Abstract
Equitable cancer care in low- and middle-income countries is crucial as mortality rates continue to rise. Artificial intelligence (AI)-powered Virtual Tumor Board Meetings (VTBMs) offer an innovative solution that facilitates real-time collaboration between experts to improve patient outcomes. By integrating AI-powered tools, VTBMs can improve diagnostic accuracy and personalize treatment plans using various data sources such as medical images and genomic profiles. In Pakistan, with limited healthcare resources and a high economic burden, the introduction of AI-powered VTBMs has the potential to revolutionize cancer care. This strategic approach will not only address the current challenges in Pakistan, but also serve as a model for improving cancer care in various developing countries.
Introduction
By 2030, cancer deaths in low and middle-income countries (LMNICs) are expected to rise to 75%, necessitating new strategies. 1 Artificial intelligence (AI) in medical practices has shown substantial promise in improving diagnostic accuracy, treatment planning, and patient outcomes. AI can play a critical role in revolutionizing tumor board meetings (TBM). TBM are integral to the multidisciplinary management of cancer patients, providing a platform for oncologists, radiologists, pathologists, surgeons, and other specialists to discuss complex cases and formulate optimal treatment plans. However, geographical constraints, resource limitations, and scheduling conflicts often hinder the effective conduct of these meetings in Pakistan. Virtual Tumor Board Meetings (VTBMs) can overcome these challenges by enabling real-time collaboration among experts, irrespective of the location.
Artificial intelligence has the potential to transform VTBMs by providing advanced analytical tools and decision support systems. AI algorithms can assist in interpreting medical images, analyzing pathology reports, and predicting treatment outcomes based on historical data. AI can match or exceed the diagnostic performance of human experts in certain scenarios, thus augmenting the decision-making process in tumor boards.
Marginalized cancer patients within Pakistan face significant disparities in accessing chemotherapy and newer targeted agents. A study identified major barriers, including financial constraints and limited availability of advanced treatments, which disproportionately affect the poor. 2 Healthcare should be accessible and equitable; therefore, the development of AI-powered VTBMs could help bridge this critical gap in cancer care. Furthermore, financial constraints prevent many from receiving adequate care. financial toxicity continues to burden many underserved regions in Pakistan. Machine learning models can predict financial distress, helping VTBMs optimize treatment plans and provide financial support. 3 Pakistan’s shortage of medical resources and limited access to healthcare highlights the urgent need for AI-driven systems. Irwin KE et al proposed their thoughts regarding the development of a virtual equity hub by adapting the tumor board model to ensure equitable cancer care for all patients. 4 The article’s primary emphasis on enhancing equity in cancer care through the innovative use of virtual tumor boards is commendable. The key findings highlight the significant disparities in cancer treatment outcomes and the necessity of a more inclusive approach to ensure that all patients, regardless of their socioeconomic background, receive optimal care. We appreciate the authors’ thorough analysis and the proposed model, which leverages digital platforms to facilitate collaboration among specialists and improve access to multidisciplinary care. This model represents a significant step forward in addressing healthcare inequities. However, AI into virtual tumor boards could further augment their effectiveness and efficiency.
AI’s Role in Enhancing VTBMs
AI is not just an enhancement but a necessary evolution to sustain the efficacy of MTBs amidst rising cancer incidences and clinical demands. Its integration fosters a shift toward precision medicine by enabling deep phenotyping of tumors through multi-OMICs analysis and radiogenomics. 5 AI-driven predictive models enhance early detection, stratify patients based on risk, and optimize therapeutic strategies, thus reducing variability in clinical decision-making. Moreover, AI supports integrative care pathways by synthesizing vast datasets, identifying subtle patterns in tumor behavior, and predicting treatment responses with higher accuracy than traditional methods. Such advancements not only accelerate decision-making but also ensure that interventions are tailored to individual patient profiles.
AI is transforming oncology by integrating imaging and pathology with multi-OMICs data to decode molecular mechanisms. 5 The accuracy of tumor grading, molecular characterization and clinical decision-making can be enhanced with the use of AI. A key advancement is the recognition that diagnostic images hold more data than the human eye can perceive. Radiomics enables the extraction of biological insights from imaging in a non-invasive manner, while radiogenomics merges imaging features with genomic data offering a deeper understanding of tumor biology.
Integrative care models play a crucial role in ensuring comprehensive cancer management. AI-driven VTBMs provide a platform for seamlessly integrating diagnostic, treatment, and rehabilitation strategies. By facilitating multidisciplinary collaboration, these AI-powered systems enhance continuity of care, ensuring that patients receive coordinated and efficient treatment throughout their cancer journey.
AI-integrated VTBMs can enhance precision in cancer care by incorporating genomic and lifestyle data into clinical decision-making. By leveraging patient-specific molecular and environmental factors, these systems enable oncologists to design targeted treatment plans that optimize therapeutic efficacy while minimizing adverse effects. This personalized approach represents a significant advancement in oncology, ensuring that treatments align with each patient’s unique disease profile.
Integration of frality assessments into AI-driven recommendations is necessary to help oncologists balance treatment intensity with patient resilence, which in turn improves outcomes for elderly and vulnerable population. Through the prioritization inclusivity, AI powered VTBMs can enhance patient-centered care, ensuring that therapeutic strategies are both effective and compassionate.
Moreover, AI can handle data from various sources, including electronic health records (EHRs), genomic databases, and clinical trial registries. Databases that catalogue somatic mutations’ effects and their clinical implications, such as COSMIC and OncoKB, can be seamlessly integrated with AI algorithms to provide actionable insights during tumor board discussions. 6 This ensures that the recommendations made are not only based on the latest evidence but are also personalized to the patient’s unique genetic profile. However, numerous challenges in integrating AI with genomic databases like COSMIC and OncoKB occur because of the country’s inadequate infrastructure and lack of data availability and technical expertise. However, with systems like Caris that employ AI to link whole-exome sequencing (WES) and whole-transcriptome sequencing (WTS) with clinical data, important insights can be drawn from successful AI applications in oncological data. This approach improves cancer treatment predictions by linking genomic profiles with drug responses. With 455 000 genetic profiles, Caris’ model could potentially be used as a paradigm for adaptation in Pakistan. To overcome the obstacles, government assistance, strategic alliances, and infrastructure investments in the healthcare sector are necessary. Establishing an efficient AI-driven system in Pakistan would entail working with global genetic databases, improving the training of medical personnel, and using public-private partnerships to guarantee the sustainability of AI.
In addition, AI has also shown promising results in employing high-dimensional oncological data for precision medicine. It is found that A1-based methodologies significantly enhance the prediction of immune checkpoint inhibitor efficacy across various cancer types. AI algorithms were found to improve the identification of novel biomarkers and meta-biomarkers by integrating multimodal data, including genomics, radiomics, and digital pathology. Although AI is often met with skepticism, its capability is represented by the AI-driven Smart Virtual Assistant that has successfully automated the extraction and classification of clinical data, achieving an impressive 94% accuracy in patient staging. 7 This high level of precision reduces the risk of human error and ensures comprehensive analysis of complex and heterogeneous patient data.
In Kenya, AI-powered mobile applications have improved the timeliness of cervical cancer screening in rural areas. Similarly, in Ethiopia, machine learning algorithms have been applied to blood smear image analysis, achieving high accuracy in leukemia diagnosis. 8 These cases highlight the transformative role of data science in cancer care across the Global South, offering cost-effective and scalable solutions to critical healthcare challenges. Additionally, the United States Agency for International Development (USAID) has been actively working to bridge the gap by identifying barriers to large-scale AI adoption in LMICs and outlining key strategies to ensure its effective use in improving health outcomes. 9 AI serves as a powerful catalyst for change when implemented effectively, with successful models across the globe showcasing its impact.
Furthermore, AI plays a crucial role in preoperative planning, enabling surgeons to use imaging and patient medical records to design precise surgical treatments. AI optimization algorithms have become essential tools for enhancing the accuracy and efficiency of preoperative planning. 5 Additionally, AI supports decision-making by efficiently retrieving and presenting relevant data.
Beyond early diagnosis, AI has shown significant promise in prognostic prediction and the personalization of cancer therapies. 10 This capability makes AI a viable solution for improving cancer care accessibility in underserved populations. However, a major challenge lies in the safe integration of AI into VTBMs. If successfully implemented, AI-driven VTBMs could be life-changing for cancer patients in resource-limited settings while also reducing the burden on healthcare providers.
AI-Integrated VTBMs in Pakistan: Challenges and Solutions
Cancer incidence and mortality are rising significantly worldwide, highlighting the need for a more efficient and tailored approach, particularly in LMICs. A study by Davis et al demonstrated that implementing virtual multidisciplinary tumor boards (MTBs) led to a 46% increase in physician attendance. 11 Physician involvement is crucial in the successful integration of AI, and combining the two could bring revolutionary advancements in cancer care.
While the benefits outweigh the challenges, the lack of empathy in AI-driven interactions can negatively impact the patient experience, emphasizing the need for human oversight to ensure a compassionate and context-aware healthcare system. Ethical concerns, adaptability, and acceptance remain key challenges; however, with the right approach, these barriers can be addressed and overcome.
Furthermore, it is essential that AI is smoothly incorporated into the clinical workflow, particularly given Pakistan’s varied population and the distinct challenges of language barriers, variable literacy rates, and inequitable access to healthcare. To guarantee the effective use of AI, Juluru et al underlined the significance of real-time monitoring, quality control, and error correction tools. 12 With the use of these tools, physicians can monitor AI decisions, step in when needed, and increase patient trust in AI generated plans. According to their study, real-time corrections improved trust, and 14 radiologists reported that AI improved workflow efficiency. 12 This strategy will establish a feedback loop, allowing physicians to confirm and enhance AI suggestions. As the target population in Pakistan is diverse, seamless communication will be essential. Considering language and literacy barriers, the AI-driven system can be customized to provide a multilingual interface and simplified explanations of treatment options, ensuring patients of all literacy levels can understand their treatment plan. For example, AI tools have the potential to translate clinical recommendations into the regional languages used in Pakistan, such as Urdu, Punjabi, Sindhi and Pashto. This considerably reduces the communication gap, contributing to confidence between clinicians and patients. Furthermore, it is essential that patient feedback is collected through simple surveys and virtual consultations. Instant tools like chatbots can also help gather input quickly. This feedback will be used to adjust AI-based decisions to ensure that care is aligned with patients’ needs and improve their overall experience.
The implementation strategy for establishing VTBMs in Pakistan includes developing robust digital infrastructure for secure video conferencing and data sharing, integrating AI-powered tools for image analysis and treatment predictions, and customizing these solutions to fit the Pakistani healthcare system. Training programs will be conducted for healthcare professionals to effectively use AI tools and participate in VTBMs, promoting continuous education and specialist collaboration. A pilot program will be launched in selected hospitals in Pakistan to assess the feasibility and impact of AI integration in VTBMs. Key criteria for selecting hospitals including varying technical capabilities, regional representation and diverse patient demographics to ensure broad applicability. The pilot program will last 6 to 12 months to allow for extensive data collection and appropriate staff training.
The benefits of VTBMs in Pakistan include enhanced collaboration, increased accessibility, improved decision-making, and cost-effectiveness in cancer care (Figure 1). Implementation Strategy and Benefits of Developing VTBM Using AI in Pakistan.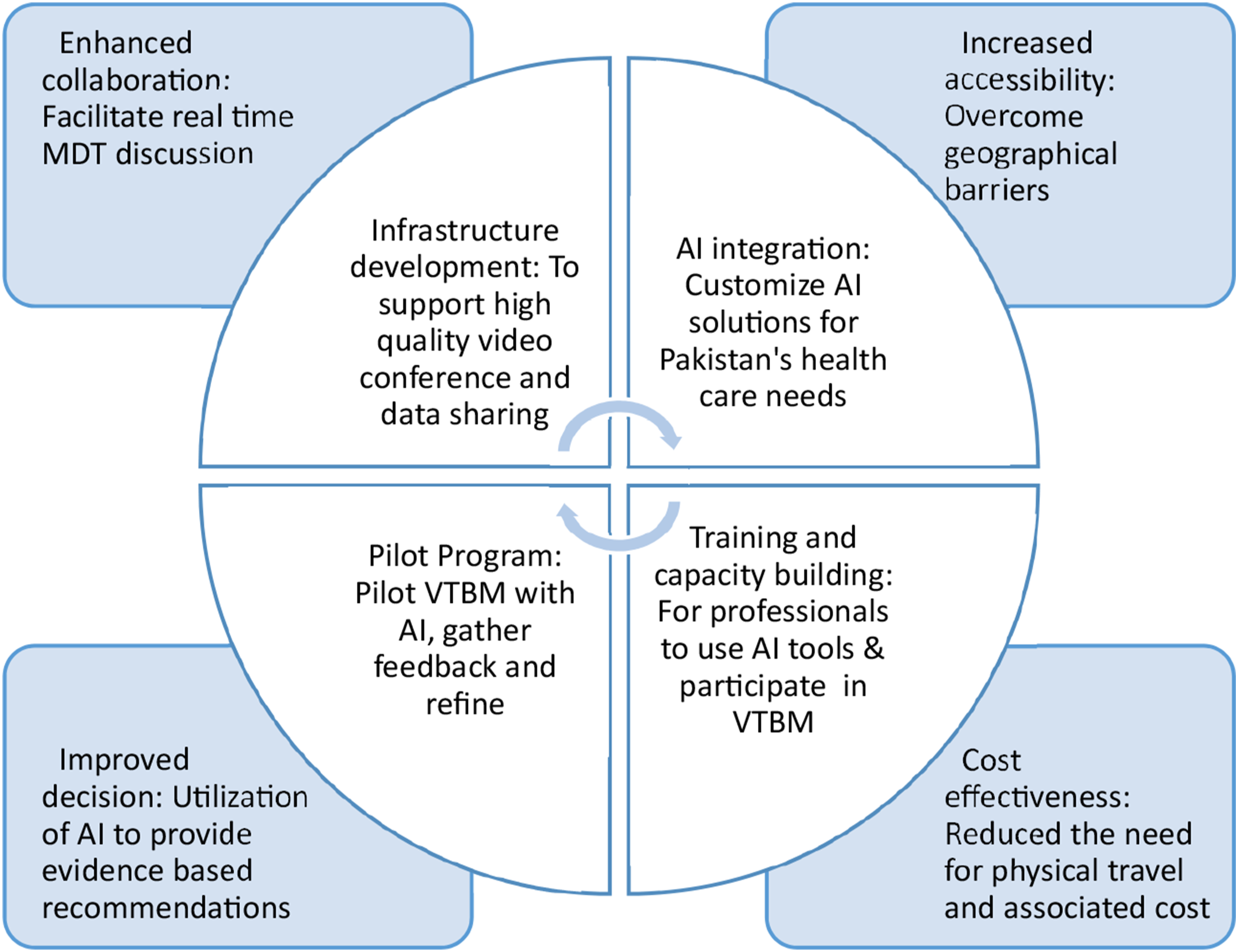
Developing AI-driven VTBMs in Pakistan presents several challenges, including infrastructure limitations, data security and privacy concerns, and the complexity of integrating AI tools into the local healthcare system. Pakistan faces a significant cancer burden, yet its oncology-focused infrastructure remains limited. Unlike developed nations, public hospitals often lack well-established tumor boards, which are essential for multidisciplinary treatment planning. This absence results in fragmented care, making it difficult for patients to receive comprehensive, expert-driven treatment. Integrating AI-driven VTBMs can help bridge this gap by streamlining collaboration among specialists, optimizing treatment recommendations, and ensuring accessibility to expert consultations regardless of geographic constraints. However, with the combined support of the government and private sectors, large-scale implementation becomes feasible. The government can provide regulatory backing and funding, while the private sector can contribute technical expertise and resources. A targeted approach focusing initially on the most prevalent cancers in Pakistan, followed by the gradual inclusion of other cancer types, would enhance adaptability and facilitate the development of a robust database over time. Additionally, Pakistan’s growing tech sector provides a strong foundation to build upon rather than starting from scratch. Moreover, underserved populations in Pakistan are open to adopting new approaches for better healthcare access. Collaborating with basic health units for early diagnosis and integrating AI-driven systems into tertiary hospitals for specialized care can help bridge the gap in cancer treatment and improve patient outcomes nationwide. Training healthcare professionals to use AI tools, managing pilot programs to evaluate feasibility, and adapting technologies to local contexts add further difficulties. Although initial setup costs, such as infrastructure and training, are high, the long-term benefits are significant. AI can reduce hospital visits by improving screening processes, enabling early diagnosis and reducing the need for unnecessary treatment. This efficiency helps reduce financial toxicity, a significant problem in underserved areas of Pakistan. AI has shown to reduce diagnostic time, improve accuracy and lower healthcare costs, ultimately saving institutions money while providing better care.
Furthermore, it is crucial to adopt international standards, such as HL7 (health level 7) and FHIR (Fast Healthcare Interoperability Resources), to address AI-driven VTBMs with the diverse electronic health registry (EHR) system. In Pakistan, many hospitals use non-standard EHR systems, which can cause significant compatibility problems when implementing AI solutions. This challenge is not unique to Pakistan; countries like Germany and China face similar difficulties, and AI systems such as IBM Watson are challenging to integrate with different medical environments and standards. 13 HL7 can help simplify how hospitals share patient data by allowing AI-powered VTBMs to access patient records from different systems without interoperability issues. FHIR, designed for modern web-based data sharing, will enable real-time data exchange between hospitals, improving AI-driven treatment recommendations. To bridge compatibility gaps between older EHR infrastructures and AI-driven platforms, middleware solutions should be deployed to convert non-standard data formats into HL7 or FHIR-compliant structures. Additionally, comprehensive training programs for healthcare IT professionals should focus on the practical implementation of HL7 and FHIR standards to ensure smooth adoption. According to a study conducted in Iran, a minimum data set (MDS) with standardized data elements facilitates uniform data collection and is a fundamental step towards interoperability. Furthermore, the use of SNOMED-CT terminologies can support semantic interoperability in addition to structural interoperability, ensuring that data is not only exchanged but also understood correctly by different systems. 14 This approach, while not specific to Pakistan, is broadly applicable and has been shown to enhance data sharing and reusability in healthcare settings. By implementing the FHIR standard and developing a well-defined MDS. Pakistan can potentially address interoperability issues in its healthcare system, which may enable a more seamless integration of AI-driven technologies like VTBMs, facilitating better patient care and research outcomes.
In addition, it is crucial to address the regulatory and ethical challenges. Pakistan’s current regulatory framework lacks specific guidelines for AI in healthcare, leading to uncertainty regarding approvals, data protection and clinical validation. An AI regulatory system should be developed to eliminate these shortcomings by focusing on clear approval pathways, robust data privacy protection and strict clinical validation to ensure AI’s safe and effective use in oncology. Ethical considerations are also critical, especially concerning AI’s decision-making and patient consent. A human-centered design approach is necessary to create ethical AI systems to ensure bias mitigation, data privacy, and consideration of many different socioeconomic contexts and cultural values entails creation of mechanisms to ensure transparency in obtaining informed consent, security of data, and accountability for AI-driven decisions to instill trust. Furthermore, alternative technologies such as homomorphic encryption, federated learning, and secure multi-party computation offer innovative solutions for secure data management without excessive energy consumption or reliance on traditional blockchain systems. 15 This holistic approach to regulation and ethics is vital for ensuring AI’s responsible and equitable implementation in diverse healthcare settings.
In order to develop an effective pilot program for AI-integrated VTBMs in Pakistan, potential biases in AI algorithms must be addressed. Biases can occur when training data do not adequately represent different populations, leading to differences in diagnosis and treatment. Pakistan has a varied geography, featuring bustling urban centers like Karachi and Lahore alongside rural regions, which can significantly influence healthcare access and outcomes.
To solve this problem, data must be collected from both urban and rural areas to ensure that the training data covers the diverse ethnic, socio-economic and geographic characteristics of the target audience. Multidisciplinary teams must monitor the development process to identify and correct deviations. This team should be involved in everything from hypothesis formation to model implementation and evaluation. Collaborating with local institutions and international organizations can facilitate access to diverse datasets and support the development of inclusive AI models.
The key metrics for evaluating AI algorithms will include diagnostic accuracy, treatment efficacy and patient outcomes. Diagnostic accuracy will be assessed using sensitivity, specificity, positive predictive value (PPV) and negative predictive value (NPV) comparing the AI diagnosis with the comments of local oncology experts.
Treatment effectiveness will be measured by aligning AI and expert advice and tracking clinical outcomes such as progression-free survival (PFS) in Pakistani patients. Patient outcomes, including overall survival (OS) and quality of life (QoL), will be compared between AI-assisted methods and traditional approaches prevalent in the Pakistani healthcare system. Employing quantitative metrics that measure both clinical effectiveness and system efficiency is essential for evaluating the impact of AI in healthcare. Progression-free survival rates (PFS) should be tracked to assess treatment outcomes, ensuring that AI-assisted decisions lead to measurable patient benefits. Diagnostic accuracy, including sensitivity and specificity, must be continuously validated against expert assessments to maintain reliability. Furthermore, the primary goal of AI implementation should be cost-effectiveness; therefore, comparative analyses must demonstrate a reduction in healthcare expenditures without compromising quality. Additionally, monitoring turnaround times for case reviews and physician adoption rates is necessary to identify workflow improvements and user acceptance. Comprehensive data collection is crucial to generating research that evaluates the current AI model’s effectiveness and ensures its applicability to other LMICs.
Long-Term Sustainability and Future of AI in Cancer Care
The FDA has approved various AI-powered medical devices, highlighting the growing role of AI in healthcare. In Pakistan, a strategic method is essential for the sustainability of AI-powered VTBMs. This includes regular AI algorithm updates based on the latest oncological research and the clinical feedback of local experts. In addition, promoting partnerships between hospitals, research institutions, and technology companies can facilitate the exchange of knowledge and resources, ensuring that the tools are effectively integrated into clinical practice. Incorporating AI tools into medical training programs will equip future healthcare professionals with the necessary skills to navigate advanced technologies. This proactive approach improves cancer care and prepares healthcare providers to effectively use AI, ultimately improving patient outcomes across the country.
Footnotes
Statements and Declarations
Author Contributions
AK, AT: Writing, draft the original manuscript, SK: Conceptualization, writing, editing, supervision.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
