Abstract
Introduction:
The hospice attending physician plays an essential role in the management and delivery of hospice care. In this role, the attending physician is chosen by the patient or health care surrogate and is a resource regarding the patient’s medical condition and needs. Nurse practitioners and physician assistants may also act in this capacity. Research recognizes the importance of the relationship between the patient and hospice attending through the end of life, but often the hospice attending role is filled by an attending from the hospice agency who generally does not have a prior relationship with the patient.
Methods:
We conducted a retrospective chart review for all patients enrolled in Rochester Regional Hospice (RRH) Care from 2020 to 2024 in Rochester, New York.
Results:
We conducted a comprehensive review of 12,328 hospice admissions from 2020 to 2024, encompassing patients receiving both routine and inpatient hospice care, with no exclusions applied. The annual average admissions totaled 2465. Over this five-year period, hospice admissions electing to use hospice agency providers as their primary attending physicians increased by 26.7%, indicating a significant upward trend in this care model.
Conclusions:
The results demonstrate a consistent increase in patients choosing hospice agency physicians as their primary hospice attending providers. Further investigation is warranted to identify the factors influencing this selection and to better understand its implications for hospice care delivery.
Keywords
Background
The primary goal of hospice care is to support quality of life for those diagnosed with a terminal illness by managing symptoms, addressing emotional, social and spiritual needs. The hospice interdisciplinary team (IDT) plays an important role in achieving this goal. The IDT includes physicians, nurses, hospice aides, social workers, counselors, chaplains, and trained volunteers. 1 The attending physician is the physician, nurse practitioner, or physician assistant chosen by the patient who has the most significant role in the determination and delivery of the patient’s medical care. This had traditionally been the patient’s primary care provider or, in some cases, an involved sub-specialist or health care provider from the hospice agency. The intent is for the attending provider to be someone who knows the patient best, often through a previous patient/provider relationship.
Research recognizes the importance of understanding both the patient and primary care provider’s experiences during the care transition to hospice. 2 While patients and families feel trust in their family physician is an important factor in electing hospice care, family physicians have noted barriers and challenges with hospice care. For example, limitations surrounding the ability to make house-calls, communication barriers with the hospice agency, and comfort level with opioid titrations. 2
Over the past decade, there has been notable growth in the number of hospice programs and hospice utilization. In 2020, there were 5058 Medicare-certified hospices in operation based on claims data. By 2022, the number of Medicare-certified hospices had increased to 5899. 3 In 2023 nearly 52% of decedents received care through hospice, according to data from the Medicare Payment Advisory Commission. 4
With the growing demand for hospice care in the United States, research recognizes the important relationship between the family physician and the patient.5,6 Evidence suggests regional variance in primary care involvement at the end of life. While Ankuda et al. demonstrated that greater PCP involvement at end-of-life was associated with less intensive care, they also found reduced hospice utilization, highlighting the complex relationship between continuity of care and hospice engagement. 6 Presently, little data exist that examines the trends of hospice agency physicians who serve as the patient’s primary hospice attending.
Methods
Study design
We conducted a retrospective chart review for all patients enrolled in Rochester Regional Hospice (RRH) Care from January 2020 to December 2024 in Rochester, New York (N = 12,328). The study included patients admitted to all levels of hospice care, including both routine and general inpatient hospice. The attending of hospice record was identified through chart review and cross-referenced with those providers acting as a clinical hospice medical director or employed by the hospice agency (RRH). There were no exclusion criteria. The study was approved by the RRH Institutional Review Board.
Setting and study population
The RRH system serves a diverse population exceeding 1.6 million individuals across an expansive service area of approximately 13,600 square miles. Within this broad geographic region, RRH provides comprehensive hospice care services through Rochester Regional Hospice, which operates across three counties in Western New York as well as the Finger Lakes region. The hospice care offerings are multifaceted, encompassing home-based hospice care, skilled nursing facility hospice care, and general inpatient hospice care designed to manage complex symptoms and provide intensive comfort-focused treatment. In addition to these settings, RRH providers also serve as attending physicians at a dedicated, free-standing inpatient hospice care center, which houses 11 inpatient beds and offers specialized, around-the-clock care for patients with acute hospice needs. The inpatient hospice capacity did not fluctuate over the five-year period. This integrated model ensures that patients across various care environments receive consistent, high-quality hospice support tailored to their individual needs.
Results
Discussion
From January 2020 through December 2024, this retrospective chart review demonstrated a 26.7% overall increase in the utilization of RRH providers serving as the primary hospice attending physicians. This upward trend suggests a growing reliance on RRH providers for end-of-life care management. Notably, during the period of 2021–2022, as the immediate impact of the initial COVID-19 outbreak began to diminish, we hypothesize that enhanced access to health care services and improved coordination of transitions into hospice care played a meaningful role in the observed 8.9% increase in RRH provider utilization. This moderate growth during the post-acute pandemic phase may reflect systemic adaptations aimed at better integrating palliative and hospice services. However, the most pronounced increase occurred in the final two years of the study period, 2023–2024, when utilization surged by 10.6%, marking the highest rate of growth across all intervals analyzed. Over the five-year study period, the average number of hospice admissions was 2465.6 patients annually, indicating a consistently high demand for hospice care services. Across the five-year period, the distribution of levels of care remained stable, with routine home care as the majority of care provided. The inpatient hospice capacity of 11 beds did not fluctuate. There was no significant year-to-year variation in the proportion of patients receiving routine versus inpatient care. A comprehensive breakdown of the raw data supporting these findings is available in Table 1.
Yearly Hospice Admission Data (*RRH—Rochester Regional Hospice Agency)
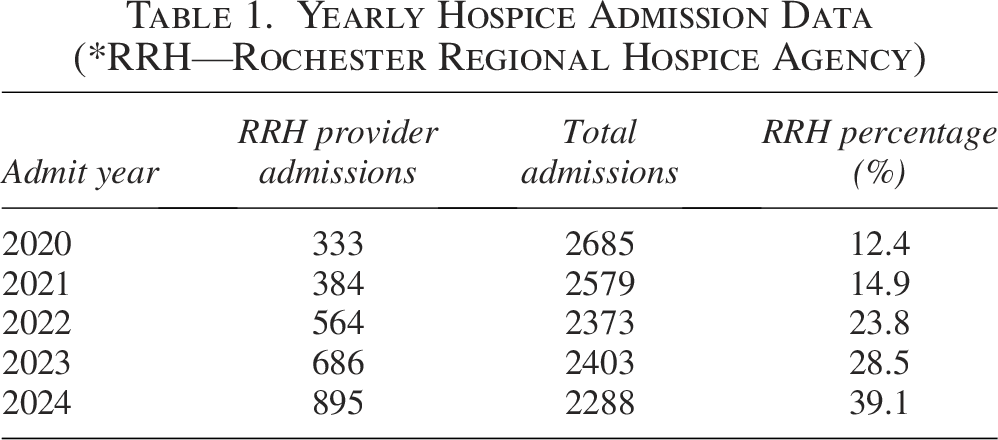

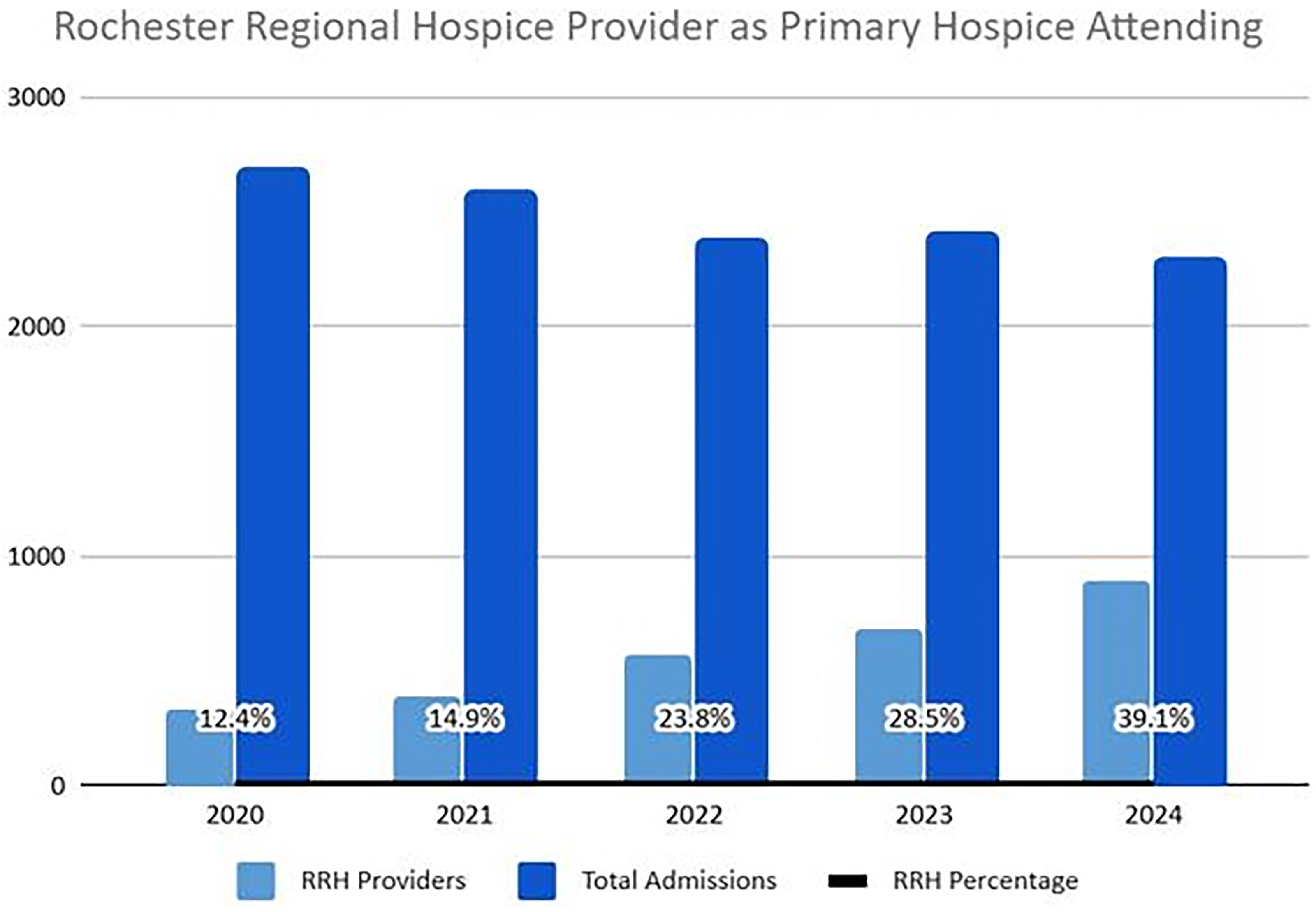
Percentage of Rochester Regional Hospice (RRH) Providers as Primary Hospice Attending.
Limitations
This study focused exclusively on a single nonprofit hospice agency, which may limit the generalizability of the findings to other hospice organizations operating under different structures, regions, or patient populations. As such, the trends observed in this analysis may not fully represent broader patterns across the hospice care landscape. Furthermore, the retrospective design of this study inherently constrains the ability to establish causality, positioning these findings primarily as hypothesis-generating rather than definitive conclusions. It is important to consider that various temporal factors, particularly those associated with the initial COVID-19 outbreak during 2020 and 2021, likely influenced the results. Specifically, pandemic-related disruptions may have significantly restricted patient transitions of care and engagement with hospice services, thereby impacting utilization patterns observed during this period. These contextual limitations underscore the need for cautious interpretation and highlight opportunities for future prospective research to more accurately delineate the drivers of hospice utilization trends.
Conclusion and Recommendations
Hospice care fundamentally relies on a highly specialized IDT that includes physicians, nurses, hospice aides, social workers, counselors, chaplains, and trained volunteers, each playing a vital role in delivering comprehensive, patient-centered end-of-life care. The complexity of hospice care demands seamless collaboration among these professionals to address the diverse physical, emotional, psychosocial, and spiritual needs of patients and their families. While existing research provides valuable insights, further investigation is necessary to generate precise, generalizable estimates regarding the factors that influence hospice care delivery. Current literature emphasizes that regional practice patterns, alongside the unique operational demands of the hospice care model—such as the requirement for after-hours availability, effective and timely communication, and proficiency in managing complex symptom control including opioid titration—significantly affect which type of physician ultimately assumes the role of hospice attending.2,4 Moreover, as hospice care continues to evolve, it is increasingly important to explore patient and family preferences in selecting their hospice attending physician, as these preferences may impact satisfaction, quality of care, and outcomes. Future studies focusing on these preferences and decision-making processes will be crucial in tailoring hospice services to better meet the individualized needs of patients and their loved ones.
Footnotes
Author Disclosure Statement
No competing financial interests exist.
Funding Information
None to report.
