Abstract
Over the past decade, there has been an increased emphasis on tailoring men’s health promotion programs. To optimize outcomes, participatory action research that involves and elicits feedback from end-users has been highlighted as important to creating gender-responsive interventions. In this scoping review, we examine (a) how participatory action research has been used to design health promotion interventions for men and (b) what constitutes a gender-responsive intervention design. Following a comprehensive search, 53 articles were included in the review, reporting on 35 men’s health promotion programs. Our findings suggest that participatory action methods harness varying degrees of end-user involvement, with a large majority limited to post-intervention evaluations rather than co-design and consumer collaboration. In addition, there are inconsistencies for applying gender-responsive approaches within programs, particularly regarding how interventions are targeted, tailored, and promoted to men. We conclude that participatory action research methods translate to varying degrees of gender responsiveness in men’s health promotion programs. That said, involving end-users at various stages of intervention design, implementation, and evaluation may increase the likelihood that programs are more attuned to masculinities and better engage participants in promoting healthy behavior change. Efforts to advance gender-responsive designs can benefit from inductively deriving and incorporating men’s masculine values.
Men have historically been underrepresented in the design and delivery of health promotion interventions across numerous social determinants (e.g., health status, cultural background, ethnicity, age) and health outcomes (Guillermo et al., 2022; Howell et al., 2023; Sharp, Spence, et al., 2020). As a result, the past decade has seen a sharp rise in community-based health interventions targeted at men, with an emphasis on marginalized sub-groups (Bottorff et al., 2015; Gross et al., 2023; S. Robertson & Baker, 2017). Herein, gender-sensitized designs for men have emerged as key to program efficacy (Fleming et al., 2014), with the centerpiece typically being traditional masculine norms (e.g., protector/provider, stoicism, self-sufficiency) that are marketed as pliable drivers for health behavior change (Griffith et al., 2020; Jewkes et al., 2015; Milner et al., 2019; Seidler et al., 2016). While these approaches have garnered some men’s engagement and benefited their health outcomes (Timm et al., 2024), many health promotion programs have been predicated on shifting men’s alignments to traditional masculine norms (Smith & Robertson, 2008). Recent calls have been made for the need to inductively derive potential end-user’s lived experiences and needs to develop more relevant and meaningful gender-responsive offerings (Galdas et al., 2023; Östlin et al., 2007).
Numerous gender-related factors (e.g., perceived societal roles) can impact the uptake of health promotion programs (Bell et al., 2023; L. M. Robertson et al., 2008; S. Robertson & Baker, 2017; Seidler et al., 2016) and there is evidence that interventions tailored to men’s interests increase engagement (Caperchione et al., 2015; Garcia et al., 2022; Seaton et al., 2017; Sharp et al., 2018; Valdez et al., 2021). Gender responsiveness, or the extent to which programs consider gender norms and promote gender equity, is an important consideration when designing and evaluating interventions (Dworkin et al., 2015). To assess this, the World Health Organisation Gender Responsive Assessment Scale (GRAS) was created with the aim of lessening gender-based health inequities (World Health Organisation [WHO], 2011). The scale outlines five categories ranging from gender-unequal to gender-responsive (WHO, 2011). While the GRAS was originally designed to address gender inequity factors in the health outcomes of women and girls (WHO, 2011), the scale has been applied to men’s health research garnering attention to the role of masculinities and the need for programs to address unproductive masculine norms (Dworkin et al., 2015; Flood, 2019; S. Robertson et al., 2013; WHO, 2011).
In shifting away from gender-mainstreaming approaches which fail to address contextual diversities between genders, gender-sensitive approaches initially emerged as good practice (Fleming et al., 2014). Several authors have developed design tools (Struik et al., 2019), program principles (Oliffe et al., 2020), and process development frameworks (Galdas et al., 2023) to guide and advance gender-sensitized men’s health promotion programming. Struik et al. (2019) evaluated the Check-Mate tool, which considered five key approaches for planning, implementing, and evaluating men’s health promotion programs. Factors included creating man-friendly spaces, incorporating appealing activities for men, using masculine ideals to increase the wellbeing of men and their families, considering aspects of men’s identities other than gender, and encouraging independence and participation (Struik et al., 2019). The authors cautioned against reinforcing traditional masculine norms, and highlighted the importance of promoting programs as user-led and owned with men as exert co-creators (Struik et al., 2019). Similarly, Oliffe et al. (2020) explored the complexities of men’s health promotion highlighting gendered caveats and contexts. Herein, men’s buy-in was aided by facilitating them to establish their own group-based masculine norms that legitimized collective self-health work (Oliffe et al., 2020). However, there has been growing evidence for the use of gender-transformative approaches that not only acknowledge but actively seek to change gender norms, roles, and relations (Galdas et al., 2023). For example, the 5C framework has been suggested as a way to help standardize the methods by which gender-transformative approaches and masculinities are incorporated and applied across a broad range of settings (Galdas et al., 2023). The framework is comprised of five main development phases (i.e., co-production with stakeholders, program cost, context, content, and communication with participants), informed by gender-transformative approaches (Galdas et al., 2023). Despite the availability of gender-responsive guidelines, the extent to which these practices and principles have been adopted within men’s health promotion programming remains unclear.
Key to gender-transformative approaches is the use of participatory action methods that involve men and relevant stakeholders to guide intervention development and design (Galdas et al., 2023; Vargas et al., 2022). These methods seek to foster collaboration, generate content, and deliver meaningful outcomes by responding to men’s health needs and experiences (Constantin et al., 2022). Moreover, participatory action methods may also be important to understanding and addressing broader social determinants (e.g., SES) that contribute to men’s health inequities (Griffith, 2024; Hankivsky & Hunting, 2022). The use of participatory action methods has been associated with increased health literacy as well as strengthening the overall success of health promotion initiatives (Freire et al., 2022; Greenhalgh et al., 2016; Vargas et al., 2022). While some variability exists in its operational definition, participatory action approaches are user-centered and aim to engage specific groups (e.g., young men) to assist in the development, implementation, evaluation, and dissemination of interventions (Constantin et al., 2022; Freire et al., 2022). Recently, co-design approaches have emerged as core participatory methods, varying in participant involvement from basic consultation, active collaboration, to near-total consumer control (Constantin et al., 2022). Vargas et al. (2022) further differentiates the co-design approach as an active and equal partnership between stakeholders to create solutions to issues previously identified in the intervention planning. Within this context, numerous methods for gathering feedback from participants may be used (e.g., focus groups, interviews, workshops) at various stages in the intervention process (i.e., ideating, creating, refining, implementing, evaluating, sharing; Vargas et al., 2022).
Despite recent guides and principles for designing men’s health promotion programs (e.g., Galdas et al., 2023; Struik et al., 2019), there is little synthesis of programs to distill what constitutes gender-responsive programs, and the role of participatory action methods in tailoring those interventions to men. Accordingly, we conducted a scoping review to examine (a) how participatory action methods are used to design men’s health promotion interventions and (b) what constitutes gender-responsive health promotion programs for men.
Methods
This review utilizes the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines and has been prospectively registered in the Open Science Framework registry (OSF registration
Eligibility Criteria
Health promotion programs broadly included interventions that actively engaged participants in health-related behavior change (e.g., physical activity, healthy eating, social connection) to improve one or more health outcomes (e.g., weight loss, mental wellbeing). Interventions may be delivered in a range of contexts and settings and that targeted sexual and/or oral health were not within the scope of this review. There were no restrictions on study design (e.g., randomized controlled trial [RCT], pre-post, interviews, mixed-method design, focus groups, etc.) provided they met the following criteria: (a) the intervention or program focused on men’s health promotion, (b) the research was conducted to identify a need and/or inform intervention development for men, (c) intervention participants were adult (18+ years) men. Mixed-gender studies were excluded as gender-blind interventions have long been the norm which so often failed to engage men (Oliffe et al., 2020; Sloan et al., 2010). In addition, it is uncommon that mixed-gender studies include and/or describe gender-tailored design elements (Sharp et al., 2022). Articles published in English from 2013 to 2023 were considered to reduce the number of eligible studies and reflect current trends and directions in the literature. No gray literature or reviews were included.
Search Strategy
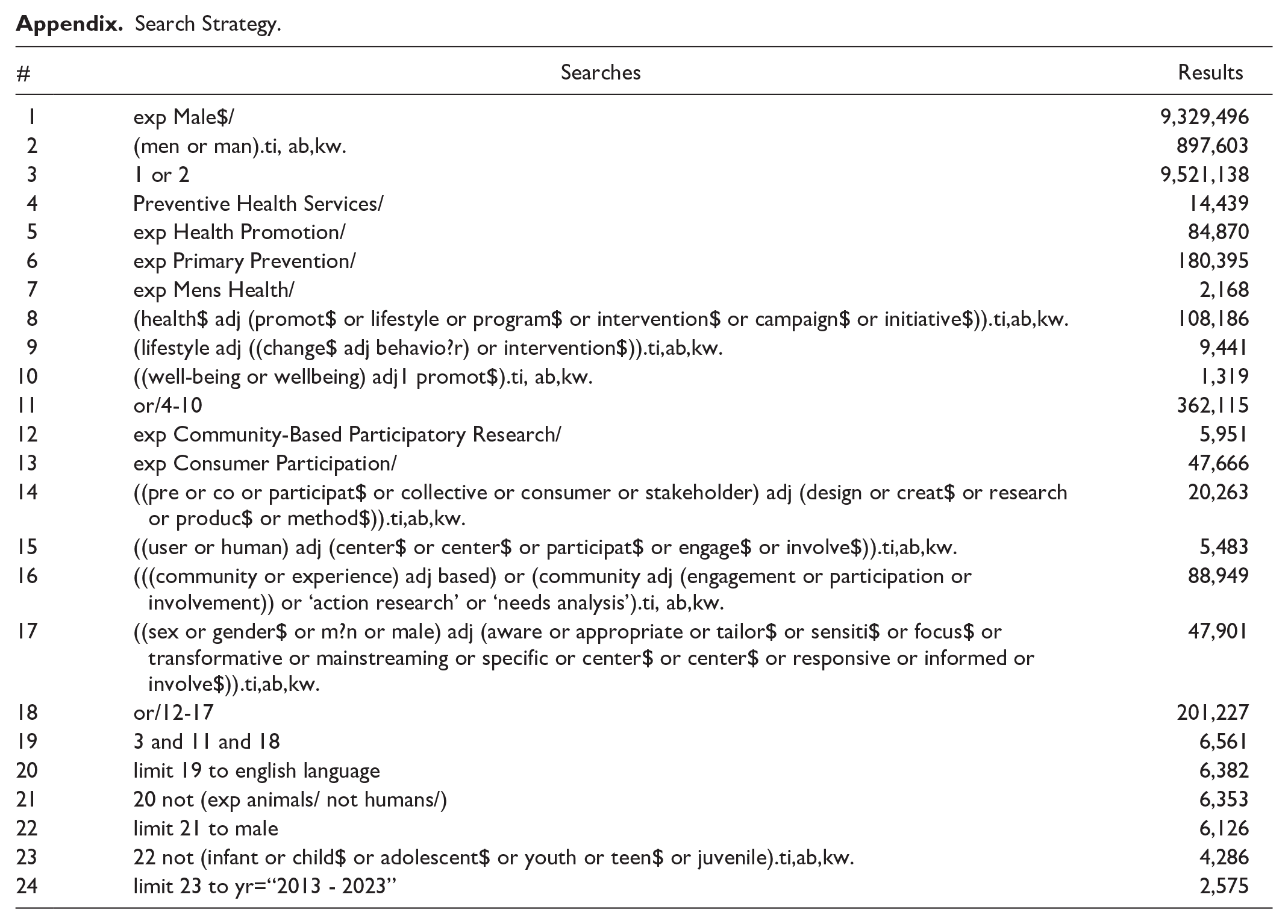
Relevant articles were identified through six electronic databases including Medline, EMBASE, CINAHL, SportDiscus, PsychINFO, and Web of Science. The search strategy (Appendix) was developed using key terms from previously identified literature and Medical Subject Headings (MeSH) terms related to: men, health promotion, men’s health, lifestyle intervention, wellbeing promotion, community-based participatory research, co-design, action research, and gender-responsive design. The strategy was developed for Medline, and the syntax was adapted across databases. References of included articles were also searched to ensure relevant articles were not missed and to reduce reporting bias. The search was conducted in April 2023 and restricted to studies published within the last 10 years. Covidence was utilized for duplicate removal, screening, and data extraction. Screening was conducted independently by two authors (CMC, CS) and any discrepancies or conflicts were resolved by a third author (PS).
Data Extraction and Synthesis
Two authors (PS, CS) independently extracted relevant data from the 53 articles, including publication details, participant information, intervention characteristics and development, level of involvement of end-users, and gender-responsive design. Where there were multiple papers for the same program, the information from each paper was collated. Intervention design and delivery features related to the co-design, recruitment, context, content and delivery, and communication style were extracted from available sources (i.e., publications, supplementary materials, program websites) and used to determine gender responsiveness, adapted from the 5C Framework (Galdas et al., 2023). Gender responsiveness was classified using the WHO Gender Assessment Scale as gender-discriminatory (upholds gender inequality), gender-blind (ignores gender expectations), gender-sensitive (considers gender expectations), gender-responsive (considers gender expectations and addresses specific needs), or gender-transformative (includes strategies to promote gender equality and amend harmful expectations) programs (Department of Gender, Women and Health, 2011). Disagreements were reviewed by a third author (CMC) and discussed during bi-weekly team meetings.
A narrative approach was used to synthesize data from the included articles regarding program characteristics, methodological quality, and WHO Gender Assessment Scale classification. The information was thematically analyzed by two authors (PS, CS), and generated keywords from which emerging codes and overlying themes were identified.
Results
Study Selection
A total of 8,954 articles were retrieved during the initial search. Title and abstract screening was conducted to exclude articles that did not meet the eligibility criteria and remove duplicates. A total of 227 articles were identified for full-text review wherein 174 articles were excluded (e.g., interventions that included female participants). Fifty-three articles were identified for inclusion in the final review to make up a total of 35 programs (see Figure 1).
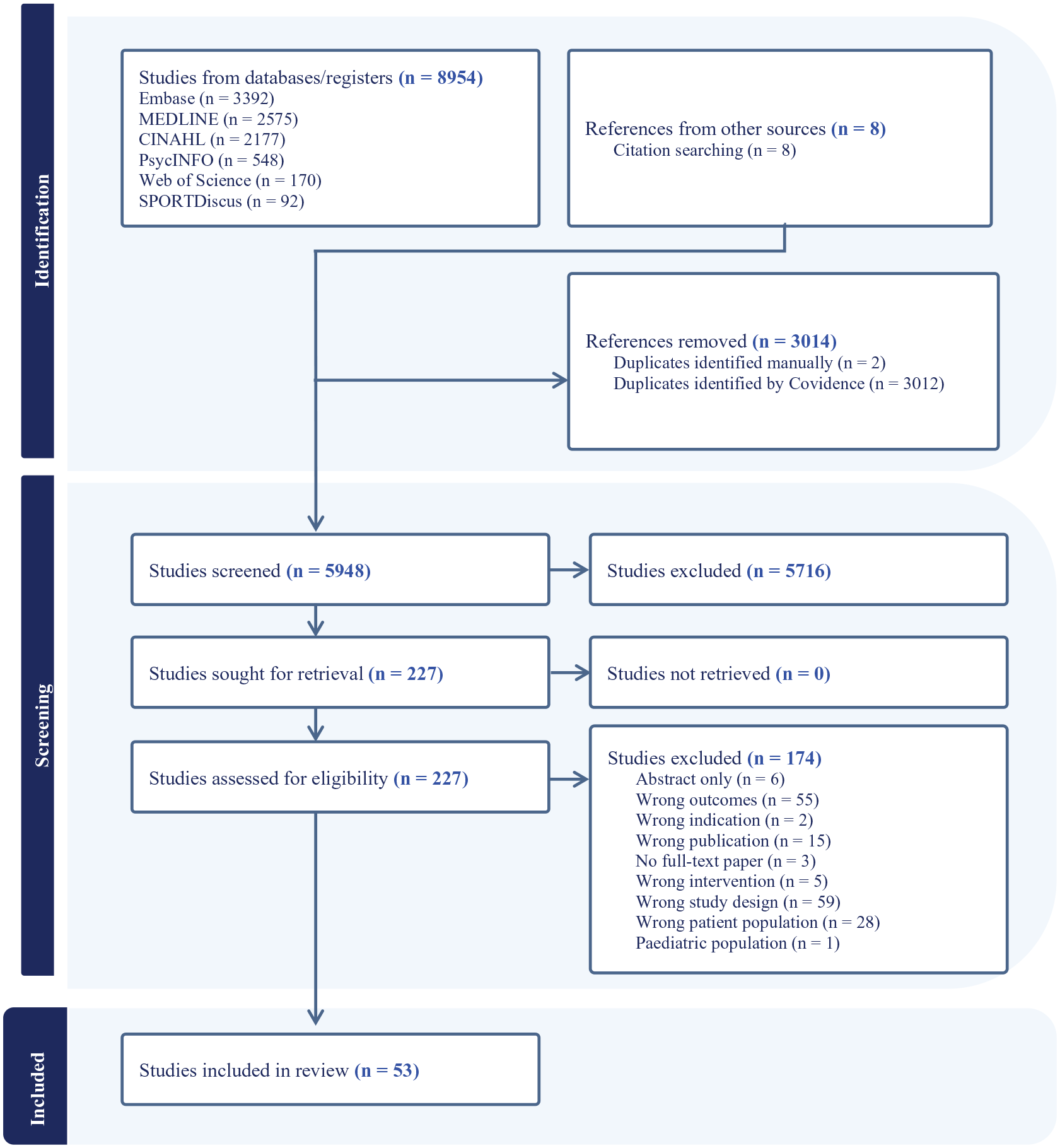
Flow Diagram of Included Articles.
Study Characteristics
All included studies were published from January 2013 to April 2023, and the programs were representative of numerous countries, including the United States (n = 8; 23%), United Kingdom (n = 7; 20%), Australia (n = 6; 17%), Canada (n = 4; 11%), New Zealand (n = 3; 9%), Ireland (n = 3; 9%), Denmark (n = 1; 3%), India (n = 1; 3%), Scotland (n = 1; 3%), and Sweden (n = 1; 3%). Study designs encompassed pilot studies (n = 13; 25%), protocols (n = 9; 17%), qualitative designs (n = 7; 13%), RCTs (n = 6; 11%), quasi-experimental designs (n = 6; 11%), mixed methods (n = 5; 9%), descriptive designs (n = 4; 8%), process evaluations (n = 2; 4%), and secondary analyses (n = 1; 2%).
Intervention and Co-Design Methods
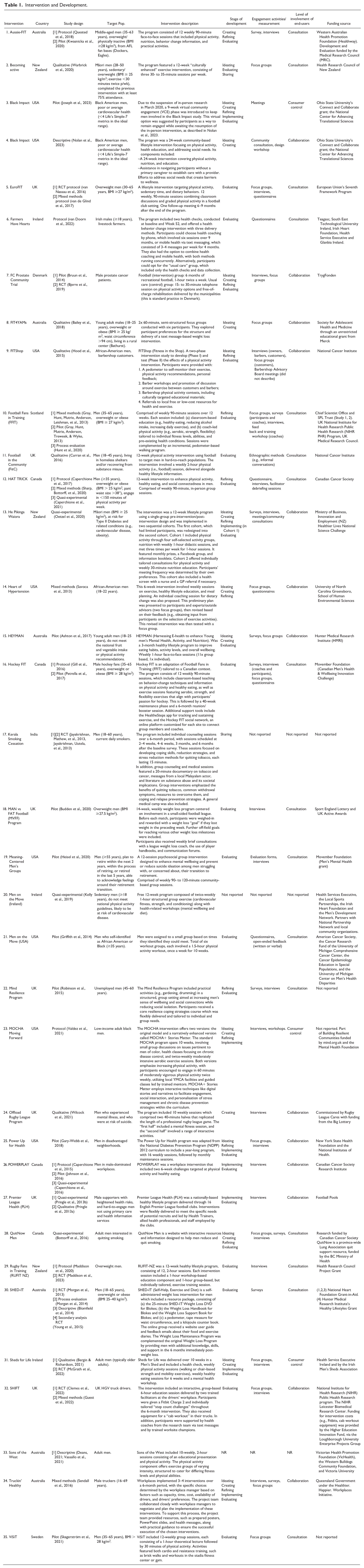
The level of end-user involvement varied with the majority of studies involving men in a consultation (n = 16; 46%) or collaboration (n = 13; 37%) capacity. Only 3 programs (9%) were identified as being consumer led. Within this, the most common stage of development to engage participants was in evaluating (n = 28; 80%) the intervention or resource (e.g., through surveys, interviews). Forty-nine percent (n = 17) involved participants before intervention implementation (i.e., ideating, creating, refining) and only 9% (n = 3) of programs included participants in all five stages of development (i.e., ideating, creating, refining, implementing, evaluating, sharing). Many programs (n = 13; 37%) involved participants at only one stage of development. Programs which were collaborative and consumer-controlled were often iterative in their design, flexibly delivered, and provided bespoke offerings tailored to the unique interest and preferences of participants. Notably, all studies were supported, in-part, by limited-term grant funding provided by government, university, and/or non-profit funding that likely limited the longevity and sustainability of many programs. Herein, some authors discussed the challenges of securing ongoing funding and reliance on volunteers (e.g., Kelly et al., 2019). Football Fans in Training (FFIT) provided one model which has been replicated internationally, whereby partnership with and delivery through professional sports organizations has allowed for sustainable delivery. Study and co-design characteristics are further detailed in Table 1.
Intervention and Development.
Gender Responsiveness
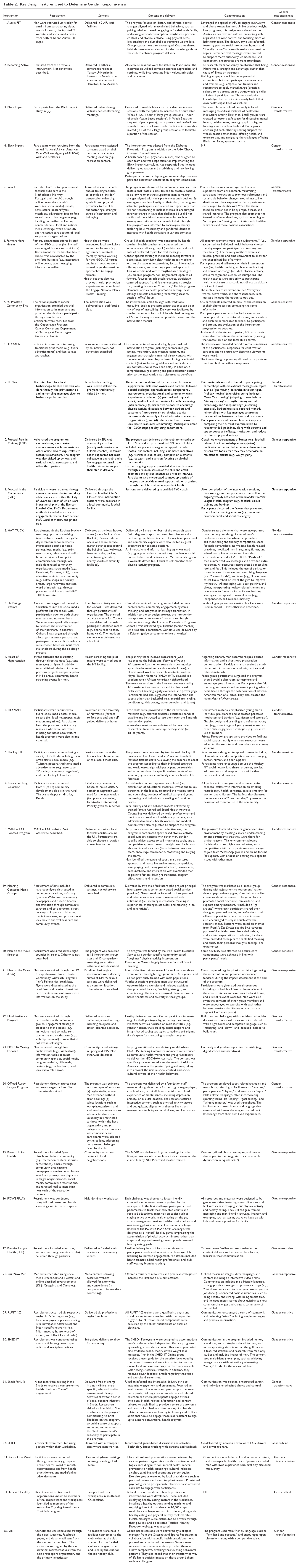
Using GRAS definitions (WHO, 2011), 34% (n = 12) of interventions were determined to be gendered-transformative, 37% (n = 13) gender-responsive, 23% (n = 8) gender-sensitive, and 6% (n = 2) gender-blind. However, there was significant heterogeneity in the use of gender-responsive terminology, as well as the application of gendered elements within and across studies related to intervention recruitment, context, content and delivery, and communication. Among gender-transformative programs, differences arose in how interventions sought to promote gender equity and address unproductive gender norms. Two-thirds of the interventions used sport and/or physical activity as the backdrop to engage men (n = 23; 66%), with 12-week group-based interventions being the most common model for men’s health promotion programs (n = 13; 37%). Gender-transformative approaches predominantly utilized group discussion to unpack socio-cultural influences. Herein, the combination of lifestyle and social change helped to facilitate conversations about gender through the use of metaphors as well as a currency for trading social capital (e.g., FITShop, HAT TRICK, Offload Rugby League Program). While some interventions leveraged men’s interest in these activities (e.g., sport fans) for recruitment and engagement, others used this as a platform for promoting social change. That said, few programs directly targeted health-related gender norms, instead focusing more broadly on gender socialization (e.g., masculine identities, peer relationships). Surprisingly, two interventions were deemed to be gender-blind as gender did not feature as an intervention consideration (despite including men-only samples). Table 2 provides an overview of key design features used to determine gender responsiveness.
Key Design Features Used to Determine Gender Responsiveness.
Discussion
Participatory Methods in Men’s Health Promotion
The current scoping review findings deepen understandings about the ways in which participatory action methods have been employed, and how they can be utilized in men’s health promotion research. This is a critical step forward given the variability in operational definitions challenging researchers to decide what elements might most effectively count as participatory action. For instance, while most studies reported the use of co-design initiatives, this was loosely defined and used interchangeably with co-production, co-creation, co-development, as well as concepts such as “collaboration,” “working in partnership,” and “engaging end-users, stakeholders, and/or consumers.” The inconsistency of terminology and associated diverse approaches have garnered much debate in health research about the level at which end-users can and/or need to be engaged in the intervention development processes (Clarke et al., 2017; Pearce et al., 2020; Slattery et al., 2020).
Beyond the semantics of participatory action methods there is much to be learnt from the patterns and diversity evident in the synthesis of the 35 programs featured in this review. Foremost, it is fair to say that participatory action research has been and is perhaps for evermore altered by the COVID-19 pandemic, wherein virtual participation (and program delivery) predominates (Oliffe et al., 2023). Deviating from traditional group-based, in-person programs, many programs necessarily pivoted to 100% online delivery with the pandemic and all that has followed. Herein, the specificities of those interactions can be understood as shifting in ways that might facilitate or incumber the involvement of stakeholders in the design and delivery of men’s health promotion programs. While new participatory action methods and models for men’s health promotion should be rooted in community-based program principles, with a focus on power and empowerment, the mechanisms and means for virtual involvement demand pragmatic diversity (and perhaps a new paradigm) for doing that process work.
As contributors, men were involved at a consumer control level in very few of the reviewed studies (i.e., researchers were involved only at the request of the end-users who create, undertake, and disseminate the results of the intervention) (Bergin & Richardson, 2021; Joseph et al., 2023; Valdez et al., 2021). Rather, they were more likely to be engaged at the consultation (i.e., seeking stakeholders’ views and using them to influence program development) or collaboration stage (i.e., continuous partnership between stakeholders and researchers) (Boote et al., 2002, 2011). Indeed, campaigns largely engaged men at the evaluation stage post-development, often in the form of feasibility or acceptability measures (e.g., focus groups, interviews, surveys). Further, few studies included men at the sharing stage of the process, and of those that did, none engaged men beyond a consultation role (Jayakrishnan, Uutela, et al., 2013; Warbrick et al., 2020) despite the possibility of greater dissemination engagement and wider public awareness (Brett et al., 2014; Constantin et al., 2022). At any phase, roughly half of the programs did not go further than an initial one-off consultation with little detail provided concerning how the information gathered was used to inform the co-design process. Overall, our findings highlight the lack of strategic and sustained contributions from those that are supposed to benefit from the interventions, a trend which presents missed opportunities to achieve the most relevant and meaningful design and implementation outcomes (Boote et al., 2011; Schulenkorf, 2010, 2012). It has long been recommended that end-users be involved in all stages of intervention development to help increase their capacity and agency within the process and to enhance the effectiveness of the program and associated dissemination (Boote et al., 2011). That said, we recognize that priority groups of end-users often face systematic disadvantages and suggest that considerations for minimizing participant burden and/or providing compensation are key to the feasibility of participatory action research methods. Where possible, we recommend identifying and working closely with key stakeholders (e.g., industry, policymakers) to leverage and sustain the design and delivery of men’s health promotion programs.
Some programs such as Aussie-FIT or Euro FIT were developed based on the literature and existing program design models (i.e., FFIT) (Quested et al., 2018; van Nassau et al., 2016). As such, these programs are likely built on “secondary participation” where diverse perspectives and evidence are considered through indirect and passive means. Secondary participation can be risky; for instance, in the case of FFIT, the program itself only engaged men in a consultation capacity at the refining and evaluation phases of development, leaving participation as an end-point rather than a program design process. Relatedly, there are numerous complexities regarding contextual and cultural factors when adapting programs that men may be able to provide valuable insight to (Copeland et al., 2022). This may be critical in the context of commercial and structural determinants of health, where profit-driven neoliberal sectors shape public health debates as well as emergent health trends (de Lacy-Vawdon et al., 2022). Taken together, increasing the participatory action of men and relevant stakeholders holds promise to effectively design meaningful programs, and increase capacity, ownership and sustainability potential for men’s health promotion programs. The sport-based intervention model has dominated men’s health promotion interventions and its success at engaging men and achieving health outcomes globally is evident (Timm et al., 2024). However, as we look to the next generation of men’s health promotion interventions addressing gender and health inequities, participatory action methods that reside outside traditional masculine arenas (i.e., sports) will be critical to scaling and sustaining innovative interventions.
Finally, the current paradigm of men’s health promotion programs is built on time-limited funding, highlighting a critical limitation in long-term program development and evaluations. All studies reviewed were at least partially supported by limited-term grants from government, university, and non-profit organizations. Programmatic funding and renewals would ease pressures on program leaders and staff and build sustained participatory actions with partners. This context underscores the necessity of stable, long-term funding solutions to ensure long-term success and the impact of men’s health promotion efforts (Oliffe et al., 2024).
Gender Responsiveness in Men’s Health Promotion Programs
Study findings revealed considerable diversity in how interventions were targeted to and tailored for men. Overall, there has been a reliance on traditional masculine norms as the centerpiece by which men’s health behavior changes are explained (and claimed) as antiquated, shifting, and/or sub-altern. In referencing gender-transformative efforts, the hegemony of traditional masculinity has prevailed to the point where we are likely blind to generational and life course changes in men’s masculine ideals. While some programs in the current review were complicit in sustaining traditional masculinity as a lynchpin for marketing and/or the pivot for lobbying change through tailored interventions, there is a need to consider “our” collective knowledge of contemporary masculinities to inductively derive and address gender-responsive approaches. It seems entirely worthwhile knowing the practices and needs of discrete sub-groups of men regarding their health. Young men, for example, have grown up in e-spaces with reports suggesting that they are increasingly isolated, lonely and unable to connect socially (Barreto et al., 2021). To be gender-responsive in this context demands knowledge of the “problem” and feasibility for a “remedy” to address challenges for contemporary masculinities. Said another way, gender responsiveness needs to understand and address young men’s isolation rather than map the problem or solution to shifting or relying on traditional masculine norms. Only one third (n = 12; 34%) of interventions were evaluated as gender-transformative, suggesting that there is still much work to be done in this regard.
While the GRAS provides an important frame, its application to men’s health promotion programs poses several challenges. The shortfall with transformative approaches is that they assume a problem orientation, often with traditional masculine norms as the baseline, and needle to be moved. The predominance of gender-sensitive programs has similarly nestled men’s health behaviors as flowing from traditional masculinities, and the lines between gender-sensitive, gender-specific, gender-transformative and gender responsive suffer the same fate—with traditional masculine norms as the baseline. In the strength-based spaces of masculinities, the healthful twist on traditional masculine norms assumes the interventions need to induce men’s reformulation of risky practices. These programs are reactive for the most part rather than responsive to the sub-group that are espoused as being tailored and responsive to. Herein, the emphasis of transformative interventions on individual responsibility for self-health have been assumed to stem from altering men’s behaviors. Social determinants of health predominantly featured as an inclusion criterion (e.g., target demographics) rather than an intervention outcome in terms of addressing health inequities at a population health level. These findings indicate strong interest in addressing the intersections of gender and culture in segmenting end-user sub-groups. This approach passes as gender-responsive in line with a social determinants of health frame, and promissory notes for focussing on addressing men’s inequities. Within these contexts, the emphasis however remains individual behavior change while the structural determinants of health rendering men to live in marginalizing conditions need attention (Heller et al., 2024). Clearly, men’s agency is, but cannot solely be, the core business of men’s health promotion programs. For the reviewed studies, and men’s health promotion more broadly, it can be difficult to estimate the broader socio-cultural impacts that programs have on masculinities, and the structural determinants of health. Yet, well-designed consumer-led programs within communities might be understood as contributing to, or stemming from, a net positive shift in our collective understanding of the interplays between gender and health.
Several programs targeted men from diverse backgrounds that often incorporate specific cultural or racial contexts which may not be fully captured in traditional gender-responsive definitions. By acknowledging and addressing these intersections, health promotion programs can be inclusive and effective. That said, significant effort has been given to providing rich descriptive data of the experiences and challenges of men from diverse backgrounds. However, few studies are able to bridge this work to effectively address underlying social determinants; Lomas (1998) highlights this disconnect, showing that 90% of the research is focused on providing groundwork that richly describes the “problems.” This gap raises questions about the feasibility of developing tailored programs for every inequity, especially in a post-COVID-19 public health care system that is financially strained (Oliffe et al., 2021). Herein, the amalgamation of programs and services for men living in marginalizing conditions enhances the reach and impact of health programs, making them more sustainable in the long term. This approach is increasingly relevant in the current economic climate, where public health care systems are reeling post-COVID. As evidenced by the studies in the current review, men can and do meaningfully adapt their health promotion programs when programs are collaboratively or consumer controlled (e.g., Bergin & Richardson, 2021; Robinson et al., 2015). Recommendations for practitioners and researchers designing health promotion programs for men are provided in Table 3.
Recommendations for Practitioners and Researchers Designing Health Promotion Programs for Men.

Strengths and Limitations
This is the first review to explore participatory action methods and the operationalization of gender-responsive interventions for men, and thus significantly contributes to a synthesis and opportunities for advancing men’s health promotion research. The importance of this work is underscored by well-documented evidence concerning the challenges with recruiting, engaging, and sustaining men in health promotion and illness-prevention initiatives (Bell et al., 2023; Bottorff et al., 2015; Howell et al., 2023; Sharp, Spence, et al., 2020) and the promising research highlighting the importance of co-design approaches (Galdas et al., 2023; Kinsman et al., 2021). In addition, this review included a rigorous methodology with a comprehensive search strategy, to include the most relevant published studies.
Despite these important strengths, our review has some noteworthy limitations. First, because we restricted our search to published research written in English and excluded gray literature (e.g., government and/or policy statements, stakeholder/end-user reports), we compromised our global understanding of some structural determinants of health. Our search strategy was also limited due to the considerable variability of terms around “co-design” and “participatory approaches,” which may have obscured some applicable research. Given the heterogeneity of interventions, we cannot confidently attribute the use of specific participatory action methods or gender-responsive approaches to improved study outcomes. Future research should aim to scale and sustain gender-responsive programs inclusive of formally evaluating specific outcomes (e.g., engagement/retention, health behaviors/outcomes). Finally, programs specific to sexual or oral health were excluded as it was considered that these concepts were too nuanced to be adequately covered in the search strategy.
Conclusion
This scoping review examined the use of participatory action methods and gender responsiveness in men’s health promotion programs. We surmise that participatory methods do not guarantee gender responsiveness when designing health-promotion programs for men. Yet, participatory methods and gender-responsive approaches can work synergistically to create programs that are informed by the needs and perspectives of men with sensitivities to the ways in which masculinities influence health behaviors and engagement (S. Robertson et al., 2013; Sharp, Spence, et al., 2020). Researchers must expressly consider how to utilize gender-transformative approaches to address contemporary health inequities that do not rely on traditional masculine norms.
Footnotes
Appendix
Search Strategy.
| # | Searches | Results |
|---|---|---|
| 1 | exp Male$/ | 9,329,496 |
| 2 | (men or man).ti, ab,kw. | 897,603 |
| 3 | 1 or 2 | 9,521,138 |
| 4 | Preventive Health Services/ | 14,439 |
| 5 | exp Health Promotion/ | 84,870 |
| 6 | exp Primary Prevention/ | 180,395 |
| 7 | exp Mens Health/ | 2,168 |
| 8 | (health$ adj (promot$ or lifestyle or program$ or intervention$ or campaign$ or initiative$)).ti,ab,kw. | 108,186 |
| 9 | (lifestyle adj ((change$ adj behavio?r) or intervention$)).ti,ab,kw. | 9,441 |
| 10 | ((well-being or wellbeing) adj1 promot$).ti, ab,kw. | 1,319 |
| 11 | or/4-10 | 362,115 |
| 12 | exp Community-Based Participatory Research/ | 5,951 |
| 13 | exp Consumer Participation/ | 47,666 |
| 14 | ((pre or co or participat$ or collective or consumer or stakeholder) adj (design or creat$ or research or produc$ or method$)).ti,ab,kw. | 20,263 |
| 15 | ((user or human) adj (center$ or center$ or participat$ or engage$ or involve$)).ti,ab,kw. | 5,483 |
| 16 | (((community or experience) adj based) or (community adj (engagement or participation or involvement)) or ‘action research’ or ‘needs analysis’).ti, ab,kw. | 88,949 |
| 17 | ((sex or gender$ or m?n or male) adj (aware or appropriate or tailor$ or sensiti$ or focus$ or transformative or mainstreaming or specific or center$ or center$ or responsive or informed or involve$)).ti,ab,kw. | 47,901 |
| 18 | or/12-17 | 201,227 |
| 19 | 3 and 11 and 18 | 6,561 |
| 20 | limit 19 to english language | 6,382 |
| 21 | 20 not (exp animals/ not humans/) | 6,353 |
| 22 | limit 21 to male | 6,126 |
| 23 | 22 not (infant or child$ or adolescent$ or youth or teen$ or juvenile).ti,ab,kw. | 4,286 |
| 24 | limit 23 to yr=“2013 - 2023” | 2,575 |
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Oliffe is supported by a Tier 1 Canada Research Chair in Men’s Health Promotion.
