Abstract
Background:
To our knowledge, no study is available comparing the change in ankle mechanics during gait after total ankle arthroplasty (TAA) based on the origin of the osteoarthritis. As the nature of trauma is different in patients sustaining post-fracture ankle osteoarthritis (PFOA) from those sustaining post-sprain ankle osteoarthritis (PSOA), it could be expected that the outcomes of TAA, in terms of ankle mechanics during gait, would be different in the 2 groups. A prospective matched comparative study was therefore performed to investigate whether patients sustaining PFOA had different outcomes in terms of changes to ankle mechanics during gait (before surgery vs 1 year after surgery), compared with patients sustaining PSOA.
Methods:
Fifteen patients with PFOA and 15 patients with PSOA scheduled for primary TAA for pain relief were recruited and peer-matched based on their demographic and spatiotemporal data. All patients underwent a 3D gait analysis before and after surgery, during which a kinematic and kinetic multi-segment foot model was used to quantify inter-segmental joint kinematics and kinetics.
Results:
The PFOA group exhibited significantly lesser pre- vs postoperative increases in ankle (Shank-Calcaneus) joint peak power, and ankle (Shank-Calcaneus) joint work after TAA compared with the PSOA group. Furthermore, the results demonstrated a trend toward greater increases in peak ankle (Shank-Calcaneus) joint plantarflexion moment and in negative ankle (Shank-Calcaneus) joint work for the PSOA group compared with the PFOA group.
Conclusion:
This study suggests that patients sustaining PFOA have smaller pre- to postoperative gains in ankle (Shank-Calcaneus) joint power and ankle (Shank-Calcaneus) joint work during gait after TAA compared with patients sustaining PSOA, with modest between-group effects. Although evidence in TAA is lacking, insights from knee replacement suggest prehabilitation and nutritional support may mitigate deficits, representing a potentially essential strategy for PFOA patients requiring further validation.
This is a visual representation of the abstract.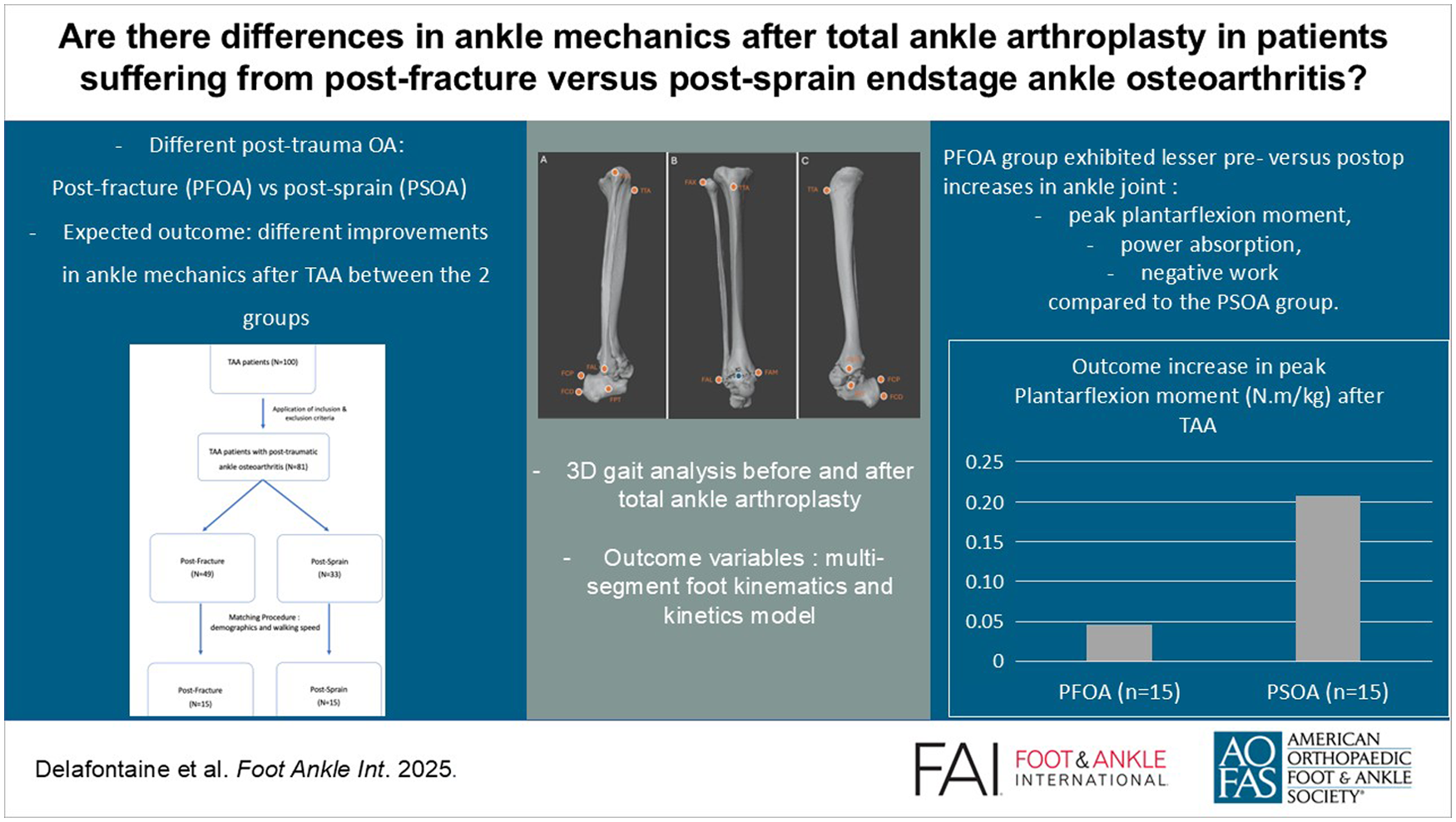
Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
