Abstract
Objectives
The purpose of this study was to survey owners regarding their practices and experiences with the administration of subcutaneous (SC) fluids at home to cats with chronic kidney disease (CKD) to gain insight that might help more owners be successful with the procedure.
Methods
A web-based survey was advertised online. Owners of 468 cats with CKD participated, 399 of whom administered SC fluids.
Results
Fifty-nine percent of the cats were domestic shorthairs, with >85% of the cats being 10 years of age or older. IRIS stage 3 was most commonly represented (37%). Ninety-five percent of owners said they discussed giving fluids with their veterinarian, with only 42% of those discussions involving additional educational resources. A large majority of owners (85%) said it was either an easy, somewhat easy/no stress or okay experience for them, and a large majority (89%) reported that the experience was easy/no stress, somewhat easy or okay experience for their cats. To increase tolerance, 57% said they gave a treat to their cat afterwards, and 60% said they warmed the fluids. Sixty-one percent reported using a 20 G or larger needle, with 49% saying size of needle affected tolerance. Seventy-four percent also felt that the length of time it took to administer fluids affected tolerance. One-hundred milliliters was the most commonly given fluid amount. Hydration status was monitored by 40% of owners by various methods, with 40% of those saying they skipped or added fluids based on hydration assessment.
Conclusions and relevance
A majority of owners gave positive feedback about their ability to learn and administer SC fluids to their cat wth CKD. Owners reported several strategies that they felt improved tolerance of fluid administration. Overall, the protocol should be tailored to the preference of the cat for best possible long-term success.
Introduction
Chronic kidney disease (CKD) is a common condition in cats that increases in prevalence with age and is associated with high morbidity and mortality in end-stage disease. Clinical signs of CKD vary, but dehydration is a common sequela secondary to the loss of urine-concentrating ability. 1 In order to combat dehydration, subcutaneous (SC) fluid administration is often prescribed. 2 A survey study by Markovich et al identified that 46.9% of cats with CKD receive SC fluids as supportive therapy. 3
Although SC fluid therapy is a common palliative treatment for CKD, there are no studies to date that have examined its efficacy. The ISFM Consensus Guidelines on the Diagnosis and Management of Feline Chronic Kidney Disease recommend SC fluids in CKD to manage dehydration. 4 Clinical experience suggests SC fluids help cats with kidney disease that cannot maintain adequate hydration to demonstrate fewer clinical signs and help manage complications such as constipation. The intent of this survey study was to document habits among owners who administer SC fluids in order to identify issues that should or could be addressed, as well as techniques that increase the likelihood of owners effectively administering SC fluids.
Materials and methods
A web-based survey was designed, consisting of 45 questions evaluating SC fluid administration frequency, type of fluid and many other variables involved with the administration of fluid in a feline (Appendix 1, supplementary material). This study was reviewed by the Colorado State University Research Integrity and Compliance Review Office and determined to not require Institutional Animal Care and Use Committee or Institutional Review Board approval. The survey was advertised to owners of cats with CKD via social media (eg, Facebook). The survey was also advertised directly to veterinarians via email, VIN, ACVIM listserv, vetprofessionals.com, etc. The survey was posted online for 4 months for public participation (July–October). In order to participate in this survey, respondents were required to own a cat with CKD.
Owners could only complete the survey once and for one pet only. The majority of questions were multiple choice or short-answer in design and some allowed multiple answers. Short answers from the owners were evaluated and grouped according to the similarity of their content. Each survey required 15–20 mins to complete. An incentive of a discount on Dr Sarah Caney’s book Caring for a Cat with Chronic Kidney Disease was offered, and all responses were anonymous. Only those responses from participants who completed the survey through to the last question were evaluated; if participants stopped before completing the survey, their data was not included in the results. Data collected from online questionnaires were collated and stored using FormSite (Vroman Systems) before downloading into a Microsoft Excel spreadsheet for analysis. Descriptive statistical analysis was performed on the data.
Results
There was a total of 468 respondents. A majority of those responses (n = 352; 75%) were from the USA. The remainder were from the UK (n = 48; 10%), Australia (n = 24; 5%) and Canada (n = 21; 5%). Seventeen other countries were represented by a range of 1–3 participants, including Belgium, Brazil, Denmark, Egypt, France, Greece, Hong Kong, Ireland, Japan, Netherlands, New Zealand, Portugal, Singapore, South Africa, Spain, Switzerland, and Zimbabwe. The USA, UK, Australia and Canada together accounted for a combined 95% (n = 445) of the results received.
There were several breeds represented within the study. Fifty-nine percent (n = 276) of cats were domestic shorthairs. The remainder were domestic longhairs (n = 46; 10%), Siamese (n = 22; 5%), Persian (n = 15; 3%) and ‘other’ (n = 109; 23%). A total of 409 cats (87%) were 10 years of age or older. Cats older than 15 years were the most commonly represented (n = 250; 53%). One-hundred and fifty-nine cats (34%) were aged 10–15 years, 47 cats (10%) were aged 5–9 years and nine cats (2%) were aged younger than 5 years. Three owners did not know the ages of their cats. The number of cats in each IRIS stage receiving SC fluids is shown in Figure 1.

The percentage of cats in each IRIS stage receiving subcutaneous fluid therapy. On the survey form, IRIS stage was listed along with creatinine values to assist those individuals who might know only one value or the other. IRIS stage 1 (serum creatinine <1.6 mg/dl [<140 µmol/l]), IRIS stage 2 (serum creatinine 1.6–2.8 mg/dl [140–250 µmol/l]), IRIS stage 3 (serum creatinine 2.9–4.9 mg/dl [251–440 µmol/l]), IRIS stage 4 (serum creatinine >5.0 mg/dl [>440 µmol/l])
Four hundred and forty-six (95%) individuals said they discussed administering fluids with their veterinarian. Of the 399 owners in the study who reported administering fluids, 58% (n = 230) were offered or directed toward additional resources, such as brochures, YouTube videos, etc, whereas 42% (n = 169) were not. A veterinarian was the most common individual to recommend giving SC fluids (n = 334; 84%), followed by owner request (n = 58; 14%). In 8% of cases (n = 32), SC fluids were recommended by another individual and in 1% of cases (n = 5) SC fluids were recommended by a nurse or technician. This question allowed multiple responses (429 responses from 399 owners). Of the 45 owners who indicated they initiated the conversation about beginning fluids on their cats, 32 (71%) were from the USA, nine (20%) were from the UK, two (4%) were from Canada, one (2%) was from Egypt and one (2%) was from Switzerland.
Of surveyed respondents, 399 (85%) said they gave SC fluids, whereas 57 (12%) did not and 12 (3%) stated that they tried but could not. Of the 399 owners who gave SC fluids, 151 (38%) had given SC fluids before, whereas 248 owners (62%) had not. Of the 57 owners who reported they did not give SC fluids, 13 (23%) never discussed it with their veterinarian, 19 (33%) stated their veterinarian said it was not needed at the time, five (9%) said it was not tolerated and two (4%) said that they were not comfortable with the procedure; 19 (33%) stated another reason for why they did not give SC fluids, the most common of which included the owner’s cat being deceased, placement of an esophageal tube and a diagnosis of heart disease.
Of the 399 owners that administered SC fluids, 37 (9%) gave fluids twice daily, 156 (39%) gave fluids once daily, 121 (30%) gave fluids 3–4 times weekly, 57 (14%) gave fluids 1–2 times weekly and 28 (7%) gave fluids on a basis other than what was listed. Lactated Ringer’s was the most commonly administered fluid type (n = 296; 74%), followed by normal saline (n = 56; 14%) as the second most common. Twenty-five (6%) used another fluid type other than the options offered, 20 (5%) used Hartmann’s and 17 (4%) used Plasmalyte. This question allowed multiple responses.
Two-hundred and sixty (65%) owners stated that one person was involved with fluid administration, 134 (34%) said that two people were involved with administration, three (1%) said three people were involved with administration and 22 (6%) selected ‘Other’, usually responding that the number of people involved in the administration varied. This question allowed multiple responses (419 responses from 399 owners). Three-hundred and sixty (90%) administered SC fluids themselves, 59 (15%) had a family member administer, 18 (5%) had a veterinary technician administer, 12 (3%) had veterinarians administer and 33 (8%) had an individual other than that listed administer. This question allowed multiple responses (464 responses from 399 owners).
One-hundred and thirty-six owners (34%) assessed hydration once daily prior to fluid administration. Fifty-five (14%) assessed hydration twice daily, 26 (7%) assessed hydration twice weekly and 38 (10%) assessed hydration once weekly. Seventy-two (18%) owners assessed hydration in a frequency other than those listed and 72 (18%) stated that they did not know how to assess hydration. Two-hundred and ninety-three (73%) owners assessed hydration via skin tent/turgor, 124 (31%) assessed mucous membranes, 54 (14%) estimated water consumption and 51 (13%) assessed hydration in a manner other than those listed; 67 (17%) stated that they did not know how to assess hydration. This question allowed multiple responses (589 responses from 399 owners). One-hundred and sixty (40%) owners skipped or added fluids based on hydration assessment, whereas 187 (47%) owners did not.
Three hundred and twenty-two (81%) owners administered fluids between the shoulder blades, whereas 77 (19%) said they administered fluids in another location. Two-hundred and eighty-eight (72%) individuals utilized a rotation pattern for needle insertion on their cats. Three-hundred and ten (78%) gave fluids utilizing gravity/drip method, 36 (9%) used high pressure by squeezing the bag, 27 (7%) used a syringe and 24 (6%) utilized a combination of methods.
One-hundred and twenty (30%) owners used a 20 G needle to administer fluids, 111 (28%) used an 18 G needle to administer fluids, 87 (22%) used a 21 G needle to administer fluids, 30 (8%) used a 22 G needle to administer fluids and 51 (13%) used a size other than the options listed to administer fluids. One-hundred and ninety-seven (49%) owners said they felt that the size of the needle used affected tolerance of fluid administration, 43 (11%) felt that the size of the needle used did not affect tolerance of fluid administration, 145 (36%) could not make an accurate assessment of the influence of needle size on tolerance of fluid administration, as they had only used one needle size; 15 (4%) had a response other than the options listed.
An amount of 100 ml was the most common amount of fluid administered, with about half of owners in the survey administering this amount (n = 207; 52%). Forty-seven (12%) gave 75 ml, 43 (11%) gave 150 ml, 39 (10%) gave 50 ml and 63 (16%) gave ‘another’ amount other than the options listed. Just over one-third of owners (n = 144; 36%) said the amount of fluid given affected the overall tolerance, whereas a similar number (n = 122; 31%) said it did not. One-third (n = 133; 33%) had only given the same amount of fluids, so could not accurately make a judgment about tolerance as it pertained to this variable.
Forty-seven (12%) owners said they added potassium supplementation to their cat’s fluids. Of those that added potassium, 23 (49%) added 20 mEq/l, three (6%) added 30 mEq/l and 21 (45%) were either not sure about the amount or added an amount other than those options listed. The most common other amount administered was 10 mEq/l. The remaining single responses included 16 mEq/l, 24 mEq/l and 40 mEq/l. Fifteen (32%) individuals who gave potassium supplementation said they felt it changed the behavior of their cats. Of the 15 owners who reported a change in behavior with potassium supplementation, eight (53%) gave 20 mEq/l, five (33%) were unsure of the potassium dose, one (7%) gave 24 mEq/l and one (7%) gave 16 mEq/l. Forty-one (10%) owners added extra vitamin B to their fluids. Of those that added extra vitamin B, 25 (61%) protected the bag and line from light.
One-hundred and fifty-five (39%) owners restrained their cats for fluid administration. Additionally, 190 (48%) owners reported distracting their cats during administration. A majority of owners (n = 227; 57%) stated they gave their cats treats after fluid administration as a form of positive reinforcement. Of those that used positive reinforcement, it was generally felt that it helped with tolerance. One-hundred and thirty (57%) said it helped, 15 (7%) said it did not help, 71 (31%) were unsure and 11 (5%) answered ‘other’.
Two-hundred and forty-one (60%) individuals stated they warmed fluids prior to administration. Of the 241 owners who said they warmed fluids, 200 (83%) reported that this increased tolerance, whereas five (2%) said that it did not and 32 (13%) did not know; four individuals (2%) gave answers other than those listed. Overall, 294 (74%) owners felt that the amount of time taken to give fluids affected their cats’ tolerance of the experience. Two-hundred and six (52%) owners said it took less than 5 mins to give fluids, 137 (34%) owners said it took 6–10 mins, 36 (9%) said it took 11–15 mins, 15 (4%) said it took 16–20 mins and five (1%) said it took more than 20 mins. One-hundred and fifty-five (39%) owners stated they have skipped fluid administration in the past 2–4 weeks owing to their cats being frustrated. During the first 2–4 weeks of fluid administration, the results were very similar, with 153 (38%) owners saying they had skipped a fluid session.
Just over 90% (n = 364) of owners changed needles after every fluid administration event. About one in 10 (n = 35; 9%) re-used needles, including at least one owner who reported only changing the needle when it got dull. Three-hundred and eighty-two (96%) stated they re-used the same bag of fluids. From the 382 owners who reused fluid bags, 152 (40%) kept and used the same bag of fluids for 2–3 weeks, whereas 86 (23%) used the same bag of fluids for less than 1 week, 33 (9%) used the same bag of fluids for 4–6 weeks and six (2%) used the same bag of fluids for more than 6 weeks; 98 (26%) responded with an answer other than those options listed and seven (2%) did not answer the question.
Of the 399 respondents administering fluids, the majority of owners reported that learning to give SC fluids very easy/quite easy or okay (Table 1). Of the 248 owners with no prior experience administering fluids, a slim majority of owners reported they did not receive resources (written, websites, YouTube videos, other) from their veterinarians to help them learn how to administer fluids. Of those owners who had no prior experience with SC fluids, most reported finding it very easy, quite easy or okay to learn, regardless of whether they received resources from their veterinarians or not (Table 2). Similarly, most owners who did have prior SC experience found it very easy, quite easy or okay to learn to administer regardless of whether they received resources or not (Table 3)
Reported difficulty level of learning subcutaneous (SC) fluid administration

Data are n (%)
Reported difficulty level of learning subcutaneous fluid administration among owners with no prior experience

Data are n (%).
Reported difficulty level of learning subcutaneous fluid administration among owners with prior experience

Data are n (%)
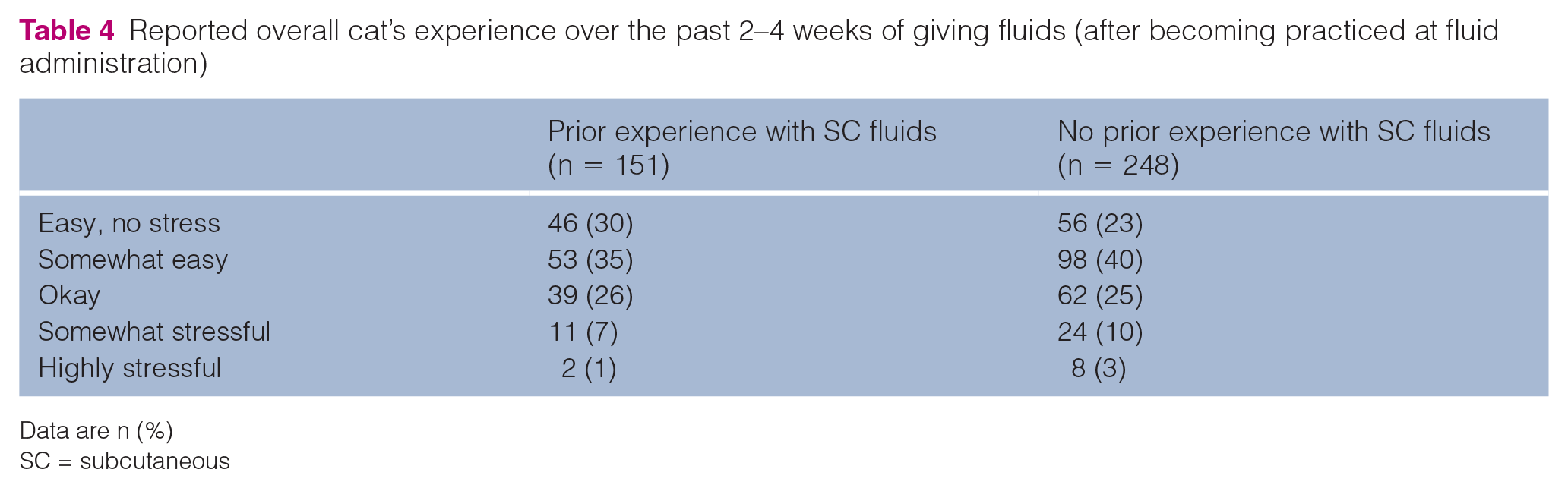
After becoming practiced at fluid administration (ie, in the past 2–4 weeks), the majority of owners reported that the experience of giving SC fluids was somewhat easy for their cats, easy/no-stress experience for their cats, or an okay experience for their cats (Table 4). Owners with prior SC fluid experience appeared more likely to report the experience as easy/no stress for their cats and less likely to report it was highly stressful for their cats. After becoming practiced at fluid administration, 155/399 (39%) respondents administering fluids reported their overall experience with administration to be easy/no stress, somewhat easy or okay for them (Table 5). Owners with prior SC fluid experience appeared more likely to report the overall experience as easy/no stress for them and less likely to report it was highly stressful for them.
Reported overall cat’s experience over the past 2–4 weeks of giving subcutaneous (SC) fluids (after becoming practiced at fluid administration)
Data are n (%)
Reported overall experience for owners in giving fluids

Data are n (%)
SC = subcutaneous
One-hundred and thirty-three (27%) owners who took the survey found out about it via Facebook, 117 (24%) found out about it via email from a cat professional/veterinary professional, 30 (6%) found out about it from a veterinary practice, 22 (5%) found out about it from a cat professional website, 22 (5%) found out about it via word-of-mouth, five (1%) found out about it via Twitter and 157 (32%) found out about it elsewhere. This question allowed multiple responses (486 responses from 468 owners).
Discussion
Overall, owners reported administering fluids as a relatively low-stress experience for both themselves and their cats. A large majority of owners (85%) said it was either an easy, somewhat easy/no stress or okay experience for them, and a large majority (89%) reported that the experience was easy/no stress, somewhat easy or okay experience for their cats. Lack of prior experience did not seem to impact the stress of the experience. Owners with no prior experience in administering fluids reported very similarly, with 84% identifying it as either easy, somewhat easy/no stress or okay for themselves, and 88% saying the same for their cats.
Although the majority of owners in this survey reported relatively positive experiences for SC fluid administration it is important to remember that for a subset of owners and cats the experience was negative. Additionally, it was somewhat surprising that IRIS stage 1 cats and a large percentage of IRIS stage 2 cats were receiving SC fluids. Considering the amount of time that a cat with IRIS stage 1 CKD may potentially have to receive fluid therapy, it is important for veterinarians to determine which cats may benefit from SC fluid therapy, discuss the balance between quality of life and treatments, and work with owners on technique to ensure the procedure is tolerated as well as possible.
The surveys indicated that several strategies were utilized in an effort to improve tolerance of the procedure. Of those owners who reported warming fluids prior to administration, 83% viewed it as an effective strategy to increase tolerance. Owners also very consistently (74%) said that the length of time of administration affected tolerance. To a lesser extent, almost 6/10 owners said that giving treats for positive reinforcement to their cats after administration increased tolerance. Needle size was also reported by most owners to have an effect on tolerance. These four strategies seemed to be the most effective at increasing tolerance and helping owners decrease stress associated with fluid administration. Owners in the study were less decisive with regard to whether or not they felt the amount of fluids administered affected tolerance. This suggests that the amount of fluids may not be as much of a factor related to tolerance as those stated in the above paragraph; however, it is potentially difficult to consider the length of time of administration as a different variable from the amount of fluids given as they are related. Additionally, many owners may not have been given advice to explore fluid volume as a variable.
A large majority of owners felt that it was either easy or okay to learn to administer fluids, even if they had not administered fluids before, but more research is needed to determine what factors contributed to the relative ease of learning. This study did find that although a majority of veterinarians currently do not provide resources, such as brochures, videos, etc, those owners who were provided resources did not necessarily find it any easier to administer fluids than those who said they did not receive resources, even among those with no prior experience giving fluids. In fact, inexperienced owners who reported receiving resources from their veterinarians were slightly more likely to find fluid administration difficult. This suggests that owners likely learned the most from in-person appointments with hands-on training over additional resources received. Veterinarians who do provide additional resources should be careful not to allow these resources to become a substitute for in-person, kinesthetic training and education.
Even though nearly all (95%) participants in this study reported talking to their veterinarians about fluid administration, it was revealed that several owners do not follow one or more recommended protocols for SC fluid administration. When educating owners, veterinarians should provide clear guidance and direction about the importance of regularly changing needles and fluid bags, as well as the benefits of rotating the location of needle insertion.
As with any survey, there is no way to ensure adequate understanding of the survey questions by all respondents. While a great deal of effort was put into crafting the questions and responses as clearly as possible, there did seem to be some questions and/or responses that were not fully understood by some respondents. The authors anticipated this and included an ‘Other, please specify’ or similar response on several questions, which allowed them to interpret and categorize appropriately. However, there were likely some respondent reporting errors due to misunderstandings.
One significant limitation of this study is that the responses received were only from those with access to technology, namely a computer and the internet. Therefore, the responses received may not be representative of the full population. Additionally, a voluntary survey like this is more likely to garner participation from more diligent owners of cats with CKD and less representative of disengaged owners. Further, some results highlighted follow-up questions that were not part of the current survey and should be addressed in future studies. Most notably, additional questions could have been asked with regard to the amount and type of client education that owners received from their veterinarians and what owners found to be the most valuable for learning. Finally, it is possible that owners may have answered some questions in a way they felt they should, thus influencing the answers to their questions. However, this did not always seem to be the case when it came to noting how often bags and needles were reused. Placebo effect may have also played a part, especially when answering if warming fluids was beneficial, as this is hard to assess critically.
Conclusions
A majority of owners gave positive feedback about their ability to learn and administer SC fluids to their cat with CKD; however, for some it was very difficult. Owners reported several strategies that they felt improved tolerance of fluid administration. Overall, balance between quality of life and interventions should be taken into consideration for feline patients with CKD and SC fluid protocols should be tailored to the preference of the cat for best possible long-term success.
Supplemental Material
Click here for Supplementary Appendix A
Online questionnaire
Footnotes
Acknowledgements
The authors wish to thank the owners and veterinarians who promoted this survey online.
Author note
The results were previously presented as a poster abstract at the 2016 ACVIM Annual Forum, Denver, Colorado, USA, and at the 2016 WSAVA Congress, Cartegena, Columbia.
Supplementary material
Appendix A. Online questionnaire.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
