Abstract
Organizational transformation in health care is critical to achieving systemic improvements, yet it lacks a cohesive body of empirical literature. Thirty-six articles met inclusion criteria in this systematic literature review of empirical studies of whole-organization transformation describing the transformation process and measures of transformation. Studies had diverse analytic (n = 14) and descriptive (n = 22) aims and were published in many different journals. Few articles provided definitions of transformation. Most employed weak research designs, about half used models for evaluation, and no common measures of transformation were used across articles. Combinations of distributed leadership, staff engagement, and culture change were recurring themes contributing to successful transformation. Two-thirds of articles used models to guide the transformation process. There was no consistency across articles in which models were used for evaluating or guiding change. Most articles reported successful transformation. The literature is methodologically weak, highlighting the need for more rigorous, theory-driven research on health care transformation.
Keywords
Background
Understanding the dynamics of organizational transformation in health care is essential for guiding improvements in care delivery, yet critical knowledge gaps remain. The purpose of this systematic literature review is to assess what is known and what is not known about organizational transformation in health care. Health care organizations face increasing challenges related to aging patient populations, rising costs, national health care reforms, and shortages and burnout of health care professionals. There have been many calls to make health care organizations more patient-centered, safe, equitable, accessible, effective and efficient (Institute of Medicine (US) Committee on Quality of Health Care in America, 2001). Despite the calls for change, national policy and structural reforms, and interventions to improve individual processes, there has not been adequate progress. Some reasons for the slow progress are that health care organizations face substantial challenges related to their complex nature, interprofessional and interdisciplinary collaboration required by transformation initiatives, power differentials across professional groups and specialties, and consideration of the interests of patients, families, and communities (Institute of Medicine (US) Committee on Quality of Health Care in America, 2001). Organizational transformation may offer solutions to these challenges (Best et al., 2012; Garritsen et al., 2024; Lee et al., 2013). This article provides an updated comprehensive review of existing empirical studies of health care organizational transformation to assess whether gaps have been addressed since previous reviews were conducted. It takes a rigorous approach to examining how organizational transformation has been studied, measured, and evaluated empirically. By analyzing the research methods, measurement approaches, and reported outcomes, we aim to offer new insights into the mechanisms of transformational change and identify areas where further investigation is needed to advance both research and practice in health care settings.
Why Transformation Is Needed
Most efforts to address the challenges in health care have focused on improvements of individual processes or parts of an organization (e.g., emergency department), as opposed to whole institution or (multi-) system level. The fields of implementation science and quality improvement both focus primarily on individual projects or parts of the organization. While these literatures recognize the importance of context to the success of interventions (Damschroder et al., 2009; Kaplan et al., 2012), they do not generally address improving the organizational context—that is, transforming the organization—to support interventions. Furthermore, although such interventions can be effective in improving specific aspects of care, their impacts remain isolated, seldom sustained, and often fail to address broader underlying barriers to delivery of high-quality care delivery (Al-Amin et al., 2024; Charns et al., 2022). Efforts at improving individual processes or parts of the organization are insufficient.
In contrast, transformation includes changing organizational culture—the collective values, norms, and assumptions that influence thought and behavior, as these are pivotal to how an organization functions (Sminia, 2016) and therefore more likely to lead to sustained changes (Hung et al., 2022). A transformational approach is defined as, “a multidimensional, multi-level, radical organizational change involving a paradigmatic shift” (Levy & Merry, 1986) that involves a sustained, organization-wide shift in patient care processes (Lukas et al., 2007) and “. . . departs radically from an organization’s past precedents, aims at large-scale readjustments, and is complex and systemic” (Lee et al., 2013).
Many approaches to organizational transformation in health care stem from other industries and employ performance improvement approaches, such as lean management (Toussaint & Adams, 2015), six sigma (Antony & Banuelas, 2002; Henderson & Evans, 2000), and principles of high reliability organizations (Roberts, 1990; Weick & Sutcliffe, 2007). These approaches involve cultivating an organizational culture that empowers staff to identify and address issues, improving processes through reduction of defects, and enhancing reliability through removal of errors while promoting an environment of “collective mindfulness,” respectively. While these have been described as supporting “whole system changes” and are intended to fundamentally change the culture and functioning of whole organizations, few transformations in health care have been reported in detail (Hung et al., 2022).
New Contribution
There have been three reviews of organizational transformation in health care since 2012 (Best et al., 2012; Garritsen et al., 2024; Lee et al., 2013) and a related, narrower review specifically on change management (Harrison et al., 2021). The (Best et al., 2012) and (Lee et al., 2013) reviews are over a decade old. Lee et al. (2013) examined antecedents, processes (or paths) and outcomes of transformational change. They noted then, “. . . that organizational transformation in health care and other industries is a nascent research interest and that there is much room for research on past and current change initiatives,” and that conceptual and prescriptive papers outnumbered the identified empirical studies, suggesting that research on organizational transformation was still in a burgeoning phase. Consequently, we expect an updated review to identify an increased number of empirical studies on this topic. In a realist review commissioned by the Saskatchewan Canada Ministry of Health, Best et al. (2012) focused on the role of government and policy rather than on processes of transformation. Garritsen et al. (2024) used the Pawson and Tilley (1997) theory of change to examine interactions among context (“social, political, economic and historical circumstances or conditions”), mechanisms of change, and outcomes. Rather than describing intra-organizational dynamics, they focused primarily on inter-organizational collaboration across health care sectors. Harrison et al. (2021) reviewed change management models that were not necessarily models of transformation, and their search terms did not include any form of “transform.” Thus, while of interest and related to the topic of transformation, the Harrison et al. (2021) review is not directly on transformation.
In addition to the need for an updated review, prior reviews identified four gaps in the literature. First, there is no consensus on the conceptualization and definition of organizational transformation, and few articles even include a definition. Garritsen et al. (2024) found that only four of the 19 articles included in their review provided definitions of care transformation. The three other review articles did not report on whether articles in their review contained definitions of transformation. However, Best et al. (2012) stated, “An evidence base . . . is urgently needed for large-system transformation (LST), as there is no agreed-on definition of LST in the literature.”
Second, there is no consolidated source of information on how transformation has been studied, evaluated, and measured, nor about the evaluation models employed. Lee et al. (2013) noted the field still has important gaps in understanding how to measure organizational transformation and its success. Best et al. (2012) commented, “Evaluation demands a careful blending of quantitative measures and accountability with qualitative methods such as interviews, ethnographic observation, and storytelling to make sense of the transformation effort.” Lacking in the literature, however, is information on the prevalence of different study designs and methods. Most studies included in these reviews did not include direct measures of transformation itself, instead reporting more distal clinical or organizational outcomes that might result from transformation. They also did not report on what conceptual models were employed to evaluate transformation in their included articles. Furthermore, lacking in prior reviews is whether articles are descriptive or analytical, following Pettigrew’s (1985) suggestion for judging research articles.
Third, there is insufficient information on the processes/dynamics of transformational change and the models used to guide transformation. Best et al. (2012) reported there is an abundance of literature on antecedents or factors that influence transformation, but much less on actions undertaken to achieve transformational change or how these actions lead to observed results. Recognizing that health care organizations are complex adaptive systems and that it is unproductive to prescribe “action X to achieve outcome Y,” Best et al. (2012) identified “five simple rules” to guide transformation. They noted, however, their review was limited to what is reported in the literature itself and that the five simple rules may not be exhaustive. Lee et al. (2013) noted, “Few of the reviewed studies characterized the overall process of transformation or described it in sufficient detail.” In their review of change management methodologies, Harrison et al. (2021) noted that change management models were often used as “guiding framework . . . in keeping with contemporary thinking regarding health care as a complex adaptive system.” They also noted, “ . . . it was not possible to detect whether the use of a model, method or process contributed to the success.” Previous reviews have not synthesized reported conclusions about the factors contributing to transformation success, or lack thereof.
Fourth, there is little information on the proportion of transformation efforts that have been successful. Lee et al. (2013) noted there are gaps in the extent to which transformation is documented in the literature and furthermore that . . . existing research literature may reflect a bias toward studies of successful transformation. This bias may in part be the result of difficulties in gaining access to organizations in which transformation initiatives stalled or failed. Lack of sufficient examination of unsuccessful initiatives raises concern about the validity of inferences about observed antecedents and consequences of transformational change. A positive publication bias may also stem from a tendency of researchers to define transformations by outcomes, such as financial turnaround, rather than by an initiative’s vision and goals.
Whether there is bias toward reporting successful transformations has not been well investigated.
To provide an updated review and address the gaps identified in the extant literature, this article aims to offer a comprehensive, systematic review of the empirical literature on organization-wide transformation in health care and to address the following specific research questions:
What are general characteristics of the literature on organizational transformation in health care?
How has organizational transformation in health care been conceptualized and defined?
How has organizational transformation been studied and measured? What conceptual models have been used to evaluate transformation?
What does the literature report on the dynamics of transformation and factors important to successful transformation? What conceptual models have been used to guide transformation efforts?
To what extent have transformation efforts in health care as represented in the literature been successful?
Method
This systematic literature review followed Preferred Reporting Items for Systematic Reviews (PRISMA, http://www.prisma-statement.org) guidelines and was pre-registered with the PROSPERO database (PROSPERO 2020 CRD42020144573). We used Covidence Systematic Review Software for article screening, full-text review, and data extraction, and MaxQDA for coding text passages.
Literature Search
Drawing on the expertise of our research librarian co-author (JS), we crafted a search strategy using a combination of available medical subject headings (MeSH, Emtree) and keywords. We searched peer-reviewed literature using PubMed, Embase, and Business Source Complete for English-language studies published from the start of the respective database records through January 13, 2023. Searches included a combination of terms related to transformation (e.g., organizational transformation, strategic organizational change, large system transformation) and health care settings. The complete search strategy is in Supplemental File 1. Search terms were informed by prior literature on organizational transformation in health care and were iteratively piloted and refined to ensure they captured known key articles of interest. Next, we searched the reference lists of included articles to identify additional articles.
Inclusion and Exclusion Criteria
In line with our definition of organizational transformation, we included empirical articles that reported on whole organization transformation and excluded those focusing on specific processes or departments or deemed to be too narrow to be fundamental, organization-wide efforts. To address gaps in understanding of settings beyond acute care, we included all health care settings. We included both quantitative and qualitative study designs to gather a holistic perspective about “how” and “why” organizational transformation efforts perform. We excluded articles that did not report qualitative or quantitative outcomes or measures of transformation, and those that failed to describe the transformation process in sufficient detail.
Study Selection Process
After removal of duplicates, two reviewers (LC, MC) independently screened all titles and abstracts. If inclusion and exclusion criteria could not be assessed conclusively during this screening, article full texts were retained and reviewed by the two reviewers. Disagreements were resolved through discussion to reach consensus.
Data Extraction and Analysis
We identified and extracted key information from each article (authors, year of publication, journal, definition of transformation, study aims, description of transformation, study design, methods, measures, number of sites, setting, country, length of time for transformation, conceptual models mentioned, extent of success, and the full texts of qualitative results and conclusions of articles) into Covidence, then downloaded the complete database into MS Excel and MaxQDA for analyses. We examined the study aims, change and evaluation models, study design, measures, and success by creating pivot tables of these fields with other study characteristics.
RQ1: General Characteristics of the Literature on Organizational Transformation
We categorized each article based on its aims into either “analytic” or “descriptive.” Analytic articles aimed to “explain,” “explore,” “understand,” “identify,” or “analyze” factors related to transformation, whereas descriptive articles aimed to “describe,” “document,” or “report.” We categorized the relation of authors to the studied organization(s) as internal (all authors employed by the organization), external (no authors employed by the organization) or both (internal and external authors). We considered consultants and external evaluators as external. We classified sites comprised of multiple entities as one site if there was a single management team for all sites (e.g., two hospitals comprising a trust) or if the transformation was of a whole multi-institutional system and data were reported only for the whole system. We also grouped articles by type of journal (e.g., health services research, health care management, clinical); however, we did not group Implementation Science with other journals and report it as a single journal.
RQ2: How Has Organizational Transformation Been Conceptualized and Defined?
In each article, we recorded whether it mentioned transformation or defined transformation and extracted any definition of transformation provided.
RQ3: How Has Organizational Transformation Been Studied and Measured?
We determined whether a study was qualitative or quantitative based on the methods reported in the article. Qualitative articles reported using interviews, focus groups, or observations. Quantitative articles reported surveys of staff, quantitative measures of quality, patient safety, or organizational performance. Articles using both qualitative and quantitative methods were classified as mixed methods. For all studies, to avoid ambiguities in terminology describing study design, we classified three features of the employed study design according to Higgins et al. (2013): inclusion of controls or comparisons, measurement of transformation before and after the intervention, site selection based on measures. We recorded conceptual theories, models, and frameworks used for evaluation of transformation, if any, and examined whether these models were used in multiple articles.
RQ4: What Are Dynamics and Factors Important to Organizational Transformation?
Data extracted as qualitative results and conclusions about transformation were analyzed through a directed qualitative content analysis using the Organizational Transformation Model (OTM) (Charns et al., 2022; Lukas et al., 2007) as a deductive coding framework; topics not covered by the model were coded inductively. We chose the OTM because it is a model of organization-wide transformation specific to health care and includes specific factors reported to be associated with successful transformation. Some of the OTM constructs were specific to Lean Management Systems. In coding, we interpreted constructs broadly (e.g., for “Improvement projects” we considered all types of projects that involved staff). Following initial coding of all articles, similar codes were inductively grouped into thematic categories based on consensus discussion among two researchers (LC, MC). As we did for models used for evaluation, we recorded conceptual theories, models, and frameworks used for guiding the transformation change process, if any, and examined whether these models were used in multiple articles.
RQ5: To What Extent Have Transformation Efforts in Health Care as Represented in the Literature Been Successful?
We categorized success of transformation as “yes” if authors described the intervention as successful in all sites, “no” if unsuccessful in all sites, “partial” if limited success in a single site or “varied” if success varied across sites in multi-site studies. To examine bias in reporting success, we used pivot tables to compare the success of transformation by article characteristics including analytic versus descriptive aims, use of models for evaluation and change, and authorship.
Results
After removal of duplicates, we identified 4,537 unique articles and retained 244 during title and abstract screening. Following full-text review, 36 articles met inclusion criteria and were included in this review (Figure 1). Detailed information on each included article is shown in Table 1. Supplementary File 2 contains distributions of article characteristics (e.g., setting) and crosstabulations of characteristics derived from the pivot table analyses. Here, we highlight the most salient findings for each of our RQs.
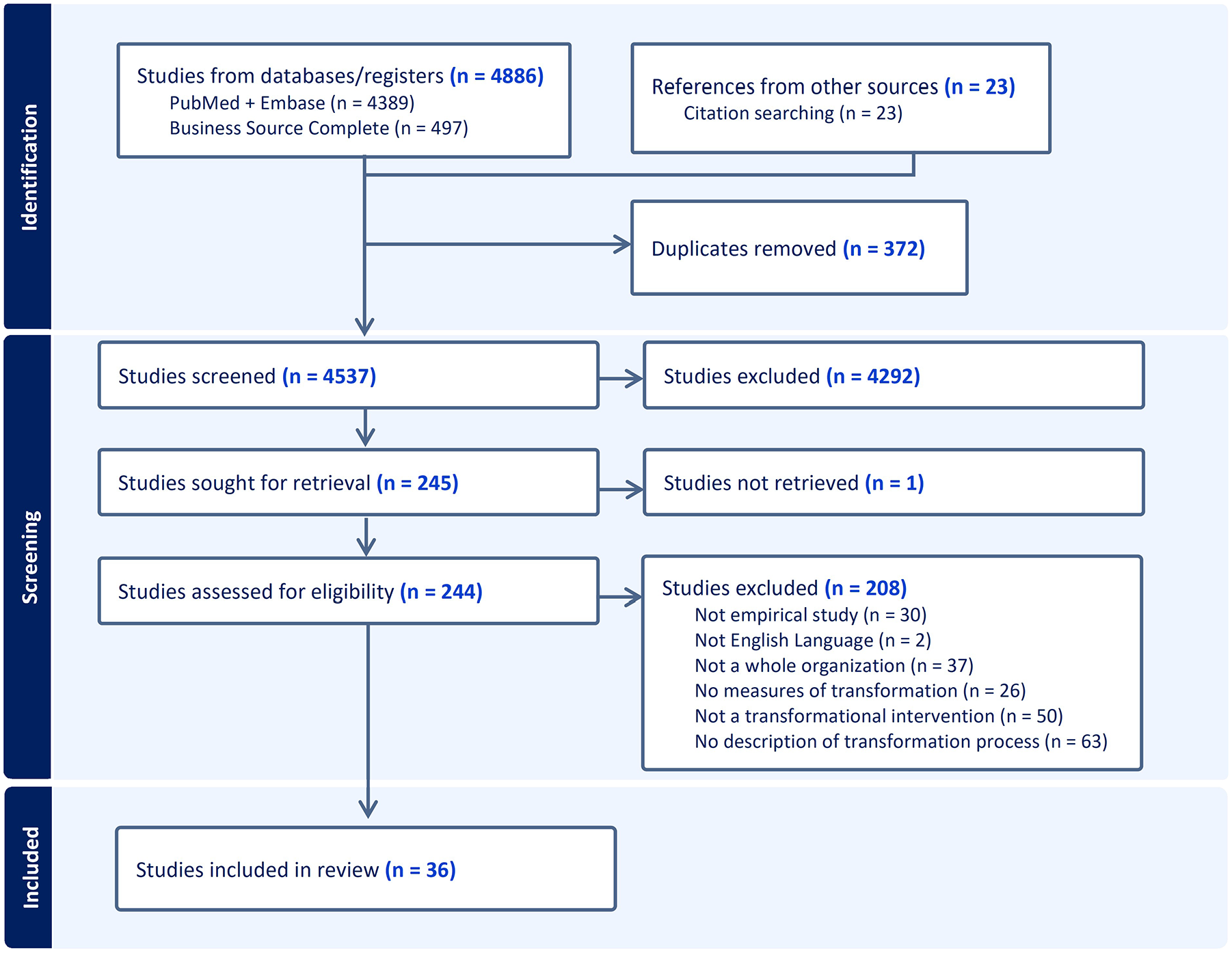
PRISMA Flowchart of Included Studies.
Characteristics of Included Articles.

RQ1: General Characteristics of the Literature on Organizational Transformation
The articles varied substantially in both scope and study aims. Examples are reducing restraints in a mental health setting, leveling power differentials between clinical professionals and their clients and community, improving diversity, equity and inclusion, and increasing patient safety. Based on their aims, we classified 14 (39%) articles as analytic and 22 (61%) as descriptive. The oldest article was published in 1996. The publication rate increased from zero to two articles annually through 2012, to one to three annually from 2013 to 2022. Most articles published after 2012 were descriptive (13/17, 76%). Twenty articles (56%) were published after the Best et al. (2012) and Lee et al. (2013) reviews. Only three of the included articles were also included in the prior Best et al. (2012), Lee et al. (2013), or Harrison et al. (2021) reviews on organizational transformation. Lukas et al. (2007) was included in all three, Henry et al. (2017) was included in Harrison et al. (2021), and McNulty and Ferlie (2004) was included in Lee et al. (2013).
Most articles (21, 58%) were set in hospitals. No other setting had more than four (11%) articles. Most articles were from the United States (20, 56%), the United Kingdom (7, 19%), and Canada (5, 14%). Articles were published in a wide range of journals. Most were the sole publication included from their respective journal. Exceptions were three articles in the Joint Commission Journal on Quality & Patient Safety and two in Academic Medicine. The highest number of articles (9, 25%) were in clinical journals (e.g., American Journal of Community Psychology), followed by eight (22%) in health care management (e.g., Australian Health Review) (see Supplementary File 2 for classification of journals). The numbers of sites ranged from one to 95. Most (23, 64%) were single-site studies. Three (8%) articles had more than 12 sites. Length of time for transformation ranged from 0.5 to 15 years, with a median of 3.5 and a mode of 3 years. The largest percentage (42%) of articles reported transformation lengths between 2 and 3.5 years, although four (11%) reported less than 2 years and eight (22%) over 7 years. Equal numbers (16, 44%) of articles had exclusively external authors and exclusively internal; four (11%) had both internal and external authors. Five studies were designed as qualitative comparison studies. They had different levels of success among sites (“varied” success in Table 1) and gave in-depth analysis of transformation processes in individual sites (Charns et al., 2022; Hunter et al., 2014; Lukas et al., 2007; Stetler et al., 2009; Wolf, 2011).
Analytic Versus Descriptive Aims
Analytic and descriptive articles differed with respect to authorship, number of sites, journal, research design, use of models, methods, measures, and success of transformation. They appear to represent different subsets of the transformation literature. Of the analytic articles, only one of 14 (7%) had exclusively internal authors and less than half (6/14, 43%) were single site. In contrast, most descriptive articles (15/22, 68%) had only internal authors and were single site (17/22, 77%). Studies with the largest number of sites (over 12) were in three descriptive articles, and the four other large studies (7 to 12 sites) were analytic. Journals primarily publishing analytic articles were in the fields of organization sciences (5/6, 83%) and health services research (3/4, 75%) and the journal Implementation Science (1/1); those primarily publishing descriptive articles were in the fields of health care quality and safety (6/6), health care management (7/8, 88%), and clinical disciplines (6/9, 67%).
The stated aims of analytic articles addressed understanding the dynamics of transformation or of factors affecting transformation, relationships between the intervention and contextual factors, people’s lived experience of creating change, or factors affecting sustainability of change. In contrast, aims of most descriptive articles were to present accounts of what was done. Aims of a few articles were to evaluate a particular program or intervention, and those of another few articles were clinically focused (e.g., “achieve baby friendly hospital designation” (Henry et al., 2017) without a stated research aim.
RQ2: How Has Organizational Transformation Been Conceptualized and Defined?
Articles varied in their conceptualization and definition of transformation. Only four articles included explicit definitions of transformation (Charns et al., 2022; Lukas et al., 2007; McNulty & Ferlie, 2004; Wolf, 2011). Most (24, 67%) referred to transformation and included only general descriptions of transformation. These definitions and descriptions shared a focus on holistic change, emphasizing significant and pervasive shifts in how the organization functions. Most descriptions highlighted “culture change” involving values, behaviors, and beliefs that reflect a fundamental shift in the way people think and work. In addition, they highlighted the impact on ideologies, structures, processes, and power dynamics, signifying deep and fundamental change. Many descriptions further underscored the importance of system-wide strategic orientation, implying that transformation is a deliberate process aimed at achieving long-term improvements across whole organizations. While continuous improvement is explicitly mentioned in the context of Lean thinking, it is an underlying theme in many articles, portraying transformation as an ongoing and dynamic process.
Articles explicitly mentioning transformation (24, 67%) tended to focus directly on large-scale, holistic changes in organizational culture, values, and principles. In contrast, articles not explicitly mentioning transformation (12, 33%) tended to focus on organization-wide but more narrowly focused improvements to achieve specific health outcomes (e.g., reducing restraints, achieving baby-friendly hospital designation) without framing these changes within the context of a broader transformation. Nearly all analytic (13/14, 93%) and half of descriptive articles (11/22) explicitly mention transformation.
RQ3: How Has Organizational Transformation Been Studied and Measured?
Study Design
Few articles (9, 25%) used either comparison or control sites. Most (22, 61%) measured transformation before and after the transformation process. Very few articles (5, 14%) reported using measures for site selection. Nine (25%) reported having none of these three research design attributes.
Methods and Measures of Transformation
There were 12 qualitative, 10 quantitative, and 14 mixed-methods studies. Half of all articles (18) reported using staff/employee surveys. Following in frequency were interviews/focus groups of staff/employees (14, 39%), interviews/focus groups of managers (8, 22%), observations (7, 19%), document review (7, 19%), quality/safety measures (7, 19%), and surveys/interviews of patients/consumers (6, 17%). Four articles (11%) used external assessments of transformation (e.g., independent panel of experts). Articles reported a range of measures related to organizational transformation. Some used direct measures of transformation, such as changes in staff engagement and in organizational culture. Others focused on indirect or downstream outcomes presumed to reflect successful transformation, including clinical or quality performance indicators, patient satisfaction, financial metrics, and external recognition (e.g., accreditation or awards). Strictly speaking, the clinical process and outcome measures and other organizational performance metrics were not measures of transformation per se, but rather were indicators of factors expected to be affected by transformation. We report them here only to reflect this literature. At most, three studies used similar surveys, an NHS staff survey; however, lack of detail in the articles precludes a definitive conclusion that they used the identical survey. Two each referred to Press Ganey surveys and AHRQ safety culture surveys; again, it is not clear if these references are to the same surveys. Some articles used measures unique to that article and setting, such as research performance, awards, human resource metrics, and achievement of trust status. One study (Charns et al., 2022) developed a composite measure of transformation based on 11 “markers” of transformation (e.g., staff engagement, staff empowerment, culture of respect) assessed for both their “depth” or “rigor of application” and “spread throughout the organization.”
Models Used for Evaluation
Nineteen articles (53%) used models for evaluation. Of these 17 (47%) reported using one or more published models. Only four published models were mentioned in more than one article: Action Research (4), Pettigrew et al.’s Strategy and Change (3), Complex Organizational Change (2), and Diffusion of Innovation (2) (Details in Supplement 2). Ten (28%) articles mentioned 11 published models that were not mentioned in any other article. Four (11%) used models for evaluation developed within that study. Use of models for evaluation increased over time; most articles (7/9, 78%) in the latest period (2018–2022) used some model for evaluation.
Analytic vs Descriptive Aims
Analytic studies were more rigorous, used different methods and measures, and provided richer descriptions of the transformation process than descriptive studies. A higher percentage of analytic (5/14, 36%) than descriptive articles (4/22, 18%) used comparisons or controls. Analytic studies primarily used qualitative methods (9/14, 64%) and interviews/focus groups with staff (9/14, 64%). Only one analytic study (1/14, 7%) used quality/safety measures and two (2/14, 14%) used staff surveys. In contrast, descriptive studies primarily used quantitative (9/22, 41%) or mixed methods (10/22, 45%), quality/safety measures (6/22, 27%), and staff surveys (16/22, 73%). The analytic articles using comparisons provided in-depth reports of differences in transformation processes. In contrast, the descriptive articles using comparison or control sites—including the three large multi-site studies noted in RQ1 (Benning et al., 2011; Jones et al., 2013; Roberts et al., 2020)—focused on staff survey results at intervention sites compared to quantitative data aggregated from multiple comparison sites and provided minimal information on the transformation process in comparison sites.
There was not a direct correspondence between the rigor of research design and articles’ contributions to understanding of transformation. Of the nine articles that had none of the three Higgins et al.’s attributes—and therefore the weakest research design—five were analytic (Bess et al., 2009; Brooks, 1996; McNulty & Ferlie, 2004; Ochocka et al., 1999; Peirson et al., 2012) and four descriptive (Corring et al., 2016; Lord et al., 1998; Roberts et al., 2020; Venturato et al., 2019). These represented 36% of all analytic articles (5 of 14) and 18% of all descriptive articles (4 of 22). All five of the analytic articles used qualitative methods and provided rich descriptions of transformation. Seven of the nine articles, including all five of the analytic articles, were evaluations that included authors external to the organizations. These external authors did not select the sites for study, engage other sites for comparison or measure before the transformation process. Six of the nine articles used qualitative (67%), two mixed (22%), and one quantitative methods (11%). That only one quantitative article had none of the Higgins et al.’s attributes is because all 10 quantitative articles included measurement of changes in survey scores and only one of these (Roberts et al., 2020) did not measure before the start of the transformation process.
A much greater proportion of analytic (11/14, 79%) than descriptive articles (8/22, 36%) used a model for evaluation. All three mentions of Pettigrew et al.’s strategy and change and two mentions of complex organizational change as evaluation models were in analytic articles.
Use of models for evaluation was more prevalent in articles with external authors and in health services research and clinical journals, and lower proportion of articles reporting single-site studies (see Supplemental File 2 for all detailed breakdowns of methods and measures).
RQ4: What Are Dynamics and Factors Important to Organizational Transformation?
Analysis of Conclusions About Transformation
In the directed qualitative content analysis, we coded 492 text segments extracted from the articles’ conclusions and qualitative results. We applied codes from 20 of the 21 constructs of the OTM and created 12 inductive codes, resulting in 32 unique codes. In each article, we coded between one and 45 segments, with an average of 14 per article. Most prevalent codes across articles were “Leadership support and commitment” (28 articles, 78%), “Organization culture” (22, 61%), “Frontline staff engagement and enthusiasm for transformation” (21, 58%), “Alignment of organizational strategy, policies and resources” (17, 47%), “Interaction of multiple factors” (16, 44%), “Capability development” (16, 44%), and “Middle manager engagement and enthusiasm for transformation” (14, 39%). Six of these seven codes were coded deductively from the OTM; “Interaction of multiple factors” was an inductive code. Other inductively identified codes were mentioned in few articles (see Table 2 for exemplary quotes).
Conclusions About Transformation.
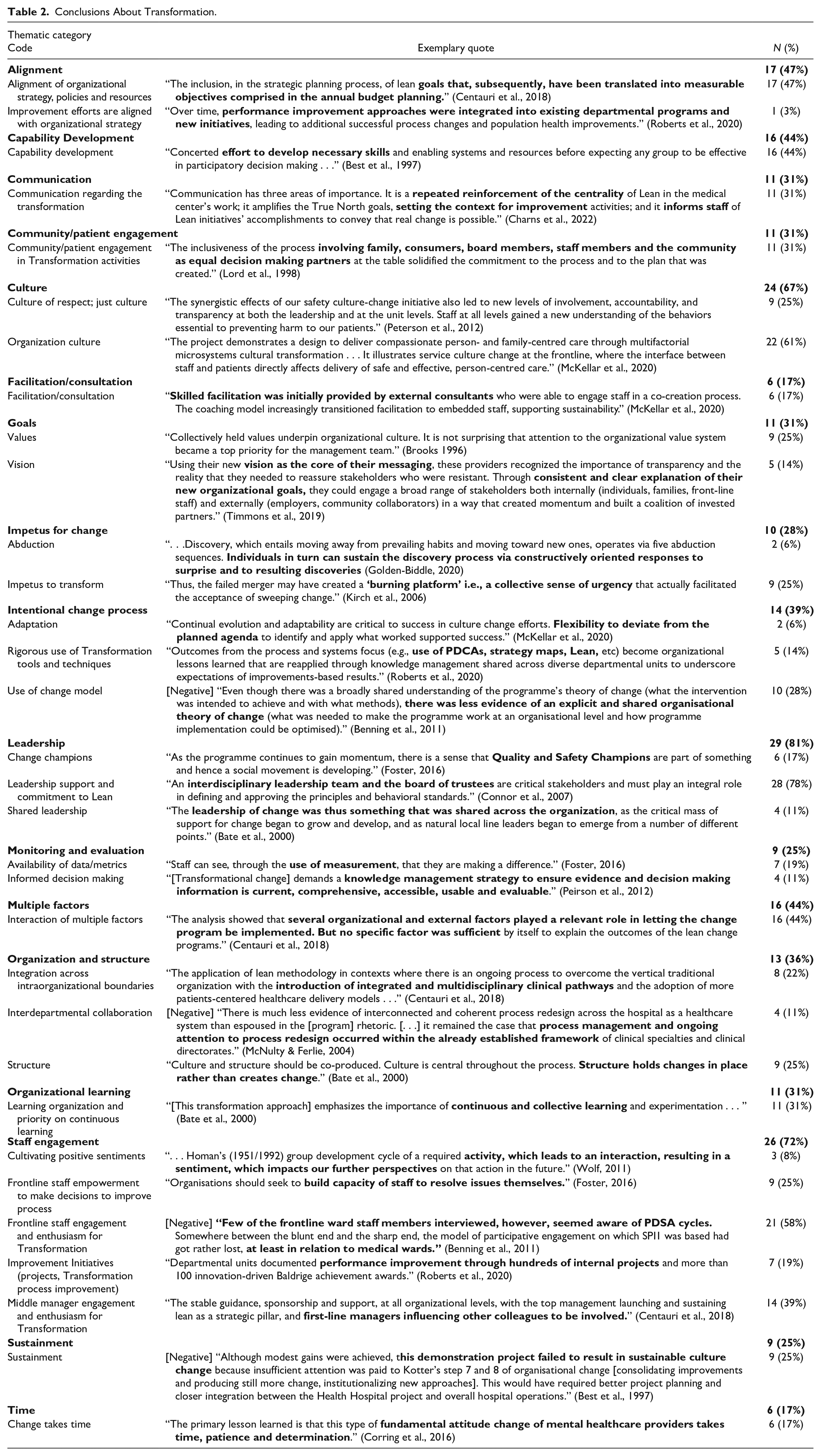
We organized codes into 17 thematic categories to produce a hierarchical coding structure (see Table 2). Categories in the largest number of articles were “Leadership” (29, 81%), “Staff engagement” (26, 72%) and “Culture” (24, 67%). Categories most frequently employed conjointly (i.e., appearing in the same article) were “Leadership” and “Staff Engagement” (23 articles, 64%) (e.g., “leadership walk rounds were intended as opportunities to connect meaningfully with staff, but were perceived as failing to achieve meaningful connection” (Benning et al., 2011, negative example)), “Leadership” and “Culture” (21, 58%) (e.g., “a focus on distributed leadership underpinned with an appreciative inquiry approach was used to promote organizational values” (Kerr et al., 2015)), and “Culture” and “Staff Engagement” (19, 53%) (e.g., “a ‘bottom-up’ approach based on principles of distributed leadership, promoting staff engagement, and encouraging continuous learning contributed to sustained culture change” (McKellar et al., 2020)). Codes from these three categories—“Leadership,” “Staff engagement,” and “Culture”—appeared conjointly in half of the articles. The coded segments revealed thematic relations among the three categories. “
Models Used to Guide Change
Twenty-three articles (64%) used models to guide change. Twenty articles (56%) used a previously published model. The most mentioned model used for change (8, 22%) was a Quality Improvement (QI) model, including Lean, Virginia Mason Production Systems (VMPS, that incorporates Lean); and the Institute for Healthcare Improvement (IHI) change model. Four (11%) used Action Research and an additional article used Transactive Planning, built on Action Research. Seven (19%) articles mentioned a published model not mentioned in any other article (Appreciative Inquiry, Baldrige, HPI, Integrated Knowledge Translation, Kotter, Process Reengineering, TeamSTEPPS) (see Supplementary File 2 for detail and citations to models).
A greater proportion of analytic (12/14, 86%) than descriptive (11/22, 50%) articles used a model for change. The use of models for change increased over time, with 17 of 24 articles (71%) published after 2007 using a model for change, compared to six of 12 (50%) from 1996 to 2007. All (7) studies having seven or more sites used a model, whereas only half of single-site studies (12/23, 52%) used a model for change. Models were used to guide change in a higher proportion of articles with external authors, and in those published in health services research, organization science, and clinical journals.
RQ5: To What Extent Have Transformation Efforts in Health Care as Represented in the Literature Been Successful?
Most articles (23/36, 64%) reported successful transformation, two partial (6%), and six unsuccessful (17%) transformation. Five (14%) studies were multi-site studies designed to compare sites having different levels of success (i.e., “varied success”). After removing these five studies from the calculation, 74% (23/31) of articles reported full success.
The reasons for failure of transformation were diverse. Examples include challenges “achieving full ‘buy-in’ . . . from all staff” (Barba et al., 2021), inability of both staff and community members to overcome traditional power differences in two community-based health and human services organizations (Bess et al., 2009), inability to sustain gains in participatory decision making for staff over 3 years in a hospital (Best et al., 1997), and failure of process reengineering in a hospital, attributed to a prior structural change that had the unintended consequence of incentivizing middle managers not to support the change (McNulty & Ferlie, 2004).
When comparing reported success against different article characteristics, we found differences in reported success by aims (analytic vs. descriptive), authorship, journal, setting, country, use of a model for evaluation, methods, research design, and measures. We did not find differences based on number of sites or use of a model to guide change.
Descriptive articles reported a higher proportion of success (17/22, 77%) and either success or partial success (19/22, 86%) than analytic (6/9, 67%) articles (No analytic articles reported partial success). Articles with exclusively internal authors reported a higher proportion of success (13/16, 81%) and either success or partial success (15/16, 94%) than those with exclusively external authors (8/11, 73%) or both types of authors (2/4, 50%). All articles published in academic medicine (2) and health care quality/safety (6) journals reported successful transformation. A high proportion of articles in clinical journals also reported success (7/9, 78%), as did articles in organization science journals (4/5, 80%). The greatest variation in reported success was in articles in health care management journals (3/7, 43% successful, 2/7, 29% partially successful, 2/7, 29% unsuccessful). Only health services research (2), health care management (1), implementation science (1) and organization science (1) journals published comparative studies with varied success. All studies in academic medical centers (2), specialty institutes (2), and health care systems (1) were successful. Success rates in other settings ranged from 50% to 75%, but small numbers of studies in each setting preclude meaningful comparisons. Small numbers of studies in some countries also preclude meaningful comparisons; however, we note differences among the United States (14/16, 88% successful), the United Kingdom (4/6 67% successful), and Canada (2/5, 40% successful and 1 partially successful, yielding 3/5, 60% either successful or partially successful). Articles not using a model for evaluation (13/16, 81%) reported more success than those that did (10/15, 67%). The highest proportion of success was reported in studies using quantitative methods (9/10, 90%), compared with those using qualitative methods (7/10, 70%) or mixed methods (7/11, 64% successful, 9/11, 82% successful or partially successful). All three studies selecting sites based on measures and two using comparison sites reported success; this contrasts with studies having none of the three features of research design in which five (56%) reported success and six (67%) reported success or partial success. All studies measuring success with external assessment (3), quality/safety measures (6), organizational performance (1), or financial performance (2) reported success. The proportion of studies reporting success was high for those using staff surveys (14/18, 78% successful, 15/18, 83% successful or partially successful). The proportion of success in studies using various qualitative measures ranged from 64% to 80%.
Discussion
Summary of Main Findings
This systematic review identified 36 articles on organizational transformation in health care. A very small percentage of all initially identified articles met our inclusion criteria, primarily because they were not organization-wide or did not provide information on the transformation process, which was an important aim of this review. We also note that for these reasons there was minimal overlap between the articles included in this review and earlier reviews by Best et al. (2012), Lee et al. (2013), and Garritsen et al. (2024).
RQ1: General Characteristics of the Literature on Organizational Transformation
There has been a very modest increase in the number of publications per year starting in 2012. This suggests that despite the growing interest in organizational transformation in health care, it is still under-researched. Although studies were conducted in six countries, most were from the United States, the United Kingdom, and Canada. Consistent with previous reviews, most studies were in hospitals, highlighting a gap in knowledge about transformation in other health care settings.
The literature on transformation is notably fragmented, characterized by the lack of concentration of articles in any particular journal. Furthermore, most studies were single-site, and the foci of transformation varied greatly. Many articles deviated from conventional scientific formats, presenting narrative reflections by senior leaders of the change efforts themselves. While these articles offer valuable insights into leadership perspectives, they may also be biased in their accounts and lack the rigor required for in-depth evaluation of the transformation process and outcomes. In addition, the reported duration of transformation initiatives varied widely, with 25% of the articles reporting periods as short as 2 years or less—a period we consider unrealistic given the complexity of large-scale organizational change. Such studies may either underestimate the success of transformational efforts that are evaluated prematurely before achieving their full potential or be overly optimistic in assessing success or in estimating time required for actual whole organization transformation.
Articles fell into two distinct subsets: analytic and descriptive. This distinction was reflected in the types of journals that publish them and their research methods and measures. Analytic articles applied overall more rigorous designs, and used qualitative methods, whereas descriptive articles were typically weaker in design, relied on quantitative surveys or performance metrics, and were more frequently authored by internal leaders.
RQ2: How Has Organizational Transformation Been Conceptualized and Defined?
Organizational transformation, although not always explicitly labeled as such, was frequently described as a fundamental cultural change or shift in organizational functioning. Only four of 36 articles included definitions of transformation, similar to Garritsen et al.’s (2024) findings. Instead, transformation was often framed within the specific context of each study, without a clear or standardized definition. Also, we found transformation was widely discussed but lacked conceptual clarity, and consistent application of frameworks was limited; this underscores the need for a more cohesive and systematic approach to studying health care transformation.
RQ3: How Has Organizational Transformation Been Studied and Measured?
Many included articles lacked detail in describing their methods and measures, and there was heterogeneity in methods and measures across articles. Studies often had weak research designs. Very few common measures were used across studies. While several studies used surveys to assess culture and staff engagement, most survey measures were unique to their context and not comparable. Similarly, a few studies used quality/safety measures, also unique to the studies. Lack of consistency in measurement makes it challenging to compare results across studies. In addition, measures of quality/safety and of organizational performance are not direct measures of transformation itself. Instead, they are measures that are assumed to be affected by transformation. Ideally, articles would include measures of factors expected to affect transformation (e.g., leadership), measures of transformation (e.g., culture change), and measures of organizational outcomes (e.g., improved patient safety).
To improve the robustness of research on organizational transformation, future studies should consider adopting stronger methodological designs, including longitudinal and mixed-methods approaches that include measurement of factors such as organizational culture and employee engagement before and after (and at times during) the transformation, that can capture the complexity and temporal dynamics of change processes. In addition, using comparison or control sites and embedding realist or process evaluation components can offer insights into how and why transformation efforts succeed or fail in particular contexts. We also suggest that the Higgins et al.’s criterion for use of measures for site selection be broadened to “assessment of sites for site selection” to include methods other than quantitative ones, such as use of expert panels. The use of conceptual models (e.g., Organizational Transformation Model) can help clarify mechanisms and guide both data collection and analysis. For example, studies such as Lukas et al. (2007) and Charns et al. (2022) provide useful examples by combining conceptual models with empirical rigor in the evaluation of large-scale transformation initiatives. Use of conceptual models also provides a vehicle for different studies to build upon each other in reporting empirical findings and for testing relationships comprising the complex dynamics of transformation. Descriptive studies that provide rich description of model constructs and their interrelationships can make important contributions to understanding transformation, much more so than descriptive studies that do not use conceptual models or theories.
RQ4: What Are Dynamics and Factors Important to Organizational Transformation?
Articles’ conclusions about transformation noted “Leadership,” “Staff engagement,” “Culture,” and combinations thereof as central to transformation. Noteworthy is the intertwining of leadership and staff engagement, specifically the focus on distributed leadership across the hierarchy and efforts to enable frontline staff to fully engage with and own transformation efforts. Changing culture is central to most definitions of organizational transformation and is consistent with Pettigrew’s findings that core beliefs are pivotal to how a firm functions and that strategic change, therefore, involves changing these core beliefs (Sminia, 2016). Harrison et al. (2022) also discuss “affective commitment” of staff, that is, “a want or desire to support the change recognising the benefits associated with it.” This conceptually is an extension of “staff engagement.” These three constructs are key elements of the OTM and are consistent with the first of the “five simple rules” from the Best et al. (2012) review: (1) “engage individuals at all levels in the change efforts,” (2) “establish feedback loops,” (3) “attend to history,” (4) “engage physicians,” and (5) “involve patients and families.” Physician engagement was included in several articles but was not explicitly mentioned in articles’ conclusions that we coded. The other “simple rules” were infrequently mentioned.
Our findings differ from the three prior reviews in that few of the included articles mentioned either context or history, whereas Best et al. (2012) specifically included context and history, Lee et al. (2013) included antecedents, and Garritsen et al. (2024) included conditions for transformation. Articles included in our review that did include history or context made clear their effects on transformation, either as a factor that contributed to failure of transformation or as a stimulus, which we coded as “Impetus to transform.”
The inconsistent use of conceptual models to guide and evaluate organizational transformation is an important characterization of this literature. Not only were few models mentioned in more than one article, but also several models that were mentioned are not models of transformation (e.g., IHI QI model, TeamSTEPPS). Based on this review, no particular conceptual model has been shown to be a better representation of the realities of transformation than any other. Future research should address development and testing of models of transformation.
Using the OTM as a framework for coding articles’ conclusions allowed a broad approach to identify factors affecting transformation, as the OTM has a large number of constructs, and we inductively added additional codes. Our findings were largely consistent with the constructs of the OTM, with 19 of 21 OTM constructs coded in more than one article. OTM constructs specific to Lean transformation appeared rarely (e.g., “rigorous use of tools and techniques,” generalized from “rigorous use of Lean tools and techniques”), or never at all (i.e., “use of standard work to increase reliability and decrease variation”) despite our effort to generalize these constructs beyond the Lean context. Beyond the factors of leadership, staff engagement, and culture, we did not find as frequent mention of other factors describing the transformation process. One reason for this is that—despite our inclusion criterion of a description of the transformation process—several articles did not address this well, focusing instead on documenting outcomes without a clear articulation of how transformation unfolded.
RQ5: To What Extent Have Transformation Efforts in Health Care as Represented in the Literature Been Successful?
Most included articles reported positive outcomes of transformation, suggesting that publication bias as represented in this literature is likely. Exceptions were five multi-site comparative studies, designed to compare transformation processes. Successful transformation was more commonly reported in articles that were descriptive, had internal authors, were published in academic medicine, health care quality and safety, clinical and organization science journals, did not use a model for evaluation, and used quantitative methods and measures. Many of these articles concluded transformation was successful based on performance measures rather than direct measures of transformation.
Strengths and Limitations
A limitation of this study is that despite a comprehensive search strategy, it is possible that not all relevant articles were identified. For example, the search did not include books that may have reported on transformation in depth. The primary literature itself has several weaknesses: the lack of detail in many of the included articles, inconsistent structure of articles making it difficult to extract information, and likely a bias toward successful transformation. Despite these limitations, this review also has notable strengths. Our search strategy encompassed both medical and business databases, ensuring a broad scope of the literature. To enhance reliability of our findings, two reviewers conducted every phase of data collection and analysis, discussing discrepancies and referring back to the original sources. We also examined several factors that might be related to bias. In addition, we achieved a more accurate description of studies’ designs by reporting their design features rather than relying on study design labels that are often applied inconsistently in the literature.
Conclusion
This review highlights the pressing need for more rigorous study and detailed description of efforts to transform health care organizations. Despite recognition of the importance of organizational transformation in health care, the literature is fragmented. Gaps identified in prior reviews a decade ago remain. Articles often lacked cohesive frameworks, consistent measures, and rigorous analyses. We strongly advocate that future studies test and build upon published models of transformation. Models provide a structure for accumulation of empirical findings across research studies. We also suggest that future studies include direct measures, such as employee engagement, of the transformation process, as well as rich descriptions of the interaction of factors affecting transformation. The absence of model-building and consistent measurement in this field may be a consequence of the dispersed nature of this literature, spanning a wide range of journals and disciplines. Lack of consistency in use of models and measures are impediments to advancement of research on organizational transformation.
The future of health care depends on our ability to innovate and transform at the organizational level. Rather than investing tremendous resources in the implementation of individual evidence-based practices and isolated quality improvements, organizational transformation efforts are needed to fundamentally shift the culture and way health care organizations function—thereby collectively facilitating introduction of new practices.
Supplemental Material
sj-docx-1-mcr-10.1177_10775587251356130 – Supplemental material for Defining and Measuring Organizational Transformation in Health Care: A Systematic Literature Review
Supplemental material, sj-docx-1-mcr-10.1177_10775587251356130 for Defining and Measuring Organizational Transformation in Health Care: A Systematic Literature Review by Lauren Clack, Jason Smith and Martin Charns in Medical Care Research and Review
Supplemental Material
sj-docx-2-mcr-10.1177_10775587251356130 – Supplemental material for Defining and Measuring Organizational Transformation in Health Care: A Systematic Literature Review
Supplemental material, sj-docx-2-mcr-10.1177_10775587251356130 for Defining and Measuring Organizational Transformation in Health Care: A Systematic Literature Review by Lauren Clack, Jason Smith and Martin Charns in Medical Care Research and Review
Supplemental Material
sj-docx-3-mcr-10.1177_10775587251356130 – Supplemental material for Defining and Measuring Organizational Transformation in Health Care: A Systematic Literature Review
Supplemental material, sj-docx-3-mcr-10.1177_10775587251356130 for Defining and Measuring Organizational Transformation in Health Care: A Systematic Literature Review by Lauren Clack, Jason Smith and Martin Charns in Medical Care Research and Review
Supplemental Material
sj-docx-4-mcr-10.1177_10775587251356130 – Supplemental material for Defining and Measuring Organizational Transformation in Health Care: A Systematic Literature Review
Supplemental material, sj-docx-4-mcr-10.1177_10775587251356130 for Defining and Measuring Organizational Transformation in Health Care: A Systematic Literature Review by Lauren Clack, Jason Smith and Martin Charns in Medical Care Research and Review
Footnotes
Acknowledgements
We would like to thank Justin Benzer and Laura Caci for their critical review and their valuable feedback.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Data Availability Statement
This study is a systematic review of publicly available literature. All data included in the review are available from the cited sources.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
