Abstract
The aim of the present study was to explore ophthalmologists’ attitudes, knowledge, and willingness to report child abuse. One-hundred-and-seven ophthalmologists employed in various hospitals in Israel completed an online questionnaire. Less than half the ophthalmologists (44.9%) reported that they had treated children whom they identified or suspected as being victims of child abuse, while only 43.9% of these reported child abuse. Despite generally positive attitudes towards reporting of child abuse among the ophthalmologists, their average level of knowledge was low. Ophthalmologists who had received training on child abuse and residents displayed a higher level of knowledge. In addition, female ophthalmologists tended to agree more that ophthalmologists are obligated to screen for and report child abuse. Moreover, female ophthalmologists expressed higher willingness to report child abuse. The present study reveals that underreporting of child abuse, and more precisely the discrepancy between identification and reporting, is present among ophthalmologists. It seems that lack of knowledge regarding identification and reporting of child abuse is the main barrier to reporting, especially among medical specialists. These findings underscore the importance of training programs on child abuse, both during formal education in medical school, and post-qualification, for all ophthalmologists, irrespective of seniority.
Introduction
Child abuse is a major worldwide health problem jeopardizing the mental and physical health of children (Viola et al., 2016). In the U.S., which is among the countries with the highest rates of child abuse, 3.5 million child abuse cases were investigated in 2019 by child protective services, while an estimated 1840 children died due to abuse or neglect (Child Welfare Information Gateway, 2021). Most of these early deaths are attributed to abusive head trauma (AHT). Eye injury due to abuse can appear in any part of the eye. However, retinal hemorrhage, present in approximately 75% of children who are victims of AHT, is the most common manifestation (Binenbaum et al., 2009).
It is acknowledged that healthcare professionals are well positioned to identify child maltreatment (Curry et al., 2018). In their daily practice, ophthalmologists may encounter children who are victims of abuse. Ophthalmologists are often consulted when there is a concern of AHT, as they are in a unique position to give a detailed clinical description of the patient’s hemorrhagic retinopathy (Christian & Levin, 2018). However, this and other ocular injuries suggestive of abusive trauma but requiring unique knowledge in ophthalmology, may also be revealed during a routine eye examination (Betts et al., 2017). Moreover, general warning signs, such as unusual parent-child interactions during medical appointments or parents' non-adherence to the ophthalmologist’s recommendations should arouse the ophthalmologist’s concern of child abuse (Curry et al., 2018).
Timely identification and reporting by a physician may prompt appropriate interventions capable of preventing negative consequences of the abuse (Lev-Wiesel et al., 2018). Despite the undisputed importance of identification and reporting of child abuse by physicians, it is also acknowledged that reported cases are only a small proportion of actual child abuse cases. Physicians often lack the necessary knowledge to identify child abuse, and one of the main reasons is a lack of formal training on this topic (Li et al., 2017; Sathiadas et al., 2018). Moreover, physicians often lack information regarding the appropriate official agencies for reporting cases of abuse. There is evidence that knowledge and adequate training of healthcare professionals on child abuse is associated with more frequent reporting behavior. It has also been found that those physicians who consider their competencies regarding child abuse to be inadequate, may be less likely to report child abuse (Moreira et al., 2014; Sonbol et al., 2012).
Of note, formal or informal training on child abuse is not included as a mandatory study topic in Israeli medical schools and in the ophthalmology specialty in particular. Moreover, differences have been observed between medical schools with regard to the content of the material taught (Ben Yehuda et al., 2010).
There is evidence that negative attitudes towards reporting child abuse are prevalent among physicians. Namely, those physicians who do suspect child abuse may be reluctant to report it due to lack of confidence to report in specific circumstances (Schols et al., 2013), confusion about whose responsibility it is to report (i.e., of the physician or the social worker) (Talsma et al., 2015), fear of offending the parents, discomfort related to addressing this sensitive issue, and concerns about the impact of intervention on the caregivers and/or themselves (Pietrantonio et al., 2013).
Notably, previous research results were inconclusive regarding the role of the physician’s gender in his/her attitudes and willingness to report. Thus, Alsaleem et al. (2019) found that gender was not associated with identification and reporting of child physical abuse. In contrast, in another study, male dentists were found to report more suspected cases of child abuse than female dentists (Sonbol et al., 2012). In addition, İnanici et al. (2020) identified a difference between male and female physicians in their attitudes towards reporting child abuse.
In some places, overseeing the reporting of child abuse and neglect by healthcare professionals are set by law (Betts et al., 2017; Curry et al., 2018). This is also the case in Israel, where the law obligates healthcare professionals to report suspected child abuse (Lev-Wiesel et al., 2018). According to this law, ophthalmologists are similarly obligated to report. Notably, in Israel consultation with an ophthalmologist does not require a referral from another healthcare professional and is covered by the basic health insurance. That is, identification of child abuse may be accidental.
Despite their unique potential role in the identification of child abuse, little is known regarding ophthalmologists' attitudes, knowledge, and willingness to report child abuse. Therefore, the aim of the present study was to explore ophthalmologists' attitudes, knowledge, and their willingness to report child abuse. In particular, this study explored whether and how attitude and knowledge were associated with willingness to report. In addition, ophthalmologists’ training experiences regarding child abuse and the role of their gender in their attitudes and willingness to report were also explored.
Materials & Methods
Research Design
This study is a quantitative correlational survey study.
Participants
A convenience sample of 107 ophthalmologists – ophthalmology specialists or residents – employed in a hospital in Israel, with at least 1 month of experience working with children, took part in the study. The mean age of the ophthalmologists was 44.77 years (SD = 11.23), with a range of 27–72. Women constituted 56.1% of the sample. Most were married (89.9%), and they had 2.0 children on average (SD = 2.3, range 0–6), while 19.6% had no children. Most of the ophthalmologists were Jewish (86.9%) and the rest were Muslim. Most defined themselves as secular (75.7%). The place of residence of most of the ophthalmologists was in Israel’s central district (69.2%).
Most of the ophthalmologists were specialists (63.6%), while the rest were residents (36.4%), with a mean of 14.20 years of experience (SD = 11.26, range 1–45). Most had completed their residence/fellowship in Israel (95.3%).
Research Instrument
Participants completed a questionnaire designed by Glasser and Chen (2006). The questionnaire was modified to suit the ophthalmology context and to present legal aspects of child abuse identification and reporting.
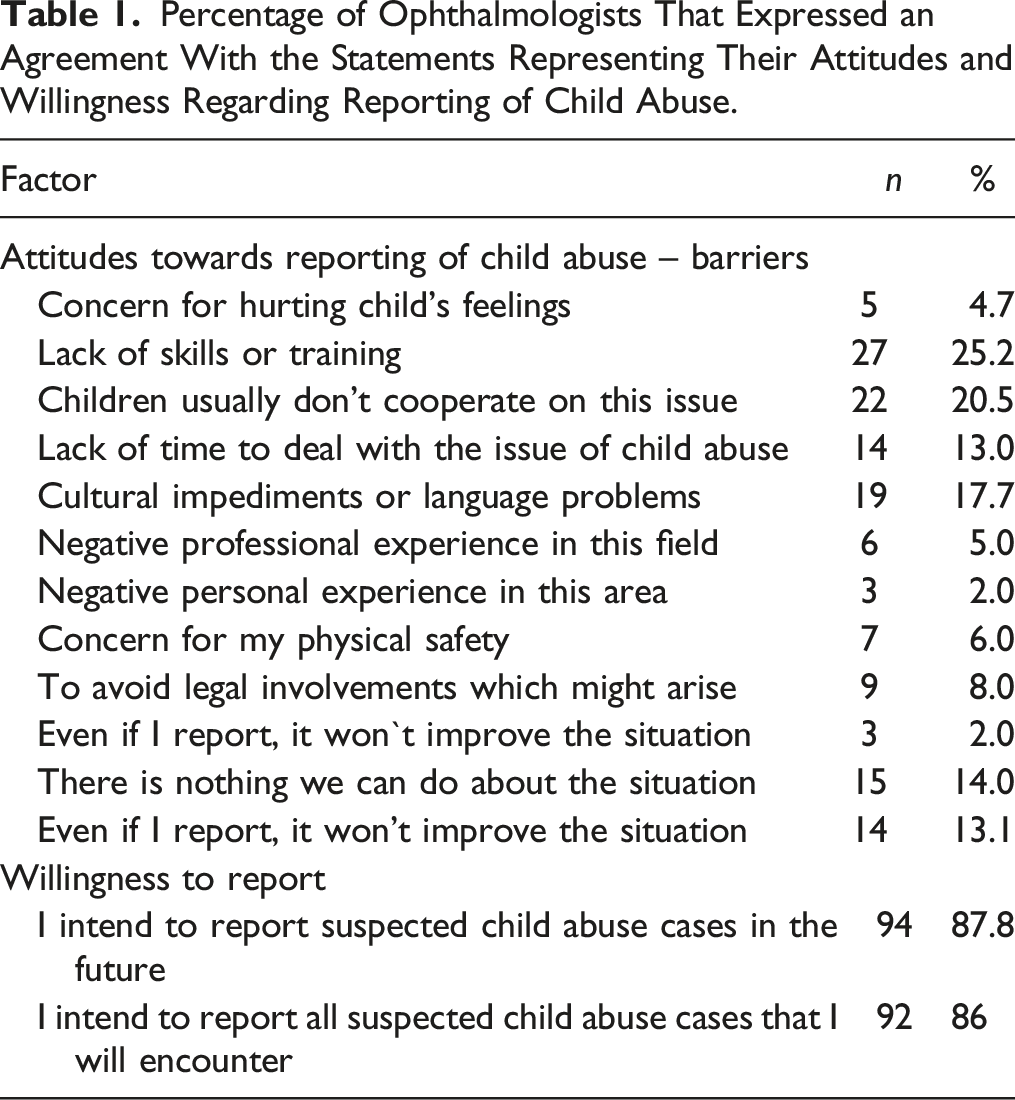
Percentage of Ophthalmologists That Expressed an Agreement With the Statements Representing Their Attitudes and Willingness Regarding Reporting of Child Abuse.
In addition, the questionnaire included three knowledge questions exploring basic knowledge regarding identification of child abuse by an ophthalmologist and the legal aspects of reporting the suspected child abuse (“What eye injury in children raises a concern of child abuse?”, “What is the legal penalty for an ophthalmologist who identifies a case of suspected child abuse but does not report it?”, and “According to the Israeli law, is an ophthalmologist obligated to report suspected child abuse to the authorities?”). The knowledge variable was calculated as a sum of the points, with a maximum score of three points (one point for each correct answer).
The internal reliability of the questionnaire’s parts in the present study ranged from 0.71 to 0.82. The questionnaire was translated into Hebrew using the back-and-forth translation method. It was reviewed by three content experts and found to be valid. The knowledge items were developed in consultation with ophthalmology experts to capture the essential aspects of knowledge related to identifying and reporting suspected child abuse cases in this medical profession.
Data Collection
The study was approved by the Helsinki Committee of the Barzilai Ashkelon University Medical Center. The questionnaire contained an introduction explaining the purpose of the study and data anonymity. Participants were aware of the future uses of their responses, including publication. The survey data were collected electronically. The researchers contacted the Israeli Ophthalmologists’ Association, which distributed the questionnaire via email to ophthalmologists in Israel. One-hundred-and-fifty email messages were sent to 150 ophthalmologists, constituting 20% of all ophthalmologists in Israel. One-hundred-and-seven completed questionnaires were obtained, for a response rate of 71.3%.
Statistical Analysis
Statistical analysis was performed using SPSS software for Windows, version 26 (SPSS, Chicago, IL, USA). Descriptive statistics – percentages, means, and standard deviations (SD) – were used to describe the research data. Pearson’s/Spearman’s correlations, Chi-square tests, and t-tests for independent samples were conducted to explore the associations between the research variables. In addition, a linear regression analysis was conducted to explore whether ophthalmologists' attitudes and knowledge predict their willingness to report. For all analyses, a level of significance of p < .05 was considered statistically significant.
Results
Less than half the ophthalmologists (44.9%) reported that they had treated children whom they identified or suspected as being victims of child abuse, with the mean number of suspected cases of child abuse reported being 3.31 (SD = 2.55, range 1–10). Of these, only 43.9% claimed that they had reported the suspected child abuse, where the mean number of reported cases was 2.33 (SD = 2.13, range 1–10).
Most of the ophthalmologists (89.7%) reported that they had not undergone a formal study course on child abuse. In addition, more than a quarter of the ophthalmologists (26%) reported not having the knowledge and experience necessary for identification and management of child abuse.
The ophthalmologists tended to express moderate attitudes towards reporting child abuse (M = 3.36, SD = 0.71). Namely, several barriers to reporting were evident. Thus, the most evident barriers were lack of skills or training, belief that children usually don’t cooperate on this issue, and cultural impediments or language problems, with approximately one fifth of the ophthalmologists expressing strong agreement that these barriers may prevent them from reporting child abuse (Table 1).
In addition, the ophthalmologists' mean level of knowledge was low (M = 1.42, SD = 0.77). Namely, 50% of the ophthalmologists knew that according to the Israeli law ophthalmologists are obligated to report suspected child abuse to the authorities. In addition, only 10.3% knew that a healthcare professional who fails to comply with this law can be sentenced to 6 months in prison. Moreover, only 28% of the ophthalmologists knew that retinal hemorrhage in a child should raise a concern of child abuse.
However, ophthalmologists who reported having undergone a formal course on child abuse were found to have a higher level of knowledge regarding its identification and management (M = 1.8, SD = 0.60) than ophthalmologists who had not undergone such training (M = 0.73, SD = 0.78) [t = −2.23 (14.20), p < .05]. Moreover, residents were found to have a higher level of knowledge regarding the identification and management of child abuse (M = 1.7, SD = 0.70) than specialists (M = 1.25, SD = 0.78) [t = −3.17 (105), p < .01].
In addition, two differences were found between female and male ophthalmologists. The first difference was in replies to one of the knowledge questions. Namely, more female ophthalmologists than male ophthalmologists knew that an ophthalmologist is obligated to report suspected child abuse to the authorities (66.7% vs. 30.3%, χ2 = 7.89 (1), p < .05]. The second difference was in the willingness to report child abuse. Namely, female ophthalmologists' willingness to report child abuse was higher (M = 5.58, SD = 0.97) than that of male ophthalmologists (M = 3.05, SD = 1.23) [t = −2.03 (105), p < .05].
Linear Regression Controlling Gender and Training Experience and Attitudes and Knowledge as Predictors of Ophthalmologists’ Willingness to Report Child Abuse.
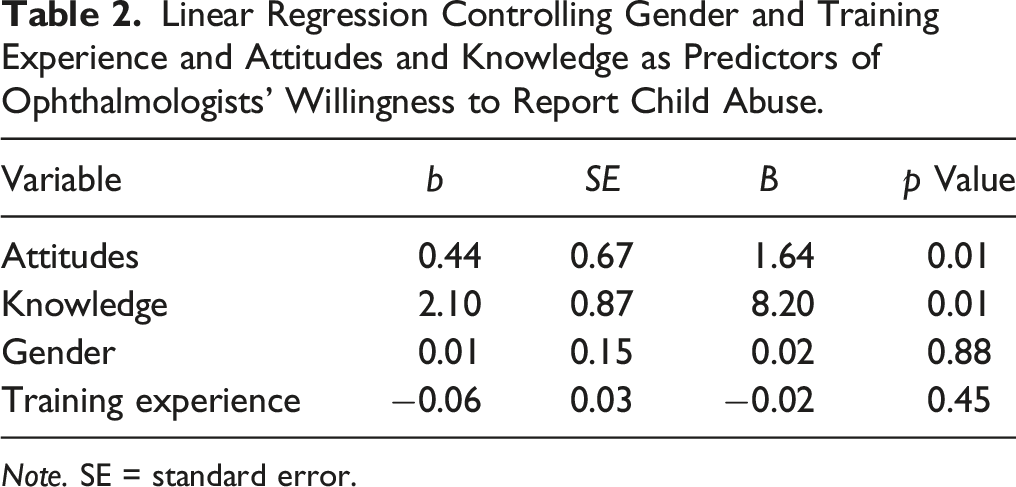

Note. SE = standard error.
Discussion
The present study explored ophthalmologists' attitudes, knowledge, and willingness to report child abuse. This study found that 45% of the ophthalmologists had treated suspected victims of child abuse, but only 43% of the suspected victims of child abuse were reported to the authorities. This finding is consistent with the literature that reveals the issue of underreporting child abuse by healthcare providers (Demirçin et al., 2017; Eads, 2013; Gubbels et al., 2021). Moreover, this finding is consistent with the literature that indicates a discrepancy between the identification and reporting of child abuse. Namely, many cases that are suspected or identified as child abuse are not reported. Thus, in the study by Sonbol et al. (2012), 50% of the dentists studied suspected child abuse but only 12% reported their suspicions.
In the present study, the ophthalmologists expressed moderate attitudes towards reporting child abuse, while several barriers to reporting were evident. In addition, the ophthalmologists’ level of knowledge regarding the identification and management of child abuse was found to be low, as revealed by the low rates of correct answers in all three knowledge questions. It is likely that this lack of knowledge was the main reason for the low reporting rate in the present study. The positive association found in the present study between ophthalmologists' level of knowledge and their willingness to report, supports this assumption. Indeed, more than a quarter of the ophthalmologists reported not having the necessary knowledge and experience to help them identify and report child abuse. Healthcare professionals’ lack of knowledge regarding identification and management of child abuse has been consistently named as one of the main reasons for failure to report cases of child abuse and neglect (Alvarez et al., 2004) even in recent studies (Alsaleem et al., 2019; Demirçin et al., 2017; Sathiadas et al., 2018; Silva-Oliveira et al., 2020; Yadav & Datta, 2017).
Attitudes and knowledge were associated with willingness to report, but not with actual reporting in the past. It is therefore advisable to carry out further studies that will examine the discrepancy between intentions and actual reporting of violence against children.
In the present study, ophthalmologists who had undergone training on child abuse had a higher level of knowledge than those who had not undergone such training. In consistence with this, dentists who received formal training on child abuse in dental school and post-qualification courses were significantly more likely to report suspected cases (Sonbol et al., 2012). There is a general agreement in the literature that increased availability of training programs on child abuse may lower physicians' lack of knowledge on this topic (Alvarez et al., 2004).
In the present study, the lack of knowledge regarding the identification and management of child abuse was more prominent among specialists, while residents had a higher level of knowledge. A possible reason for this is that the specialists' formal training program in medical school did not include the topic of child abuse and the physician’s role in the identification and management of child abuse. Moreover, this finding may indicate that there is also a lack of postgraduate training on child abuse for medical staff. It should be noted that in the study by Demirçin et al. (2017), no statistically significant difference was found in the level of knowledge between general practitioners and residents. This discrepancy may be explained by differences in education programs in various countries. Nevertheless, Demirçin et al. (2017) similarly linked their finding to a lack of postgraduate training on child abuse.
In this study, female ophthalmologists expressed a higher awareness of ophthalmologists’ obligation to report suspected child abuse to the authorities. In addition, female ophthalmologists expressed higher willingness to report suspected cases of child abuse. These findings suggest that female ophthalmologists attributed greater importance to ophthalmologists' role in identifying and managing child abuse. It should be noted that in several previous studies, the physician’s gender was not found to be associated with his/her attitudes towards identifying and managing child abuse (Alsaleem et al., 2019; Demirçin et al., 2017). In contrast, another study, conducted among dentists found that it was male dentists who tended to report more suspected cases of child abuse, compared to female dentists (Sonbol et al., 2012). Therefore, the physician’s gender may sometimes play a role in the physician’s attitudes towards identifying and managing child abuse, and this role may be culture dependent. In a previous Israeli study by Ben Natan et al. (2012), which explored healthcare professionals’ attitudes towards screening female patients for domestic violence, female healthcare professionals similarly expressed less tolerant attitudes towards domestic violence than did male professionals.
Research Limitations
The convenience sampling limits the generalizability of the research results. The research results may be prone to self-selection bias, i.e., it is possible that ophthalmologists who took part in the study had a-priori more positive attitudes towards the identification and management of child abuse. In addition, the research results may be prone to social desirability, due to the considerable sensitivity of the research topic. Moreover, the cross-sectional research design does not allow establishing cause and effect.
Conclusion
The present study reveals that underreporting of child abuse, and more precisely the discrepancy between identification and reporting, is also present among ophthalmologists. It seems that lack of knowledge regarding the identification and reporting of child abuse is the main barrier to reporting, especially among specialists. These findings underscore the importance of training programs on child abuse, both during formal education in medical school and post-qualification, for all ophthalmologists irrespective of their seniority. These programs should encompass both professional and legal aspects of managing child abuse in the ophthalmology practice.
In addition, the results of this study suggest that gender may play a role in ophthalmologists' attitudes towards reporting of child abuse. However, further research is warranted to confirm the presence of differences between male and female ophthalmologists, as well as the nature of these differences.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
