Abstract
Background
As human activity expands into remote, extreme, and extraterrestrial environments, the role of nursing must evolve accordingly. Traditional nursing education rarely prepares nurses to function autonomously in settings where infrastructure, support, and resources are minimal or absent.
Purpose
The aim of this study was to present a conceptual framework and methodologic approach for educating nurses to operate competently and confidently in Earth's most remote regions, space, and extreme environments.
Methods
A multistep curriculum development process is described that includes a needs assessment, recruitment of subject matter experts, faculty development, and train-the-trainer strategies. Deliberate faculty training, hands-on experiential learning, and competency validation are integrated into a Doctor of Nursing Practice program filled with immersive simulation and field exercises, competency checkoffs, and program-evaluation metrics.
Results
Expected outcomes include measurable gains in self-efficacy, simulation performance, skills mastery, and postgraduation deployment in remote/space operating settings.
Conclusion
This model offers a path for graduate nursing education to prepare professionals for frontiers beyond hospital walls. Establishing outcome metrics and iteratively refining training will validate success and guide future expansion.
Introduction
The 21st century is seeing an expansion of human presence into more remote, harsh, and previously inaccessible spaces, such as polar outposts, deep-sea research stations, desert field sites, and even off-planet installations. With such expansion comes the critical need for medical care in environments far removed from conventional healthcare infrastructure. While physicians, expedition medics, and paramedics often receive specialized training for austere or field-based practice, nursing education has not yet fully embraced this evolving paradigm. This is not to minimize the essential contributions of these other disciplines but rather to emphasize that nurses also have a vital role, particularly in sustaining long-term care, monitoring, patient education, and holistic support, which are foundational elements of nursing. As missions and deployments become longer in duration, the continuous presence of well-prepared nurses is not just beneficial, it is essential.
Extreme/austere environments, for the purpose of this article, include geographic or operational settings that impose substantial physiologic, logistic, and environmental stressors (eg, extreme cold, heat, altitude, pressure, microgravity, and radiation) and where medical resources, supply chains, and infrastructure are minimal or absent. This working definition is a culmination from the Wilderness Medical Society's wilderness medicine 1 and hostile medicine as coined by the World Extreme Medicine Society. 2 Underserved in this context refers to locales with limited or no continuous access to healthcare personnel, diagnostic equipment, or referral pathways due to remoteness, geographic barriers, or unstable political/environmental conditions. 3
Access to healthcare in remote environments has measurable consequences for patients. Traumatic injuries in remote or rural areas have higher prehospital mortality than those in urban settings due to prolonged time to definitive care.4,5 In Australia, injury-related hospitalizations and death rates increase with remoteness; for instance, age-standardized injury hospitalization rates in very remote areas are more than twice those in major metropolitan centers. 6 These disparities highlight the urgent need for clinicians, including nurses, to be trained in delivering care in austere, isolated, and logistically challenging settings. Climate extremes exacerbate injury risks. Injury-related hospitalizations increased nearly 20% on days with very high ambient temperatures compared with the coldest days. 7 In regions with limited infrastructure, heatwaves, storms, or environmental hazards may overwhelm the local capacity to respond. 8
Given the expansion of human activity into Earth's most extreme environments, and even into space, nurse educators must begin preparing nurses for roles that extend far beyond traditional clinical settings. As space exploration, lunar bases, and private missions accelerate, healthcare delivery in microgravity, radiation-exposed, and psychologically isolating environments will become a reality. Other health professions have advanced structured training pathways in these areas, particularly within emergency medicine (EM). While several wilderness medicine fellowship opportunities exist for nurse practitioners, these programs are limited in number and scope, and most of the wilderness medicine fellowships remain targeted toward physicians and physician assistants. Medical and physician assistant students pursuing a career in EM may opt for a wilderness medicine track within the EM program. 9 In contrast, nursing education lacks broadly accessible doctoral-level curricular pathways that prepare nurses across diverse backgrounds for practice in extreme and austere environments beyond traditional wilderness settings. Nurses bring essential skills in long-term care, monitoring, injury/illness prevention, patient education, and psychological support, roles that become even more critical during prolonged missions or deployments. A research study by Abate and Mekonnen 8 showed that the knowledge and practice of nurses in prehospital emergency care were inadequate, even less than previous studies had suggested. Without dedicated preparation, nursing may be excluded from these emerging frontiers of care not due to a lack of value but due to a lack of readiness.
This paper presents a model for reversing that trajectory, an educational framework that prepares post–Master of Science in Nursing graduate nurses to operate safely, ethically, and effectively in extreme environments through a dedicated curriculum track embedded within advanced nursing education. It outlines strategies for faculty development, immersive experiential learning, competency validation, and program evaluation, offering a scalable model to ensure that nurses are not only present but also prepared, wherever care is needed.
Methods: Curriculum Development and Implementation
The curriculum framework was grounded in competency-based education, experiential learning, and professional identity formation, emphasizing adaptability, leadership, and interprofessional collaboration in austere and high-risk settings. Decisions were made to ensure academic rigor, reproducibility, and measurable outcomes using a structured, evidence-informed approach to address known gaps in nursing preparedness for extreme environments.
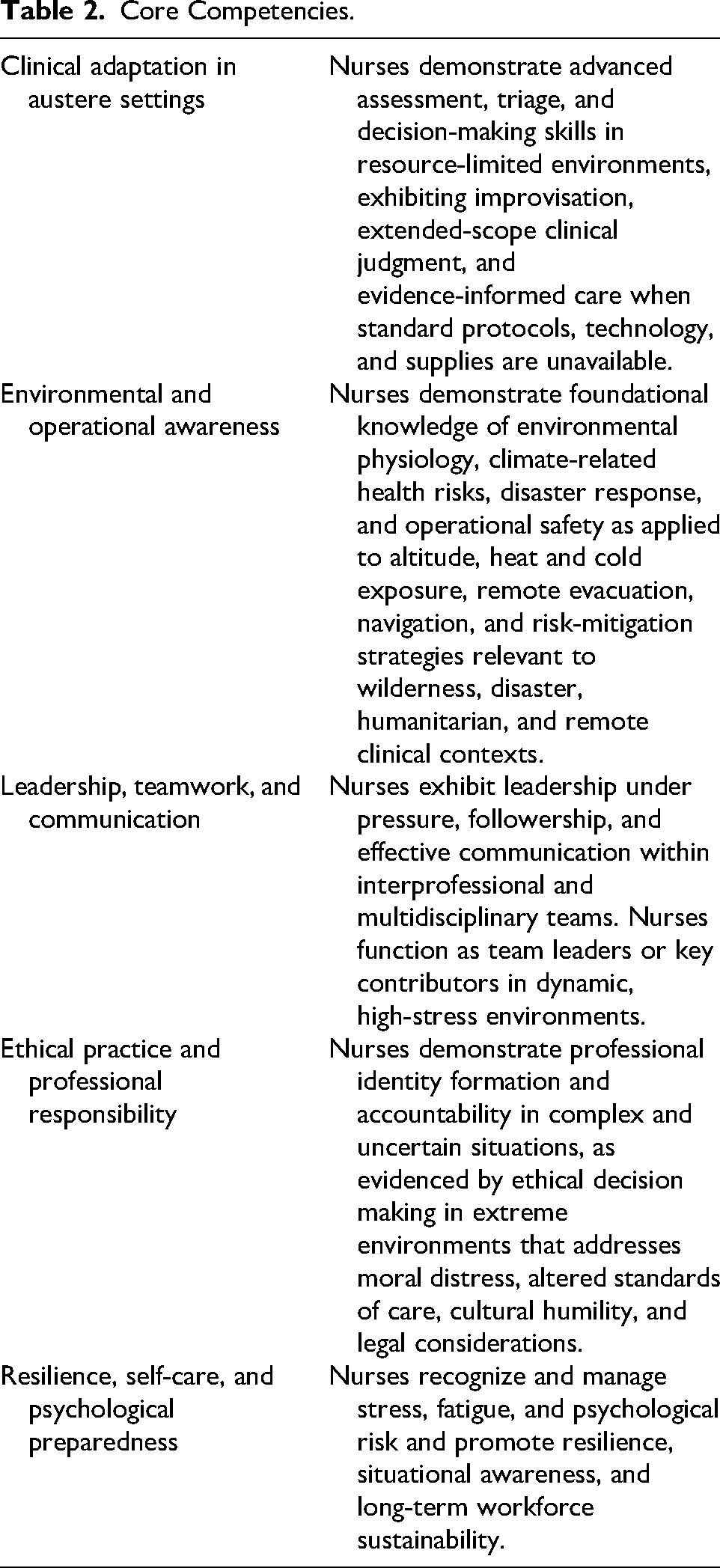
Development of the extreme environments Doctor of Nursing Practice (DNP) track occurred through an iterative process of needs assessment, curriculum mapping, implementation, and refinement (Table 1). The process began with a comprehensive needs assessment and gap analysis. A team compared existing graduate nursing curricula with established competency frameworks from wilderness medicine, 10 military prolonged field care, 11 remote and offshore medicine, 12 and aerospace medicine. 13 This benchmarking process was supplemented by interviews and surveys conducted with clinicians experienced in extreme environments, including expedition medics, polar health professionals, military medical staff, and space medicine personnel. Participants in these interviews and surveys were provided with the relevant competency frameworks and overviews of existing graduate nursing curricula. They were asked to identify gaps in current training, specify skills and knowledge requiring experiential learning, and highlight critical competencies needed for independent practice in austere environments. This combined approach allowed the needs assessment to capture both structured benchmarks and practical, real-world requirements for extreme environment nursing. Findings from the needs assessment revealed consistent deficiencies in traditional graduate nursing education related to survival and self-sufficiency, environmental pathophysiology, independent clinical decision making with limited support, remote diagnostics, and leadership in isolated or resource-limited contexts. These findings informed us of the foundation of the new curriculum design. Table 2 lists our core competencies that were used throughout the development of the curriculum.
Timeline of Development for the Doctor of Nursing Practice Extreme Environments Track.

Core Competencies.
To ensure domain-specific accuracy and relevance, subject matter experts (SMEs) were recruited from key organizations such as the Wilderness Medical Society, World Extreme Medicine, the College of Remote and Offshore Medicine, and military medical teams. Curriculum mapping, scenario development, content review, and mentorship of faculty were completed. The involvement of SMEs ensured that the material reflected current best practices and operational realities in extreme care settings. The curriculum framework is designed to be layered, beginning with personal survivability in various extreme environments. Fundamental impacts of the environments on physiology and nursing interventions will be covered in environmental domains and completed with organizational and operational applications of each of the extreme environments. As courses progress, content will be continually evaluated for an iterative model of continuous process improvement, allowing for real-time alterations to meet the needs of the students while maintaining student outcome goals.
Faculty development was a parallel priority. Faculty members were selected based on prior experience, expedition support, military healthcare, wilderness leadership, or similar domains as well as desire and willingness to take the nursing profession to the edge. For faculty lacking technical experience in specific environments, formal training was pursued. This included certifications in cold weather medicine, dive and marine medicine, wilderness expedition leadership, and simulated microgravity environments. A train-the-trainer model was implemented to facilitate program scalability: Initial faculty cohorts will become certified to teach future modules and mentor subsequent instructors.
The program was developed by modifying an existing DNP program, allowing students to meet standard DNP competencies while specializing in extreme environment care. Entrance requirements include a graduate degree in nursing (Master of Science in Nursing) from an accredited program and a current Registered Nurse license. Applicants also need a statistics course with a grade of B or better and completion of the three P's (advanced pharmacology, advanced physical assessment, and advanced pathophysiology). Courses and modules were designed to align with established credit structures and academic outcomes while integrating new domains such as survival techniques, environmental physiology, remote diagnostics, equipment adaptation, improvisational care, and crisis leadership. Table 3 provides a high-level overview of these courses, showing how each aligns with core competencies and associated experiential methods. These competencies were organized around environmental categories including alpine/arctic, desert/tropical, maritime/space, and politically unstable or logistically isolated regions.
Outline of Curriculum—Mapped to Competences.

The DNP Extreme Environment track curriculum is now fully developed (Table 1). Recruitment and admission of the inaugural cohort are planned for the fall of 2026. Faculty involved in the program have completed foundational training in relevant extreme environment and wilderness medicine disciplines, with ongoing mentorship and certification activities to ensure readiness for program implementation.
Learners entering the DNP Extreme Environment track may come from diverse clinical backgrounds, and many may not have prior experience in prehospital or emergency care settings. Nursing practice in prehospital environments requires a distinct cognitive framework emphasizing rapid assessment, priority setting, and care delivery in resource-limited or austere settings. Prior experience in emergency nursing, emergency medical services, or flight/transport nursing may support readiness for these environments; however, the program does not require prehospital training for learners without such backgrounds. Awareness of this variability is important for understanding learner preparation and the context in which the track is implemented.
The DNP Extreme Environment track follows a hybrid model, primarily online with time required on campus or on selected sites for experiential learning, which serves as the curricular cornerstone. Immersive hands-on activities included outdoor simulations in cold, heat, altitude, and jungle-like conditions; high-fidelity simulations incorporating environmental stressors such as low light, dehydration, and communication delays; and scenario-based clinics set in mock remote locations. Students also will gain exposure to portable diagnostic equipment, unmanned aerial vehicle–supported logistics, and remote telemedicine platforms. Instruction emphasizes progression from personal survival skills to team-based clinical care in extreme and austere settings.
Competency assessment is multimodal, ensuring that students can apply their knowledge under pressure and in realistic conditions. Objective-structured clinical examinations were adapted to reflect the challenges of care in remote environments. Hands-on checkoffs cover technical skills such as shelter construction, water purification, and use of field-adapted ultrasound. Scenario performance will be evaluated by SMEs using standardized rubrics, and debriefing sessions will promote reflective learning. Peer evaluations and team-based assessments will reinforce leadership, collaboration, and adaptability. Clinical hours will be obtained by capstone/research projects as well as approved field experiences from courses such as the Wilderness Life Support for Medical Professionals course or expeditionary trips such as alpine search and rescue, maritime medical internships, or humanitarian expositions as a nurse. Clinical hours can be completed with physicians, nurse practitioners, or nurse leaders who work or serve in extreme environments.
Graduates who demonstrate advanced proficiency will be invited to enter the train-the-trainer pathway. These individuals will participate in faculty development, lead simulation activities, and support future cohorts, creating a sustainable model for institutional capacity building and long-term curricular growth.
Program evaluation includes both formative and summative metrics. Pre- and postcourse self-efficacy surveys will measure changes in confidence related to extreme environment competencies. Objective-structured clinical examinations and checkoff data will provide quantitative evidence of skill acquisition. Simulation performance, qualitative student feedback, SME assessments, and time-to-task metrics will be used to monitor learning progression. Postgraduation follow-up will be initiated to track deployment into remote or extreme roles, contribution to publications or projects, and continued engagement with the program as instructors or mentors. Longitudinal monitoring will be used to evaluate knowledge retention, evolving practice, and the broader impact of the program on nursing capacity in extreme environments.
Curriculum Overview
The DNP Extreme Environment track is structured to sequentially build knowledge and skills across core competency domains, integrating classroom instruction with experiential learning in each environmental category. This overview highlights the organization of courses, the progression of content, and how experiential methods are embedded throughout the curriculum.
On completion of core modules, students will participate in a culminating capstone field simulation to integrate all learned competencies. In this immersive scenario, students will plan, establish, and operate a healthcare clinic in a simulated extreme environment. Students will be responsible for infrastructure setup, supply and logistics planning, patient triage, diagnostics, team coordination, and evacuation planning. This integrated scenario will allow for the assessment of applied competencies across all domains under realistic constraints and will reinforce leadership, problem solving, and adaptability in austere settings.
Challenges and Mitigation Strategies
Developing an DNP Extreme Environment track has presented several notable challenges. First, there are no existing nursing-specific models to directly emulate; therefore, the curriculum must carefully adapt knowledge from military, expedition, and wilderness medicine disciplines while maintaining a distinct nursing perspective. By a distinct nursing perspective, we mean an approach that emphasizes holistic patient assessment, care coordination, advocacy, ethical decision making, and the application of nursing theory and standards in resource-limited and high-risk settings. This nursing perspective will ensure that care remains patient centered and safety focused, even when adapted from practices in other disciplines. Addressing faculty capability gaps is essential, requiring formal certifications, ongoing mentorship, and implementation of a train-the-trainer model to build scalable expertise. Resource intensity poses another hurdle because acquiring durable equipment, advanced simulation modules, and accurate environmental replicas involves substantial cost. Securing grant funding and strong institutional support thus is critical to program sustainability. Safety considerations are paramount during field exercises, necessitating strict oversight, conservative safety margins, and a phased approach to experiential learning to minimize risk. Furthermore, maintaining fidelity across diverse environments is complex; equipment that is effective in one setting may be unsuitable in another, underscoring the need for modular and interoperable design of teaching tools and gear. Finally, evaluating the program's real-world impact demands long-term partnerships and systematic follow-up of graduates deployed to genuinely extreme settings, ensuring that training translates to effective practice in the field.
Discussion and Future Directions
This educational model represents a critical shift in nursing training, moving beyond traditional institutional settings and toward the most challenging frontiers where care delivery is essential but isolated and complex. The DNP Extreme Environment track aims to develop nurses who are not only clinically competent but also resilient, autonomous, and capable of innovative problem solving in resource-scarce and unpredictable conditions. By equipping graduate nurses with specialized skills to function independently in austere settings, this program addresses a crucial gap in nursing education and expands the nursing profession's reach into new domains.
Several key areas warrant further development to strengthen and sustain this training paradigm. Formal research is needed to evaluate long-term outcomes among graduates, including their deployment to extreme environments, retention in specialized roles, and the impact of their care on patient outcomes. Building strategic partnerships with space agencies, polar research stations, and organizations operating in remote health settings will be essential to provide real-world opportunities and enhance curricular relevance. Additionally, expanding the program into certificate offerings or continuing-education courses could extend access to practicing nurses seeking specialization in extreme environment care. Comparative studies investigating different training models, cost-effectiveness, and the translational impact of this education will further inform best practices and resource allocation.
Beyond program expansion and research considerations, the DNP Extreme Environment track could potentially be adapted for nurses entering through different DNP pathways, including clinical or leadership-focused programs. Implementation in tracks outside the current student population may require additional educational experiences to cultivate an emergency mindset, particularly for learners without prior acute or prehospital experience.
Furthermore, early preparation at the undergraduate level could be valuable for developing foundational extreme environment knowledge and skills. Introducing this content in prelicensure programs may help cultivate interest in advanced practice tracks, establish a pipeline of nurses ready for DNP-level specialization, and support the formation of special interest groups focused on expedition experiences, team-based learning, and skill development. Although not currently implemented at the undergraduate level, this approach represents a potential strategy to enhance career progression and seed future enrollment in advanced extreme environment nursing programs.
While the current DNP Extreme Environment track focuses on preparing nurse post–Master of Science in Nursing graduate nurses for practice in austere and high-risk settings, nurses across a variety of experience levels and specialties, including registered nurses, certified registered nurse anesthetists, certified nurse-midwives, and clinical nurse specialists, also can contribute meaningfully to wilderness and extreme environment practice. Acknowledging these roles highlights the potential for adapting the curriculum principles presented here to create educational programs that prepare diverse nursing professionals for practice in extreme environments. Such efforts could expand workforce capacity, enhance interdisciplinary collaboration, and ensure that care in austere settings benefits from the full spectrum of nursing expertise.
As humanity continues to explore and inhabit deserts, polar regions, deep oceans, and even outer space, nursing must evolve to accompany these endeavors. By rigorously preparing nurses for the unique challenges of extreme environments, we ensure that wherever human presence extends, high-quality and compassionate care follows. This initiative represents not only an expansion of nursing practice but also a commitment to advancing health equity and resilience in the most demanding contexts.
Footnotes
Author Contribution(s)
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
