Abstract
The rise in depressive and anxious symptoms in postsecondary students has marked a significant increase in demand for mental services. In a context of limited resources, multilevel approaches are recommended. The present study examines the predictive link between demographic factors, depressive and anxious symptoms, and acquired learning, following a universal prevention (UP) intervention, and the choice to actively participate or not in a targeted prevention (TP) intervention. The study utilized binary logistic regression and focused on 967 symptomatic postsecondary students. Results showed that higher weekly work hours diminished the likelihood of participating, whereas higher academic goals increased the likelihood. In addition, we examined whether baseline sociodemographic factors moderated the efficacy of the TP intervention. Mother’s education level was a significant moderator but not weekly work hours, study hours, or grades. The current study highlights the varied ways in which sociodemographic characteristics influence participation and efficacy of prevention interventions.
Keywords
Depressive and anxious symptoms, characterized by sadness, worry, irritability, fatigue, insomnia, feelings of guilt, and difficulty concentrating (American Psychiatric Association, 2013), are associated with risk of dropout and impaired quality of life in college students (Auerbach et al., 2018). Furthermore, increases in distress have been documented over the last 25 years, especially in young people aged 18 to 34 (Blanco et al., 2008; Stallman, 2010). The presence of a depressive episode, if not treated, increases the likelihood of subsequent episodes by 30%, with future episodes occurring closer together over time (Richards, 2011). As reported by Auerbach et al. (2018), the World Health Organization (WHO) World Mental Health International College Student survey showed that demands for mental health services far exceed available resources. Studies have also demonstrated that less than 50% of students identified with problematic internalized symptoms receive services (Cheung et al., 2019; Merikangas et al., 2011). Thus, there is an urgent need to develop accessible cost-effective prevention strategies, to identify high-risk students for more targeted intervention, and to match the intervention level to the needs of each student. Multilevel prevention programs pursue these goals through a stepped approach. Existing programs are promising, but they present several limitations and are rarely multilevel.
School-Based Prevention Programs for Internalizing Disorders in Postsecondary Students
School-based mental health services reduce barriers that have been shown to be associated with service access, including cost, geographic location, and stigma. Results of two meta-analyses supported the efficacy of cognitive-behavioral universal (Conley et al., 2015) and targeted (Conley et al., 2017) prevention programs for the reduction of depressive symptoms in postsecondary students. Post-test and follow-up effect sizes were around .60 for targeted programs. The authors found that targeted interventions showed higher effect sizes than universal interventions. An additional meta-analysis by Breedvelt et al. (2018), however, did not find any link between efficacy and study characteristics, such as level of intervention, underlying theoretical framework, or specific symptom focus. This meta-analysis included studies with student and non-student samples, which the authors suggested may explain their contradictory findings. Higher effect sizes in depression-specific interventions (e.g., compared to stress reduction) have been explained by the fact that programs explicitly designed to address depressive symptoms contain more components that directly target risk factors for depression (Amanvermez et al., 2021; Breedvelt et al., 2018; Conley et al., 2017). Regarding universal interventions, Conley and colleagues (2015) found that these interventions were especially effective in reducing anxious and depressive symptoms when they included a supervised skills practice component and focused on graduate rather than first-year college students. Graduate students may be more motivated, more mature, and have more experience managing the stress of higher education. However, first-year college students have been identified as the most at risk of experiencing distress and dropping out (Arria et al., 2013), suggesting that effective programs for freshman college students are especially desirable.
Existing examinations of prevention programs present several limitations, including a lack of published protocol manuals, which compromises implementation fidelity across sites and studies, and the absence of an evaluation of long-term outcomes or intervention efficacy on specific program determinants (see Marcotte et al. [2024] for an exception). Meta-analyses have reported that programs are generally not designed expressly to prevent internalizing disorders; however, depressive or anxious symptom changes are often the only outcomes measured. Moreover, a central limitation of the prevention field that must be addressed is the lack of comprehensive multilevel prevention programs specifically designed for delivery in the school or college context.
The Need for a Multilevel Approach
Traditional approaches to identifying at-risk students and delivering mental health services in schools and colleges have generally been reactive and, above all, incomplete (Romer et al., 2020). Methods such as the occurrence of disciplinary incidents or teacher/instructor referrals may be efficient for identifying students presenting externalizing problems; however, they are not effective for identifying students with less observable internalizing symptoms. Moreover, in their drive for autonomy, emergent adults may be more reluctant to access services and may try to resolve their emotional problems alone and/or minimize the intensity of their symptoms (Eisenberg et al., 2012). Multilevel approaches are proactive, as they rely on systematic screening procedures and offer a continuum of interventions adapted to each student’s needs (Romer et al., 2020).
There is a growing interest in adopting this type of multilevel service delivery (Fabiano & Evans, 2019) in the postsecondary context. However, this approach has rarely been applied in tertiary institutions. The present study adopted Christner and Mennuti’s (2009) and Christner et al.’s (2011) multilevel model of mental health services delivery in a postsecondary educational setting. These authors suggest first offering a universal prevention (UP) intervention, either to specific grades or the entire student body, with this level usually being implemented by instructors during a regular class. The objective of the UP level is to foster individual protective factors and to reduce vulnerability including decreasing the use of maladaptive coping strategies, in order to avert difficulties before they occur. This level also centers on providing information about various available resources (e.g., tutoring, peer support). UP interventions are generally able to respond to the needs of up to 85% of students (Christner & Mennuti, 2009). Furthermore, the UP level should include a screening procedure to identify at-risk students, and identified students should then be offered a more targeted intervention, most often in a small group format over multiple sessions. Targeted interventions typically aim to increase knowledge about mental health and stress management and provide opportunities for practicing newly developed skills. Targeted prevention (TP) interventions are generally based on one or more evidence-based approaches such as behavioral activation, anxiety management, cognitive restructuring, and social skills learning. Finally, identified students who meet the diagnostic criteria for mental health disorders should be referred for individual treatment.
Overall, the research examining mental health prevention programs has provided promising results for reducing distress in young people in postsecondary school contexts. Multiple meta-analyses report reductions in symptoms following UP and TP interventions, even when programs were not specifically designed to address clinical symptoms. Although systematic screening procedures are beginning to be included in prevention programs, their use remains inconsistent, and when they are implemented, it is generally without being fully integrated into a multilevel model. Finally, despite increased interest in multilevel approaches in school contexts, still very few studies have implemented both a universal and a targeted intervention in a single integrated program. Thus, the cumulative or interactive effects of sequential levels of prevention intervention remain unknown.
The Aims of the Present Study
The present study applied a multilevel prevention program with both UP and TP interventions and a systematic screening procedure for identifying at-risk students, in a sample of postsecondary students. Two study aims were pursued: (1) to examine whether sociodemographic factors, symptoms, or acquired learning in at-risk UP participants influenced their decision to participate or not, in the TP intervention and (2) to examine whether current symptoms of distress, level of mother’s education, work hours, study hours, or grades influenced the efficacy of the TP intervention.
Method
Procedure
This study is part of a longitudinal quasi-experimental multilevel prevention project called Zenstudies: making a healthy transition to college. Dissemination and evaluative study of the program in Québec cégeps within six Quebec postsecondary institutions across the province. Zenstudies: Making a Healthy Transition to Higher Education is a mental health prevention program first published in French by (Marcotte et al., 2016) and in English in 2021 (Marcotte et al., 2021). This multilevel program comprises a UP intervention and a TP intervention. The UP intervention consists of a 75- to 90-minute in-class workshop delivered by class instructors. This workshop aims to foster knowledge about mental health and strategies for making a successful transition to college. To assess learning on these topics, we utilized a brief 6-item scale (the Quiz) administered pre, post, and follow-up the UP workshop. In addition, students were screened for anxiety and depression symptoms using two surveys derived from the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) diagnostic criteria. Those students who exhibited clinical levels of symptoms were eligible for further intervention. For more details on the UP intervention, see Marcotte and colleagues (2023, 2024). The TP intervention consists of ten 90-minute workshops hosted by two mental health professionals. These workshops focus on mental health knowledge including cognitive-behavioral principles, mindfulness, and anxiety management (e.g., graded exposure). The intervention also aims to develop feelings of belonging to college and academic, career, and life goals and values. For more details on the TP intervention, see Marcotte and colleagues (2024). TP participants completed online measures pre (Time 1, T1), post (Time 2, T2), and 3 months later (Time 3, T3). All participants completed the study in French. Ethical approval for the overall project was issued by the ethics committee of the University du Québec à Montréal, and participants were compensated CND$15–40.
Participants
All participants in the current study were students at the preuniversity CEGEP (Collège d’Enseignement Général et Professionnel) level of education, across the province of Quebec. Students in Quebec graduate secondary school at the end of Grade 11 and proceed to CEGEP for 2 years of preuniversity or vocational training. Thus, in general, CEGEP students are the equivalent of grade 12 and freshmen college students in the United States, while some older students seeking to acquire the necessary qualifications for university entrance may also be present. In total, students from six geographically dispersed CEGEPs participated in the current study.
For details of the participation selection process, see Figure 1. The current study focused on two samples of participants, one from each program level. The initial UP sample included 2,400 students. Of these, 1,336 did not meet the symptom criteria for continuation, and 97 were eliminated from the analyses because they were older than the upper limit of Arnett’s (2000) emerging adult age criteria (≥ 30 years), or they did not provide postintervention data. Independent-samples T-tests showed that the 97 eliminated participants were older, t(69.35) = 10.67, p < .001, and they reported lower depressive, t(912) = −8.52, p < .001, and anxious symptoms, t(62.77) = −8.61, p < .001. They did not differ on preworkshop quiz scores, t(48.76) = −1.75, p = .086, from retained participants. Thus, the final sample of UP-identified participants included 967 students with clinical levels of symptoms, a mean age of 19.92 years (range = 16–29; SD = 2.02), 75.1% identified as female, 24.0% as male, .2% as non-binary, and .7% did not report on gender. The majority endorsed North American (88.2%) cultural identity, and the remaining 11.8% endorsed a variety of different cultural identities including African, Asian, European, and Latin American.
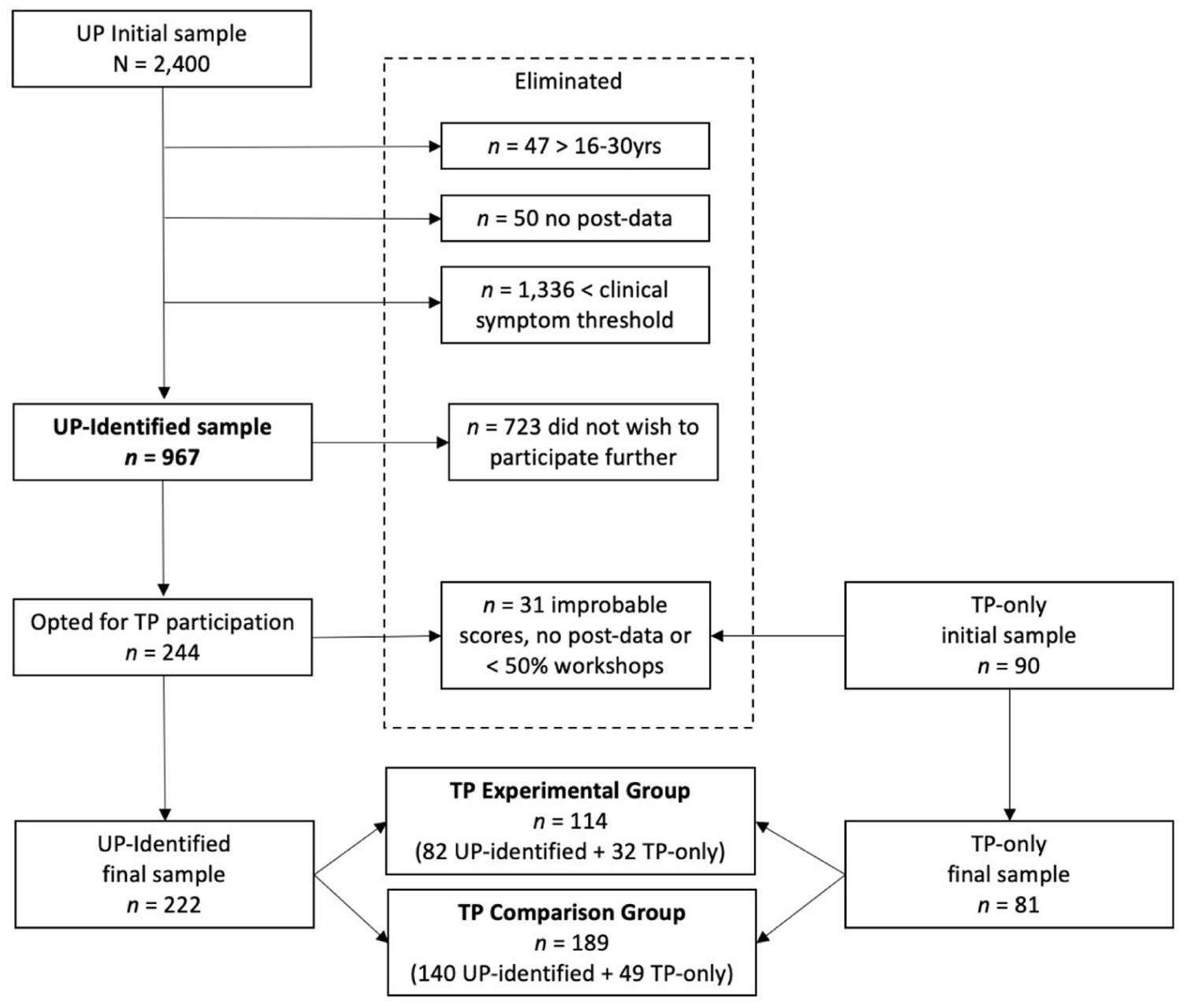
Flowchart of the Selection of Study Participants.
Our second sample included students who completed the TP intervention. Of the previous 967 UP-identified students, 244 opted to continue to the TP, and 90 new students experiencing symptoms entered the TP directly. Of these 334 students, 31 were eliminated from the analyses, either because they did not provide T2 data, they had improbable scores, or they attended less than 50% of the workshops. Independent-samples T-tests showed that the eliminated participants had higher T1 depressive symptoms, t(292) = 2.73, p = .007; however, they did not differ on age (p = .077), or T1 anxious symptoms (p = .933) from the retained sample. Thus, the final TP sample was composed of 303 students (114 experimental, 189 comparison), with a mean age of 17.52 years (SD = 1.54), 79.2% identified as female, 13.9% as male, 6.9% did not report on gender, and no students reported non-binary or transgender identity. The majority endorsed North American (86.8%) cultural identity, and the remainder a variety of other identities (e.g., African, Asian, European and Latin American).
Measures
During both the UP and the TP, participants completed a sociodemographic survey, including age, gender and sexuality, cultural identity, student status, hours studying, and hours working. In addition, they reported on their mother’s completed education (from 1 = primary school to 4 = university, 0 = if unknown), and the UP participants also reported their education goals (from 1 = secondary school is sufficient to 3 = I plan on going to university, 0 = if undecided).
Measures in the UP-Identified Sample
Current symptoms during the UP were assessed using two brief scales derived from the DSM-5 criteria for generalized anxiety and major depression (APA, 2013). Items were rated as present or absent. Scores of five or more for depression, and four or more for anxiety were considered clinically significant.
To assess mental health knowledge and the transition to college, a brief questionnaire (called the Quiz) comprising six items was administered pre and post the UP intervention. Items assessed transition-related beliefs (e.g., I should know what I want to do with my life, by the time I arrive in college), mental health (e.g., Being in good mental health means not experiencing symptoms of anxiety or stress), and knowledge of strategies for promoting mental wellness (e.g., Engaging in pleasant activities is an effective strategy for coping with depressive feelings). Items were rated from 1 completely true to 4 completely false and mean total pre- and post-scores were calculated. To indicate quiz learning, a pre- to post-difference score was computed.
Measures in the TP Sample
Depressive and Anxious Symptoms
Depressive symptoms were assessed with the Beck Depression Inventory-II (BDI-II; Beck et al., 1996), comprising 21 items across the past 2 weeks. Items are rated 0–3 (range = 0–63) and higher scores indicate more depressive symptoms. The Beck Anxiety Inventory (BAI, Beck & Steer, 1990) was utilized to assess symptoms of anxiety in the past week. The BAI comprises 21 items, rated from 0 to 3 (range = 0–63). Higher scores indicate more anxious symptoms. Studies have supported the validity and reliability of the French BDI-II and BAI (see Bouvard & Cottraux, 2010 for details). In the current study, T1 Cronbach’s alphas were BDI, α = .91 and BAI, α = .92.
Analytic Strategy
Preliminary analyses included intercorrelations and descriptives for non-categorical variables in each sample. Then, two distinct analytic approaches were adopted. First, in the UP-identified (n = 967) sample, we conducted binary logistic regressions to examine whether demographic factors, clinical symptoms, or quiz learning predicted the likelihood of actively participating in the TP, compared to opting out or joining the nonactive comparison group. These analyses were conducted using SPSS Statistics, v28 (IBM, 2021), and all predictors were coded to be continuous. Second, in the TP participants (n = 303), we completed moderation analyses to examine whether changes in BDI and BAI, differed by level of mother’s education (secondary school, CEGEP, university), weekly work hours (none, 1–10, >10), weekly study hours (<6, 6 to 9, >9), or grades (below average, average, above average). We utilized Hayes’s PROCESS macro (v4.2, 2022) for SPSS. Change scores were calculated by subtracting T1 from T3 scores, and, as all moderators were ordinal, we selected sequential coding, such that each level was compared to the level directly below. PROCESS provides an overall model score and a change of R2 score (ΔR2) for the interaction. In addition, PROCESS uses a bootstrap procedure to estimate bias-corrected 95% confidence intervals (CIs) to test moderation significance. This bootstrapping procedure overcomes the limitations of previous stepwise approaches, yielding results that are less impacted by sample size (Hayes, 2009).
Results
Preliminary Analyses
T1 intercorrelations, means, and standard deviations for the UP-identified sample are presented in Table 1. Age was positively related to work hours, but not clinical symptoms or quiz learning. Work hours were significantly related to more depressive but not anxious symptoms. Depressive and anxious symptoms were significantly positively correlated. Anxious symptoms were the only variable related to higher quiz learning. In the TP participants, the correlation between changes in depressive and anxious symptoms was positive and significant (r = .39, p < .001).
Intercorrelations, Means, and Standard Deviations in the UP-Identified Sample.
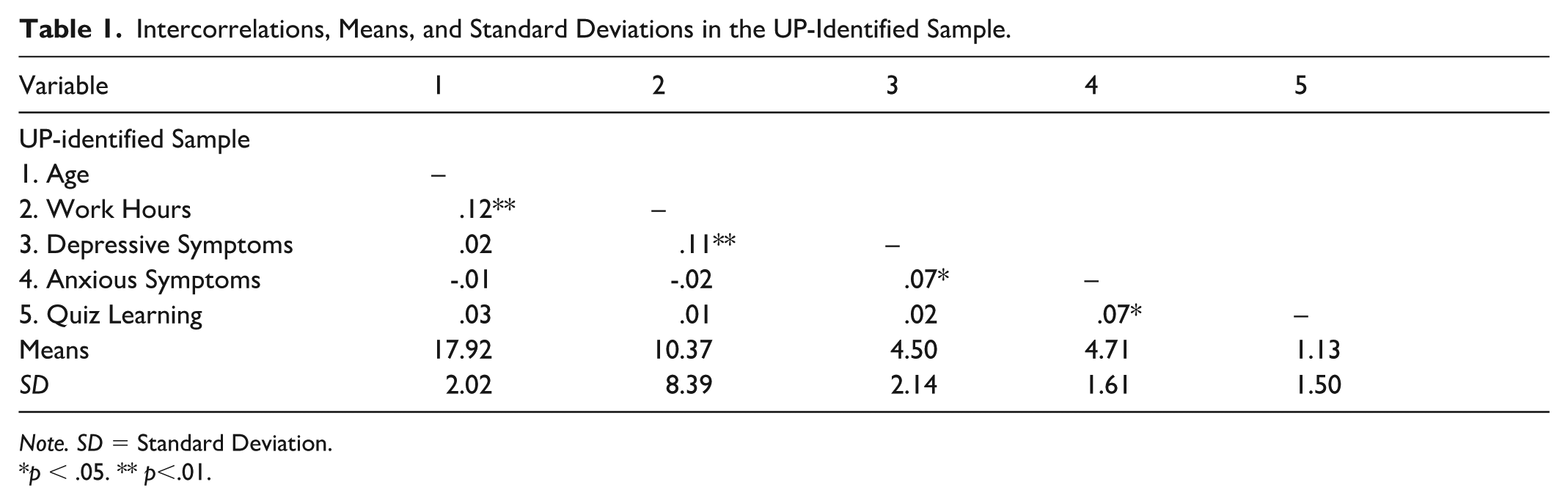
Note. SD = Standard Deviation.
p < .05. ** p<.01.
Binary Logistic Regression Analyses in the UP-Identified Participants
We conducted three binary logistic regressions to examine whether (1) sociodemographic factors, (2) symptoms, or (3) quiz learning, predicted the likelihood of actively participating in the TP intervention (dependent variable: [1] Yes, join the TP experimental group, [0] No, join the TP comparison group or opt-out). Table 2 summarizes the results.
Binary Logistic Regressions in the Universal Prevention-Identified Participants.
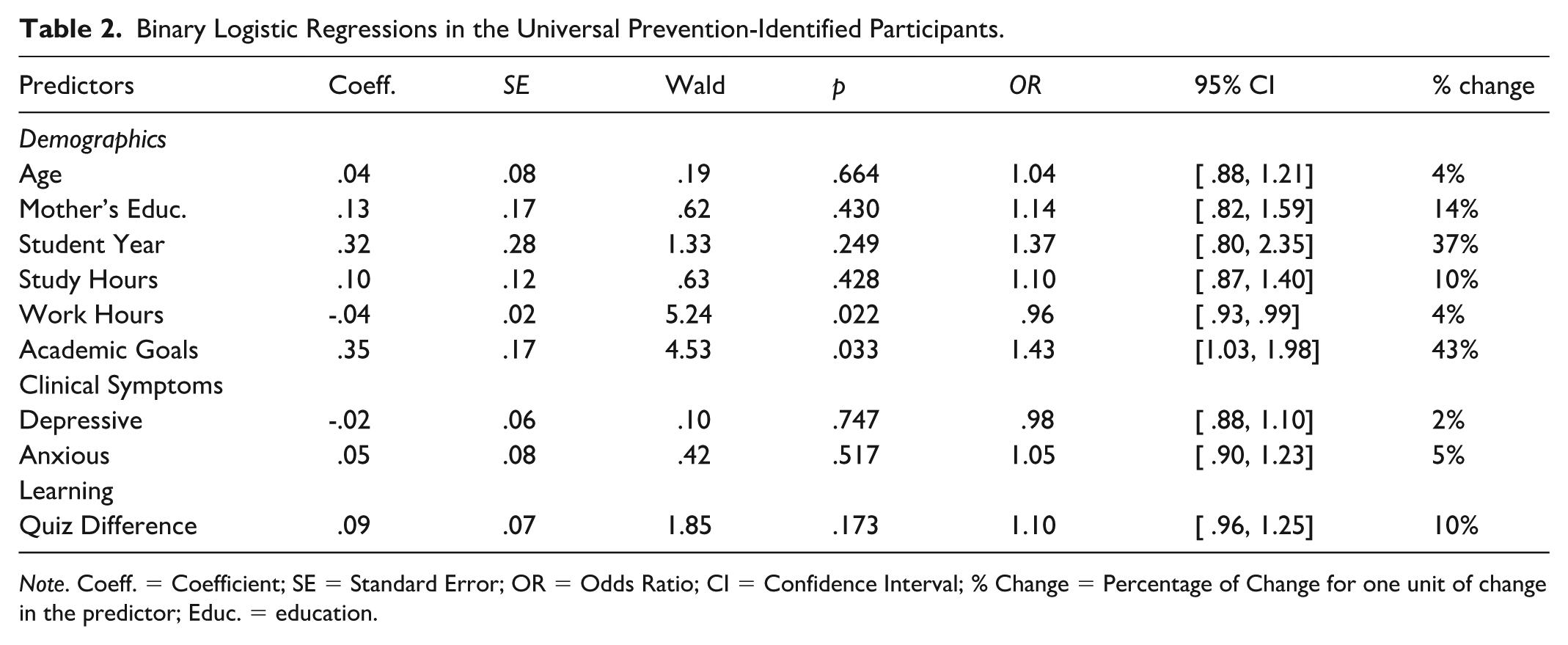
Note. Coeff. = Coefficient; SE = Standard Error; OR = Odds Ratio; CI = Confidence Interval; % Change = Percentage of Change for one unit of change in the predictor; Educ. = education.
First, we examined whether age, mother’s education level, student year, study hours, work hours, or academic goals increased the likelihood of opting for the experimental group. Regarding model fit, the chi-square, χ²(6) = 14.36, p = .026, indicated that our model was significantly better than an intercept-only model. The Cox and Snell (R2= .023), the Nagelkerke (R2= .048), and the nonsignificant Hosmer and Lemeshow test, χ2(8) = 13.51, p = .095, also supported our model (Tabachnick et al., 2013). The classification table indicated that the model exhibited excellent specificity with 100% of those not opting for the TP experimental group being predicted; however, the model exhibited poor sensitivity, since none of those who opted for the TP experimental group were predicted. Regarding the regressions, work hours, b = −.041, SE = .02, Wald χ²(1) = 5.24, p = .022, and academic goals, b = .354, SE= .166, Wald χ²(1) = 4.53, p = .033, were the only significant factors. Transformation of the odds ratios into percentages of change (Pampel, 2020) indicated that the odds of active participation (OR = .96, CI = [.93, .99]), decreased by 4% per unit increase in work hours, and the odds (OR = 1.43, CI = [1.03, 1.98]), increased by 43% per unit increase in academic goals.
Second, we examined whether UP reported depressive or anxious symptoms predicted the likelihood of active TP participation. The chi-square, χ²(2) = .50, p = .779, the Cox and Snell (R2 = .001) and the Nagelkerke (R2 = .001) did not support the model, although the Hosmer and Lemeshow test, χ2(8) = 4.68, p = .791, did. The classification table again showed excellent specificity (100% prediction of not opting-in to the experimental group), but poor sensitivity (0% prediction of opting-in). For the regressions, neither UP anxious (p = .517), nor UP depressive symptoms (p = .747) predicted active TP participation.
Finally, for amount of quiz learning, the chi-square, χ²(1) = 1.76, p =.184, the Cox and Snell (R2 =.002) and the Nagelkerke (R2 = .004) did not support the model, although the Hosmer and Lemeshow test, χ2(3) = 6.33, p = .097, did. The classification table again showed excellent specificity but poor sensitivity, and greater learning during the UP did not predict active participation in the TP (p = .173).
Moderation Analyses in the TP Participants
To investigate whether T1 sociodemographic factors impacted the efficacy of the TP intervention, we conducted moderation analyses examining changes (T3 minus T1 scores) in BDI and BAI, by level of mother’s education, work hours, study hours, or grades. The only significant moderation was for mother’s education level and changes in depressive symptoms. Table 3 presents the model summary, change in R2 scores, and the conditional slopes for mother’s education level. The conditional slope analyses showed that depressive symptoms decreased significantly more in the experimental group, in the mothers who completed secondary school and those who completed university, but not in the mothers who completed preuniversity CEGEP.
Moderation Analyses in the Targeted Prevention Participants.
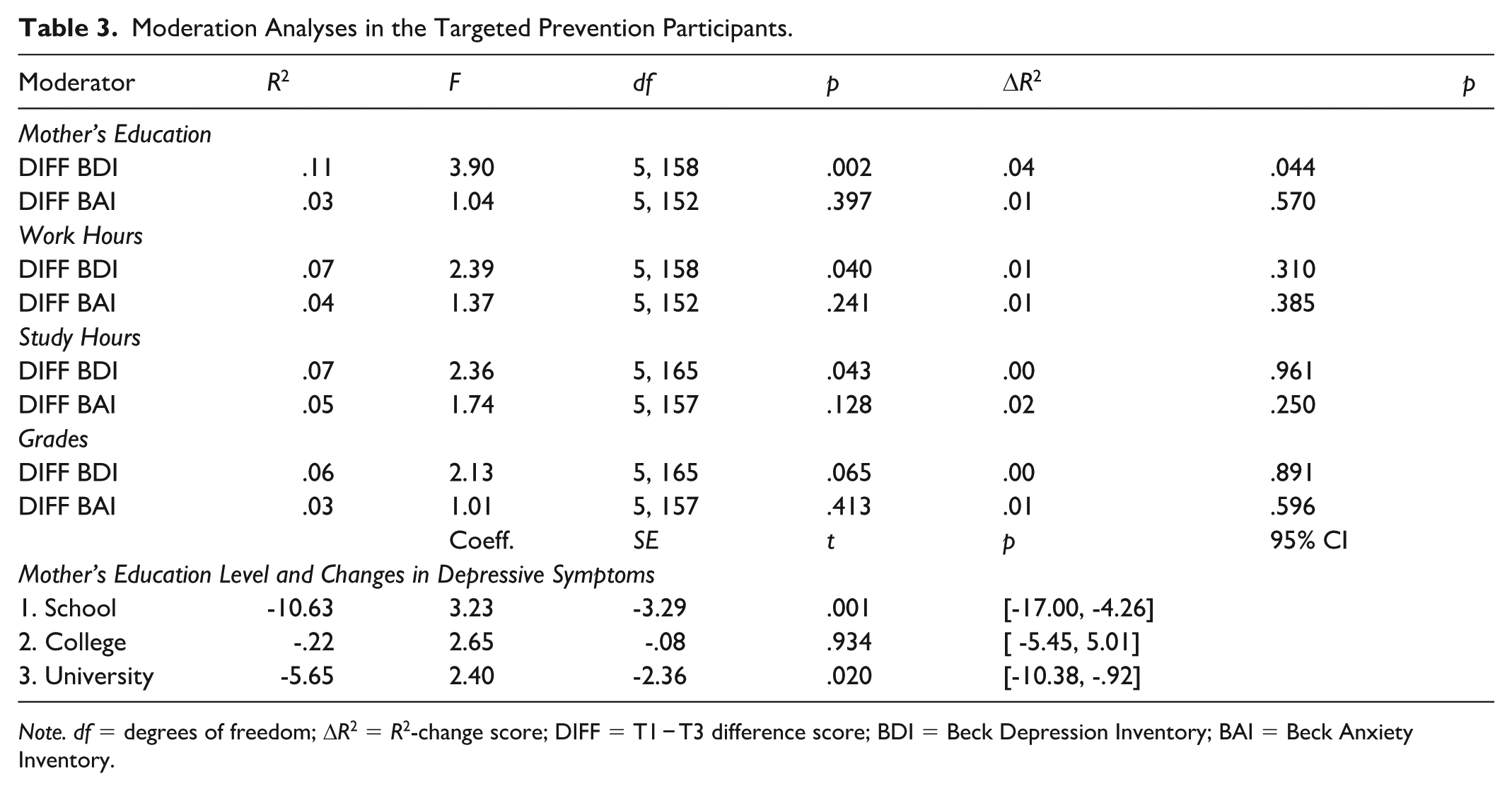
Note. df = degrees of freedom; ΔR2 = R2-change score; DIFF = T1 − T3 difference score; BDI = Beck Depression Inventory; BAI = Beck Anxiety Inventory.
Discussion
The present study provides empirical support for the need to orient mental health interventions and programs in tertiary education institutions toward multilevel prevention programs. Zenstudies is an integrated multilevel program designed to prevent depressive and anxious symptoms in students experiencing the transition to postsecondary education. As is common in the prevention field, Zenstudies utilizes reported depressive and anxious symptoms as the criteria for identifying at-risk students who are eligible for the targeted level of the program. This criterion makes sense when implementing an intervention that specifically targets distress prevention. However, there is a lack of research examining the relationship between participant characteristics and opting-in to targeted programs, or their downstream effects on intervention efficacy. The current study sought to address this lacuna using a two-step approach. First, in a sample of students who completed the UP and were eligible for further intervention, we identified which individual characteristics influenced participant decisions to actively participate or not in the TP intervention. Second, in those participants who opted for the TP intervention, we examined whether their sociodemographic characteristics moderated the efficacy of the TP intervention on clinical symptoms.
Surprising and contrary to our expectation, results showed that the intensity of current depressive or anxious symptoms did not constitute a significant predictor of continued participation. Several hypotheses may explain this result. First, despite reporting current clinical levels of symptoms, participation in the UP intervention may have been sufficient for some students to feel that they were now adequately equipped to deal with their distress themselves, using the tools they had acquired. Second, given that emergent adulthood is a period of accrued independence, some students may have believed that they could manage their emotional distress without external assistance (Eisenberg et al., 2012). Finally, given that the entire sample exhibited depressive and/or anxious symptoms, this result may be a type 2 error due to a small variance between the groups. Additional studies, with larger samples, are necessary to shed more light on this finding.
We also examined several sociodemographic variables, and results indicated that work hours and academic goals significantly influenced the decision to participate in the TP. In particular, elevated academic goals were an important motivator for opting-in (43% increased likelihood). These students may have considered the opportunity to increase their skill set and knowledge for coping with their current distress, as a means to further their school performance and, by consequence, their academic success. This finding is in line with existent studies supporting a positive relationship between mental health and academic success (Garcia, 2016). Furthermore, previous research on attitudes and knowledge regarding the uptake of mental health services has shown that, in an economic model, the benefits of asking for help must be greater than the cost (Eisenberg et al., 2012). Although participation in the program interventions was free, there were still associated non-monetary costs such as time required to complete the workshops, as well as potential embarrassment and shame. Thus, it is possible that those students with high academic goals were more likely to participate because they viewed their participation as a worthy investment toward academic success. Conversely, our results showed a significant negative relationship for the number of weekly work hours, such that the more hours worked, the less likely participants were to opt-in. Applying the economic model to understanding this result, students who were already working in addition to classes, may have concluded that more intensive participation (10 weekly workshops) was too costly. From a normative perspective, an important question is when and whether help-seeking is necessary. Emerging adults may not be best equipped to make cost–benefit analyses of this question, either because they are not sufficiently knowledgeable about mental health issues, or because they do not adequately assess their own symptoms. Previous research suggests that many young people do not know that treatments for anxiety and depression are effective (Eisenberg et al., 2012). A recent Danish study (Leick et al., 2022) examining participation in a program to prevent lifestyle-related diseases reported that 53% of participants who had refused to participate exhibited at least one risky health behavior (e.g., smoking, poor diet). Refusals were associated with lack of time but also with participant’s beliefs that they were healthy and had healthy lifestyle habits.
The final factor influencing choice to participate that we considered was the level of knowledge acquired during the UP intervention (quiz score difference). We did not find support for a relationship, suggesting that the efficacy of the initial level of intervention may neither help nor hinder further participation in a multilevel intervention program. Au contraire, our results suggest that other factors influence this choice. To our knowledge, no studies have examined this factor to date; however, our relatively small and homogeneous sample suggests that this finding should be interpreted with caution.
The second aim of the current study consisted of examining factors that influence the efficacy of the TP intervention. It is important to note that in a previous study, we found positive support for the efficacy of the UP and TP interventions (Marcotte et al., 2023, 2024). The participants in the active TP group, compared to those in a passive-comparison group, showed improvements not only in depressive symptoms but also in cognitive distortions, the use of mindfulness techniques, anxiety management, and personal goals. Furthermore, these positive improvements were maintained at follow-up 3 months after the intervention.
Results of the present study supported mother’s level of education as a significant moderator of changes in depressive symptoms. Having completed secondary or university levels of education, but not CEGEP, was associated with larger decreases in depressive symptoms. Regarding more highly educated mothers, this result is in line with previous studies demonstrating that youth presenting with externalizing problems, who had a more highly educated mother benefited more from participation in a preventive program (Curry et al., 2006; Rieppi et al., 2002). In a previous pilot study on the implementation of Zenstudies, we also found that students in the TP intervention, whose mothers had completed postsecondary education, reported fewer depressive symptoms at post-test than those whose mothers did not (Marcotte et al., 2018). Past studies have suggested that higher levels of education in mothers may be linked to positive intergenerational effects on cognitive abilities, based on other research showing correlations between higher maternal education and higher cognitive abilities in emerging adults (Kong et al., 2015). Thus, postsecondary students whose mothers are more highly educated may be better able to benefit from cognitive-behavioral interventions because of better cognitive resources to process and integrate the content presented in the programs. However, it remains difficult to understand the presence of a relationship for two of the three levels but not for the CEGEP level. It is unclear whether this is a replicable or spurious finding, such that further studies examining the influence of mother’s education level are warranted.
Limitations and Future Directions
It is important to consider some limitations of the present study. Although this study constitutes a first step in the analysis of the multilevel implementation of a prevention program, the number of participants remains relatively small due to the participant selection process, as well as the low TP opt-in rate. Regarding participants, the majority identified as North American and female; this limits the generalizability of the findings to other cultural identities and genders. Although the current sample was recruited across multiple institutions, it was completed entirely in French and in one single Canadian province, again limiting generalizability. Finally, in addition to extending the current findings to larger, more diverse samples, utilizing mixed methods and multilevel statistical models, future studies will need to go beyond sociodemographic variables to determine additional factors that might influence decisions to participate including social support, stigma, and cultural factors.
Conclusion
The current study demonstrates that current symptoms alone are not sufficient to guarantee that those who would benefit from a second level of intervention will opt-in when presented with the option. Thus, identifying factors that can encourage young people to engage in prevention programs that have been proven to ameliorate student mental health is vital, in order to promote the development and well-being of young people.
Footnotes
Acknowledgements
The authors want to thank the students and staff of the Cégep de Gaspésie-Les-Iles, La Pocatière et Institut de technologie agro-alimentaire, Trois-Rivières, Terrebonne, Lévis-Lauzon, and Collège André-Grasset for their collaboration in the present study.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for this research was provided by the Rossy Foundation.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
