Abstract
Perivascular epithelioid cell tumor (PEComa) belongs to a family of rare mesenchymal neoplasms that share characteristic morphologic, immunohistochemical and molecular findings. In this report, we provide a detailed clinicopathological characterization of a PEComa incidentally discovered in the right lung of a 53-year-old woman. This tumor with epithelioid cell morphology and myomelanocytic differentiation demonstrated a TFE3::YAP1 fusion by targeted RNA sequencing. While a subset of PEComas shows TFE3 rearrangements, fusion with YAP1 has not been systematically documented in this entity. Clear cell stromal tumor of the lung and epithelioid hemangioendothelioma characteristically display the TFE3::YAP1 fusion; however, as currently defined, both lack myomelanocytic features. Here, we describe a novel TFE3 fusion partner that further expands the spectrum of molecular alterations seen in PEComa.
Keywords
Background
Perivascular epithelioid cell tumor (PEComa) can occur sporadically or in association with tuberous sclerosis complex (TSC), an autosomal dominant disorder that is associated with loss of TSC1or TSC2 gene function. 1 Indeed, sporadically occurring PEComas are also commonly defined by loss of the TSC1/TSC2 complex or rearrangements involving TFE3 gene. 2 A subset of PEComas have been described with a TFE3 rearrangement, which is mutually exclusive with TSC1 or TSC2 mutations. Of the TFE3 rearranged PEComas, SFPQ (formally PSF) is the most cited gene fusion partner.3,4 Here we report a detailed clinicopathological description of a PEComa of the lung with a novel gene fusion and discuss its differential diagnosis.
Patient Presentation
A 53-year-old woman presented to the emergency department with a 4-week history of congestion, non-productive cough, and intermittent right mid to lower lateral rib pain. The patient denied any previous smoking or illicit drug use. Her history was otherwise notable for hypertension. Chest imaging revealed a 3.1 cm solitary round mass within the right lower lung with moderate metabolic activity (Figure 1), which raised concern for a low-grade malignancy (eg, carcinoid tumor) versus granulomatous disease. Navigational bronchoscopy with biopsy of the lesion was non-diagnostic. A right lower lobe lobectomy was attempted. However, at surgery the mass appeared to be resting on the hilum just above the pulmonary artery and was attached to the visceral pleura of the right lower and right middle lobes of lung. Also apparent were dense fibrous adhesions and small perforating vessels to the lower lobe pulmonary artery. Since intraoperative consultation with frozen section assessment could not provide a definitive diagnosis and to avoid vascular injury, further dissection was aborted. A diagnostic biopsy with partial mass resection was performed. On gross examination, the resected mass measured up to 3.2 cm and displayed friable yellow/tan to dark brown cut surfaces. Histologically, the tumor mass was composed of predominantly epithelioid cells arranged in sheets and nests with intervening delicate thin-walled vessels (Figure 2A and B). The tumor cells had eosinophilic and clear cytoplasm (Figure 2C), and round to ovoid nuclei with mild nuclear pleomorphism (Figure 2D). Rare mitoses were identified throughout the lesion, comprising less than 1 mitosis per 2 mm2 (less than 1 mitosis per 50 high-power fields). Areas of cytoplasmic melanin, occasional lymphocytes and eosinophils were also evident by light microscopy. The tumor also showed focal (less than 10%) spindle cell morphology (Figure 2E) and occasional intratumoral macrophages (Figure 2F). No necrosis was present. By immunohistochemistry, the tumor was strongly positive for HMB45, microphthalmia transcription factor (MiTF), transcription factor binding to IGHM enhancer 3 (TFE3), and focally positive for smooth muscle actin (SMA) (Figure 3). The tumor was negative for keratin AE1/AE3, S100, SOX10, synaptophysin, chromogranin, thyroid transcription factor 1 (TTF1), PAX8, ALK, CD1a, h-caldesmon and desmin. The Ki-67 proliferative index was approximately 5% to 10%. The light microscopic and immunophenotypical features of the tumor were consistent with PEComa of the lung. Based on the relatively small size (<5 cm) and low mitotic rate (<1/50 high power fields), the tumor would be classified as benign. 5 Initial DNA-based NGS testing detected a YAP1::TFE3 fusion by intron tiling, which was confirmed by targeted RNA sequencing. The chimeric transcript was characterized by break points involving exon 4 of YAP1 (NM_001282101.1) and exon 7 of TFE3 (NM_006521.4) (Figure 4). A right lower lobe lobectomy with right middle lobe wedge resection for complete resection of the tumor was performed 3 months following the biopsy. The postoperative course was uneventful.
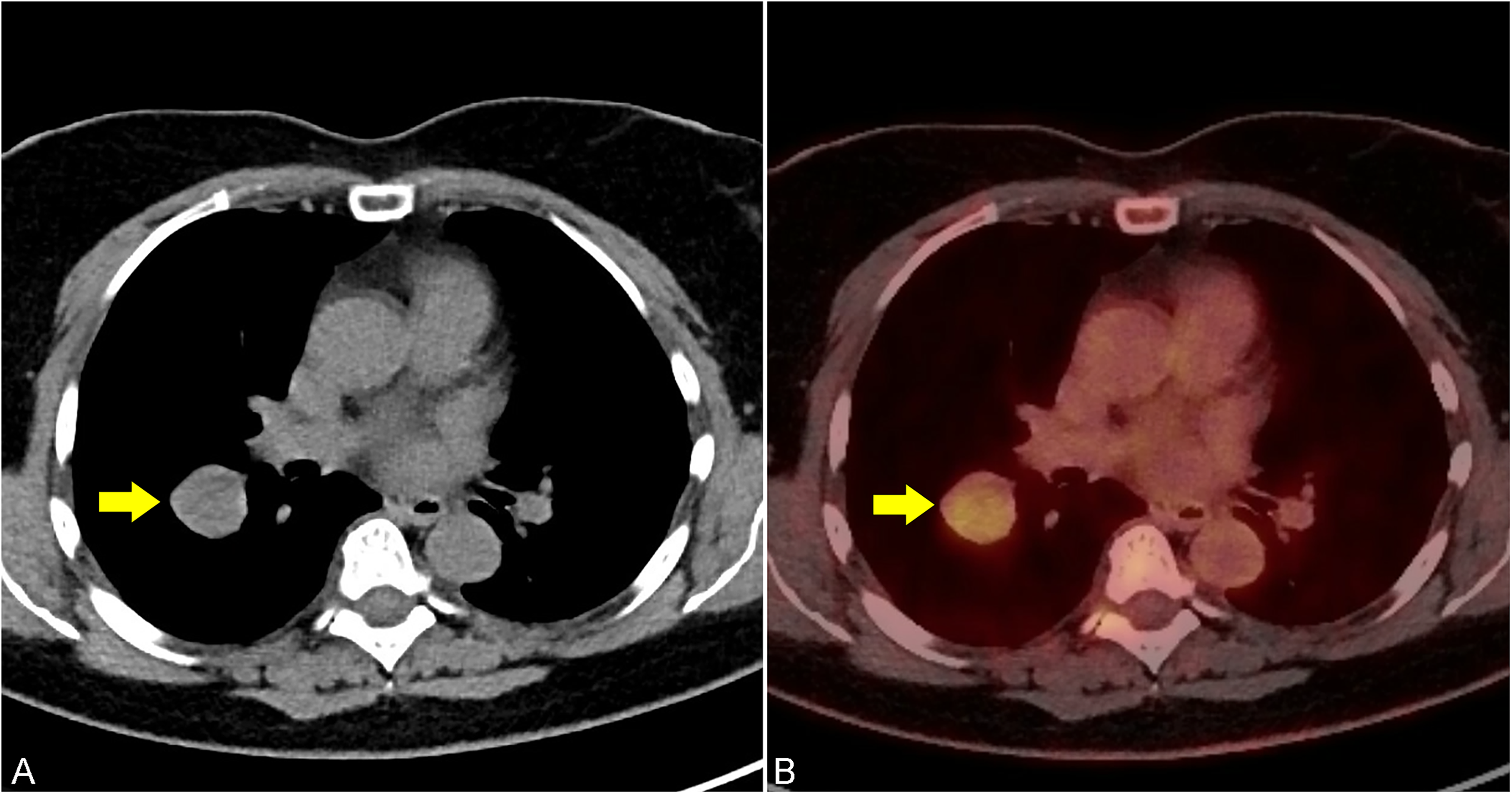
Imaging findings. (A) A right perihilar mass with possible eccentric calcification measuring 3.1 × 3.0 cm is noted on computed tomography (CT) of the chest. (B) Corresponding fused positron emission tomography/computed tomography (PET/CT) image shows moderate FDG avidity and maximal SUV of 4.5. There is no hypermetabolic axillary, mediastinal, or hilar lymphadenopathy.
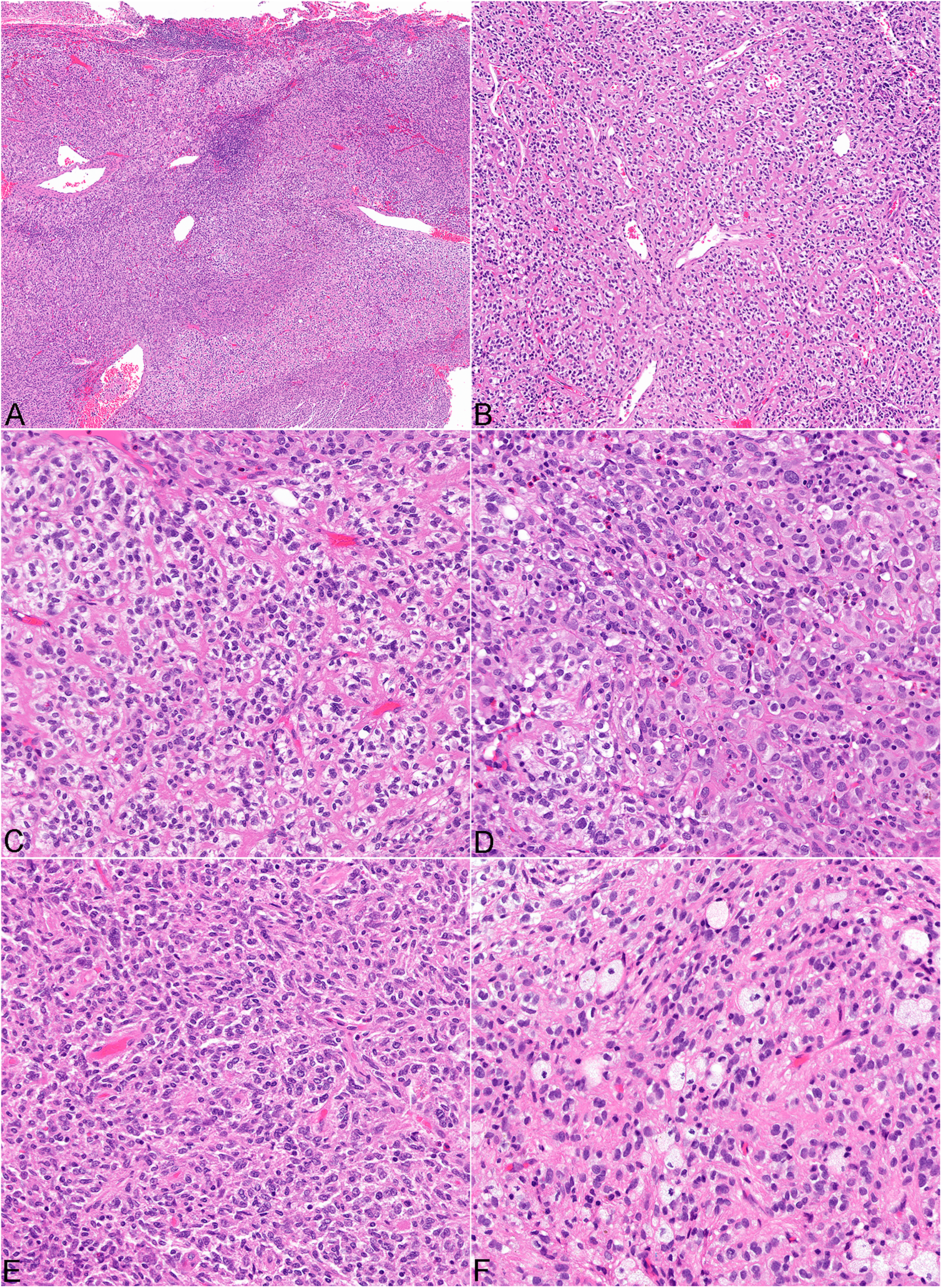
Light microscopic findings. A well-circumscribed tumor with vague lobular architecture is apparent at low magnification (A); H&E, original magnification ×2. The tumor is composed of sheets of predominantly epithelioid cells associated with aberrant slit-like vessels (B); H&E, original magnification ×10. The clear cell cytoplasmic changes are present throughout the tumor (C); H&E, original magnification ×20. The tumor also shows small foci of mild cellular pleomorphism (D), focal spindle cell morphology (E), and occasional clusters of intratumoral macrophages (F); H&E, original magnification ×20.
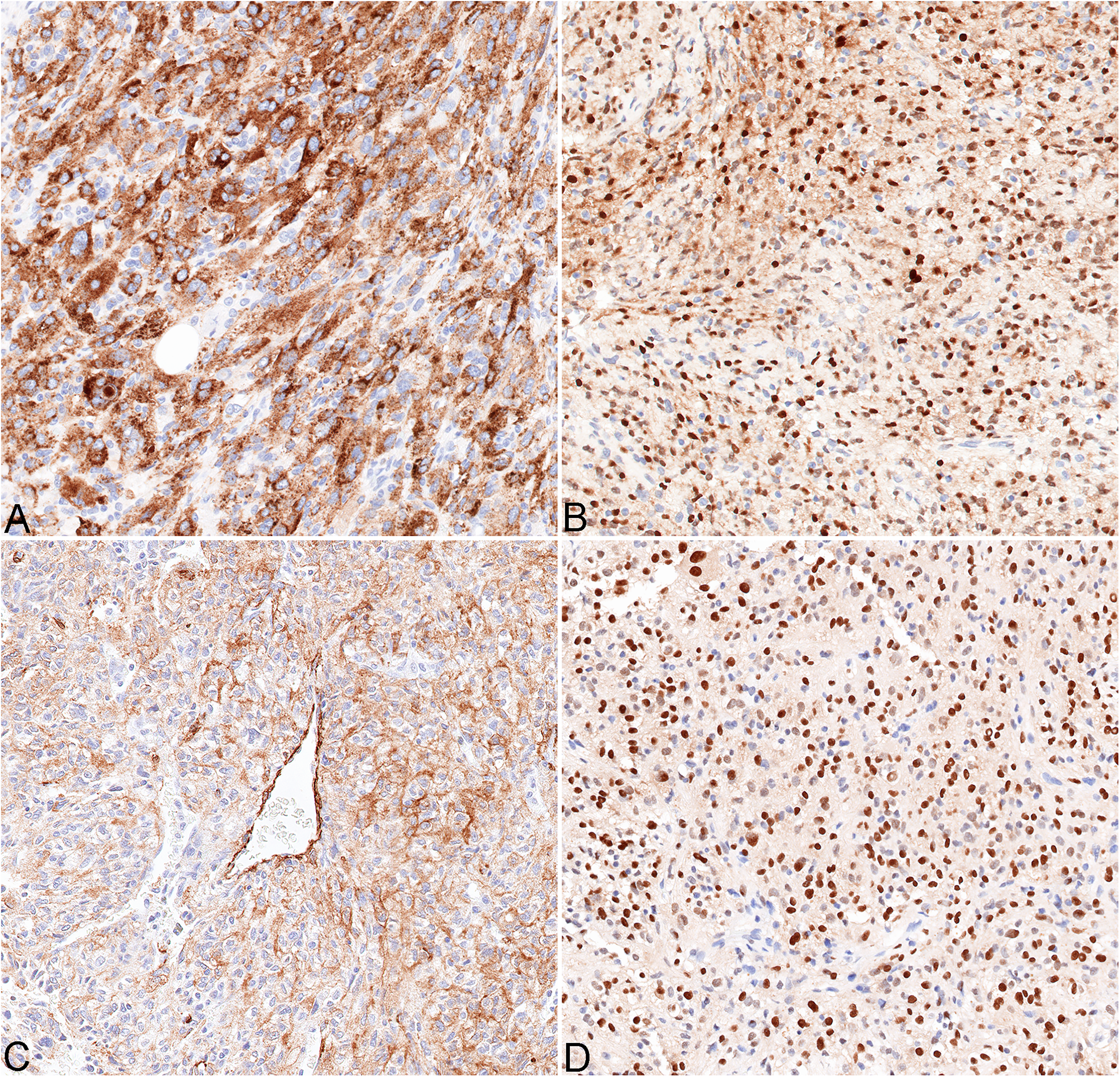
Immunohistochemical findings. The tumor shows melanocytic differentiation as evident by strong cytoplasmic expression of HMB45 (A) and nuclear expression of MITF1 (B). There is focal cytoplasmic expression of SMA (C) and diffuse nuclear expression of TFE3 (D). Immunohistochemistry, original magnification ×20.
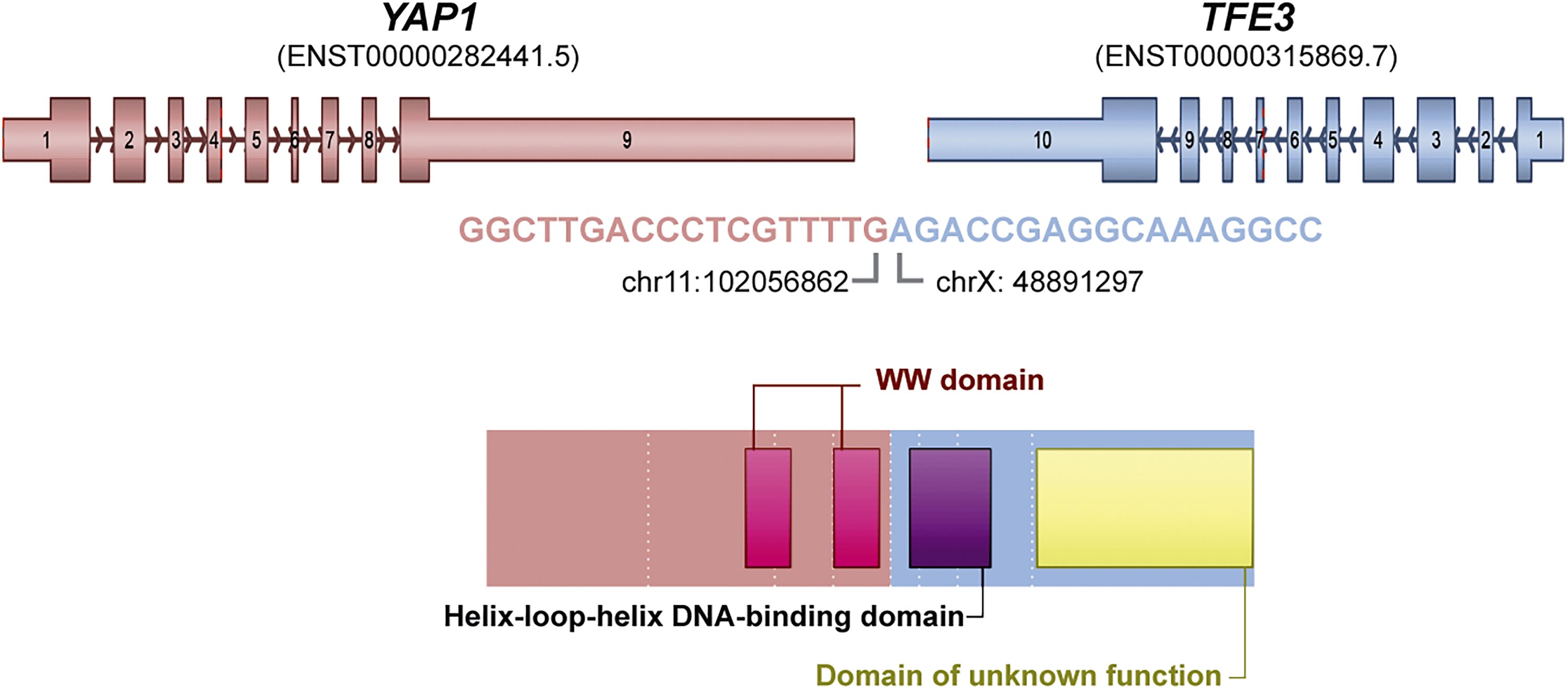
Molecular findings. The in-frame YAP1 exon 4 (breakpoint: GRCh37/hg19 chr11g.102056862) to TFE3 exon 7 (breakpoint: GRCh37/hg19 chrX g.48891297) fusion was identified by using a RNA-based hybrid-capture sequencing approach of 190 genes recurrently rearranged in solid tumors. Base-calling and file alignments were generated by BaseSpace (Illumina) with analysis for gene fusions carried out by the Arriba software package.
Discussion
“Sugar Tumor”: Historical Perspective and Classic Clinicopathological Findings
Originally named by Liebow and Castleman in 1971, PEComas of the lung were referred to as “sugar” tumor due to the high glycogen content evident on histochemical stains. 6 PEComas typically occur in the periphery of the lung and are often discovered incidentally. They can measure up to 7 cm in size 7 and are often benign in nature. 6
Currently, PEComas represent a family of rare mesenchymal tumors that share characteristic morphological and immunophenotypical findings. Bonetti et al first proposed the entity in 1992 after noting the distinctive perivascular epithelioid cells that expressed melanocytic antigens in both the clear cell “sugar” tumor of the lung and the epithelioid component of angiomyolipoma (AML) of the kidney. 8 Now, the entities in the PEComa family of tumors comprise lymphangiomyomatosis, 9 primary extrapulmonary sugar tumor, 10 clear cell myomelanocytic tumor of the falciform ligament, 11 and a group of nonspecified PEComas that arise in the soft tissue. 12 The perivascular epithelioid cell does not currently have a known normal counterpart. 13
Morphologically, PEComas are composed of epithelioid cells with cytoplasmic clearing and show minimal cellular atypia. The tumor cells are characteristically arranged around blood vessels and often infiltrate the smooth muscle of vessels. 14 By definition, PEComas typically co-express smooth muscle markers, including smooth muscle actin and desmin, as well as melanocytic markers including Melan-A, HMB45, and MiTF. 15 In a subset of PEComas, the presence of melanin pigment has been described. 16
Molecular Profile of PEComas
Conventional PEComas, including AML and lymphangioleiomyomatosis, have a strong association with tuberous sclerosis with characteristic TSC1/TSC2 loss of function seen in both syndromic and sporadic PEComas.1,2 TSC1 and TSC2 genes encode the hamartin and tuberin proteins respectively which interact to regulate cell proliferation, migration, and differentiation through inhibition of the rapamycin (mTOR) signaling pathway. 17 Consequently, previous molecular studies have shown a majority of PEComas with inactive TSC2 demonstrate upregulated mTOR signaling. 18
A distinct subset of PEComas have been described with defining TFE3 rearrangements and immunoreactivity for the TFE3 protein.15,19 These lesions share the morphologic and immunophenotypic findings consistent with the PEComa classification, but distinctively have a predilection for relatively young age at presentation (mean age 23.6 years) and exhibit an alveolar pattern of epithelioid tumor cells. 15 Notably, all reported tumors lack TSC2 gene mutations. 20 TFE3, located on Xp11.2, is a member of the microphthalmia-associated transcription factor family (MiT family) which also includes MITF, TFEB, and TFEC. 3 TFE3 rearrangements are associated with several other neoplasms including alveolar soft part sarcomas, Xp11 translocation renal cell carcinomas, clear cell stromal tumors of the lung (CCST-L), and epithelioid hemangioendotheliomas (EHE). Interestingly, TFE3 rearranged alveolar soft part sarcoma and renal cell carcinoma both share several morphologic features with TFE3 rearranged PEComas including alveolar/nested architecture and epithelioid cells.21,22 Given these similarities, Righi et al suggested that PEComa should be added to the MiT transcription factor family of tumors. The SFPQ (PSF)::TFE3 gene fusion has been found to be a common fusion in TFE3 rearranged PEComas, and has previously been described on at least 8 occasions.3,4,23 The YAP1::TFE3 gene fusion has been reported in CCST-L 24 as well as EHE. 25
Epithelioid Hemangioendothelioma
EHE is a rare malignant vascular neoplasm commonly arising in the soft tissue, bone, lung, skin, and liver. 26 Histologically, they are comprised of epithelioid cells in a myxohyaline stroma. 27 EHE has been characterized by the recurrent t(1;3)(p36.3;q25) translocation that results in the chimeric WWTR1::CAMTA1 gene fusion.28,29 A subset of EHE harbor the YAP1::TFE3 gene fusion 25 ; however, they are less frequent than the conventional WWTR1::CAMTA1 fusion. Notably, most EHE in this subset have a solid growth pattern with minimal intervening stroma. 30 Due to the lack of vasoformative properties, the PEComa in our patient is easily distinguishable from EHE.
Clear Cell Stromal Tumor of the Lung
CCST-L is a rare mesenchymal neoplasm, with only 25 tumors reported in the English language literature. The entity was first described in 2013 by Falconieri et al as a stromal tumor with endobronchial growth of clear tumor cells within a vascular background. 31 Despite the morphologic similarities to hemangioblastoma, CCST-L do not express S-100 or inhibin-α, which is the characteristic of hemangioblastoma. 32 Additionally, pulmonary hemangioblastoma is exceedingly rare, with only 4 reported in the English literature since 1943 33 and is a cardinal feature of Von Hippel Lindau (VHL) syndrome. 34 CCST-L are not associated with VHL but commonly express TFE3 and harbor TFE3::YAP1 fusions.33,35,36 PEComas can show at least focal spindle cell morphology, and therefore CCST-L is an important differential diagnostic consideration. However, PEComas characteristically express melanocytic markers while CCST-L do not, and use of immunohistochemistry helps to separate these tumors in most occasions. 24
While our manuscript was under review, a report describing 2 “inflammatory spindle cell PEComas” with the similar TFE3::YAP1 gene fusion was published. 37 The tumors occurred in elderly Japanese men who smoked and reportedly showed predominantly spindle cell morphology with a significant inflammatory component. One of the 2 tumors had increased mitotic counts and focal necrosis. The spindle cell morphology is a defining feature of CCST-L, however, the presence of myomelanocytic differentiation allowed the authors to classify the tumors as PEComas. Furthermore, the unique morphology and the presence of the TFE3::YAP1 fusion caused the authors to question whether the 2 tumors represent a distinct subset of PEComa, and whether the presence of the overlapping morphological and molecular features suggest a potential relationship between PEComa and CCST-L. The tumor detailed in our report occurred in a young never smoker adult woman and was predominantly composed of epithelioid cells. The tumor showed easily identifiable expression of myomelanocytic markers, had low proliferative and mitotic counts, and showed focal spindle cell and inflammatory changes. The morphologic overlap with CCST-L and the presence of the TFE3::YAP1 gene fusion in a PEComa documented in this report support a potential morphological continuum between these 2 entities.
List of Abbreviations
CT, computed tomography; PET/CT, positron emission tomography/computed tomography; EHE, epithelioid hemangioendothelioma; CCST-L, clear cell stromal sarcoma of the lung; AML, angiomyolipoma; SMA, smooth muscle actin; TFE3, transcription factor binding to IGHM enhancer 3; TTF1, thyroid transcription factor 1; MiTF, microphthalmia transcription factor; TSC, tuberous sclerosis complex.
Footnotes
Acknowledgments
The authors are thankful to Shawn Scally for excellent assistance in figures preparation.
Author Contributions
WM, MRA, JA, AG, and DMD participated in data collection; WM and KS wrote the manuscript text; MRA, SS, JA, AG, DMD, and KS edited the manuscript. The authors read and approved the final manuscript.
Consent for Publication
This study is exempt from the regulatory requirements of the National Institutes of Health (NIH) regarding studies on human subjects, based on the criteria described in section 4 of 46.101(b) of 45 CFR 46 “as research involving the collection or study of existing data, documents, records, if the information is recorded by the investigator in such a manner that subjects cannot be identified, directly or through identifiers linked to the subjects.” 38 According to the institutional guidelines, the patient's consent is not necessary for a case report with de-identified patient-specific information.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics Approval and Consent to Participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Trial Registration
Not applicable, because this article does not contain any clinical trials.
