Abstract
This study aimed to examine whether obstetric violence predicts traumatic childbirth perception among women. This cross-sectional study included 307 women who gave birth within the healthcare system. Data were collected via an online survey using validated scales. Findings showed moderate levels of traumatic childbirth perception, with obstetric violence significantly associated with higher perceptions of trauma. Marital status, psychological history, pregnancy planning, conception method, and prenatal education attendance also influenced perception. These factors together explained 25.8% of the variance. Promoting respectful maternity care and trauma-informed practices is crucial for improving maternal mental health outcomes.
Keywords
Introduction
Childbirth is one of the most significant and transformative experiences in a woman's life, encompassing complex physical, emotional, and psychological dimensions. While it can be a positive and empowering event, it also has the potential to be traumatic, leading to lasting psychological effects (Aksu & Serçekuş, 2023; Altuntuğ et al., 2024; Rousseau et al., 2022; Simpson & Catling, 2016). The perception of childbirth as traumatic refers to a woman's subjective interpretation of the birthing experience, which can occur at any stage of labor and is often linked to the threat of injury or death to herself or her baby (Yazıcı Topçu & Aktaş, 2022). The reported incidence of traumatic childbirth varies significantly across populations, ranging from 5% to 68.6% (Barut & Uçar, 2023; Türkmen et al., 2020). Traumatic childbirth perception is strongly associated with maternal mental health outcomes, including postpartum depression, anxiety, and stress (Türkmen et al., 2021). Additionally, posttraumatic stress disorder (PTSD) following traumatic childbirth affects approximately 2%–8.5% of mothers (Bingol & Bal, 2020).
Several factors contribute to traumatic childbirth perception, including unexpected medical interventions, complications during labor, loss of autonomy, and insufficient emotional or physical support from healthcare providers (Aksu & Serçekuş, 2023; Annborn & Finnbogadóttir, 2022). Obstetric violence refers to the mistreatment, disrespect, and abuse women may encounter in healthcare settings during pregnancy, childbirth, and the postpartum period (Castro & Frías, 2020). This form of violence encompasses a wide range of behaviors, including non-consensual medical procedures, verbal abuse, neglect, and the denial of autonomy in decision-making processes. Obstetric violence not only undermines women's rights but also has profound implications for their psychological well-being, contributing to feelings of helplessness, fear, and trauma during and after childbirth (Çetin et al., 2024; Fors et al., 2024). Obstetric violence is recognized globally as both a public health and human rights issue. Studies conducted worldwide have shown that women in both high-income and low- and middle-income countries encounter various forms of obstetric violence during childbirth. Cultural norms, healthcare systems, and societal expectations surrounding women's roles in childbirth are critical factors that shape women's experiences and their likelihood of encountering obstetric violence (Çetin et al., 2024; Frías & Castro, 2024; Martinez-Vázquez et al., 2022).
The psychological effects of obstetric violence can be examined through various theoretical frameworks that explain trauma responses. One such framework is the Shattered Assumptions Theory (Janoff-Bulman, 1992), which posits that individuals hold fundamental beliefs about the world being a safe place, trustworthy people, and having control over their lives. Traumatic events, such as obstetric violence, can profoundly disrupt these core assumptions, leading to significant psychological distress. In other words, obstetric violence could be a predictor of the perception of childbirth as trauma, as it challenges an individual's fundamental assumptions about safety, trust, and control over their own body. Women who experience mistreatment during childbirth may lose confidence in healthcare systems and professionals. According to the Shattered Assumptions Theory, this violation of autonomy and trust not only disrupts their belief in a just and predictable world but may also intensify the perception of childbirth as a traumatic event (Janoff-Bulman, 1992). Recent evidence from systematic reviews, meta-analyses, and meta-synthesis studies indicates that obstetric violence is a widespread and systemic issue embedded within sociocultural norms and healthcare structures, affecting women's autonomy, dignity, and emotional well-being across diverse birth settings (Hakimi et al., 2025; Küçük & Yeşilçiçek Çalik, 2025; Li et al., 2025). However, the role of obstetric violence as a strong predictor of traumatic childbirth perception has not been extensively studied at the international level. Addressing this gap is essential for developing effective interventions to ensure respectful and supportive care for women during childbirth.
Research Questions
This study aims to examine the impact of obstetric violence experienced during women's most recent childbirth on their perception of childbirth as traumatic and to identify the sociodemographic and obstetric factors associated with this perception. By focusing on women's most recent birth experiences, the study seeks to provide a clearer understanding of how obstetric mistreatment influences birth trauma perception. The research questions guiding this study are as follows:
What are the levels of traumatic childbirth perception among women? What sociodemographic and obstetric factors are associated with traumatic childbirth perception? What is the relationship between obstetric violence and traumatic childbirth perception? To what extent does obstetric violence predict traumatic childbirth perception?
Methods
Design
This study employed a descriptive cross-sectional design using an online survey and snowball sampling method. The study was structured and reported according to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) checklist for cross-sectional studies.
Settings and Participants
The participants were Turkish women who met the following inclusion criteria: being between 18 and 65 years old, having experienced at least one live birth within the Turkish healthcare system, being literate, having Turkish as their native language, having no current physician-diagnosed neuropsychiatric disorder, having internet access, and participating voluntarily. The exclusion criterion for this study was incomplete responses to the data collection tools. Data were collected between August and September 2024 from women who met the inclusion criteria. A purposeful snowball sampling method was employed to recruit participants. The initial participants were selected from the researcher's personal and professional networks and were encouraged to share the survey link within their social circles to broaden the participant pool. The required sample size was determined using G*Power 3.1.9.7 software (Franz Faul, Universität Kiel, Germany). For multiple regression analysis with 18 predictors (17 descriptive variables and one independent variable), assuming a small-to-moderate effect size (0.09), a power level of 80%, and a significance level of 0.05, the required sample size was calculated to be 239 participants (Faul et al., 2007). To account for a potential 15% dropout rate, it was estimated that approximately 275 participants would be needed to maintain the required sample size. A total of 328 participants completed the survey and were assessed for eligibility. Of these, 21 were excluded for not meeting the inclusion criteria, resulting in a final sample of 307 women who completed the study. Data were collected using a structured questionnaire via Google Forms, and participants were invited to complete the survey through social media platforms, including Facebook, WhatsApp, Instagram, and LinkedIn.
Instruments
Semi-Structured Data Collection Form
The researchers developed a data collection form that included 17 questions about participants’ age, marital status, education level, employment status, perceived income level, history of abuse, history of psychological disorder (defined as a past physician-diagnosed depressive or anxiety disorder that was not active at the time of data collection), number of pregnancies, planning status of the last pregnancy, time since previous delivery, mode of conception, attendance at prenatal preparation courses during the last pregnancy, type of facility where childbirth took place, mode of delivery, newborn's sex, presence of newborn health problems, and perceived support during childbirth.
Obstetric Violence Scale
This scale was developed by Castro and Frías (2020) to assess violence potentially associated with women's childbirth experiences (Castro & Frías, 2020). The Turkish validity and reliability study of the scale was conducted by Kömürcü Akik in 2023. The scale consists of 11 items scored as Yes = 1 and No = 0. Higher scores indicate a greater level of obstetric violence, with total scores ranging from 0 to 11. A score of 0 means no experience of obstetric violence, while higher scores reflect increased levels of violence (Kömürcü Akik, 2023). The original study reported a Cronbach's alpha of 0.73; the Turkish version showed a Cronbach's alpha of 0.72; in the current study, the Cronbach's alpha coefficient was found to be 0.71.
Traumatic Childbirth Perception Scale
This scale was developed by Yalnız et al. in 2016 to assess the perception of traumatic childbirth. It consists of 13 items scored between 0 and 10, with total scores ranging from 0 to 130. Higher scores indicate a higher level of traumatic childbirth perception. The total scale score of 0–26 points indicates very low, 27–52 points low, 53–78 points medium, 79–104 points high, and 105–130 points very high perception of traumatic birth (Yalnız et al., 2016). The original study reported a Cronbach's alpha of 0.90. In the current study, the Cronbach's alpha coefficient was found to be 0.92.
Data Collection
Written permission for the study was obtained from the relevant ethics committee prior to data collection. The data were collected using an online survey form created via Google Forms, a secure online survey platform. Following ethical approval, the survey link was distributed through various social media platforms, including Facebook, WhatsApp, Twitter, Instagram, and LinkedIn. Participants were invited to complete the survey through these platforms and were encouraged to share the survey link within their social circles to facilitate wider dissemination. The initial participants were selected from the researcher's personal and professional networks. Participants could view the research questions only after reading and agreeing to the Informed Consent Form on the questionnaire's first page. The informed consent form outlined the purpose of the research, the confidentiality of the collected information and its use exclusively for scientific purposes, the importance of answering the questions honestly, and the participant's right to withdraw from the study at any time without any consequences. Participants agreed: “I have read the information and voluntarily agree to participate in this study.” After providing consent, participants completed the survey by responding to the provided questions and submitting their answers via Google Forms. The survey submission was finalized by clicking the submit button. The completion of the survey took approximately 15–20 min.
Ethical Considerations
The official ethical approval for this study was obtained from the Hacettepe University Faculty of Nursing Research Ethics Committee in Ankara (No. E-51986023-605-00003651582, Decision No: HAE 24/1). The ethical guidelines of the Ethics Working Committee of the Association of Internet Researchers (AoIR) were followed when researching the Internet. The informed consent form, presented on the first page of the online survey, provided detailed information about the study, including its purpose, the confidentiality of the collected data, and the voluntary nature of participation. Participants were required to give prior informed consent by selecting the confirmation statement: “I have read the information and voluntarily agree to participate in this study.” Those who did not provide consent were unable to access the survey questions. Participants were assured of their right to withdraw from the study at any time without any consequences and of the confidentiality and anonymity of their responses. The collected data were used solely for academic purposes. The researchers declare no conflicts of interest or financial benefits related to this study.
Data Analysis
Data were analyzed using SPSS version 23.0 software. Descriptive statistics, including frequency, percentage, mean, and standard deviation, were used to summarize the sociodemographic and obstetric characteristics of the participants. The scores from the Obstetric Violence Scale and the Traumatic Childbirth Perception Scale were reported using mean, standard deviation, and minimum–maximum values. The normality assumption was assessed through skewness and kurtosis values, which ranged between −1.5 and +1.5, indicating a normal distribution. In descriptive statistics, mean and standard deviation were used to present numerical variables with normal distribution.
In contrast, categorical variables (e.g., marital status, education level, employment status, perceived income level, history of abuse, history of psychological disorder, mode of conception, and perceived support during childbirth) were summarized using frequency and percentage values. Independent t-tests and one-way analysis of variance (ANOVA) were performed to compare Traumatic Childbirth Perception Scale scores across different sociodemographic and obstetric groups. Pearson correlation coefficients were used to assess relationships between obstetric violence and traumatic childbirth perception. In univariate analysis, predictors were selected based on statistically significant relationships with the dependent variable (p < .05). Multicollinearity among independent variables was evaluated before conducting regression analysis. The variance inflation factor (VIF) values ranged from 1.016 to 1.094, below the threshold of 10, and tolerance values ranged from 0.914 to 0.985, indicating no multicollinearity issues. The Durbin–Watson statistic was 1.885, indicating no autocorrelation in the regression model (acceptable range: 1.5–2.5) (Hair et al., 2010). Hierarchical linear regression analysis was conducted to examine the predictive effects of obstetric violence and other significant variables on traumatic childbirth perception. All statistical analyses were two-tailed, and a significance level of p < .05 was considered statistically significant.
Results
Table 1 presents the descriptive characteristics of the participants. The mean age of the participants was 36.66 ± 6.25 years. The majority were married (88.9%) and had an undergraduate degree or higher (69.7%). Most participants were multiparous (65.5%). Among delivery modes, the most common was a planned cesarean section (41.7%), followed by vaginal and emergency cesarean births. Detailed sociodemographic and obstetric characteristics are provided in Table 1. Following the descriptive characteristics, the mean Total Traumatic Childbirth Perception Scale score was 60.50 ± 32.44 (range: 0–130), and the mean Total Obstetric Violence Questionnaire score was 0.79 ± 1.38 (range: 0–7).
Demographic Characteristics.
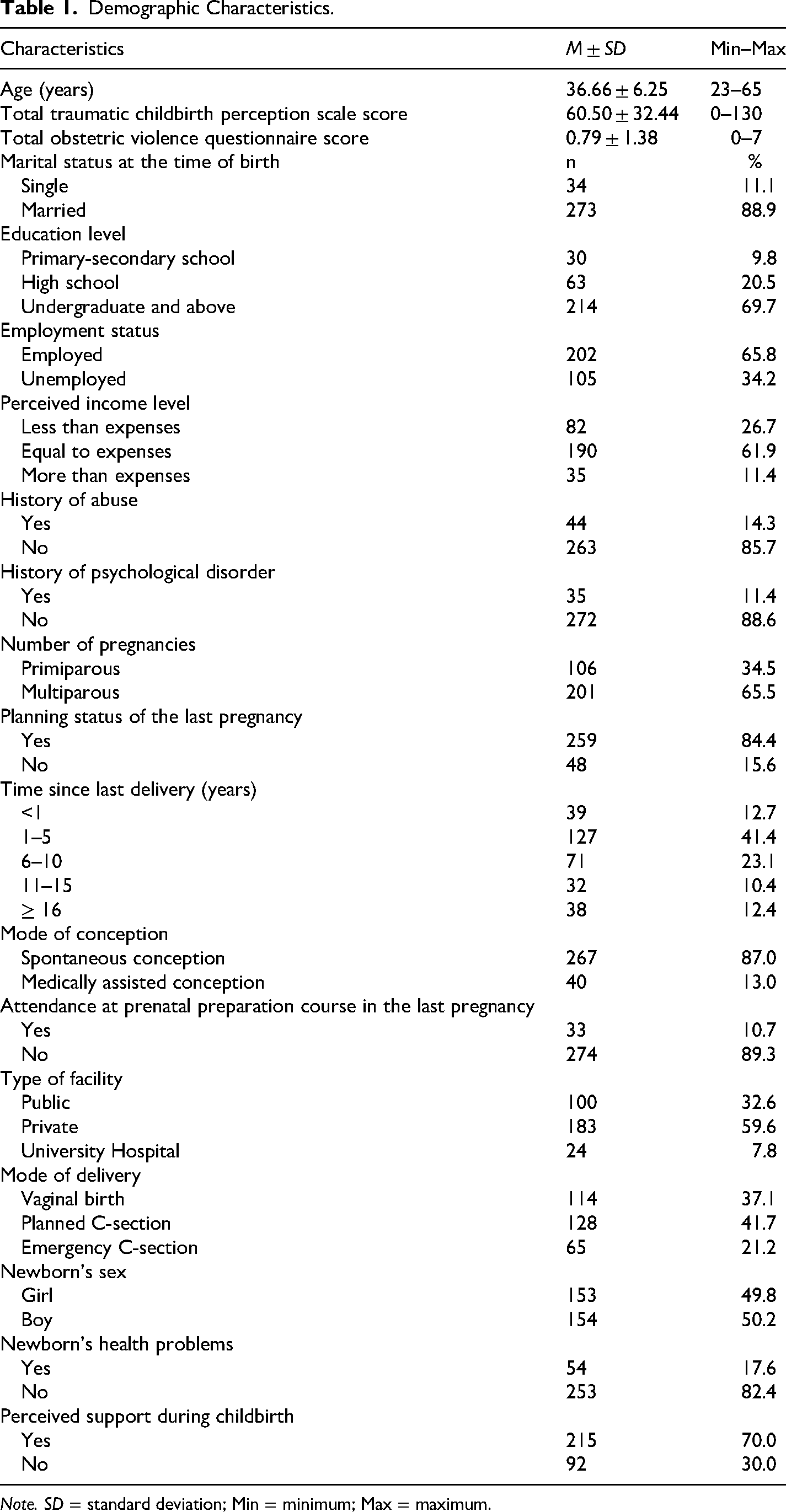

Note. SD = standard deviation; Min = minimum; Max = maximum.
Table 2 presents the findings of the univariate analysis of the Traumatic Childbirth Perception Scale. A statistically significant difference was found in traumatic childbirth perception scores based on marital status, perceived income level, history of psychological disorder, planning status of the last pregnancy, mode of conception, attendance at prenatal preparation courses, and perceived support during childbirth. Higher traumatic childbirth perception scores were reported among single participants (t = 2.957; p = .003), those with income less than expenses (F = 5.596; p = .004), participants with a history of psychological disorder (t = 3.304; p = .001), and those whose last pregnancy was unplanned (t = −5.792; p < .001). Additionally, those who conceived spontaneously had significantly higher scores than those who underwent medically assisted conception (t = 4.214; p < .001), while those who did not attend a prenatal preparation course had higher traumatic childbirth perception scores (t = −2.759; p = .006). Moreover, participants who did not perceive support during childbirth had significantly higher traumatic childbirth perception scores (t = −2.340; p = .020).
Univariate Analysis of the Traumatic Childbirth Perception Scale.
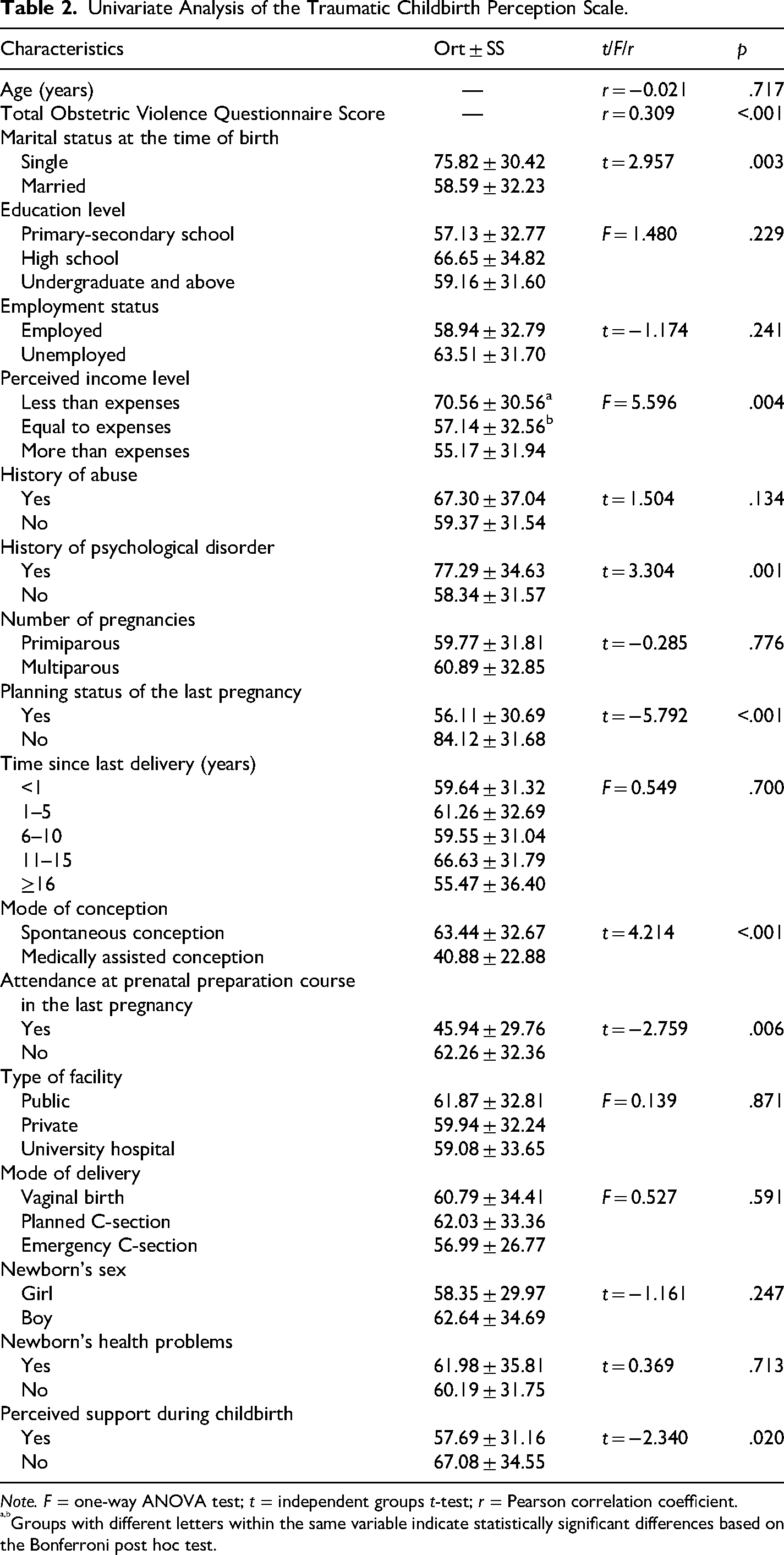
Note. F = one-way ANOVA test; t = independent groups t-test; r = Pearson correlation coefficient.
Groups with different letters within the same variable indicate statistically significant differences based on the Bonferroni post hoc test.
Table 3 presents the results of the hierarchical linear regression analysis that was conducted to determine the predictors of traumatic childbirth perception. The regression model included variables significantly associated with traumatic childbirth perception. In Model 1, marital status, perceived income level, history of psychological disorder, planning status of the last pregnancy, mode of conception, attendance at a prenatal preparation course, and perceived support during childbirth were included. Model 1 was statistically significant (F = 11.215; p < .001) and explained 20.8% of the variance in traumatic childbirth perception. Statistically significant predictors in this model included marital status (β = 0.119; p = .023), history of psychological disorder (β = 0.140; p = .008), planning status of the last pregnancy (β = 0.265; p < .001), mode of conception (β = 0.209; p < .001), and attendance at a prenatal preparation course (β = 0.116; p = .027). In Model 2, obstetric violence was added to the model. This model remained statistically significant (F = 12.969; p < .001) and explained 25.8% of the variance in traumatic childbirth perception. Significant predictors in this model included marital status (β = 0.106; p = .037), history of psychological disorder (β = 0.138; p = .007), planning status of the last pregnancy (β = 0.232; p < .001), mode of conception (β = 0.197; p < .001), attendance at a prenatal preparation course (β = 0.114; p = .024), and obstetric violence (β = 0.233; p < .001).
Hierarchical Linear Regression Analysis of Predictors of Traumatic Childbirth Perception.
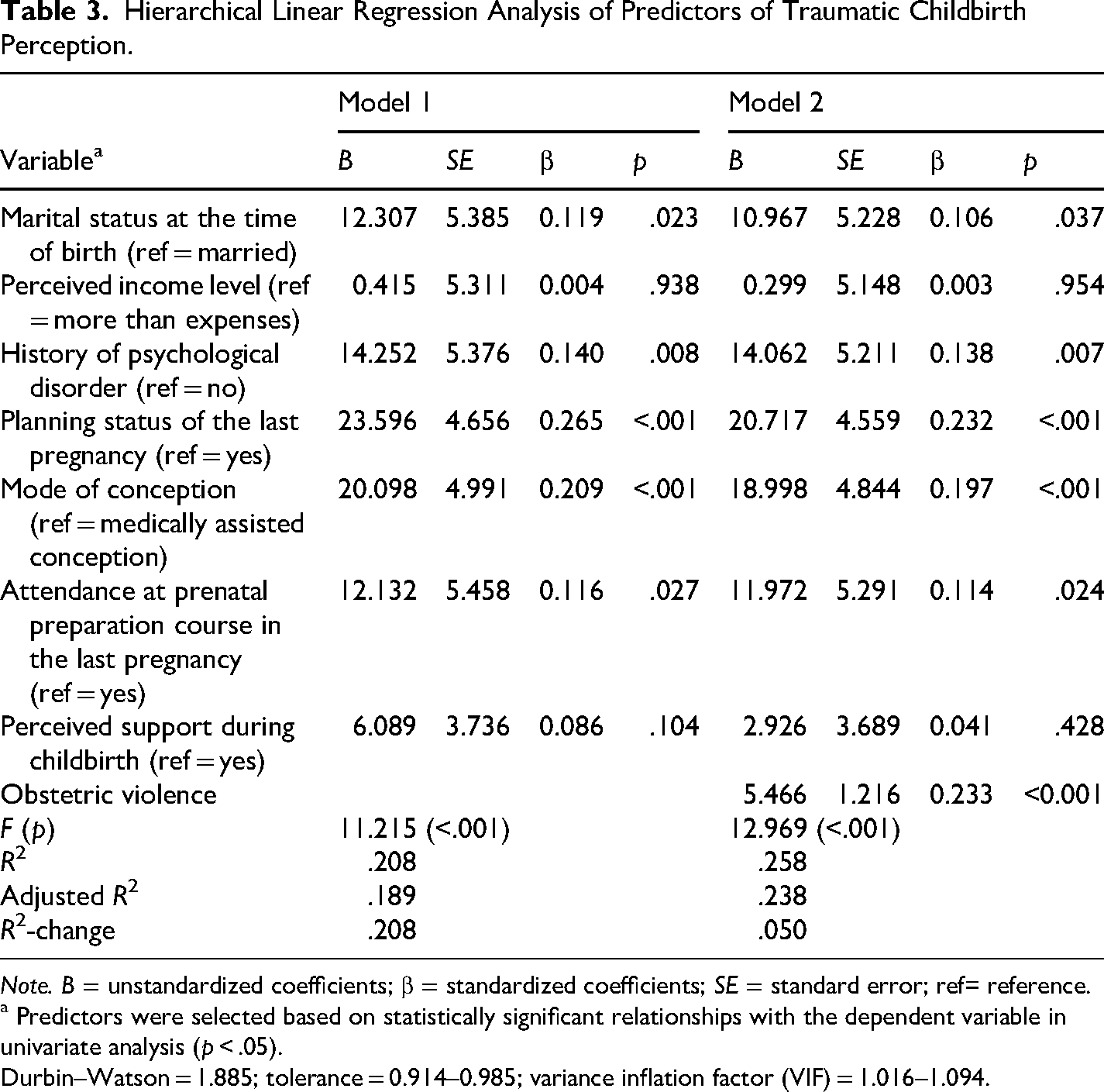
Note. B = unstandardized coefficients; β = standardized coefficients; SE = standard error; ref= reference.
a Predictors were selected based on statistically significant relationships with the dependent variable in univariate analysis (p < .05).
Durbin–Watson = 1.885; tolerance = 0.914–0.985; variance inflation factor (VIF) = 1.016–1.094.
Discussion
This study examined the impact of obstetric violence during women's most recent childbirth on their perception of childbirth as traumatic. It explored the sociodemographic and obstetric factors associated with this perception. The findings indicate that obstetric violence is a key determinant of traumatic childbirth experiences, highlighting the lasting psychological impact of mistreatment during labor and delivery. Additionally, both sociodemographic factors—such as marital status at the time of birth, perceived income level, and history of psychological disorder—and obstetric factors, including the planning status of the last pregnancy, mode of conception, attendance at prenatal preparation courses, and perceived support during childbirth, were found to influence birth trauma perception significantly. These results suggest that birth-related distress is shaped not only by medical interventions but also by broader social and psychological contexts surrounding childbirth.
The findings of this study indicate that the total Traumatic Childbirth Perception Scale (TCPS) score was 60.50 ± 32.44, corresponding to a moderate perception of traumatic childbirth based on the scale classification (53–78 points). This result suggests that while some participants reported relatively low trauma perceptions, a considerable proportion experienced childbirth as a moderately traumatic event. Altuntuğ et al. (2024) reported a higher mean TCPS score of 74.3 ± 27.7, indicating a moderate-to-high level of perceived trauma among postpartum women (Altuntuğ et al., 2024). Similarly, the study by Yazıcı Topçu and Aktaş (2022) found a mean TCPS score of 70.49 ± 17.43, also suggesting a moderate-to-high perception of traumatic childbirth (Yazıcı Topçu & Aktaş, 2022). The differences in mean scores between studies may be attributed to sample characteristics, healthcare settings, and contextual factors, including the level of obstetric support and interventions during childbirth.
Marital status was a significant predictor of traumatic birth perception, with single women reporting higher trauma scores. However, being married did not necessarily protect against birth trauma, as many married women still felt unsupported. This highlights that the quality of support, rather than marital status alone, plays a crucial role in shaping childbirth experiences. Prior research suggests that partner presence does not reduce birth trauma unless accompanied by meaningful emotional and practical support (Chen et al., 2022). Some single women may have benefited from alternative support sources, such as family or healthcare providers, mitigating their risk. Although perceived social support was associated with birth trauma in initial analyses, it was not a significant predictor in the hierarchical regression model. This suggests that its impact may be indirect, potentially moderating the effects of obstetric violence or psychological distress. Additionally, stronger predictors such as pregnancy planning and mode of conception may have overshadowed its direct effect. These findings emphasize the need to strengthen not only partner involvement but also broader support networks, including healthcare providers and family members, to reduce birth trauma risk.
Perceived income level was associated with traumatic childbirth perception in our study, with lower perceived income linked to higher traumatic perception scores. However, in the hierarchical regression analysis, it was not a significant predictor in Model 1. This may be due to the presence of stronger predictors in the model, such as pregnancy planning status and mode of conception, which might have overshadowed the independent effect of perceived income. Previous studies suggest that financial difficulties can exacerbate childbirth-related distress, notably by limiting access to healthcare resources and increasing stress levels (Çankaya & Ocaktan, 2022). Although perceived income did not independently predict traumatic childbirth perception in our model, its indirect effects should not be overlooked. Future research should investigate potential pathways through which financial constraints contribute to childbirth experiences, such as healthcare accessibility and psychological well-being.
The history of psychological disorders was another significant factor associated with the perception of traumatic childbirth. A review highlighted that women with previous depression or other psychological problems may be more likely to perceive their birth as traumatic (Simpson & Catling, 2016). One possible explanation for this heightened risk is that women with a history of depression may interpret their surroundings and childbirth experiences as more distressing and threatening due to cognitive biases (Urban et al., 2018). Furthermore, prior depression may reduce psychological resilience, making women more susceptible to the emotional impact of unexpected or uncontrollable birth complications. This may contribute to more negative evaluations of their birth experience (Nagle et al., 2022).
In addition to these sociodemographic factors, the planning status of the last pregnancy played a crucial role in traumatic childbirth perception. Women whose pregnancies were unplanned reported significantly higher levels of traumatic perception. Supporting this finding, a study by Yalnız Dilcen et al. also demonstrated that women with unplanned pregnancies perceived childbirth as significantly more traumatic compared to those with planned pregnancies. These results highlight the potential psychological burden of unplanned pregnancies and their association with an increased perception of birth trauma (Yalnız Dilcen et al., 2021). The lack of psychological readiness may intensify feelings of distress, leading to a heightened perception of childbirth as traumatic.
The mode of conception influenced traumatic childbirth perception in our study. Women who conceived spontaneously reported higher levels of traumatic perception, possibly due to lower medical supervision and psychological preparation. However, Wang et al. (2025) found that birth trauma scores were slightly higher in assisted conception, though the difference was not significant (Wang et al., 2025). This suggests that while assisted reproductive technologies offer support, they may not entirely prevent traumatic birth experiences. These findings may be influenced by uncertainty and unpredictability in spontaneous conception, leading to increased stress and loss of control.
In contrast, assisted conception involves more medical oversight, which may enhance preparedness. However, the emotional and physical demands of fertility treatments, along with heightened expectations, could contribute to trauma perception. Further research is needed to explore these dynamics. In addition to conception mode, prenatal preparation also played a crucial role in shaping traumatic childbirth perception. Women who did not attend such courses reported higher traumatic childbirth perception scores. Prenatal preparation programs provide valuable information about the childbirth process, pain management techniques, and coping strategies, all enhancing a woman's sense of control and reducing fear during labor (Gagnon & Sandall, 2007). The lack of such preparation may leave women feeling unprepared and vulnerable, increasing the possibility of perceiving childbirth as traumatic. Supporting this, Yalnız Dilcen et al. found that women with lower birth knowledge had significantly higher traumatic childbirth perception scores (Yalnız Dilcen et al., 2021). Similarly, İnan Kırmızıgül et al. reported that women who did not attend a pregnancy school had higher traumatic birth perception scores, although the difference was not statistically significant (İnan Kırmızıgül et al., 2025). Additionally, Çankaya and Ocaktan (2022) observed that receiving education on birth preparation and delivery methods during pregnancy was linked to lower traumatic birth perception scores. However, this relationship was not statistically significant (Çankaya & Ocaktan, 2022). These findings highlight the importance of prenatal education in reducing childbirth-related trauma by increasing knowledge and preparedness.
Although sociodemographic and obstetric factors are important in understanding traumatic childbirth perception, the overlooked yet substantial impact of obstetric violence deserves particular attention. In our study, obstetric violence was significantly correlated with traumatic childbirth perception, highlighting its impact on birth experiences. Consistently, higher levels of obstetric violence were significantly associated with increased traumatic childbirth perception. In addition, the hierarchical regression analysis demonstrated that obstetric violence remains a significant predictor of traumatic childbirth perception even after controlling for other variables. When obstetric violence was included in the model, it increased the explained variance in traumatic childbirth perception from 20.8% to 25.8%. This finding aligns with existing literature indicating that mistreatment and abuse during childbirth can have profound psychological consequences (Annborn & Finnbogadóttir, 2022; Avcı & Kaydırak, 2023; Çetin et al., 2024; Martinez-Vázquez et al., 2022). Obstetric violence, including non-consensual medical interventions, verbal abuse, and neglect, can disrupt a woman's sense of autonomy and safety, leading to feelings of helplessness and fear. According to the Shattered Assumptions Theory (Janoff-Bulman, 1992), such traumatic events can fundamentally alter core beliefs about the world being a safe place and healthcare providers being trustworthy, contributing to the development of trauma-related symptoms. This underscores the critical need for healthcare systems to address obstetric violence and promote respectful maternity care practices. Training healthcare professionals to provide patient-centered care, ensuring informed consent, and fostering supportive environments during childbirth are essential strategies to reduce the incidence of traumatic birth experiences.
Strengths and Limitations
A key strength of this study is its focus on obstetric violence, a relatively underexplored factor in the context of traumatic childbirth perception, particularly in middle-income countries like Turkey. Using validated scales and a robust sample size enhances the reliability of the findings. Additionally, applying the Shattered Assumptions Theory provides a strong theoretical framework to understand the psychological mechanisms underlying traumatic birth experiences. However, the study has several limitations. The cross-sectional design prevents causal inferences, and the reliance on self-reported data may introduce recall bias. Furthermore, because the time elapsed since participants’ most recent childbirth varied, the findings may be influenced by differences in memory recall. Using an online survey and snowball sampling method could result in selection bias, potentially limiting the generalizability of the findings to the broader population of women. Furthermore, cultural factors specific to Turkey may influence the findings, and comparisons with other countries should be made cautiously.
Implications for Practice and Future Research
The findings of this study have important implications for clinical practice and public health policy. Addressing obstetric violence through healthcare provider training, policy reforms, and patient advocacy is crucial to improving maternal health outcomes. Incorporating trauma-informed care practices into maternity services can help create safer and more supportive environments for women during childbirth. Future research should explore longitudinal designs to establish causal relationships between obstetric violence and traumatic childbirth perception. Comparative studies across different cultural and healthcare contexts would provide valuable insights into the global prevalence and impact of obstetric violence. Additionally, qualitative research exploring women's narratives can deepen our understanding of the nuanced ways in which obstetric violence affects childbirth experiences.
Conclusion
This study highlights the significant impact of obstetric violence on the perception of childbirth as traumatic, emphasizing the need to address mistreatment during labor and delivery. While sociodemographic and obstetric factors also contribute to birth trauma perception, obstetric violence emerged as a particularly influential factor, increasing the explained variance in traumatic childbirth perception. These findings underscore the urgent need for healthcare systems to implement respectful, supportive, and individualized maternity care practices, strengthen informed consent processes, and train healthcare professionals to adopt patient-centered approaches. Reducing obstetric violence is essential not only for improving childbirth experiences but also for safeguarding maternal mental health.
Footnotes
Acknowledgments
We would like to thank all participants for their cooperation and contribution to this study.
Ethical Considerations
The official ethical approval for this study was obtained from the University Faculty of Nursing Research Ethics Committee in Ankara (No. E-51986023-605-00003651582, Decision No: HAE 24/1). Written informed consent was obtained from the nursing students. The study was conducted according to the Declaration of Helsinki (1964) and later amendments.
Consent to Participate
All participants provided informed consent prior to their inclusion in the study.
Consent for Publication
Participants consented to the publication of anonymized data.
Author Contributions
Merve Mert-Karadas: conceptualization, data curation, formal analysis, investigation, methodology, project administration, resources, supervision, visualization, writing—original draft, and writing—review and editing. Cansu Akdag Topal: conceptualization, data curation, formal analysis, investigation, methodology, supervision, visualization, writing—original draft, and writing—review and editing. Fatma Uslu-Sahan: conceptualization, data curation, investigation, methodology, supervision, writing—original draft, and writing—review and editing. Sevda Yildirim: conceptualization, data curation, investigation, methodology, supervision, writing—original draft, and writing—review and editing.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request. Due to privacy and ethical restrictions, the data are not publicly available as they contain information that could compromise the confidentiality and anonymity of research participants. All data have been stored securely and will be permanently deleted 5 years after the conclusion of the study.
