Abstract
We developed the Multidimensional Adolescence Anhedonia Scale (MAAS), a novel measure designed to assess not only consummatory and anticipatory, but also recall anhedonia in adolescents. In Study 1 (
Anhedonia, traditionally defined as the loss of interest or pleasure in activities typically enjoyed, is a feature of numerous mental health conditions, ranging from post-traumatic stress disorder to schizophrenia (American Psychiatric Association [APA], 2022). It is also a cardinal symptom of depression, one of the most common mental health conditions in adolescence. In fact, anhedonia has been shown to predict the severity and persistence of adolescent depression, treatment response, and risk for suicidality (Gabbay et al., 2015). Despite this, there remains a paucity of comprehensive measures of anhedonia developed for use in adolescents. Given that adolescence is a unique developmental period with a distinct reward system functioning (Ely et al., 2021), and that experiences of pleasure and motivation differ from those in adults (Hewitt et al., 2023; Watson et al., 2021), there is a need for scales developed with and for this age group. With this aim in mind, we report on the development and validation of a novel, multidimensional measure of anhedonia for use in adolescent populations.
Past work has often framed anhedonia as unitary, emphasizing “loss of pleasure” as central to this experience (Ho & Sommers, 2013). This emphasis on decreased hedonic capacity is reflected in some of the most often used measures of anhedonia, such as the Snaith-Hamilton Pleasure Scale (SHAPS; Snaith et al., 1995). First developed for adult populations, most were designed to measure reduced enjoyment of current rewarding activities or consummatory anhedonia. While important, this definition neglects a growing body of evidence suggesting that anhedonia is a more global and multidimensional construct. For example, the
Multidimensional measures of anhedonia are differentiated in several ways. One of the most common distinctions is temporally based, distinguishing
The disparate outcomes and pathophysiology underlying these differing manifestations of anhedonia underline the importance of measures (e.g., the Anticipatory and Consummatory Interpersonal Pleasure Scale [ACIPS; Gooding et al., 2016]) that distinguish between its temporal phases. Yet, there is also evidence of an additional temporal category of anhedonia related to past experiences of pleasure (i.e.,
Recent work further highlights deficient positive memory recall as both a symptom and a risk factor for adolescent depression. For instance, depressed, at-risk, and healthy adolescents show a gradient of positive memory deficits (Begovic et al., 2017). Such deficits have also been shown to predict adolescent depressive symptoms at 1-month follow-up (Askelund et al., 2019). Screening for those having difficulty retrieving positive memories and experiencing associated pleasure (i.e., recall anhedonia) may help to identify individuals vulnerable to the persistent course of early-onset depression. Yet, to date, no scales have included recall among temporal facets of anhedonia. Rather, the processes underlying impaired recall of positive experiences are typically measured using time-intensive experimental paradigms or tasks that are ill-suited for screening. This underlines the need for measures of recall anhedonia, which might inform both screening efforts and more nuanced understandings of anhedonia in adolescent populations.
To address these gaps, we developed and tested the Multidimensional Adolescent Anhedonia Scale (MAAS) across two separate studies. Given extant correlations among facets of anhedonia, we aimed to develop a scale that could be used both as a composite measure (i.e., with a total score reflecting a general anhedonia construct) and as a multidimensional measure of specific facets of anhedonia. Based on extant literature (e.g., Ho & Sommers, 2013), we defined these facets of adolescent anhedonia as deficient anticipation of future rewards (i.e., anticipatory anhedonia), decreased enjoyment/interest in present activities (i.e., consummatory anhedonia), and difficulty retrieving positive memories and experiencing associated pleasure (i.e., recall anhedonia). Drawing from this definition, we first developed a large pool of items and evaluated their psychometric properties in a split sample of older adolescents in Study 1. After exploring the dimensionality of these items, we confirmed both long and brief versions of the MAAS structure, which were further tested and validated in a younger adolescent sample in Study 2.
Across both studies, we hypothesized that the MAAS would demonstrate good convergent validity, as evidenced by at least moderate correlations with other anhedonia measures. We also predicted that the MAAS would show good concurrent and discriminant validity, as shown by stronger correlations with measures of psychopathology for which anhedonia is a core symptom (i.e., depression; APA, 2022) compared with disorders for which it is not (i.e., anxiety, disordered eating). Furthermore, we anticipated stronger correlations of the MAAS with constructs closely linked to reward processing (i.e., positive affect, reward responsiveness), compared with those less closely related (i.e., negative affect, behavioral inhibition, impulsive approach; Carver & White, 1994; Watson et al., 1988). Finally, we expected that the MAAS would demonstrate incremental validity by more strongly predicting depressive status (high vs. low depressive symptoms) than other measures of anhedonia (Study 1), and predictive validity by predicting depressive status at 6-month follow-up (Study 2).
Study 1 Methods
Item Development
The initial items for the MAAS were created using the sequential system of test construction (Jackson, 1970). We first developed an operational definition of anhedonia based on a comprehensive literature search on the presentation and experience of anhedonia in adolescents. This operational definition was informed by Ho and Sommers’s (2013) proposed chronological framework of anhedonia and consultations with clinicians specializing in adolescent psychopathology. We then trained a group of experienced research assistants and graduate students in item-writing. They were subsequently provided with the operational definition of anhedonia in adolescence and wrote an approximately equal number of items for each of the anhedonia dimensions: recall, consummatory, and anticipatory. Within each subconstruct of anhedonia, an approximately equal number of items were also written to capture both total loss of pleasure (e.g., “I don’t feel excited about anything anymore”), dampened experience of pleasure (e.g., “I don’t feel as excited about things as before”), and lessened duration of pleasure (e.g., “I get bored faster than I used to”). This was done to more comprehensively capture differing experiences of anhedonia, which may range in degree and severity. Moreover, item writers included items describing pleasure in specific domains (i.e., relationships, school/employment, hobbies/activities, food/drinks) as well as pleasure experienced more broadly.
Importantly, items were also written to be relevant to adolescent interests, activities, and experiences. For example, domain-specific items focused primarily on school, friends, and family, as opposed to work, romantic relationships, or experiences traditionally pleasurable to adults (e.g., the sound of crackling wood in the fireplace) that have been used in previous measures (e.g., the SHAPS; Snaith et al., 1995; the Temporal Experience of Pleasure Scale [TEPS]; Gard et al., 2006). Adolescent-specific experiences of anhedonia were also captured by items describing feelings such as boredom, a common manifestation of decreased pleasure during this time (Spaeth et al., 2015). Additional items reflected salient developmental themes related to adolescence, such as “growing up” or planning for the future. Efforts were also made to limit the reading level of items to ensure they could be easily understood by younger and older adolescents. We further aimed to limit the content to anhedonia rather than other related but less central constructs (e.g., effort, connection), or constructs related to depression (e.g., low mood, self-esteem). This resulted in a total of 575 items developed by the item-writers, of which 122 were selected by study authors after duplicates, double-barreled items, and items that did not reflect the intended construct were removed, in consultation with clinicians specializing in adolescent psychopathology. At this stage, a decision was also made to focus on items describing anhedonia experienced more broadly, rather than within specific domains (e.g., relationships), to facilitate use of the measure with both younger and older adolescents. Below, we report how we determined our sample size, all data exclusions, all manipulations, and all measures in the study.
Participants
In total, 701 older adolescents residing in Canada were recruited from university classrooms and participated in this study in 2020. Participants were excluded if they withdrew consent to participate (
Sample Characteristics.

Additional identities in Study 1 include Chinese-Filipino, Chinese-South-East Asian, East-Indian-South-East Asian, Black-Chinese-White, Black-Middle Eastern, Chinese-East Indian-White, Chinese-Filipino-White, Chinese-Japanese-White, Chinese-Middle Eastern-White, Chinese-South Asian, East Indian-South East Asian, Filipino-Indigenous, Filipino-South East Asian, and Japanese-Korean. bAdditional identities in Study 2 include Chinese-Filipino, Chinese-South-East Asian, Black-Hispanic, Chinese-Japanese, Chinese-Central Asian-Jewish, East Indian-Middle Eastern-White-Jewish, East Indian-South Asian-White, Hispanic-White-Taiwanese, Middle Eastern-South Asian-West Asian, Chinese-Vietnamese-British, Indian-Caucasian, and White-Mayan Indian.
Procedures
Approval from the Institutional Research Ethics Board was obtained before recruitment. Participants provided consent, after which they completed a 1-hour online survey that included a demographic questionnaire, 122 anhedonia items developed by the research team, and several questionnaires assessing convergent, discriminant, and concurrent validity of these items.
Measures
MAAS Item Pool
The 122 self-report items developed and selected by the research team were presented individually to participants. Participants rated the past 2-week frequency of each item on a 5-point Likert-type scale (from 1 =
Convergent Validity
Convergent validity of the MAAS was assessed via associations with additional measures of anhedonia. The SHAPS (Snaith et al., 1995) is a 14-item self-report measure assessing pleasurable experiences in the past few days. Items capture pleasurable experiences relating to interests and pastimes, social activities, sensory experiences, and food and drink. Higher scores reflect higher levels of anhedonia. Good to acceptable internal consistency was demonstrated across Subsamples A and B, α = .78–.86.
The Dimensional Anhedonia Rating Scale (DARS; Rizvi et al., 2015) is a 17-item self-report measure that assesses anhedonia in four domains (social activities, pastimes/hobbies, sensory experiences, and food/drinks). Participants gave examples of enjoyed activities in each category and then rated desire, motivation, effort, and consummatory pleasure for the examples provided, with higher scores indicating
The Anticipatory and Consummatory Interpersonal Pleasure Scale-Adolescent (ACIPS-A; Gooding et al., 2016) is a 17-item self-report measure that assesses consummatory and anticipatory anhedonia in the social domain (Gooding et al., 2016), with higher scores indicating
Concurrent and Discriminant Validity
Concurrent and discriminant validity of the MAAS was assessed by examining associations with measures assessing related constructs (i.e., depression, positive affect, reward responsiveness) relative to less-related constructs (i.e., anxiety, negative affect, behavioral inhibition, and impulsivity-related behavioral approach). The Center for Epidemiological Studies Depression Scale for Children (CES-DC; Faulstich et al., 1986) is a 20-item self-report measure of depressive symptom frequency for children and adolescents. Higher scores indicate greater depressive symptom severity. The CES-DC demonstrated excellent internal consistency (α = .91) across both subsamples.
The Generalized Anxiety Disorder-7 (GAD-7; Spitzer et al., 2006) is a 7-item self-report measure of generalized anxiety disorder symptoms, where higher scores indicate
The Positive and Negative Affect Scale (PANAS; Watson et al., 1988) is a 20-item self-report measure that assesses past-week positive and negative affect, each captured by 10 items. The PANAS Positive affect subscale, α = .88–.89, and the PANAS Negative affect subscale, α = .87–.89, both demonstrated good internal consistency across both subsamples.
The Behavioral Inhibition and Activation System scale (BIS-BAS; Carver & White, 1994) is a 24-item self-report questionnaire designed to measure two motivational systems: behavioral approach (BAS) and behavioral inhibition (BIS). The BAS comprises three subscales assessing motivation to follow one’s goals (BAS-Drive), impulsivity-related behavioral approach toward novel environmental rewards (BAS-Fun Seeking), and sensitivity to pleasant reinforcers in the environment (BAS-Reward Responsiveness). Higher scores indicate greater behavioral activation. The BAS demonstrated good to acceptable internal consistency across all subsamples (BAS-Drive: α = .77–.81; BAS-Fun: α = .73; BAS-Reward: α = .75–.76), although estimates for the BAS-Fun subscale fell slightly below a cut-off of .70 in Subsample A (α = .66). The Behavioral Inhibition Scale (BIS; Carver & White, 1994) assesses motivation to avoid aversive outcomes, with higher scores indicating greater behavioral inhibition. The BIS demonstrated good to acceptable internal consistency across both subsamples, α = .74–.82.
Data Analytics Plan
Exploring the Factor Structure
Subsample A (
Confirming the Factor Structure
Subsample B (
Although longer versions of a scale may be useful by allowing for more diverse content coverage across the full breadth of a construct while maximizing reliability, we also aimed to develop a brief version to increase MAAS accessibility in contexts with time constraints (e.g., clinical settings; Groth-Marnat, 2009). Thus, separate CFA analyses were undertaken using Subsample B to (a) confirm the structure of the 24-item version from subsample A, and (b) further eliminate items using psychometric information (e.g., factor loadings, impact on reliability coefficients and factor analysis fit indices) as well as conceptual criteria (i.e., removing similar or redundant items while still capturing content breadth), resulting in a brief version of the scale. In doing so, we adhered to current recommendations for short-form measure development where appropriate (e.g., Smith et al., 2000).
Internal Consistency, Reliability, and Validity
To assess internal consistency, we calculated Cronbach’s alpha (α) and McDonald’s omega (ω) using the
Study 1 Results
EFA in Subsample A
The factor structure of the draft 122-item questionnaire was first explored in Subsample A. After first examining inter-item correlation matrices, we removed 3 items with consistently very high (more than 10
Preliminary Exploration of the Factor Structure and Item Reduction
A parallel analysis (Horn, 1965) was first conducted, suggesting four factors be retained. This output was compared with the scree plot of actual and simulated eigenvalues, which displayed one large factor and a break after four factors for the actual data, with four factors clearly visible above the line for simulated data (see Supplemental Figure 1). Thus, a PAF with an Oblique Promax Rotation (due to correlations between factors; de Winter & Dodou, 2011) was run with the four-factor solution explored. The solution produced was theoretically salient, with factors representing consummatory anhedonia (e.g., “
Importantly, items were also removed with content validity in mind to ensure items representing key aspects of conceptual content were retained (Flora & Flake, 2017). For example, items in the recall anhedonia subscale retained content that captured both a lack of pleasure upon recall and deficient recall of positive emotions or experiences using multiple positive emotion descriptors (e.g., enjoyment, excitement). Items in the anticipatory anhedonia subscale likewise included content referring to both a total loss and a decrease in the duration or intensity of positive emotions (e.g., excitement, enjoyment), as well as increased boredom when anticipating future events. The consummatory anhedonia subscale further included items capturing loss or change in the duration or intensity of interest, excitement, and enjoyment, as well as boredom. This resulted in a total of 24 items being included for further exploration, reflecting consummatory (8 items), anticipatory (8 items), and recalled (8 items) dimensions of anhedonia (see Table 2; see Supplemental Table 2).
Factor Loadings for the 24-item MAAS Three-Factor Solution.
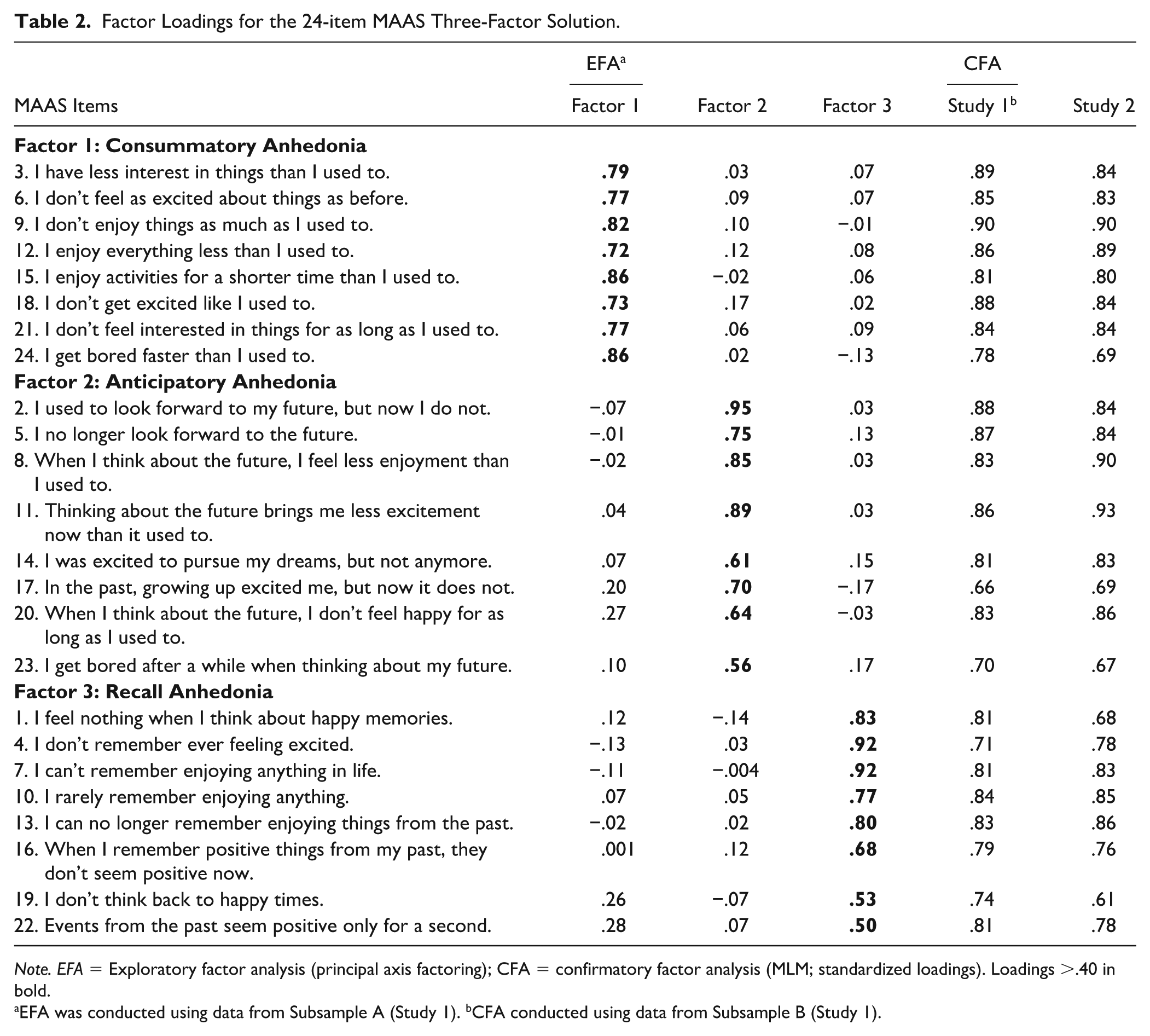
EFA was conducted using data from Subsample A (Study 1). bCFA conducted using data from Subsample B (Study 1).
Further Evaluation of the Factor Structure
Parallel analysis and the scree plot of actual and simulated eigenvalues were re-run with the remaining 24 items (see Supplemental Figure 2). All methods identified a three-factor solution, which was re-examined using PAF with Promax rotation. The three-factor solution resulted in a theoretically meaningful distinction between the anticipatory, consummatory, and recalled dimensions of anhedonia. All items loaded > .40 onto a principal factor and cross-loaded < .30 on other factors (see Table 2). Fit indices were good, TLI = .96, RMSEA = .06, with 70% of the variance explained. Factor correlations were
Confirming the Factor Structure in Subsample B
The factor structure identified in Subsample A was confirmed in participants randomly selected for Subsample B (
24-Item MAAS
Given the strong correlation between factors in the previous analysis (
12-Item MAAS
After confirming the factor structure of the 24 items selected in analyses for Subsample A (see Supplemental Table 2), we aimed to establish a brief 12-item version of the measure by testing additional CFA models. As mentioned above, we considered both psychometric performance (i.e., factor loadings, impact on fit index values within factor analyses, impact on reliability coefficients) and the extent to which items captured content breadth mentioned above while limiting redundancy. Items with more similar wording or content within the same subscale were first identified and then removed iteratively to examine which had the greatest benefit for psychometric performance. For example, items 7, 10, and 13 each referenced difficulty recalling past enjoyment, and so the latter item was retained because it yielded the best fit indices and reliability metrics. Items with relatively larger correlated residuals, within- and across-scales, were also considered for removal. 3 For example, items 7 and 23 had a residual correlation of .12 and their inclusion had less impact on psychometric performance, and were similar to other items; thus, these items were removed. This process continued until an initial 12-item set was selected via consultation between the first, second, third, and last authors and then proposed and agreed to by the remaining authors.
The 12 items chosen maximized selection criteria and were used to confirm the three-factor structure previously demonstrated by the 24-item version of the measure. Factor loadings for these items are presented in Supplemental Table 3. The three-factor CFA conducted using the 12 items selected for further analysis demonstrated excellent fit to the data (robust TLI and CFI = .98, robust RMSEA = .06, 90% CI [.03, .08], SRMR = .03). Factor correlations were
Internal Consistency
Both the 24- and 12-item versions of the MAAS demonstrated strong internal consistency across Subsamples A and B: MAAS-24 Total α = .97–.97, ω = .97–.97; MAAS-12 Total α = .94–.94, ω = .94–.95 (see Supplemental Table 4). The same was true of recall, anticipatory, and consummatory subscales across subsamples and scale versions (MAAS-24: α = .93–.96; ω = .93–.96, MAAS-12: α = .86–.91; ω = .88–.91). Item correlation matrices are presented in Supplemental Table 5.
Convergent Validity
As expected, the MAAS-24 total score was significantly and moderately correlated with all other measures of anhedonia, with minimal differences in the strength of correlations demonstrated across Subsamples A and B (see Table 3). The MAAS-24 Anticipatory subscale was slightly more strongly correlated with the ACIPS-A Anticipatory relative to the Consummatory subscale. However, the MAAS-24 Consummatory subscale was not more strongly correlated with the ACIPS-A Consummatory relative to the Anticipatory subscale. For brevity, convergent validity correlations for the MAAS-12 are reported in detail in Supplemental Table 6. However, the same pattern of results was demonstrated, with the difference in strength of correlations between the MAAS-24 and MAAS-12 ranging from −.04 to +.06 across all samples and subscales. Correlations among convergent, concurrent, and discriminant measures are presented in Supplemental Table 7.
Bivariate Spearman’s Correlations of the MAAS-24 with Convergent Validity Measures Across Studies 1 (Subsamples A and B) and 2.
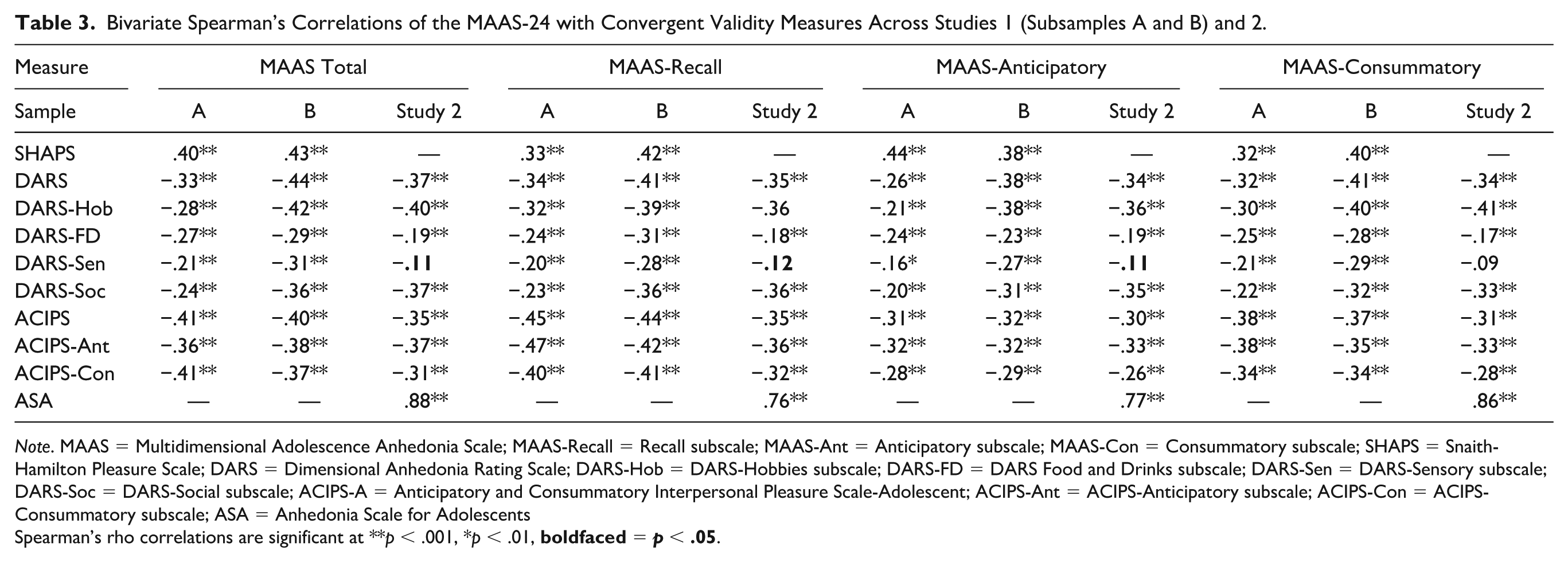
Spearman’s rho correlations are significant at **
Concurrent and Discriminant Validity
The MAAS-24 total score correlated strongly with depression (i.e., CES-DC) and moderately with anxiety (i.e., GAD-7) across Subsamples A and B (see Table 4). Consistent with hypotheses, there was also a significant difference in the strength of these associations,
Bivariate Spearman’s Correlations of the MAAS-24 with Concurrent and Discriminant Measures Across Studies 1 (Subsamples A and B) and 2.
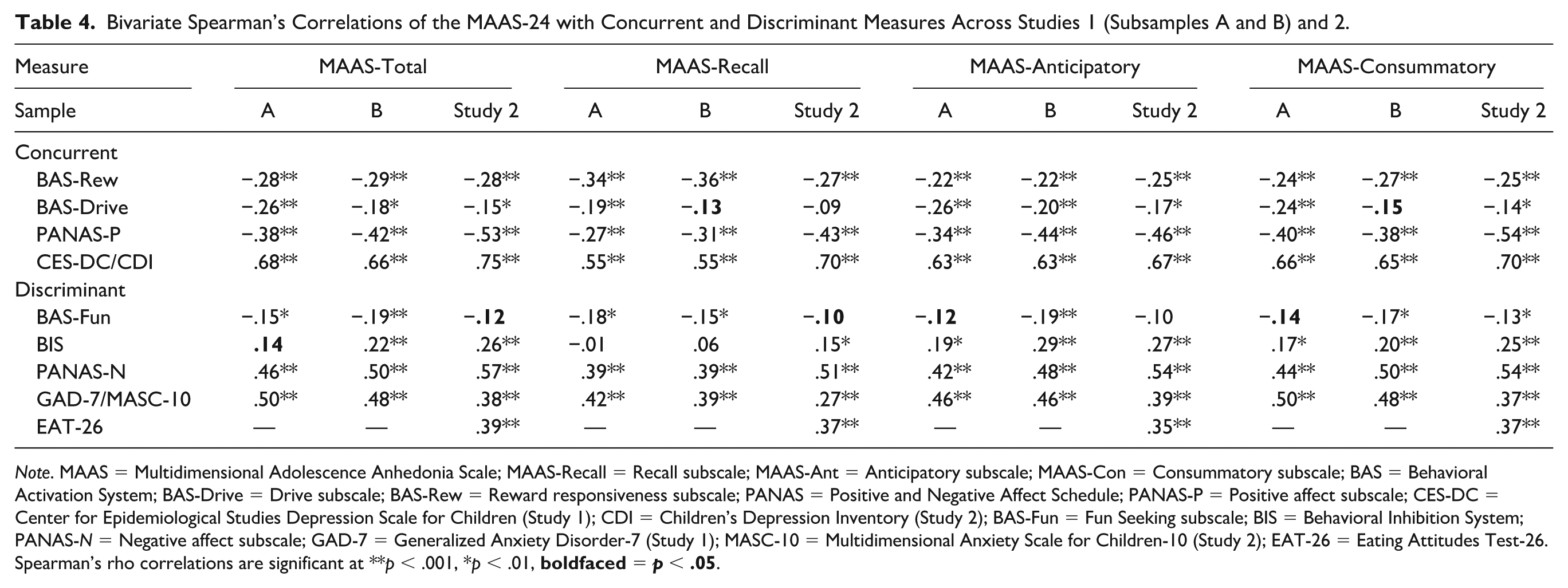
Spearman’s rho correlations are significant at **
Next, small correlations were demonstrated between the MAAS-24 total, anticipatory, and consummatory scores and personality traits of reward responsiveness (i.e., BAS-Reward), with moderate correlations found for the MAAS-24 Recall subscale (see Table 4). There were also small correlations between the MAAS-24 and other traits relating to behavioral approach (i.e., BAS-Drive, BAS-Fun) and inhibition (i.e., BIS). Importantly, associations across subsamples were significantly (or marginally) stronger for reward responsiveness relative to impulsive approach,
Incremental Validity
A series of hierarchical linear regressions tested whether the MAAS-24 (and MAAS-12) better predicted depressive symptoms (i.e., CES-DC scores) relative to other measures of anhedonia (i.e., the ACIPS-A, SHAPS, and DARS total scores) across Subsample B.
4
Across all models, entering the MAAS-24 or MAAS-12 total scores as a predictor in Step 2 significantly improved model fit and prediction of depressive symptoms (all
Study 1 Hierarchical Linear Regressions Predicting Depressive Symptoms from MAAS-24 and Convergent Measures of Anhedonia (Subsample B).
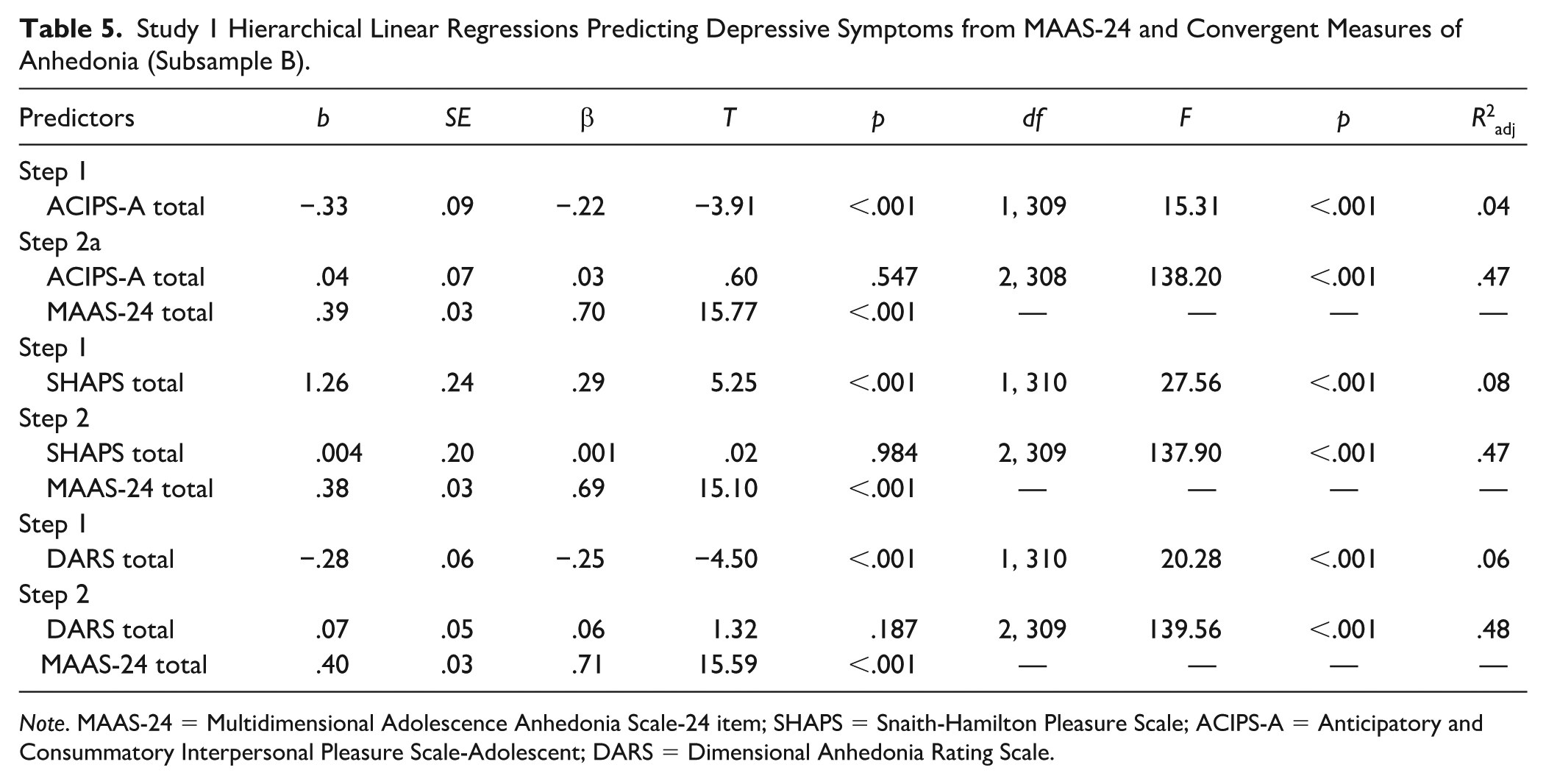
Study 2
To further assess the structure, validity, and reliability of the MAAS-24 and MAAS-12 in a sample of a greater range in age, we recruited a broader online sample of adolescents from across North America. We also aimed to establish test–retest reliability, rank order stability, and predictive validity by administering a 6-month follow-up survey.
Study 2 Method
Participants
Participants between 12 and 19 years old were recruited from Canada and the United States through social media advertisements in 2021. Although 493 participants completed the study, we excluded those younger than 12 or older than 19 years at the time of completing the first survey (or who did not report a valid birthdate;
Procedures
Approval from the Institutional Research Ethics Board was obtained before recruitment. Participants younger than 16 years old provided assent (after parental consent was obtained), and participants older than 16 provided consent before participation. Adolescents then completed an online survey consisting of a demographic questionnaire, the MAAS items, and measures of convergent, discriminant, and concurrent validity. Participants were also invited to complete the same survey 6 months later in return for a $10 gift card.
Measures
Multidimensional Adolescence Anhedonia Scale
The MAAS-24 and MAAS-12 self-report measures of anhedonia assessed three separate dimensions of anhedonia: anticipatory, consummatory, and recall (see Supplemental Table 2). Participants rated how often they experienced each item in the past 2 weeks on a 5-point Likert-type scale ranging from
Convergent Validity
We assessed convergent validity using alternative measures of anhedonia, including the DARS (Rizvi et al., 2015) and ACIPS-A (Gooding et al., 2016), with good to acceptable internal consistency observed in this sample: DARS total score, α = .88; DARS individual subscales, α = .76–.89; ACIPS-A, α = .87; ACIPS-A individual subscales, α = .70–.80. We also administered the Anhedonia Scale for Adolescents (ASA; Watson et al., 2021), which was published after Study 1 was completed. The ASA is a 14-item multifaceted measure of past 2-week anhedonia with three subscales capturing various associated experiences, such as flattening of emotion and loss of pleasure and joy, lack of motivation or effort, and loss of connection, purpose, and belonging. Higher scores indicate
Concurrent and Discriminant Validity
As in Study 1, concurrent and discriminant validity were assessed by examining associations with measures assessing related constructs (i.e., positive affect; PANAS-Positive [Watson et al., 1988], pleasure; BAS-Reward Responsiveness [Carver & White, 1994], motivation; BAS-Drive) relative to unrelated or less-related constructs (i.e., negative affect; PANAS-Negative [Watson et al., 1988], impulsive approach; BAS-Fun Seeking [Carver & White, 1994], and behavioral inhibition; BIS). All showed excellent to acceptable internal consistency: PANAS-Positive, α = .87; PANAS-Negative, α = .87; BAS-Drive, α = .75; BIS, α = .80, apart from the BAS-Fun (α = .63) and BAS-Reward (α = .68) subscales, which fell below an established cutoff of .70.
We also assessed concurrent validity with an alternative measure of depression, the Children’s Depression Inventory-Short (CDI; Kovacs, 1978), given its prevalence in the literature. The CDI is a 10-item self-report measure of children and adolescents’ experience of depression in the past 2 weeks, where higher scores indicate
Moreover, discriminant validity was further assessed with age-appropriate measures of anxiety (i.e., Multidimensional Anxiety Scale for Children [MASC-10; March et al., 1997]) and disordered eating (i.e., Eating Attitudes Test [EAT-26; Garner et al., 1982]). The MASC-10 is a 10-item self-report measure of anxiety for children and adolescents, with higher scores indicating more frequent anxiety symptoms (March et al., 1997). The MASC-10 demonstrated acceptable internal consistency in this sample, α = .74. The EAT-26 is a 26-item self-report measure that assesses disordered eating behaviors and cognitions. Higher scores indicate
Data Analytics Plan
Analyses were conducted using R 4.3.0 (R Core Team, 2023). We specified CFA models with maximum likelihood estimation, and Satorra-Bentler scaled chi-square test statistic and robust standard errors to test the factor structure using the
Internal Consistency, Reliability, and Validity
Cronbach’s α and McDonald’s ω were calculated using the
Study 2 Results
Preliminary Analyses
Participants’ characteristics are summarized in Table 1 (and Supplemental Table 1). The MAAS-24 and MAAS-12 were significantly associated with age, such that higher scores were associated with being older, MAAS-24:
Confirmatory Factor Analysis
MAAS-24
We next confirmed the factor structure identified in Study 1, again using CFA with maximum likelihood estimation and robust model fit indices. As before, the KMO (.97) and Bartlett’s test of sphericity (
MAAS-12
The unidimensional CFA model based on ratings for the 12-item measure demonstrated mediocre fit across multiple indices, robust CFI = .84, robust TLI = .81, robust RMSEA = .16, 90% CI = [.15, .18], SRMR = .07. However, fit was again improved by fitting the three-factor CFA model, robust CFI = .98, robust TLI = .97, robust RMSEA = .06, 90% CI = [.05, .08], and SRMR = .03. Here, the largest standardized residual was no greater than 0.10 for the covariance between Item 1 and Item 5 (see Supplemental Table 3). Moreover, standardized factor loadings ranged from .67 to .94. Factor correlations were
Reliability
Internal Consistency Reliability
The MAAS-24 and MAAS-12 scores had strong internal consistency at baseline and 6-month follow-up (α = .97–.97, ω = .97–.97; MAAS-12 Total α = .93–.94, ω = .93–.94 [see Supplemental Table 4]). The same was true of recall, anticipatory, and consummatory subscales (MAAS-24: α = .92–.95, ω = .92–.95; MAAS-12: α = .83–.93, ω = .83–.93). Item correlation matrices are presented in Supplemental Table 10.
Test–Retest Reliability
All participants were invited to complete the MAAS again approximately 6 months after the initial survey. Of these, a subset (
Rank-Order Stability
To supplement our analyses examining absolute stability of MAAS scores from baseline to 6-month follow-up, we additionally examined relative or rank order stability among the MAAS subscales. As expected, we found that baseline MAAS Recall scores were more strongly correlated with Recall at follow-up, MAAS-24:
Convergent Validity
As in Study 1, the MAAS-24 total was significantly and moderately correlated with the DARS and ACIPS-A (see Table 3). The MAAS-24 Anticipatory subscale was also more strongly correlated with the ACIPS-A Anticipatory, relative to the ACIPS-A Consummatory subscale, although the reverse pattern did not emerge for the MAAS-24 Consummatory subscale. For the ASA, on the other hand, strong correlations were observed with the MAAS-24 total score. Validity correlations for the MAAS-12 are reported in detail in Supplemental Table 6. However, the same pattern of results was demonstrated, with the difference in strength of correlations between the MAAS-24 and MAAS-12 ranging from 0 to +.03 across subscales. Correlations among convergent, concurrent, and discriminant measures are presented in Supplemental Table 11.
Concurrent and Discriminant Validity
The MAAS-24 total score correlated strongly with depression (i.e., CDI), and moderately with anxiety (i.e., MASC-10) and disordered eating (i.e., EAT-26; see Table 4). As hypothesized, it was also more strongly correlated with depression (i.e., CDI) relative to anxiety (i.e., MASC-10),
Next, as in Study 1, small correlations were demonstrated between the MAAS-24 total score and measures of reward responsiveness (i.e., BAS-Reward) and other personality traits of behavioral approach and inhibition (i.e., BAS-Drive, BAS-Fun, BIS). The MAAS-24 total score remained more strongly correlated with reward responsiveness (i.e., BAS-Reward) compared to impulsive approach (i.e., BAS-Fun),
Predictive Validity
To assess the predictive validity of the MAAS in those who completed the follow-up surveys (
Discussion
This study aimed to develop and validate a multidimensional measure of anhedonia that assesses not only consummatory and anticipatory but also
MAAS items loaded onto separate factors capturing loss of interest/enjoyment and boredom (i.e., consummatory anhedonia), decreased future-oriented anticipation (i.e., anticipatory anhedonia), and difficulty remembering positive experiences or experiencing associated positive emotions (i.e., recall anhedonia). Perhaps due to the domain-general phrasing of items, it was significantly but moderately correlated with other measures such as the DARS, which focuses on mostly consummatory pleasure across specific domains (e.g., food/drinks; Rizvi et al., 2015). The MAAS total score was also moderately correlated with the ACIPS-A, with the strongest support for convergence between the MAAS and ACIPS-A anticipatory subscales. Although results yielded less consistent support for the convergence of the MAAS consummatory subscale, it should be noted that factor analyses of the ACIPS-A items have not consistently distinguished temporal dimensions of interpersonal pleasure (Gooding & Pflum, 2014; Gooding et al., 2016). Our findings should be interpreted with this drawback in mind and might be further explored in work that adopts disparate (e.g., task-based) measures of anticipatory and consummatory anhedonia. On the other hand, the MAAS total score showed the strongest convergence with the ASA (Watson et al., 2021), of which there was some overlap with its indicators. For example, the ASA also included items measuring loss of overall enjoyment (e.g., “
Although not otherwise captured by existing scales, impaired recall of positive experiences has been well-documented in both depression and other forms of psychopathology characterized by anhedonia (APA, 2022; Werner-Seidler & Moulds, 2011). Both concurrent and prospective associations found here are also consistent with previous findings that positive memory deficits reflected in recall anhedonia are both symptomatic and predictive of adolescent depression (Askelund et al., 2019; Begovic et al., 2017). In fact, recall anhedonia explained unique prospective variance in depression (i.e., when controlling for anticipatory and consummatory anhedonia), emphasizing its importance as an early warning sign in this regard. Whereas positive memories and their associated emotions may confer resilience (e.g., by facilitating emotional recovery from stress; Tugade & Fredrickson, 2004), difficulties with recall may strengthen the depressogenic effects of stressors common in adolescence. Recall difficulties are also linked to various other risk factors for adolescent depression (e.g., negative self-cognitions; Askelund et al., 2019) and may give rise to other temporal facets of anhedonia. For example, anticipating future experiences of pleasure is likely to rely on recalling past experiences. Correspondingly, our subscales were distinguishable (e.g., in factor analyses) yet strongly correlated. This supports positive memory recall as a focus of prior interventions targeting anticipatory anhedonia (and depression) in adults (Hallford et al., 2024). The MAAS may be used to identify adolescents who may benefit most from such interventions.
Additional evidence for concurrent and discriminant validity of the recall and other subscales supports the utility of the MAAS for this purpose. For example, scores on the recall and anticipatory subscales at Time 1 were most strongly correlated with respective scores at follow-up in Study 2, relative to other subscales. Although this was less apparent for consummatory anhedonia, all subscales explained unique variance in concurrent depression in Study 1. This suggests differential associations with aspects of depression (or other aspects of psychopathology characterized by anhedonia), which might be explored using the MAAS in future research. Moreover, while the MAAS total score was more strongly correlated with depression than other measures of psychopathology, these differences were especially apparent for the recall anhedonia subscale. This may have been due to its comparatively weaker association with anxiety. One possible explanation is that mental representations of past positive experiences are less accessible to the kind of future-oriented worry that often characterizes anxiety. The MAAS recall subscale can be used to test this prospect in future work.
Relatedly, there were small and often nonsignificant correlations of the MAAS recall with the BIS, a measure of behavioral inhibition which has well-established links with anxiety (e.g., Fox et al., 2021). In contrast, the MAAS recall was moderately correlated with reduced responses to reward, even more so than anticipatory and consummatory subscales. Perhaps for this reason, expected differences in associations of the MAAS and reduced responses to reward (i.e., BAS-Reward; Carver & White, 1994) versus BIS were especially apparent for this subscale. Conversely, anticipatory and consummatory subscales showed more consistent albeit small correlations with the BIS, as described in other measures (e.g., the ASA; Watson et al., 2021). This may have contributed to some instances where this difference was nonsignificant for the MAAS total score. While more consistent when comparing associations of the MAAS with the BAS-Reward versus impulsive-related approach (i.e., BAS-Fun), experimental work testing how different facets of anhedonia are impacted by such constructs might help to elucidate processes both shared and unique across its dimensions.
Interestingly, the MAAS total score was not more strongly correlated with positive relative to negative affect (similar to the ASA; Watson et al., 2021), a pattern also reflected across its subscales. This contrasts with studies that validated adult measures of anhedonia in adolescent samples (e.g., the DARS; Hewitt et al., 2023). One possibility is that correlations with measures of anhedonia developed specifically with and for use in adolescents may better reflect age-based nuances in its underlying processes. For example, adolescents’ reward processing could be more strongly influenced by their negative mood (elsewhere shown to decrease reward sensitivity and alter positive memory recall; Hervas & Vasquez, 2013; Werner-Seidler & Moulds, 2011). To the extent that adolescent-specific measures can facilitate research on differences in the presentation of anhedonia and its associated mechanisms across development, the MAAS may help to further clarify the questions presented here. Given that many older adolescents’ experiences referenced in our measure may overlap with emerging adulthood (e.g., salience of growing up, pursuit of dreams), future work might also test whether our measure could be validly used among those in their 20s to further inform this developmental approach.
While important, this work was limited in a number of ways. Subsequent research might build on our use of self-report measures by using other methods (e.g., cognitive tasks) to further elucidate neurocognitive mechanisms underlying the facets of anhedonia measured by the MAAS. Additional limitations pertain to sample characteristics (e.g., non-clinical), which might pose constraints on the generalizability of our findings. Future studies should assess whether the MAAS can discriminate between adolescents with and without a depression diagnosis, or other diagnoses associated with anhedonia (e.g., psychosis). Second, although we administered the MAAS to a younger adolescent sample between the ages of 12 and 19 years old in Study 2, the mean age was approximately 16 years old. As such, it may be important to replicate our findings in a sample with a broader age range. Moreover, the structure was derived in older adolescents and then validated in a younger adolescent sample. Although we confirmed the structure independently in both samples, it remains possible that the initial structure of the measure is most applicable for older adolescents. Of note, this sample was also recruited within the first year of the COVID-19 pandemic, a stressor that may have exacerbated levels of anhedonia in Study 2. While the high school years are also particularly characterized by high levels of boredom and apathy (Spaeth et al., 2015), with some work showing that negative biases in recall of emotional experiences begin to emerge around this time (Zurbriggen et al., 2021), further study is needed to disentangle the influence of the pandemic on age-related differences in scores.
Conclusion
The MAAS is among the first measures of anhedonia designed for use in adolescence and the only one thus far to discriminate between anticipatory, consummatory, and recalled anhedonia. This scale has strong psychometric properties and may inform research on the multidimensionality of anhedonia and its heterogeneous presentation across forms of psychopathology and development. Such research may further yield a better understanding of the mechanisms underlying these differing manifestations, which could help to identify specific targets for intervention. This aim may be especially important in adolescence, where deficient reward processing is often among the first warning signs of a lifelong battle with mental health, suggesting that tailored interventions are urgently needed. As such, the MAAS may be of use for both researchers and clinicians seeking to better understand the multidimensionality of anhedonia in adolescence and fills an important gap in the psychometric literature.
Supplemental Material
sj-docx-1-asm-10.1177_10731911261423154 – Supplemental material for Development and Validation of the Multidimensional Adolescent Anhedonia Scale
Supplemental material, sj-docx-1-asm-10.1177_10731911261423154 for Development and Validation of the Multidimensional Adolescent Anhedonia Scale by Bronwen Grocott, Bita Zareian, Jackson Hewitt, Sabrina Ge, Paul Hewitt, Seonwoo Hong, Martin M. Smith, Xinli Chi and Joelle LeMoult in Assessment
Footnotes
Data Availability
Research data are available upon request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by a Canada Graduate Scholarship—Doctoral (BG), Joseph-Armand Bombardier Canada Graduate Scholarship—Master’s and Doctoral (BZ), and a Psi Chi Undergraduate Research Grant (SG).
Ethical Considerations
This research was approved by the University of British Columbia Behavioral Research Ethics Board on February 3, 2020 (H20-00119). Respondents gave written informed consent and assent before participation.
Supplemental Material
Supplemental material for this article is available online.
