Abstract
The toxicity of 3 chemical forms of beryllium (Be) was compared in this study. A total of 160 mice equally divided into 4 groups were exposed by inhalation (nose only) for 3 consecutive weeks, 5 d/week, 6 h/d. One group was used as control, while the 3 others were exposed to fine particles of Be metal, Be oxide (BeO), or Be aluminum (BeAl). Except for the controls, the target level of exposure was 250 μg/m3. In all, 35 mice/group were sacrificed 1 week postexposure and another 5 mice 3 weeks postexposure. The BeO group showed the highest lung Be concentration with higher interleukin 12 (IL-12) and interferon-γ (IFN-γ) levels, while the Be group produced the most severe lung inflammation and higher tumor necrosis factor-α (TNF-α) and CD4+ T cells levels. Data suggested that Be and BeO apparently produced more pulmonary toxicity than BeAl. However, this conclusion is not definitive, because of different confounding factors such as particle sizes, specific surface area, and solubility.
Keywords
Introduction
Beryllium (Be), a naturally occurring metal, has been utilized in aerospace, automotive, energy, defense, medical, and electronics industries for more than half a century. It is a unique material exhibiting physical and mechanical properties unmatched by any other metal. 1 The Be industry produces 3 primary forms of Be: Be alloys, Be metal, and Be oxide (BeO).2,3
Workers exposed to Be particles may develop acute Be disease, sensitization (BeS), chronic Be disease (CBD), or lung cancer. 4 Numerous studies indicate that sensitization may progress to CBD.5,6 Chronic Be disease is a progressive granulomatous lung disease characterized by mononuclear cell infiltration and granulomatous inflammation in the lungs. 7 The immunological reactions observed in affected individuals are Be-specific hypersensitivity responses involving CD4+ T-lymphocytes, production of T helper 1 (Th1) type cytokines, and the subsequent generation of granulomatous inflammation in the lungs.7–9
Cases of workers with BeS or CBD challenge the scientific community for a better understanding of Be toxicity. In 2007, the province of Quebec reduced the occupational exposure limit (OEL) from 2 to 0.15 µg/m3 for an 8-hour time-weighted average (TWA), 10 while the threshold limit value–time-weighted average (TLV-TWA) recently adopted by the American Conference of Governmental Industrial Hygienists 11 is 0.05 µg/m3 compared with the previous one of 2 µg/m3.
Beryllium-induced toxicity may be related to atmospheric concentration, particle size, chemical form, and duration of exposure.12–14 Previously, Salehi et al 15 focused on the immunologic effects resulting from a nose-only exposure of C3H/HeJ mice to fine particles of Be compared to coarse particles. Their findings suggested that exposure to fine particles may induce more pronounced inflammatory and immunological effects: higher splenocyte proliferation and higher levels of cytokine in bronchoalveolar lavage (BAL) including interleukin 12 (IL-12), tumor necrosis factor-α (TNF-α), and interferon-γ (IFN-γ).
The main objective of this study was to determine the immunotoxicity of each of the 3 chemical forms of Be particles commonly used in industries: Be metal (Be), Be oxide (BeO), or Be aluminum (BeAl). This is especially relevant since there are different prevalence rates of sensitization and CBD depending on the process and chemical form of Be.
Materials and Methods
Animals
A total of 160 C3H/HeJ 9-week-old male mice weighing between 24.9 and 25.9 g (The Jackson Laboratory, Bar Harbor, Maine) were used in this experiment. This strain, with a known mutation in TLR-4, was utilized as it may display the same chronic lung lesions as in human CBD, such as the morphology with more prominent lymphocytic infiltration, 16 allowing a better follow-up of the Th1 type immune reactions. Moreover, this strain of mice was used because Nikula et al 17 conducted a nose-only inhalation exposure to Be metal for 90 minutes with the same strain of mice as well as A/J strain. Both strains had interstitial compact aggregates of lymphocytes and granulomatous pneumonia 6 months later.
Mice were divided into 4 groups of 40; each of them was nose-only exposed in the same inhalation chamber. The first group was used as a control and was exposed to High Efficiency Particulate Filtered Air (HEPA)-filtered air, while the 3 other groups were exposed to particles of less than 5 µm of 3 different Be species (Be, BeO, and BeAl) obtained from Brush-Wellman (Cleveland, OH). Mice were housed in polycarbonate cages with stainless steel wire lids under controlled temperature and humidity, with 12:12-h light/dark cycles. Animals were given NIH-07 chow ad libitum when they were not exposed. Ethical Committee on Animal Care of the University of Quebec in Montreal approved all the experimental procedures.
Chemicals and Reagents
RPMI 1640 (GIBCO, Invitrogen Life Technologies, Mississauga, Ontario, Canada) medium was supplemented with 10% heat inactivated fetal calf serum (HyClone, Fisher Scientific, Toronto, Ontario, Canada), 100 U/mL penicillin (Invitrogen), 100 μg/mL streptomycin (Invitrogen), 2 mmol/L
Inhalation Exposure
The exposure was conducted in a metallic nose-only inhalation chamber that is able to expose 48 mice simultaneously. Be aerosol was generated, with a flow rate of 22 L air/min, by a fluidized bed aerosol generator. A stainless steel pressure tank from the American Society of Mechanical Engineers (ASME) that allowed settling of larger Be aerosol particles was used in order to obtain particles smaller than 5 μm diameter. For logistical reasons, the 4 groups were exposed alternately during 3 consecutive weeks, 5 d/week and 6 h/d. All methodological details related to the inhalation exposure, to the prevention of cross-contamination, and to human and environmental monitoring were published in Salehi et al 15 and in Muller et al.18,19 In brief, at the end of the each experiment (for a given chemical form of Be), all the sources of Be were removed from the laboratory and the generator and the inhalation chamber were cleaned. All the measuring devices, the animal husbandry cabinet, counters, doors, floors, hood, and trolley on which the mice were transported were washed with soapy water. The hatch, its walls, floor, and bench were also washed. Moreover, cleaning with soapy water was performed for the closed installations. 19 These precautions combined with the relative stability of the temperature and humidity in the laboratory and in the inhalation chamber should have avoided any significant confounding effect on the results by not having groups coming down in parallel.
The target level of exposure was 250 μg/m3. The mass median aerodynamic diameter (MMAD) was measured using a Marple Personal Cascade Impactor (Series 290) and a MOUDI (Uniform Deposit Impactor, model 100, MSP Corp., Minneapolis, Minnesota) once a week. These impactors were designed to determine the aerodynamic diameter between 0.5 to 22 μm and 0.05 µm to 10 µm, respectively. The rationale for the 250 µg/m3 concentration was provided in detail previously. 15 Briefly, this level was derived from the sole toxicological subchronic inhalation study focusing on immunological effects. Stiefel et al 20 observed increased activity of T cells in rats after exposure to 500 μg/m3. To derive a level of exposure for mice, the difference between animal species in inhalation rate and body weight was considered and similarity in dose per unit of body weight was ensured.
Sacrifice
A total of 35 mice in each group were sacrificed 1 week after the end of exposure, following intraperitoneal injection of an overdose of an anesthetic cocktail consisting of ketamine (Vetalar, 100 mg/mL), xylazine (AnaSed, 20 mg/mL), and acepromazine (Ayerst, 10 mg/mL) and exsanguinated by cardiac puncture. Blood and several tissues (spleen, liver, kidneys, and lung) were collected. The last 5 mice in each group were sacrificed 3 weeks after the end of exposure to examine the effect of recovery period on the severity of lung inflammation. The choice to sacrifice mice at 1 and 3 weeks post exposure was based on the literature review, showing that a longer latency period could induce a more pronounced inflammation.
Tissue Collection
After sacrifice, the lung, spleen, liver, and kidneys were excised, weighed, and packaged for chemical analysis. Blood samples (1-2 mL) were also collected from the abdominal aorta during the exsanguinations. Samples were immediately frozen at −45°C and stored at −70°C until their chemical analysis by Inductively Coupled Plasma Mass Spectroscopy (ICP-MS, Elan DRC II, Perkin Elmer, Concord, Ontario, Canada), according to an adapted method described in Krachler et al. 21 Briefly, the tissues were digested in 6 mL of a nitric acid (Optima Grade, 70% volume/volume [v/v]; Fisher Scientific, Ottawa, Ontario, Canada) and perchloric acid (Trace metal Grade, 70% p/p; JT Baker, Phillipsburg, New Jersey) in a proportion of 3:1. For the BeO group tissues, 500 µL of sulfuric acid (Optima Grade, 95% w/w; Fisher Scientific) were added to the 6 mL of nitric acid mixture and perchloric acid to increase the likelihood of a complete solubilization of the particles.
For each group (n = 40), a maximum of 15 lungs were used for Be analysis, 16 for BAL and 44 subsamples for histological purposes at 1 and 3 weeks after the end of exposure, respectively. For the spleen, a maximum of 18 were used for Be analysis and 20 for the flow cytometry and other immunologic analysis. Moreover, 5 were used for Be lymphocyte proliferation test (data not shown). For kidneys, liver, and blood, a maximum of 37 samples of each group were used for Be analysis. Specific sample sizes may be different because of the loss of some mice during the exposure.
Bronchoalveolar Lavage
Following euthanasia, the trachea was cannulated and 1 mL of precooled sterile phosphate-buffered saline ([PBS] GIBCO) was slowly inserted through the trachea, pooled, and collected in a 15-mL plastic tube on ice. The PBS remained in the lung for 30 seconds. The washing was repeated twice with the same volume of PBS. The BAL was aliquoted and stored at −80°C until cytokine measurement.
Cytokine Measurement
Supernatants from BAL were analyzed for ILs (IL-12, IL-2, and IL-4), for TNF-α, and for IFN-γ using specific 2-site enzyme-linked immunosorbent assay (ELISA) kits, according to instructions provided by the manufacturer (BioLegend, San Diego, CA). The measurement for each condition was performed in triplicate. The lower limits of detection for IL-12, IL-2, IL-4, TNF-α, and IFN-γ were 2, 1, 1, 2, and 4 pg/mL, respectively.
Preparation of Lymphoid Cell Suspension From Spleen
The lymphoid cells in spleen were harvested using physical disruption. Briefly, spleens were pooled from animals and placed in dissociation cups (Sigma, Mississauga, ON, Canada), containing 3 mL complete RPMI. Mononuclear cells were separated using physical disruption until mostly fibrous tissue remained. The collected cell suspensions were filtered through 75 μm cell strainers in 50 mL plastic tubes and centrifuged at 300g for 10 minutes. The cells pellets were washed twice with 1× PBS then lysed with ACK (0.15 mol/L NH4Cl, 10 mmol/L KHCO3, and 0.1 mmol/L Na2EDTA) lysing buffer to remove the red blood cells. Cells were washed and counted with an automatic counter (Coulter Corporation, Miami, Florida). The total cells were adjusted with complete medium to 2.5 × 106 cell/mL and used for the flow cytometry analysis.
Flow Cytometry Analysis
Fluorescent-labeled antibodies specific for cell surface and intracellular markers were used to determine the percentage of cells expressing CD4+, CD8+, CD19, and intracellular IFN-γ in the mononuclear cell suspension from spleen. Three-color fluorescence staining was performed using the following monoclonal antibodies, as described by Salehi et al. 15 Mononuclear cells, harvested from spleen or lungs, were incubated with a protein transport inhibitor, GolgiStop (4 μL in 6 mL) for 4 hours at 37°C. After stimulation, 1× 106 cells were washed with PBS containing 1% bovine serum albumin (BSA) and stained with anti-CD4, anti-CD8, or anti-CD19 for 30 minutes in the dark. Cells were fixed and permeabilized with Cytofix/Cytoperm (Becton Dickenson (BD), Mississaugua, ON, Canada), for 20 minutes and washed twice with 1× Perm/wash buffer (BD) then stained with anti-IFN-γ antibodies for 30 minutes at 4°C. Fluorescence intensity was detected using a FACSCalibur cytometer and CellQuest software (BD). The lymphocytes were recognized by gating in forward and side scatter based on cell granularity and size. Isotype controls were used to define negative populations.
Histological Assessment of Lung Tissues
The whole lungs were clamped off and airways were perfused with 10% neutral buffered formalin until the pleura was smooth. The heart/lung/trachea were removed and kept in formalin for 24 hours. Lungs were removed and inflated with formalin using a tissue processor (LEICA TP 1020) overnight. The left lobe was embedded in paraffin, sectioned with a microtome (LEICA RM 2125 RT) at 5 µm thicknesses, and stained with hematoxylin and eosin (H&E). An inflammation score was determined by 2 independent investigators blinded to the treatment groups and graded on a scale of 1, 2, 3, and 4, corresponding to no inflammation, mild, moderate, and severe inflammation, respectively.
Statistical Analysis
For continuous-dependent parameters, groups were compared using 1-way analyses of variance (ANOVA). Following statistically significant results with the ANOVA, pairwise comparisons were performed using the Tukey procedure. Preliminary assumptions, such as normality of residuals and homoscedasticity of variances, were verified and no major discrepancies were observed. For categorical-dependent parameters, groups were compared using the Pearson chi-square test. Pairwise associations between quantitative variables were estimated using the Pearson correlation coefficient. The significant level was set at .05, then results were considered statistically significant for P < .05. All data are presented as means ± standard deviations (SDs). All statistical analyses were performed using SPSS 9.0 (SPSS Inc, Chicago, Illinois).
Results
Based on the cascade and the MOUDI impactors, the mean MMAD ± GSD (Geometric Standard Deviation) were 0.41 ± 0.03, 1.50 ± 0.1, and 4.40 ± 1.6 μm, while the average concentrations in the inhalation chamber were 248 ± 10, 254 ± 31, and 253 ± 49 μg/m3 for BeO, Be, and BeAl, respectively. The mean daily chamber temperatures ranged from 22°C to 25°C, and relative humidity from 25% to 40%.
Table 1 shows blood and tissue concentrations. The most striking result is related to lung concentrations showing a huge discrepancy between Be species, with mice exposed to BeO displaying the highest value. Interestingly, the lung concentration found in mice exposed to BeO was significantly different (P < .05) from Be and BeAl exposed mice. Moreover, the extrapulmonary tissue levels were higher in mice exposed to BeAl except for spleen tissue, and these levels were significantly higher (P < .05), when compared with BeO and Be in kidneys and blood. Finally, the Be levels found in every extrapulmonary tissue (spleen, liver, and kidneys) were also greater in BeO-exposed mice compared to Be-exposed mice, although the differences were not significant.
Mean Be Tissue Concentrations in Mice Following Exposure to Be, BeO, and BeAl and for the Control Group a

Abbreviations: Be, beryllium; BeO, Be oxide; BeAl, Be aluminum; SD, standard deviation.
a Means with the same superscript capital letters are significantly different (P < .05).
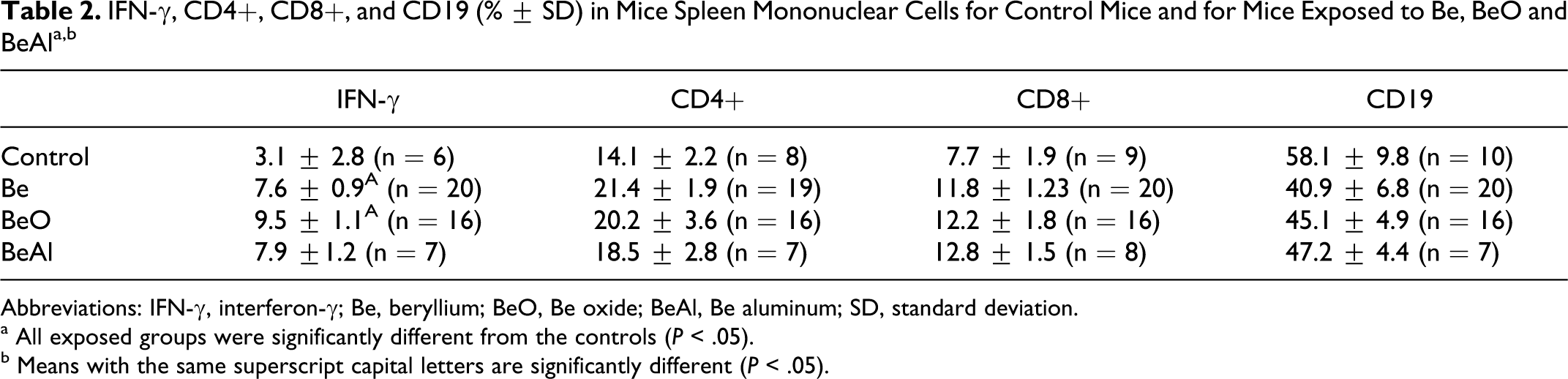
Splenic mononuclear cells expressed significantly different levels of CD4+, CD8+, CD19, and IFN-γ in all exposed mice compared to controls (Table 2). Except for the significantly higher level of IFN-γ found in mice exposed to BeO compared to Be, the different chemical forms data were in the same range for each cytokine.
Abbreviations: IFN-γ, interferon-γ; Be, beryllium; BeO, Be oxide; BeAl, Be aluminum; SD, standard deviation.
a All exposed groups were significantly different from the controls (P < .05).
b Means with the same superscript capital letters are significantly different (P < .05).
The results of the ELISA from BAL are presented in Table 3. Data indicated that significantly lower concentrations of IL-4 were obtained for the 3 exposed groups compared to controls, while IFN-γ concentration was higher in BeO. Finally, IL-12 was significantly higher in BeO compared to controls and BeAl group; and IL-2 was significantly higher in BeAl group compared to control, Be, and BeO groups.
Mean Cytokines Concentration in BAL (pg/mL ± SD) for Control Mice and for Mice Exposed to Be, BeO, and BeAl a
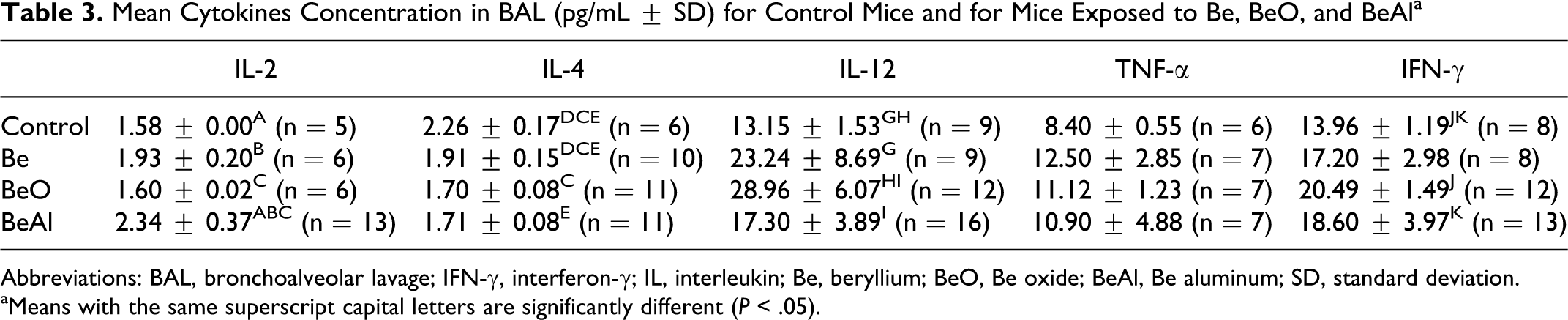

Abbreviations: BAL, bronchoalveolar lavage; IFN-γ, interferon-γ; IL, interleukin; Be, beryllium; BeO, Be oxide; BeAl, Be aluminum; SD, standard deviation.
aMeans with the same superscript capital letters are significantly different (P < .05).
Table 4 shows the distribution of the histological scores of lung inflammation in mice 1 and 3 weeks after the end of exposure compared to controls. There was a significant difference between the controls and the exposed groups in the distribution of scores. Mice exposed to Be tend to have a greater lung inflammation than mice exposed to the other chemical forms, although the difference was not significant.
Histological Scores of Lung Inflammation for the Control Group and for Mice Exposed to Be, BeO, and BeAl Sacrificed 1 and 3 Weeks After the End of Exposure
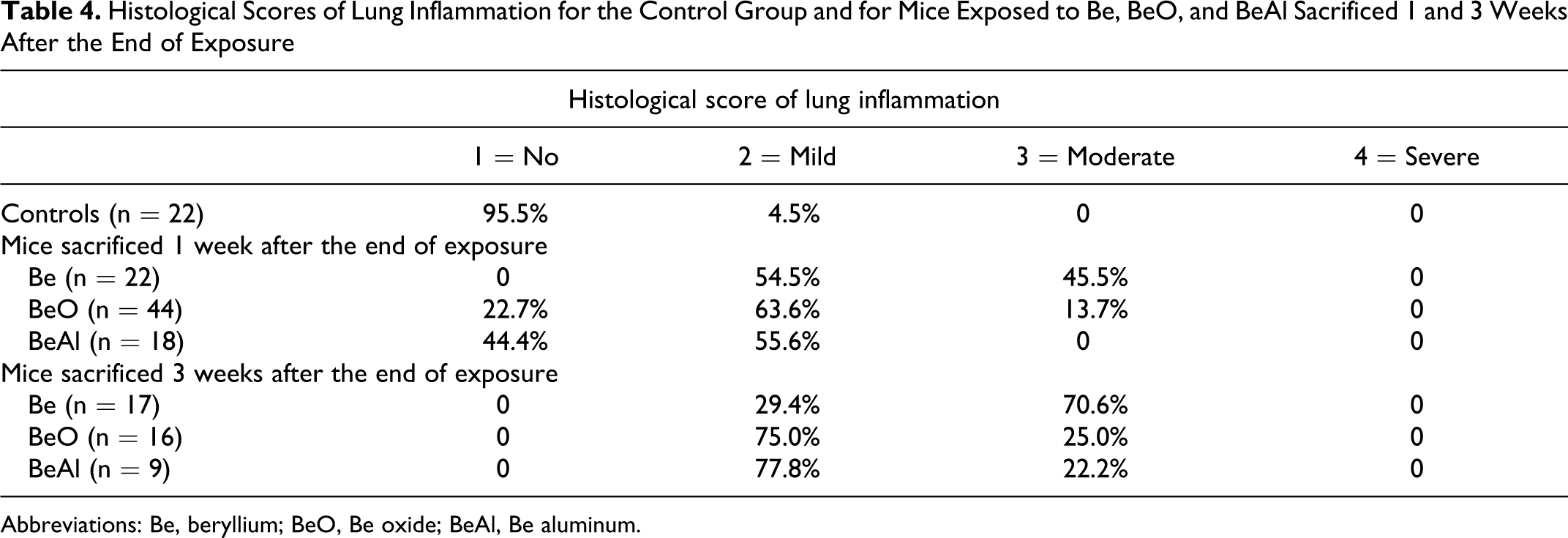
Abbreviations: Be, beryllium; BeO, Be oxide; BeAl, Be aluminum.
Moreover, the inflammation scores for mice sacrificed 3 weeks after the end of exposure were higher than those sacrificed 1 week after the end of exposure (no statistical difference). The Be- and BeO-exposed animals were characterized by a mononuclear cell infiltrate predominantly peribronchially, with some perivascular infiltration. In those animals sacrificed 3 weeks after the completion of inhalation exposure, the infiltrate was more prominent, with large granulomatus-like structures noted in the peribronchial region. The most intensive inflammation was observed in mice exposed to Be but no granuloma was observed. Photomicrographs of lung sections from representative animals within each group at ×40 magnification are presented in Figures 1 and 2.
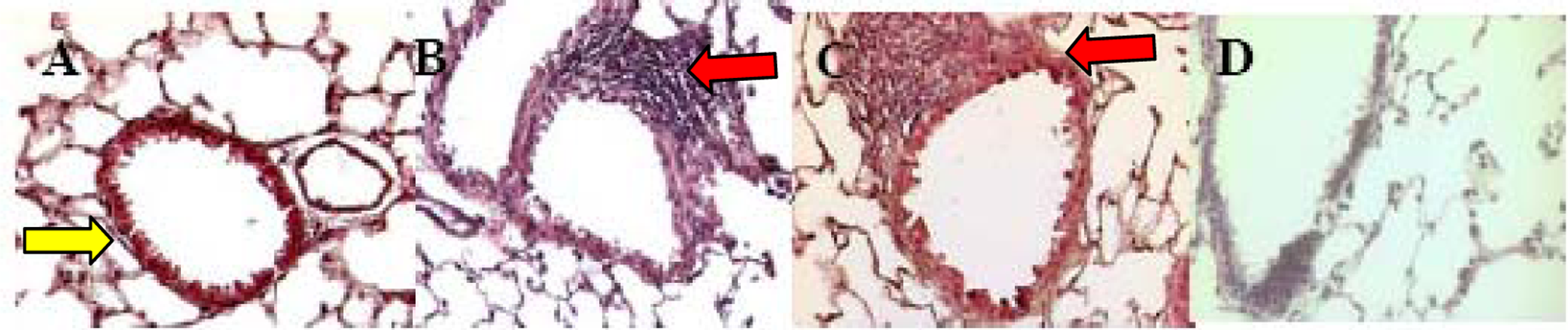
Photomicrographs (×40 magnification) of standard lung histology in control mice (A) and in those exposed to Be (B), BeO (C), and BeAl (D) sacrificed 1 week after the end of exposure. The arrow in A indicates normal airway; the arrows in B and C indicate the abnormal mononuclear cell infiltrate adjacent to the airways. Little inflammation was detected following exposure in D. Be indicates beryllium; BeO, Be oxide; BeAl, Be aluminum.
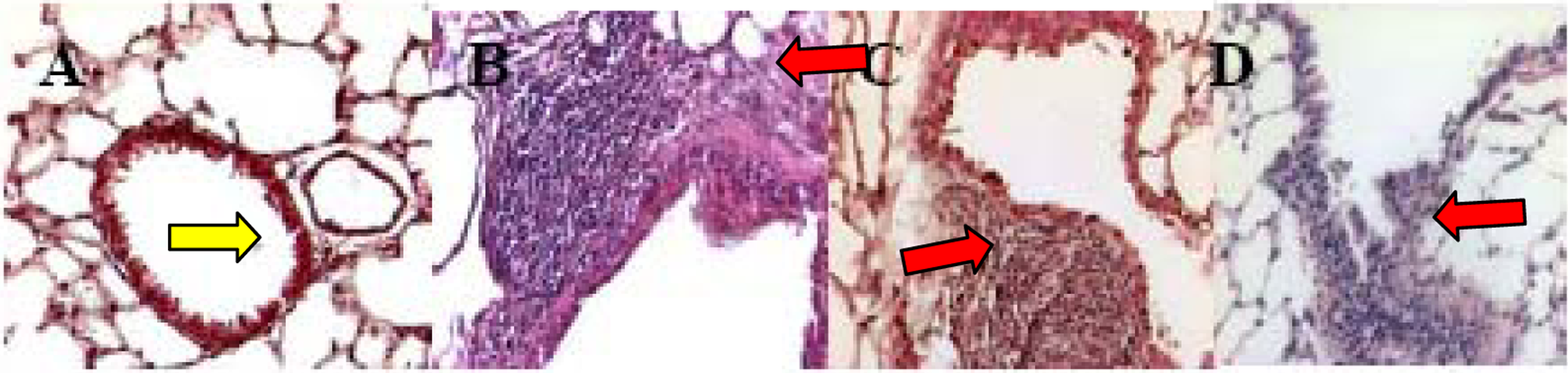
Photomicrographs (×40 magnification) of standard lung histology in control mice (A) and in those exposed to Be (B), BeO (C), and BeAl (D) sacrificed 3 weeks after the end of exposure. The arrow in A indicates normal airway; the arrows in B, C, and D indicate the abnormal mononuclear cell infiltrate adjacent to the airways. The inflammatory infiltrates were larger than those noted after 1 week and were now detected in the BeAl condition (D).Be indicates beryllium; BeO, Be oxide; BeAl, Be aluminum.
Discussion
The results showed several links between chemical form, lung inflammation, and production of some cytokines. Overall, data suggested that Be and BeO produced greater pulmonary toxicity than BeAl. The BeO group had the highest lung Be concentration with a higher IL-12 and IFN-γ, while the Be group showed more severe lung inflammation on histology. However, it is not easy to determine which chemical form between them should be considered more toxic, even if the exposure concentration was equivalent for each form. Indeed, the variation in particle size could play an important role in the rate of deposition and the internal dose to the lung.
Particle deposition in the alveolar region can eventually lead to cellular immune responses and formation of noncaseating granulomas lesions. 6 With respect to the regional deposition of inhaled monodisperse particles in mice found by Raabe et al, 22 inhaled Be with an average MMAD of 1.5 µm should show about a 50% deposition in the nasopharyngeal region, while the BeAl with an average MMAD of 4.4 µm should reach a nasopharyngeal deposition of at least 60%. Be oxide, with the smallest average MMAD of <1 µm, should have about a 15% deposition in the nasopharyngeal region. According to the same authors, the MMADs obtained in this study should lead to about 11%, 40%, and <1% deposition into the lung for Be, BeO, and BeAl, respectively. These rates of deposition correlate with the results of pulmonary concentrations measured.
The BeAl, with the largest average particle size and thus highest nasopharyngeal deposition, may be more efficiently cleared by the mucociliary escalator and ingested.23,24 Moreover, since liver, kidney, and spleen present higher BeAl tissue concentrations, we can hypothesize that a significant fraction of this chemical form is more absorbed in the lung than Be and BeO or that the BeAl cannot be rapidly excreted from the body. This may explain the lower lung concentrations.
Moreover, it has to be recognized that a greater amount of material depositing more central in the respiratory tract, as expected for BeAl, will lead to a greater relative amount of inhaled material being cleared to the gastrointestinal (GI) tract via the mucociliary escalator. This, coupled with a possibly greater solubility of BeAl, especially in the acidic milieu of the stomach, could also explain the results.
The BeAl results can also be explained by the physicochemical form of the deposited particles that has an influence on the clearance process. 25 In fact, it was suggested that relatively insoluble particles are retained in the lung more tenaciously than soluble material, favoring a longer local residence time in the respiratory tract. Data therefore indicated that BeAl, a slightly more soluble material than Be and BeO, undergoes more efficient dissolution in respiratory secretions and is more easily trapped by alveolar macrophage or dendritic cells for fine particles, resulting in a more rapid translocation of the material to lymphatic, blood, and other tissue excreta.23,26–29 Interestingly, this finding was also demonstrated in Muller et al, 18 where the urinary Be levels were higher for the BeAl-exposed group compared to the Be and BeO groups during and after the exposure.
Be oxide, with the lowest MMAD and the highest lung deposition together with its poor water solubility, is likely to have a longer local residency in the respiratory tract, more specifically in the alveolar space, than the other studied Be forms. It is the BeO form that showed the highest IL-12 and IFN-γ concentrations in the BAL albeit the Be form was associated with the highest histological scores of lung inflammation.
The results of standard histology showed that an exposure to any of the 3 chemical forms of Be can induce lung inflammation in mice. This subchronic exposure led to similar histology compared to that observed in patients with CBD, although Nikula et al 17 and Finch et al 30 established that lung effects in humans seem to be greater than those seen in animal models. However, these investigators observed some microgranulomas and severe aggregated lymphocytes after exposure to high levels of Be. The data also showed that Be exposed group develop more areas of moderate inflammation, suggesting a significant link between lung inflammation and chemical form. This finding is consistent with other animal studies that were conducted to investigate pulmonary effects following Be exposure.16,29,31
In the present study, mice sacrificed 3 weeks after the end of exposure showed a more advanced lung inflammation compared to those sacrificed only 1 week after, as measured by the number of animals with moderate inflammatory changes. This is consistent with the results obtained in Salehi et al 15 and also in agreement with those of another nose-only inhalation study where mice from the same strain were exposed to Be metal for 90 minutes and developed interstitial compact aggregates of lymphocytes and granulomatous pneumonia 6 months later. 17 Haley et al 32 explained that interstitial infiltration of lung is dose-dependent and severity of lung lesions increased with time and lung burden. All these results indicate that lung inflammation continues, even potentially increases, after the cessation of exposure. As suggested by Stefaniak et al, 33 the Be particles retained in the lung may undergo dissolution slowly and may contribute to Be dosimetry for years after the exposure has ceased. The long-term retention of Be in lung and slow mobilization of this material are important factors in producing CBD in sensitive individuals. 29
It has been established that the development of granulomatous inflammation in the lungs of patients with CBD is associated with activation and accumulation of CD4+ T cells. 9 Although the exact nature of Be antigen is unknown, there is evidence suggesting that Be ions may become complexes with peptides that are ultimately recognized by CD4+, inducing BeS. 25 In this study, Be groups expressed significantly more CD4+ T cells compared to control.
T cells are activated in the presence of Be antigen and upon contact, they produce and release proinflammatory Th1-type cytokines, mostly, IFN-γ, TNF-α, and IL-2. 34 These immunological activities lead to the formation of noncaseating granulomas in the lungs. Tumor necrosis Factor-α, produced by activated cells of both neutrophils and macrophages, may exert effects on cell recruitment at sites of inflammation and, eventually, induce granulomatous structures. 35 In host defense, IL-2 and IFN-γ induce protective cell-mediated immunity and delayed-type hypersensitivity reactions. 36
Data from the BAL cytokine assessment indicate a pattern of Th1-type cytokine secretion in mice exposed to Be. This group expresses more TNF-α, while BeO group expresses more IFN-γ and IL-12. The latter is another proinflammatory cytokine mostly produced by phagocytic cells which is essential for the proliferation of activated T cells and IFN-γ secretion from activated T cells. Interleukin 12 also prevents apoptosis of CD4+ cells. 37 Note that the IL-2 and IL-4 levels obtained in this study are too low to be reliably quantified.
In conclusion, the main results indicated that Be and BeO seemed to induce more toxicity than BeAl. However, one need to be cautious with this interpretation, because the BeAl particle size is quite larger than the other particle forms, and this difference does not allow a real appreciation of the effects of each chemical form. Indeed, the rate of lung deposition clearly influences the immunological effects resulting from the inhalation exposure. Given the increasing concerns over the immunologic aspects of Be, it is of utmost interest to researchers/environmental regulation agencies to better understand how and which form of Be induce the greatest threat to human health.
Footnotes
Acknowledgments
The authors enormously appreciate the professional advice of Yves Cloutier and Vincent Paquette from the IRSST and the technical supports of Elmira Aliyeva, Lise Gareau, Natalya Karp, Issa Lozano, Julienne Lama and Louis Zayed. Dr Mazer is a Chercheur-National supported by the Fonds de la Recherche en Santé du Québec.
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
This research was supported by the Institut de recherche Robert-Sauvé en santé et en sécurité du travail (IRSST) [IRSST099-320], and the Costello Foundation.