Abstract
Feline aural inflammatory polyps are benign growths originating from the tympanic cavity or the Eustachian tube. They usually occur in young cats, which present either signs of otitis externa and otitis media, or respiratory signs, depending on the direction of polyp growth. Neurological signs are also reported. Simple traction and ventral bulla osteotomy (VBO) are the most common techniques used for treating this condition in cats; corticosteroids are recommended to reduce risk of recurrence given the inflammatory nature of the disease. The most common complications after treatment are Horner’s syndrome, polyp recurrence and facial nerve paralysis. The aim of this report is to describe the per-endoscopic trans-tympanic traction (PTT) technique for treating feline aural inflammatory polyps and to report the short- and long-term follow-up of this procedure. PTT allowed resolution of the aural inflammatory polyps in 94% of cats during a mean long-term outcome of 19 months. Three cats (8%) developed Horner’s syndrome immediately after the PTT procedure, which resolved within a few weeks, and five cats had polyp recurrence (13.5%). Only two cats had a poor outcome and were diagnosed with chronic otitis media at 22 months, and chronic otitis media and polyp recurrence at 46 months after the PTT procedure, respectively. PTT was shown to be an effective technique for treating aural inflammatory polyps and registered fewer neurological complications (8%) than VBO (57–81%) or simple traction (43%), and a recurrence percentage (13.5%) similar to VBO (0–33%) and much lower than traction alone (57%).
Introduction
Feline aural inflammatory polyps are the most common non-neoplastic pedunculated lesions that arise from the mucosa of either the tympanic cavity (aural inflammatory polyps) or the auditory tube (middle ear polyps). Polyps arising from the auditory tube can grow in both directions (middle ear and nasopharyngeal polyps). Feline inflammatory polyps usually occur in young cats, and they can cause either upper respiratory or aural clinical signs that do not resolve with a conservative medical regimen.1–5
Clinical signs observed in cats with inflammatory polyps are usually gradual in onset and chronic in nature, and depend on the definitive site of the polyp growth. Aural inflammatory polyps results in chronic otitis externa, with head-shaking and otorrhoea. Horner’s syndrome, head tilt, ataxia and facial paralysis may also be observed with middle and inner ear involvement.1–4,6,7 The most common clinical signs in cats with nasopharyngeal polyps are nasal discharge, stertorous breathing and sneezing.1–4,7 Dysphagia, megaesophagus, regurgitation, pulmonary hypertension and severe dyspnoea have been rarely reported.1–3,8,9
Both conventional and video-otoscopy can show a smooth pink-coloured mass arising in the ear canal or protruding from the middle ear cavity and occupying the ear canal, while rhinopharyngeal polyps can be confirmed on digital palpation, rostral traction of the soft palate or retrograde rhinoscopy, and they appear as smooth, pale pink, roundish lesions partially or totally occluding the rhinopharynx.1,2,4,5
The aetiology of feline inflammatory polyps is unknown. It is unclear whether polyps are congenital in origin or a response to an inflammatory process from chronic viral infections, or a consequence of chronic upper respiratory or middle ear inflammation.2–5,7,10
Histopathologically, feline inflammatory polyps consist of well-vascularised fibrous connective tissue covered by stratified squamous or columnar epithelium; inflammatory cells, primarily lymphocytes, plasma cells and macrophages are present within the stroma and are especially dense in the submucosal areas of the tissue.1–4
Methods used to remove aural inflammatory polyps are simple traction, ventral bulla osteotomy (VBO), traction after vertical ear canal incision and laser ablation. Total ear canal ablation with or without lateral bulla osteotomy has also been reported for aural polyp removal.
VBO has been suggested as the treatment of choice when involvement of the tympanic cavity is observed.1–4,6,11–18
Regardless of the removal technique, postoperative complications such as Horner’s syndrome, vestibular syndrome, facial nerve paralysis, chronic otitis media and interna can occur; these complications can be temporary or permanent.2–4,11–14
Use of corticosteroids after removal seems to reduce the risk of recurrence given the inflammatory origin of the feline inflammatory polyps.2,4,11
The aim of this work was to evaluate the feasibility and the efficacy, and to report the short- and long-term outcome, of a minimally invasive technique for treating feline aural polyps called per-endoscopic trans-tympanic traction (PTT).
Materials and methods
Medical records of cats referred and diagnosed with aural polyps, presented between March 1999 and July 2010 at the School of Veterinary Medicine, University of Milan, Italy, were reviewed.
Inclusion criteria were a complete medical record, including signalment, history and clinical signs, radiological findings, video-otoscopy, histological examination and a minimum follow-up of 6 months' duration. Thirty-seven cases fulfilled the inclusion criteria.
Radiological scoring was established as follows: ‘normal’ when no changes were detected; ‘mild’ when an increased radiopacity in the horizontal canal and/or within the bulla was noted; ‘moderate’ when an increased radiopacity in the horizontal canal and/or within the bulla and/or thickening of the septum and/or changes in the tympanic bulla contour (enlargement, thickening or irregularity) were noted; ‘severe’ when increased radiopacity in the horizontal canal and/or within the bulla, changes in the bulla contour and/or thickening of septum and/or alterations of the petrous bone were noted.
The cases that presented with concurrent nasopharyngeal polyps were treated using the trans-oral traction-avulsion technique. 1
PTT technique description
After cleaning and flushing the ear canal with a 0.9% saline solution and/or ceruminolytic agent (squalene), the cat was positioned in lateral recumbency with the affected side upper most.
Under endoscopic vision, the polyp was grasped with a curved mosquito forceps, then a traction–torsion manoeuvre was applied; when rupture of the polyp occurred the residual portion of the polyp was completely removed under endoscopic visualisation with the use of small biopsy forceps or Volkmann curettes. The dorsolateral compartment of the middle ear was curetted by means of an ear knife, an ear loop and small pinch biopsy forceps under direct visualisation. When necessary, the septum of the tympanic cavity was disrupted for better cleaning of the ventromedial compartment of the bulla. Local irrigations with refrigerated 0.9% saline solution were used to reduce and control the bleeding. All the procedures were carried out by CM.
All cats received methadone hydrochloride (Metadone Cloridrato; Molteni), 0.5–1.0 mg/kg intramuscularly before the procedure, but post-procedure pain medication was not necessary in any case. In all cases, the samples collected were submitted in buffered formalin 10% for histopathological evaluation.
Short-term outcome was assessed on clinical re-examination, conventional otoscopy or video-otoscopy between 1 and 2 months after the PTT procedure at the teaching hospital.
Long-term outcome was assessed on clinical re-examinations, conventional otoscopy or video-otoscopy at the teaching hospital or at the referring veterinarian surgery and via telephone interviews.
The short- and long-term outcome was classified as follows: ‘excellent’ when normal clinical and otoscopic evaluation was obtained, ‘good’ when clinical and otoscopic signs of otitis externa and persistence of neurological signs detected at initial presentation were noted, and ‘poor’ when clinical and otoscopic signs of ongoing otitis media or recurrent polyp and persistence of neurological signs detected at initial presentation were observed.
On telephone interviews, the persistence of neurological signs was not considered by the owners to be affecting the quality of life of their animals, but for us were considered to be affecting the clinical outcome.
The presence of an intact, but opaque, ear drum after PTT was considered to be a normal finding at re-examination because it is part of the healing process after rupture. The presence of stenotic ear canal was not considered a PTT sequela when already detectable during the initial video-otoscopy.
Results
Signalment and clinical signs
The study group was composed of 37 cats. The cats were aged between 5 and 192 months, with a mean age of 47.5 months. There were 17 males (10 intact and seven neutered) and 20 females (17 of which were spayed). Thirty-one cats were domestic shorthairs; the other cats belonged to different breeds (two Persian cats, one Devon Rex, one Norwegian, one Siamese and one Maine Coon).
The duration of clinical signs varied from 1 to 48 months, with a mean duration of 8.04 months. Prior to presentation, all cats had received different treatment, predominantly topical therapy, without success.
At admission, all but three cats had clinical signs of otitis externa, including otic discharge (purulent: 25 cats; ceruminous: seven cats; mixed: two cats), head-shaking (nine cats) and ear-scratching (six cats). During physical examination, standard otoscopy allowed visualisation of the mass in the horizontal portion of the ear canal in 13 cats. In four cats, the polyp was visible without the aid of the scope.
Neurological signs were identified in 11 cats. Head tilt was present in eight cats, ataxia in seven cats, Horner’s syndrome in four cats and facial nerve paralysis in three cats. One cat only had neurological signs at presentation, which consisted of left head tilt, Horner’s syndrome and ataxia. Another cat was reported to have had previous signs of vestibular syndrome, but these were not detectable at admission.
Signs of obstructive upper airway disease were recorded in 10 cats, but only six cats were diagnosed with a concurrent nasopharyngeal polyp and one cat with concurrent idiopathic lymphoplasmacytic rhinitis based on histopathological examination of nasal biopsies. Eight cats presented nasal discharge (seven purulent, one serous), six cats stertorous breathing and three cats sneezing. In two cats a mass displacing the soft palate was detected on digital palpation. Two cats with aural and nasopharyngeal polyps had only upper respiratory signs at presentation.
Dysphagia was present in four cats, and regurgitation and lingual dysfunction in one cat.
Imaging findings
Radiological changes of the bullae were present in 36 cats and absent in one. Three cats had bilateral involvement of the tympanic bullae; two cats were diagnosed with bilateral aural polyps and one cat with an aural polyp and contralateral otitis media.
Main radiological findings were cloudiness in the middle ear cavity (34), increase radiopacity of the horizontal ear canal (25), thickening of the tympanic wall (25), alterations of the petrous bone (12), enlargement of the bulla (11), thickening of the septum (seven), irregularity of the bulla wall (four) and thickening of the ear canal (two). According to the radiographic scoring, two cats were graded as ‘normal’, seven as ‘mild’, 16 as ‘moderate’ and 12 as ‘severe’ (Figure 1). All six cats with nasopharyngeal polyps showed increased radiopacity of the rhinopharynx.
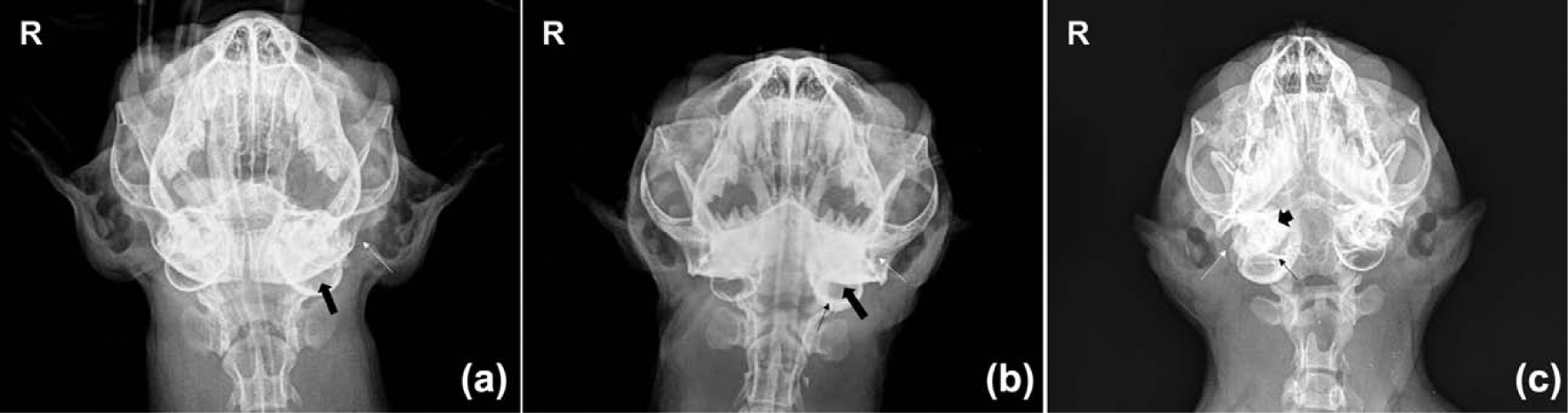
Radiological scoring of feline aural inflammatory polyps (10° rostrocaudal ventrodorsal view of the tympanic cavity). (a) Note the increased radiopacity of the left ear canal (white arrow) and middle ear cavity (thick black arrow) (case classified as ‘mild’); (b) Note the increased radiopacity of the left ear canal (white arrow) and middle ear cavity (thick black arrow), and the thickening of the bulla contour (thin black arrow) (case classified as ‘moderate’); (c) Note the increased radiopacity of the right ear canal (white arrow) and middle ear cavity, the severe bulla enlargement, the thickening of the septum (thin black arrow), and remodelling and the petrous bone involvement (short black arrow) (case classified as ‘severe’). The contralateral ear in every image is normal (courtesy of M Di Giancamillo)
During video-otoscopy, the polyp stalk was visible within the middle ear cavity in six cats, five of which had a proliferated mucosa lining the middle ear cavity. Two cats had a stenotic horizontal ear canal. In three cats, otitis media was diagnosed in the contralateral ear.
In all cats but one, a smooth pinkish to white in colour and rounded-to-oval mass was detected in the ear canal or the middle ear cavity. In the other cat, the mass did not have the typical appearance of a polyp and endoscopic biopsies were performed; in this cat, PTT was carried out after histopathological confirmation of an inflammatory polyp.
Post-PTT treatment and immediate complications
Thirty-nine PTT procedures were performed in 37 cats (39 ears) for removal of aural inflammatory polyps and in six cats PTT was combined with trans-oral traction avulsion of the concurrent nasopharyngeal polyp. The appearance of the middle ear cavity after the PTT procedure is shown in Figure 2.

(a) Endoscopic appearance of a feline aural inflammatory polyp: note the presence of a pinkish round mass occluding the horizontal ear canal. (b) Free ear canal after per-endoscopic trans-tympanic traction and at the top of the image the white aspect of the tympanic cavity after curettage; a moderate quantity of blood is still notable around the tympanic cavity and along the ear canal. On the left side within the bulla there is an artefact from saline solution reflecting the light of the endoscope
All but two cats were given postoperative antibiotic treatment, with either amoxicillin/clavulanic acid 20 mg/kg q12h (Synulox; Pfizer) in 13 cats or enrofloxacin 5 mg/kg q24h (Baytril; Bayer) in 23 cats. The choice of antibiotic was based on real-time cytological swab of the ear canal: amoxicillin/clavulanic acid and enrofloxacin were chosen when cocci bacteria and rods bacteria, respectively, were identified.
Twenty-one cats received concurrent corticosteroid treatment in the postoperative period with prednisolone (Vetsolone; Bayer) 1 mg/kg q12h tapered down over a 3 week period.
Three cats developed Horner’s syndrome immediately after PPT, which resolved spontaneously within a few weeks postoperatively (2–6 weeks).
Histopathology
In all cats, the histopathological examination was consistent with an inflammatory polyp.
Short- and long-term outcomes
Overall, five recurrences (13.5%) were recorded. Three recurrences occurred in the short-term outcome and the cats had normal, moderate and severe radiological scoring, respectively; the other two recurrences occurred in the long-term outcome, and both cats had a moderate radiological scoring. Of the five cats that had polyp recurrence, three were not discharged with corticosteroids. The recurrences were spread over the 11 years of the case series and therefore were not likely to be affected by the experience of the surgeon.
The short-term outcome was considered ‘excellent’ in 11 cats, ‘good’ in 21 cats and ‘poor’ in five cats. In the cats with excellent short-term outcome, two had an opaque ear drum and the other nine had normal examination. In the cats with good short-term outcome ceruminous otorrhoea was found in 20 cats, an opaque ear drum in eight cats, head-shaking in three cats, ear-scratching in two cats, head tilt in three cats and partial stenosis of the horizontal canal in two cats.
In the five cats with a poor outcome, three cats had recurrent aural polyps 1.0, 1.5 and 2.0 months after the PTT procedure and were treated again with PTT; two cats had an excellent long-term outcome at 24 and 6 months after the first PTT, and one cat had a poor long-term outcome because of aural polyp recurrence and chronic otitis at 46 months after the first PTT procedure. The other two cats were diagnosed with otitis media at 1 and 2 months after the PTT procedure. Both cats were treated with antibiotics based on culture and sensitivity results and corticosteroids, with a good long-term outcome in one cat at 15 months after the PTT procedure and a poor long-term outcome in the other cat at 22 months because of the presence of chronic otitis media.
The long-term outcome ranged from 6 to 60 months, for a median follow-up of 19.6 months. The outcome was considered ‘excellent’ in 20 cats, ‘good’ in 15 cats and ‘poor’ in two cats. In the cats with excellent long-term outcome, 14 had normal examination and six had an opaque ear drum. In the cats with good long-term outcome, nine showed ceruminous otorrhoea, four persistent head tilt, three occasional episodes of ataxia, two ear-scratching and one an opaque and thickened ear drum. The two cats with poor long-term outcome already had a poor outcome in the short-term outcome and showed signs of chronic otitis media at 22 months and chronic otitis media and polyp recurrence at 46 months after PTT, respectively.
Other occurrences during long-term follow-up were recurrent aural polyp in one cat 5 months after PTT that was treated again with PTT with an excellent outcome 9 months after the first PTT procedure; recurrent rhinopharyngeal polyp in one cat 4 months after PTT and traction avulsion procedures, which was again treated by a traction avulsion technique without further recurrences; diagnosis of contralateral aural polyp in one cat 13 months after the PTT procedure, which was treated by PTT with a good long-term outcome for both ears at 24 months after the first PTT; and ongoing otitis media in one cat 3 months after PTT, which was successfully treated with antibiotics based on culture and sensitivity results with a good long-term outcome at 60 months after PTT.
Of the five cats that had polyp recurrence, three were not discharged with corticosteroids. All the cats that were diagnosed with otitis media after PTT were discharged with corticosteroids. Both cats with poor short- and long-term outcomes had received corticosteroids.
Discussion
The aim of this study was to evaluate the feasibility, efficacy, and the short- and long-term outcomes of PTT as a minimally invasive technique for the treatment of aural inflammatory polyps in cats.
In our case series, signalment with no gender predisposition, clinical findings, imaging findings and histopathological findings were similar to those that have been previously reported, but domestic shorthair cats were over-represented. 2–4,11,14,19
Only in one cat was histological examination of biopsy samples performed before proceeding with PTT because of an atypical appearance of the mass in the ear canal. Biopsy sampling and histological confirmation should be performed before traction or surgery when certainty of the presence of an aural polyp is not straightforward.
In this study, 94% (35/37) of cats were successfully treated with PTT. However, as reported in other studies, some clinical signs of ear disease, such as ceruminous otorrhoea, head-shaking, ear-scratching and the persistence of a degree of neurological signs in cats that were exhibiting neurological signs at presentation, were recorded during follow-up.2,4,8,11–14
One cat developed a contralateral polyp 13 months after PTT. This has only been reported once. 8 The cat was successfully treated with PTT and had a good long-term outcome.
In the veterinary literature, traction alone and VBO are the most common used techniques for the treatment of aural inflammatory polyps. VBO has been recommended as the treatment of choice when middle or inner involvement is present. Short-term complications, such as Horner’s syndrome and polyp recurrence, are the most frequent complications, and Horner’s syndrome is usually temporary. Facial nerve paralysis and otitis interna have been rarely reported.2–4,11–14
Immediate post-PTT procedure complications were temporary Horner’s syndrome in three cats (8%), and resolved a few weeks after the procedure. This percentage is lower than what has been reported for VBO (57–81%) or traction alone (43%) in other studies.11–14
None of the cats in this study developed temporary or permanent facial nerve paralysis after PTT.11,14
In this study, three cats were diagnosed with otitis media within 3 months of the PTT procedure being performed (8%), but only two cats were diagnosed having chronic otitis media (2%) at 22 and 46 months on long-term outcome. To the best of our knowledge, chronic otitis media has been addressed in other studies as a possible long-term complication, but no percentages are available or deducible.2,4,11
Of the six cats that had concurrent nasopharyngeal polyps, one cat that did not received corticosteroids had a recurrent nasopharyngeal polyp 4 months after traction and was again treated with traction with no further recurrence. These findings are in agreement with what has been previously reported.1–5,11,14
Overall in this study, recurrence of an aural inflammatory polyp after PTT occurred in five cats (13.5%), and three cats had recurrence in the short-term outcome and two cats in the long-term outcome at 5 and 46 months, respectively, after PTT. This last cat was considered to have a poor outcome according to the outcome assessment, but had a normal follow-up up to 40 months after PTT, and for us it is questionable whether a diagnosis of an aural polyp after 4 years should be considered a recurrence or a new polyp. Two recurrences occurred in two cats that received corticosteroids and two in cats that had not received corticosteroids. These results are in agreement with what has been reported previously.2–4,11
The percentage of recurrence for PTT (13.5%) is lower than that reported for traction alone (57%) and similar to the percentages reported for VBO (0–33%).7,9,11–14 VBO offers surgical exposure of the bulla, which allows extirpation of the mucosal lining the tympanic cavity.1,3,4,6 PTT allowed visualisation of the stalk in six cats and curettage of the bulla in all cases thus increasing the success rate of the single traction procedure.
In this study, it was not possible to trace all the anaesthesia records to evaluate the mean duration of PTT, but the minimum duration time available was 45 mins and the maximum was 2.5 h. Although minimally invasive and effective, PTT can be time-consuming.
Conclusions
PTT is an effective and minimally invasive technique for the treatment of aural inflammatory polyps in cats. PTT should be performed after a learning curve has been accomplished and by an experienced endoscopist because it allows visualisation and cleaning of the dorsolateral compartment of the bulla, which contains important neurological structures that should not be damaged.
Footnotes
Acknowledgements
We thank Dr Anna Di Donato for data collection from the paper records in the archives.
Conflict of interest
The authors do not have any potential conflicts of interest to declare.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
