Abstract
Background:
This study investigates revision surgery rates in patients with Ehlers-Danlos Syndrome (EDS) or hypermobility spectrum disorder (HSD) following ankle surgery for instability compared to matched controls.
Methods:
A retrospective cohort study was conducted using the PearlDiver Mariner 170 Database. Patients undergoing ankle ligament repair procedures were identified using Current Procedural Terminology (CPT) codes. The experimental cohort included patients with EDS or HSD with at least 2 years of follow-up data, excluding other connective tissue disorders and confounding conditions. Propensity score matching was used to create a matched control group. The primary outcome was the rate of revision ankle ligament repair within 2 and 5 years. The secondary outcome was the effect of patient risk factors associated with revision. Revision rates were compared between cohorts using multivariable logistic regression. Statistical significance was set at P < .05.
Results:
The 2-year cohort included 805 patients with EDS/HSD and 805 matched controls, whereas the 5-year cohort consisted of 480 patients in each group. Procedures primarily involved modified Brostrom repair, lateral ankle ligament reconstruction, and arthroscopic-assisted repairs. Patients with EDS/HSD had significantly higher revision rates at 2 years (13.8% vs 6.3%) and 5 years (19.4% vs 7.3%) (P < .0001). Multivariate analysis identified EDS/HSD as an independent risk factor for revision surgery, with adjusted odds ratios of 2.41 (95% CI 1.71-3.45; P < .0001) at 2 years and 3.11 (95% CI 2.07-4.77; P < .0001) at 5 years.
Conclusion:
This study highlights the significant challenges in surgical management of ankle instability in patients with EDS and HSD. The risk of surgical failure increases over time, with a 3.1-fold increase in revision surgery rates at 5 years postoperatively compared with matched controls. These findings emphasize the need for specialized surgical approaches and comprehensive perioperative care to address the unique risks in this population. Future work should compare specific repair techniques and graft choices in this high-risk cohort.
This is a visual representation of the abstract.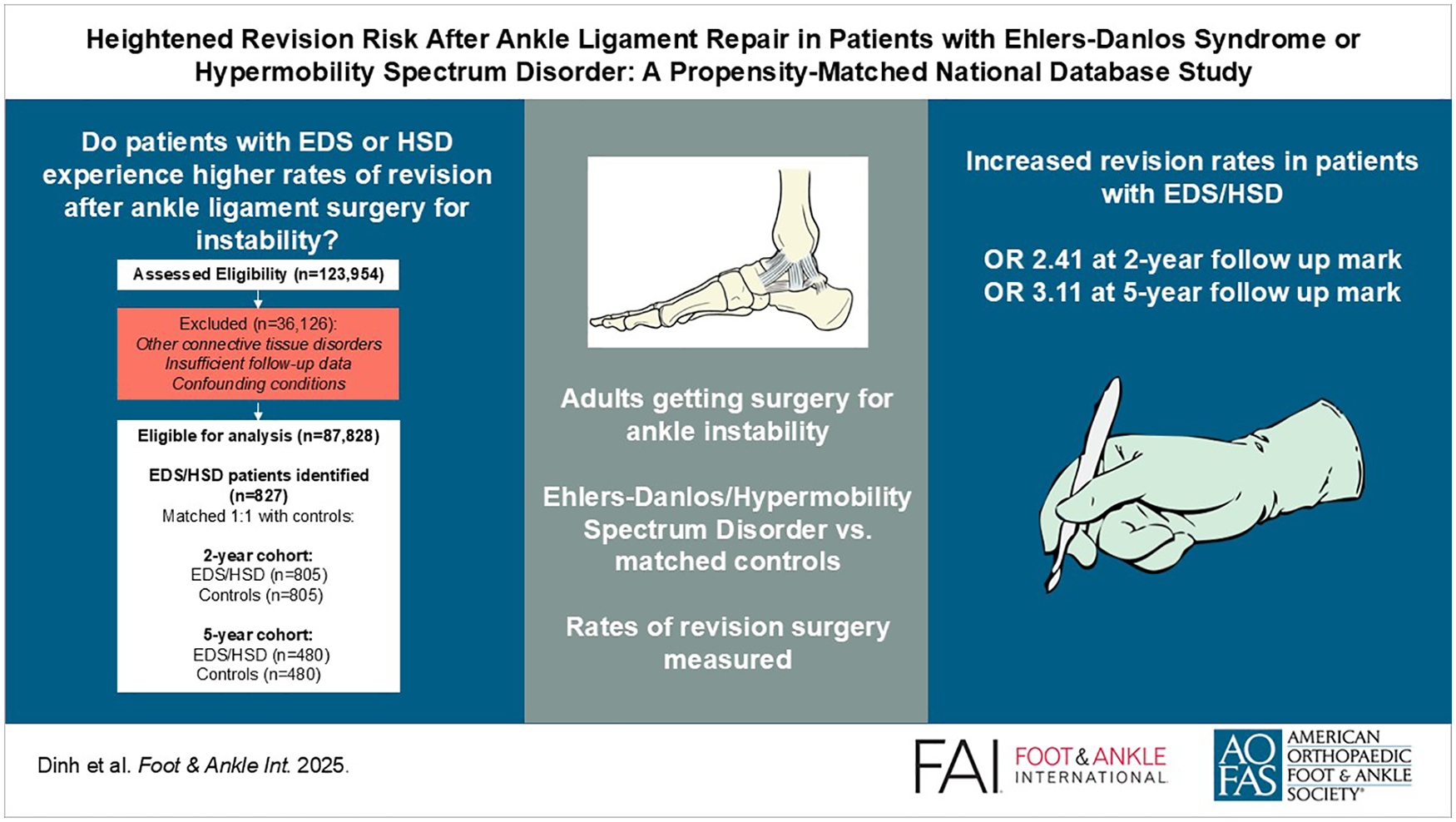
Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
