Abstract
On examination of a breast mass surgically excised in a 69-years-old woman, a pure invasive micropapillary carcinoma (MPC) was diagnosed (Figure 1). At close examination, intensely eosinophilic syncytial-multinucleated giant cells (CD68+) percolating the stromal bands were identified (Figure 1). The breast carcinoma illustrated here shows therefore a combination of 2 rarities, namely, an invasive micropapillary growth pattern and an osteoclast-like giant cell (OGC) component. The World Health Organization blue book classifies the “carcinoma with osteoclast-like stromal giant cells” among rare variants of invasive carcinomas of no special type (IC-NSTs) 1 ; however, OGCs can also accompany a variety of breast cancer special types (cribriform, tubular, mucinous, papillary, lobular, squamous and other metaplastic patterns1,2). Identification of giant cells populating MPCs can be challenging as they feature the same size as the micropapillae and only differ in staining (more eosinophilic cytoplasm) (Figure 1).
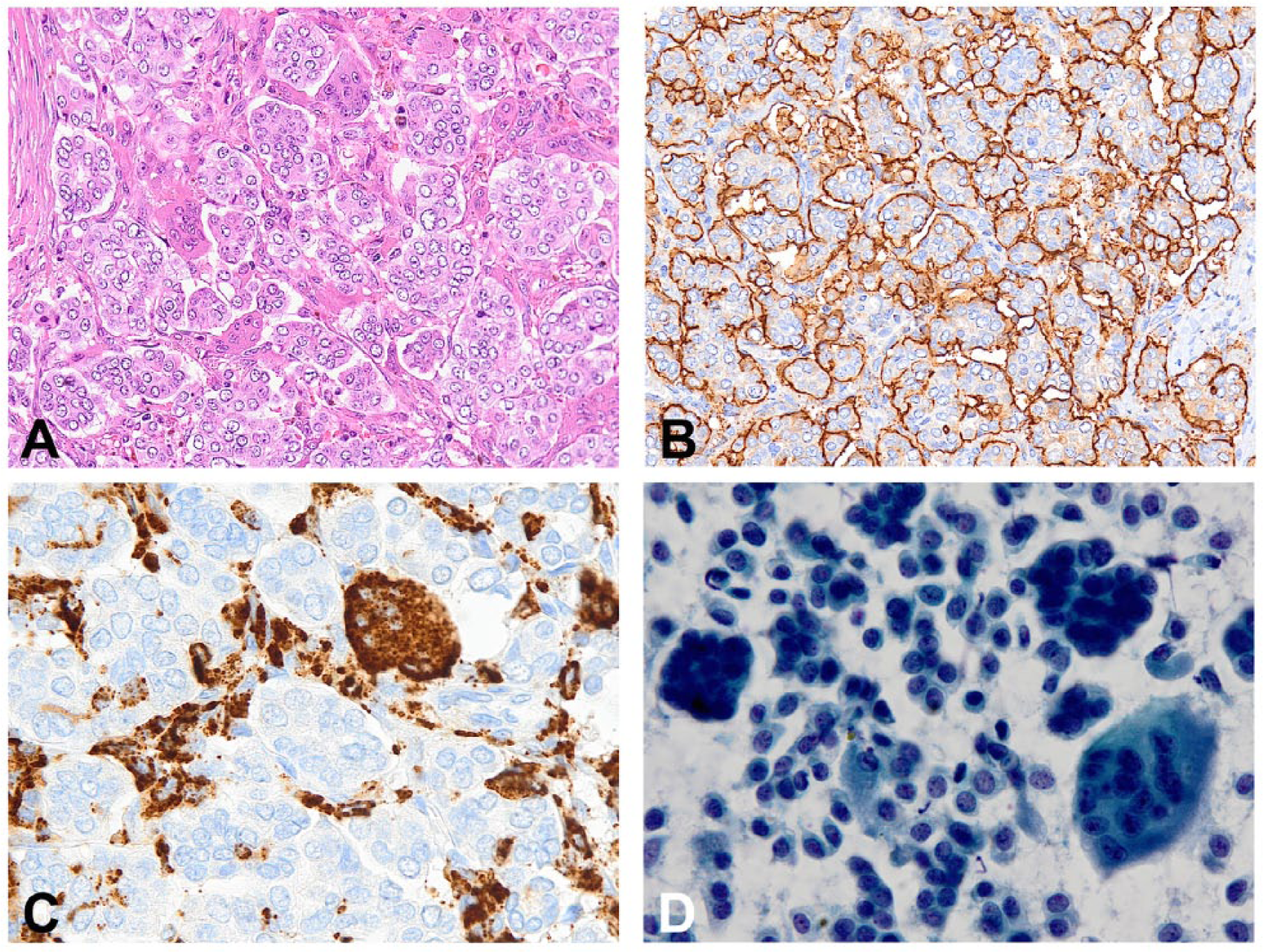
Micropapillary carcinoma of the breast with an osteoclast-like giant cell component. Pure invasive micropapillary carcinoma: neoplastic cells are arranged in small cell clusters immersed in a spongy stroma (A), showing the so-called “inverted polarity” (MUC1 expression lining the stroma-facing border of the morulae) (B). Intensely eosinophilic syncytial-multinucleated giant cells of histiocytic origin (CD68+, MUC1−) percolating the stromal bands (A, C). Following review of cytological specimens of presurgical diagnosis, multinucleated giant cells scattered among small cell clusters of neoplastic cells were also identified (D).
Osteoclast-like giant cells are hypothesized to derive from macrophages by syncytial fusion but not by mitosis without cell division 3 ; however, the mechanism of OGC formation and accumulation in breast carcinoma is still largely unknown. 2 An open question remains about their prognostic significance: a study on metaplastic carcinomas with an OGC component reported a 5-year survival rate fairly similar to that of patients affected by IC-NST. 1 Further studies on large cohorts would be needed to definitely ascertain whether or not a diagnosis of breast carcinoma with osteoclast-like stromal giant cells may affect patient clinical outcome. 1
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: We would like to acknowledge AIRC grant support (MFAG 13310) to CM.
