Abstract
Identifying dual-eligible beneficiaries who use Medicaid-funded long-term services and supports (LTSS) is difficult, hindering efforts to monitor use and improve quality. We demonstrate a strategy that uses only Medicare data to identify nursing home (NH) users and Medicaid home-and-community-based-service (HCBS) waiver participants by leveraging the fact that these groups exclusively qualify for zero cost-sharing in Part D. In a multistate cohort of low-income older adults, we identified Part D LTSS beneficiaries (dual-eligible beneficiaries with zero Part D cost-sharing) in Medicare enrollment records and verified LTSS use in NH assessments and Medicaid HCBS data. Over 96% of NH/HCBS waiver users in MDS or Medicaid data were correctly identified as Part D LTSS beneficiaries, and 93% of beneficiaries without NH or HCBS waiver use were accurately identified as not being Part D LTSS beneficiaries. Leveraging Part D data could support more timely evidence on quality and outcomes for dual-eligible LTSS users.
Keywords
Introduction
Dual-eligible individuals with Medicare and Medicaid who use long-term services and supports (LTSS) face exceptional risks for poor health outcomes and high costs (Fabius et al., 2022; Figueroa et al., 2017; Kane et al., 2013; Keohane et al., 2018; Konetzka et al., 2012). Advancing quality of care for dual-eligible beneficiaries depends on timely access to comprehensive data on nursing home (NH) and home-and-community-based services (HCBS) use. Unfortunately, identifying Medicaid-funded LTSS use has traditionally required complex, expensive data linkages. This data gap impedes efforts to monitor and improve health outcomes.
This article investigates an easier option for identifying dual-eligible beneficiaries who use LTSS based on Medicare enrollment data detailing Part D Low-income Subsidy (LIS) benefits. Almost all (98%) dual-eligible beneficiaries have Part D (Centers for Medicare & Medicaid Services, 2020) since enrollment is automatic unless beneficiaries opt out. Only dual-eligible beneficiaries with Medicaid-funded NH use or, since 2012, HCBS waiver participation qualify for Part D LIS zero cost-sharing, creating an opportunity to identify LTSS users.
Given Part D cost-sharing rules, this method only identifies individuals who access HCBS through specific programs: a 1915(c) waiver, 1115 waiver, or a 1915(i) HCBS state plan. All states offer at least some HCBS services through one of these programs. The most common HCBS waiver program is the 1915(c) waiver, which enrolls Medicaid participants who qualify for an institutional level of care due to factors like needing assistance with multiple activities of daily living (Skira et al., 2022). An 1115 waiver or 1915(i) state plan can also include individuals who need less than an institutional level of care. All three of these programs can be limited to specific Medicaid populations, like older adults. States can also limit the 1915(c) and 1115 waiver programs to certain geographic areas and create waiting lists to cap enrollment. Services covered can vary, ranging from personal care to adult day center use to respite care. Nationally, 1915(c) waivers and 1915(i) state plans are the largest source of Medicaid HCBS dollars, funding 58% of HCBS services (Stepanczuk et al., 2024).
In contrast to these HCBS programs, HCBS offered as a personal care or home health state plan benefit must be universally available statewide without waiting lists for Medicaid participants who meet basic requirements (like needing assistance with activities of daily living). All states must offer home health services as a state plan benefit. States can choose to offer personal care services as a state plan benefit; 34 states have elected this option (Musumeci et al., 2019). Dual-eligible beneficiaries who exclusively access HCBS through state plan benefits do not qualify for zero cost-sharing in Part D and thus cannot be identified as HCBS users based on their Part D benefits level. Nationally, dual-eligible beneficiaries are more likely to access HCBS through waiver programs (19% with any HCBS waiver use vs. 9% with only HCBS state plan use). Total Medicaid spending per HCBS state plan user is lower than spending per HCBS waiver user (about $18,000 vs. $56,000), which is consistent with waivers having stricter eligibility criteria (usually NH level of care) than state plan benefits (Medicare Payment Advisory Commission [MedPAC] & Medicaid and CHIP Payment and Access Commission [MACPAC], 2024).
By demonstrating that it is feasible to identify a large fraction of dual-eligible LTSS users based solely on Medicare data, we aim to facilitate timely research for this critical population. To validate using zero Part D cost-sharing as an LTSS indicator, we analyzed its sensitivity and predictive value in linked administrative data from a cohort of predominantly low-income adults. Among dual-eligible beneficiaries with NH or HCBS 1915(c) waiver use according to their Part D LIS benefits, we measured and described the characteristics of beneficiaries with or without corresponding LTSS use in NH assessments and Medicaid data. Using data from our cohort and state-wide Medicaid claims, we also described the characteristics of individuals who used personal care services without waiver participation and are not identified by this strategy.
New Contribution
Why propose a method of identifying LTSS users that does not include all HCBS users? The state of evidence on the impact of the COVID-19 pandemic illustrates the need for thinking broadly about how we measure LTSS. Researchers quickly used Medicare enrollment data to report mortality rates in assisted living settings (Thomas et al., 2021) and newly collected facility-level data to provide evidence on deaths in NHs (Gorges & Konetzka, 2020), but to the best of our knowledge, there is only limited evidence of mortality rates among Medicaid HCBS users (Kaye & Caldwell, 2023), despite this population’s exceptional risk for poor outcomes. Our proposed flag, available on a widely used Medicare data source, could be used to provide this type of timely, important evidence that highlights areas where analyses with more robust LTSS data are needed. This type of approach has been embraced in dementia research using administrative datasets. Even though claims-based dementia measures underrepresent adults with mild cognitive impairment and adults with dementia in several racial and ethnic groups (Grodstein et al., 2022), identifying large numbers of patients with dementia in national datasets is an important starting point for evidence. We argue the same is true for LTSS users.
Method
Study Population, Data, and Measures
This study used data from the Southern Community Cohort Study (SCCS), a cohort of adults age 40 to 79 primarily recruited at community health centers in 12 Southeastern states during the years 2002 to 2009 (Signorello et al., 2010). The SCCS is approved by the Vanderbilt University Institutional Review Board. Validation analyses use linked 2010-2018 Medicare and Medicaid MAX and TAF data files and Minimum Data Set (MDS) NH assessments, which are required for all patients admitted to Medicare or Medicaid certified NHs.
Our study population included dual-eligible beneficiaries who reached age 65 by 2021, lived in SCCS recruitment states, and had at least 1 month of Medicare enrollment with full Medicaid and Part D between 2010 and 2018 (Supplemental Appendix Figure 1). We refer to the new measure as the Part D LTSS indicator: a binary flag for whether beneficiaries had Part D LIS zero cost-sharing for at least 1 month per calendar year according to the Medicare Beneficiary Summary File, which includes monthly indicators for level of Part D LIS benefits (detailed in the Supplemental Appendix).
To identify long-term NH use in a given year, we checked whether beneficiaries had either a quarterly or annual MDS assessment. Since all study members are dual-eligible, we assumed long-term stays were Medicaid-funded. Because MDS records are available more consistently across states, we used MDS data instead of Medicaid NH claims.
We identified any Medicaid HCBS waiver use during a year based on whether Medicaid enrollment data indicated participation in a HCBS 1915(c) waiver or a beneficiary had any outpatient HCBS 1915(c) waiver claims (see the Supplemental Appendix). All states in our sample had 1915(c) waivers; no sample states had 1915(i) programs for older adults during our study period. One state (Tennessee) predominantly offered HCBS through a Section 1115 managed care waiver. Not all Section 1115 waiver participants in Tennessee use HCBS, which precludes using waiver participation to identify HCBS users. Therefore, we report results for Tennessee separately.
To understand how many beneficiaries who have nonwaiver HCBS use might be missed since they do not qualify for Part D zero cost-sharing, we also identified whether beneficiaries had any Medicaid-funded personal care use based on procedure codes. We chose to focus on personal care since procedure codes are more consistently available in MAX and TAF data than other types of HCBS use. Unlike home health care services, where Medicare might be the primary payer for dual-eligible beneficiaries, Medicaid is the primary funder of personal care.
Other variables include age, whether beneficiaries qualified for Medicaid due to poverty via the Qualified Medicare Beneficiary program, Medicare Advantage participation, state of residence, and mortality from the Medicare enrollment files and self-reported measures from the SCCS baseline survey: sex, race, education level, marital status, and household size. Based on established algorithms (Chronic Conditions Warehouse, 2022), we identified any history of Alzheimer’s disease or related dementias (ADRD), chronic obstructive pulmonary disease (COPD), diabetes, heart failure, ischemic heart disease, or chronic kidney disease in the Medicare Provider Analysis and Review File (MedPAR—inpatient and skilled nursing facility admissions, including hospitalizations for most Medicare Advantage enrollees) and outpatient and carrier traditional Medicare claims. The total number of inpatient stays is from the MedPAR data.
Analytic Approach
First, we report the number of Part D LTSS beneficiaries (i.e., those with the indicator) from 2010 to 2018, including an anticipated increase in 2012 when HCBS users first qualified for Part D zero cost-sharing. We then selected one random observation per individual over the time span 2012 to 2018 to observe each person only once in validation analyses. We compared individuals’ characteristics across four categories: (1) No Part D LTSS indicator; (2) Part D LTSS indicator with any long-term NH use (confirmed in MDS data); (2) Part D LTSS indicator with Medicaid HCBS waiver use (confirmed in Medicaid data) and no long-term NH use; and (3) Part D LTSS indicator without verified LTSS use. This latter group includes individuals who did not use LTSS and have the Part D LTSS indicator in error. This group may also include LTSS users whose LTSS use is not captured under our LTSS definition or with available data sources.
We assessed the Part D LTSS indicator’s reliability by first measuring sensitivity, or the percentage of beneficiaries with NH or Medicaid waiver use (in MDS or Medicaid data) who had the Part D LTSS indicator. Specificity assessed the percentage of beneficiaries without use of these services who did not have the Part D LTSS indicator. The positive predictive value indicated the percentage of Part D LTSS beneficiaries who had NH or Medicaid waiver use. The negative predictive value measured the percentage of beneficiaries without the Part D LTSS indicator who did not use these services. Subgroup analyses report these measures using only TAF or MAX data and among beneficiaries aged 65 and above with ADRD, COPD, or heart failure.
Our preferred measure of LTSS potentially misses some NH and HCBS waiver users. For example, someone who moved to a NH in November and had their first quarterly MDS completed in January would not be identified as a LTSS user in their admission year. To assess how the LTSS measurement approach affected results, we assessed validation results under broader definitions of LTSS: (1) any HCBS waiver use or long-term NH use in the prior, current, or subsequent calendar year and (2) any HCBS waiver use or any NH use (including short stays) in the current calendar year. Failing to identify HCBS waiver use due to unreliable Medicaid data would also lead to undercounting LTSS users. Therefore, we repeated validation analyses among individuals who have a linked Medicaid record and reside in a subset of states with more reliable Medicaid HCBS waiver data according to the T-MSIS Data Quality Atlas.
Even with perfect data that could reliably identify all NH and HCBS waiver users, the Part D LTSS indicator will not identify individuals who exclusively use state plan HCBS services and are not eligible for zero Part D cost-sharing. To understand this population, we selected all beneficiaries with either HCBS waiver use or a Medicaid personal care services claim and compared their characteristics based on whether or not they were identified by the Part D LTSS indicator. If beneficiaries had multiple years of HCBS use, we randomly selected 1 year for this analysis. In states where SCCS recruitment occurred, we also used state-wide Medicaid data to report the percentage of dual-eligible HCBS users aged 65 and above who used personal care services without concurrent participation in a 1915(c) program in a given year. We examined whether this percentage varied by age, race, sex, type of Medicaid benefits, or state.
Results
The number of Part D LTSS beneficiaries more than doubled from 318 and 350 in 2010 and 2011, respectively, to 946 in 2012 when Part D LIS zero cost-sharing expanded to include HCBS users (Figure 1). In 2012, we identified 292 Part D LTSS beneficiaries with long-term NH use, 539 with Medicaid HCBS use, and 115 beneficiaries with unverified LTSS use.
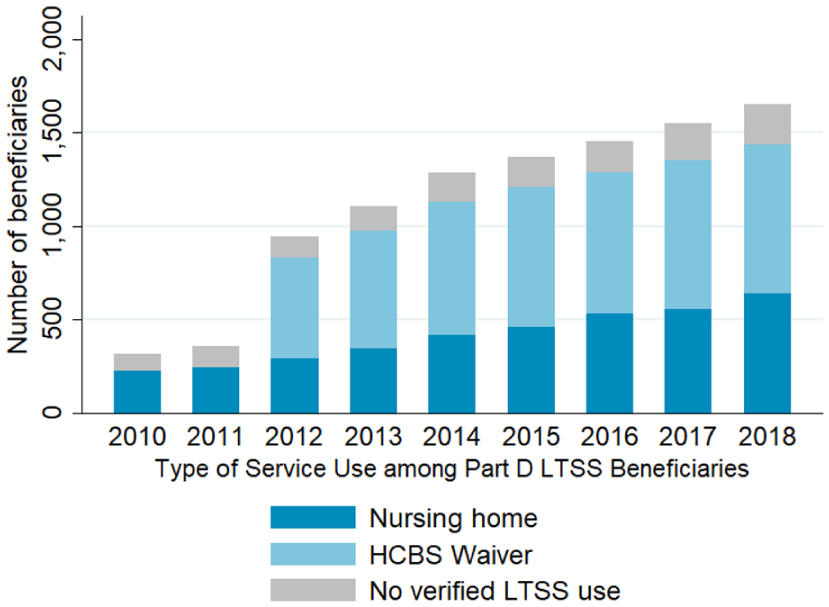
Number of Cohort Members With Long-Term Services and Supports Use According to Part D Low Income Subsidy by Type of Long-Term Services and Supports Use.
After randomly selecting one observation per beneficiary across years 2012 to 2018, beneficiaries with the Part D LTSS indicator showed several signs of poor health (Table 1, Supplemental Appendix Table 2). Relative to beneficiaries without the Part D LTSS indicator, Part D LTSS beneficiaries with HCBS waiver use were older (mean age of 72.1 vs. 68.4) and had higher prevalence of ADRD (21.9% vs. 5.8%), COPD (27.6% vs. 19.6%), and heart failure (37.1% vs. 16.9%). These differences were even larger for Part D LTSS beneficiaries with NH use. Type of LTSS use varied by race: 59.3% of Part D LTSS NH users were Black compared to 77.1% of Part D LTSS HCBS users. Like beneficiaries with verified LTSS use in Medicaid or MDS data, Part D LTSS beneficiaries who did not have verified LTSS use were older (mean age 72.6) and had a high prevalence of ADRD (38.7%).
Characteristics of Cohort Members by Long-Term Services and Supports Use Identification in Part D Data.
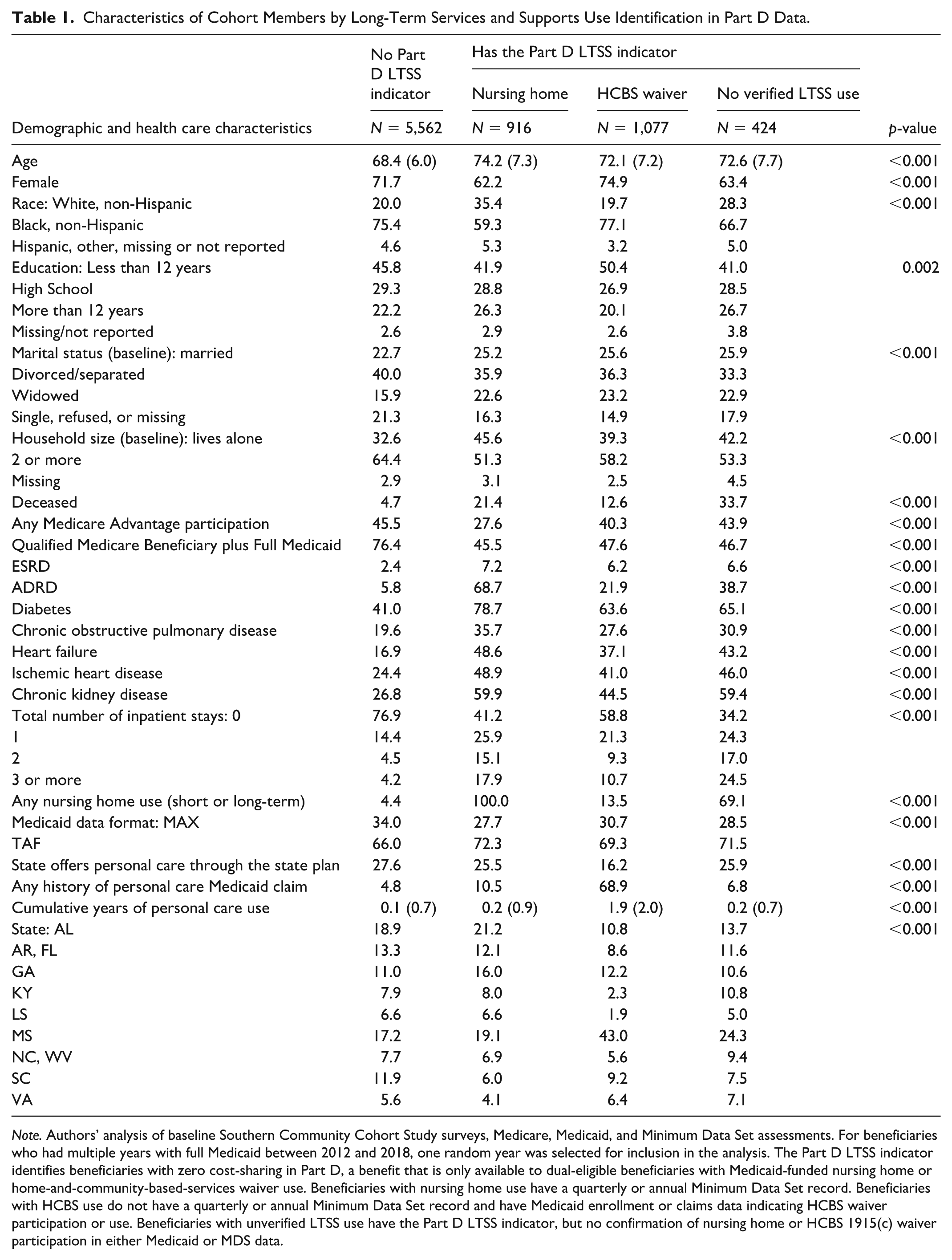
Note. Authors’ analysis of baseline Southern Community Cohort Study surveys, Medicare, Medicaid, and Minimum Data Set assessments. For beneficiaries who had multiple years with full Medicaid between 2012 and 2018, one random year was selected for inclusion in the analysis. The Part D LTSS indicator identifies beneficiaries with zero cost-sharing in Part D, a benefit that is only available to dual-eligible beneficiaries with Medicaid-funded nursing home or home-and-community-based-services waiver use. Beneficiaries with nursing home use have a quarterly or annual Minimum Data Set record. Beneficiaries with HCBS use do not have a quarterly or annual Minimum Data Set record and have Medicaid enrollment or claims data indicating HCBS waiver participation or use. Beneficiaries with unverified LTSS use have the Part D LTSS indicator, but no confirmation of nursing home or HCBS 1915(c) waiver participation in either Medicaid or MDS data.
Performance of Part D Long Term Services and Supports Indicator, by Population and LTSS Definition.
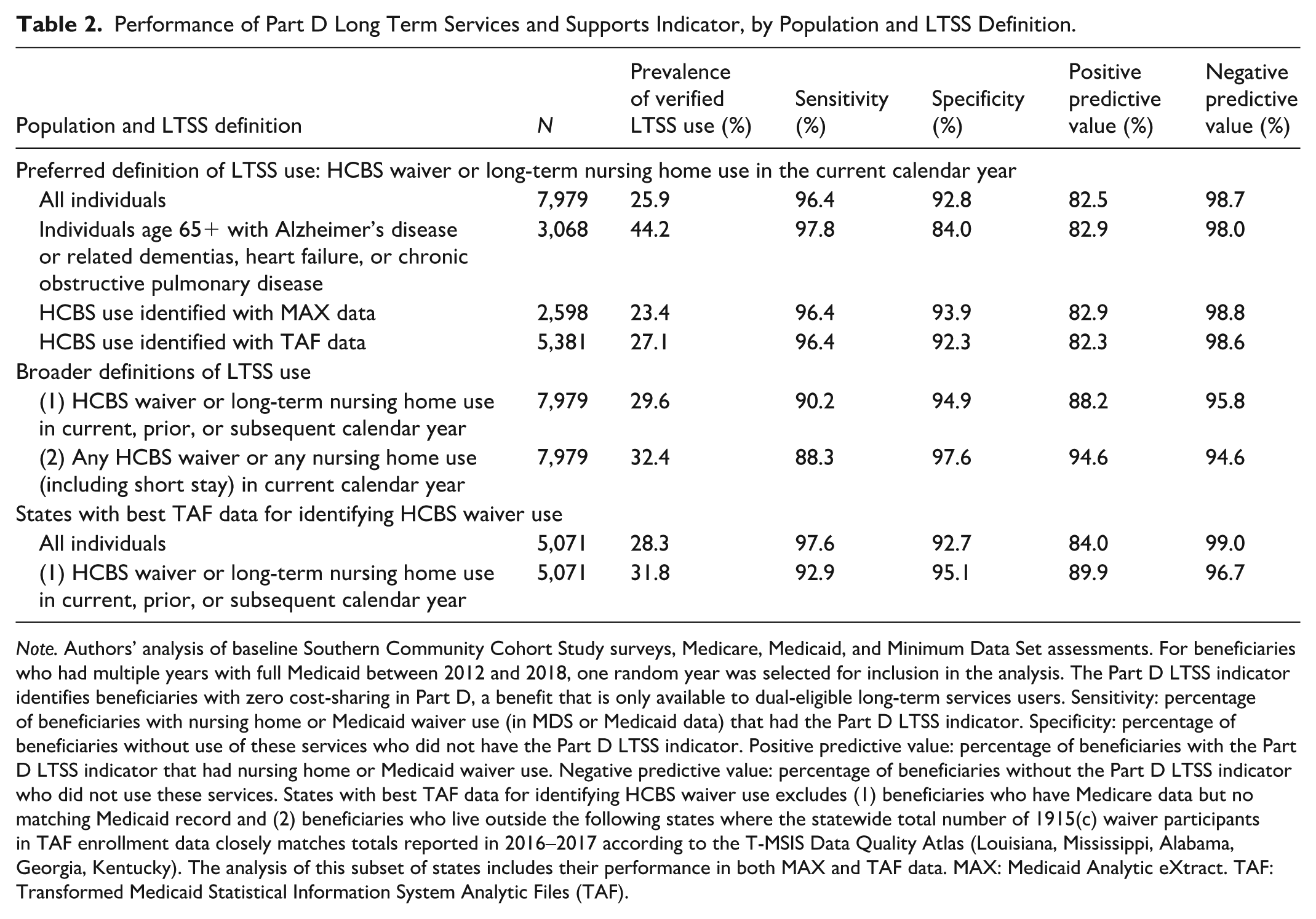
Note. Authors’ analysis of baseline Southern Community Cohort Study surveys, Medicare, Medicaid, and Minimum Data Set assessments. For beneficiaries who had multiple years with full Medicaid between 2012 and 2018, one random year was selected for inclusion in the analysis. The Part D LTSS indicator identifies beneficiaries with zero cost-sharing in Part D, a benefit that is only available to dual-eligible long-term services users. Sensitivity: percentage of beneficiaries with nursing home or Medicaid waiver use (in MDS or Medicaid data) that had the Part D LTSS indicator. Specificity: percentage of beneficiaries without use of these services who did not have the Part D LTSS indicator. Positive predictive value: percentage of beneficiaries with the Part D LTSS indicator that had nursing home or Medicaid waiver use. Negative predictive value: percentage of beneficiaries without the Part D LTSS indicator who did not use these services. States with best TAF data for identifying HCBS waiver use excludes (1) beneficiaries who have Medicare data but no matching Medicaid record and (2) beneficiaries who live outside the following states where the statewide total number of 1915(c) waiver participants in TAF enrollment data closely matches totals reported in 2016–2017 according to the T-MSIS Data Quality Atlas (Louisiana, Mississippi, Alabama, Georgia, Kentucky). The analysis of this subset of states includes their performance in both MAX and TAF data. MAX: Medicaid Analytic eXtract. TAF: Transformed Medicaid Statistical Information System Analytic Files (TAF).
The Part D LTSS indicator demonstrated high sensitivity and specificity (Table 2). The overall prevalence of NH use in MDS data and HCBS waiver use in Medicaid data was 11.6% and 15.0%, respectively, with 25.9% of the cohort using one or both forms of LTSS. Among all verified LTSS users in MDS or Medicaid data, almost all (96.4%) had the Part D LTSS indicator. Among all beneficiaries without MDS or claims-based indicators of LTSS service use, 92.8% did not have the Part D LTSS indicator. Sensitivity and specificity were largely consistent across different subpopulations. The negative predictive value, or the share of beneficiaries without the Part D LTSS indicator who did not have confirmed LTSS use, was 98.7% in our main analyses and ranged from 94.6% to 99.0% in sensitivity analyses.
Most Part D LTSS beneficiaries had confirmed LTSS use in MDS or Medicaid data, as indicated by the positive predictive value: 82.5% in the overall population. The positive predictive value was higher in sensitivity analyses where we verified more LTSS users by examining states with better Medicaid data quality (84.0%) and with broader definitions of LTSS use. When every beneficiary who had LTSS use in the prior, current, or subsequent year was counted as a verified LTSS user, the positive predictive value increased to 88.2% in the overall population and 89.9% in the subgroup with better Medicaid data quality. The positive predictive value increased to 94.6% in the overall population when we counted any NH use, regardless of length of stay, as verified LTSS use. However, the sensitivity of the Part D LTSS indicator, or how frequently the indicator is present among verified LTSS users, declines to 88.3% under the broadest LTSS definition because it includes individuals whose NH stays are primarily covered by the Medicare skilled nursing facility benefit, not Medicaid LTSS benefits.
Among beneficiaries with any Medicaid data indicating HCBS waiver or personal care services use, the Part D indicator failed to identify 15.5% (Table 3) who had a personal care claim but no concurrent HCBS 1915(c) waiver participation in the same year. Personal care users not identified by the Part D LTSS indicator exclusively lived in the 5 states with a personal care state plan benefit and were more likely to qualify for Medicaid as a Qualified Medicare Beneficiary (QMB) (88.2% vs. 48.0%), had lower education levels (60.7% with less than 12 years of education vs. 49.9%), and were less likely to have ADRD (16.1% vs. 25.2%).
Characteristics of Cohort Members With 1915(c) Waiver Use or Personal Care Use by Long-Term Services Use Identification in Part D Data.
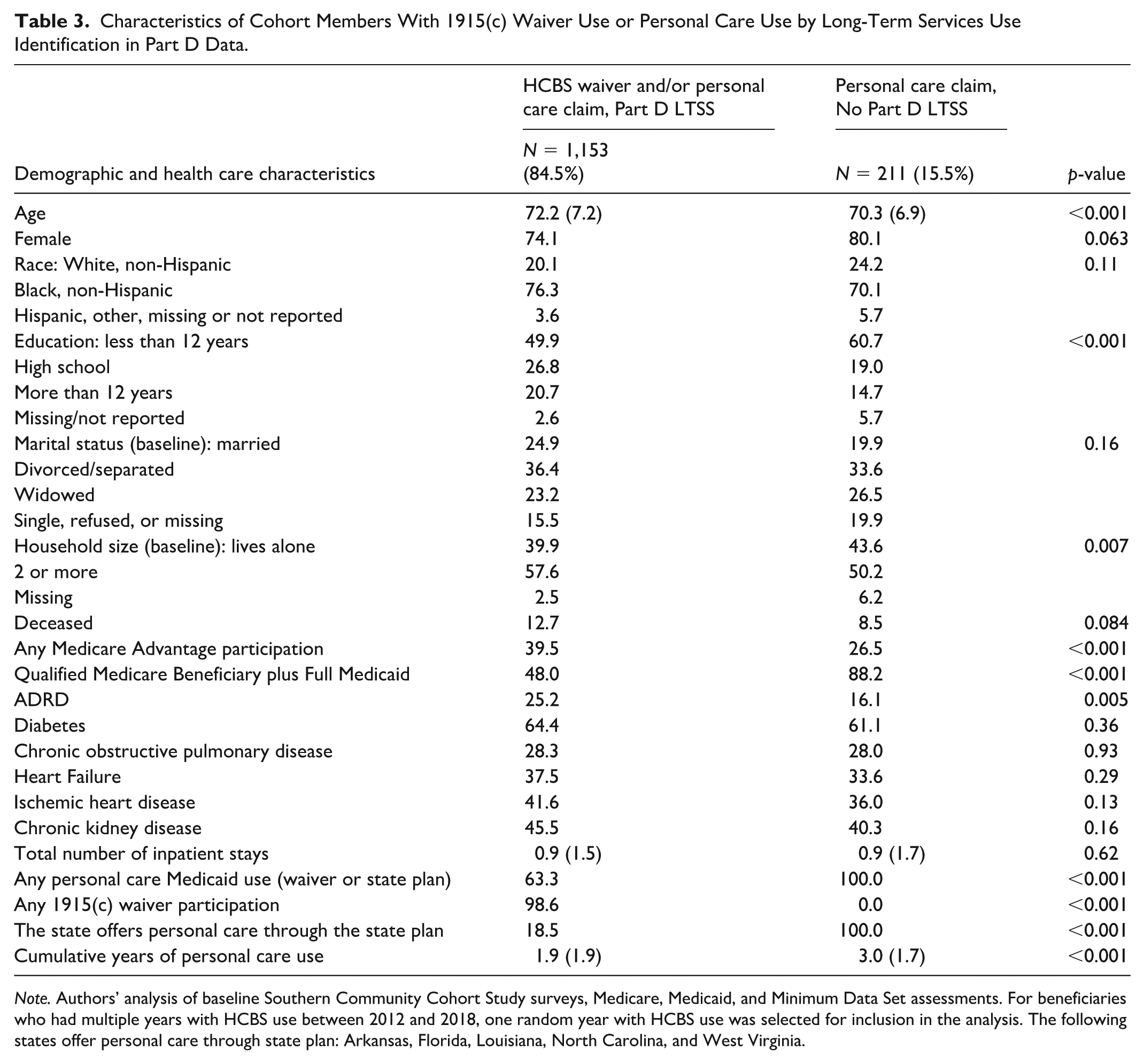
Note. Authors’ analysis of baseline Southern Community Cohort Study surveys, Medicare, Medicaid, and Minimum Data Set assessments. For beneficiaries who had multiple years with HCBS use between 2012 and 2018, one random year with HCBS use was selected for inclusion in the analysis. The following states offer personal care through state plan: Arkansas, Florida, Louisiana, North Carolina, and West Virginia.
In pooled state-wide Medicaid data for dual-eligible beneficiaries age 65 and above (Supplemental Appendix Table 3), the populations with the highest rates of any HCBS use (waiver or personal care) included beneficiaries who were female (18.8% with any HCBS use), aged 85 and above (25.9%), or Black (22.8%). Exclusively using personal care benefits without waiver use in the same year was more common among female HCBS users (21.6% with exclusive personal care use vs. 17.9% for males) and among those who qualified for Medicaid via the QMB program (30.1% vs. 9.3% for non-QMB HCBS users). A total of 16.0% of White HCBS users exclusively used personal care services. Exclusive personal care use was more common among HCBS users who were Black (24.9%), Hispanic (25.3%), American Indian, Native Hawaiian or Pacific Islander (59.6%), had unknown race (20.0%), or reported multiracial or other race and ethnicity (65.3%). With the exception of exclusive personal care use among Hispanic HCBS users, these differences were much larger when we limited the study sample to states that offer personal care as part of their state plan. Among HCBS users in these states, exclusively using personal care benefits without waiver participation was also more common among younger beneficiaries (38.2% among those age 65–74 vs. 28.6% among those age 85+) and among Asian HCBS users (49.9%). When we examined these results on a state-by-state basis in states that offer personal care as a state plan benefit, exclusive personal care plan use in 2018 ranged from a high of 63.6% HCBS users in North Carolina to a low of 12.1% users in Florida (Supplemental Appendix Table 4), suggesting wide variation across states in how many state plan personal care HCBS users could be missed by the Part D LTSS indicator.
Discussion
The Part D LTSS indicator had high predictive power for beneficiaries with long-term NH use or Medicaid HCBS 1915(c) waiver use, suggesting that using Medicare enrollment data on zero cost-sharing for Part D drugs is a feasible approach for identifying dual-eligible NH residents and Medicaid HCBS waiver participants. This indicator could make it possible to easily do subgroup analyses of dual-eligible LTSS users in studies that only have access to Medicare data due to data use agreement restrictions or resource constraints.
To understand the utility of the Part D LTSS indicator, the performance of another commonly used measure, dementia diagnoses in claims data, can provide important context. Claims data demonstrate 79% sensitivity and 88% specificity in identifying dementia (Grodstein et al., 2022). The corresponding values for the Part D LTSS indicator are higher at 96% sensitivity and 93% specificity, suggesting that the Part D LTSS measure outperforms a widely accepted method that has proved useful in identifying which older adults are at highest risk for poor health outcomes due to cognitive impairment.
However, the Part D LTSS indicator did not identify HCBS users who used HCBS services outside of waiver programs. In our study sample, self-reported data indicate HCBS users missed by the indicator are more likely to have lower education levels and are less likely to have dementia. In state-wide data, exclusive use of personal care services without concurrent 1915(c) waiver use is more common among HCBS users who are female, belong to a racial or ethnic minority group, and qualify for Medicaid with income below the poverty level.
Because of these findings, there are several important considerations in using the Part D LTSS indicator. First, it only identifies Medicaid-funded LTSS use among dual-eligible beneficiaries with full Medicaid and Part D. Even so, that group accounts for a large share of LTSS users, especially in NHs: 63% of NH residents rely on Medicaid (Kaiser Family Foundation, n.d.). Second, the Part D LTSS indicator fails to identify dual-eligible beneficiaries who exclusively access HCBS through Medicaid state plans, which is about a third of HCBS users and about 20% of LTSS users (MedPAC & MACPAC, 2024). This limitation introduces bias: the HCBS population identified by the Part D LTSS indicator will be disproportionately male, older, White, and higher income compared to the population identified with complete Medicare, Medicaid, and MDS data. This issue will introduce less bias in states that do not offer personal care as a state plan benefit. Because of these limitations, the Part D LTSS indicator should be used as a starting point, not a definitive marker, to provide preliminary evidence on opportunities to improve outcomes among dual-eligible LTSS users.
Our study has several limitations. We did not examine the proportion of people with home health claims only without concurrent waiver use because home health cannot be identified as consistently as personal care services across MAX and TAF data sources, and personal care is more common than home health plan use among dual-eligible beneficiaries. Furthermore, home health state plan services may include short-term post-acute care where Medicare is the primary payer. If we included the use of home health state plan services, we may identify a larger share of individuals who use only home health state plan services without concurrent waiver use. According to national estimates, five states in our sample (Florida, Kentucky, North Carolina, Virginia, and West Virginia) reported more than 1,000 dual-eligible home health users (of all ages) in 2022, but it is not clear how many of these home health users may have concurrently used personal care or HCBS waiver services (Stepanczuk et al., 2024).
Other limitations include that this cohort is not representative of the Southeast region or the national dual-eligible population. In our main validation analysis that spans 2012 to 2018, the prevalence of NH use (12%) and HCBS waiver use (15%) is lower than the national 2021 prevalence of these services (15% and 19%, respectively; MedPAC & MACPAC, 2024). The validation results may change in populations whose LTSS prevalence is different. Validation analyses should be repeated with national Medicare, Medicaid, and MDS records, especially to understand whether this indicator identifies dual-eligible beneficiaries enrolled in 1915(i) programs. Additional analyses could also explore whether it is reasonable to assume that individuals with the Part D LTSS indicator who do not have MDS records are HCBS users. In this study, self-reported survey measures were collected multiple years prior to LTSS use for some beneficiaries. A large share of the study population participated in Medicare Advantage and lacked complete claims data for identifying chronic conditions. State-wide analyses relied on administrative data for identifying race and ethnicity, which are incomplete and may be inaccurate.
In a multistate sample of dual-eligible beneficiaries, a beneficiary’s level of cost-sharing assistance in the Part D LIS program reliably identified whether beneficiaries had NH or Medicaid HCBS 1915(c) waiver use. Researchers should consider using this approach to provide more robust, timely data about health outcomes for dual-eligible LTSS users, a population where better evidence is urgently needed.
Supplemental Material
sj-docx-1-mcr-10.1177_10775587251394772 – Supplemental material for Identifying Dual-Eligible Beneficiaries With Long-Term Services and Supports Use in Medicare Enrollment Data
Supplemental material, sj-docx-1-mcr-10.1177_10775587251394772 for Identifying Dual-Eligible Beneficiaries With Long-Term Services and Supports Use in Medicare Enrollment Data by Laura M. Keohane, Emmaline Keesee, Chanee D. Fabius and David G. Stevenson in Medical Care Research and Review
Footnotes
Acknowledgements
The authors would like to thank Taofik Oyekunle for programming assistance with Medicaid data and Kyle Braun and Khrysta Baig for their contributions to an earlier version of this work.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the National Institute on Aging (R01AG068606 and R01AG068606-01S1). The Southern Community Cohort Study was funded by the National Cancer Institute (U01CA202979). Dr. Keohane was additionally funded by Award Number K01AG058700 from the National Institute on Aging. SCCS data collection was performed by the Survey and Biospecimen Shared Resource which is supported in part by the Vanderbilt-Ingram Cancer Center (P30 CA68485). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
