Abstract
Objective
Patients with cancer often use complementary and alternative medication (CAM). This research aims to study the current attitude of healthcare professionals toward the use of CAM to improve current care.
Methods
A questionnaire on both the current practice and opinions about CAM use was sent to healthcare professionals in Amsterdam UMC, who work for the department of hematology or oncology. Oncologists, hematologists, residents, (specialized) nurses, dieticians, (hospital)pharmacists, and pharmacy technicians were asked to participate in this study.
Results
Among eligible healthcare professionals, 77 responded to the questionnaire (34%). Overall, 87% of healthcare professionals indicate it is important to be aware of their patient's CAM use, and all find the potential of drug–herb interactions important. However, more than half of the healthcare professionals inquire about the patient's CAM use infrequently. In addition, only 15% of the healthcare professionals stated they had sufficient knowledge of CAM to advise patients on their use of CAM.
Conclusions
Healthcare professionals are aware of the potential risks of CAM use in combination with anti-cancer treatment. However, CAM use is not yet discussed with every patient. This may be due to healthcare professionals’ lack of knowledge about CAM.
Introduction
Anti-cancer therapy can be exhausting and significantly impact patients' physical and mental health. For some patients, this can be a reason to inquire about other options such as complementary and alternative medication (CAM), sometimes also referred to as “integrative medicine.” CAM can be defined as alternative medical systems, such as traditional Chinese medicine, Ayurveda, mind–body interventions including prayer and meditation, biologically based therapies such as vitamins, herbs, and dietary supplements, and body-based interventions including massage, chiropractic, and energy-based interventions. For the pharmaceutical consultations and interventions, we focused our research on biologically based therapies. The prevalence of CAM use varies across regions but is generally high in patients with cancer.1,2 In addition, up to 70% of patients do not bring up their CAM use in communication with their healthcare professionals during consults. 3 Some of the biological CAMs have the potential to negatively affect anti-cancer therapy, for example, through herb–drug interactions. 4 Proper information from healthcare professionals to patients may prevent interactions with CAM. However, the use of CAM by patients is often only partially known by healthcare professionals. 5 This missing information on the use of CAM can thus lead to unknown drug–herb or other interactions with therapy failure or amplification of the side effects of the conventional anti-cancer therapy as a result. Some previous studies on the perceptions and beliefs of healthcare professionals are available, but targeted mainly just physicians6–8 or pharmacists. 9 In oncology care, patients communicate with a wide range of professionals, including also nurses, dieticians, and pharmacy technicians. Therefore, we aimed to study the opinions of all healthcare professionals involved in care for patients undergoing systemic therapy in our facility toward CAM use.
Methods
Setting and population
The hospital pharmacy of the Amsterdam UMC has developed a methodology to circumvent potential unawareness about CAM use and drug–CAM interactions. At each clinical admission, a pharmacy technician performs a medication reconciliation with the patient. This includes inquiring about the patient's use of biologically based CAM in a nonjudgmental manner. All CAMs the patient reports using are added to the home drug list in the electronic patient file. Potential interactions are assessed by a pharmacist, and if intervention is necessary, the pharmacist gives a piece of advice to the patient and their physician, which is also documented in the electronic patient files. To assess if our methodology of mapping and assessing CAM use meets the expectations of healthcare professionals, we performed a survey in our institution. The healthcare professionals for this study were thus selected from the Amsterdam UMC and were working in the department of oncology, hematology, or the hospital pharmacy. An email was sent to all individual healthcare professionals in the following occupations: hematologists, oncologists, residents, (specialized) nurses, dieticians, (hospital)pharmacists, and pharmacy technicians. The email included a brief description of the study and an URL link to a confidential web-based questionnaire, built into the program Survalyzer (Survalyzer, Zurich, Switzerland). A brief email reminder was sent after one week. This survey was performed in line with the principles of the Declaration of Helsinki for medical research involving human subjects. Healthcare professionals passively consented to participate by filling in the survey.
Survey and analysis
The survey (Appendix 1) was based on information from the literature6–9 and some preliminary informal interviews with various healthcare professionals involved in oncology (a specialized oncology nurse, a hematologist, and a pharmacist). Before dissemination, the survey was checked on content and language by a pharmacist from another institution and by a scientist in the biomedical field. The first section of the survey asked demographic questions. The CAM use in daily practice was surveyed in the second section of the questionnaire. The last section questioned the present state of CAM knowledge and professional opinions about CAM. Questionnaires, where only demographic data but no subsequent answers were given by the participant, were excluded from the study. Descriptive statistics were used to summarize the healthcare professionals’ characteristics and outcome variables. The data were analyzed with Excel (Microsoft Excel version 2016, Richmond, USA).
Results
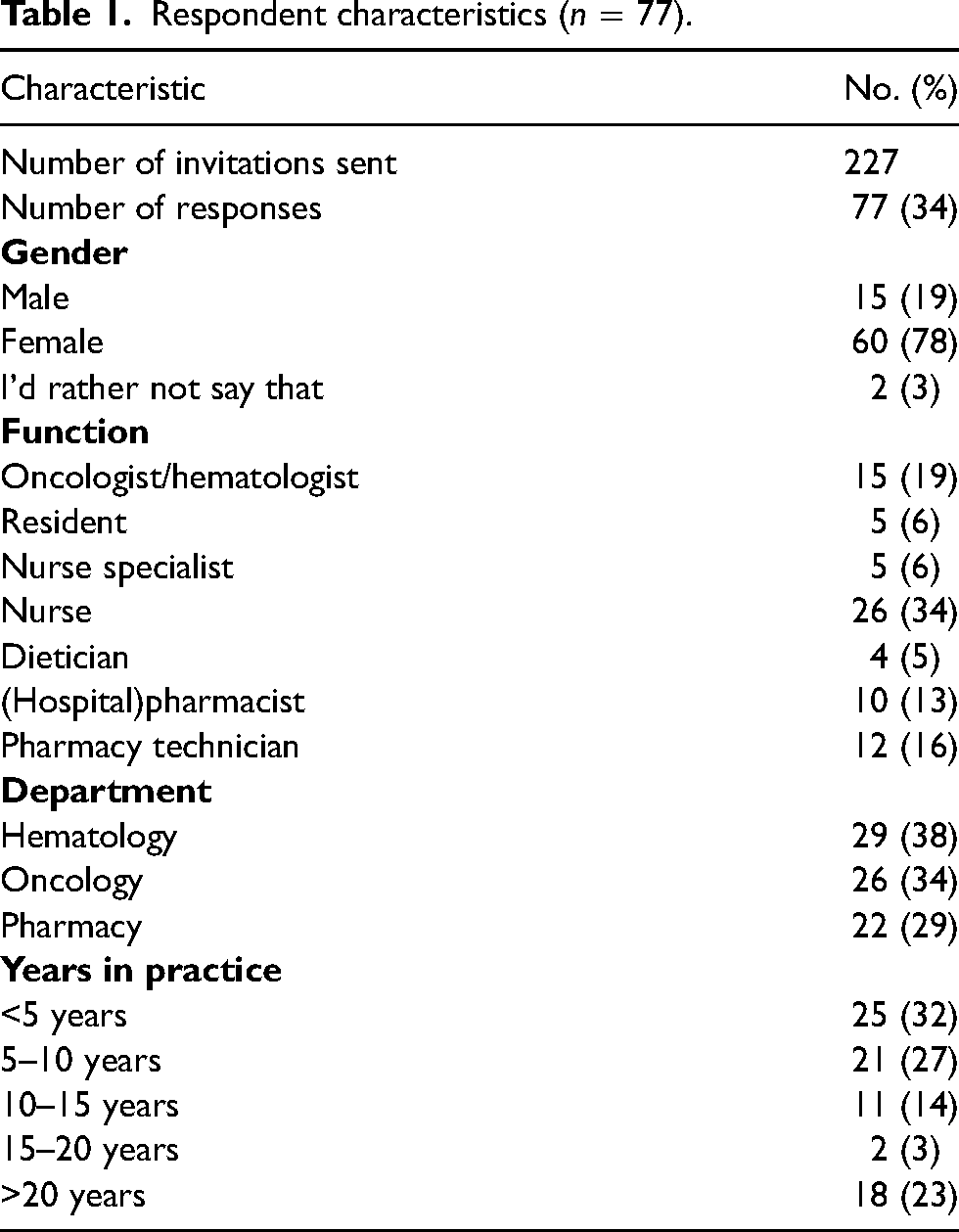
Two hundred twenty-seven emails were sent to healthcare professionals practicing in oncology and hematology at the Amsterdam UMC (VUmc). Seventy-seven healthcare professionals responded to the survey, yielding an overall response rate of 34%. Three participants completed only the demographic data. Their responses were not included in the study. Demographic data showed that of the 77 healthcare professionals that completed the study, 19% were men, and 78% of respondents were women, 32% of the respondents are healthcare professionals practicing <5 years (Table 1). Healthcare providers at the Amsterdam UMC do not often advise their patients to start using CAM (Figure 1). The vast majority of healthcare professionals (72%) advise <20% of patients to start using CAM. Many healthcare professionals also do not routinely ask their patients general questions about their use of CAM. If it comes up, patients are often advised to stop all CAM use. Overall nearly 50% of healthcare professionals bring up the patient's CAM use in less than half of the consultations and 60% of the oncologists and hematologists only ask about the patient's CAM use in 20% to 40% of the consultations. Conversely, just 16% of the other (non-doctor) healthcare professionals ask about the patient's CAM use in more than 80% of consultations. The data of the respondents who indicated that they do not speak/treat patients have been omitted in Figure 1. Additionally, a small number of patients mention their use of CAM on their own initiative during a consultation. The primary explanation given by healthcare professionals for this small number is that the patients do not see CAM as medication and do not believe it to be harmful. To the question “How many of the patients you speak to or treat use CAM?” More than 70% percent of the respondents indicated that this is <60% of patients.
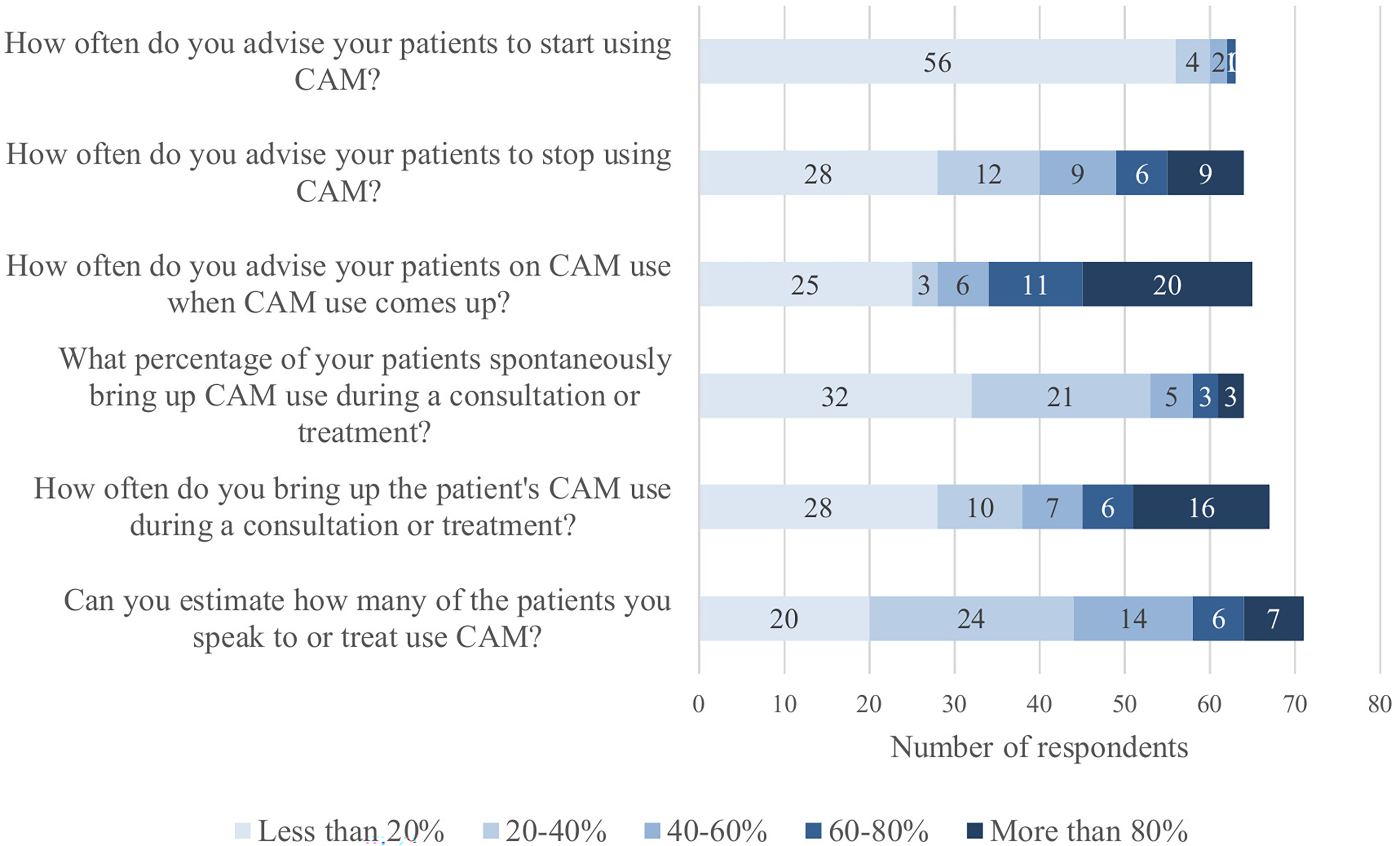
Healthcare professional opinion patterns toward complementary and alternative medicine (CAM) use by cancer patients. Number of responses per category. Participants who indicated “I don’t speak/treat patients” are not included in this figure.
Respondent characteristics (n = 77).
Strikingly, all healthcare professionals, including oncologists and hematologists, indicate that it is important (38%) or very important (49%) to know about the patient's use of CAM. Additionally, all healthcare professionals consider the possible interactions between CAM and oncolytic drugs important or very important, 35% and 65%, respectively.
For more in-depth analysis, the healthcare professionals were divided into three groups according to their field of expertise. Oncologists, hematologists, and residents make up the group of “physicians.” “Pharmacy” includes (hospital)pharmacists and pharmacy technicians, whereas physician assistants, specialized nurses, and non-specialized nurses are grouped as “nurse.” The last group consisted of dieticians. The majority of healthcare professionals say they do not know enough about CAM to appropriately and safely advise their patients. In comparison to the physicians, the pharmacy staff members score themselves to have a slightly greater knowledge of CAM (Table 2).
Response to the question: “I have enough knowledge of CAM to be able to answer questions from patients in a correct and safe manner.”

CAM: complementary and alternative medicine.
The healthcare professionals are divided into groups: physicians (oncologists, hematologists, and residents), nurses (specialized nurses and non-specialized nurses), dieticians, pharmacists, and pharmacy technicians.
Finally, the relevance of performing therapeutic drug monitoring on tyrosine kinase inhibitors (TKIs) when used concomitantly with CAM was surveyed by doctors and pharmacists. The majority of professionals recommended that the TKI levels should be monitored. Precisely, 39% of respondents even said this should be done with every adjustment in TKI and CAM doses.
Discussion
The high prevalence of CAM use among patients is often unknown to healthcare professionals. Even though all healthcare professionals believe it is important to be aware of their patients’ usage of CAM, they frequently do not talk about CAM with their patients. Precisely, 85% of healthcare professionals feel they do not know enough about CAM, which may be the reason why they do not always discuss CAM use in practice.
In a previous survey conducted in the United States, oncologists reported to have more knowledge about CAM (about one-third said they had sufficient knowledge) 7 than we found in our survey. Even higher percentages were reported from Italy, where almost 60% of oncologists feel they are well-informed about CAM. 8 But in another study, it was reported that 80% of the healthcare providers were unsure to advise on the benefits, limitations, and potential harms of CAM use in cancer-related situations, which is more consistent with our findings. 10 About half of the healthcare professionals surveyed in our study inquired about patients’ CAM use in <50% of the consultations. Remarkably, oncologists and hematologists ask even less about this, namely, 60% ask about this in only 20% to 40% of the consultations. According to Lee et al., 7 discussing CAM with the patient contributes to a better patient–physician relationship.
This study is the first to investigate the beliefs and attitudes toward CAM in a broad multiprofessional panel of healthcare providers that also includes dieticians (who often discuss food supplements with patients) and pharmacy technicians (who perform medication verification and reconciliation with patients). It is not without any limitations, though. The sample of healthcare professionals in this study does not represent all the healthcare professionals in the Netherlands, since this is a single-center study. In addition, the sample size is too small to allow for elaborate statistical analysis. Finally, there is a possibility that existing interest in CAM would increase the willingness to participate in this study, which could lead to selection bias. The length of the survey or types of questions, however, did probably not discourage respondents from participating, since only three respondents had incomplete responses. In our opinion, a larger follow-up study on this topic in the Netherlands and preferably also in a multinational setting is warranted. Comparisons between the various healthcare professions are feasible when the research groups are bigger. In addition, the uptake of advice from the different healthcare professionals on CAM by their patients is still an under-researched area of care.
Conclusion
Healthcare professionals are aware of the potential risks of CAM use in combination with anti-cancer treatment. However, CAM use is not yet discussed with every patient. This may be due to healthcare professionals’ lack of knowledge about CAM.
Footnotes
Acknowledgements
The authors would like to express their gratitude to all participating healthcare professionals.
Author contributions
All authors contributed to this study's conception and design. Data collection and analysis were performed by OS, MR, and MC. The manuscript was written by OS and was commented on by MR and MC. All authors read and approved the final manuscript.
Data availability
The dataset is available on reasonable request and based on the data use policy of Amsterdam UMC by sending an email message to the corresponding author.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work received regular institutional funding.
