Abstract
Children with neuromotor impairments experience difficulties with upper limb movement. Upper limb exoskeletons offer the potential for a better therapy experience for this population through personalized treatment and facilitating movement throughout the arm, including the shoulder, elbow, forearm, wrist, and hand. However, limited exploration of the interaction and usability between these devices and children has been done. Therefore, this study explores the interaction between children and upper limb exoskeletons. To achieve this goal, this paper reviews 10 articles (out of 181 papers) concerning the application and effectiveness of upper limb exoskeletons in children’s rehabilitation. Upper limb exoskeletons were evaluated in these studies based on pediatric participants’ task performance (e.g., inserting an object into a hole) as well as subjective perspectives (e.g., comfortability and usability). Results showed that upper limb exoskeletons were proved to be effective in facilitating children’s upper limb movement in bimanual coordination and unilateral movements. Through tasks designed to require specific movements or the manipulation of objects, researchers noted improvements across coordination, precision, smoothness, quality of movement, and others. The improvements were related to the functioning of upper limb muscles (e.g., biceps and triceps). Limitations for these studies include (1) the lack of control groups when collecting data, (2) possible test-retest reliability concerns when studying the feasibility of exoskeleton use, and (3) implications for long-term efficacy and adaptability for individual physical differences in children. Additionally, some studies exclusively studied healthy children rather than testing devices with children who suffer from motor impairments, which affects the generalizability of results.
Introduction
Children with limited mobility in their upper limbs experience restricted opportunities to explore and interact with the surrounding environments, reducing their independence in activities of daily living (e.g., eating, playing, etc.) (Park et al., 2021; Shikako-Thomas et al., 2008). This unfortunate constraint can arise from health issues, including but not limited to cerebral palsy (Odding et al., 2006; Park et al., 2021), muscular dystrophy/atrophy (Janssen et al., 2016), and acquired brain/spinal cord injury (Biffi et al., 2018), which can profoundly impact children’s physical (Plasschaert et al., 2019), cognitive, and social development (Michielsen et al., 2011) as they transition into adulthood.
Traditional rehabilitation approaches for children with upper limb mobility issues involve physical and occupational therapy, aimed at building strength and regaining independence through targeted exercises and activities. However, these traditional approaches necessitate a sustained commitment to sessions with specialized therapists and specific equipment, which can be challenging to families and facilities, especially in under-resourced areas (Bosecker et al., 2010; Krebs et al., 1998). The rehabilitation process may become more difficult if children and their caregivers get discouraged due to the absence of immediate progress, as improvement often varies from one patient to another and generally requires time to become evident. Furthermore, obtaining reliable feedback from child patients can be tricky, as these patients may struggle to accurately convey their progress, especially after engaging in therapy sessions that are physically demanding and tiring (Aubin et al., 2014).
Alternative approaches emerge to complement traditional rehabilitation approaches. Treatments such as neuromuscular electrical stimulation are proving beneficial in enhancing upper limb strength, flexibility, and functionality (Wright et al., 2012). Incorporating virtual reality into therapy training programs (Roberts et al., 2021) has also been shown to increase engagement and effectiveness. What is more, the advent of assistive technologies, especially upper limb exoskeletons, not only alleviates the dependency on therapists and equipment but also offers the potential for a better therapy experience through personalized treatment and timely feedback (Bosecker et al., 2010; Krebs et al., 1998).
Exoskeletons such as ARMIN III (Nef et al., 2013), CADEN-7 (Sanjuan et al., 2020), InMotion2 (InMotion Arm, n.d.), Armeo Spring (Biffi et al., 2018), and WristBot (Cappello et al., 2015), among others, have been launched to aid in upper limb rehabilitation. And there is extensive ongoing research developing prototypes (e.g., robotic devices) for this purpose. However, to the best of the authors’ knowledge, the majority of these products and studies primarily cater to the needs of adults (Falzarano et al., 2019), rather than children who are in crucial stages of physical and cognitive development. The recommendations for children’s use of exoskeletons, especially upper limb exoskeletons, are limited. While the reviews by Gaudet et al. (2021) and Falzarano et al. address pediatric access to upper limb exoskeletons, they tend to focus more on the specifications of the exoskeletons. There is limited exploration of the interaction and usability between these devices and children, a factor that is critical for the successful adoption and sustained use of exoskeleton technology among children.
Therefore, the purpose of this study is to explore the application and effectiveness of upper limb exoskeletons in children’s rehabilitation, particularly focusing on the interaction part between children and these devices. Toward this end, our objectives are to (1) explore how upper limb exoskeletons are being used in the rehabilitation of children, (2) identify key contributions upper limb exoskeletons can offer children during rehabilitation, and (3) uncover the factors that promote or hinder successful and consistent use of upper limb exoskeletons among children.
Methods
Literature Search Strategy
This study follows the Preferred Reporting of Items for Systematic Reviews and Meta-Analyses (PRISMA) protocol. A literature search was carried out across the Web of Science, Scopus, Engineering Village, and PubMed in December 2023 and January 2024. The search has been conducted using the following keywords: (Exo*) AND (Children OR Pediatric) AND (Upper Limb OR Upper Extremity OR Arms).
Study Selection, Data Extractions, and Analysis
A total of 181 papers were found from keyword searching. The 166 papers (after removing duplicates) were carefully checked and evaluated using the following inclusion criteria: (1) the paper is not a review paper, (2) the paper involves human subject experiments with human participants recruited, (3) the paper reports on human performance metrics for upper limb mobility (e.g., error rates, mobility assessments, etc.), (4) the paper is not a case study of one patient and (5) the paper is published in English. The first round of screening was based on titles and abstracts and conducted by researchers (PM, SY, and SM) and narrowed down the scope of available papers to 39. The second round of screening, full-text screening, was carried out by the leading researcher (PM), resulting in 10 papers being selected for the study (Figure 1). Throughout the screening process, eligibility discrepancies were resolved through discussion among the research team until there was consensus achieved. For example, it was decided that case studies involving the observation of a single pediatric patient would be ineligible for the review due to the low generalizability of results to other children. Information was then extracted from all eligible papers including characteristics of the metadata (author, year, title), devices (specification of exoskeleton and other devices), experiment design (# of participants, independent variables, dependent variables, etc.), results, conclusions, and additional notes. A descriptive and qualitative synthesis was then developed based on information retrieved from the papers that passed the full paper review process.
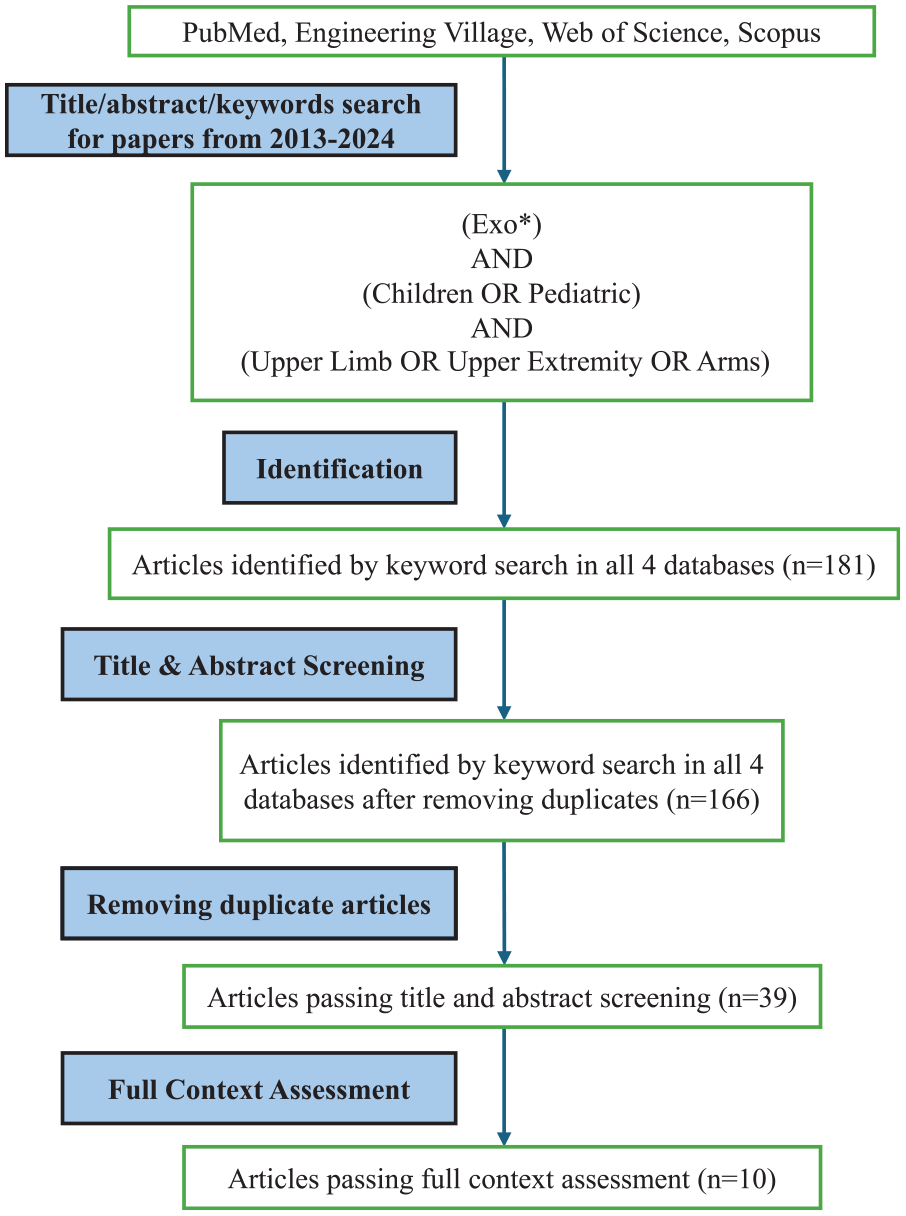
Flowchart for the review process.
Results
Dataset Characteristics
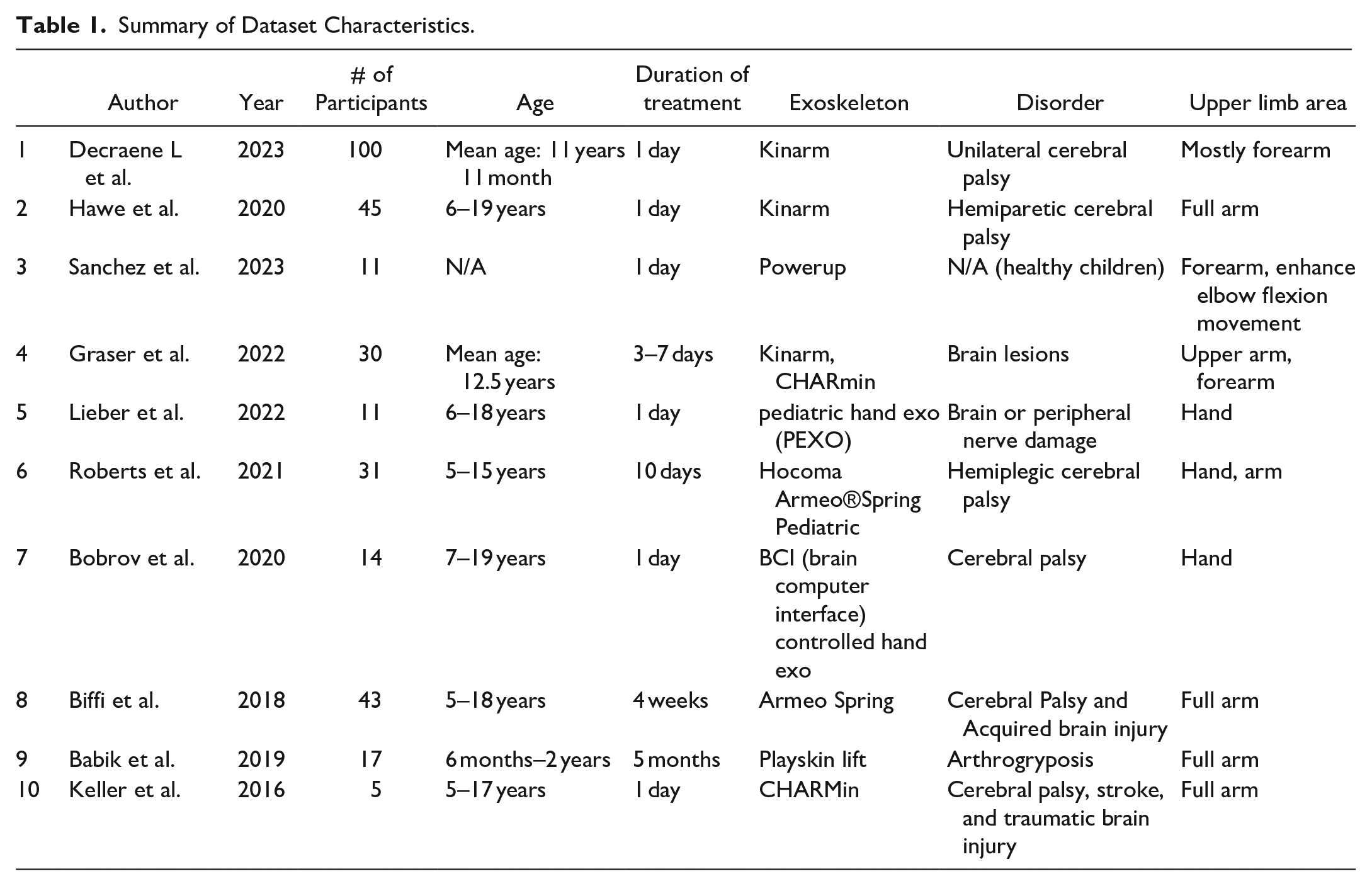
Table 1 shows the dataset characteristics of the 10 papers. The age of the participants in the included 10 studies ranged from 6 months to 19 years. The number of participants included in each study ranged from 5 to 100. The category of health conditions/disorders, the duration of treatment, and the type of exoskeleton devices are also summarized in this table.
Summary of Dataset Characteristics.
Regarding the functionality of upper limb exoskeletons, among the 10 studies, the review reveals that 40% focused on full arm support (Babik et al., 2019; Biffi et al., 2018; Hawe et al., 2020; Keller et al., 2016), 20% concentrated on elbow and forearm assistance (Decraene et al., 2023; Sanchez et al., 2023), and 30% specifically provided hand support for children with various neuromotor disorders (Bobrov et al., 2020; Lieber et al., 2022; Roberts et al., 2021). Over half of the studies (60%) applied exoskeletons to children with cerebral palsy (Biffi et al., 2018; Bobrov et al., 2020; Decraene et al., 2023; Hawe et al., 2020; Keller et al., 2016; Roberts et al., 2021), The remaining studies explored the use of exoskeletons for other health conditions, such as congenital or acquired brain injuries (Biffi et al., 2018; Graser et al., 2022; Keller et al., 2016; Lieber et al., 2022), arthrogryposis (Babik et al., 2019), or stroke (Keller et al., 2016).
In terms of contributions of exoskeletons, the review identifies varied focal points: among the 10 studies, 40% emphasized tasks involving bimanual movements (Decraene et al., 2023; Hawe et al., 2020; Lieber et al., 2022; Roberts et al., 2021), while 40% evaluated the support of exoskeletons for coordination, precision, and overall quality of movement (Biffi et al., 2018; Graser et al., 2022; Keller et al., 2016; Sanchez et al., 2023). Additionally, audiovisual technologies were integrated into 40% of the studies involving the manipulation of virtual objects (Bobrov et al., 2020; Decraene et al., 2023; Keller et al., 2016; Roberts et al., 2021), and the direct manipulation of physical objects using exoskeletons was involved in 30% of the studies (Babik et al., 2019; Keller et al., 2016; Lieber et al., 2022). A subjective evaluation was carried out in one study (Roberts et al., 2021) via a questionnaire that explored the ease of training, overall enjoyments and frustrations, and technical challenges encountered by the child participants.
The duration of treatment in these studies ranges from 3 days to 5 months. It is important to note that in 4 of the 10 studies (Babik et al., 2019; Biffi et al., 2018; Graser et al., 2022; Roberts et al., 2021), children with neuromotor impairments experienced benefits to their upper limb mobility. These studies involved continued treatment over a specified period of time, longer than 1 day. The actual domain of these improvements varies, however, due to the use of different exoskeletons focusing on a particular part of the upper limb such as the hand or elbow, as well as different assessment measures used. For example, Lieber et al. (2022) and Babik et al. (2019) have demonstrated improvement in the manipulation of physical objects as the course of treatment using an exoskeleton progresses. Furthermore, while Decraene et al. (2023) focused on improvements in bimanual coordination, Biffi et al. (2018) instead described changes to movement velocity and fluidity. Despite these differences, these four studies explored in this review suggest a possible dose-response relationship in pediatric upper limb rehabilitation with the use of exoskeletons.
Collective analysis of task performance demonstrated the effectiveness of upper limb exoskeletons in enhancing movement during the rehabilitation process. Although the impact of upper limb exoskeletons differed based on the design of exoskeletons and the impairment level of children, there was a consistent improvement observed in both bimanual and unilateral movements, muscle activation, and movement quality. These findings are vital for the continued development of upper limb exoskeletons designed for pediatric rehabilitation, considering factors such as ease of use and various other considerations.
Discussion
The review highlights the benefits of the use of exoskeletons in pediatric rehabilitation for children with upper limb mobility challenges. Setting aside individual differences, upper limb exoskeletons proved to be substantially effective in facilitating upper limb movement. Notable improvements were observed in bimanual coordination and unilateral movements. Through tasks designed to require specific movements or the manipulation of objects, researchers noted improvements across coordination, precision, smoothness, quality of movement, and others. The improvements were related to the functioning of upper limb muscles (e.g., biceps and triceps for exoskeletons offering elbow support).
The studies covered in this review come with certain limitations. First, the variability in neuromotor disorders among the participants makes it challenging to generalize the findings to all children with a variety of individual needs. Notably, one study included only healthy children, despite the primary focus on addressing upper limb mobility challenges (Sanchez et al., 2023). Enhancing the reliability of these findings could involve quantifying and documenting the neuropsychological conditions among the participant population, allowing for a more precise definition and offering the potential to model device effectiveness based on neuropsychological conditions.
Secondly, the methods used to evaluate upper limb exoskeletons in current research may not adequately measure their long-term benefits. Most of the studies did not include follow-up sessions with participants, which is crucial given that motor disorders can impact children across multiple years. To fully understand the potential of exoskeletons, future research needs to examine their use over extended periods.
As previously described in this review, there are four articles with continued treatment over time revealing improvements in multiple domains of upper limb mobility and functionality. This reflects a dose-response relationship between the quantity of treatment and resulting benefits to mobility with the use of exoskeletons. Prior literature already establishes a known possible benefit to physical performance by increasing the frequency of exercise routines such as resistance training (Schoenfeld et al., 2017). Because the research demonstrates that children stand to potentially experience exponential benefits to their mobility with continued treatment, this dose-response relationship presents implications for the nature of exoskeleton-based treatment and research among pediatric subjects and encourages the long-term observation of how a treatment regimen may produce changes in movement ability over time. It may not be enough to observe a same-day improvement in certain mobility skills if long-term efficacy is unknown. Not only should treatment sessions be consistent, but also critical observation of progress in mobility improvements.
Children experiencing neuromotor difficulties are often delayed in achieving physical developmental milestones that would normally be reached naturally as the year progresses, so it is imperative to study how the use of exoskeletons can help align impaired children’s developmental timeline with that of healthy children.
Future Directions
For future research being conducted on the topic of pediatric use of exoskeletons, there are several ways to focus efforts on particular aspects of the experience of using exoskeletons that may provide more robust, generalizable findings.
For example, although this review, like many existing prior reviews in this field, focuses on either upper limb or lower limb exoskeleton use, it would be prudent to aim for future studies that involve only specific limb sections. A review on solely hand or wrist exoskeletons or only elbow mobility would yield insights with stronger implications for a targeted sub-population of pediatric exoskeleton users. Alternatively, including research studies focused on specific mobility skills can also achieve more reliable findings in a review.
Furthermore, encompassing a larger number of prior articles in the review will garner more robust, generalizable findings. Although the present review is comprehensive in covering the use of exoskeletons in various areas of the upper body and several different human performance measures, it lacks an in-depth analysis of any one domain. Subsequent research efforts should be aimed at not only narrowing the field of interest but also expanding the breadth of literature included for review.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
