Abstract
Introduction:
The growing global aging population intensifies the burden on informal caregivers, particularly for individuals with chronic conditions. Family health nursing offers a model emphasizing relational care and psychosocial support, yet evidence on its impact on family resilience and coping remains fragmented.
Objective:
To map scientific literature on family-centered nursing interventions and their association with the promotion of resilience and family coping, acting on resilience and coping, which in turn function as mediators of care empowerment in informal caregivers and families.
Methods:
Following PRISMA 2020 guidelines, this systematic literature review included studies published between March 2015 and March 2025 in English, Portuguese, French, and German. Databases consulted: CINAHL, MEDLINE, Scopus, Web of Science, and Psychology and Behavioral Sciences Collection. Methodological quality was assessed using Joanna Briggs Institute (JBI) tools, and data synthesis employed a metanarrative approach.
Results:
Seven studies were included: 1 systematic review, 2 scoping reviews, 2 qualitative studies, 1 quantitative study, and 1 opinion article. Interventions like psychoeducation, mindfulness, and cognitive-behavioral therapy (CBT) promoted emotional regulation, reduced caregiver burden, and strengthened relational resilience, positively impacting the care recipient's quality of life. The metanarrative identified four themes: (1) Meaning-making through adversity (Benefit Finding and Posttraumatic Growth); (2) Relational and contextual mediation of resilience; (3) Transformative potential of psychosocial nursing interventions; and (4) The relationship between informal caregiver resilience and care recipient quality of life.
Conclusions:
Family-centered nursing interventions significantly enhance the psychosocial well-being and adaptive capacities of caregivers and families. Future longitudinal, methodologically robust, and culturally sensitive studies are needed to generalize these findings.
Implications for Clinical Practice:
This review highlights the importance of structured, family-sensitive interventions in family health nursing, promoting caregiver and family engagement, health system sustainability, and improved quality of life in long-term care.
Introduction
As the global population ages and chronic diseases become more prevalent, families are increasingly involved in the ongoing care of dependent individuals, 1 posing significant risks to caregiver and family health, especially without structured support, directly impacting the care recipient. The increase in chronic diseases and population aging has intensified dependence on informal caregivers and the importance of family contexts, often exposed to high levels of stress and overload, especially in the absence of institutional support.1 -3
Family health nursing offers an integrated approach, viewing the family context as inseparable from care.4,5 Although previous studies have demonstrated that family health nursing interventions can improve therapeutic adherence, reduce caregiver burden, and promote family cohesion, which are important precursors for resilience and coping,6 -8 literature still reveals a gap in understanding the relationship between nursing practices and enhancing resilience and coping strategies, essential for overcoming adversity and maintaining family stability. 9
Background
Family health nursing has proven effective in including informal caregivers in therapeutic care, promoting family cohesion, with evidence of better health outcomes.4,5,10
Structured psychosocial interventions, such as psychoeducation, mindfulness, and cognitive therapies, contribute to emotional regulation and reduction of informal caregiver burden, especially in complex contexts.11 -15 Coping and resilience emerge as central dimensions for the sustainability of care,16 –19 with programs focused on strengthening resilience reducing burnout and the costs associated with providing care.20 -22 The literature indicates that the promotion of family resilience should not be understood as a spontaneous process, but as a result of contextually sensitive, culturally adjusted clinical interventions guided by scientific evidence.21,22
Multiple factors influence family resilience and coping, including individual attributes (such as self-efficacy and emotional regulation), family-level dynamics (communication patterns, cohesion, and adaptability), and contextual conditions (institutional support, access to healthcare services, and health policies).23 -25
Family resilience refers to adapting positively to adversity.12,16 Resilient families achieve better health outcomes for both caregivers and those supported. 26 Family coping involves cognitive and behavioral strategies to manage care-related stress. Research indicates caregivers with stronger coping skills experience lower stress, depression, and burnout.27,28
Many undergraduate nursing curricula still fail to adequately enhance psychosocial skills.29 -31 Literature highlights developing comprehensive programs with structured educational interventions for emotional support and fostering resilience, adaptable to diverse cultural contexts. Combined strategies positively impact caregiver burden and mental health.32 -34
Longitudinal studies show family resilience interventions reduce hospital service use, promote well-being, and contribute to health system sustainability. 20 Interventions promoting active coping prevent caregiver illness and improve family relationships.35,36
Expanding research and implementing nursing programs focused on strengthening family resilience and coping is an ethical and scientific imperative, advancing nursing by promoting not only technical care but also emotional and social sustainability for caregiver families. Investing in this perspective is essential for effective health policies, caregiver well-being, and care recipient quality of life.
The objective of this literature review is to map the scientific literature on family-centered nursing interventions and their association with the promotion of resilience and family coping acting on resilience and coping, which in turn function as mediators of care empowerment in informal caregivers and families.
Methods
This systematic review followed PRISMA 2020 guidelines 37 for rigorous evidence identification, selection, and synthesis. A metanarrative approach 38 was adopted to integrate diverse epistemological and methodological perspectives on complex phenomena like resilience and coping in family health nursing.
Eligibility Criteria
Studies published between March 2015, and March 2025 were included, focusing on family-centered nursing interventions directly or indirectly impacting resilience and coping in informal caregivers, families, and care recipients. The choice of a 10-year time frame, instead of the commonly recommended 5 years, was justified by the scarcity and heterogeneity of studies directly linking family health nursing, resilience, and coping. Restricting to 5 years would have resulted in an insufficient evidence base for meaningful synthesis.
Inclusion Criteria
Articles in English, Portuguese, French, and German were included if they demonstrated nursing interventions improving physical, emotional, functional, and relational health for the care recipient, informal caregiver, and/or family. Eligible study types were systematic reviews, scoping reviews, randomized controlled trials, expert opinion studies, and umbrella reviews.
Exclusion Criteria
Grey literature, clinical trial protocols, and systematic literature review protocols were excluded. Purely descriptive studies without interventions, validation studies of assessment tools, and conference abstracts were excluded to ensure methodological rigor.
Research Strategy
“Mesh” terms or similar, including “family nursing centered care,” “resilience,” “coping,” “caregivers,” and “elderly,” combined with Boolean operators, guided the research question: “What is the impact of family-centered nursing interventions, in the dimensions of resilience and coping, for the person being cared for, caregiver, and family?”
Information Sources
Databases consulted were CINAHL Plus with Full Text, MEDLINE with Full Text, Scopus, Web of Science, and Psychology and Behavioral Sciences Collection. PubMed was accessed via MEDLINE.
Selection Process
Four independent researchers systematically searched, evaluated, and synthesized evidence from February to March 2025, following Stratton guidelines 39 and PRISMA recommendations. 37
Data Items
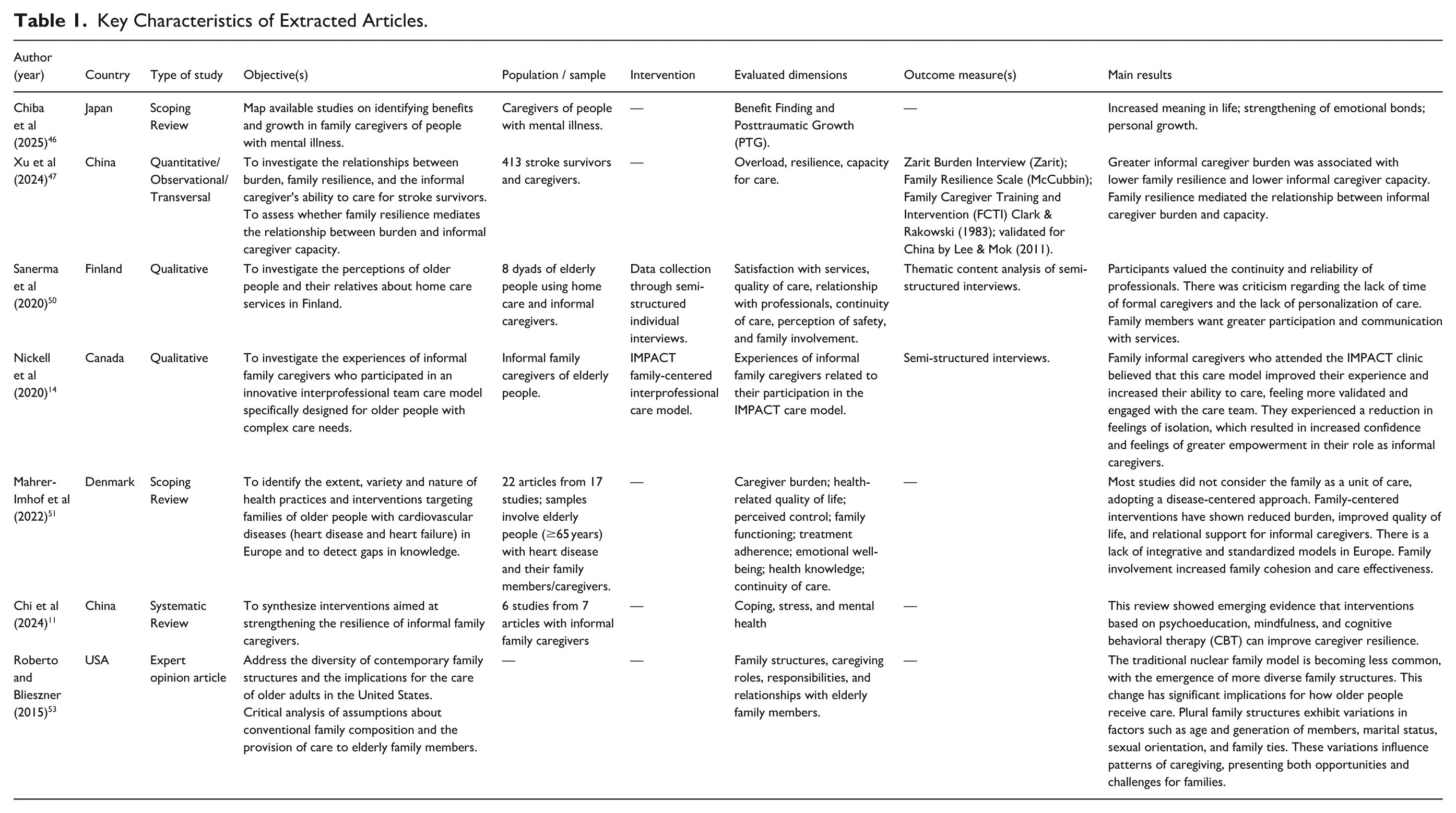
During data extraction, a descriptive evaluation using an instrument (Table 1) captured Author, Year, Country, Objective(s), Study Type, Population/Sample, Intervention, Dimensions Evaluated, Outcome Measure(s), and Main Results.
Key Characteristics of Extracted Articles.
Following analysis, researchers agreed on 4 themes: “Construction of meaning through adversity: Benefit Finding and Post-Traumatic Growth (PTG)”; “Relational and contextual mediation of resilience: Family dynamics and interactions with health professionals”; “Transformative potential of psychosocial nursing interventions: From technical practice to relational practice”; and “Relationship between informal caregiver resilience and quality of life of the person being cared for: mediating role of coping and psychosocial interventions.”
Four independent reviewers verified inclusion/exclusion criteria compliance and data quality. All studies from March 2015 to March 2025 meeting linguistic and health improvement criteria were included. No studies were excluded based on sociocultural factors or geographic region. Studies on diagnostic assessment, care planning, and/or specific intervention strategies for the care recipient, caregiver(s), and family were included. Quality assessment involved duplicate exclusion, blind evaluation by four independent reviewers, full-text review, and PRISMA flowchart presentation. Each study was assessed by two independent reviewers, with disagreements resolved in consensus meetings. Risk of bias was appraised using JBI tools.
Quality Assessment
To assess study quality, Joanna Briggs Institute (JBI) criteria were applied based on study type.40 -44 The review included 1 systematic review, 2 scoping reviews, 2 qualitative, 1 quantitative study, and 1 expert opinion article. Recognizing no standard quality assessment for scoping reviews, the team relied on authors’ assessments or conducted their own, following Levac et al guidelines. 45
All included articles were thought of good (2/3) or moderate (1/3) quality. No articles were removed after researcher consensus, even those with lower JBI scores, indicating their continued contribution.
Data Extraction, Analysis, and Synthesis
Table 1 summarizes key characteristics of extracted articles: Author, Year, Country, Objective(s), Study Type, Population/Sample, Intervention, Dimensions Assessed, Outcome Measure(s), and Main Results.
The metanarrative approach 38 was used to address complex, interdisciplinary research, integrating diverse theoretical and methodological traditions. This was particularly useful given the heterogeneity of resilience, coping, and nursing interventions in family contexts. The approach involved identifying narratives in individual studies, aggregating them into broader themes, and critically interpreting these themes within existing literature. This choice was justified by study heterogeneity and the need for deeper understanding of family care experiences and meanings.
Results
This systematic literature review identified 7 articles, demonstrating high geographical and cultural heterogeneity (Denmark, China, Japan, Canada, Finland, USA), which enriches its findings.
The included articles were analyzed using Greenhalgh et al (2005) metanarrative approach and synthesized into four major interpretive axes: (1) Meaning-making through adversity: Benefit Finding and Post-Traumatic Growth; (2) Relational and contextual mediation of resilience: Family dynamics and interactions with health professionals; (3) Transformative potential of psychosocial nursing interventions: From technical to relational practice; and (4) Relationship between informal caregiver resilience and quality of life of the care recipient: mediating role of coping and psychosocial interventions. Figure 1 illustrates the systematic review flow. 37 The research team thoroughly discussed these themes, interpreting current knowledge and evidence on nursing interventions and health gains for patients, caregivers, and families, also suggesting future research.
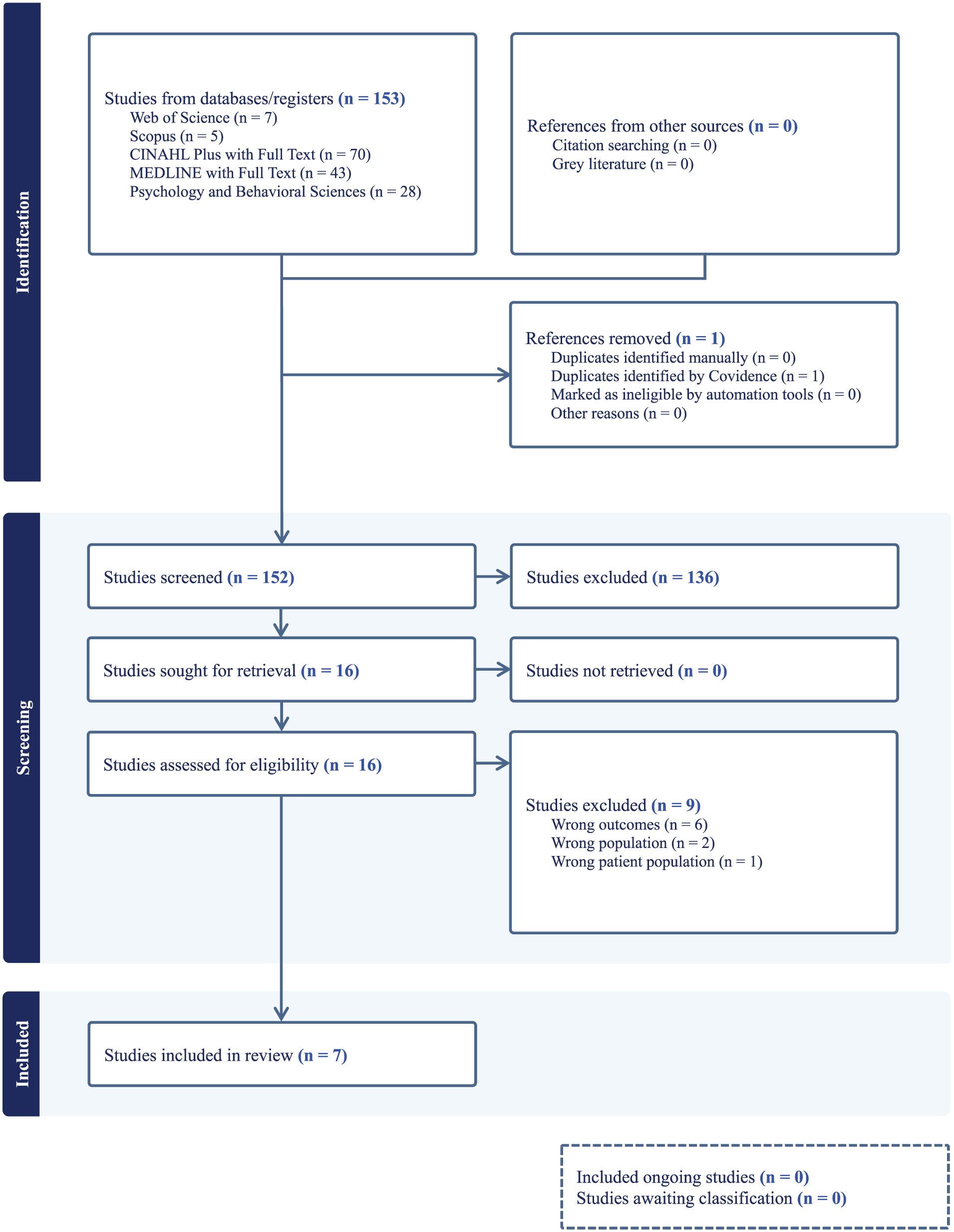
PRISMA flowchart.
Making Sense of Adversity: Benefit Finding and Post-Traumatic Growth
Studies by Chiba et al (2025) and Xu et al (2024) offer an innovative perspective, viewing informal care as a potentially transformative experience beyond stress.46,47 In prolonged adversity, caregivers can develop Benefit Finding and Post-Traumatic Growth (PTG), leading to increased life appreciation, personal growth, expanded spirituality, and strengthened family bonds. They use Benefit Finding and Growth (BFG) to show how reflective coping generates subjective gains, including stronger caregiver identity.
These findings align with Janoff-Bulman’s (1992) cognitive reconstruction model, where traumatic events can reorganize mental schemes, promoting positive meaning from suffering. 48 Re-establishing adversity becomes a fundamental adaptation vector, linked to individual and family resilience. Xu et al (2024) further reinforce that caregivers understanding their role report less emotional exhaustion, greater self-efficacy, and better quality of life, even with high care complexity. This is mediated by social support, family cohesion, and subjective reconstruction capacity. 47 Gaugler et al (2013, 2020) support this, noting resilient caregivers combine psychosocial skills and contextual resources to face stressors with less emotional exhaustion, transforming care into a path of personal growth despite suffering.12,49
Relational and Contextual Mediation of Resilience: Family Dynamics and Interactions with Health Professionals
This dimension explores how social relationships, particularly among caregivers, family, and health professionals, mediate and strengthen resilience. Patient-focused home care and trusting interactions between families and health teams positively impact perceived care effectiveness and caregiver well-being. 50
This aligns with Mahrer-Imhof et al (2022) analysis of European care practices in cardiovascular diseases, showing policies promoting active family participation as co-agents reduce caregiver burden. 51 Their approach aligns with Baumeister and Leary (1995) social motivation theory, emphasizing the human need for belonging in adverse contexts. 52
Literature points to continuous institutional support, service accessibility, and therapeutic coherence as crucial for building trust and maintaining hope among caregivers. Xu et al (2024) identify relational support as a direct protective factor against burnout, highlighting social and professional networks as mediators of suffering and adaptive strengthening. 47
Roberto and Blieszner (2015) analysis deepens understanding of family resilience as a relational, multisystemic phenomenon, highlighting diverse family structures' impact on elder care. Non-traditional families (friends, alternative intergenerational networks, reconstituted unions) play significant informal support roles, challenging normative models. These expanded structures are crucial for caregiver emotional and practical sustainability, especially amid institutional fragility. 53
Family resilience, here, is a dynamic, multisystemic, relational process, influenced by structural and intersubjective factors. 16 It critically mitigates caregiver burden. Family resilience is positively associated with PTG and negatively with caregiver burden for stroke survivors. 15 PTG partially mediated this, suggesting interventions promoting family resilience can reduce caregiver burden. Actively including families in therapeutic plans improves disease management and protects caregiver mental health, leading to more sustainable long-term care.10,54
Transformative Potential of Psychosocial Nursing Interventions: From Technical to Relational Practice
This axis focuses on psychosocial interventions by nurses and interdisciplinary teams, demonstrating transformative potential in care. Chi et al (2024) synthesize robust evidence on psychoeducation programs, mindfulness-based interventions, and cognitive-behavioral therapies (CBT) effectiveness in promoting caregiver resilience and reducing stress. 11
Psychoeducation, offering structured information on disease, coping, and emotional support networks, reduces burden and promotes control. 11 Mindfulness, reduces psychological suffering and promotes emotional well-being via experiential acceptance. CBT promotes adaptive changes, helping caregivers restructure dysfunctional thoughts, developing effective coping skills.13,55
Interprofessional, person- and family-centered care models recognizes caregivers as therapeutic partners, leading to greater self-efficacy, better role adaptation, and significant stress reduction. 14 This broadens care beyond instrumental activity to a relational, emotional practice requiring empathy and communication.
Intervention effectiveness improves with cultural sensitivity, sustained longitudinal application, and integration into daily family health nursing. Chi et al (2024) still warn of the need for greater methodological standardization, essential component definition, and rigorous effectiveness evaluation across sociocultural contexts. 11 Consolidating evidence-based psychosocial nursing practices strengthening caregiver resilience is a significant advance in humanizing care and promoting mental health in chronic vulnerability. Caregivers who attribute positive meaning to care have higher satisfaction, lower depressive symptoms, and less perceived stress.26,35 This indicates that interventions promoting reflection, emotional sharing, and narrative construction of suffering are fundamental for constructive coping and lasting resilience.
Relationship Between Informal Caregiver Resilience and Quality of Life of the Person Being Cared For: Mediating Role of Coping and Psychosocial Interventions
The quality of life for individuals cared for at home significantly depends on the caregiver's emotional, cognitive, and relational skills. Recent studies show that higher caregiver resilience and adaptive coping strategies directly correlate with better outcomes for care recipients, including greater therapeutic adherence, emotional stability, and physical/psychological well-being.
Caregiver resilience is the ability to face adversity, adapt to care demands, and maintain positive psychosocial functioning. 17 Resilient caregivers exhibit lower burnout and depression, positively impacting interaction quality with the care recipient. 26
Moreover, caregiver experiences of Benefit Finding and Post-Traumatic Growth (PTG) link to a more positive perception of their role, directly influencing their motivation and emotional availability toward the care recipient. 46 Such caregivers adopt empathetic, proactive behaviors, creating a stable, emotionally nourishing relational environment that benefits the care recipient’s well-being.
Literature indicates adaptive coping strategies—problem-solving, positive reappraisal, acceptance—significantly reduce caregiver stress, correlating with decreased involuntary neglect and improved care consistency. 47 Conversely, dysfunctional coping (denial, avoidance) associates with greater burden and poorer care recipient health outcomes. 56
The positive impact of evidence-based psychosocial interventions—cognitive-behavioral therapies, mindfulness programs, digital support—on caregiver quality of life is well-documented. 11 By promoting emotional regulation and strengthening care skills, these interventions have an indirect but significant effect on care recipients’ clinical and subjective outcomes, especially in chronic conditions like dementia, stroke, and neurodegenerative diseases.14,26
Evidence also suggests integrating informal caregivers as therapeutic partners in person- and family-centered care models contributes to better therapeutic plan adherence and functional recovery rates for the care recipient. 10 This active collaboration builds trust and promotes care continuity, directly impacting the care recipient's emotional and functional stability.
Therefore, evidence consistently indicates that strengthening informal caregivers' resilience and coping strategies through systematic, context-sensitive psychosocial interventions is key to promoting the care recipient's quality of life. Caregiver resilience not only mitigates chronic stress effects but also enhances the ability to provide empathetic, effective, and humanized care, directly benefiting the care recipient's health trajectory.
Discussion
The metanarrative highlights the complex experience of informal care, transcending views of stress and overload. Studies demonstrate that experiencing care during prolonged adversity can be transformative, leading to positive psychological outcomes like Benefit Finding and Post-Traumatic Growth (PTG) .46,47 These phenomena lead to greater life appreciation, personal growth, spiritual expansion, and stronger family bonds. Benefit Finding and Growth (BFG) illustrates how reflection on difficulties yields significant subjective gains, including for caregiver identity construction.
These findings echo Janoff-Bulman’s (1992) cognitive reconstruction model: traumatic events reorganize mental schemes, positively attributing meaning to suffering. 48 Reenacting adversity is crucial for adaptation and individual/family resilience. Xu et al (2024) reinforce that caregivers understanding their role show less emotional exhaustion, greater self-efficacy, and improved quality of life, even in complex situations. This is influenced by perceived social support, family cohesion, and subjective reconstruction. 47
Resilience, in this context, is a relational and multisystemic phenomenon. 53 Social relationships, especially between caregivers, family, and health professionals, fundamentally mediate and strengthen resilience. Patient-focused home care with trusting health team interaction positively impacts perceived care effectiveness and caregiver well-being. Health policies promoting active family participation as care partners also prove beneficial. Continuous institutional support, service accessibility, and therapeutic coherence are essential for building trust and hope. Family resilience positively associates with PTG and negatively with caregiver burden, with PTG partially mediating this. 15
Regarding psychosocial interventions, the metanarrative highlights the transformative potential of those conducted by nurses and interdisciplinary teams. Studies demonstrate the effectiveness of psychoeducation programs, mindfulness-based interventions, and cognitive-behavioral therapies (CBT) in promoting caregiver resilience and reducing stress. 11 Psychoeducation provides structured information; mindfulness reduces psychological distress; CBT promotes adaptive cognitive/behavioral changes. Care models centered on the person and family recognize caregivers as therapeutic partners, leading to greater self-efficacy and less stress Assigning a positive meaning to the caregiving experience is associated with greater satisfaction and a reduction in the symptoms of stress and depression linked to the process.26,35
The interface between informal caregiver resilience and care recipient quality of life is highly relevant. Caregiver resilience and adaptive coping are fundamental determinants for the care recipient's home quality of life. Findings indicate resilient caregivers experience less burnout and greater emotional capacity, positively impacting interaction and care.17,26 Processes like Benefit Finding and Posttraumatic Growth bolster caregiver motivation and empathy, fostering a stable affective environment. 46 Effective coping strategies reduce stress and prevent neglect, contrasting dysfunctional strategies that aggravate caregiver burden and negatively impact care recipient health.14,56 Systematic, context-sensitive psychosocial interventions strengthening caregiver resilience and coping positively impact the care recipient’s quality of life.11,14 Integrating caregivers as partners also favors therapeutic adherence and functional recovery. 10 Caregiver resilience mitigates chronic stress, enhancing the ability to provide empathetic, effective, humanized care, directly benefiting the care recipient’s health trajectory.
What This Article Adds
This systematic literature review offers a fresh perspective on informal care, moving beyond the traditional focus on stress. It integrates recent studies46,47 to highlight the transformative potential of care during prolonged adversity, introducing Benefit Finding and Growth (BFG) as key to caregiver adaptation and identity.
Unlike literature emphasizing negatives, this review shows how caregivers build resilience through cognitive reconstruction, 48 reframing adversity to find intrinsic benefits. It underscores resilience’s relational and multisystemic nature, stressing the vital role of family dynamics 53 and social/professional support47,50 in reducing burden and boosting caregiver well-being.
The review also explores the transformative potential of psychosocial interventions by nurses and interdisciplinary teams (eg, Cheng et al, 2024; Chi et al, 2024; Nickell et al, 2020).11,14,56 Showcasing effectiveness of psychoeducation, mindfulness, and cognitive behavioral therapy, it advocates their systematic integration into family healthcare to strengthen caregiver resilience.
Finally, it clearly links informal caregiver resilience to the care recipient’s quality of life. Higher caregiver resilience and adaptive coping lead to better outcomes for those receiving care, emphasizing caregiver-focused interventions as an indirect but crucial way to improve recipient well-being. This work synthesizes knowledge with a new lens, advocating a holistic approach that recognizes inherent growth in informal care.
Strengths and Limitations
This systematic literature review exhibits several methodological strengths. Rigorous adherence to PRISMA 2020 guidelines ensured robust evidence identification and synthesis. Adopting a metanarrative approach integrated diverse epistemological and methodological perspectives, crucial for analyzing complex phenomena like family resilience and coping. The comprehensive search across CINAHL, MEDLINE, Scopus, Web of Science, and Psychology and Behavioral Sciences Collection maximized scope.
Four independent researchers meticulously conducted the study selection, minimizing bias through sequential assessment. Quality assessment of included studies using Joanna Briggs Institute (JBI) tools reinforced synthesis validity, ensuring good or moderate methodological quality. Data synthesis yielded 4 main thematic axes, providing an organized results structure. Finally, researchers' in-depth discussion ensured accurate knowledge interpretation and future research suggestions.
Despite these strengths, limitations warrant acknowledgment. The limited number of included studies (n = 7) may restrict generalization. The heterogeneity of study types (systematic/scoping reviews, qualitative/quantitative studies, expert opinion) introduces inherent variability. The acknowledged difficulty in assessing scoping review quality is a potential limitation. Furthermore, the specific focus on nursing interventions may have excluded relevant interventions from other health disciplines.
Relevance for Clinical Practice
This systematic review highlights crucial implications for clinical nursing practice, especially in family health. Findings reinforce integrating structured, family-sensitive interventions into daily practice. Such strategies promote active caregiver and family involvement, ensuring healthcare system sustainability and optimizing quality of life in long-term care.
The synthesis underlines the transformative potential of psychosocial interventions led by nurses (eg, psychoeducation, mindfulness, CBT). These reduce emotional burden, strengthen adaptive skills, and expand the meaning of care for caregivers. Their implementation empowers caregivers, improving their psychosocial well-being and care quality.
The review emphasizes care models centered on the patient and their family, recognizing the informal caregiver as a therapeutic partner. This relational approach fosters self-efficacy, role adaptation, and stress reduction in caregivers, contributing to care sustainability.
Ultimately, this study supports nursing practices valuing the family context, resilience, and effective coping, acknowledging the fundamental role of informal caregivers. It advocates their integration into public policy intervention networks. Prioritizing active listening, emotional support, and personalized interventions refines family health nursing, enhancing support for caregivers and families in complex care contexts.
Conclusion
This review examines how family-centered nursing interventions foster resilience and coping in informal caregivers and families. Interventions like psychoeducation, mindfulness, and CBT effectively modulate emotional regulation, ease caregiver burden, and strengthen relational resilience, optimizing the care recipient’s quality of life. The study emphasizes resilience and coping as dynamic processes, shaped by family ties, social support, and nursing interventions. The synergy between benefit finding, posttraumatic growth (PTG), and clinical practices of active listening and therapeutic bonding is crucial for caregiver mental health and sustainable home care. Integrating evidence, this review advocates for more sensitive and contextualized family health nursing, highlighting the need for family-centered care that empowers caregivers as therapeutic agents. Future research should include longitudinal studies, randomized trials, neurophysiological explorations, care model comparisons, and participatory methodologies.
Footnotes
Acknowledgements
The research team thanks their families for their support during this study. Additionally, we thank Ana Carolina Simões Carvalhinho, Ricardo Jorge Pratas Silva for their support in text revision and collecting data.
Author Contributions
RM, JG and EC contributed to the conceptualization. RM, JG and MP contributed to the curation of data. RM, JG, EC and MP contributed to the formal analysis of the studies. RM, JG, EC and MP contributed to the methodology.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Secondary data, obtained from other studies, available at accessed databases.
PROSPERO registration
This review wasn’t registered. Protocol was not prepared.
