Abstract
Introduction:
Several studies have shown increased occurrence of migraine in ADHD patients. However, there is less evidence on whether migraine patients also have a higher ADHD frequency. The aim of this paper is determining whether the prevalence of ADHD symptoms or impulsivity is higher in patients with episodic migraine.
Methods:
An observational cohort study has been conducted. Patients with episodic migraine were included. The ADHD Rating scale, the Adult ADHD Self-Report Scale, and the scale of impulsiveness of Plutchik were used.
Results:
The mean value of inattention, hyperactivity and impulsivity scores on the ADHD scale was 5 ± 3.8 in cases and 2.7 ± 2.2 in controls (
Conclusion:
Adults with migraine have a higher prevalence of ADHD symptoms. This should be considered when assessing these patients.
Introduction
Attention-deficit-hyperactivity disorder (ADHD) is a neuropsychiatric syndrome characterized by inappropriate levels of hyperactivity, impulsivity in motor, emotional and social responses, a general lack of inhibition, and pervasive inattention (Matthews et al., 2014). Symptoms usually emerge in childhood, with a current prevalence rate of 5% in 4 to 17-year-olds (Matthews et al., 2014), but ADHD is a lifelong condition often underdiagnosed in adults unless it has been diagnosed early in childhood. Several retrospective studies have shown a prevalence in adults of around 4% (Magnin & Maurs, 2017). In ADHD adults symptoms are still present with attentional predominance, but also observations of hyperactive or impulsive behavior (Ivanchak et al., 2012). Migraine is a common and potentially debilitating chronic neurologic disorder presenting significant and clinically important psychiatric comorbidities. Patients with episodic and chronic migraine usually report impulsive behavior and lack of attention and concentration during attacks and interictal phases (Bergman-Bock, 2018; Muñoz et al., 2016). Moreover, the prevalence of migraine could be higher in ADHD patients. The relation between migraine and ADHD has been extensively studied and research suggests that ADHD patients have a higher migraine frequency (Arruda et al., 2020; Hansen et al., 2018; Kutuk et al., 2018; Salem et al., 2018). Most studies have been carried out in children and adolescents and have studied migraine in ADHD patients. Hansen et al. assessed the prevalence of migraine and ADHD in participants from the Danish Blood Donor Study and found that migraine was strongly associated with ADHD (
Thus, understanding the relation between migraine and ADHD may be relevant in several respects. First, it might emphasize the need to consider ADHD symptoms in the treatment of migraine. Besides, it might advance an in-depth understanding of a possible common mechanism underlying both disorders.
As mentioned before, most studies to date have been conducted in children or adolescents and have been based on ADHD patients who have been assessed for migraine headache. Therefore, our work provides a different approach since it has been conducted in adults suffering migraine, whose ADHD symptoms may be unnoticed, and it analyses the prevalence of traits compatible with ADHD.
The main objective of this paper is determining whether the prevalence of ADHD symptoms or impulsivity is higher in patients with episodic migraine.
Methods
An observational cohort study has been conducted. The sample size was calculated using an estimation formula of the difference of two proportions to compare the frequency of occurrence of ADHD-related symptoms in migraine patients compared to healthy controls. Thus, for a level of confidence (95%), with a statistical power of 80%, estimating an a prioristic proportion of 5% of ADHD in the control group and 15% in migraine patients, a minimum required sample size of 100 cases was estimated, with a ratio of 1.5 controls per one case.
The subjects were selected from all consecutive patients treated in a headache clinic. The researcher explained to each participating subject the study, purpose, procedure, estimated duration, potential risks and benefits of participating in the study, as well as any inconvenience it could imply. Each participant was told participation was voluntary and that they could reject or abandon the study at any time, without affecting their subsequent medical treatment or their relationship with the treating physician. All subjects were given sufficient time to read and understand the patient information sheet before signing the consent form and received a copy of the document signed. The diagnosis of migraine was made by a neurologist specializing in headaches following the International Headache Society criteria. All patients that met criteria for episodic migraine and were older than 18 years old and had at least one attack/month, were included if the informed consent form was signed. Patients were excluded if they met criteria for chronic migraine or were taking preventive treatment for migraine or drugs that could influence attention and concentration.
To assess attention deficit, hyperactivity, and impulsivity, both the ADHD Rating scale (ADHD-RS) and the Adult ADHD Self-Report Scale (ASRS) were used. A final clinical diagnosis was not made, yet the frequency of symptoms suggestive of ADHD in both groups was analyzed. The ASRS is the World Health Organization’s (WHO) rating scale for adult ADHD to measure current ADHD symptoms. It consists of 18 items based on DSM IV symptoms/criteria for ADHD, which are measured on a 5-point scale (0 Never/Seldom and 4 Very often), yielding a possible score range from 0 to 72. Items 1 to 9 (Part-A) cover the symptoms of inattention; items 10 to 18 (Part-B) the symptoms of hyperactivity and impulsivity. This scale is useful for ADHD adult screening and diagnosis and should be used in conjunction with a clinical interview to provide additional information. ASRS has a high internal consistency (Cronbach’s alpha of .92). If the respondent scores often or very often in four or more items in Part-A, the individual symptom profile is considered highly consistent with ADHD diagnosis in adults.
However, the ADHD-RS is an 18-item scale reflecting the DSM-V criteria for ADHD. It consists of an inattention subscale with nine items and a hyperactivity/impulsivity subscale with other nine items. The beginning of sentences with “often” is omitted, and respondents are asked about the occurrence frequency of these symptoms in the last 6 months. Each item is scored from 0 to 3 points depending on the frequency (never, sometimes, frequently, constantly), and higher scores indicate the problem behavior. The final score of the ADHD-RS consists of the sum of the direct scores, independent of the rater. It was initially designed to be administered to child patients, but it has been adapted for adult subjects. The ADHD-RS has a high internal consistency (Cronbach’s alpha value of .8) and has been validated in Spanish, showing that it is a valid scale to differentiate ADHD adults from non-ADHD subjects (Richarte et al., 2017). For this work, if ≥6 items were met as frequent or constant on the inattention subscale, a diagnosis of ADHD inattentive subscale was considered; if ≥6 items were met as frequent or constant on the hyperactivity/impulsivity subscale a diagnosis of ADHD hyperactive subscale was considered; and if ≥6 items were met as frequent or constant on both subscales, a diagnosis of ADHD mixed subscale was considered.
Impulsiveness was measured using the scale of impulsiveness of Plutchik (PIS). It consists of a questionnaire of 15 Likert items with four possible answers (never, sometimes, often, almost always), scored respectively 0 to 3, with the exception of questions 4, 6, 11, and 15 that are scored in contrast. The final value is obtained by adding the score for each item, so it will be between 0 and 45. In the Spanish version, the authors propose a cut-off point of 20, with a sensitivity of 60% and a specificity of 74%. The internal consistency of the scale according to Cronbach’s alpha reliability coefficient was .9.
In all cases, demographic- and migraine-related variables were collected. The categorical variables were summarized in frequencies and percentages, while the numerical ones in averages and standard deviations (SD) or in medians and interquartile ranges (IQR), depending on whether the normality assumptions were given. The percentages were compared with the chi-square test; means, to the
Results
Two hundred fifty patients were included: 100 cases (90% female) and 150 controls (85% female). Median age was 40.29 ±9.87 years among cases and 40.14 ±12.17 years among controls. The social and demographic characteristics of cases and controls are listed in Table 1.
Baseline Characteristics of Cases and Controls.
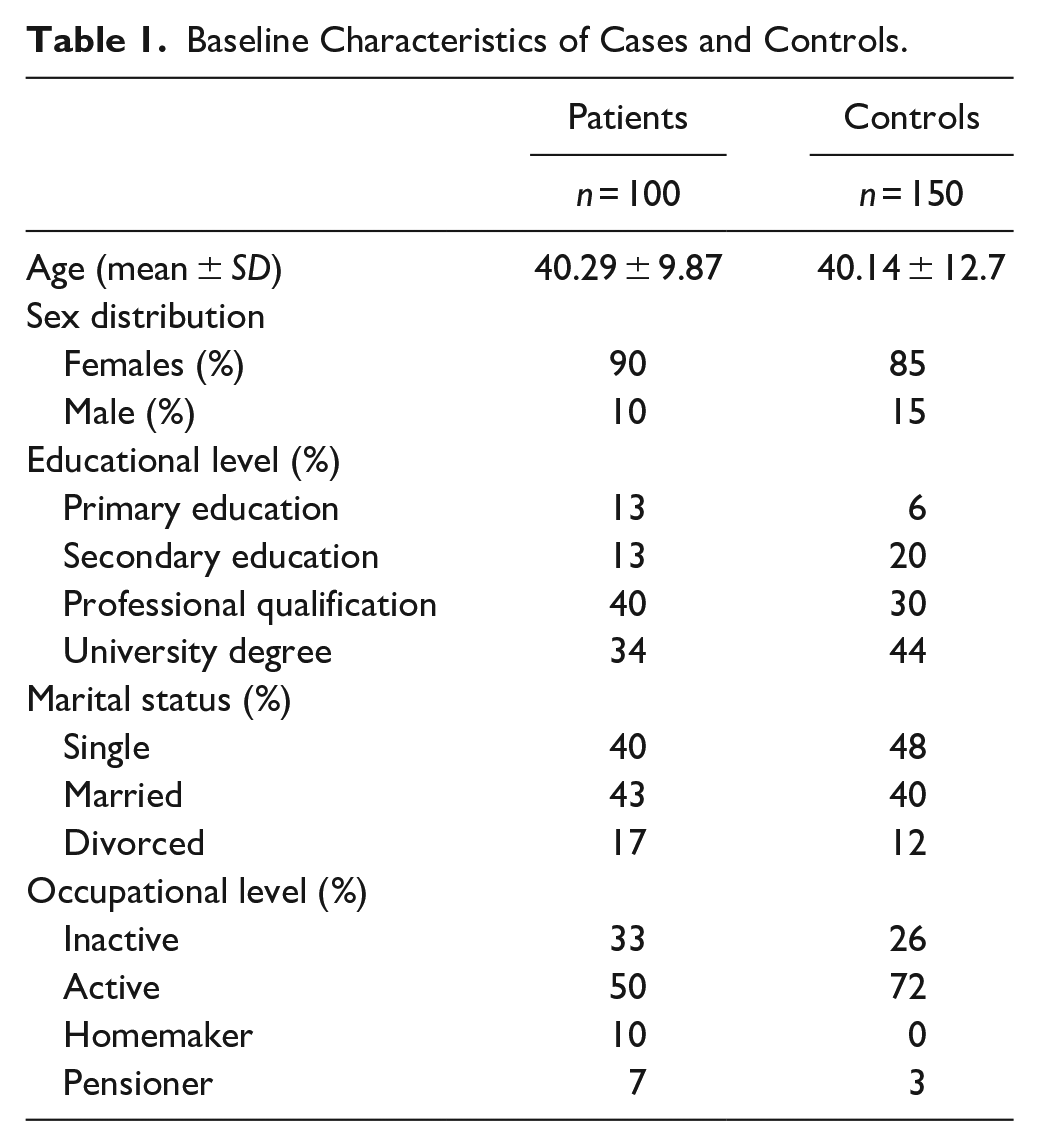
Seventy cases suffered from migraine without aura, while 30 presented a migraine with aura. Ten cases (10%) had less than one attack per month, 64 (64%) had between two and four attacks per month, and 26 (26%) had more than four attacks per month.
The mean value of inattention, hyperactivity and impulsivity scores on the ADHD scale was 5 ± 3.8 in cases and 2.7 ± 2.2 in controls (
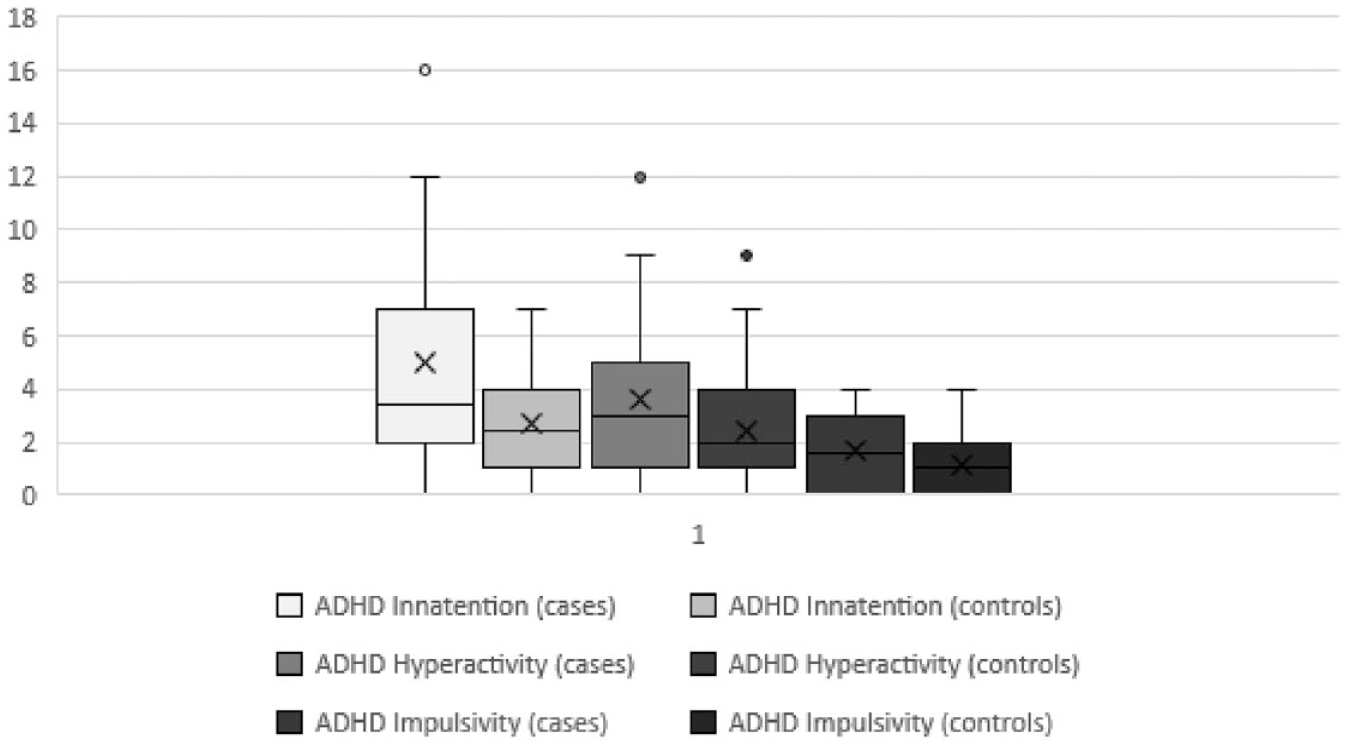
Scores on the ADHD-RS-IV scale in cases and controls.
The mean ARSR scale score was 15 ± 10.8 in cases and 12.3 ± 7.5 in controls (
No differences were obtained between migraine patients without aura and with aura in ADHD scores for inattention (5.3 ± 3.9 vs. 4.4 ± 3.7, respectively,
The median on the PIS scale was 15 ± 6.5 in the cases and 12 ± 5 in the controls (
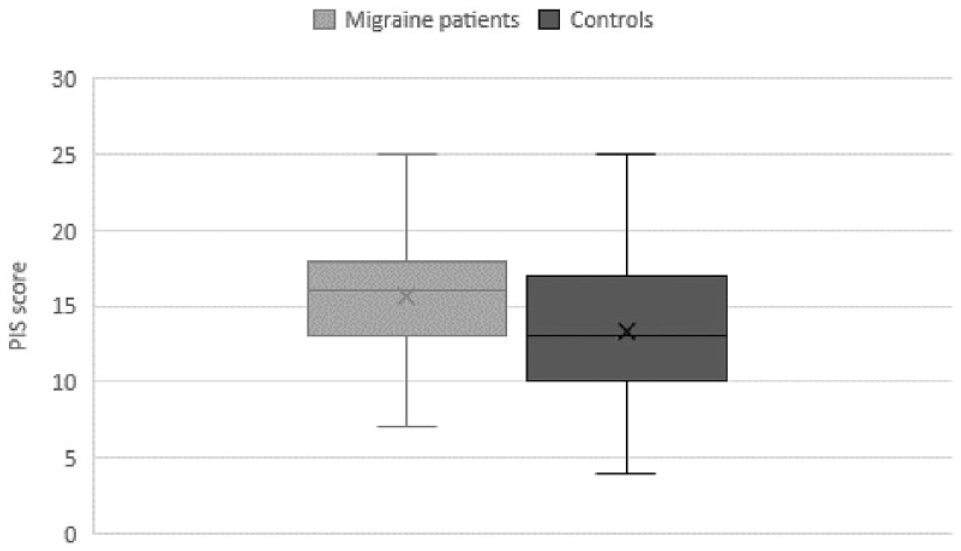
PIS score in cases and controls.
Discussion
In our study, we found higher scores on the inattention, hyperactivity, and impulsivity items of the ADHD scale, as well as a higher total score on the ASRS scale in migraine patients than in healthy controls. Despite we have not been able to demonstrate a statistically significant relationship between migraine and ADHD in adults, there seems to be a tendency toward some association as the analysis of the ASRS results suggest. The frequency of patients who scored four or more items as often or very often in Part-A of the test was five times higher in patients with migraine than in controls, although not statistically significant (
A previous study by Fasmer et al. (2011) already referred an association between ADHD and migraine. The authors used a methodology different from ours since patients with ADHD diagnosis (
In our work there was no difference in ADHD and ASRS scores between patients without and with aura, not a correlation with the number of days with headache. Although these results may be influenced by the smaller sample size than in other published studies, it is possible that the association between ADHD symptoms and migraine is due to pathophysiological links between the two conditions, and not to the subtype of migraine or the number of days with pain.
Studies on impulsivity in migraine patients are limited. A study by Muñoz et al. (2016) involving 155 patients with chronic migraine or headache with analgesia abuse found no associations between Plutchik scale scores or the presence of impulsivity with either CM or MO. Tanik et al. (2020) enrolled 55 patients aged between 18 and 55, all diagnosed with episodic migraine, and 40 healthy controls in a prospective cross-sectional study and found no significant difference in terms of impulsivity (
Migraine has been associated with different psychiatric comorbidities, such as anxiety and depression. The pathophysiology of migraine is complex and not fully understood, although different structures and neurotransmitters involved in the genesis of migraine, such as serotonin and glutamate, have been described (Dodick, 2018). In migraine, a phase of neuronal hyperexcitability has been identified, as well as the hypersensitivity of patients to different stimuli. Additionally, a genetic susceptibility to migraine has been observed (Dodick, 2018). The etiology and pathophysiology of ADHD are incompletely understood. There is evidence of a genetic basis for ADHD, but it is likely to involve many genes with small individual effects. Differences in the dimensions of the frontal lobes, caudate nucleus, and cerebellar vermis have been demonstrated (Tripp & Wickens, 2009). Dysfunction in dopaminergic pathways may contribute to the clinical manifestations of ADHD (Sharma & Couture, 2014). There is evidence that low levels of serotonin neurotransmission are associated with increased impulsivity (Keele, 2005). Impulsive patients also show dysfunction in the pathways that mediate the generation and regulation of emotions (corticolimbic and corticostriatal) (Hazlett et al., 2005). Therefore, these disorders may share pathophysiological mechanisms that explain their association.
The limitations of our work include the cohort design, which does not allow for follow-up, as well as the diagnosis of ADHD based on self-administered questionnaires. Also, the sample size did not allow us to obtain deterministic results that could have been improved with a larger sample. However, we consider the inclusion of a group of cases with a well-defined diagnosis of migraine to be a strength, as well as the inclusion of a control group.
Therefore, in this work, we have shown that there is a tendency in migraine patients to a higher prevalence of ADHD symptoms, as well as a tendency to a higher impulsive personality trait. Although these results cannot be considered definitive, they can help delimit the psychiatric and personality comorbidities of patients with migraine.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
