Abstract
Objectives
The aims of this study were to evaluate: owners’ perceptions and priorities on the treatment and monitoring of feline diabetes mellitus (DM); the perceived effectiveness of the communication between veterinarians and clients regarding disease management; and the impact DM has on the owners’ everyday lives and human–pet bonds.
Methods
An initial questionnaire, then an adapted second questionnaire, were available to owners of cats with DM on vetprofessionals.com.
Results
A total of 748 questionnaires were completed. At diagnosis, fewer than half of veterinarians discussed how to recognise unstable diabetes (46%) or home blood glucose monitoring (HBGM) (40%). Owners were disappointed that the importance of diet on diabetic remission/stabilisation and HBGM were not discussed. Only 49% of respondents were supervised by a veterinarian/veterinary nurse while first drawing up insulin and injecting their cat. Websites/online forums that owners found themselves were most useful when learning about their cat’s diabetes (76% agreed). Over a third of cats (39%) were not fed a ‘diabetic’ diet but, impressively, 71% of owners used HBGM. Initial concerns about costs, boarding, the effect on their daily life and potential negative impact on the human–pet bond reduced significantly after initiating treatment (P <0.0001).
Conclusions and relevance
Caring for a diabetic cat requires significant owner commitment, plus support by the veterinary team for the owner and their cat. It is difficult to discuss all aspects of this complex disease with the owner in a single consultation; hence, it is important to involve the entire veterinary team in owner education and provide owners with informative material (eg, useful websites, printouts). Understanding owners’ priorities, fears, and which monitoring methods have helped others, is paramount to achieve owner compliance and satisfaction, and so improve the health and welfare of diabetic cats. This study provides useful information on the management of feline DM, which can be instrumental in educating future owners.
Introduction
Diabetes mellitus (DM) is a common disease in cats, affecting one in 200 cats in the UK,1,2 and one in 80 in the USA. 3 Veterinarians’ perceptions on the best treatment options have evolved over the past two decades,4,5 and the psychological and social impact of DM on the quality of life (QoL) of the owners has been evaluated. 6 However, there is little information about owners’ priorities in the treatment of this disease, or about which management options they find most useful.
Treatment of feline DM varies depending on a cat’s temperament and comorbidities, plus the owner’s home situation, including finances. The aim in newly diagnosed cats is to maximise the chances of remission while avoiding hypoglycaemia; for long-term diabetic cats (>6 months), the aim is to control clinical signs. 7 Diabetic remission is thought to result from reversal of glucotoxicity through a combination of effective insulin treatment, low-carbohydrate diet (<12% metabolisable energy [ME] from carbohydrates) and the management of concurrent diseases.7,8 Remission rates in newly diagnosed cats have been reported to be up to 84%.7,9 Glargine and protamine zinc insulin (PZI) have been proposed as the most appropriate insulins for cats,10,11 combined with low-carbohydrate diets.12,13 Home blood glucose monitoring (HBGM) can improve the glycaemic control of diabetic cats and the QoL of owners, who feel more in control, especially of recognising hypoglycaemia.14,15
Excellent communication between veterinarian and client is paramount to achieve good diabetic control and, where possible, achieve remission. However, DM is complex, and it is not possible to discuss all aspects of the disease in a 10–15-min consultation, which is the standard length of a small animal practice consultation in the UK. 16
The aims of this study were to evaluate: owners’ perceptions and priorities on the treatment and monitoring of their cat’s DM; perceived effectiveness of communication between the veterinarian and client regarding case management; and the impact the disease has on the owners’ everyday life and human–pet bond.
Materials and methods
This study comprised two online questionnaires open to people who currently or previously owned a cat with DM. A first questionnaire (24 questions) was available worldwide from 29 July 2015 to 26 January 2016 via www.vetprofessionals.com (see file 1 in the supplementary material). It asked about: treatment options offered; which factors were most important to the owner for decision-making at diagnosis; what support they received from their veterinary clinic; their concerns and priorities during monitoring; their views on HBGM and insulin pens; and what they felt could have improved their cat’s QoL. A second, simplified, version of this questionnaire was available from 10 October 2017 to 23 December 2017 (see file 2 in the supplementary material): 21 of the initial 24 questions were adapted from the first questionnaire; questions related to insulin administration and discussion between owner and veterinarian at diagnosis were excluded. The questions took a variety of forms, including numerical scoring (from 0 to 10), selecting a single option from a drop-down menu, multiple choice and free-text statements. Responders had to be at least 18 years old and could only complete one questionnaire per household. Ethical approval for both questionnaires was gained from the University of Edinburgh Veterinary Ethics Committee.
Data from the two surveys were combined. To do this, questions in the first survey that asked for a scaled response were changed to ‘yes’, ‘no’ or ‘not applicable’ to fit the answer choices in the second survey. For example, if the answer options were 1 = very helpful, 2 = slightly helpful, 3 = neither helpful nor unhelpful, 4 = poor, 5 = very poor, N/A = I did not received this support; when respondents chose 1 or 2, their response was changed to ‘yes’; when they chose 4 or 5, their response was changed to ‘no’; those who answered 3 were not analysed, as the response was not covered by the second survey answer choices. Descriptive statistics and frequency distribution were performed using Microsoft Excel. The importance of different factors to the owners’ decision-making before and after treatment was compared using a χ2 test; statistical significance was set at P <0.05.
Results
A total of 862 questionnaires were received; 114 were removed because of duplication or minimal completion, leaving 748 useful replies (279 from the first questionnaire and 469 from the second). Not all owners responded to all questions; hence, the total number of answers for each question was variable. Most respondents lived in the USA (n = 319; 43%), followed by the UK (n = 268; 36%), Canada (n = 51; 7%) and the Netherlands (n = 45; 6%), plus smaller numbers from another 23 countries (see file 3 in the supplementary material).
Population
Cats were from both sexes (412 neutered males, 210 neutered females, 66 entire males, 60 entire females) and in the following age categories: 11 cats were <5 years of age, 180 cats were 5–10 years old, 343 cats were 11–15 years old, 202 cats were ⩾16 years and 12 cats were of unknown age. Most (n = 492/699; 70%) had been diagnosed with DM more than a year before, while 18% (n = 129/699), 8% (n = 55/699) and 3% (23/699) had been diagnosed 4–12 months, 1–3 months, and <1 month before, respectively. Of 676 cats that were alive at the time the questionnaires were completed, 18% (n = 122/676) were in diabetic remission.
Owner education
The topics most often discussed between owner and veterinarian at the time of diagnosis were insulin treatment (n = 237/260; 91%) and frequency of clinic revisits (n = 190/260; 73%). Fewer than half of veterinarians discussed how to recognise unstable diabetes (n = 119/260; 46%), diabetic remission (n = 106/260; 41%) or HBGM (n = 103/260; 40%) (Figure 1). At diagnosis, fewer than half of the owners (n = 323/717; 45%) were confident or very confident at recognising and treating hypoglycaemia (Figure 2).

Topics discussed between veterinarian and owner at the time of diagnosis. The horizontal axis shows the percentage of cases where each topic was discussed (n = 260)

Level of confidence at recognising the signs of hypoglycaemia and knowing what to do in this situation (n = 717)
One quarter of owners reported they had not been shown how to draw up (n = 66/259; 25%) or administer the insulin (n = 70/259; 27%), and only 49% (n = 125/256) were supervised by a veterinarian or veterinary nurse while first drawing up insulin (or saline) and injecting their cat. Figures 3 and 4 show how difficult it was for owners to draw up and administer the insulin the first time they did it, and how this later improved with experience.

Level of difficulty drawing up the correct amount of insulin for the first time (yellow), compared with the last time (blue) the owner had to do it. The horizontal axis shows the percentage of owners that chose each option (n = 241)

Level of difficulty administering the insulin for the first time (yellow), compared with the last time (blue) the owner had to do it. The horizontal axis shows the percentage of owners that chose each option (n = 243)
The ‘needle and syringe’ was the method of insulin administration used by most owners (n = 238/265; 90%); ‘insulin pens’ were only used by 10% (n = 27/265). Of concern, 41% (n = 100/243) of owners had, at some point, injured themselves when injecting their cat (for 94% of these owners, on fewer than five occasions). Most injuries occurred with ‘needle and syringe’ (n = 91/100; 91%), and a few with needles during HGBM (n = 6/100; 6%) or with ‘insulin pens’ (n = 3/100; 3%). Of 14 respondents who shared their experiences of ‘insulin pens’, only two (14%) agreed or strongly agreed this was easier to use than a traditional ‘needle and syringe’, eight (57%) disagreed and four (29%) found the two methods to have a similar difficulty.
Decision-making at diagnosis
Owners were asked to select useful sources of information about feline DM from a list. Websites/online forums that they had found themselves were the most useful resource to learn about their cat’s diabetes (Table 1).
Usefulness of various sources of information about diabetes in cats (n = 748)
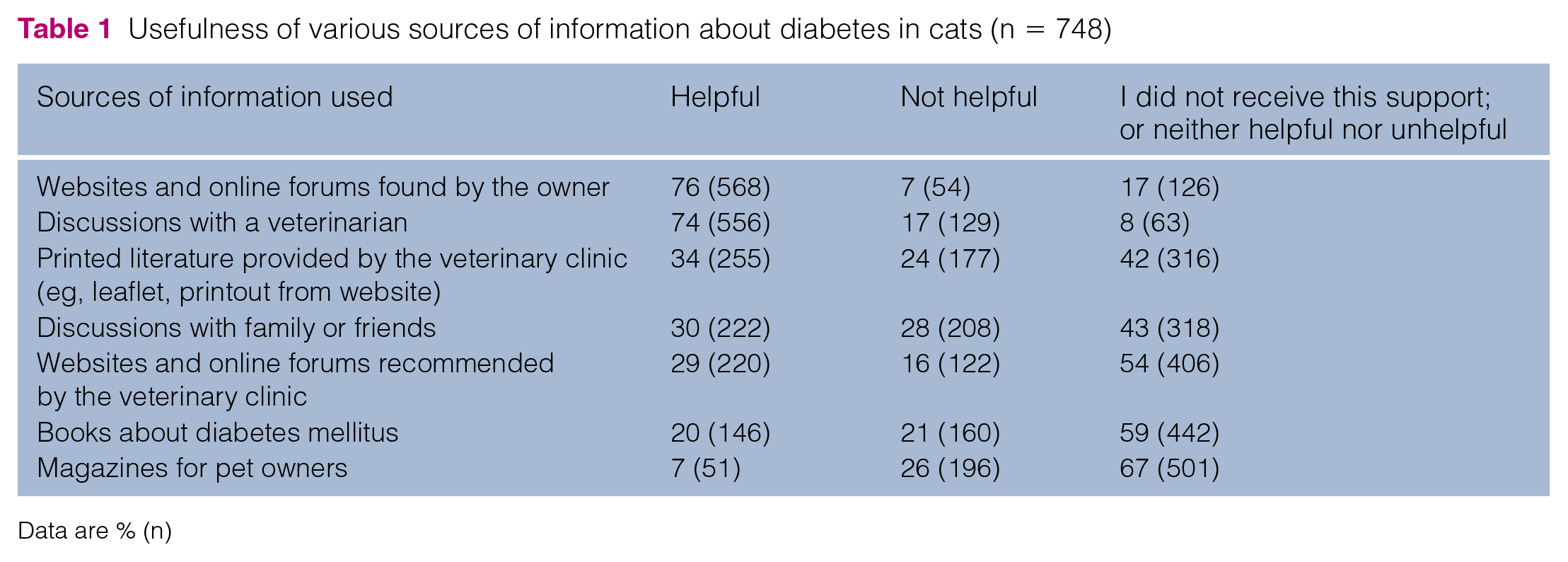
Data are % (n)
The most important factors when deciding on treatment were ‘what is best for my cat’ and ‘veterinarian recommendations’, which were selected by nearly 100% (n = 739/741) and 86% (n = 613/716) of owners, respectively. Fewer owners selected ‘ease of treatment’ (n = 443/682; 65%) or ‘fear of injections’ (n = 156/595; 26%).
To determine what impact the daily management of their cat’s DM had on their QoL, owners were asked to recall if certain issues factored into their decision-making when their cat was diagnosed. Owners were then asked how important they currently found those same factors. The major initial concerns were costs and finding someone to take care of their cat when they were away. These factors concerned a significantly higher number of owners before treatment than after treatment (P <0.0001) but continued to worry over a half of the owners. Overall, owners felt that caring for a diabetic cat had less effect on their daily lives and their human–pet relationship than they had believed it would before starting treatment (P <0.0001) (Table 2).
Proportion of affirmative responses by owners to opinions felt before and after starting treatment for their diabetic cat

Treatment
Treatments prescribed to control diabetes are presented in Figure 5. Insulin was used to treat 93% (n = 681/736) of the cats. Most (n = 334/417; 80%) were treated with insulin twice daily; 14% (n = 58/417) received a variable dose and frequency of insulin (depending on blood glucose measurements), 6% (n = 24/417) received insulin once daily and one cat (1/417; 0.2%) received insulin three times daily. Food supplements and oral hypoglycaemic drugs were only given to 5% (n = 36/736) and 1% (n = 9/736) of cats, respectively.

Treatments and dietary interventions given to control diabetes. The horizontal axis shows the percentage of cats given each treatment (n = 736)
In the UK, Lente was the most commonly used insulin (n = 50/79; 63%); much smaller numbers of cats were treated with glargine (n = 14/79; 18%) or PZI (n = 9/79; 11%); a negligible number of cats was treated with other insulin types. Glargine was the preferred insulin type in the USA (n = 60/154; 39%), Canada (n = 10/24; 42%) and Australia (n = 6/9; 67%), followed by PZI in the USA and Lente in the latter two countries.
About one-third of cats (n = 244/736; 33%) were fed ‘a special diet prescribed by the veterinarian for the management of diabetes’ (Figure 5). A similar percentage (n = 203/736; 28%) were fed a diet chosen by their owners to help control diabetes – this percentage may, in reality, be higher, as ‘a diet for management of diabetes not prescribed by the veterinarian’ was not offered as an answer option from the drop-down menu. Instead, this information was obtained from the free-text answer option, where owners explained they had elected to feed a commercial or, less commonly, home-prepared, generally wet, low-carbohydrate diet. Comments showing negativity towards veterinary diets (the high cost and the high carbohydrate content of some diets) and towards veterinarians who had not discussed diet were common. Over one-third of cats (n = 289/736; 39%) were not fed a diet to help diabetic control.
Monitoring
The preferred methods for monitoring diabetic control at home are shown in Figure 6. Half of the owners using HBGM (n = 138/260; 53%) received this advice from the internet; 27% (n = 70/260) received this advice from their veterinarian; the remaining respondents had been advised by a friend, relative, veterinary nurse or had decided to undertake HBGM based on previous experience as diabetics themselves or as the owner of a previous diabetic cat. Over two-thirds of owners who used HBGM claimed to do it ‘once or more every day’, on average (n = 355/522; 68%) (Figure 7). Many owners commented that they measured blood glucose several times per day to follow ‘the tight regulation protocol’, which is recommended on several online forums for owners of diabetic cats (eg, http://diabeticcathelp.com/forum). Some responders commented that they measured their cat’s blood glucose as frequently as ‘every 2 hours’, or ‘sometimes as high as 20–30 times/day’. Only a third of owners using HBGM found it difficult or very difficult when they first started to do this (Table 3).

The preferred methods for monitoring diabetic control (n = 708). HBGM = home blood glucose monitoring

Average frequency of home blood glucose monitoring (n = 522)
Level of difficulty of home blood glucose monitoring when the owners first started to use this (n = 522)

The main problems experienced during HBGM included difficulty restraining the cat and obtaining enough blood for testing. The part of the cat’s body that owners found the easiest to collect blood from was ‘the vein on the edge of the ear’ (n = 403/522; 77%). Less popular sites included ‘the area between the marginal vein and the edge of the ear’ (n = 49/522; 9%), the middle of the ear (n = 25/522; 5%), the foot pads (n = 28/522; 5%) or other areas of the body generally not specified. When asked to offer advice to owners new to this technique, they frequently recommended ‘watching online videos on how to do this’, and ‘warming the ear first, using a water bottle warmed in the microwave’.
Owners were asked if anything could have improved theirs and their cat’s QoL; they often wished their veterinarians were more knowledgeable about the role of diet in treating feline DM, and had advised them to use HBGM. Giving insulin, changing to a low-carbohydrate diet, and performing HBGM were, in their opinion, the factors that played the most significant role in controlling their cat’s diabetes.
Discussion
This is the largest survey to date reporting owners’ priorities and perceptions on the treatment and monitoring of their diabetic cats; it also assesses the effectiveness of communication between veterinarians and clients when advising owners of cats with DM. Owners who experienced more difficulty or had greater concerns were likely selected for, as they were likely more motivated to search for help online and to complete the online questionnaire. Our study clearly shows that veterinary communication needs to be improved if we are to offer the best care for our diabetic cats and their owners.
Feline DM is complex and several aspects need to be discussed with the owner upon diagnosis. Sadly, fewer than half of veterinarians discussed how to recognise an unstable diabetic (46%), diabetic remission (41%) or HBGM (40%). Despite evidence that low-carbohydrate diets may lead to higher diabetic remission rates8,9 and improved glycaemic control, 14 a quarter of veterinarians did not discuss a dietary change. There were many comments from owners who were angry or disappointed about the omission of discussion about the importance of diet on diabetic stabilisation and remission.
Many owners were not shown how to draw up (25%) and administer insulin (27%), or were not supervised by a veterinarian or veterinary nurse while doing this for the first time (51%). Moreover, only 45% felt confident in recognising signs of hypoglycaemia. As hypoglycaemia can be life threatening, veterinarians must ensure that this is discussed in the initial consultation. Knowing how difficult it is to discuss all aspects of the disease in one standard consultation (and how unlikely the owner is to recall all that is said), it is important to involve the entire veterinary team in the education of these owners; for example, having an initial appointment with the veterinarian, followed by an appointment with a veterinary nurse. Additionally, giving leaflets and printouts to the owner, as well as advice on good websites, will save the veterinarian time and likely result in a well-informed, more satisfied client. Most owners (76%) stated that websites/online forums that they had found themselves were the most useful resource to learn about their cat’s diabetes. Veterinarians must acknowledge the importance of internet research and be prepared to direct their clients to websites with accurate and useful information on disease management (eg, www.vetprofessionals.com or icatcare.org).
Owners’ initial concerns included difficulties in arranging for someone to look after their cat during holidays (77%), costs (69%), the effect that caring for a diabetic cat would have on their lives (41%) and a negative impact on the human–pet bond (40%). All these concerns reduced significantly after initiating treatment (P <0.0001); this information can be given to future owners to help reduce their fears and stress at the time of diagnosis. ‘Boarding difficulties’ and ‘difficulties leaving their cat with friends or family’ had previously been reported among the main concerns of owners of diabetic cats. 6
Insulin pens were only used by 10% of the respondents who, in general, did not feel they were easier to use than a traditional ‘needle and syringe’. However, 91% of injuries associated with injections occurred with ‘needle and syringe’, and while not directly comparable, only 3% of respondents had injured themselves using an insulin pen. Insulin pens may be especially helpful when low doses of insulin need to be accurately administered. 17
Lente was the most commonly prescribed insulin in the UK, whereas glargine was the most common insulin used in the USA, Canada and Australia. In the UK, Lente was the only insulin licensed for cats at the time of the surveys (PZI is now licensed in the UK too). In contrast, veterinarians working in some other countries can prescribe whichever insulin type they prefer. Recently published guidelines on the management of feline DM recommend starting treatment with long-acting insulin such as glargine or PZI, as they are likely to provide the best glycaemic control and higher remission rates.12,17
About one-third of cats were fed a veterinary prescription diet designed for the management of feline diabetes. Another third were fed non-prescription diets chosen by the owners to help control diabetes. Although most of these owners said these were wet low-carbohydrate diets, others seemed to believe that all that is needed is to switch to a tinned food of some sort. Their overall impression was that prescription diets are expensive and too high in carbohydrates. Although the relative contribution of diet in increasing the probability of remission is unknown, diets containing <12% ME from carbohydrates are often recommended by experts in feline DM to improve glycaemic control and maximise the probability of remission.4,7,18 Such carbohydrate reduction is only achievable by feeding canned diets with higher protein and/or fat contents, as all dry cat foods that are not specifically formulated for diabetes treatment, especially ‘cheaper’ supermarket diets, contain higher carbohydrate content. The following veterinary endocrine blog offers an easy explanation on how to calculate ME from carbohydrates for different diets, as well as an automatic carbohydrate calculator: https://endocrinevet.blogspot.com/2014/01/how-to-calculate-carbohydrate-and.html. A comparison of the carbohydrate, fat and protein contents of several prescription and commercial diets can be found in file 4 in the supplementary material. This web link and table can be given to owners for guidance when choosing the best diet for a diabetic cat.
The preferred methods to monitor diabetic control at home were to assess their cat’s general demeanour, appetite and thirst (>89% of respondents), followed by body weight (75%) and HBGM (71%). The percentage of owners using HBGM was higher than reported in 2010, 6 which may indicate the increasing popularity of this monitoring tool over the past 8 years. Surprisingly, and perhaps rather intrusively for the cats, over two-thirds of owners who used HBGM claimed do it ‘once or more times every day’. HBGM has been shown to improve remission rates, reduce the need for clinic visits and improve the QoL of owners and cats, mainly by reducing owners’ concerns (eg, about costs and hypoglycaemia).15,19 The majority of our owners received advice about HBGM from the internet; however, they wished this had been recommended by their veterinarian. Owners found the easiest site to collect blood for HBGM from to be the marginal ear vein.
There are caveats to the results generated by this survey, as cat owners who completed the questionnaires are likely to be dedicated owners who had performed online searches and found the Vet Professionals website or Facebook page. In addition, previous studies report diabetic remission rates of up to 84%, whereas only 18% of cats in our study were in remission – it is likely that results represent the points of view of owners of cats with more difficult to control diabetes. The fact that internet access was required to complete the survey potentially lowered the proportion of underprivileged owners, or owners from countries with poor internet accessibility. Moreover, the survey relied on owners recalling details of their cat’s diabetes and discussions with their veterinarian, which may have resulted in some recall bias.
Conclusions
Caring for a diabetic cat requires significant owner commitment, plus support by the veterinary team for the owner and their cat. It is difficult to discuss all aspects of such a complex disease in one consultation; hence, it is important to involve the entire veterinary team in owner education and provide the owners with informative material (eg, websites, printouts) and ongoing support. Understanding owners’ priorities and fears, as well as which monitoring methods have helped them, is paramount to achieving owner compliance and satisfaction, and so improve the health and welfare of diabetic cats. This study provides useful material for the management of feline DM, which can be instrumental in how we educate future owners.
Supplemental Material
Supplemental_File – Supplemental material for Priorities on treatment and monitoring of diabetic cats from the owners’ points of view
Supplemental material, Supplemental_File for Priorities on treatment and monitoring of diabetic cats from the owners’ points of view by Carolina SC Albuquerque, Bretta L Bauman, Janina Rzeznitzeck, Sarah MA Caney and Danièlle A Gunn-Moore in Journal of Feline Medicine and Surgery
Footnotes
Acknowledgements
The authors would like to thank Vet Professionals, MSD Animal Health and Dr Vaz for their financial support.
Supplementary material
The following files are available online:
File 1: Questionnaire 1
File 2: Questionnaire 2
File 3: Data on the survey respondents
File 4: Comparison of carbohydrate, protein and fat contents of several veterinary prescription and feline maintenance diets
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This work was partially supported by Vet Professionals and MSD Animal Health.
Ethical approval
This work involved the use of client-owned animals outside of established internationally recognised high standards (‘best practice’) of individual veterinary clinical patient care. The study therefore had ethical approval from an established committee as stated in the manuscript.
Informed consent
Informed consent was obtained from the owner or legal custodian of all animals described in this work for data analysis. No animals or humans are identifiable within this publication, and therefore additional informed consent for publication was not required.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
