Abstract
Introduction
Submersion injuries are rare yet life-threatening events. The Trauma Quality Improvement Program (TQIP) registry is the largest national trauma registry in the United States. We describe the epidemiology and outcomes of submersion injuries in the TQIP registry.
Methods
We analyzed data from the TQIP registry for all encounters with a primary or secondary mechanism that included a submersion or drowning description. We used descriptive statistics to portray encounter data including disposition and survival. We used inferential and multivariable logistic regression analyses to identify associations with survival
Results
From 2017 to 2023, there were a total of 8,014,737 trauma encounters, of which, 1677 met our inclusion criteria of a primary or secondary mechanism that included a submersion injury. Of the 1150 survivors, 656 (57%) were discharged home without additional services planned. In our multivariable logistic regression, we noted the following associations with survival: age in years (unit odds ratio, 0.98; 95% CI, 0.98–0.99), male sex odds ratio 1.25 (95% CI, 0.89–1.73), prehospital arrest odds ratio 0.15 (95% CI, 0.11–0.21), interfacility transfer odds ratio 0.52 (95% CI, 0.37–0.71), any signs of life on arrival odds ratio 11.33 (95% CI, 5.90–21.75), head/neck injury odds ratio 0.42 (95% CI, 0.31–0.58), thorax injury odds ratio 0.36 (95% CI, 0.24–0.55), abdomen injury odds ratio 0.36 (95% CI, 0.24–0.56), extremities injury odds ratio 2.70 (95% CI, 0.65–11.16), skin injury odds ratio 1.49 (95% CI, 0.69–3.21), any in-hospital arrest odds ratio 0.13 (95% CI, 0.08–0.20), emergency department intubation odds ratio 0.97 (95% CI, 0.65–1.43), and hypothermia <35°C odds ratio = 0.30 (95% CI, 0.21–0.44).
Conclusions
Submersion injuries were rare in the TQIP registry. In the setting of trauma, most survived to hospital discharge, of whom most were discharged home. Prehospital arrest, in-hospital arrest, lack of signs of life on arrival to the emergency department, and serious injuries to all body regions were associated with lower survival to discharge.
Introduction
Background
Submersion injuries, also called drowning, are rare yet life-threatening events. Submersion injuries account for 9.29 per 100,000 emergency department (ED) visits. 1 Such injuries can occur in isolation but also can occur in the setting of other events, such as motor vehicle trauma or boating injuries. Previous estimates suggest that nearly 10 submersion injury deaths occur in the United States every day, most of whom are adults. 2 Although most submersion events are nonfatal, many result in long-term neurologic sequelae. Moreover, submersion injuries are also a major cause of unintentional death in children. 3 Out-of-hospital cardiac arrest in the setting of submersion injuries portends a poor outcome, with Youn et al noting a 16% survival rate, but good neurologic outcomes occurred in 43% of those who survived. 4 Hansen et al assessed the annual healthcare costs associated with submersion injury.5 They found that there were nearly 12,000 visits to the ED per year, of which 6% of patients died, and 24% were admitted. They estimated the total ED costs to be ∼$12.5 million, with total in-patient costs to be $27.5 million, resulting in $40 million in total annual costs. 5 El Sibai et al examined >12,000 patients and found that nearly 1 in 8 had a poor functional outcome.1 Moreover, they found that submersion injuries in conjunction with motor vehicle trauma carried a significantly higher risk of a poor outcome. 1
One systematic review of 24 studies assessed factors associated with a favorable neurologic outcome.6 The authors found that submersion duration of <5 min was associated with favorable neurologic outcomes, whereas submission times >25 min were universally fatal. 6 The studies included in that review ranged from 28 to 1737 patients. Another systematic review analyzed 3 studies assessing interventions following submersion injury and found that in-water rescue breaths were associated with better outcomes and that no conclusions could be drawn between compression-only cardiopulmonary resuscitation (CPR) versus standard CPR, and the authors concluded that there are limited data to inform treatment guidelines. 7 There still exists a need for larger datasets on submersion injuries that have discharge and outcome data. Trauma registry data offer unique insights into submersion injuries that occur concomitantly with another injury.
Goal of This Study
We describe the outcomes of submersion injuries in a US national trauma registry and identify associations with survival. We sought to perform a secondary analysis that focused on children <18 y of age.
Methods
Ethics
We submitted a request for and obtained data from the American College of Surgeons Trauma Quality Improvement Program (TQIP) database, including the additional facility keys that are deidentified versions of the facility name. The US Army Medical Center of Excellence regulatory office reviewed Protocol 24-00011n and determined that it met the definition of research not involving human subjects. We followed the Strengthening of the Reporting of Observational Studies in Epidemiology (STROBE) reporting guidelines. 8
TQIP Description
The TQIP database has been maintained by the American College of Surgeons since 2008. Submitting data are mandatory for verified trauma centers, and TQIP also collects patient information from other centers that do not meet verification criteria on a volunteer basis. The goal of the program is to provide national data to aid trauma centers in standardizing trauma care, providing local and national quality improvement, and to provide data needed for best practices guidelines. As of 2023, there were >800 participating centers where trained registrars enter data for trauma encounters that meet entry criteria. 9
Case Selection and Variables
We analyzed trauma encounters with a primary or secondary mechanism that included submersion or drowning. Signs of life were defined using the arrival vital signs with a heart rate, systolic pressure, or respiratory rate of >0 breaths/min or a Glasgow Coma Scale (GCS) score of >3. Respiratory assistance on arrival was based on the arrival vital signs metric. Prehospital cardiac arrest was based on the dedicated vital signs metric. In-hospital CPR was based on the core quality metric of cardiac arrest (no timing data) or procedure codes relevant to CPR. If the procedure code time was less than or equal to the ED LOS, we considered the CPR as performed in the ED. ED intubation was defined similarly and using methods previously described. 10 We defined pediatric patients as persons <18 y of age. The presence of alcohol was based on the core variable captured for alcohol concentration, if ordered. Past medical history was based on the core variables captured.
Data Analysis
We performed all statistical analysis using JMP Statistical Discovery from SAS (version 17; SAS Institute, Cary, NC). Continuous and ordinal variables are presented with medians and interquartile ranges. Categorical variables are presented as percentages and numbers. Missing variables were managed through pairwise deletion. Multivariable logistic regression models were constructed to test for associations with survival and adjusted for potential effect modifiers based on clinical relevance.
Results
Overall
From 2017 to 2023, there were a total of 8,014,737 total trauma encounters, of which 1677 (0.02%) met our inclusion criteria with a primary or secondary mechanism that included a submersion injury (Table 1). Of the 1150 survivors, 656 (57%) underwent discharge home without additional services planned. There were 365 survivors (44%) who had any alcohol documented, with 145 (17%) who had a documented concentration ≥0.2 mg/dL. Of those who had a drug screen performed (n=683), there were 51 (7%) positive for cocaine, 15 (2%) positive for methamphetamine, 25 (4%) positive for opioids, and 137 (20%) positive for marijuana. There were 19 (1%) that received extracorporeal membrane oxygenation (ECMO) support during the hospitalization, with the median time from arrival to ECMO initiation of 8 (3–62) h, with 2 patients initiated in the ED. Of those placed on ECMO, 15 survived to discharge. Of those with an arrival GCS score of 15 (n=578), 571 (99%) survived to discharge, none died in the ED, and 65 (11%) were discharged directly home from the ED. Based on place-of-injury codes, the most common locations were public water (n=237), followed by pools (n=166; see online Supplemental Figure S1). Most injuries were from unspecific mechanisms (see online Supplemental Figure S2). Any signs of life on arrival were highly associated with survival to discharge (Table 2). The most common in-hospital events were acute kidney injury and ventilator-associated pneumonia (see online Supplemental Figure S3). There were 694 patients who had prehospital cardiac arrest, of whom 276 (40%) survived to discharge, with 113 (41%) discharged home without additional services planned. There were 256 who had an in-hospital cardiac arrest, of which 48 (19%) survived to discharge, with 12 (25%) discharged home without additional services planned.
Patient Characteristics.
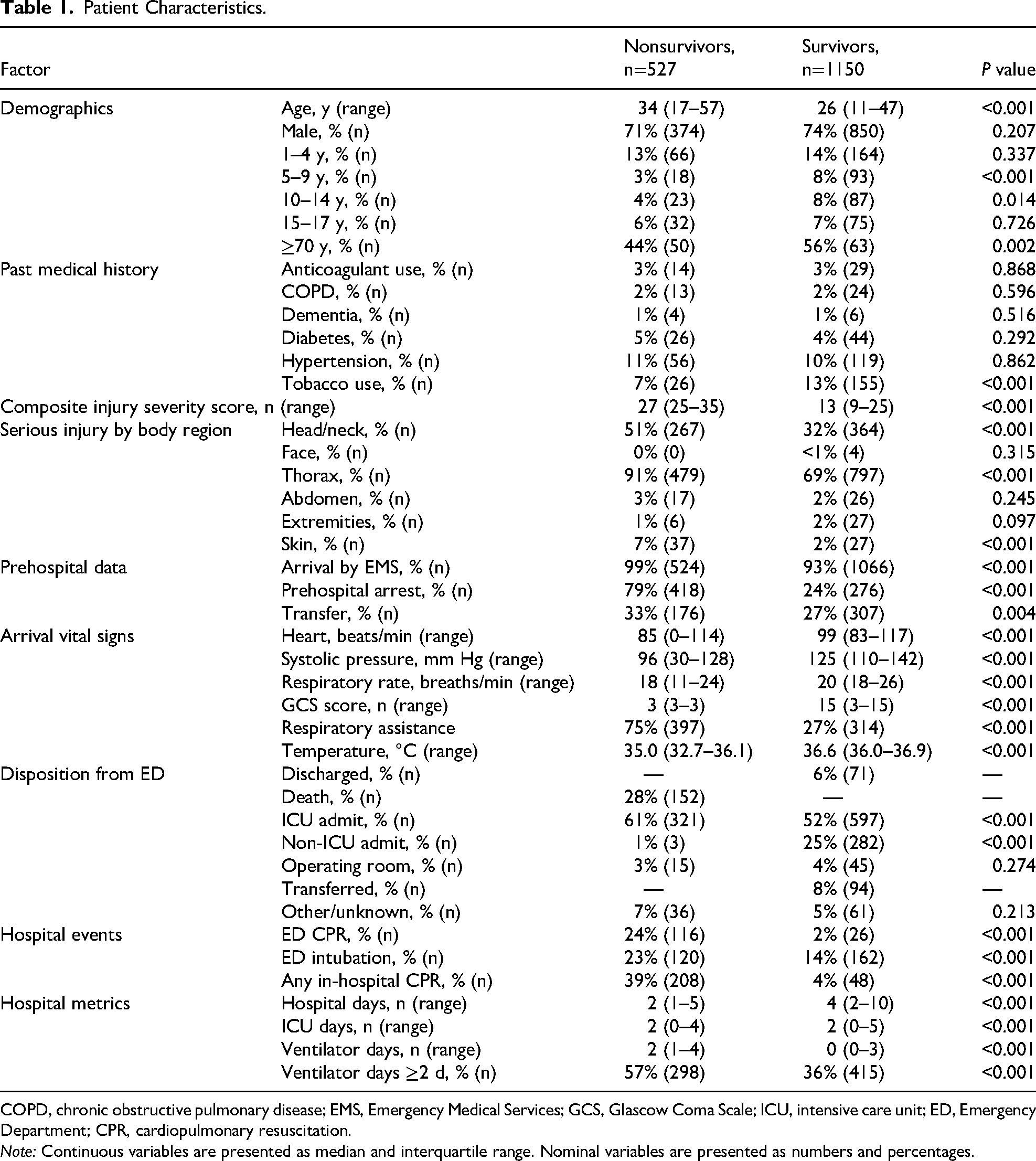
COPD, chronic obstructive pulmonary disease; EMS, Emergency Medical Services; GCS, Glascow Coma Scale; ICU, intensive care unit; ED, Emergency Department; CPR, cardiopulmonary resuscitation.
Note: Continuous variables are presented as median and interquartile range. Nominal variables are presented as numbers and percentages.
Multivariable Logistic Regression Model with Discharge Survival as the Outcome Variable.
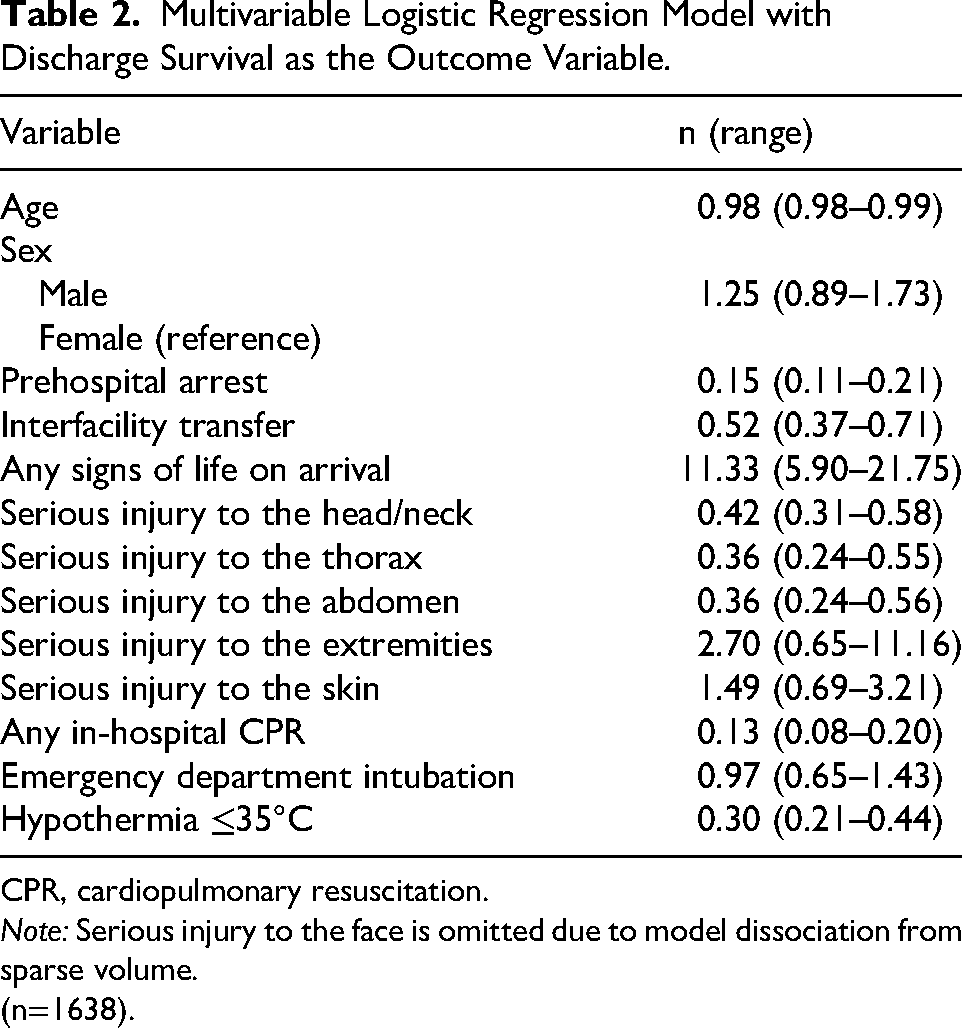
CPR, cardiopulmonary resuscitation.
Note: Serious injury to the face is omitted due to model dissociation from sparse volume.
(n=1638).
Pediatric Subanalysis
There were 558 trauma patients with a documented age <18 y who met the inclusion criteria for this subanalysis (Table 3). Of the 419 survivors, 271 (65%) were discharged home without additional services planned. There were 14 (1%) who received ECMO support during the hospitalization, with the median time from arrival to ECMO initiation of 44 (13–86) h and with no cases of initiation in the ED. Of those placed on ECMO, all survived to discharge. Of those with an arrival GCS score of 15 (n=216), all survived to discharge, and 33 (15%) were discharged directly home from the ED. There were 239 who had prehospital cardiac arrest, of which 121 (51%) survived to discharge, with 59 (25%) discharged home without additional services planned. There were 67 who had an in-hospital cardiac arrest, of which 19 (28%) survived to discharge, with 6 (9%) discharged home without additional services planned. Age 5 to 9 y and signs of life on arrival were associated with survival to discharge (Table 4).
Pediatric Patient Characteristics.
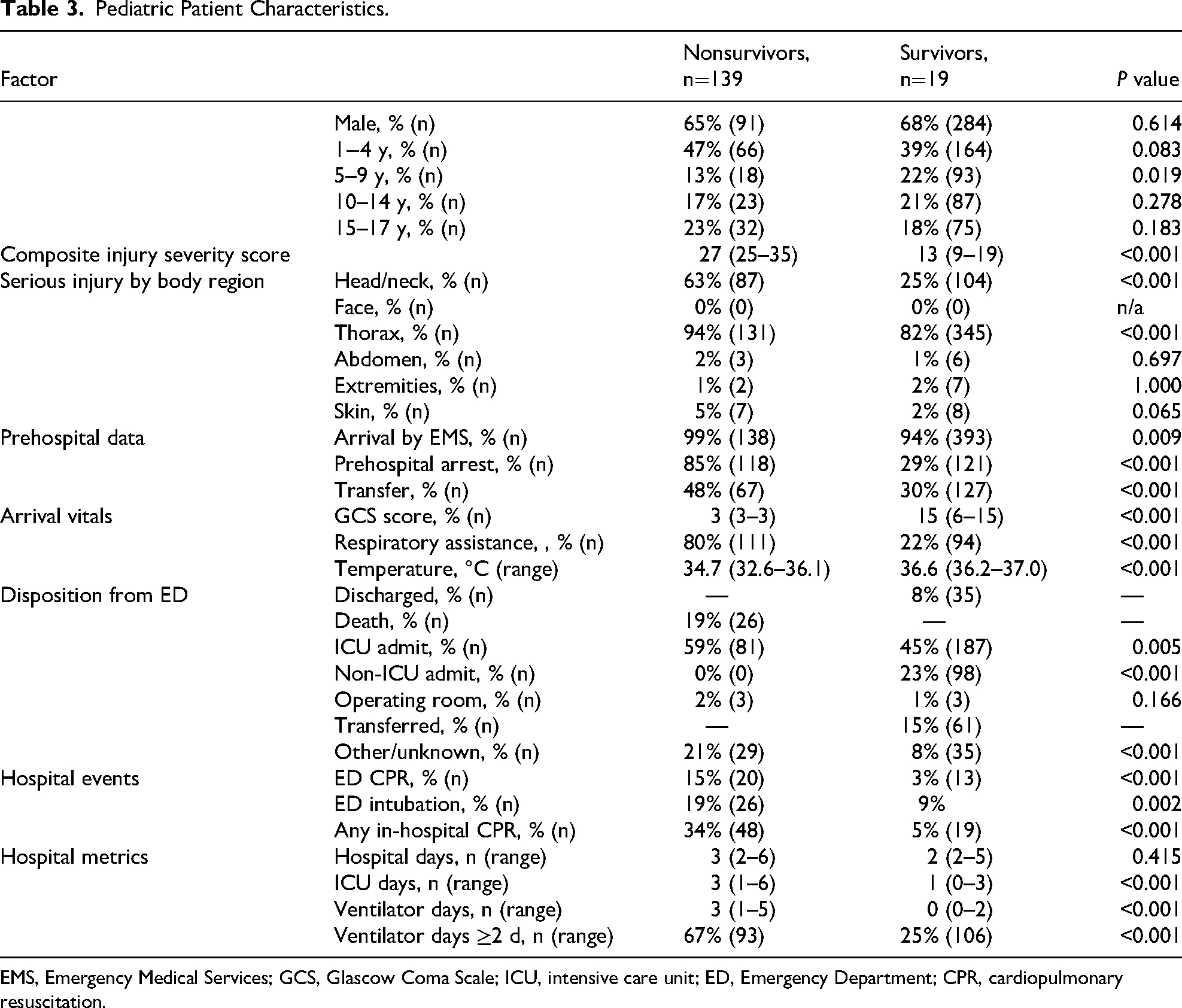
EMS, Emergency Medical Services; GCS, Glascow Coma Scale; ICU, intensive care unit; ED, Emergency Department; CPR, cardiopulmonary resuscitation.
Multivariable Logistic Regression Model with Discharge Survival as the Outcome Variable Among Pediatrics.
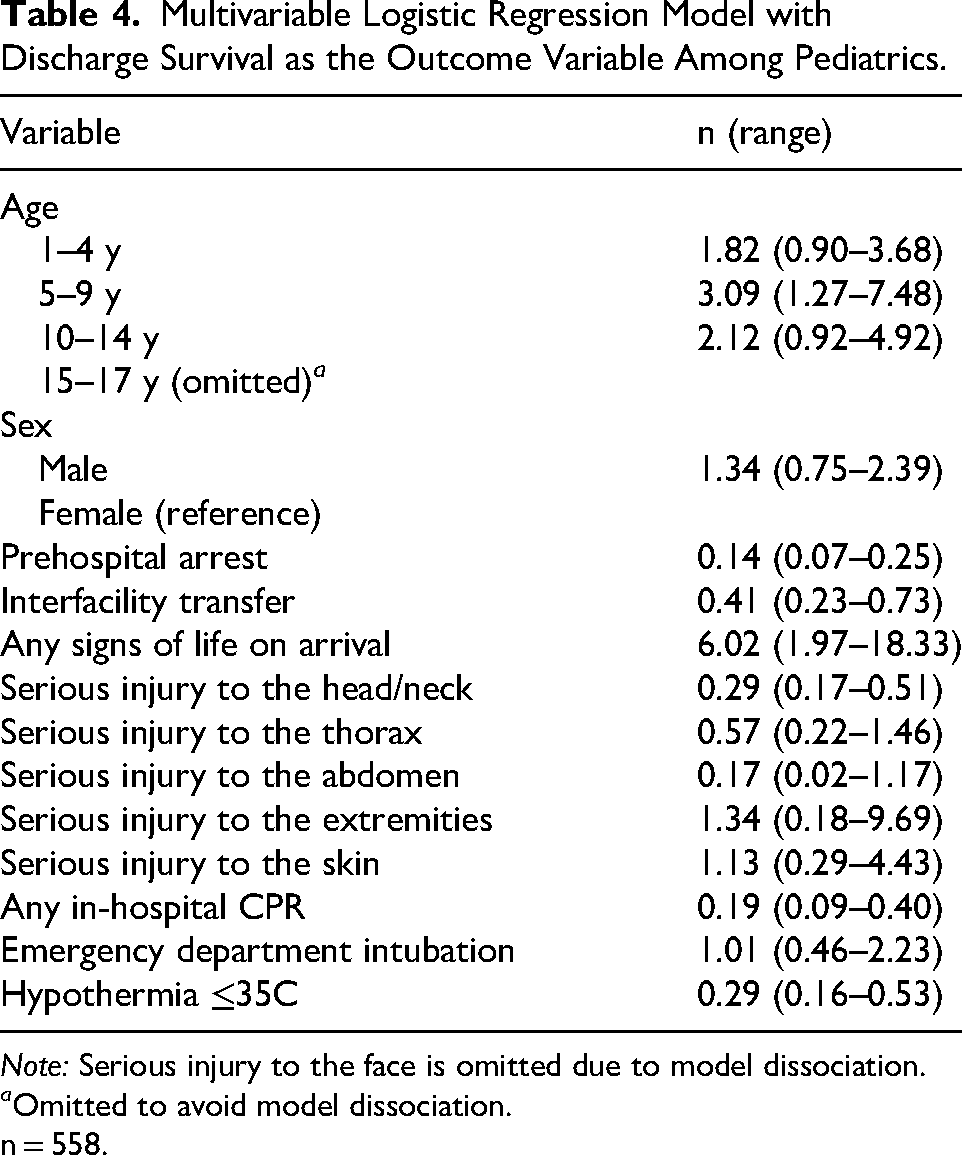
Note: Serious injury to the face is omitted due to model dissociation.
a Omitted to avoid model dissociation.
n = 558.
Discussion
In this analysis spanning 7 y in the largest national trauma registry in the United States, we found that most patients presenting after submersion injury survived to discharge, with a large number discharged home without additional services. This indirectly suggests that most of the survivors had good neurologic outcomes. Although the findings associated with prehospital and in-hospital arrest are unsurprising, there are several other findings that require further interpretation. One notable finding was the association of interfacility transfers with increased mortality. We hypothesize that this is less likely due to deterioration of the condition enroute and more reflective of the selective nature of the referring facilities only transferring the most critically injured patients. 11 Although our regression models controlled for measured variables of illness severity, we cannot control for unmeasured confounders. The association of increased mortality with nearly all the seriously injured body regions is unsurprising, but the proportion of serious injury by body region was substantially higher than other previous reports from the same registry, even among the most critically injured.10,12 This highlights the polytrauma nature of many submersion injuries. Further, we were surprised by the lack of an association of ED intubation with mortality, particularly because patients requiring that procedure are among the most critically injured. 13 Our study offers unique insight into submersion injuries that occur in the setting of trauma using very large datasets that span >800 trauma centers as of 2023.
Our pediatric data are consistent with other data reported in the literature. Children <5 y of age remain at the highest risk of submersion injuries and have the highest fatality rates.14–17 This is unsurprising given that the recommendation is for children to start swim lessons and water safety classes as young as 1 y of age, yet most do not achieve adequate swimming skills until at least age 4 y. 18 Our reported outcomes are not as granular as recent focused pediatric studies, but the number of pediatric patients discharged without need for additional services supports the reported positive neurologic outcomes in the pediatric population.
Our study includes several strengths when compared with other studies. This is one of the largest studies published to date that includes outcome data such as the discharge location of those requiring admission. The study by El Sibai et al is probably most comparable, for which they had a large size (n=12,529), but their data also carried limitations frequently seen with big data studies.1 Although they did have data regarding the outcomes after ED evaluation, they lacked hospital data including adverse events, which we reported. Moreover, we reported the final discharge location for the more critically injured patients, including those requiring intensive care and ventilatory support. 1 Although these big data studies do not contain the same granularity as some of the smaller studies, the larger size allows for more powerful statistical analyses often uncovering less common events, such as acute kidney injury and ventilator-associated pneumonia, which we have reported. Other rare events of specific interest to the submersion injury population were the inclusion of patients requiring extracorporeal support, with relatively high survival. Aside from the study by El Sibai et al, our study represents a large sample and the only one drawn from the TQIP registry.
There are several limitations to our study. The primary limitation is that despite the large size of the database, it lacks granularity relevant to submersion injuries. Most notably absent is the submersion time, witnessing of the event, and in the setting of prehospital arrest, whether bystander CPR was performed. These details are particularly important because previous studies have noted that submersion time is a key factor in predicting survival.1,6 A related limitation is that our regression analysis could only control for measured confounders. However, the large size of the database allowed us to make assessments as to the frequency in which submersion injuries happen in the setting of trauma. Second, there are injury severity requirements that must be met to be included in the registry. As such, those with isolated submersion without other trauma are likely not captured to any reliable degree. Lastly, the inclusion of the injury codes required to be identified for the study relies on adequate documentation, which may have resulted in omissions of potential encounters for which submersion injuries were present but not documented.
Conclusions
Submersion injuries were rare in the TQIP registry. In the setting of trauma, most submersion patients survived to hospital discharge, and most were discharged home. Prehospital arrest, in-hospital arrest, lack of signs of life on arrival to the ED, and serious injuries to all body regions were associated with lower survival to discharge.
Supplemental Material
sj-docx-1-wem-10.1177_10806032251393142 - Supplemental material for Submersion Injuries in the United States Trauma Quality Improvement Program Trauma Registry from 2017 to 2023
Supplemental material, sj-docx-1-wem-10.1177_10806032251393142 for Submersion Injuries in the United States Trauma Quality Improvement Program Trauma Registry from 2017 to 2023 by Steven G. Schauer, Ashley E. Sam and Michael D. April in Wilderness & Environmental Medicine
Footnotes
Author Contribution(s)
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: SGS and MDA have received funding from the US Department of Defense in the form of grants to their institution for unrelated efforts. SGS has received grant funds from SeaStar Medical for unrelated efforts. No salary support has been provided. We have no other conflicts to report.
Disclaimer
The views expressed in this article are those of the authors and do not reflect the official policy or position of the US Army Medical Department, Department of the Army, Department of Defense, or the US Government.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
