Abstract
Background:
Pediatric intensive care unit (PICU) nurses are regularly exposed to high-stress situations, particularly when dealing with patient death and postmortem care. While much attention has been paid to the physical demands of their role, the emotional and psychological impacts of these experiences are often overlooked. Understanding how nurses regulate their emotions in such high-pressure environments is essential for improving their well-being and providing better care.
Objective:
This study aims to explore the emotional burdens faced by PICU nurses, particularly in the context of patient death and postmortem care. It examines how nurses regulate their emotions in response to these experiences and how these emotional responses affect their professional roles and personal lives.
Methods:
The study was conducted at Zhejiang Children’s Hospital. A total of 15 PICU nurses, with at least two years of experience, participated in semi-structured, in-depth interviews. The data were analyzed using reflexive thematic analysis, allowing for a detailed exploration of emotional experiences, coping strategies, and the emotional impact of postmortem care.
Results:
The analysis revealed four major themes: (1) emotional and physical strain of patient loss; (2) fear and unease in postmortem care; (3) navigating professionalism amid emotional turmoil; and (4) impact on parenting and career choices.
Conclusions:
PICU nurses face significant emotional challenges when dealing with patient death and postmortem care. These emotional burdens affect not only their professional roles but also their personal lives. Developing effective emotional support systems and training for nurses can enhance their emotional regulation and improve both their well-being and the quality of care they provide.
Key Message
This study examines the emotional impact of postmortem care on pediatric intensive care unit nurses, revealing significant psychological and physical distress. It underscores the importance of targeted emotional support, enhanced training, and coping strategies to improve nurses’ well-being and sustain quality care in high-stress clinical settings.
Introduction
The role of nurses in pediatric intensive care units (PICUs) involves not only delivering high-level medical care but also offering emotional and psychological support to critically ill children and their families. The emotional toll on health care professionals, especially those working in environments where death is frequent, is substantial. Research indicates that the psychological burden experienced by nurses in such high-pressure settings is multifaceted, impacting their emotional, physical, and professional lives.1,2 Among these challenges, the emotional and psychological effects of caring for children at the end of life, and particularly during postmortem care, remain a critical issue. 3
The experience of death, especially the death of a child, is uniquely distressing. Nurses often form deep emotional connections with their pediatric patients, and these connections can result in intense feelings of grief, sadness, and helplessness when the patient dies. 4 These emotions are compounded by the nurses’ roles as both caregivers and witnesses to these traumatic events, often placing them in a difficult position between emotional engagement and professional duty. As found in the literature, the grieving process among PICU nurses is not only related to the loss itself but also to the ongoing emotional impact of their caregiving roles.5,6
Studies have shown that postmortem care is one of the most emotionally taxing aspects of a nurse’s work in the ICU.7–9 The involvement of nurses in this process often triggers profound emotional reactions, particularly when the patient is a child. 10 Nurses must navigate a complex emotional landscape, balancing their personal grief and professional obligations. The concept of “professional bereavement,” which refers to the emotional burden that health care workers face in the aftermath of a patient’s death, has been explored in previous research, showing that the grief experienced by nurses can lead to emotional exhaustion and, in some cases, professional burnout. 11
However, despite the documented emotional toll, there is limited research exploring the specific experiences of nurses in pediatric postmortem care, particularly in ICU settings. This gap in the literature underscores the need for further investigation into how emotional stress impacts nurses’ physical and psychological health, and how these effects may influence their professional practices. Additionally, understanding how nurses cope with these experiences and how they manage the emotional strain is critical in providing better support systems and interventions aimed at improving nurses’ well-being.
This study aims to fill this gap by exploring the emotional and physical burdens experienced by PICU nurses in postmortem care. It focuses on the grief and emotional challenges they encounter, the physical manifestations of stress, and the implications for both their professional practice and personal lives. Through qualitative interviews, the study provides insights into the lived experiences of nurses working in high-stress environments and contributes to a deeper understanding of the emotional health of pediatric critical care nurses.
Methods
Research design
This study adopted a qualitative design grounded in emotion regulation theory, 12 which explores how individuals manage their emotions in response to stress and challenges. This theory is particularly relevant for understanding how PICU nurses cope with the emotional burdens arising from patient death and postmortem care. It focuses on how nurses regulate emotions such as grief, anxiety, and emotional exhaustion in a high-stress environment. Additionally, it examines how these emotional regulation processes affect their professional roles and personal lives, including relationships with family. By applying this theoretical framework, the study aims to gain insights into the emotional coping mechanisms of PICU nurses and their impact on well-being and resilience.
Setting
The study was conducted in the PICU of a tertiary children’s hospital in China. In this unit, the nurse-to-open-bed ratio is approximately 1.42:1. During night shifts, each nurse typically provides care for four to five critically ill patients. Shift scheduling follows a rotating pattern, with one night duty every five to six days. Nurses usually require two days of rest after night duty, which reduces the continuity of nurse–patient assignments, although scheduling practices aim to maintain consistency whenever possible.
Postmortem care in this setting is carried out according to established hospital procedures. After the death of a patient, the primary nurse conducts body care and may invite parents to participate at the bedside. If parents decline, the nurse completes the procedure independently. Once the body is cleansed and dressed, hospital logistics staff transport it to the morgue. Parents are generally permitted to remain with the child for a limited period, typically between 0.5 and 2 hours, before transfer. After the transfer, they usually do not stay in the morgue, and the nurse remains responsible for the ongoing care of other patients in the unit.
Nurse allocation within the PICU is determined by the number of open beds, and the staffing of each unit is relatively fixed. Following a patient’s death, no routine leave is granted to the responsible nurse. Leave is considered only in cases where psychological symptoms significantly interfere with the ability to perform routine duties.
Participants
The participants were PICU nurses who met the following inclusion criteria: (1) at least two years of experience working in the PICU; (2) direct involvement in postmortem care and the death of pediatric patients during the past year; and (3) willingness to participate in the study. The exclusion criteria were nurses who had recently experienced major personal or family trauma.
Purposeful sampling was employed to ensure that the participants could offer in-depth and relevant perspectives on the research topic. 13 Eligible nurses were identified in collaboration with the PICU head nurse by reviewing their work records to confirm their years of experience and recent involvement in postmortem care. The focus was on nurses who had sufficient experience in PICU settings, as they were best equipped to provide detailed accounts of the emotional challenges they face.
Recruitment
After identification, eligible nurses were approached in person by the research team and provided with detailed information about the study objectives, procedures, and confidentiality measures. Interviews were scheduled at times convenient for the participants. All 15 nurses who were contacted agreed to participate in the study, and written informed consent was obtained before the interviews. The study ensured confidentiality by anonymizing the data and emphasizing the voluntary nature of participation. To acknowledge participants’ contributions, a small gift was provided as an incentive.
Data collection
Data were collected through semi-structured, in-depth, face-to-face interviews conducted from February to April 2025. The interviews aimed to explore the emotional experiences of nurses, focusing on their reactions to patient death, the process of postmortem care, and the subsequent emotional impact. All interviews were conducted by the first author (W.X.), a female nurse with extensive experience in qualitative research and interviewing. The interviewer was professionally acquainted with the participants as a colleague in the same hospital, which helped establish rapport and trust. However, there was no supervisory relationship between the interviewer and the participants. Interviews were held in private rooms within the hospital to ensure confidentiality and minimize distractions. Each interview lasted between 30 and 60 minutes and was audio-recorded using encrypted devices with participants’ consent. The interviewer employed active listening, probing, and the strategic use of silence to encourage participants to share their experiences in depth. Reflexive notes were taken after each interview to document emerging themes and contextual observations. 14
Data analysis
The analysis followed a thematic approach, using Braun and Clarke’s 15 six-step process: (1) familiarization with the data, (2) generating initial codes, (3) generating themes, (4) reviewing themes, (5) defining and naming themes, and (6) producing the report. The transcription of interviews was completed within 24 hours of the interview. Data analysis was conducted using qualitative data analysis software NVivo to organize and examine the data systematically. The research team independently developed the initial codes and themes, and regular discussions were held to refine and validate the findings. The credibility of the analysis was enhanced by the inclusion of diverse participant perspectives, the researcher’s expertise in pediatric care, and the iterative process of theme development. Themes were further reviewed and discussed to ensure that they accurately represented the experiences of the participants.
Since the interviews were conducted in Chinese, all transcriptions were first analyzed in the original language to preserve cultural and linguistic nuances. Selected participant quotations were then translated into English for reporting. The translation process involved forward translation by bilingual members of the research team, followed by independent checking to ensure accuracy and fidelity to the original meaning. Where necessary, wording was refined collaboratively to best capture the participants’ intended expressions in English while retaining contextual meaning.
Ethical considerations
The study was approved by the Ethics Committee of Zhejiang Children’s Hospital (Approval Number: 2024-IRB-0249-P-01). The study adhered to the ethical guidelines set forth in the Declaration of Helsinki. Informed consent was obtained from all participants prior to the interviews. The confidentiality of all participants was assured, and no personal identifying information was included in the final analysis. Participants were informed of their right to withdraw from the study at any point without any consequences.
Results
The study cohort comprised a total of 15 PICU nurses, with 4 males and 11 females. The participants had a median age of 34 years, with ages ranging from 25 to 42 years. A detailed overview of their demographic characteristics can be found in Table 1.
Characteristics of the Nurses Participating in the Study
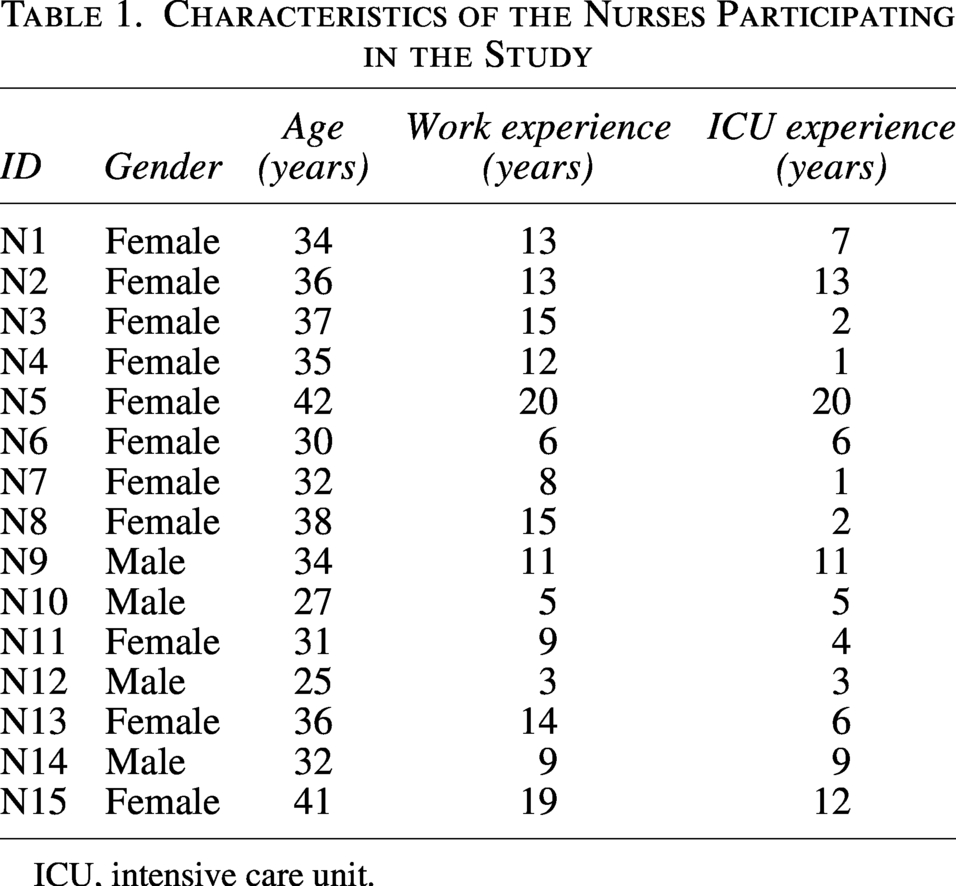
ICU, intensive care unit.
Theme 1: Emotional and physical strain of patient loss
Subtheme 1: Physical symptoms of emotional stress.
Nurses reported experiencing intense emotional stress when faced with patient deaths, a stress that manifested both psychologically and physically. This physical response was particularly pronounced when there was a strong emotional bond with the patient. For instance, N1 shared:
“He had been in our department for over two years. I used to feed him rice porridge and make him laugh during my shifts… That day, his parents decided to withdraw treatment. I happened to be off that day, and I didn’t dare to come to the ward. When I returned to work, seeing the bed where he used to stay made me cry. It was very oppressive at work, and I couldn’t sleep at night. I had insomnia, which made my migraine worse. I had many nightmares and would wake up crying.”
N3 described her physiological response upon hearing about the death of another child: “That day, I heard that a child in the ward had passed away. I felt like I couldn’t breathe, it was hard to catch my breath. I had no mood for work, didn’t want to talk, and felt really awful. I couldn’t look at the parents, because if I did, I couldn’t stop my tears.”
N12 recounted his first experience of participating in a resuscitation, where he did not directly witness a death but still felt a great deal of physical tension, shown by involuntary muscle spasms:
“I was completely lost, not knowing what to do, standing at the foot of the bed. My mind and body weren’t in sync. I was so nervous that the corner of my mouth twitched. My colleague saw me and asked what I was doing and why I was smiling… I wasn’t smiling at all. I was just so nervous that my mouth twitched involuntarily, and my colleague thought I was smiling.”
Subtheme 2: Grief and emotional bonds in pediatric care
In pediatric intensive care, emotional bonds between nurses and patients gradually developed through daily caregiving, extending beyond professional duties. When a child reached a critical or terminal stage, these bonds often deepened into profound grief, triggering overwhelming emotional reactions among nurses. The loss of a patient would frequently bring back memories of previous care experiences, underscoring the deep emotional impact of their role in such intense situations. N4 shared her experience of witnessing a family’s final goodbye with their child:
“Today, the mother was at the bedside, saying her final words to the child. My heart felt so heavy, I couldn’t hold back my tears, and I really wanted to cry… After the parents signed the consent for withdrawal of treatment, the patient’s heart rate slowly dropped. Suddenly, I was reminded of a patient in the hematology department years ago who also had life support withdrawn. Those memories came rushing back, and seeing this made me realize how frightening death is, how close it is to life, and how fragile life truly is.”
N5 also shared her emotional reaction when she heard the parent say their final goodbye to their child:
“The parents came in and said their final goodbye to the patient, saying, ‘You will always be our son, please come back and find us…’ Hearing that, I just couldn’t handle it, tears started flooding out, and I quickly turned around to compose myself, but I couldn’t control it. It was just too sad.” She further explained the profound impact this emotional resonance had on her work and personal life: “That day, I was really busy, but after that child passed away, I couldn’t calm down. I needed to talk to my colleagues to process it. When I got home, I had no appetite and didn’t feel like eating.”
Theme 2: Fear and unease in postmortem care
Subtheme 1: Fear and anxiety in facing death
In postmortem care, nurses reported experiencing significant emotional fluctuations, particularly when they were first exposed to a deceased body or had to frequently handle death. The natural fear of death, combined with unfamiliarity in handling a deceased body, created emotional challenges that nurses found difficult to avoid. For example, N10 described his fear when he had to touch the body of a deceased patient:
“When I went to remove the wristband of the deceased patient and touched his arm, it felt cold, and I could feel my hand was cold too. I was really scared…”
The strong discomfort nurses feel when touching a body, especially the coldness, deeply triggers their fear of death. N13 also described the emotional impact when encountering a deceased body:
“When I saw my colleague closing the body bag and getting ready to cover the face, I just couldn’t handle it in that moment. I had to turn away and take a moment to collect myself. Every time something like this happens at work, I need to talk to my husband when I get home, or I just can’t shake the feeling.”
Another nurse, N9, expressed: “Every time I face a body, there’s always this inexplicable tension, especially when I see a child’s body. The cold, lifeless feeling makes it hard for me to look directly at them. Sometimes, I even feel like I’m not strong enough, and I get this sense of fear when I face all of this.”
Subtheme 2: Uncertainty in Postmortem procedures
In addition to the emotional shock, nurses also reported facing practical confusions and uncertainties during postmortem care, particularly when they lack proper training. Nurses expressed that when performing postmortem care, especially when dealing with specific procedures for the first time, they felt lost and unsure of how to proceed. The nurses feel confused about regional funeral customs and special family requests, especially when they are unfamiliar with the details. Moreover, insufficient handovers during shift changes can result in nurses not fully understanding the family’s needs and cultural background, which affects the quality of care and respect for the family.
N14 recalled: “When I first performed post-mortem care, I felt like I knew nothing, especially regarding regional customs, such as children’s funeral requirements. I didn’t even realize these details at first. Later, I learned that I might have overlooked some of them, and I truly felt guilty about it.”
These unintentional oversights not only confused the nurses but also added to their psychological burden, especially when they were unable to meet the family’s expectations, which left them feeling deeply guilty.
N6 stated: “Sometimes during shift changes, I may not receive all the handover information, which causes me not to fully understand the special requests of the parents. At those times, I was really afraid I hadn’t done enough, that I hadn’t fulfilled my duties as a nurse.”
This problem with information transfer highlights the challenges nurses face during shift changes, particularly when it comes to understanding the family’s individual needs. A lack of detailed handover can lead to mistakes or oversights in care.
N7 added: “I’ve always felt that post-mortem care requires extreme attention to detail, especially when it comes to children. Many times, I felt like I hadn’t fully met the family’s expectations, and some procedures may not have been up to their standards. That feeling of powerlessness made me frustrated. Especially since we often don’t receive enough post-mortem care training, and most of the procedures are learned on the job. It always leaves me with this uneasy feeling, afraid of not doing well and disappointing the family.”
Theme 3: Navigating professionalism amid emotional turmoil
Subtheme 1: Suppressing emotions for professional duty
Nurses reported experiencing significant emotional fluctuations when facing the death of a patient, particularly when the patient was a young child. The emotional waves of helplessness and sadness that accompany such situations are often unavoidable. However, nurses expressed the need to suppress and manage their emotional reactions in order to remain rational and continue fulfilling their professional duties. For example, one nurse shared her approach when discussing the death of a child patient:
Dealing with a child’s resuscitation and death is really heartbreaking and sad, but sometimes, there’s nothing you can do. When I’m doing post-mortem care, I always tell each child, ‘You don’t have to suffer anymore. I hope in your next life, you’ll have a healthy body.’”
This emotional powerlessness resonated with many nurses when confronted with death. Despite the deep feelings of pain and regret, nurses emphasized the importance of adjusting their mindset to perform each task with calmness and rationality. One nurse reflected on this rational approach:
After working in the ICU for a long time, seeing patients die from severe illness, although it’s regretful, I can still face it calmly. When patients die, sometimes it feels really sad, but seeing the pain they endured during their illness, death can also be a relief.
Through this cognitive adjustment, nurses come to view death as an inevitable part of life, helping them to alleviate the emotional impact and maintain a balance between emotion and reason. This emotional suppression and rationalization not only help nurses cope with emotional upheaval but also play a key role in maintaining professionalism in their work. By viewing death as an inevitable life stage, nurses can transform emotional fluctuations into rational responses, allowing them to focus on their nursing tasks.
Subtheme 2: Balancing grief and professionalism
While nurses report effectively managing the emotional fluctuations caused by death through rationalization, grief and a sense of loss remain unavoidable emotional experiences. This emotional impact is especially profound when dealing with critically ill children or patients with whom nurses have developed a close personal connection. The key to managing these emotions lies in finding a balance between emotional responses and professional responsibilities, particularly by showing respect for the patient’s final journey. N6 shared her emotional experience when witnessing the death of a critically ill child:
“Seeing the child’s condition so severe, when the child died, I couldn’t stop crying. I couldn’t work for a while. I felt the patient was so pitiful, and I couldn’t face the severity of the child’s condition in the ICU. I took two months of sick leave, and later, with the support and guidance of my colleagues, I slowly adjusted.”
Even though nurses may manage death rationally, they still need time and support to regain emotional balance when confronted with such profound emotional impacts. During this time, acceptance of their emotions and support from colleagues become crucial factors in their emotional recovery. Although nurses often feel unbearable sadness and reluctance when faced with a deceased body, they continue to ensure that the patient is treated with dignity through professional care, fulfilling their responsibility between life and death. This “final care” is not only a professional duty but also a deep respect for the patient’s dignity and a way for nurses to regulate their emotions. N4 described the emotional challenge she faced during postmortem care:
“During post-mortem care, I felt it was extremely frightening and heartbreaking, but reason told me to respect the patient and provide proper care, allowing them to leave with dignity.”
Theme 4: Impact on parenting and career choices
Subtheme 1: Shifts in parenting perspectives
After experiencing the emotional impact of child death in their professional roles, nurses reported substantial changes in how they approached parenting and family life. These shifts were not limited to heightened awareness of health risks but also extended to how they valued daily interactions with their children and redefined their expectations for them.
N1 reflected on how her ICU experience changed her perspective after becoming a parent: “I used to work in the ICU, where we frequently dealt with deaths, especially among blood disorder patients. After having my own child, I became especially worried that my child might get sick too. After returning home, my attitude toward my child changed. I now think that as long as he is happy and joyful, that’s enough. I try to live in the moment. Before bed, I always tell him, ‘Mommy loves you,’ and I even make a little love gesture. I feel like I cherish every day.”
Several nurses described becoming more protective and health conscious, expressing constant concern over minor symptoms. N2 emphasized this heightened vigilance:
“When I get home and see my two children, I think, as long as they’re healthy and safe, that’s all that matters. If my child has a fever and I need to get blood tests, I always want to check extra indicators. I tend to overthink everything.”
This sense of heightened worry was echoed by N7, who found herself unusually anxious when her child showed even minor discomfort: “When I get home and my daughter feels a little unwell, I get really nervous, always fearing something worse might happen.”
However, some nurses also showed a more relaxed attitude toward parenting, especially when it came to managing their children’s academic pressure. For example, N8 said: “Now that my child is in third grade, if he says he has too much homework and can’t finish it, we just let him stop and go to bed. We’ve become a bit more relaxed, not wanting our child to work too hard.”
Subtheme 2: Workplace fatigue and career decisions
Long-term work in the ICU, particularly with frequent exposure to death, leaves many nurses feeling both physically and emotionally drained. The constant exposure to life-and-death situations and the normalization of death within their daily routines have profound emotional impacts. Many nurses find themselves overwhelmed by the emotional toll, which sometimes leads them to reconsider their professional roles. Specifically, some nurses actively avoid ICU positions, seeking roles in less emotionally demanding departments in an effort to alleviate the psychological burden. This shift underscores the significant impact of the work environment on nurses’ mental health and demonstrates how emotional fatigue can influence both career decisions and psychological adaptation.
For example, N1 shared: “I worked in the ICU for 7 years, then 5 years in a general ward. If I had the choice, I wouldn’t go back to the ICU. It feels so suffocating there, whereas the general ward is much brighter. So now, I don’t have high expectations for myself. I just want to be happy and enjoy each day.”
N5’s change also illustrates how the pressure of the work environment deeply affects their mental state: “I’ve been in the ICU since graduation, but in the last six months, I transferred to a general ward. It’s a lot less stressful, and I don’t feel so burdened at work. I really don’t want to go back to the ICU.”
Other nurses, after experiencing the death of a child, faced even more severe emotional exhaustion and emotional fluctuations. N6 described her reaction: “Since I had my own child, I thought I could return to the ICU, but I felt overwhelmed. Seeing those children, I didn’t know what to do. I couldn’t even touch them. Even turning a patient’s body felt difficult. Seeing how severely ill they were, and then some of them dying, I couldn’t stop crying. I couldn’t focus, and I had to take sick leave for two months. Eventually, with the support of my colleagues, I slowly started to adjust.”
N11 described her physical and emotional responses due to the emotional impact of her work: “Now that I have my own child, seeing the children in the hematology ward makes me feel really heavy. I’m always worried if my child might get sick like that. At night, I have nightmares and sometimes wake up crying. During the day, I’m exhausted at work. Even though my colleagues are looking out for me, I still feel like I can’t cope. I’ve lost a lot of weight, and I went to see a therapist. After some time off, I still couldn’t adjust, and I’m thinking about quitting.”
Discussion
This study highlights the significant emotional and physical challenges faced by PICU nurses, particularly in the context of patient death, postmortem care, and the emotional spillover into their personal lives. Nurses in this high-stress environment frequently experience intense emotional distress, which not only manifests psychologically but also physically, with symptoms such as insomnia, headaches, and anxiety. These findings align with previous studies that have identified the physical manifestations of emotional stress in nurses working in intensive care settings.16,17 The emotional burden of caring for critically ill children, combined with the frequent exposure to death, places a considerable strain on nurses’ physical and mental well-being.
The emotional bond between nurses and pediatric patients plays a significant role in the intensity of this distress. 18 When nurses form close emotional connections with their patients, the death of a child often leads to deep grief and emotional turmoil. 19 This emotional resonance can sometimes trigger past traumatic memories, further compounding the emotional impact. 17 While nurses are trained to maintain professionalism and emotional control, this study shows that their emotional responses are often inevitable, particularly when confronted with the death of a young patient. This finding supports existing research on the emotional toll of death on ICU nurses, indicating that despite attempts at emotional suppression, they continue to experience significant grief.20,21 From the perspective of emotion regulation theory, these responses illustrate the limitations of suppression strategies, which are commonly employed in high-stress clinical settings. Although suppression may enable task completion in the short term, it is often associated with heightened physiological stress and increased emotional exhaustion over time, as observed in our findings. The repeated need to regulate intense emotions in the face of frequent patient deaths may further deplete nurses’ psychological resources, heightening the risk of burnout.
In addition to the emotional challenges, nurses also face practical difficulties during postmortem care. Many nurses reported feelings of fear and discomfort when handling deceased bodies, especially those of children. This fear is not only related to the unfamiliarity of the task but also to the natural human aversion to death.22,23 Moreover, the lack of comprehensive training in postmortem care exacerbates these feelings of uncertainty and anxiety, as nurses often struggle with cultural and family-specific funeral requirements. 24 It is also important to consider how the specific institutional and cultural context in China shapes nurses’ experiences of postmortem care. In the study setting, nurses who provide postmortem care typically remain responsible for other critically ill patients and are not routinely relieved of clinical duties following a child’s death. This practice may be influenced by staffing resources and cultural norms, which can differ across countries and regions. The absence of structured relief or dedicated time for emotional recovery may intensify distress, as nurses must immediately resume high-intensity care for other patients without sufficient psychological adjustment. These contextual factors likely contribute to the cumulative stress and emotional fatigue observed in this study. Consistent with emotion regulation theory, such continuous exposure to emotionally charged situations without recovery opportunities increases the reliance on suppression and accelerates resource depletion, ultimately undermining nurses’ resilience and well-being.
Furthermore, the study revealed the emotional spillover effects of work on nurses’ personal lives. Many nurses expressed heightened anxiety and overprotectiveness toward their children after experiencing the trauma of patient death. This emotional shift suggests that the emotional burdens of nursing extend beyond the workplace, influencing nurses’ parenting styles and family dynamics. While some nurses became more protective, others adopted a more relaxed attitude toward their children’s academic pressures. These changes reflect the complex ways in which nurses cope with emotional stress by adjusting their personal and professional lives. This finding aligns with previous studies that have shown how occupational stress can manifest in nurses’ home lives, influencing their relationships and parenting behaviors.25,26 Reflexive notes were particularly valuable in analyzing these spillover effects. During the research process, documenting our own assumptions and emotional reactions helped us to remain aware of how our preconceptions about parenting and family dynamics might have influenced interpretation. Incorporating these reflections ensured that the analysis remained centered on the nurses’ voices, foregrounding their lived experiences of how professional stress reshaped family life rather than the researchers’ prior expectations.
Finally, the study highlights the significant work-related fatigue and emotional oppression experienced by nurses, particularly those in high-stress environments like the PICU. Many nurses reported feeling emotionally drained and, in some cases, actively sought to transition to less emotionally taxing roles. This reaction indicates the long-term psychological toll of working in environments where death is a frequent occurrence. Such findings are consistent with research showing that emotional exhaustion is a common response among nurses working in critical care who regularly deal with patient death.27,28 The cumulative effect of this emotional burden underscores the need for better institutional support, including mental health resources and career flexibility, to help nurses cope with the demands of their work.
Implications of the study
The findings of this study have several significant implications for clinical practice in pediatric intensive care. First, the experiences of nurses reporting insomnia, migraines, nightmares, and other physical symptoms of emotional stress after patient deaths highlight the urgent need for institutional support. Hospitals should provide structured counseling services, grief management workshops, and regular debriefings to help nurses manage the psychological and physical effects of their work. These interventions could reduce long-term distress and improve overall well-being. Second, the deep grief and emotional bonds reported by nurses suggest that grief is not only a personal reaction but an inherent part of pediatric intensive care. Clinical leaders should normalize grief as a professional experience and create supportive spaces such as peer support groups or reflective practice sessions. This approach can reduce feelings of guilt and isolation, fostering healthier coping strategies. Third, reports of fear and uncertainty in postmortem care, particularly when nurses lack adequate training or clear handover information, emphasize the need for improved training and communication systems. Specialized education on postmortem care, including cultural considerations and protocols for addressing family needs, would boost nurses’ competence and confidence. Enhancing handover procedures can also minimize the risk of oversights, ensuring that families receive care that is respectful and culturally sensitive. Fourth, the findings highlight the psychological strain of balancing professionalism with intense emotional experiences. While nurses often suppress their emotions to continue caring for patients, this can lead to emotional exhaustion. Institutions should promote emotional resilience training and routine debriefings, providing nurses with opportunities to express and regulate their emotions constructively. Cultivating a culture that values both professionalism and emotional authenticity can improve nurses’ psychological well-being while maintaining high standards of care. Finally, the impact of patient deaths on nurses’ parenting perspectives and career decisions reflects the broader effects of PICU work beyond the clinical setting. Emotional spillover into family life and reports of career changes due to emotional fatigue suggest that flexible scheduling, role rotations, and mental health leave could be important strategies for retention and long-term adaptation. By recognizing the overlap between professional and personal lives, health care institutions can create environments that better support nurses both at work and at home. In sum, these implications emphasize that providing emotional, psychological, and practical support for nurses is critical not only for their well-being but also for maintaining the quality and sustainability of pediatric intensive care.
Limitations
This study provides valuable insights into the emotional challenges faced by PICU nurses, but it has several limitations. The sample size was small and limited to nurses from specific hospitals, which may affect the generalizability of the findings. Future research should include a larger, more diverse sample from various regions and health care settings. Additionally, this study relied on semi-structured interviews, which may introduce subjectivity and bias. Combining qualitative and quantitative methods in future studies could provide a more comprehensive analysis of the long-term emotional impact on nurses. Furthermore, this study did not explore cultural differences in emotional responses. Cultural attitudes toward death may affect how nurses process grief and interact with families, suggesting that future research should examine these factors across different cultural contexts. While this study identified emotional exhaustion and stress, it did not explore how institutional support could alleviate these issues. Future studies should focus on how improving work environments and offering psychological support can reduce burnout and emotional fatigue. Last, the study lacked a longitudinal approach to assess the long-term effects of emotional distress. Future research should track nurses over time to understand how their mental health evolves and how existing support systems impact their well-being. Long-term studies could offer valuable insights into strategies for improving the mental health and career sustainability of nurses in high-stress environments.
Conclusion
This study highlights the significant emotional and psychological challenges faced by PICU nurses, particularly in relation to patient death and postmortem care. Nurses may experience emotional distress and physical symptoms, such as insomnia and anxiety, which seem to be linked to their emotional connections with patients. The lack of adequate training in postmortem care, along with emotional spillover into personal lives, appears to exacerbate these challenges. Addressing these issues could involve improving institutional support, such as enhanced training, emotional resilience programs, and better work–life balance. Strengthening both external support systems and nurses’ internal resources may help improve their well-being, job satisfaction, and ultimately the quality of care provided.
Authors’ Contributions
W.X. and B.X. carried out the studies, participated in collecting data, and drafted the article. W.X. and X.L. performed the statistical analysis and participated in its design. W.X., B.X., X.L., J.Z., and S.Y. participated in the acquisition, analysis, or interpretation of data and drafted the article. All authors read and approved the final article.
Footnotes
Author Disclosure Statement
No competing financial interests exist.
Funding Information
This study was supported by the Natural Science Foundation of Zhejiang Provincial Department of Education Project (Y202454325).
