Abstract
The efficacy of radioiodine treatment of feline hyperthyroidism is well established; however, limited information is known about owners’ perceptions or experiences of radioiodine. This study aimed to examine factors that influence owner treatment choices and their opinions following radioiodine. Surveys were sent to owners of cats referred for radioiodine treatment between 2002 and 2011 (radioiodine group; 264 cats) and owners of non-radioiodine-treated hyperthyroid cats seen at first-opinion practices (control group; 199 cats). The response rate was 67.0% (310 returned: 175 radioiodine, 135 control). Of 135 controls, 72 (53.3%) were unaware of radioiodine as a treatment option. Owners of cats ⩾15 years old and uninsured cats were less likely to pursue radioiodine. Cost of treatment, travel distance, potential human or animal health risks and waiting periods for radioiodine had a low impact on owners’ treatment choice. Owners reported a moderate level of concern about treatment hospitalisation length, which included (158 respondents) the possibility of the cat being unhappy 130 (82.3%), owner missing the cat 102 (64.6%), inappetence 50 (31.6%), other pets missing the cat 32 (20.3%), development of co-morbid disease 28 (17.7%) and side effects 25 (15.8%). Owners assessed their cat’s quality of life on a scale of 1 (very poor) to 10 (excellent), as 4 (4) (median [interquartile range]) pre-radioiodine (134 respondents) and 9 (2) post-radioiodine (131 respondents). Of 132 respondents, 121 (91.7%) were happy with their decision to choose radioiodine. The results of this questionnaire may assist veterinarians in addressing common owner concerns when discussing radioiodine as a treatment option for hyperthyroidism.
Introduction
Hyperthyroidism, secondary to functional adenomatous hyperplasia, is the most common feline endocrinopathy. Treatment options include those that require long-term management and monitoring of efficacy (anti-thyroid medications or iodine-restricted diet; Hill’s y/d) and those that aim to be curative (surgical thyroidectomy or radioiodine).
Treatment options differ in their potential efficacy, side effects, costs, ease of administration and availability, and some cats will receive several different treatments over time.1–4 Radioiodine is considered the ‘gold standard’ treatment; however, not all owners pursue this option.2,5 The advantages of radioiodine include a high cure rate, treatment of ectopic tissue, lack of requirement for anaesthesia and longer survival times compared with medical treatment.1,6 Additionally, with long-term medical management, hyperfunctional thyroid tissue continues to enlarge, which may, potentially, increase the risk of malignant transformation of benign disease. 7 The disadvantages of radioiodine include limited availability and waiting times owing to a small number of centres offering this treatment in the UK, cost, the potential for iatrogenic hypothyroidism and the requirement for confinement in hospital after treatment.2,8,9
Clear communication between veterinarians and owners regarding potential treatment options, risks, costs and outcomes is important to optimise management for patients and clients; however, relatively few studies have examined cat owners’ perceptions or experiences of veterinary treatment.5,10–21 A survey of owners of medically managed hyperthyroid cats found that 18.9% of owners would have liked more explanation of treatment and 30.6% would have liked more information on long-term management. 5 Relatively limited access to, or experience of, radioiodine treatment by UK general practice veterinarians may influence their recommendations to clients.
To our knowledge, only one published study has examined owners’ experiences and opinions of medical treatment of hyperthyroid cats, but none have examined owners’ perceptions or experiences of radioiodine treatment. 5 The aims of this study were to identify factors that influenced cat owners’ decision to treat their hyperthyroid cats with radioiodine, and to evaluate their experiences and opinions following radioiodine.
Materials and methods
Questionnaire design
An owner questionnaire was formulated comprising 20 questions in four sections: pet signalment, prior knowledge of radioiodine, assessment of factors influencing the owners’ decision to choose radioiodine and experiences of radioiodine treatment (summarised in Figure 1). A pilot of 20 questionnaires was conducted to assess survey design and the survey was then revised. A linear analogue scale of 1–10 was used for questions regarding factors that may have influenced treatment choice (1 = not concerned or no impact on their decision; 10 = extremely concerned or a large impact on their decision) and quality of life (QoL) (1 = very poor QoL; 10 = excellent QoL). All other questions required ‘tick-box’ and/or ‘free-text’ answers. A copy of the questionnaire is available in the Supplementary material. Questionnaires were posted in December 2011 with pre-paid return envelopes included. Non-responders were posted a card reminder after 2 weeks and a replacement questionnaire and pre-paid return envelope after 4 weeks. Entry into a prize draw for supermarket vouchers was offered as an incentive to maximise the response rate.

Flow diagram summarising questionnaire sections and topics used to collect information about the perceptions and experiences of radioiodine treatment from owners of hyperthyroid cats. Group 1 included control group cats whose owners were not aware of radioiodine as a treatment option; group 2 included control group cats whose owners were aware of radioiodine, but did not pursue it; group 3 included cats that were referred for radioiodine, but did not receive it; and group 4 included cats that received radioiodine
Control population: definition and selection
Non-radioiodine-treated hyperthyroid cats seen at five first-opinion UK practices within the referral catchment area of The Feline Centre at Langford Veterinary Services, University of Bristol (control group, 199 cats) were recruited as controls. Controls were selected from hospital records between January 2002 and October 2011 (the first 20–60 hyperthyroid cats were selected alphabetically) and included cats that had previously received medical and/or surgical or no treatment. Cats diagnosed with hyperthyroidism within the previous month were excluded because owners may not have had sufficient time to consider treatment options.
Case population: definition and selection
All hyperthyroid cats referred for assessment for radioiodine at The Feline Centre between January 2002 and October 2011 (radioiodine group, 264 cats) were selected for inclusion in the study. Cats treated within the previous month were excluded to allow owners time to assess the cat’s response to treatment. Cats treated with high-dose radioiodine (1110 MBq) for thyroid carcinoma were excluded because different treatment costs and hospitalisation requirements would have applied to these cases.
Respondents were further sub-divided into four groups: group 1 included control group cats whose owners were not aware of radioiodine as a treatment option; group 2 included control group cats whose owners were aware of radioiodine, but did not pursue it; group 3 included cats that were referred for radioiodine, but did not receive it; and group 4 included cats that received radioiodine. The term ‘control group’ in this study refers to combined groups 1 and 2, and the ‘radioiodine group’ refers to combined groups 3 and 4.
χ2 tests were used to analyse associations between categorical data collected for control and radioiodine groups in relation to age of the cat, breed, owners’ prior knowledge of radioiodine, pet insurance status, and outcome of, and satisfaction with, radioiodine treatment. The Mann–Whitney test was used to analyse associations between ordinal data collected for control and radioiodine groups in relation to the impact of radioiodine costs, concerns about potential human health risks, the impact of travel distance to a radioiodine centre, concerns about hospitalisation, QoL before and after treatment, and treatment outcomes. The Wilcoxon signed rank test was used to compare medians between QoL scores of cats before and after radioiodine treatment. Data analysis was performed using SPSS 19. P values of <0.05 were considered significant. Non-normal data distribution was assumed.
Results
The overall response rate for the questionnaire was 67.0% (310/463); the response rate for the radioiodine group was 66.3% (175/264) and for the control group was 67.8% (135/199). Thirteen questionnaires were returned because the addressee was no longer at that address. The number of respondents for each sub-group were as follows: group 1 – 72, group 2 – 63, group 3 – 41 and group 4 – 134.
Signalment (questionnaire section 1)
Signalment data for control and radioiodine group cats at the time of diagnosis of hyperthyroidism are summarised in Table 1. Control group cats were significantly more likely to be pedigree breed cats (P = 0.04) and to fall into the ⩾15 years age group (P <0.001) than radioiodine group cats.
Signalment data reported by questionnaire respondents for all cats at the time of diagnosis of hyperthyroidism

The age of six cats and the breed of one cat were not reported
Significant differences are shown in bold
Owner knowledge of radioiodine treatment (questionnaire sections 1 and 2)
Of 135 control group cats, 72 (53.3%) respondents had not heard of radioiodine as a treatment option for hyperthyroidism (group 1). Of all respondents who had heard of radioiodine (groups 2–4), 80/238 (33.6%) respondents reported that they had knowledge of radioiodine prior to their cat’s diagnosis of hyperthyroidism. Sources of previous knowledge are summarised in Table 2.
Sources of previous knowledge of radioiodine treatment reported by questionnaire respondents in a study of owners’ perceptions and experiences of radioiodine treatment for feline hyperthyroidism (groups 2–4)

More than one answer was possible
Factors that may affect treatment decision (questionnaire sections 2 and 3)
Respondents in groups 2–4 scored, on a scale of 1–10, the level of impact or concern they felt in relation to several factors that may have influenced their decision to choose radioiodine when considering treatment options. Results for these questions and comparisons between groups are summarised in Table 3.
Respondents’ scores* for the level of impact or concern they felt in relation to several factors on their decision to choose radioiodine when considering treatment options for their hyperthyroid cat (groups 2–4)

NA = not applicable
Scores from a scale of 1–10; 1 = no impact/concern; 10 = extremely concerned or a large impact
Of 238 respondents (groups 2–4), 129 (54.2%) had no pet health insurance to cover treatment of hyperthyroidism. Group 3 and 4 cats were significantly more likely to have insurance, 96 (54.9%) of 175 cats compared to 13 (20.6%) of 63 group 2 cats (P <0.001).
Group 3 and 4 respondents had several concerns regarding hospitalisation length, which are summarised in Table 4.
Concerns about hospitalisation length for radioiodine treatment reported by questionnaire respondents in a study of owners’ perceptions and experiences of radioiodine treatment for feline hyperthyroidism (groups 3 and 4)

More than one answer was possible
Several reasons were given by group 3 and 4 respondents for choosing to pursue radioiodine treatment, which are summarised in Table 5.
Reasons for pursuing radioiodine treatment reported by questionnaire respondents in a study of owners’ perceptions and experiences of radioiodine treatment for feline hyperthyroidism (groups 3 and 4)

More than one answer was possible
Of 158 group 3 and 4 cats assessed for treatment, 134 (84.8%) received radioiodine (group 4). Reasons for not receiving radioiodine given by owners of 18 group 3 cats included co-morbid disease (13), elected thyroidectomy owing to long radioiodine waiting period (1), elected thyroidectomy because no ectopic thyroid tissue was identified by scintigraphy (1), owner felt that their cat would be frightened by hospitalisation (1), the cat died before radioiodine treatment (1), and the cat had a mild total thyroxine elevation and was managed medically (1). Co-morbid diseases reported included neoplasia (5), cardiomyopathy and/or congestive heart failure (4), chronic kidney disease (2) and feline immunodeficiency virus (1).
Experiences of radioiodine treatment and QoL (questionnaire section 4)
Of 134 group 4 respondents, 132 reported hospitalisation lengths as follows: 3 weeks by 43 (32.6%), 5 weeks by 36 (27.3%), ‘other’ length by 33 (25.0%) and ‘uncertain’ by 20 (15.2%). Of group 4 cats, owner concerns about hospitalisation length were not significantly different when the 3 or 5 week categories were compared (P = 0.354).
Following radioiodine, 129 group 4 respondents reported response to treatment as 98 cats (76.0%) were cured, nine cats (7.0%) had a partial response, seven cats (5.4%) responded but had recurrence of hyperthyroidism at a later date, and 15 cats (11.6%) were reported to have had no response to treatment. Five respondents did not answer this question.
Group 4 respondents assessed their cat’s QoL on a scale of 1 (very poor) to 10 (excellent) as 4 (4) (median [interquartile range]) pre-radioiodine and 9 (2) post-radioiodine (Figure 2). There was a significant difference between QoL scores before and after radioiodine treatment (P <0.001). The median QoL score after radioiodine treatment was significantly different when ‘response to treatment’ categories were compared (cured; partial response; responded but had recurrence; and no response) (P <0.001). When the response to treatment categories were regrouped as cured or not (partial response; responded but had recurrence; and no response), a significant difference between groups remained: cured 9 (2) and not cured 8 (3) (P <0.001).
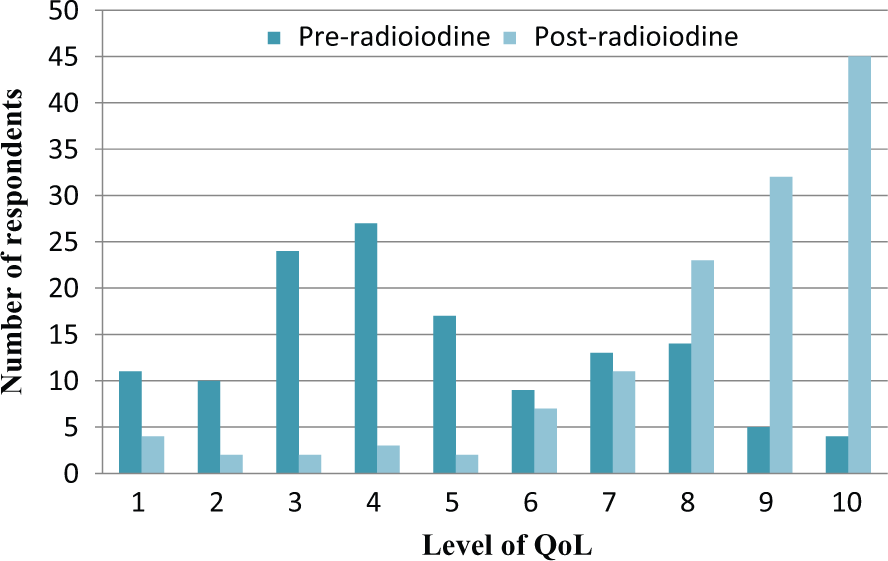
Quality of life (QoL) scores (score based on a scale of 1–10: 1 = very poor QoL; 10 = excellent QoL) for hyperthyroid cats before (n = 134) and after (n = 131) radioiodine treatment reported by questionnaire respondents in a study of owners’ perceptions and experiences of radioiodine treatment for feline hyperthyroidism (group 4)
Of 132 group 4 respondents, 104 (78.8%) were ‘happy with their decision to treat their cat with radioiodine and the outcome of treatment’, 17 (12.9%) were ‘happy with their decision to use radioiodine, but were unhappy with the outcome’ and 11 (8.3%) ‘regretted their decision to treat their cat with radioiodine’. Respondents whose cats were not cured (partial response; responded but had recurrence; and no response) were significantly more likely to report that they were either ‘happy with their decision to use radioiodine, but were unhappy with the outcome’ or that they ‘regretted their decision to treat their cat with radioiodine’ (P <0.001). Respondents who were ‘happy with their decision to treat their cat with radioiodine and the outcome of treatment’ were significantly more likely to report a higher QoL score for their cat after radioiodine treatment than those respondents that were either ‘happy with their decision to use radioiodine, but were unhappy with the outcome’ or those that ‘regretted their decision to treat their cat with radioiodine’ (P = 0.04).
Discussion
Four management options for hyperthyroidism are currently available, each with advantages and disadvantages that need to be considered by both the owner and managing veterinarian. Formulation of a treatment plan requires consideration of both patient and owner factors, and while the efficacy of radioiodine is well established, limited information is known about owners’ perceptions or experiences of this treatment.2,5,6
Sex and breed distributions in this study were similar to previous reports.2,22 Control group cats were significantly more likely to be ⩾15 years old at diagnosis of hyperthyroidism compared with radioiodine group cats. Reasons for this may include reluctance of owners of older cats to pursue referral and radioiodine, reluctance of veterinarians to recommend radioiodine or the presence of co-morbrid disease. Eight cats were reported to be 3–6 years old at diagnosis; however, hyperthyroidism is rare in young cats.2,22 These ages may have been reported incorrectly owing to the questionnaire’s retrospective nature and estimated ages for cats acquired from shelters. Control group cats were significantly more likely to be pedigree breed cats than radioiodine group cats; however, the reason for this is unclear, although confounding from another variable is likely.
Of control group respondents, 53.3% reported no knowledge of radioiodine, highlighting a gap in owners’ knowledge of possible management options. Similarly, a survey of hyperthyroid cat owners found that 29.7% of owners of medically managed cats had only been offered oral anti-thyroid medication as a treatment. 5 Reasons for this may include poor recall or understanding by owners of treatments offered, veterinarians offering other options first, veterinarians assessing that radioiodine was not appropriate for an individual cat or lack of veterinarian experience with referral for radioiodine therapy. A survey of UK general practitioners found that 58.9% of respondents agreed with the statement ‘radioiodine is the gold standard treatment for hyperthyroidism’; however, 55.7% had no experience of referral for radioiodine. 23
Several factors that may influence treatment decisions made by hyperthyroid cat owners were evaluated. Respondents in groups 2–4 reported that concerns about potential human health risks, costs and travel distance had a low impact on treatment decisions. However, group 2 respondents were significantly less likely to have pet insurance than respondents in groups 3 and 4. The significance of this was unclear owing to questionnaire design; however, it is possible that financial concerns did affect either the owner’s decision to pursue radioiodine or the veterinarian’s decision to recommend radioiodine. For example, social desirability bias may have influenced respondents’ answers to questions about the cost of treatment. A survey of UK general practitioners found that their preferred hyperthyroid treatment was long-term management with oral anti-thyroid medication, followed by thyroidectomy and then radioiodine, although this was influenced by cost, with radioiodine the preferred treatment option if cost considerations were excluded. 23
Of group 3 and 4 respondents, 59.9% reported that they pursued radioiodine on veterinary advice; however, 64.3% pursued radioiodine because they personally considered it the best treatment. Veterinarians have an important role in owner education; however, the results of this study suggest that many owner decisions were reached without recommendation and that 33.6% of respondents knew about radioiodine before their cat was diagnosed with hyperthyroidism (Table 2). Owing to the retrospective nature of data collection, however, the accuracy of this figure must be treated with caution.
Many group 3 and 4 respondents were concerned about the length of hospitalisation required. Interestingly, the level of concern of group 4 respondents, while considering treatment options, did not vary with their cat’s actual required hospitalisation length. Common concerns were that their cat would be unhappy and that the owner would miss their cat. These concerns highlight the importance of the human–animal bond, and the need for information and reassurance from veterinarians providing radioiodine services. The hospitalisation period at The Feline Centre reduced from 5 to 3 weeks in 2007, and in 2012 to 2 weeks (additional requirement for 2 weeks of indoor confinement following discharge). The post-treatment confinement length is determined by local radiation protection supervisors, which accounts for regional variations.
The overall radioiodine cure rate reported by group 4 respondents was 81.4%, with 7.0% reporting a partial response. There are several possible reasons for this lower cure rate compared with other publications.2,6,8,9 Owners whose cats did not respond or had a partial response may have been more motivated to complete the questionnaire. Cats may take weeks to months after radioiodine to achieve maximal thyroxine reduction, that is, cats treated in the preceding 6 months may not yet have achieved their maximal thyroxine reduction and may have been reported as partial or non-responders by owners. 6 Recall bias was also suspected to have contributed; of 15 cats that respondents reported had no response, review of available clinical records showed a complete response in one and partial responses in two. Finally, at the time of survey, a fixed low-dose radioiodine protocol was used at The Feline Centre (111 MBq SC), but a variable dosing schedule is now used, which may be associated with higher first time cure rates. 24
As anticipated, many group 4 respondents reported a significant improvement in their cat’s QoL scores following treatment and that they were happy with their decision to treat their cat with radioiodine. Owners of cats that were not cured following treatment were more likely to report lower QoL scores and, not surprisingly, were also more likely to be dissatisfied with their decision to use radioiodine. Interestingly, of those respondents who regretted their decision to use radioiodine, 3/11 reported that this was because their cat developed co-morbid disease following treatment rather than because radioiodine treatment failed.
Limitations of this study include its retrospective nature, which may have resulted in recall bias. Non-response bias was not assessed and might have been present as questionnaire respondents might have been more likely to have held strong positive or negative perceptions and/or experiences of radioiodine than non-responders. Control cat owners who did not return the questionnaire may have been less likely to have heard of radioiodine and may have been less motivated to participate than those who had heard of radioiodine. The year of hyperthyroidism diagnosis was not recorded in this study, and this variable could not be included in the analysis. Questions relating to QoL were subjectively, and retrospectively, assessed by owners, and may not have accurately reflected their cat’s QoL. There were study limitations related to the questionnaire design, with respondents progressively finishing the survey at different stages. In particular, group 2 respondents were not asked to explain why they did not pursue radioiodine treatment.
Further research into the perceptions of hyperthyroid cat owners of the available treatment options may include investigation of why some owners select radioiodine and others do not, despite being aware of it as a treatment option. Multivariate analysis, to control for confounding factors, of potential risk factors, such as concerns about costs, length of hospitalisation and insurance status, may provide further information about the decision-making of cat owners.
Conclusions
The results of this study suggest that owners of hyperthyroid cats are often unaware of radioiodine as a treatment option. Owners of cats ⩾15 years old and uninsured cats were less likely to pursue radioiodine. The cost of treatment, travel distance, potential human or animal health risks, and waiting periods for radioiodine all had a low impact on owners’ treatment choice. Owners reported a moderate level of concern about treatment hospitalisation length. The majority of owners reported an improvement in QoL following treatment. Overall, 91.7% of owners were happy with their decision to treat their cat with radioiodine. The results of this questionnaire may assist veterinarians in addressing common owner concerns when discussing radioiodine as a potential treatment option for feline hyperthyroidism.
Supplemental Material
Click here for Supplementary Appendix
A copy of the questionnaire used in this study
Footnotes
Acknowledgements
We thank the cat owners who completed the questionnaire, and also Caroline Blundell, Owen Davies, Zuzana Jacmenikova, Kate Murphy, Juliet Pope, Severine Tasker and Steve Tasker for assistance with the recruitment of control cat owners.
Supplementary material
A copy of the questionnaire used in this study is available online as Appendix 1.
Conflict of interest
The authors do not have any potential conflicts of interest to declare.
Funding
This questionnaire was funded by The Langford Trust. Lara Boland’s position was funded by International Cat Care (formerly the Feline Advisory Bureau). Jane Murray’s position is funded by Cats Protection. Catherine Bovens’ position was funded by MSD Animal Health.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
