Abstract
Objectives:
We aimed to evaluate histologic findings in upper gastrointestinal (UGI) biopsies of pediatric inflammatory bowel disease (IBD) patients, their correlation with endoscopic features, and association with disease activity.
Methods:
UGI biopsies from 50 pediatric IBD patients (31 Crohn’s disease [CD] and 19 ulcerative colitis [UC]) were retrospectively reviewed. Esophageal, gastric, and duodenal samples were categorized as highly suggestive, suspicious, or unlikely for UGI involvement. Associations with endoscopic abnormalities, colonoscopic disease extent, and simplified Geboes scores were analyzed.
Results:
Highly suggestive findings were most common in the antrum (60%), followed by the corpus (26%), esophagus (24%), and duodenum (20%). Focal enhanced gastritis (FEG) was the leading feature and appeared more frequently in UC than CD, though without statistical significance. H. pylori–negative active chronic gastritis, distinct from FEG, was identified and classified as suspicious for involvement. Duodenal findings including cryptitis, crypt abscesses, crypt distortion, villous blunting, and foveolar metaplasia may reflect IBD-related changes rather than nonspecific inflammation and were more frequent in UC, but not significantly. Highly suggestive findings in the esophagus and duodenum correlated with endoscopic abnormalities, whereas gastric findings did not. In contrast, highly suggestive antral and corpus findings were associated with higher simplified Geboes scores.
Conclusions:
UGI involvement in pediatric IBD is easily overlooked and requires careful assessment. Integrating histologic, clinical, and endoscopic findings is essential, as characteristic UGI features may influence disease evaluation and therapeutic decision making.
Keywords
What Is Known
Upper gastrointestinal tract involvement in inflammatory bowel disease (IBD) is common, particularly in pediatrics.
No specific histomorphologic findings in upper gastrointestinal tract biopsies are diagnostic of IBD.
What Is New
FEG was the predominant lesion throughout the esophagus to the duodenum and was observed more often in UC than in CD, although the difference did not reach statistical significance.
H. pylori–negative active chronic gastritis may be related to IBD.
Cryptitis, crypt abscesses, crypt distortion, and foveolar metaplasia, particularly when present together, may be associated with IBD rather than nonspecific inflammation.
The presence of FEG in antrum may serve as a clue for duodenal involvement; therefore, duodenal biopsies should be carefully evaluated for potential disease-related histologic features.
Introduction
Upper gastrointestinal (UGI) tract involvement in inflammatory bowel disease (IBD) is common, particularly in pediatric patients.1-3 Ileocolonoscopy and esophagogastroduodenoscopy are recommended as part of the initial work-up for all children with suspected IBD, according to the European Society for Pediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN) Porto Criteria for diagnosing IBD. Multiple biopsies (2 or more per section) should be obtained from all segments of the visualized gastrointestinal tract, even in the absence of upper gastrointestinal (UGI) symptoms or macroscopic lesions. 4
While earlier studies emphasized that UGI tract involvement is a suggestive finding for Crohn’s Disease (CD), it is no longer considered a distinguishing feature between CD or ulcerative colitis (UC).2,5,6 Although no specific histomorphologic findings in UGI tract biopsies are diagnostic of IBD, several features have been described in esophageal, gastric, and duodenal biopsies in both CD and UC.5,7-13
In this study, we aimed to assess the histological findings in UGI tract biopsies of pediatric patients with IBD, focusing on the frequency of these findings, their correlation with endoscopic findings, and their association with the severity of histologic disease activity in colonoscopic biopsies.
Methods
Ethics Statement
This study was approved by the Clinical Research Ethics Committee of the Istanbul University Faculty of Medicine (file number: 2025/316).
Patients
This study included 50 pediatric patients diagnosed with IBD between 2017 and 2024, all of whom underwent simultaneous esophagogastroduodenoscopy and ileocolonoscopy. Atypical or unclassified variants were not included. Both initial and follow-up biopsies were selected for the heterogeneity. The clinical and endoscopic findings were retrieved from the hospital database.
Twenty-six control cases (celiac disease, H. pylori gastritis, and nonspecific findings) were included for comparison.
Endoscopic Features
Endoscopic findings in the esophagus, stomach, and duodenum were recorded from esophagogastroscopy. Ileocolonoscopy findings were graded using the Mayo endoscopic score (0-3). 14
Histopathologic Findings
Histologic findings in the biopsies taken from the esophagus, stomach, and duodenum were retrospectively reviewed by 2 blinded gastrointestinal pathologists. All archived Hematoxylin-Eosin (H&E) stained biopsy sections were re-examined. All patients had at least 2 biopsy specimens taken from each part of the distal and proximal esophagus, corpus, antrum, bulb, and second part of the duodenum.
UGI tract biopsies were categorized into 3 groups based on histologic findings: 'highly suggestive' of involvement, 'suspicious' for involvement, and 'unlikely' to indicate involvement. Each biopsy site was evaluated and classified individually. A case was classified as highly suggestive of UGI tract involvement if at least 1 site demonstrated such histologic features. If none of the sites exhibited these features, the case was considered unlikely to be involved. Cases showing equivocal findings were categorized as suspicious for involvement.
Assessment of Esophageal Biopsies
Intraepithelial lymphocytosis, was defined as infiltration of more than 50 intraepithelial lymphocytes per high-power field (HPF, ×400), with no more than rare granulocytes 15 and was considered highly suggestive of involvement. The presence of reflux esophagitis-like changes or papillary vascular congestion was considered suspicious for esophageal involvement.
Assessment of Gastric Biopsies
Gastritis was classified according to the Sydney criteria.16,17 The presence of active chronic gastritis, inactive chronic gastritis, focally enhanced gastritis (FEG), nonspecific findings such as edema or congestion, and Helicobacter pylori status (positive or negative) were documented. Helicobacter pylori-negative granulomatous gastritis and/or FEG was accepted as highly suggestive of gastric involvement.1,3,9,18 FEG is defined as the presence of at least 1 foveolum or small groups of foveola or gastric glands surrounded and infiltrated by inflammatory cells with or without granuloma formation in a background of normal mucosa. 18 Lymphocytes and histiocytes are commonly observed in FEG, along with fewer neutrophils and eosinophils.11,19 Biopsies showing varying degrees of active chronic gastritis, with or without ulceration, and negative for Helicobacter pylori were classified as suspicious for gastric involvement.
Assessment of Duodenal Biopsies
The histologic findings such as active or chronic inflammation in the lamina propria, granulomatous inflammation, cryptitis, crypt abscesses, crypt destruction/rupture, crypt distortion, ulceration, foveolar metaplasia, intraepithelial lymphocytosis, basal lymphoplasmacytosis, and villous blunting were evaluated. The presence of more than 1 histologic feature, such as marked cryptitis or crypt abscesses, crypt destruction or rupture, crypt distortion, granulomatous inflammation, villous blunting, or basal lymphoplasmacytosis, was considered highly suggestive of duodenal involvement. Histologic findings, such as minimal architectural crypt changes with active chronic inflammation, or focal active chronic duodenitis with sparse cryptitis, were classified as suspicious for duodenal involvement.
Evaluation of Histologic Disease Activity Scores in Ileocolonoscopic Biopsies
Colonoscopic biopsies, were evaluated for histologic disease activity using the Simplified Geboes Score (SGS; 0-4). 20 The highest grade observed across the various colonic sites was used to determine the overall activity score.
We compared esophagastroduodenoscopic findings with UGI tract histologic findings and further analyzed the relationship between UGI tract involvement and the SGS.
Statistical Analysis
Descriptive statistics are presented as mean ± SD or n (%). Categorical variables were compared using χ² or Fisher’s exact tests, and non-normally distributed continuous variables using Mann–Whitney U or Kruskal–Wallis tests. Analyses were 2-tailed with 95% confidence intervals; P < .05 was considered significant. Statistical analyses were performed using SPSS v25.
Results
Patient Characteristics
A total of 31 patients (62%) had CD and 19 had (38%) UC. The mean age was 12.2 (±4.7 SD, range: 1-17) years. The biopsies of 31 patients (62%) were initial diagnostic biopsies, and the biopsies of 19 patients (38%) were taken under treatment. A total of 12 patients had repeated biopsies. In cases of repeated biopsies, the one performed during the period of most severe clinical symptoms was considered for statistical analyses. The clinical features of the patients are summarized in Supplemental Table 1.
Esophagogastroscopic Findings
Erythema, edema, mucosal nodularity, erosion, and aphthous ulceration were observed at varying frequencies in both UC and CD (Supplemental Table 2).
Histologic Findings
Esophagus
Intraepithelial lymphocytosis was observed in 15.8% (3/19) of patients with UC and 29% (9/31) of those with CD. Overall, it was detected in 24% of the study group. Among the 12 IBD cases showing intraepithelial lymphocytosis, both proximal and distal esophageal biopsies were involved in 5 cases (41.7%), only the proximal esophagus in 5 cases (41.7%), and only the distal esophagus in 2 cases (16.6%), while it was absent in the control group (P = .016). In the control group histologic findings compatible with reflux esophagitis–like changes were observed in 2 patients (7.7%) in the lower esophageal biopsies. In these 2 control cases, a small number of intraepithelial lymphocytes were occasionally observed, but they did not reach our predefined threshold of >50 intraepithelial lymphocytes per HPF and were therefore not considered pathologic. Papillary vascular congestion was a notable finding in the study group (42%); however, it was considered as a nonspecific finding, as it was observed in the control group as well (53.5%). Because most biopsies were superficial, the subepithelial limited area could be evaluated in only 4 (8%) cases, and mild chronic inflammation was observed in one of them.
Histologic findings of the esophagus were shown in Figure 1.
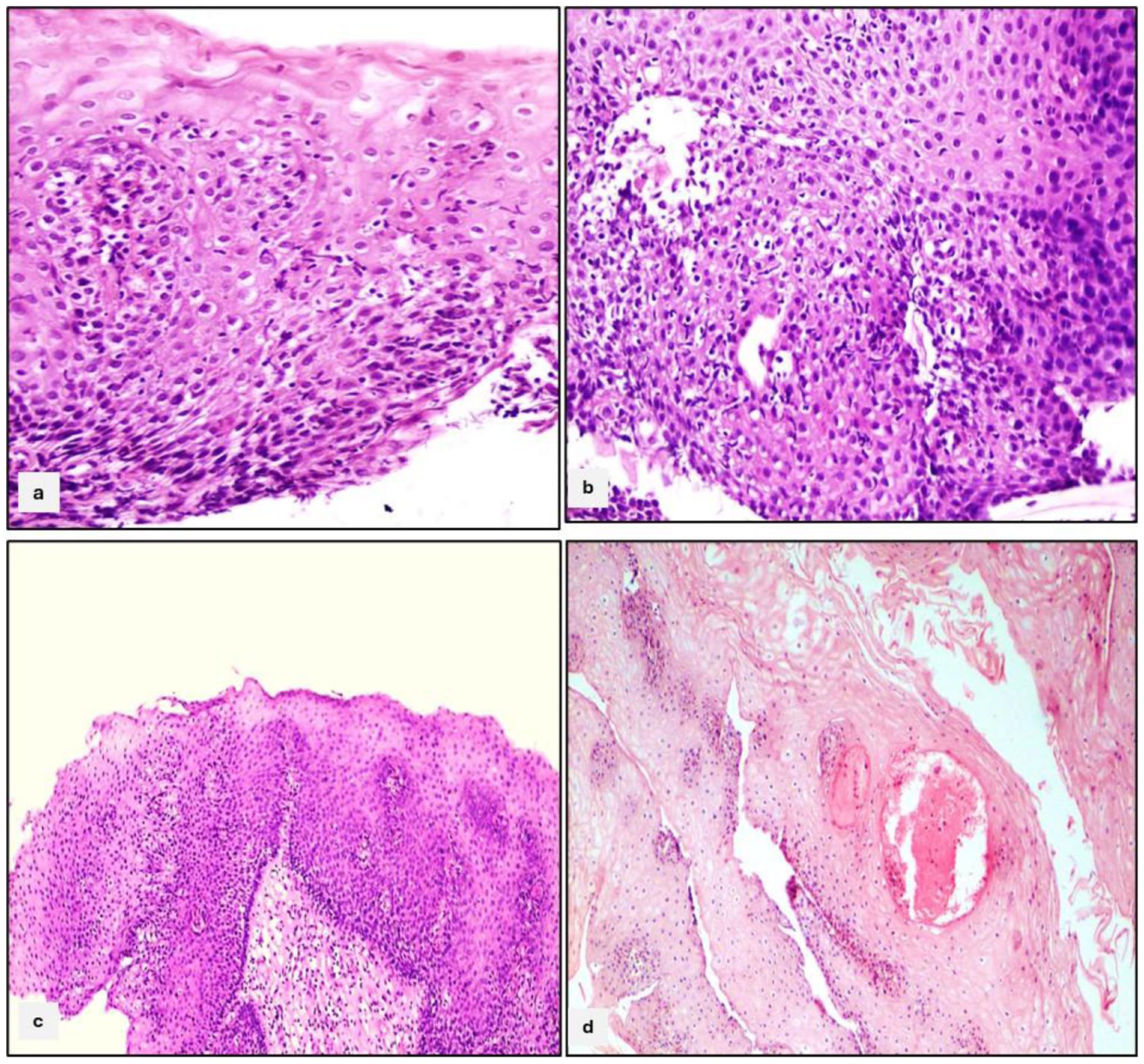
Histologic findings in the esophageal mucosa. Intraepithelial lymphocytosis is observed in the peripapillary area of the squamous epithelium (a). A tangential section of the squamous epithelium reveals intraepithelial lymphocytosis, with an incidental basal cell hyperplasia-like appearance (b). Basal cell hyperplasia and papillary elongation, classified as nonspecific findings, resemble reflux esophagitis-like changes (c). Papillary vascular congestion is seen as a nonspecific histologic finding (d).
Stomach
Both FEG and H. pylori-negative granulomatous gastritis, were detected in UC and CD patients in both antrum and corpus biopsies at varying frequencies (63.2% vs 45.2% in the antrum and 31.6% vs 22.6% in the corpus, respectively). Findings related to both entities were absent in the control group biopsies. Granuloma was observed only in the antrum of 4 CD patients (8%) and in the duodenum of 3 CD patients (6%).
Varying degrees of active chronic gastritis without H. pylori infection were observed in the antrum of 9 patients (18%) and the corpus of 11 patients (22%). Mild to moderate inactive chronic gastritis was observed in the antrum of 3 patients (6%) and the corpus of 5 patients (10%).
Histologic findings of the stomach were shown in Figure 2.
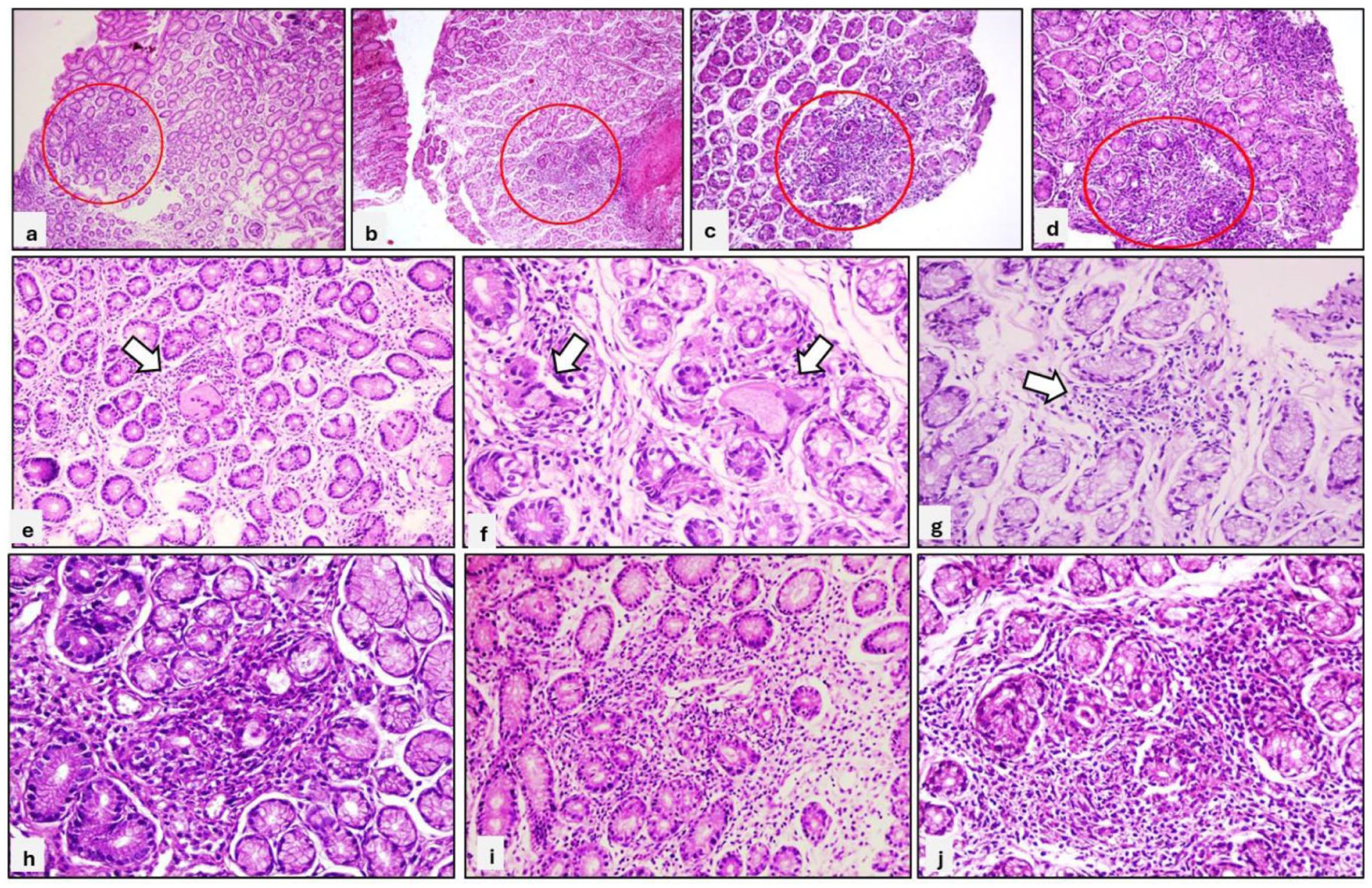
Histologic findings of FEG in the gastric mucosa. FEG is observed in the antrum and corpus, (circled areas), in a background of normal mucosa at lower magnifications (a-d). FEG with granuloma formation is observed in some cases (e and f). Focal inflammatory cells around the glands in the antrum is noted at higher magnification (g). A mixed inflammatory cell infiltration is present around the glands and within the glandular epithelial cells (h-j). Gland rupture is observed in certain areas (i).
Duodenum
Cryptitis and crypt abscess were observed in the bulb of 14 patients (28%) and the second part of 12 patients (24%), with a higher frequency in UC compared to CD (36.9% vs 22.6% in the bulb and 31.6% vs 19.4% in the second part, respectively). Crypt distortion was noted in 14% of cases (n = 7) in second part and in 16% of cases (n = 8) in the bulb. Villous blunting or shortening was observed in 10% of cases (n = 5) in the second part and in 8% of cases (n = 4) in the bulb. Intraepithelial lymphocytosis was observed in only 3 patients (6%) in the second part, compared to 10 (38.4%) in the control group, all of whom had celiac disease. In the study group, obvious foveolar metaplasia, characterized by distinct, separate foci, and easily recognizable under high-power magnification, was detected in multiple fields in 34% of cases (n = 17) in the bulb and 8% (n = 4) in the second part of the duodenum. Notably, obvious (multifocal) foveolar metaplasia was absent in the control group; however, focal foveolar metaplasia, limited to a few enterocytes, was observed in 15.4% of cases (n = 4) in the bulb and 7.7% (n = 2) in the second part of the duodenum.
Granulomas were observed in 3 patients (6%) with CD. Histologic findings of the duodenum were shown in Figure 3.
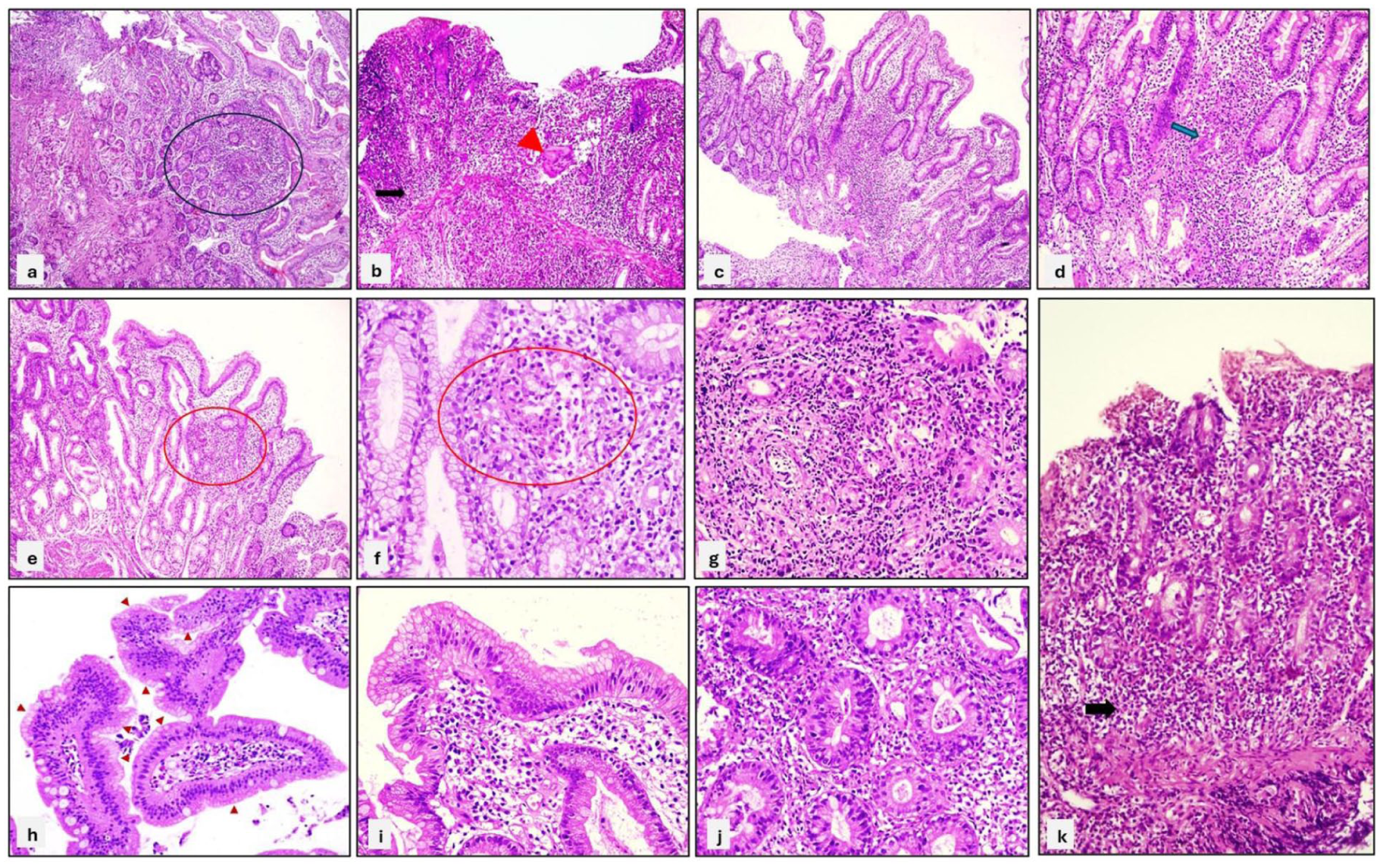
Histologic findings in the duodenal mucosa. Low-power magnification shows dense infiltration of inflammatory cells in the lamina propria (encircled) (a). Villous blunting, basal lymphoplasmacytosis (arrow), a multinucleated giant cell (arrowhead), and inflammation in the lamina propria extending into the submucosa are observed (b). Crypt distortion, focal villous shortening, and increased inflammation in the lamina propria (c) and crypt rupture seen at a higher magnification (arrow) are present (d). Similarly, focally dense inflammation and crypt distortion are observed (e). Higher magnification reveals crypt abscess and crypt rupture (encircled) (f). Mixed inflammation with cryptitis and crypt rupture is observed (g). Foveolar metaplasia is seen in the surface epithelium (arrowhead) (h) and (i). Higher magnification of cryptitis and crypt abscess (j). Basal lymphoplasmacytosis (arrow), villous blunting, and mixed inflammation are noted (k).
The distribution and frequencies of histopathologic features in study and control cases were summarized in Supplemental Table 3.
Histopathologic Findings in the Involvement (Highly Suggestive, Suspicious, and Unlikely for Upper GI Involvement) Groups by Biopsy Sites
Twelve patients (24%) had highly suggestive finding characterized by intraepithelial lymphocytosis in the esophagus. In the antrum, 30 patients (60%) showed either FEG (n = 26) or H. pylori-negative granulomatous gastritis (n = 4), while 13 patients (26%) exhibited FEG in the corpus as a highly suggestive finding. Additionally, 10 patients (20%) demonstrated more than 1 highly suggestive feature such as cryptitis/crypt abscesses, crypt destruction or rupture, crypt distortion, granulomatous inflammation, villous blunting, or basal lymphoplasmacytosis in the second part of the duodenum and the duodenal bulb.
Supplemental Table 4 summarizes the frequencies of histologic findings in both sites across the 3 categories: highly suggestive of involvement, suspicious for involvement, and unlikely to be involved.
Evaluation of Repeated Biopsies
Twelve patients underwent repeated biopsies, of whom 75% had CD and 25% had UC. Histologic findings in these patients are provided in the Supplemental Table 5.
Comparison of UGI Tract Histologic Involvement Groups and Endoscopic Findings Between UC and CD Patients
Abnormal endoscopic findings were more frequent in CD than UC, with a significant difference limited to the antrum (P = .043). No significant differences between UC and CD were observed across esophageal, gastric, or duodenal involvement categories (all P > .05; Table 1).
Comparison of the Histologic and Endoscopic Findings Between UC and CD Patients.
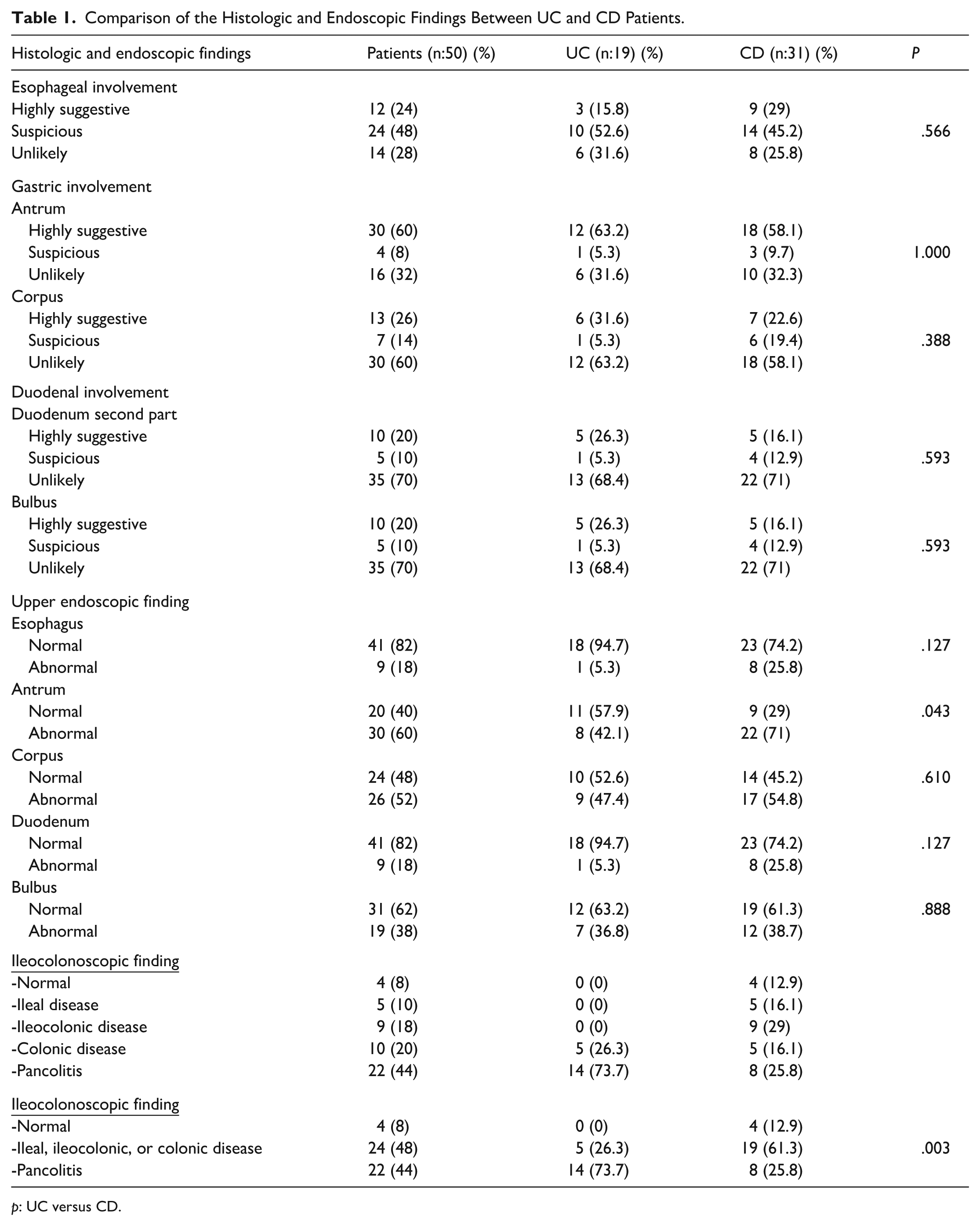
p: UC versus CD.
In the overall patient cohort, a statistically significant concordance in the presence of highly suggestive findings was observed between the duodenum and antrum (P = .03), as well as between the antrum and corpus (P = .001).
Colonoscopic findings differed between UC and CD. Pancolitis was more frequently observed in UC than in CD (73.7% vs 25.8%, respectively; P = .003). No ileal or ileocolonic disease was observed in UC; however, in CD, ileal disease and ileocolonic disease were observed in 16.1% and 29% of patients, respectively.
Correlation Between Esophagogastroscopic Findings and Highly Suggestive Histologic Findings
A correlation analysis was conducted to evaluate the association between endoscopic findings and highly suggestive histologic features indicative of UGI involvement. Significant correlations were observed in the esophagus (P = .001), duodenum (P = .043), and bulbus (P = .020), indicating that endoscopic abnormalities in these regions were more likely to correspond with histologic changes suggestive of disease involvement. In contrast, no significant associations were identified in the antrum (P = .556) or corpus (P = .424).
Association of Histologic Involvement Groups with Clinical Features, Endoscopic Activity, and Histologic Activity
Among the 50 patients, 36 (72%) exhibited highly suggestive findings in at least 1 UGI tract biopsy site (esophagus, corpus, antrum, or duodenum), while 4 (8%) showed no involvement. Additionally, 10 cases (20%) exhibited suspicious findings for involvement in at least 1 location.
Patients with highly suggestive findings were older (P = .007), while no differences were observed in gender, diagnosis, symptoms, or Mayo endoscopic score (all P > .05) among the 3 UGI tract histologic involvement groups
Highly suggestive findings in the antrum and corpus were observed more frequently in patients with higher SGS (P = .016 and .008, respectively). Among patients with higher SGS (scores ≥3), 74.4% exhibited highly suggestive findings in stomach, compared to only 28.6% of those with lower scores (scores <2). In contrast, no significant association was identified between highly suggestive findings in the duodenum and SGS (P = .327).
When overall UGI tract involvement was evaluated, defined as the presence of highly suggestive findings in at least 1 site, patients with higher SGS were more likely to exhibit such findings; however, this association did not reach statistical significance (P = .053; Supplemental Table 6). Additionally, among patients with pancolitis, 5 of 8 CD patients (62.5%) and all 14 UC patients (100%) showed highly suggestive findings. Overall, 86.4% of patients with pancolitis exhibited highly suggestive findings, compared to 60.7% of patients with other disease extents (P = .045).
Discussion
We conducted a detailed evaluation of histologic findings in UGI tract biopsies of pediatric patients and analyzed their relationship with endoscopic findings, as well as their association with the histologic disease activity score in colonoscopic biopsies.
The most common finding was FEG, which was twice as frequent in the antrum as in the corpus. Several studies have reported that FEG is more commonly observed in CD than in UC; however, it is not considered a distinguishing feature between the 2. Reported prevalence rates of FEG range from approximately 0% to 55% in UC patients and 1% to 69% in those with CD.1,3,8-11,13,19,21 Contrary to previous reports, we observed a higher prevalence of FEG in UC compared to CD, both in the antrum and the corpus, although these differences were not statistically significant.
In some studies, the frequency of FEG in IBD has been reported to be very low, in contrast to other reports. A large case series found FEG to be infrequent in CD (5%) and entirely absent in UC (0%). The authors noted that chronic active and chronic inactive gastritis were the most commonly observed forms of gastric inflammation in IBD. 1 Similarly, another study reported FEG in only 6.3% of patients, all of whom had CD, with no cases of FEG observed in UC. 21 A more recent study reported the presence of FEG in just 2% of UC cases and 1% of CD cases. 8 In that study, histologic descriptions included focal, multifocal, or diffuse inflammation, as well as superficial or deep inflammatory involvement. In our study we observed the presence of H. pylori-negative active chronic gastritis in some of the cases. Twelve of the 50 patients underwent repeat biopsies; of these, 10 initially presented with FEG but later developed H. pylori negative-active chronic gastritis, or vice versa. However, establishing a definitive association based on this finding alone remains challenging but this observation may suggest that H. pylori-negative active or inactive chronic gastritis may indicate UGI involvement. Further studies are warranted to determine whether these forms of gastritis represent histopathological features of IBD.
The variability in reported frequencies may reflect inconsistent application of FEG terminology, possibly influenced by limited awareness among general pathologists or by the tendency to classify diverse inflammatory patterns under a single descriptor owing to heavy workloads. In addition, differences in sampling practices among endoscopists, such as the number and distribution of biopsies obtained from each site, may also contribute to variability across studies, as insufficient sampling could limit the detection of this focal lesion. Moreover, considering that FEG is not a finding specific to IBD, caution should be exercised before making definitive interpretations. 19
Studies have reported that duodenitis occurs in approximately 13% to 47% of IBD cases, with a higher prevalence in CD than in UC.1,3,13,21 However, detailed histopathologic descriptions of duodenal involvement in IBD remain limited in the literature. Among patients categorized as highly suggestive for UGI involvement, the most frequently observed histologic feature in the bulb was cryptitis and/or crypt abscess formation, followed by foveolar metaplasia, crypt rupture, crypt distortion, villous blunting, basal lymphoplasmacytosis, and granuloma formation. Similarly, in the second part of the duodenum, cryptitis, and/or crypt abscess were again the most common findings, followed by villous blunting, crypt distortion, erosion/ulceration, foveolar metaplasia, crypt rupture, basal lymphoplasmacytosis, and granuloma formation. Foveolar metaplasia, a nonspecific finding reflecting chronic reactive or adaptive changes in the duodenal mucosa, is commonly seen in peptic duodenitis. 22 It has been reported as more frequent in CD than in Behçet’s disease among H. pylori–negative patients. 23 Although not specific to IBD, its presence, particularly alongside other inflammatory features, may support IBD-related mucosal injury. Assessing UGI involvement in IBD can be challenging, as subtle duodenal changes are often underestimated or labeled as nonspecific duodenitis. The combined presence of cryptitis, crypt abscesses, crypt distortion, and foveolar metaplasia may more strongly suggest IBD-related inflammation. Given the coexistence of highly suggestive findings in the antrum and duodenum, we recommend careful evaluation of duodenal biopsies for possible IBD-related changes when FEG is present in the antrum.
Although reports on esophageal involvement in IBD are limited, intraepithelial lymphocytosis, granulomas, and chronic inflammation in the lamina propria have been associated with the disease.15,24-26 While intraepithelial lymphocytosis is considered as a nonspecific finding, also reported in conditions such as infections, motility disorders, and certain medical histories, 27 it appears more frequently in IBD, particularly CD. 15 In our study, intraepithelial lymphocytosis was observed in 24% of IBD patients but in none of the controls, with no difference between UC and CD.
Granulomas have been very rarely observed in UGI tract in IBD.1,3,11,28 Although other histological findings are nonspecific, the rare presence of granulomas may be a supportive finding for CD. We found granulomas in only 4 patients with CD, with a higher likelihood of occurrence in antrum than in corpus. Duodenal granulomas were identified in only 3 patients who were diagnosed with CD. Previous studies have reported that esophageal granulomas can be detected at a frequency of 2.7% to 12%.24,25 No esophageal granulomas were observed in our cohort, likely due to the limited sampling depth of the mostly superficial biopsies, which often lacked or contained only a small portion of the lamina propria. Consequently, it was not possible to reliably assess submucosal features such as lymphoplasmacytosis or smooth muscle hypertrophy in esophagus. Obtaining deeper biopsies or performing additional sections may increase the likelihood of detecting granulomas and allow for the evaluation of other potential submucosal changes.
Studies comparing UGI tract involvement and the degree of histologic disease activity in IBD are limited. In a study by Ushiku et al, 11 no association was found between active colitis and FEG; however, an association was observed between active ileitis and FEG. 11 Highly suggestive findings, particularly in the antrum and corpus, were observed more frequently in patients with higher SGS in our study. Additionally, a relationship was identified between pancolitis and highly suggestive findings of UGI tract involvement, regardless of the underlying IBD subtype.
Although the clinical significance of UGI involvement remains unclear, a previous study reported active UGI inflammation in patients with refractory UC and suggested that it may predict response to medical therapy. 29 Prospective studies are needed to clarify whether UGI involvement is associated with poorer prognosis or warrants modifications in treatment strategies, particularly in asymptomatic patients. 19
A potential limitation of this study is that it was conducted in pediatric patients. Further research involving both pediatric and adult populations is warranted to enable comparative analysis of UGI tract involvement across age groups. Despite this limitation, our study offers a comprehensive evaluation of histologic findings in the UGI tract of pediatric patients with IBD.
Conclusion
Assessing UGI tract involvement in IBD remains challenging and may be overlooked. Careful evaluation in conjunction with clinical features is essential. Since UGI tract involvement may influence patient management and therapeutic decision-making, thorough histopathological assessment is critical, with heightened awareness of characteristic UGI findings in the context of IBD.
Supplemental Material
sj-docx-1-pdp-10.1177_10935266261431388 – Supplemental material for Upper Gastrointestinal Biopsy Findings in Pediatric Inflammatory Bowel Disease: Histologic and Clinicopathologic Correlations
Supplemental material, sj-docx-1-pdp-10.1177_10935266261431388 for Upper Gastrointestinal Biopsy Findings in Pediatric Inflammatory Bowel Disease: Histologic and Clinicopathologic Correlations by Melek Büyük, Neslihan Berker, Sidar Bağbudar, Doğu Vurallı Bakkaloğlu, Zerrin Önal, Özlem Durmaz and Mine Güllüoğlu in Pediatric and Developmental Pathology
Footnotes
Author Note
ORCID iDs
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
