Abstract
Background
.
Hormone receptor (HR) expression is a critical marker that plays a role in the treatment and management of breast cancer. Even if patients receive hormone treatment with a hormone positivity rate of over 1%, it is controversial at what level of positivity they benefit from treatment and contribute positively to their prognosis.
Methods
.
We retrospectively examined the estrogen receptor (ER) / progesterone receptor (PR) expression status, clinicopathological findings, and survival data of 386 patients who underwent surgery for breast cancer. ER/PR expressions of the patients were evaluated according to Allred, H-score and were also grouped according to staining percentages. Separate cut-off values were determined for each of these evaluation methods, and the prognostic power of these methods was investigated using receiver operating characteristic analysis.
Results
.
The prognostic power of all methods was found to be similar in terms of predicting survival. According to the staining percentage of the patients, survival was excellent if the ER value was >80% and the PR value was >1%.
Conclusions
.
All recommended methods for reporting HRs have similar prognostic power. However, in patients with high percentage staining for ER using these methods, the prognosis is excellent. As a result, we predict that if the percentage of ER staining is low, changing the treatment management of patients may be considered clinically.
Introduction
Hormone receptors (HRs), including estrogen receptor (ER) and progesterone receptors (PRs), are involved in tumorigenesis in breast cancers. HR promotes malignancy by increasing cell growth, differentiation, apoptosis, and angiogenesis. 1 These pathways can be interrupted by endocrine-targeted therapies, such as selective ER modulators, aromatase inhibitors, and selective ER degraders. 2
Immunohistochemical studies are the gold standard method used worldwide to determine HR status, since immunohistochemistry can be easily performed on paraffin blocks of tumors and is cost-effective.3,4 In surgical pathology practice, immunohistochemical study results are generally used together with prevalence and intensity parameters, and ER/PR staining evaluation is performed in this way. According to the College of American Pathologists (CAP), scoring systems such as Allred and H-Score, which are based on prevalence and intensity in reporting, are available. 5 However, the most commonly used method in clinical practice is to determine only the prevalence, which is equivalent to the staining percentage. Because, according to the American Society of Clinical Oncology (ASCO)/CAP guidelines, hormone-targeted therapies are beneficial in patients with a nuclear staining prevalence above 1%. 6 There are studies in the literature that suggest different cut-off values for HR status rather than 1%. According to the latest ASCO/CAP guidelines published in 2020, patients with HR status between 1 and 10% were reported to have low receptor positivity because they behave differently from patients with higher positivity. It is thought that these patients benefit less from hormone-targeted therapies, and relapse and progression occur more frequently.7,8 Based on different cut-off recommendations in the literature, the aim of our study is to compare the CAP's recommended reporting systems and to retrospectively review the cut-off values of these systems that predict the survival of patients.
Material Method
Patient Selection
Patients with breast cancer who underwent surgery at our hospital between 2010 and 2022 were identified by scanning the hospital database. Among 410 patients diagnosed with breast cancer, those who received neoadjuvant treatment (12 patients), those who were metastatic at the time of diagnosis (10 patients), and those who died within the first month after the operation (2 patients) were excluded and 386 patients were included in the study.
Study Design
Patient age, gender, clinical follow-up information of the patients, and radiological imaging results for outcome follow-up were obtained from the hospital database. Hematoxylin Eosin, ER, PR, human epidermal growth factor 2 (HER2), and Ki67 stained slides of the patients were re-evaluated by two pathologists (ÇÖ, OO) without knowing the first pathology report information. The staining status of the HRs is significantly affected by fixation. The specimens evaluated in our study had an average fixation time of 48-72 h. The unsuitable immunohistochemistry slides were re-stained with ER antibody (SP1, Ventana) and PR antibody (1E2, Ventana) on an automatic platform with the same stains routinely used at our center. Whether the staining on the ER/PR slides was homogeneous or heterogeneous, the staining prevalence as percentage values (1%-100%), and the staining intensity as weak, intermediate, and strong were recorded (Figure 1).
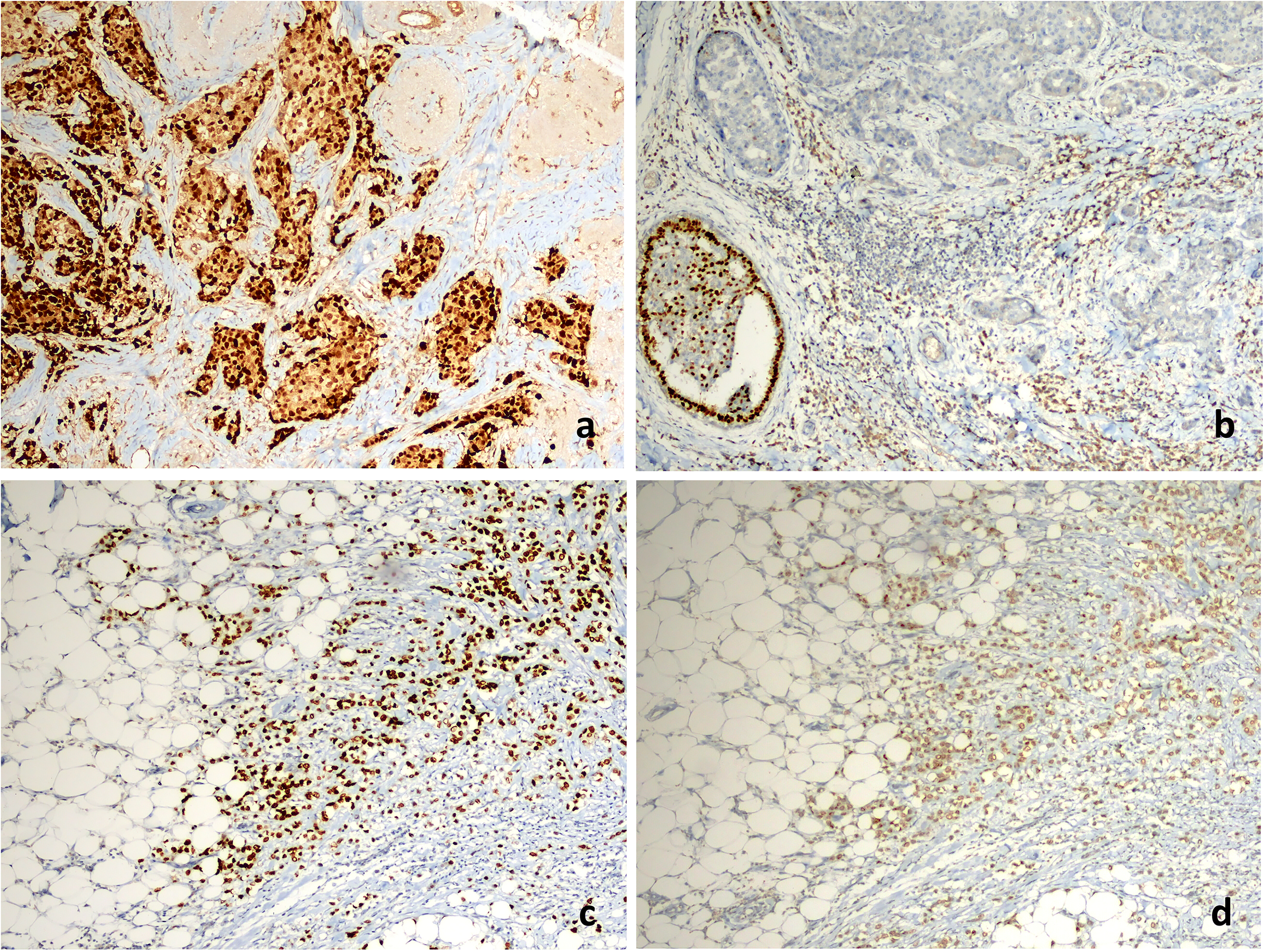
(a) A figure of an invasive ductal carcinoma patient with heterogeneous staining by ER immunohistochemistry; strong nuclear expression in 70% of tumor cells, Allred score: 7, H-score: 210 (anti-ER antibody ×100); (b) no immunoreaction with ER immunohistochemistry; Allred score: 0, H-score: 0 (anti-ER antibody ×100); (c) a figure of an invasive lobular carcinoma patient with heterogeneous staining by ER immunohistochemistry; strong nuclear expression in 80% of tumor cells, Allred score: 8, H-score: 240 (anti-ER antibody ×100); (d) weak intensity staining with PR immunohistochemistry in the same patient in (c); weak nuclear expression in 70% of tumor cells, Allred score: 6, H-score: 80 (anti-PR antibody ×100). Abbreviations: ER, estrogen receptor; PR, progesterone receptor.
For HER2, complete membranous staining above 10% was considered positive.5,6 The Ki67 proliferation index was considered to be 14% and above as high, and below as low.9,10 When molecularly subtyping patients, according to ASCO's recommendation, those with ER and PR staining above 1% were considered positive ER/PR. The patients were histologically subtyped according to the World Health Organization classification, graded according to the Nottingham grading system, and staged according to TNM.11,12,13
Patients were scored according to the scoring systems in Table 1. The ER/PR groups were created according to staining percentages. Cut-off values were re-determined by receiver operating characteristic (ROC) analysis based on the total scores obtained according to Allred, H-score, and survival status. Immunohistochemical staining for both receptors was evaluated as homogeneous staining if there was staining of equal intensity all over the slide, and as heterogeneous staining if there was staining of different intensities. This decision was made by evaluating all areas of the slide as a visual eyeball.
Allred, H-Score and ER groups for Estrogen and Progesterone Receptor Evaluation.
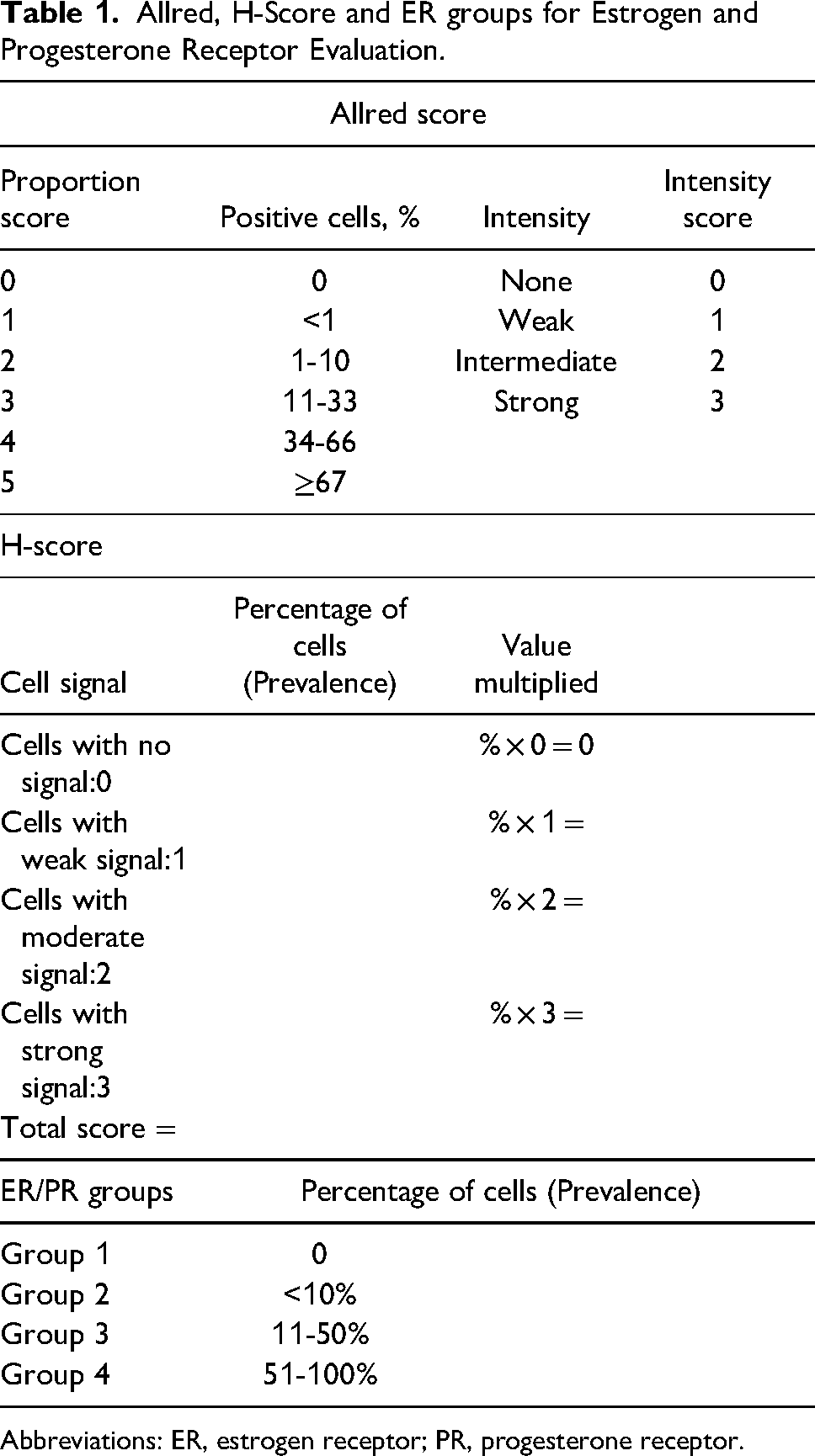
Abbreviations: ER, estrogen receptor; PR, progesterone receptor.
Statistical Analysis
Statistical analyses were performed using IBM SPSS Statistics (version 22.0; SPSS Inc., Chicago, IL, USA). The association between groups for categorical variables was analyzed using the chi-square (Pearson's chi-square) and Fisher's exact tests. ROC curve analysis was performed to determine the ideal cutoff value for survival prediction for all methods. A 5% type-1 error level was used to determine statistical significance.
Results
Homogeneous staining with ER was observed in 299 patients and heterogeneous staining was observed in 87 patients. For PR, homogeneous staining was observed in 279 patients, whereas heterogeneous staining was observed in 107 patients. No significant relationship was detected between the ER/PR staining pattern, clinicopathological parameters, and survival.
New cut-off Evaluation Results for Estrogen Receptor
According to the Allred score results for ER, the cut-off value in the ROC analysis was 7. Thus, 161 and 225 patients were evaluated in the ER-negative and ER-positive groups, respectively. As the nuclear and histological grades of the patients increased, more patients had an ER Allred score of <7. These patients had more metastases and more advanced stages (Table 2).
Relationship Between Different ER Scoring Systems and Clinicopathological Parameters.
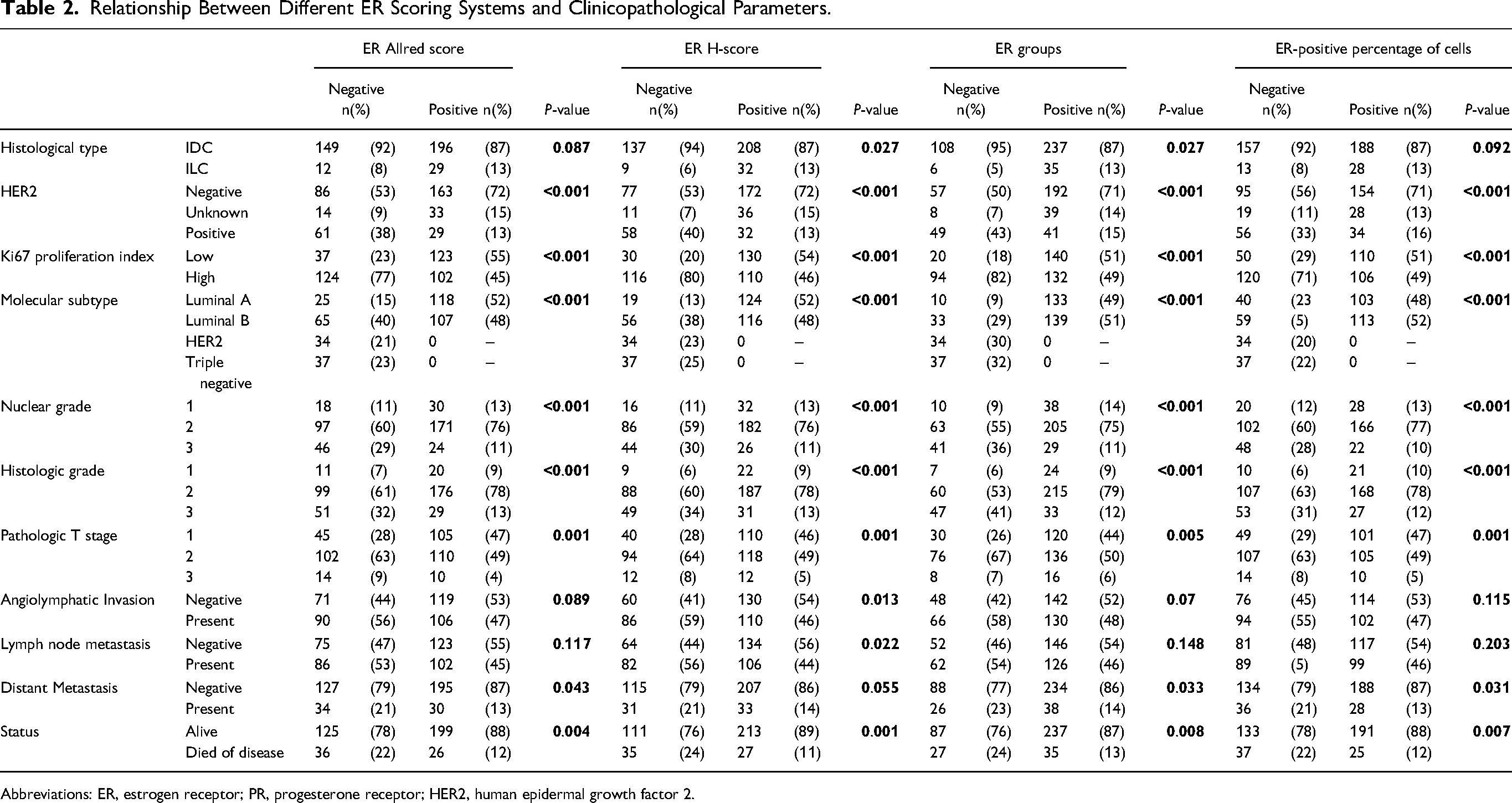
Abbreviations: ER, estrogen receptor; PR, progesterone receptor; HER2, human epidermal growth factor 2.
The newly determined cut-off value for the H-score was 185. Accordingly, 146 of the patients were in the ER-negative group and 240 were in the ER-positive group. In patients with an ER H-score <185, angiolymphatic invasion and axillary lymph node metastasis were observed in more patients, as well as higher nuclear and histological grade, similar to ER-negative patients according to the Allred score.
When the patients were grouped according to the percentage of ER staining, survival varied significantly in the group above 50%. No significant differences were observed in the <10% group. Accordingly, the ER was <50% in 114 patients and ER was above 50% in 272 patients. ER staining below 50% was associated with a higher nuclear and histological grade, advanced stage, and more distant metastases.
In the ROC analysis based on survival according to the percentage of cells positively stained with ER, the cut-off value was found to be 82%. The percentage of ER staining was below 82% in 170 patients and above 82% in 216 patients. Accordingly, in patients with ER positivity below 82%, higher nuclear and histological grade, advanced stage, and more distant organ metastases were observed.
The relationship between cut-off values found according to different ER scoring systems and clinicopathological parameters is shown in Table 2.
New Cut-off Evaluation Results for Progesterone Receptor
According to the Allred score results for PR, the cut-off value in the ROC analysis was 1. A total of 123 patients were PR-negative and 263 patients were PR-positive according to the Allred score. Patients with a PR Allred score < 1 had higher Ki67, higher nuclear and histological grade, and distant organ metastasis.
The new cut-off value found in the ROC analysis of the H-score results of PR expression was 110. The H-score was below 110 in 222 patients and above 110 in 164. Patients with a low H-score had higher Ki67, higher nuclear and histological grade, more advanced stage, and distant organ metastasis.
When grouped according to PR staining percentage, survival was significantly improved in the group with >10% PR staining. PR staining was below 10% in 123 patients and above 10% in 263 patients. In the group with PR < 10%, higher Ki67 expression, higher nuclear and histological grade, advanced stage, increased angiolymphatic invasion, and more axillary lymph node and distant organ metastases were observed.
According to the staining percentage of PR, a significant change in survival was observed at expression levels > 1%. Accordingly, 122 patients had less than 1% staining in PR, and 264 patients had >1% staining. In patients with PR expression below 1%, higher Ki67, higher nuclear and histological grades, increased angiolymphatic invasion, more axillary lymph nodes, and distant organ metastases were observed.
The relationship between cut-off values found according to different ER scoring systems and clinicopathological parameters is shown in Table 3.
Relationship Between Different PR Scoring Systems and Clinicopathological Parameters.
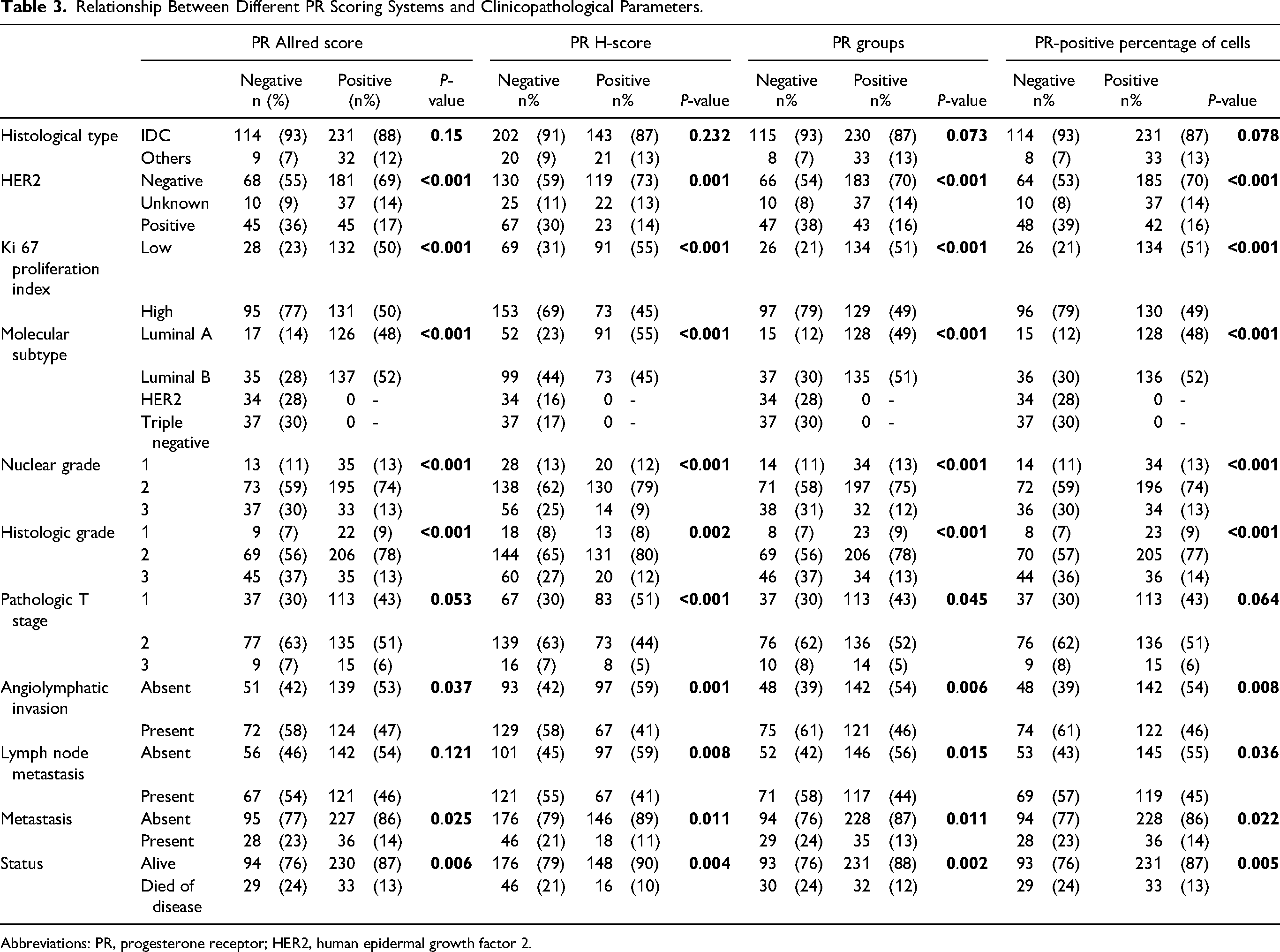
Abbreviations: PR, progesterone receptor; HER2, human epidermal growth factor 2.
Comparing the Survival Predictive Potential of ER/PR Scoring Systems
In patient slides, the effect of homogeneous or heterogeneous expression of ER and PR throughout the tumor on survival was investigated, but no significant relationship was found between both (For ER p:0.334, for PR p:0.845). The area under the curve (AUC) values for ER/PR showed similar results in terms of prognostic value in predicting survival in the ROC analysis of Allred, H-Score, percentage groups, and percentage of cell groups. AUC values and ROC analysis graphs of the groups are presented in Table 4 and Figure 2.
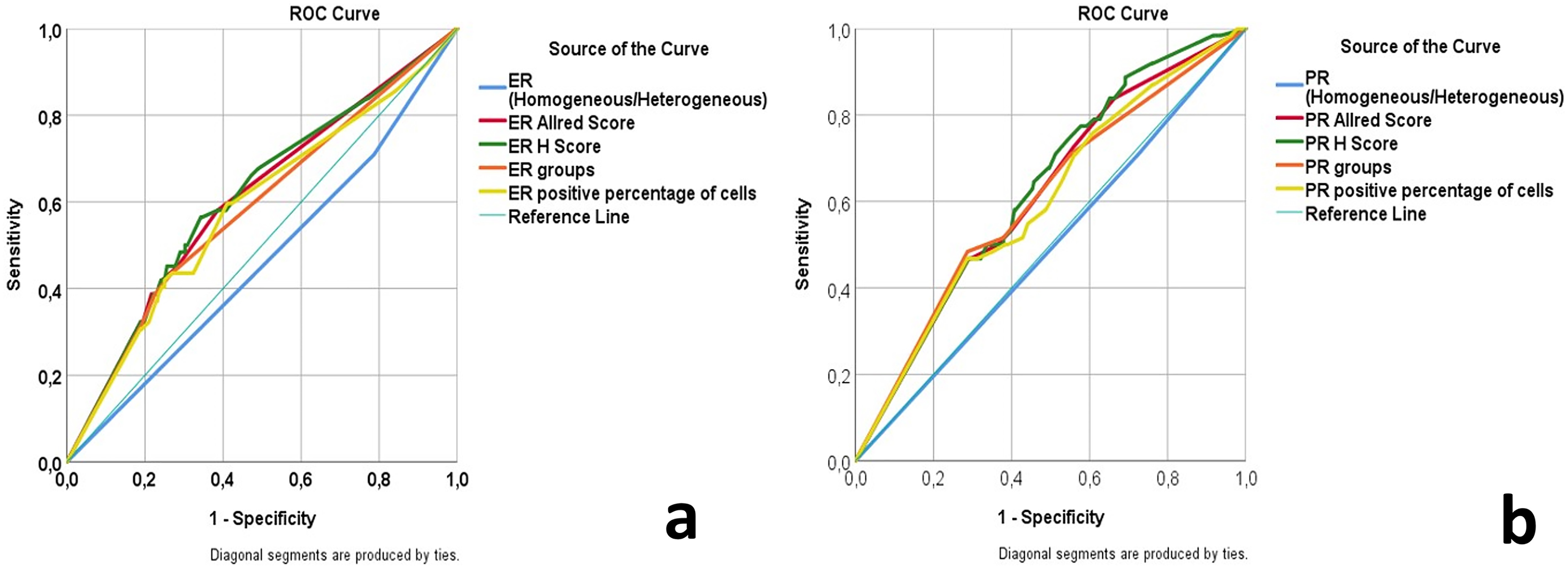
ROC analysis of groups created according to the scoring system of ER (a) and PR (b). Abbreviations: ER, estrogen receptor; PR, progesterone receptor; ROC, receiver operating characteristic.
Cut-off and AUC Values in ROC analysis of Allred, H-index, Percentage Groups and Percentage of Cells Groups for ER/PR.
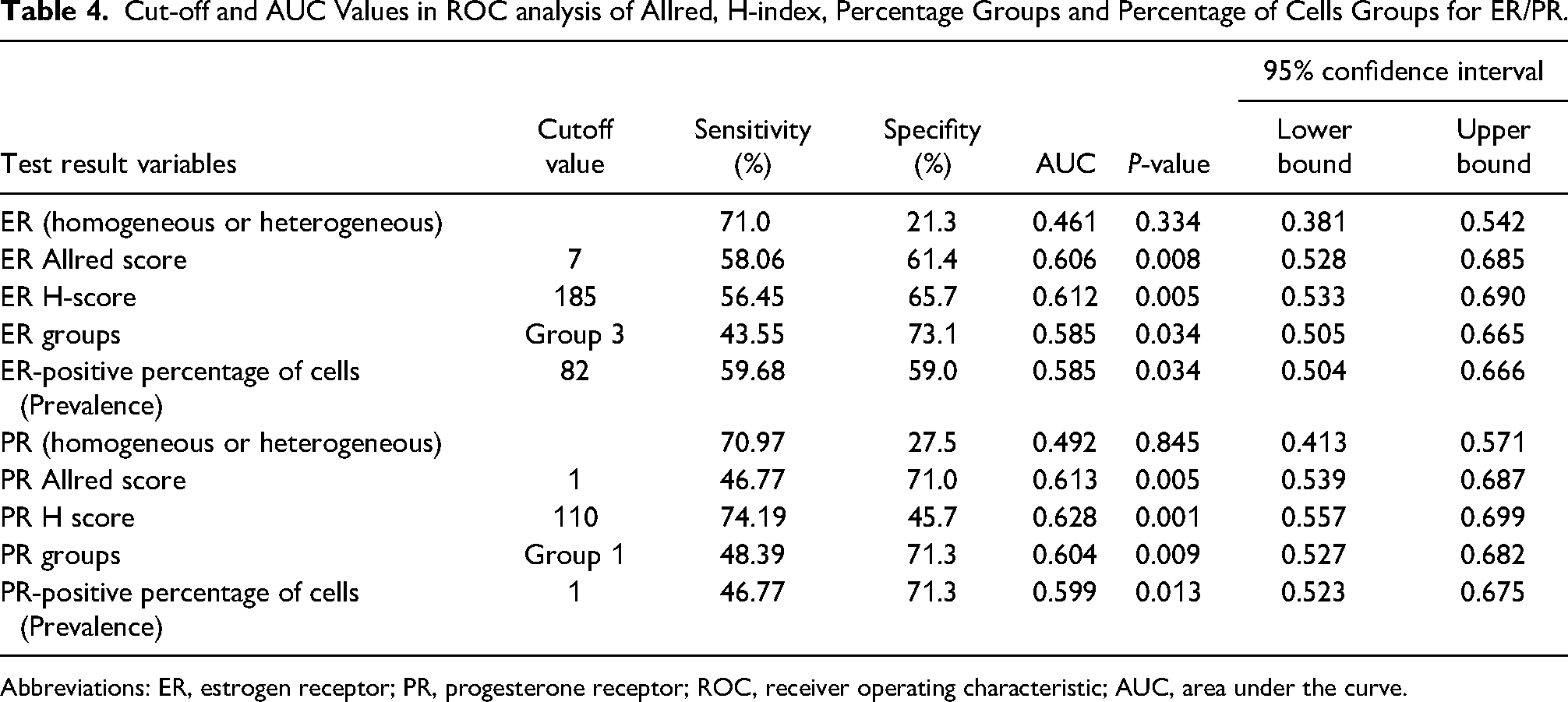
Abbreviations: ER, estrogen receptor; PR, progesterone receptor; ROC, receiver operating characteristic; AUC, area under the curve.
Discussion
HR expression is a critical marker that plays a role in treatment management in breast cancers. Although ASCO reports that all expressions above 1% can benefit from treatment, after numerous studies proved that expressions below 10% behave like Triple-negative tumors, ASCO included patients with expressions between 1 and 10% in the “low hormone expression” group. 6 Again, in the literature, it has been reported that over 75% benefit from hormone-targeted therapy in patients with Allred scores 7 and 8 (H-score equivalent to >100). Some argue lower scores provide less benefit. 14 Based on different opinions, it is important to determine which patient group benefits from endocrine-targeted therapies, as it will bring additional methods in the treatment of patient groups with low expression. Studying the pathways that suppress ER/PR expression may benefit in optimizing the treatment of these patients. 15
The gold standard method for evaluating ER/PR expression is a visual evaluation of immunohistochemical studies under a light microscope. In a study comparing the evaluation results of ER/PR expression between the human eye and automated systems, the superiority of the automated system over the human eye could not be proven. 16 However, since IHC can be affected by many factors during the tissue preparation phase, it must be repeated without being reported as negative in patients where the pathologist suspects fixation artifacts. 17 Besides problems in the fixation phase of the tissues, areas where tumor necrosis is observed may also appear as false staining loss. Nadji et al reported that when all these causes are excluded, focal staining of the ER is very rare. 18 In patients with focal staining, the histological appearance of ER-negative cells and pleomorphism should be investigated. In our study, homogeneous or heterogeneous ER/PR staining was evaluated according to the staining intensity, but no significant relationship was found between survival and other clinicopathological parameters and the staining pattern. Patients with obvious fixation artifacts were excluded from the study, but the majority of patients who were heterogeneous in terms of staining intensity were significant. This may be because the IHC stain reaches the cells in different amounts. Allred and H-score systems are systems that evaluate the intensity of staining as a parameter, as well as the prevalence of staining. 5 Hill et al argued that intensity, used as a parameter of these systems, is more correlated with survival than prevalence. 19 However, intensity evaluation is affected by various factors, such as the subjective evaluation of the pathologist, the concentration of the IHC stain and its distribution in the tissue. In addition, in this study, these systems and prevalence alone were found to have similar prognostic power in terms of predicting survival. For these reasons, when reporting hormone status, providing only prevalence data in daily pathology is a very reliable and more practical method.
Hormone status may also predict benefit from cytotoxic chemotherapies, in addition to predicting benefit from endocrine-related therapies. It is known that hormone-positive patients benefit less from chemotherapeutic treatment in neoadjuvant treatments. 20 In the Oncotype Dx study, it was reported that especially non-Luminal A hormone-positive patients benefited more from adjuvant chemotherapy than Luminal A patients.21,22 This information can be used as a supportive parameter for the addition of cytotoxic chemotherapy in treatment, especially in hormone-positive patients with low ER/PR expression. 23 Luminal A tumors are less chemosensitive than non-Luminal A tumors because ER/PR expression is a reflection of the gene expression profile. 24
The gene expression profile is an important guide in the decision for chemotherapy, especially in early-stage hormone-positive patients. However, this method is not easily accessible all over the world. Prat et al, in their study comparing studies based on gene expression profile and the scoring system called IHC4 based on ER, PR, HER2, and Ki67 values, showed that IHC-based scores of patients provided similar findings with gene expression profiles. 25 Again, in many studies, it has been reported that patients with ER expression below 10% are like Basal-like or HER2-positive tumors in terms of gene profile.26,27,28 Although IHC-based hormone staining status does not completely replace the expression profile, IHC-based evaluation of hormone expression provides precious information since it is more globally accessible and cost effective. With these results, ER/PR expression level can be used as a guiding parameter in chemotherapy decision-making, especially in early-stage patients where adjuvant chemotherapy is discussed.
Although it is thought that ER expression increases PR expression and therefore both hormone expressions are correlated, it is also known that various growth factors reduce PR expression.17,29 Supporting this, it is shown that HER2 is expressed at a higher rate in patients with ER + PR- than in patients with ER + PR+. 29 Similarly, Ono et al reported that PR expression was an important prognostic marker in Luminal A node-negative patients. 30 In our study, the relationship between ER and PR expression was not evaluated, but the relationship between PR expression and prognostic parameters was evaluated separately. According to our results, the cut-off values of PR are smaller than the values found for ER. This supports the idea that PR is more decisive than ER.
In our study, the cut-off value based on the prevalence of ER staining was found to be 82%. Accordingly, patients with ER expression >82% are expected to have an excellent prognosis. This 82% value appears to differ greatly from the value in the literature, where expression below 10% indicates a prognosis similar to ER-negative tumors.26,31 However, our study was designed to determine the optimal cutoff value that determines survival and differs from these studies in the literature. Similar to our study, Richard et al, in their study evaluating the prevalence of staining of HRs, showed that expression above 80% for ER was a positive prognostic parameter. 32 According to these researchers, as the percentage of ER positivity increased, local recurrence decreased and overall survival improved. In the same study, although survival tended to be better in patients of expression above 80% for PR, this was not found to be statistically significant. In our study, PR expression value was found to be different from ER. This may be due to other parameters affecting PR expression mentioned previously.
Makhlouf et al investigated the relationship between ER expression and response to endocrine therapy in two large cohorts consisting of 7559 and 1047 patients. 33 According to this study, the response to endocrine therapy was optimal when ER expression was 100%, but differences in the response to treatment occurred when ER expression was below 100%. With ER expression below 50%, there was a significant decrease in response to treatment, whereas with ER expression below 9%, the results were similar to those of ER-negative patients. Similarly, there were significant differences among the H-scores of 30, 100, and 200. In our study, high H-score, high Allred score, and high percentage of ER expression were found to be associated with good prognosis, as in the study by Makhlouf et al Based on these results, it can be predicted that patients with high ER expression will benefit greatly from endocrine treatment. However, there were various limitations in this regard; for example, other characteristics of the patients, such as HER2 status, Ki67 level, and histological type, which affected their response to treatment and survival, were not homogeneous. In addition, since our study was designed retrospectively, it is not known whether the materials of all patients had optimal fixation times and undetected technical problems.
Conclusion
Although the effectiveness of hormone-targeted therapy is known for hormone expression above 1%, it is still controversial which expression value can be used as a prognostic and therapeutic cut-off. According to the results of our study, prognosis improves perfectly in the presence of high ER expression. In addition to the prognostic and predictive value of our results, the findings also provide insight into the investigation of additional treatment methods, especially in patients with early-stage low hormone expression.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics Approval
Our study's ethics committee approval was obtained from Recep Tayyip Erdoğan University Faculty of Medicine, non-interventional clinical research ethics committee chairmanship
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Trial Registration
Not applicable, because this article does not contain any clinical trials.
