Abstract
Practical relevance:
Dermatophytosis (ringworm) is the most important infectious and contagious skin disease of cats in shelters. Its importance relates to the fact that it can affect all cats, but tends to affect those which would otherwise have good chances for adoption. Although many diseases in shelters fit this description, dermatophytosis is of particular significance because of associated public health concerns.
Clinical challenges:
Disease management in animal shelters is challenging because new animals are frequently entering the population, numerous animals are often housed together, and resources are almost always limited.
Global relevance:
Outbreaks of dermatophytosis occur worldwide and no animal shelter is completely shielded from possible introduction of the disease into the population.
Audience:
This article offers a flexible stepwise approach to dealing with a known or suspected outbreak of dermatophytosis in an animal shelter. It is based on the authors’ experiences spanning more than a decade of responses and/or consultations. While primarily aimed at veterinarians involved in shelter medicine, the principles largely apply to other group-housing situations, such as catteries and breeding establishments.
Aims:
The goals in dealing with a potential dermatophytosis outbreak are to ascertain if the ‘outbreak’ is actually an outbreak, to develop a shelter-specific outbreak management plan and to implement a long-term plan to prevent recurrences.

Why such concern over ‘outbreaks’?
Dermatophytosis is the most common contagious and infectious skin disease of cats. 1 It is of particular importance in shelters because it is highly contagious; affects kittens, which are one of the most sought-after populations in a shelter; and may also be a public health concern. This article will focus primarily on outbreaks caused by Microsporum canis, which is the most common cause of dermatophytosis in cats, 1 and the most commonly isolated pathogen from cats in shelters. Infections with Microsporum gypseum, Trichophyton species and Microsporum persicolor have been reported,2,3 but do not present as treatment challenges in shelters.2,3 M gypseum is a geophilic dermatophyte; infections are inflammatory and cure rapidly with appropriate treatment. Trichophyton species infections are uncommon in cats but, when found, tend to be seen on the ear margins or face of adult cats in winter and/or in kittens and cats surrendered from a farm or stable where large animals are housed.4,5 In the authors’ experience, infections with Trichophyton species cure rapidly with appropriate treatment.
The term ‘outbreak’ refers to the occurrence of a disease in excess of what is normally expected. Thus, even a single case of a contagious disease that has been absent from a population or not previously diagnosed could be considered an ‘outbreak’. With respect to dermatophytosis in shelters, any suspicion should be taken seriously as this disease may evoke a negative response in staff that is disproportionate to the pathogenesis of the disease. This stems from the fear of contagion, environmental contamination and the potential for human infection. In the shelter setting, the fear of increased euthanasia is also a concern. Although dermatophytosis is a self-limiting, non-fatal disease, the resources required to treat numerous animals may not be available. Hence, rapid response to even a single possible infection can be life-saving for the cat and may prevent a widespread outbreak.

STEP 1: Initial contact (day 1)
An oft-heard, but erroneous, statement in feline dermatology is: ‘It’s ringworm until proven otherwise.’ Because of this, any skin lesion not easily explained is assumed to represent dermatophytosis. When contacted about a suspected ‘outbreak’, therefore, the most important task is to collect information to confirm the disease is present – or, at least, that a plausible explanation exists.
Since many initial contacts are via telephone or email, the focus is on obtaining answers to some key questions, as outlined in the box below. 6 Before asking any questions, however, it is helpful to allow the caller to describe the circumstances that led them to believe the disease is present, as this may reveal information that might not otherwise be shared; the caller may, for example, reveal that they are not certain they are interpreting fungal cultures properly. It is important to note that the caller may or may not have all of this information readily available and several conversations may be necessary.
It is possible that the answers to these questions will confirm the shelter has a true out-break in many cats. Or, findings may indicate that only one or two cats are affected and the disease is contained. Conversely, the interview may lead to a suspicion that there is, in fact, no outbreak. Frequently, in the authors’ experience, misinterpretation of diagnostic tests (eg, color change in dermatophyte test medium [DTM]) has led to the assumption of an outbreak.
STEP 2: Shelter staff first response (day 1 or 2)
If the level of suspicion for an outbreak is very high based on initial discussions, it may be important to alter the flow pattern for cats entering a shelter in such a way that unexposed cats are protected from exposure. This is commonly referred to as a ‘clean break’ and is described in Step 5.
If additional information is needed before making a risk assessment, the following steps are recommended to contain or limit any further spread of disease pending collection of that information and/or a site visit.
– Remove any unnecessary items or clutter from hallways or wards to facilitate cleaning.
– Mechanically remove debris via sweeping or vacuuming, then scrub the hard or non-porous surfaces with a detergent until they are visibly clean and rinse with clean water. This is referred to as a ‘hard clean’. Organic debris must be removed and surfaces pre-cleaned before disinfection, as most disinfectants will not work in the presence of organic debris. Rinsing of the surface with water is necessary because detergent residue may inactivate some disinfectants. Excess water should be removed from the surface prior to application of a disinfectant; the surface does not need to be dry but puddles of water should not be present.
– Apply a disinfectant to properly prepared (ie, visibly clean) surfaces and allow a 10 min wetting time. This is the minimum time stipulated on most disinfectant labels to ensure sporicidal activity.


High levels of sanitation are important first lines of defense against the spread of disease in shelters, and should be maintained daily. A common misconception, and often a cause of great concern to staff, is that dermatophyte spores multiply in the environment. It is important to emphasize that this is not the case and that the source of spores is naturally infected hairs. Hence, the most important part of disinfection and prevention of the spread of spores is continual mechanical removal using routine cleaning methods. 7
The term ‘one step’ is found on many commercial products listed as sanitizers or disinfectants and refers to a ‘pattern’ of use. In order to obtain this label claim, the product needs to be able to clean a lightly soiled surface and sanitize it in one wipe. Studies to support efficacy claims as a ‘sanitizer’ require documentation of 99% efficacy within 5 mins against selective bacteria (eg, Staphylococcus), but not fungal spores. 8 Careful reading of products labelled as ‘one step’ cleaners will reveal recommendations to apply only to surfaces that have been thoroughly cleaned (ie, pre-cleaned to remove organic material).
If organic debris is removed, many common disinfectants with label claim for efficacy against Trichophyton mentagrophytes are effective against M canis when used liberally and allowed a 10 min contact time. 9 Commonly used disinfectants in shelters include accelerated hydrogen peroxide, enilconazole, sodium hypochlorite and potassium peroxymonosulfate.
STEP 3: Assessment of suspect animals (days 1 to 3)
As with any suspected disease occurrence, animals that are presumed to be affected require veterinary assessment.
Whenever possible, it is best to avoid moving cats throughout the facility. This will minimize spread of infectious material in the event that true infection is present. The risk of cross- contamination can be minimized by examining each cat on a clean towel or fresh newspaper, which is then put aside for washing or disposed of properly, with the surface being disinfected prior to examining the next cat. Everyone involved in animal examinations should wear gowns and gloves, making sure to change gloves between cats; gowns should be changed between wards and rooms or after handling a highly suspect cat. If known, cats should be examined in reverse order of likelihood of infection (ie, those thought to be free of infection should be examined first).
Cats are first examined in ‘white light’ (ie, room light or with a flash light if room lighting is poor). This is followed by examination with a Wood’s lamp (Figure 1). Although the sensitivity of this test is considered low, 1 the authors have found Wood’s lamp examination to be very useful because it will often identify lesions or fluorescing hairs not seen in room light or help confirm suspicion in cats with obvious skin lesions. Fluorescing hairs are often masked by crusts, so it is important to gently avulse crusts to look for these hairs. It is also important to spread the hair to find positively fluorescing hairs (Figure 2). In addition to examining obvious lesions, it is common to find fluorescing hairs on the face and near the ears in early infections (Figure 3). In kittens, fluorescing hairs are often found in the axilla.
Hairs for direct examination can be collected into red top serum tubes or in the center fold of paper that is then placed in an envelope or self-sealing plastic bag. On-site examination of hairs is easily performed using mineral oil; clearing agents are not needed.


Wood’s lamp positive interdigital hairs. These hairs were not seen at all and, therefore, not noted to be infected/suspicious
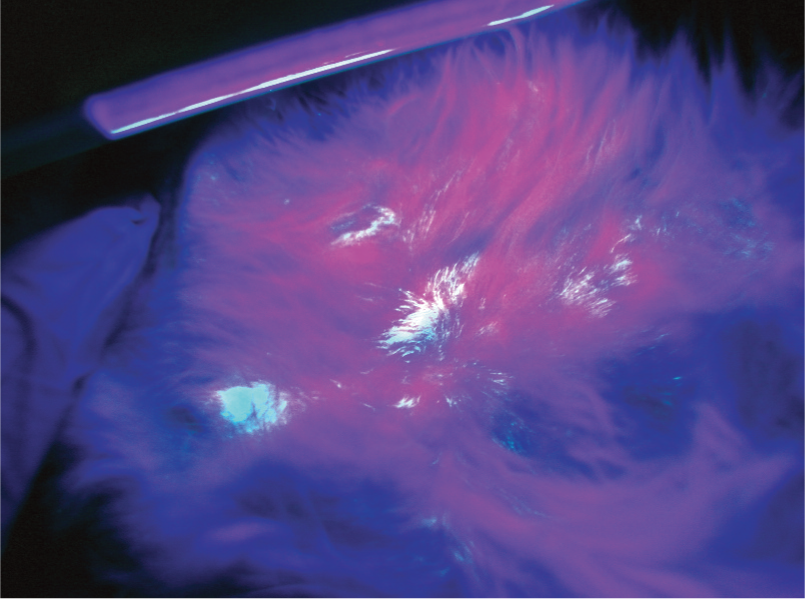
Wood’s lamp positive hairs. These hairs were only found after spreading the overlying hair

Wood’s lamp positive lesion on examination in room light
Samples for fungal culture should be collected from cats with suspected inflammatory lesions, cats that have been in close contact with lesional cats, and cats that have been in suspected contaminated environments. Ideally, collect as many samples as possible from suspect cats from these categories. It is important to sample the face and within the ear canal, as these are early infection sites. Areas with visible lesions should always be sampled last. If large numbers of cats are involved it may be more important to confirm a trend than to identify each affected individual since it may not be possible to evaluate every cat in one day.
The question as to what is an adequate number to sample needs to be considered on a case-by-case basis and the practitioner will need to rely on their clinical acumen to make this determination. For example, the disease may be confirmed by examination of highly suspect cats. However, if the staff cannot identify such cats then the focus may be the most likely affected populations (ie, kittens and newly admitted cats) or cats with obvious skin lesions. It is not possible to be prescriptive here – this is the ‘art’ of clinical practice.

Any newly discovered highly suspect cat should be moved to isolation. Otherwise, all cats are kept in their location until Step 8.
In the authors’ opinion, if suspicion of dermatophytosis is high, it is not necessary to obtain fungal cultures simply to document contamination of the environment, which is expected. Rather, environmental sampling is important to assess the efficacy of cleaning because of the risk of false-positive fungal culture results. Environmental samples should only be obtained during this step if staff members have had adequate time to clean and disinfect; otherwise it is advisable to wait until appropriate cleaning has been done.
STEP 4: Planning the response (days 3 to 4)
Dermatophytosis can often be confirmed via positive Wood’s lamp examination and positive direct examination of fluorescing hairs while confirmatory fungal cultures are pending. Indeed, it would be very unusual for there to be an outbreak of M canis dermatophytosis without any Wood’s lamp positive cats. Thus the information collected in Steps 1 and 3 is usually sufficient in terms of making a preliminary plan.
Plans are situation-specific. The plan for managing an outbreak that is contained to a newly admitted litter of kittens will clearly differ from a plan to manage endemic dermatophytosis.
Even though dermatophytosis is a treatable and curable disease, not all shelters will treat infected cats. Some shelters may elect to treat some and euthanize others. Other shelters may elect to euthanize all cats with documented infections. Only by working with the shelter to institute appropriate screening at intake and educating staff on how to both identify suspect cats and make a definitive diagnosis can future outbreaks be prevented or identified sooner.

What is the capacity of the organization to respond to the disease outbreak?
What is the overall impact on the animals, resources, operations and public image of the facility?

What will the shelter do to prevent a recurrence or future outbreaks?
It is likely that many cats present to shelters already infected with dermatophytosis. Effective screening is a strong preventive measure since cases identified at intake or before other critical movement (eg, to foster homes, off-site adoption areas, adoption centers or within the facility) can be managed much more easily and are less likely to cause spread of disease than unrecognized cases.
STEP 5: Establishment of a ‘clean break’ (days 2 to 5)
If shelter intake will continue, a clean break should be implemented quickly. As mentioned earlier, clean break is a term used to describe a strategy that alters the flow pattern for cats entering a shelter in such a way that unexposed cats are protected from exposure to disease.
At the time of surrender, in addition to routine admission procedures, cats are carefully examined for skin lesions in room light and with a Wood’s lamp. If cats are low risk (no lesions and Wood’s lamp negative) and other-wise deemed healthy, they are diverted into a designated housing area (ie, clean break area) that has been disinfected and is separated from other areas housing exposed or potentially exposed (‘dirty’) cats in the shelter. These cats become the adoptable population until the outbreak is contained. All other cats are diverted into housing for cats in the shelter. The question of what happens to truly infected cats depends on the shelter’s planned response. Cats can leave the clean break area if adopted or if they need medical care. The only cats that can enter the clean break area are newly admitted cats, as illustrated below.

Establishing and maintaining a clean break strategy contains an outbreak while the shelter mobilizes for the remaining steps of the response and allows for safe continuation of admission. Depending on the severity of the concerns regarding exposure, varying degrees of separation can be considered. If concerns are minimal, then the designated clean break area may continue to hold animals considered to be low risk for contagion. However, if the risk is high, even cats that may have been exposed must be removed from the clean break area; in these circumstances, the ‘clean’ areas should be reserved for new unexposed animals entering the facility as determined by intake screening (examination, Wood’s light examination, examination of fluorescing hairs). Shelter resources will determine if fungal cultures are performed on all new admissions or subpopulations (eg, Wood’s lamp positive cats, kittens, Wood’s lamp negative but lesional cats). Separate equipment and staff should be dedicated to the clean break area.
In order to maintain the clean break area, intake staff members need to be trained to screen incoming animals for suspicious clinical signs. An unidentified infection in an incoming animal could contaminate the clean break area. Animals that are suspect on screening should not be admitted into the clean break area. If necessary, an intermediate area may be established to allow time to confirm or clear suspects before deciding on which pathway they should follow. This area would house cats with pending fungal cultures/direct examinations and/or cats with skin lesions that cannot otherwise be explained.
STEP 6: Screening of the entire suspect population (days 3 to 5)
Screening should include thorough examination in both room light and with a Wood’s lamp, direct examination of fluorescing hairs, and selective use of fungal cultures. Since fungal cultures will be the greatest cost, other than investment in veterinary care, strategic and selective culturing can be the difference between an affordable response and over-whelming resource expenditure.
Fungal culture remains the ‘gold standard’ for diagnosis of dermatophytosis in individual animals. Shelter-wide screening can provide a global overview of the culture status of cats and provides a safety net by helping to identify infected animals with lesions that were missed on examination. In shelter practice, the cost of an in-house fungal culture rarely exceeds the cost of other point-of-care diagnostics (eg, feline leukemia and feline immuno deficiency virus testing) that are frequently performed routinely before adoption.

Arguments against shelter-wide fungal culturing are many. First, unless the number of cats in the shelter is very small or the organization’s resources almost inexhaustible, shelter-wide screening of cats may simply not be feasible. Secondly, to be most useful, fungal cultures need to be examined daily so, ideally, are performed in- house (Figure 5). This requires dedicated space and (potentially multiple) trained staff. Thirdly, it is a misconception that culturing the population of cats is ‘better’ or ‘time saving’. In every case, an investment must be made in thorough evaluation of the skin and hair coat. Fungal culture data can only be interpreted in conjunction with knowledge about the presence or absence of skin lesions. So, even if shelter-wide screening is possible, cats still need to be examined. Fourthly, even though this is a disease of public health concern, evidence is lacking that culturing without a concurrent examination that screens for lesions is a superior method of protecting staff compared with rapid identification of suspect animals via examination, appropriate isolation, cleaning, proper staff hygiene and use of gowns and gloves. Finally, there is no evidence-based data to prove that shelter-wide screening versus a more targeted approach results in a better outcome for the cats or the shelter.

Positive M canis growth on DTM using the toothbrush culture technique. These images show examples of ‘too-many-to-count’ colonies on a plate. (a) This is typical of a culture from a truly infected cat, but equally may indicate poor compliance with cleaning. Note that individual colonies can still be seen.

Early growth of M canis from the culture plate shown in Figure 4b. Note the ends of the hyphae are thickened and sporulation is just starting. This is a classic finding to recognize when reading fungal cultures
Resource-sparing approaches to fungal culture screening of at-risk cats
There are two common resource-sparing approaches to fungal culture screening of at-risk cats. Both involve intensive examination of cats in room light and with a Wood’s lamp, to detect subtle/early lesions that are so easily missed on examination in room light, and microscopic examination of fluorescing hairs.
In the first approach, fungal cultures are reserved for exposed cats that have negative Wood’s lamp examinations, regardless of lesion status. The assumption here is that lesional, Wood’s lamp positive cats with microscopically confirmed infections are ‘truly positive’ and fungal culture is not necessary. This approach is dependent on the skill of the examiner and could potentially lead to treatment of some cats that are not truly infected.
In the second approach, fungal cultures are reserved for cats with skin lesions. In this approach, positive Wood’s lamp examinations and confirmatory direct examinations can be used to identify cats with strong enough suspicion to start treatment pending fungal culture results.
In-house fungal cultures are strongly recommended because daily examination can rapidly detect culture-positive status of cats.
STEP 7: Use of clinical data to group cats based on risk (days 5 to 6)
Although definitive culture results are usually not available for 7–14 days, by this point in the investigation there should be a great deal of information to hand on which to base treatment decisions.
Essentially, it should be possible to group cats as follows:
Lesions present, and Wood’s lamp negative/awaiting culture results.
Daily examination of cultures may reveal signs of fungal culture growth as early as 3–4 days (Figure 6), which may be sufficient for a cat to be moved to a different risk category.

This culture plate shows a classic presentation of early growth of M canis on DTM, and, pending microscopic confirmation, would be considered suspicious. The darkly pigmented colony is a contaminant
STEP 8: First cat ‘shuffle’ and assessment of environmental cleaning (days 5 to 6)
Step 8 is the first of two cat ‘shuffles’, in which cats are moved within the facility so that they are housed according to the risk groups they were sorted into in Step 7. (A second shuffle [Step 10] is often needed once further information or confirmation is available.) When working with staff in shelters, the authors prefer to talk in terms of cat ‘shuffle’ rather than ‘segregation’ because it has a more positive connotation. It is also a more accurate description of what actually happens!
Since open, unused housing space is often not available, ‘shuffling’ may involve cleaning and disinfecting many cage areas or wards if large numbers of cats need to be moved from one area to another. Truly infected/high risk cats should ideally be physically separated in a ward or room away from the rest of the population. If a dedicated room is not available a separate area within a room/ward can be created, though this approach is associated with a greater risk of spread of dermatophytosis.
In group housing set-ups, at-risk cats (ie, exposed but not lesional) should be physically separated from low-risk cats. If animals are housed in individual housing units, and separate rooms are not available, at-risk animals may be identified via cage cards. These animals would be cared for after non-suspect animals. This requires training and compliance to be successful but minimizes cage shuffling, which may be stressful for cats. One practical solution is to hang numbers on the cages that correspond to the order in which cats should be cared for.

It is critical to assess the efficacy of environmental decontamination after cleaning and disinfecting because fomite carriage can contribute to positive culture results, making it difficult to interpret screening and/or monitoring cultures. If preliminary culture results are showing >10 colony-forming units per plate (cfu/plate), this is compatible with poor compliance with cleaning protocols and/or the presence of actively infected cats. It is important to remember that the results being assessed may be from 1 week prior. If environmental cultures are showing heavy contamination of spores, cleaning protocols on the day of sampling were inadequate and should be reviewed and corrected as needed. The most common weakness is an insufficient hard clean (see pages 408–409). If repeat fungal cultures are showing a decrease in the number of cfu/plate this is indicative of decontamination. The ultimate goal is no growth of pathogens.
STEP 9: Evaluation of fungal culture results (days 7 to 14)
Shelters not performing fungal cultures in-house should work with laboratories that will report preliminary culture results at least every 7 days. They need only report whether the culture is suspect, positive or negative and the number of cfu/plate up to 10. While not an onerous task, it is critical to be sure that the laboratory knows how to properly inoculate a fungal culture plate when a toothbrush sample is submitted. Often laboratories will simply select hairs to culture rather than stab the bristles into the culture plate. If the bristles are not stabbed onto the surface of the plate, cfu/plate cannot be reported.
Ideally, as discussed, fungal cultures should be processed in-house (see accompanying article). A search of the organization’s volunteer base may well reveal individuals with laboratory expertise who are more than able and willing to monitor these cultures. Alternatively, training volunteers to carry out daily screening of cultures, looking for red media color change and characteristic fungal growth, can save enough staff time to make in-house processing possible.
An important advantage of performing in-house cultures is that it allows the plates to be observed daily; results are available more rapidly and cfu/plate can be counted. In the authors’ approach to outbreak management, the number of cfu/plate, combined with the presence or absence of lesions, is used for the final determination of risk assessment and decisions about treatment, as follows:

Three examples of M canis-positive fungal plates from cats determined to be culture positive due to fomite carriage. Note the low numbers of cfu/plate. On re-examination these cats were still lesion-free and Wood’s lamp negative. In all three cases, repeat fungal cultures were negative
STEP 10: Second cat ‘shuffle’ as culture results are confirmed (days 7 to 14)
Over the next 7 to 14 days, as fungal culture results become available, it will be necessary to shuffle cats again as their risk/infection status is confirmed. In the laboratory of one of the authors, 99% of culture-positive infected cats were identified within 14 days (KA Moriello, University of Wisconsin, unpublished data 2003–2013). Although the recommendation is to hold plates for 21 days, in a shelter situation treatment decisions can be made by day 14 if there is growth of M canis.
Plates can be discarded once they are positive and the number of cfu/plate has been recorded. Plates should also be discarded if there is rapid and heavy overgrowth of contaminants; it may be necessary to re-culture some cats. All plates from cats under treatment or that show no growth on screening should be held for 21 days.
It is important to emphasize that each time cats are moved, they should be examined for skin lesions and re-examined with a Wood’s lamp.
STEP 11: Long-term response plan
Institution of a screening program at shelter intake is the key to preventing future out-breaks in the shelter. Even if treatment is not within the organization’s capabilities, screening at intake is a crucial and very cost-effective tool to prevent future outbreaks.

When resources allow, providing the option of treatment for at least some animals can be a preventive tool in itself. When staff know treatment may be an option, identification and reporting of problems improves.

Summary Points
The stepwise response outlined in this article intended to be used as a guide when there is a suspected outbreak in a shelter.
The steps are summarized as follows:
STEP 1: Initial contact/interview to collect information to determine if the suspicion is valid
STEP 2: Staff action to contain spread: isolate suspect cats, limit movement of cats, enhance cleaning
STEP 3: Veterinary assessment of suspect cats to confirm true disease
STEP 4: Planning and discussion of the response options with the organization
STEP 5: Diversion of the flow of new admissions to protect them from the exposed population
STEP 6: Cost-effective screening of the entire population
STEP 7: Use of available information to group cats based on risk: truly infected/high risk, suspicious/moderate risk or non-lesional/low risk
STEP 8: ‘Shuffling’ of cats based on risk and assessment of environmental cleaning
STEP 9: Evaluation of available fungal culture results
STEP 10: ‘Re-shuffling’ of cats based on new information (ie, fungal culture results)
STEP 11: Long-term response to prevent/minimize outbreaks
Responses are situation-specific and some steps may be combined on the same day and/or may not be needed in a particular situation.
Footnotes
Funding
The authors have received no specific grant monies from any funding agency in the public, private, commercial or not-for- profit sectors for the preparation of this review article. Research studies cited in the article were funded by extramural research grants (Maddie’s Fund [![]() ], Winn Feline Foundation, Companion Animal Grant–University of Wisconsin) or unrestricted gifts for research on feline dermatophytosis.
], Winn Feline Foundation, Companion Animal Grant–University of Wisconsin) or unrestricted gifts for research on feline dermatophytosis.
Conflict of interest
The authors declare no conflict of interest.
