Abstract
The issue of work-related musculoskeletal disorders (WMSDs) stemming from manual handling tasks remains a significant economic and societal burden, with healthcare workers being one of the most persistently affected groups. Exoskeletons have seen growing implementation for aiding manual handling tasks in industrial sectors. Traditional measurements and analyses of joint kinematics and dynamics commonly utilize optical motion capture systems and force plates. Nevertheless, the limitations of optical motion capture systems include their dependence on marker visibility and the necessity for a controlled lab environment. An innovative wireless technology featuring miniaturized, skin-mounted sensors, BioStamp nPoint (MC10, Inc., MA, USA) exhibits significant potential in addressing the challenges mentioned above. Therefore, the objective of this study was to explore a flexible sensor-based approach to assessing the effects of a back exoskeleton on joint kinematics during patient handling.
Objectives
The issue of work-related musculoskeletal disorders (WMSDs) stemming from manual handling tasks remains a significant economic and societal burden, with healthcare workers being one of the most persistently affected groups (BLS, 2020). Exoskeletons have seen growing implementation for aiding manual handling tasks in industrial sectors. The rising popularity of passive back-support exoskeletons can be attributed to their lightweight design and user-friendly features. These exoskeletons have emerged as a preferred choice across diverse industrial environments. Given their potential, passive back-support exoskeletons could present a promising solution for healthcare workers grappling with the challenge of manually handling patients.
Prior research has indicated that the use of a back support exoskeleton can lead to a reduction in back muscle activity and affect various parameters such as the trunk flexion angle and hip flexion angle, while performing patient handling tasks (Chen et al., 2023; Hwang et al., 2021; Ivaldi et al., 2021) or lifting tasks (Koopman et al., 2020). However, most of them used the marker-based method (Chen et al., 2023; Hwang et al., 2021) or IMU-based system (Ivaldi et al., 2021). Only a few (Yin et al., 2021, 2024) have explored the feasibility of the flexible sensor-based system.
Traditional measurements and analyses of joint kinematics and dynamics (Chen et al., 2023; Koopman et al., 2019) commonly utilize optical motion capture systems and force plates. Nevertheless, the limitations of optical motion capture systems include their dependence on marker visibility and the necessity for a controlled lab environment. Inertial measurement units (IMUs) present a more agile alternative, yet their utilization, particularly in naturalistic settings, encounters challenges such as performance interference and data artifacts arising from the sensor size and attachment problems (Yin et al., 2021).
An innovative wireless technology featuring miniaturized, skin-mounted sensors, BioStamp nPoint (MC10, Inc., MA, USA) exhibits significant potential in addressing the challenges mentioned above (Sen-Gupta et al., 2019). Prior research (Yin et al., 2024) has successfully developed a flexible sensor-based system capable of measuring kinematics in the torso, low-back, and lower extremities during symmetrical lifting tasks. However, Yin’s model can only measure joint motion in a sagittal plane. Thus, there persists a pressing need for the development of a more comprehensive whole-body model, not only to evaluate the effectiveness of low-back exoskeletons in lifting scenarios but also to assess their performance in complex asymmetric handling tasks under naturalistic settings (e.g., patient handling tasks).
Therefore, the objective of this study was to explore a flexible sensor-based approach to assessing the effects of a back exoskeleton on joint kinematics during patient handling.
Approach
Six healthy participants, three males and three females (age: 23.5 ± 2.2 years, weight: 66.4 ± 11.0 kg, height: 1.68 ± 0.08 m), were recruited. The study protocol was approved by the Institutional Review Board of Texas A&M University. Upon obtaining written informed consent, participants were given sufficient time to acquaint themselves with the operation of the exoskeleton (Laevo V2.5, Delft, The Netherlands) and to familiarize themselves with the experimental tasks.
Participants were instructed to perform three simulated patient handling tasks, with and without wearing the exoskeleton (Chen et al., 2023). Each task was repeated five times. The order of three tasks (a), (b), and (c) was completely randomized with two-minute inter-trial breaks. Before the patient handling tasks, participants were asked to perform 2 min of repeated symmetric lifting as a reference task, designated as task (r).
A total of 11 BioStamp nPoint sensors were strategically placed on the subject to acquire kinematics data for multiple segments (Figure 1). In addition to Yin’s seven-sensor model configuration (Yin et al., 2024), additional four sensors were attached to the arms and forearms, for capturing the elbow flexion/extension motions. Sensors on the sacrum and thigh segments were intended to estimate the left and right hip flexion/extension. Sensors on the sternum and arms segments were intended to estimate the left and right shoulder flexion/extension.
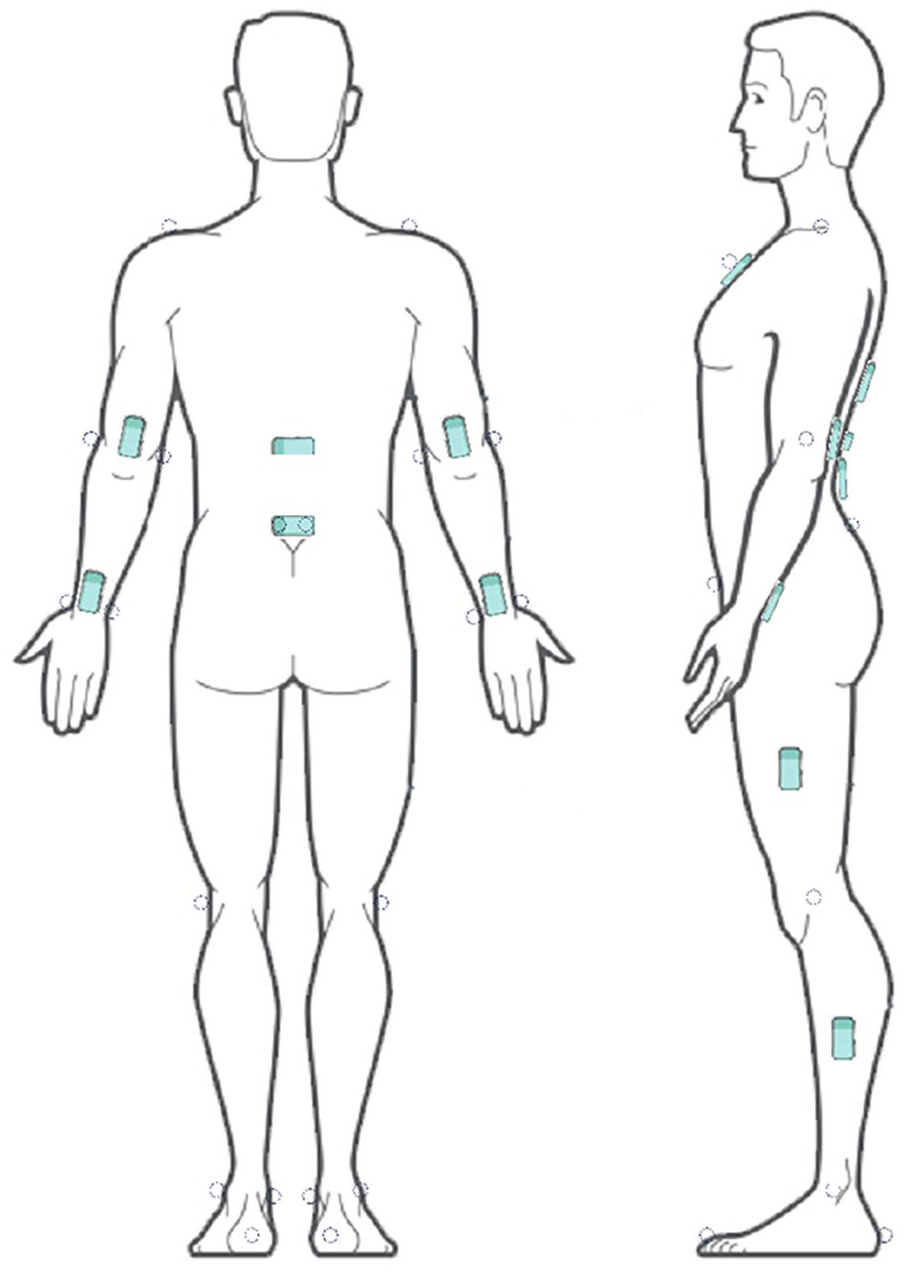
Sensor and reflective marker placement. Pictures were created by adapting images from MC10 Inc., MA, USA.
Two static trials were conducted for each participant to calibrate the flexible sensor-based system. This involved capturing both marker-based and sensor-based motions, with and without the exoskeleton, ensuring accurate alignment and synchronization.
Findings
The grand mean RMSE (and Pearson’s correlation coefficient r) between sensor- and marker-based measurements across all subjects were 12.63° (.906), 10.61° (.877), 8.83° (.916), 9.02° (.796), and 12.66° (.926), 10.02° (.782), 9.24° (.681), 8.46° (.726) for task (r), (a), (b) and (c) respectively, when under WITHOUT condition and WITH condition. The lumbar flexion angle profiles for a representative subject during task (r), (a), (b), and (c) are shown in Figures 2 and 3. The proposed system showed good (r > .75) to excellent (r > .90), and moderate (r > .5) to excellent (r > .9) agreement (Poitras et al., 2019) for the whole-body joint kinematics, between the sensor-based and marker-based systems while performing the lifting task and patient handling tasks, respectively. This included elbow, shoulder, lumbar, hip, knee, and ankle flexion angles.
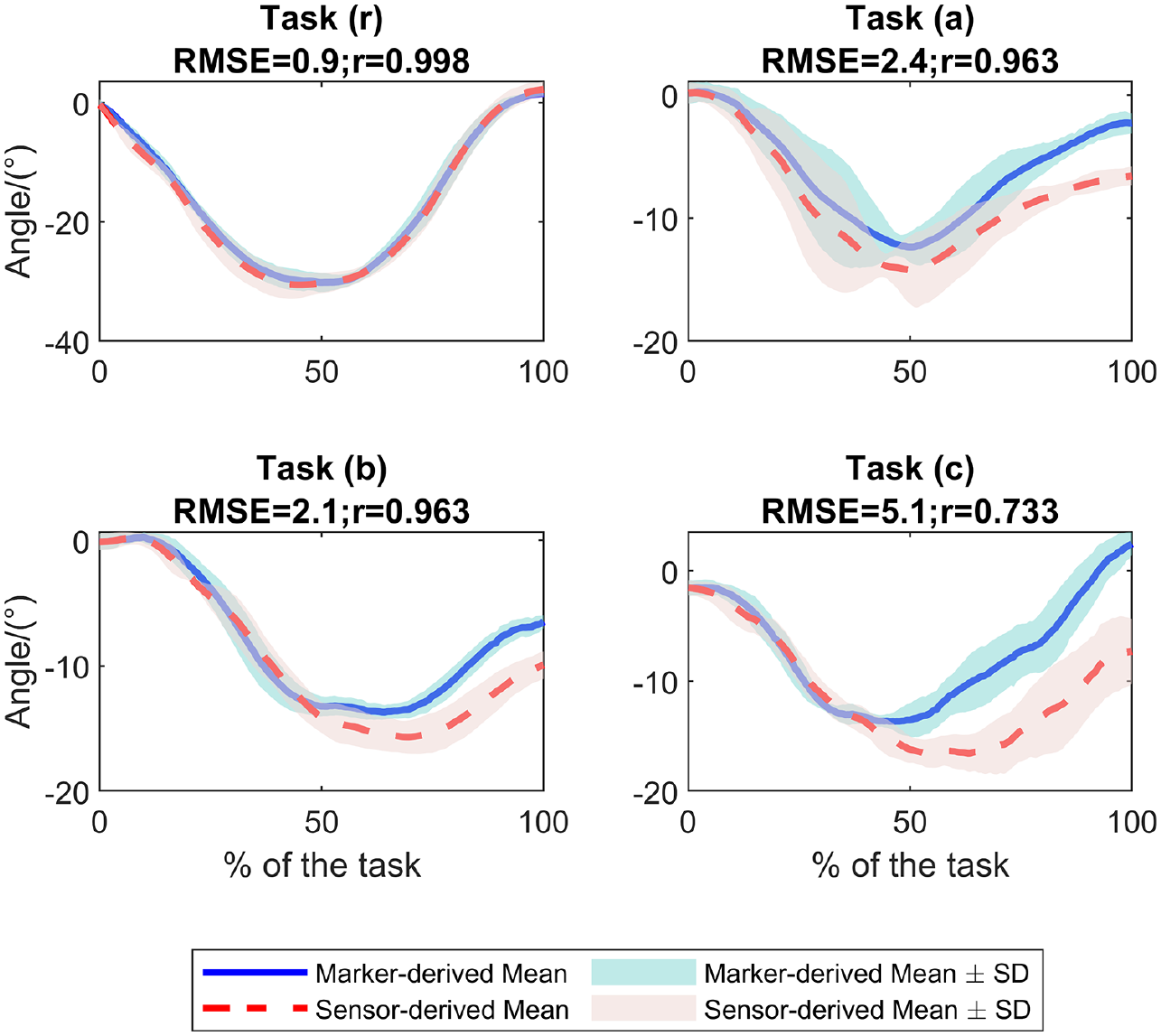
Lumbar flexion angle profiles during tasks (r), (a), (b), and (c) derived by marker-based method and the proposed sensor-based method, under WITHOUT exoskeleton condition.
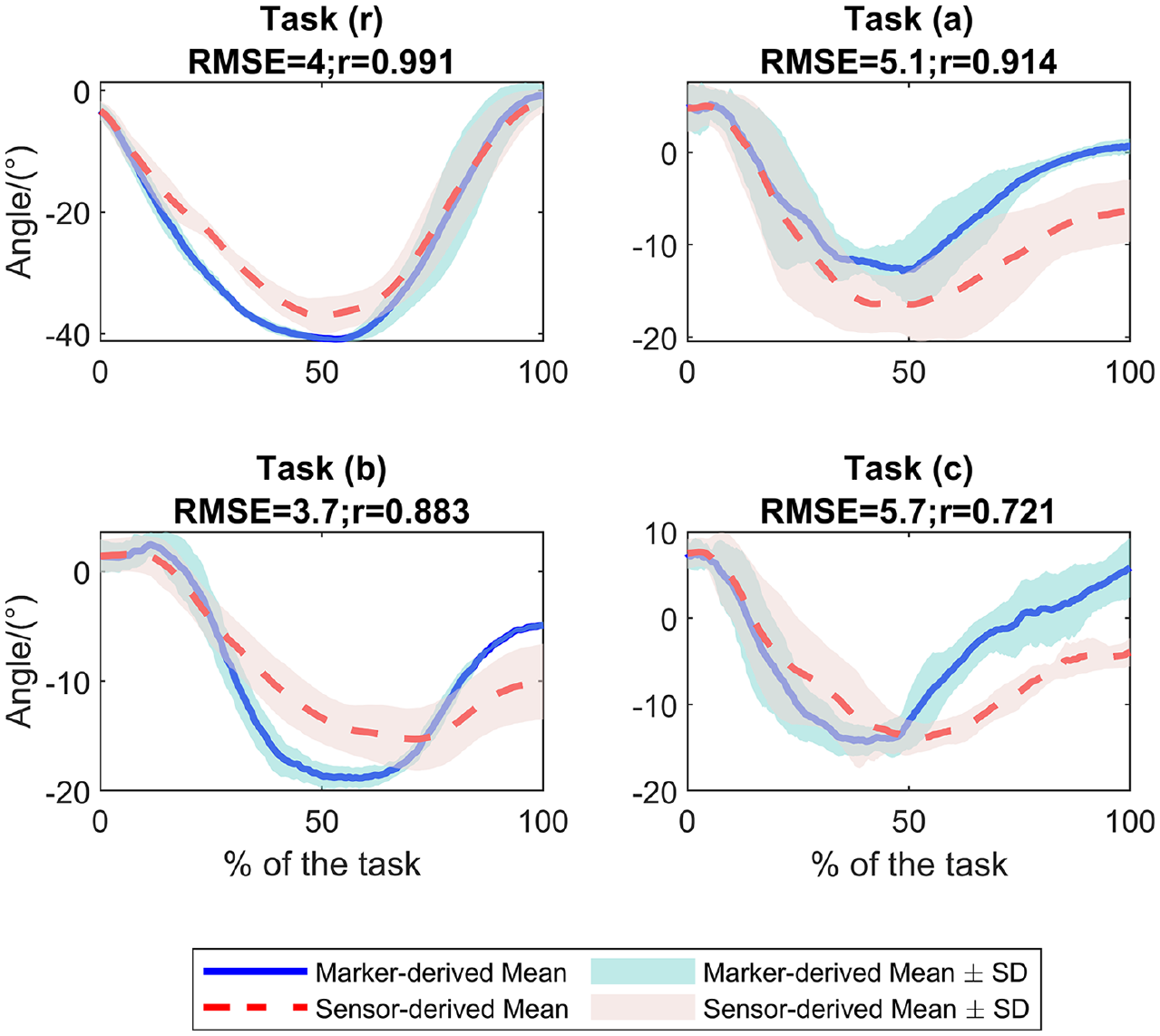
Lumbar flexion angle profiles during tasks (r), (a), (b), and (c) derived by marker-based method and the proposed sensor-based method, under WITH exoskeleton condition.
Takeaways
This study concludes with three takeaways. First, the flexible sensor-based approach presents a feasible methodology for assessing the biomechanics of exoskeleton-assisted patient handling. Second, the presence of task asymmetry and complexity may negatively impact the accuracy and precision of flexible sensor-based measurements. Third, the use of exoskeletons appears to marginally increase the discrepancy between kinematics captured by flexible sensors and those obtained through conventional marker-based systems.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Disclaimer
The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the National Institute for Occupational Safety and Health (NIOSH), Centers for Disease Control and Prevention (CDC). Mention of any company or product does not constitute endorsement by NIOSH/CDC.
