compacta of the substantia nigra (SNpc), followed by depigmentation of the SNpc and the formation of Lewy bodies (LB). Symptoms of PD typically manifest when 60–70% of dopaminergic neurons in the SNpc are lost. 2 PD is characterized by motor and non-motor symptoms, with visual impairment being one of the most common non-motor symptoms. 3 Ocular changes observed in PD patients include deterioration in visual functions, visual hallucinations, a decrease in spontaneous blinking, alterations in eyelid movements such as blepharospasm, and abnormal eye movements. In Parkinson's patients, ocular surface disorders, especially dry eye, are commonly seen. 4
Dry eye disease (DED) is a multifactorial disease of the ocular surface, characterized by the loss of homeostasis of the tear film, accompanied by ocular symptoms in which tear film hyperosmolarity, ocular surface inflammation, damage, and neurosensory abnormalities are involved. As a result of ocular surface inflammation, there is a loss of epithelial and goblet cells, and squamous metaplasia develops in epithelial cells. 5
Conjunctival impression cytology (CIC) is based on the principle of taking epithelial samples by sticking cellulose acetate filter paper to the conjunctival surface to examine the structural organization of the conjunctival epithelial cells. Cells taken from the superficial layers of the epithelium are examined with the light microscope. CIC is used in the diagnosis of many disorders on the ocular surface as it can help with characterization of cell morphology of the conjunctival epithelium, nucleus/cytoplasm ratio, and goblet cell density. 6
Many studies have been conducted analyzing the ocular surface and DED in PD.7,8 However, no study in the literature has examined ocular surface changes using CIC in Parkinson's patients. The aim of our study was to assess ocular surface changes through tear breakup time (TBUT), the Schirmer test, the Ocular Surface Disease Index (OSDI) questionnaire, and CIC in early-stage PD, and to compare the results with those of the healthy control group.
Methods
The study was designed as a cross-sectional clinical study. Patients with early-stage PD who were under follow-up at the Neurology Clinic of Necmettin Erbakan University Faculty of Medicine Hospital between October 2022 and October 2023 and met the inclusion criteria were included in the study. A study group was formed with the right eyes of 49 PD patients. According to the Hoehn-Yahr Scale, 9 26 of the PD patients were stage 1, and 23 were stage 2. Patients were excluded from the study if they had systemic disorders such as connective tissue diseases, autoimmune diseases, or diabetes, apart from early-stage (stage 1–2) PD and hypertension. Patients with ocular pathologies, such as conjunctivitis, keratitis, eyelid disorders, or ocular surface disorders; those with a history of contact lens use; those with a history of intraocular or periocular surgery, including refractive or eyelid surgery; smokers and alcohol consumers; and those using any topical ocular medication, including artificial tears and cyclosporine eye drops, were excluded from the study. The control group consisted of the right eyes of 45 age- and gender-matched healthy subjects who visited the Eye Clinic of Necmettin Erbakan University Faculty of Medicine Hospital for routine eye examinations and met the inclusion criteria. The study was conducted in accordance with the principles of the Declaration of Helsinki and was approved by the Necmettin Erbakan University Ethics Committee (Ethics Committee Decision No: 2022/4022).
All participants included in the study underwent a detailed eye examination, including best-corrected visual acuity measurement, biomicroscopic anterior segment examination, fundus examination, and intraocular pressure measurement. After the initial assessment, tear breakup time (TBUT) was measured first, followed by the Schirmer test 30 min later. Conjunctival impression cytology (CIC) samples were collected on the following day.
In the OSDI survey, five questions were asked in the first part, four in the second part, and three in the third part. Ocular symptoms in each section were scored from 0 to 4 according to their frequency (0: never, 1: sometimes, 2: half of the day, 3: most of the time, 4: all the time). The OSDI score, ranging from 0 to 100, was calculated using the following formula: [Total score×25 / number of valid questions].
For TBUT evaluation, a fluorescein strip was moistened with a drop of physiological saline and applied to the lower fornix. The patient was then asked to blink three times. The cornea was examined under cobalt blue light using a biomicroscope, and the time between the last blink and the appearance of the first dry spot on the cornea was recorded as TBUT. The mean of three measurements was calculated. Values below ten seconds were considered indicative of dry eye. For the Schirmer test, a 5 × 35 mm filter paper strip was placed in the conjunctival fornix at the outer one-third of the lower eyelid without topical anesthesia. After five minutes, the length of wetting on the paper was measured in millimeters. Values below 10 mm were considered abnormal. TBUT and Schirmer tests were performed by the same ophthalmologist (AOG).
Cellulose acetate filter paper (3 × 4 mm size) with an oval-cut triangular shape was cut and prepared for conjunctival impression cytology. 10 CIC samples were obtained from the patients’ inferotemporal interpalpebral bulbar conjunctiva one day after the other tests, under the same conditions and in the same room, by the same ophthalmologist (AT). Samples taken from the conjunctiva with cellulose acetate paper and fixed in separate vials were stained with Periodic Acid Schiff (PAS) and Hematoxylin-eosin (H&E) and evaluated with an Olympus Bx43 direct light microscope. The nucleus-to-cytoplasm ratio, the histological characteristics of the nucleus (size and shape), the degree of eosinophilic staining of the cytoplasm, the presence of intercellular connections, the PAS staining of goblet cells and the shape of goblet cell nuclei were evaluated in five separate areas under a light microscope. 10 Cytological changes were staged between 0 and 3 according to the Nelson classification system (Figure 1). The evaluation and staging of cytology were performed by an experienced pathologist (PO). Grades 2 and 3 were considered abnormal.
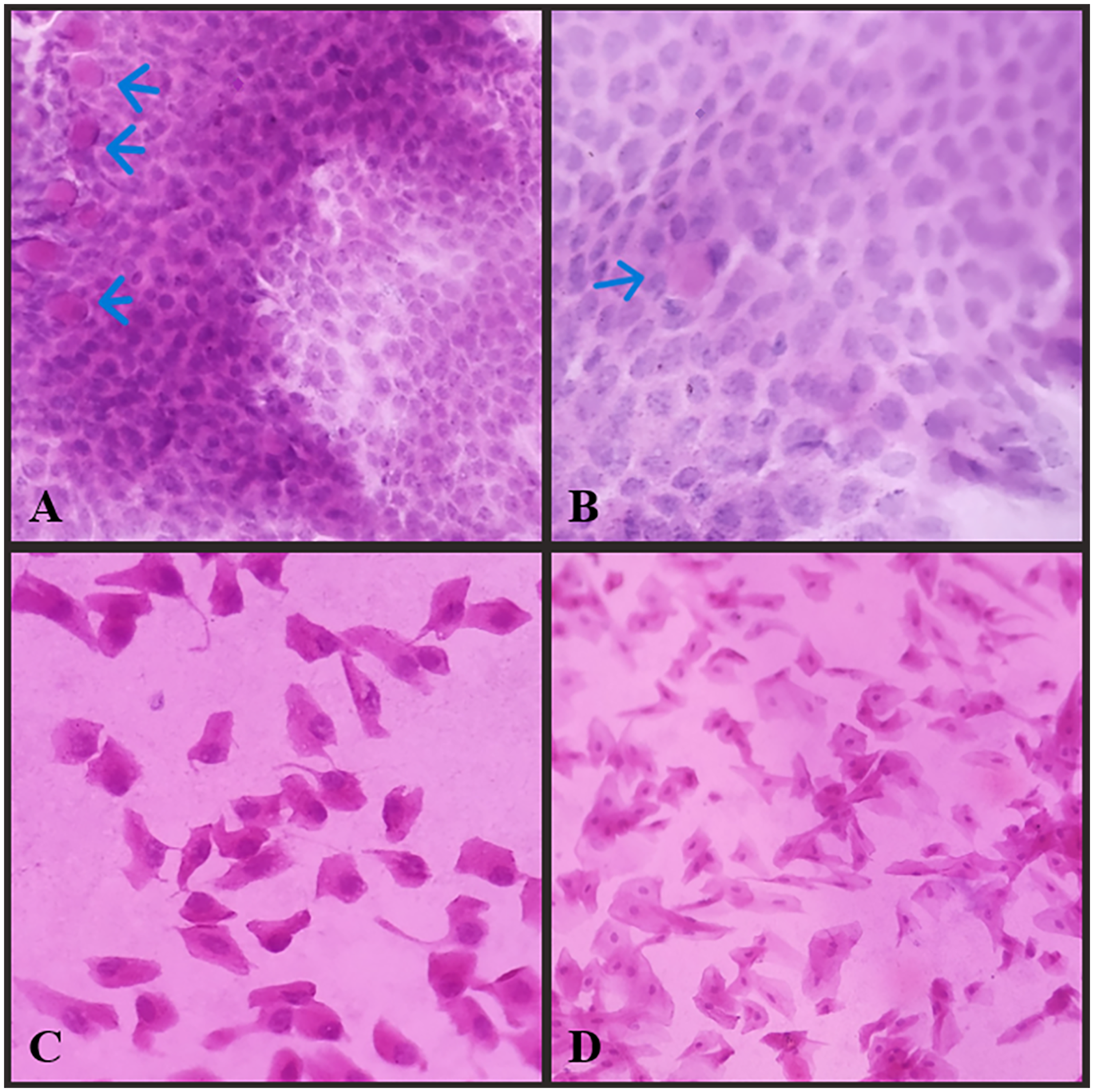
Representative images of Nelson conjunctival impression cytology (CIC) grades 0–3 (200×, hematoxylin and eosin stain). With the progression in the degree of CIC, the nucleocytoplasmic ratio of squamous epithelial cells decreases. In grade 3, nuclei in epithelial cells are pyknotic or absent. Goblet cells are observed as vacuolated or cylindrical cells with hematoxylin and eosin staining, and their number decreases with advancing CIC degree. (Arrows indicate goblet cells.) A Nelson grade 0, B Nelson grade 1, C Nelson grade 2, D Nelson grade 3.
Statistical analysis was performed using IBM SPSS Statistics version 20.0 (IBM Corp., Armonk, NY, USA). The suitability of continuous variables for normal distribution was assessed using the Kolmogorov-Smirnov test. Continuous variables were expressed as mean ± standard deviation (SD), while categorical variables were presented as numbers (n) and percentages (%). The Pearson chi-square test was used to compare categorical variables between two independent groups. The independent samples t-test was used to compare continuous variables with a normal distribution, whereas the Mann-Whitney U test was used for continuous variables that did not follow a normal distribution. Spearman's correlation test was used for correlation analysis of continuous variables. A two-sided p-value of <0.05 was considered statistically significant.
Results
Of the 49 early-stage PD patients included in the study, 27 were male (55.1%) and 22 were female (44.9%). The mean age of the PD group was 66.1 ± 7.2 years. Of the 45 participants included in the study as the control group, 29 were male (64.4%), 16 were female (35.6%) and their mean age was 65.3 ± 7.8 years. There was no significant difference between the two groups in terms of mean age and gender (p = 0.606, p = 0.357, respectively) (Table 1).
Comparison of the demographical characteristics, schirmer test result, TBUT, OSDI score, and CIC stage between Parkinson's and control groups.
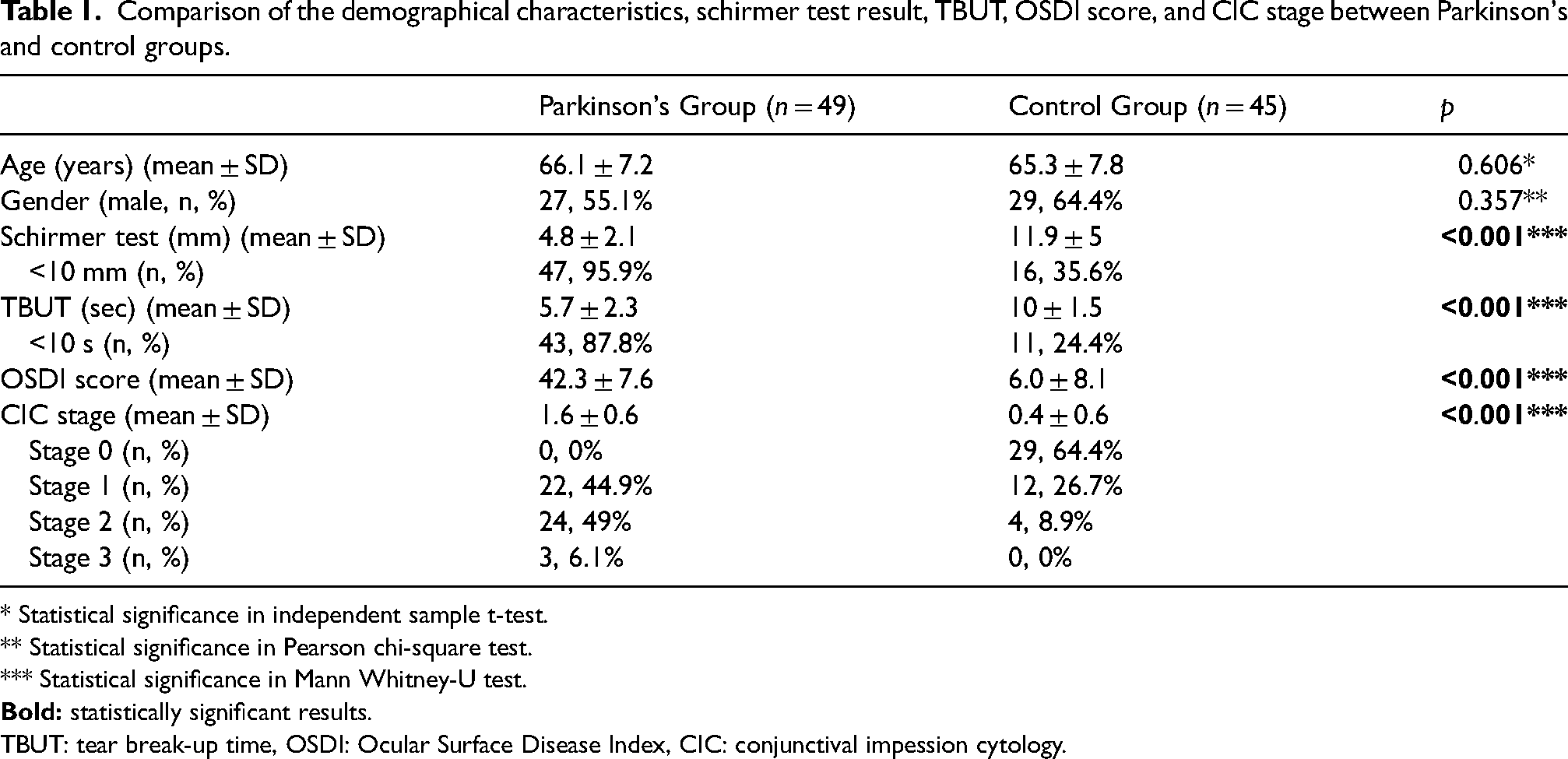
* Statistical significance in independent sample t-test.
** Statistical significance in Pearson chi-square test.
*** Statistical significance in Mann Whitney-U test.
TBUT: tear break-up time, OSDI: Ocular Surface Disease Index, CIC: conjunctival impession cytology.
The mean Schirmer test value was 4.8 ± 2.1 mm (2–10) in the PD group and 11.9 ± 5 mm (4–20) in the control group. Schirmer test results of the PD group were significantly lower than that of the control group (p < 0.001). Tear breakup time was 5.7 ± 2.3 s (2–10) in the PD group and 10 ± 1.5 s (7–12) in the control group. Similar to the Schirmer test results, the tear breakup time of the PD group was significantly lower than the control group (p < 0.001). On the other hand, the mean OSDI score was 42.3 ± 7.6 (28.1–56.2) in the PD group and 6 ± 8.1 (0–21.8) in the control group. The OSDI score results of the PD group were significantly higher than the control group (p < 0.001). In addition, the mean CIC stage was 1.6 ± 0.6 (1–3) in the PD group and 0.4 ± 0.6 (0–2) in the control group and this difference was also significant (p < 0.001). Conjunctival impression cytology of PD group showed stage 1 in 22 (44.9%), stage 2 in 24 (49%), stage 3 in 3 (6.1%) patients. There were no patients with stage 0. In the control group, conjunctival impression cytology detected stage 0 in 29 (64.4%), stage 1 in 12 (26.7%), stage 2 in 4 (8.9%) patients, while stage 3 was not detected (Table 1).
Schirmer test, TBUT, OSDI score, CIC stage, and age data obtained from patients in the PD group were analyzed for correlation. It was found that there was a moderate negative correlation between the Schirmer test and CIC stage (rs = -0.477, p < 0.001) and a weak positive correlation between the OSDI score and CIC stage (rs = 0.335, p = 0.019), and both these correlations were statistically significant (Figure 2).
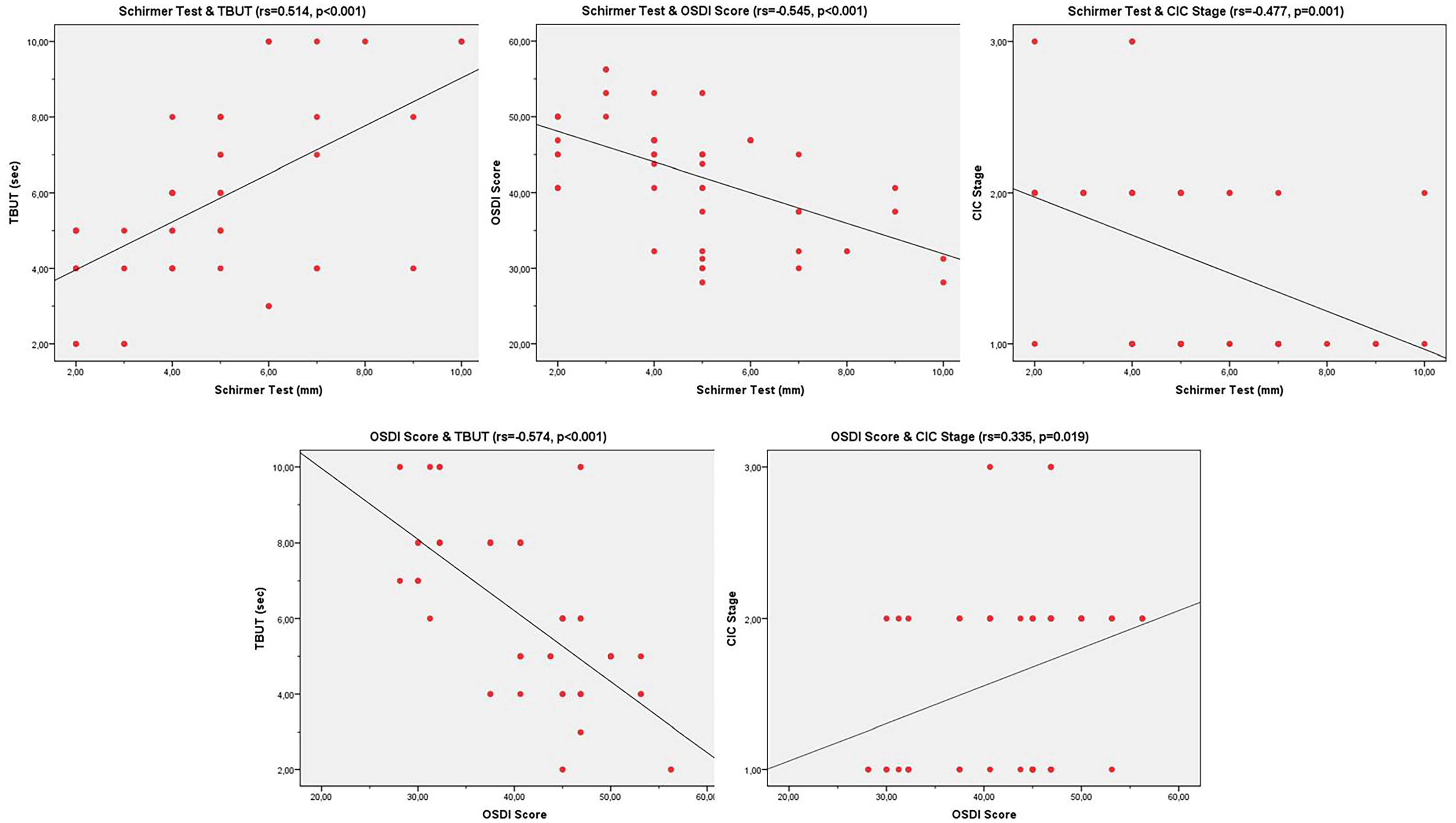
Bivariate scatterplots showing the statistically significant correlations in the Parkinson's group. (TBUT: tear break-up time, OSDI: Ocular Surface Disease Index, CIC: conjunctival impession cytology, rs: Spearman's correlation coefficient).
Dıscussıon
PD is the second most common neurodegenerative disorder after Alzheimer's disease. 11 It is characterized by dopamine deficiency in the striatum due to the degeneration of dopaminergic neurons in the substantia nigra and the accumulation of alpha-synuclein. 12 The prevalence of DED in Parkinson's patients is estimated to be between 53% and 60%. Various mechanisms are implicated in the development of DED in PD. Decreased dopamine levels in the central nervous system of Parkinson's patients lead to a significant reduction in their blink rate. 13 Blinking is necessary to protect the eye from external stimuli and to distribute tears across the ocular surface. 14 Changes in the composition and structure of meibum lipids contribute to an increased susceptibility to dry eye disease in Parkinson's patients. 15 The most commonly used tests for diagnosing dry eye disease are TBUT and the Schirmer test. However, these tests have low sensitivity and specificity and cannot detect morphological or cytological changes in the conjunctiva 16 Diagnostic tests with higher sensitivity and specificity, such as tear osmolarity measurement and conjunctival impression cytology, have been developed. 17 However, tear osmolarity measurement could not be performed in this study due to technical limitations. While many studies have assessed the ocular surface and DED in PD, no studies have simultaneously evaluated CIC and ocular surface changes together in Parkinson's patients.18–20
Numerous studies have reported abnormalities in ocular surface and tear parameters in patients with PD.21–23 Ulusoy et al. evaluated dry eye with the Schirmer test in Parkinson's patients and found the results to be significantly lower compared to the control group. 22 Demirci et al. reported that the TBUT, blink rate, and Schirmer test results in Parkinson's patients were significantly lower than those of the control group. 24 Similarly, in our study, Schirmer test and TBUT results were significantly lower in Parkinson's patients compared to the control group.7–24 Low levels of the Schirmer test and TBUT in Parkinson's patients may be due to a decreased exocrine secretion function of the lacrimal glands. Decreased blinking rate due to the loss of dopaminergic neurons in the central nervous system and low dopamine levels, corneal hypoesthesia causing decreased reflex lacrimation, and autonomic dysfunction have also been reported to play a role. 25 Decreased corneal sensitivity in Parkinson's patients may be one of the mechanisms contributing to the deterioration of tear film parameters. In their study investigating corneal sensitivity and tear functions in neurodegenerative diseases, Ornek et al. found that corneal sensitivity and Schirmer test results in Parkinson's patients were significantly lower than those of the control group. 7 Decreased corneal sensitivity may result in decreased neural impulses from the ocular surface to the central nervous system and decreased secretion from the lacrimal gland. Arrigo et al. conducted a study on early-stage Parkinson's disease patients who had never received pharmacological treatment and identified an increase in nerve fiber beadings and tortuosity using confocal microscopy. Additionally, magnetic resonance imaging assessing structural changes in the trigeminal nerve revealed a decrease in fractional anisotropy and an increase in mean diffusivity parameters. The changes in the trigeminal and corneal neuropathy observed by Arrigo et al. align with our findings, as they may contribute to the reduction of neural impulses from the ocular surface and the associated decline in lacrimal gland function. Together, these results highlight the significance of early neurodegenerative changes in Parkinson's disease and their direct impact on tear production. 26 Low TBUT values in Parkinson's patients indicate that there may be a disorder in the lipid layer of the tear film. Blinchevsky et al. have reported changes in the meibum lipid composition and structure in patients with PD. 15
We found that the mean OSDI score was significantly higher in the PD group than in the control group. Decreased tear production and tear quality cause increased dry eye complaints and an increase in the OSDI score in Parkinson's patients.
In the pathophysiology of DED, mediators activated by tear hyperosmolarity lead to a decreased expression of glycocalyx mucins, apoptotic death of surface epithelial cells, and loss of goblet cells. 27 It has been shown that the number of conjunctival goblet cells is significantly reduced from impression cytology samples in dry eye patients. 28 In their study on dry eye patients, Kumar et al. determined that there is a relationship between the morphological and cytological changes occurring on the ocular surface, tear function tests, and conjunctival impression cytology. 16 In our study, the mean CIC stage in Parkinson's patients was significantly higher than that in the control group. This is important as it shows that the increased dry eye disease in Parkinson's patients, as previously shown, may also cause cytological changes on the ocular surface. In the Parkinson's group, a negative correlation was found between the CIC stage and Schirmer test results, and a positive correlation was found with the OSDI score.
Our study is the first to evaluate CIC and tear parameters together in early-stage PD patients, and not only supports the susceptibility of these patients to dry eye, but also shows the relationship between conjunctival goblet cell loss and squamous metaplasia. Our findings may contribute to the literature on the pathophysiological mechanisms of ocular surface involvement in PD. The limitations of our study include the inclusion of only early-stage PD patients, a relatively small patient population, and the inability to perform meibography and osmolarity measurements during the evaluation of the ocular surface due to technical constraints. Additionally, the single-center design and lack of long-term follow-up can also be considered limitations.
In conclusion, DED is a common condition in early-stage PD patients and negatively affects their quality of life. Research has shown that in PD, in addition to a significant decrease in tear production and quality, there may also be cytological changes on the ocular surface. Large-scale studies with long-term follow-up will be beneficial in revealing the relationship between PD and DED.
Footnotes
Data availability
The data that support the findings of this study are available from the corresponding author, AT, upon reasonable request.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This study was approved by the Clinical Research Ethics Committee of the Meram Faculty of Medicine, Necmettin Erbakan University, and followed the tenets of the Declaration of Helsinki. (Decision No: 2022/4022)
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Informed consent was taken before each individual's participation in this study.
