Abstract
Background:
Minimally invasive hallux valgus surgery can rarely result in a distinct radiologic finding termed the “Filament Union sign,” characterized by a thin, filamentous bone bridge at the osteotomy site <25% of the metatarsal head width and associated with minimal medial, lateral, or central remodeling. This study aimed to determine its prevalence and identify potential contributing factors.
Methods:
A retrospective radiographic cohort study analyzed 726 feet that underwent percutaneous fourth-generation transverse osteotomy for hallux valgus correction between November 2017 and January 2023. Primary outcome was presence of the filament union sign. Secondary outcomes included patient-reported outcome measures and radiographic deformity analysis.
Results:
The filament union sign was identified in 24 feet (3.3%, 95% CI: 2.0%-4.6%) with 15 cases (62.5%) occurring in patients who underwent bilateral procedures and 2 patients exhibiting bilateral filament union. Although both groups showed similar baseline characteristics, the filament union group demonstrated statistically but not clinically significant increased Manchester-Oxford Foot Questionnaire (MOXFQ) Index scores (20.6 ± 16.9 vs 13.0 ± 15.7, P = .040) at final follow-up. There was no significant difference in individual MOXFQ domains, P > .05. Preoperative hallux valgus angle was significantly associated with filament union (odds ratio 1.08, 95% CI 1.02-1.15, P = .006). All cases in the filament union group achieved bony union, with 1 case of nonunion observed in the nonfilament group. No instances of fracture or metalwork failure were observed in the filament union group.
Conclusion:
The filament union sign is an uncommon radiographic finding following percutaneous hallux valgus surgery, occurring in 3% of cases. Although its presence was associated with statistically significant decreased functional outcomes, this difference did not meet the threshold for clinical significance and was also not associated with an increased rate of mechanical failure/fracture or revision surgery rate. Further research is needed to fully understand the mechanical and biological factors contributing to this pattern of bone healing.
This is a visual representation of the abstract.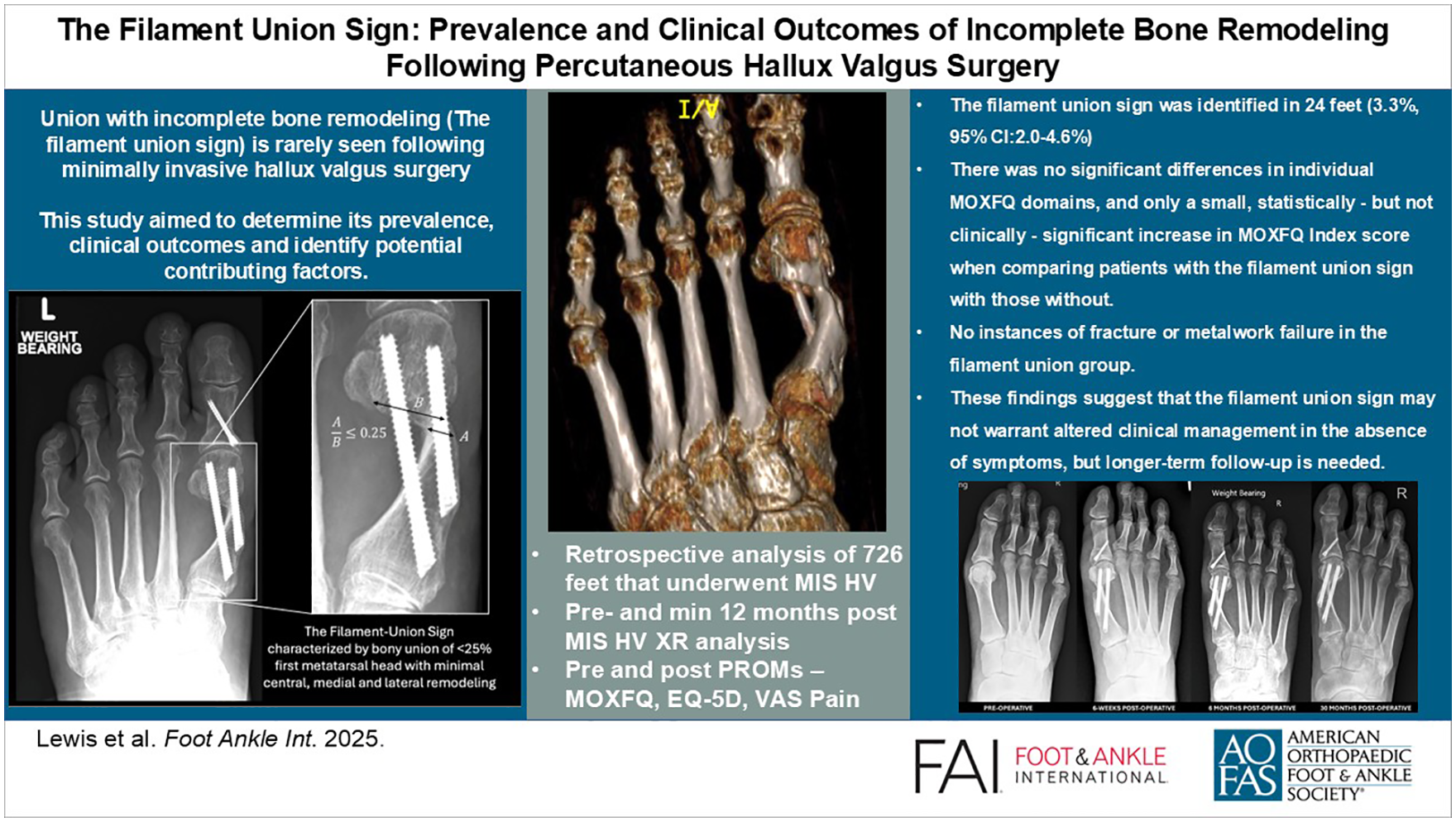
Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
