Abstract
The aim of this systematic review was to (a) identify the specific information and support needs of family members caring for ABI survivors and (b) assess the effectiveness of current support systems and resources available. A comprehensive search of the literature was carried out, focusing on studies that were published between the years 2000 and 2025. Seventeen studies met the inclusion criteria. The review employed a narrative synthesis approach to collate findings across papers. The analysis identified five key themes: ABI Knowledge, The Strain of Unsupported Transitions, Emotional and Financial Cost, ABI Support Groups, and Supporting Social Connectedness. The findings indicate significant gaps in current systems of support and information for families of individuals with ABI. Inconsistencies in the delivery of ABI-related information during the acute stage create stress among family members. The post-acute stage presents challenges with instrumental support and insufficient emotional and peer support. This review demonstrates the importance of a more flexible, person-centered approach in supporting families of ABI relatives. Providing tailored interventions and information, with consistent social welfare support are vital in improving the quality of life for both caregivers and ABI survivors.
Introduction
Acquired brain injury (ABI) is defined as any form of damage to the brain occurring after birth, most often due to strokes, tumors, infections, or direct blows and/or trauma to the head. Affecting approximately 69 million people annually worldwide, ABI has broad social and economic impacts, with over 13 million individuals affected by strokes alone (Dewan et al., 2018). Advancements in medical care have increased survival rates following ABI, creating a growing population living with its life-altering, long-term effects (Fins, 2015). These effects vary widely depending on the injury severity and location but may include cognitive, physical, sensory, behavioral, and emotional impairments (Feigin et al., 2013). The long-term nature of the needs of individuals with ABI means that they may require family members to assume caregiver roles to support them in their daily lives (Kratz et al., 2017).
Despite evidence of the profound impact of caregiving responsibilities on families having been documented as long ago as the 1970s (Romano, 1974), long-term support systems for individuals with ABI and their families remain limited (Norman et al., 2023). Families of individuals with ABI often report feeling burdened with managing the daily caregiving needs of their loved ones (Juengst et al., 2022; Lieshout et al., 2020). These responsibilities can include “activities of daily living” such as feeding, washing, and dressing, but can also include wider activities such as managing and organizing appointments, attending appointments as advocates, and meeting transport and communication needs (Muliira et al., 2024). This can lead to emotional stress, financial strain, and social isolation for caregivers (Bermejo-Toro et al., 2020; Kokorelias et al., 2020). This burden intensifies when their loved ones with ABI are unable to return to work, especially if they were previously the primary financial provider. A systematic review of papers reporting post-injury employment prevalence found that over 50% of individuals with moderate or severe TBIs were able to return to work post-injury (Gormley et al., 2019). Without adequate access to long-term care and support, families face subsequent experiences of significant emotional distress and uncertainty (Hickman & Douglas, 2010) with wide-reaching social and economic challenges (Azman et al., 2020).
Despite the crucial role of family members, there is a notable lack of standardized support available to them following ABI (Gan et al., 2010; Norman et al., 2020). Research has found that families struggle with a lack of sufficient access to information and support services, encountering barriers that hinder their ability to manage the behavioral and emotional challenges posed by ABI (Norman et al., 2023; Pindus et al., 2018). Families frequently report unmet needs, highlighting the requirement for accessible, practical support to improve their well-being alongside ABI survivors. Guidance from healthcare professionals is essential to help families adapt and navigate information and support services to understand the long-term implications of ABI. Education surrounding the effects of ABI and access to social and psychological support networks are fundamental in enhancing caregivers’ resilience and coping abilities (Kitter & Sharman, 2015).
This systematic review aims to build upon the findings of previous research by Pindus et al. (2018) and Norman et al. (2023) by identifying the specific information and support needs of family members caring for ABI survivors and assessing the effectiveness of current support systems and resources. Specifically, this systematic review aimed to (a) evaluate the types of information and support family members need while caring for individuals with ABI, and (b) assess the effectiveness of the support and information currently available.
Methods
This systematic review followed the methodological framework of Arksey and O’Malley (2005). The process consists of a clearly defined research question, the identification of relevant research studies, with specific inclusion and exclusion criteria. Data were then extracted and pooled. Each stage of the research process is described in greater detail below.
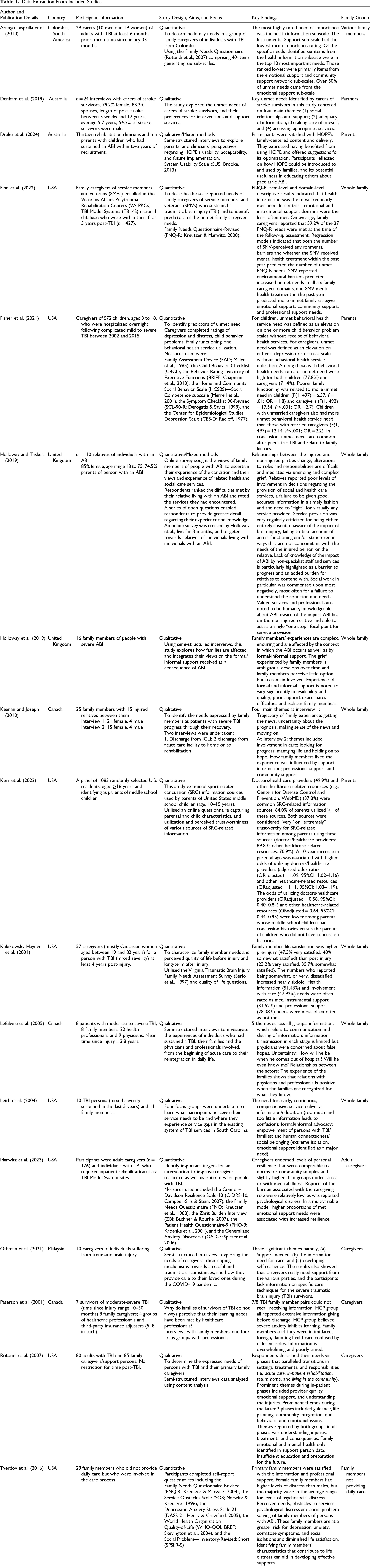
Author and publication year Participant information Main findings relating to support and information needs Recommendations and conclusions
Results
Across the seven databases, and through review of the reference list of relevant research articles, 230 papers were obtained. Following discussions between the authors and the removal of duplicate studies and those focusing on experiences not relevant to the review, 213 studies were excluded. The final number of studies that met the inclusion criteria was 17 (see Figure 1 for a flowchart of this process). Of the included studies, seven were quantitative studies, eight were qualitative, and two utilized a mixed methods approach. Methodological rigor and quality of reporting varied across the studies, providing a complex landscape to navigate when synthesizing the data. Studies represented populations across the globe, with projects recruiting from South America (1), Malaysia (1), the United Kingdom (2), Australia (2), Canada (3), and the USA (8). It is clear from these studies that similar difficulties were reported by families after ABI, despite geographic location and differences in societal structures. The included 17 studies were coded, and five themes were developed, using the approach outlined by Popay et al. (2006): (a) ABI Knowledge, (b) the strain of unsupported transitions, (c) Emotional and Financial Cost, (d) ABI support groups, and (e) Supporting Social Connectedness (see Table 1). Where studies were quantitative in nature, summaries and findings, and the author conclusions were collated for inclusion within the thematic analysis.
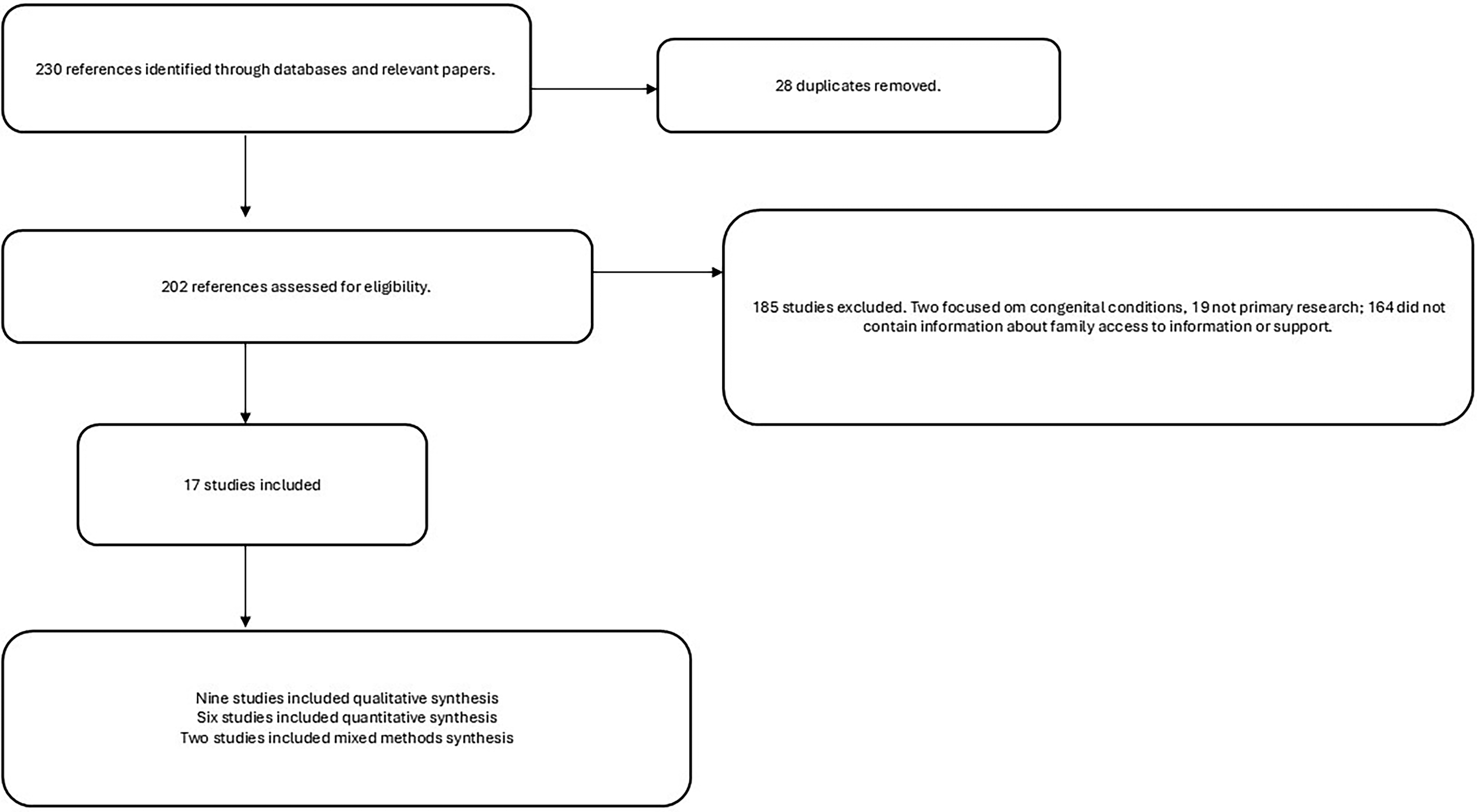
Flowchart of the systematic review process.
Data Extraction From Included Studies.
ABI Knowledge
Family members expressed a strong need for clear, consistent, and trustworthy ABI information. Six studies (Denham et al., 2019; Finn et al., 2022; Holloway & Tasker, 2019; Keenan & Joseph, 2010; Kerr et al., 2022; Kolakowsky-Hayner et al., 2001) highlighted that family members greatly rely on healthcare professionals for information, particularly during the acute stage of care. However, information was reported to be provided inconsistently, leading to frustrations for family members (Holloway et al., 2019; Holloway & Tasker, 2019; Paterson et al., 2001). Additionally, discrepancies in perceptions of healthcare professionals and family members regarding the appropriateness of ABI information provided at discharge often caused families to need to seek ABI support from voluntary organizations (Holloway et al., 2019). A single point of access to information and care needs was noted as crucial for family members (Holloway et al., 2019; Paterson et al., 2001). Families frequently struggled with inconsistent information, resulting in frustration and delays in accessing necessary resources.
The Strain of Unsupported Transitions
At the post-acute stage, six of the 17 studies described family members expressing a need for more comprehensive information to adequately prepare for their long-term responsibilities and adapt to the new home environment (Denham et al., 2019; Holloway et al., 2019; Kolakowsky-Hayner et al., 2001; Lefebvre et al., 2005; Othman et al., 2021; Rotondi et al., 2007). Health information was provided in some instances (Finn et al., 2022) at this stage of care; however, there was an overall lack of emotional support and access to peer support (Kolakowsky-Hayner et al., 2001; Marwitz et al., 2023). Practical assistance and the impact of transportation barriers were highlighted as ongoing problems with no support provided (Denham et al., 2019; Kolakowsky-Hayner et al., 2001). Families felt that their quality of life and overall satisfaction reduced post-injury, with a need for long-term support and frequent follow-ups being seen as vital for managing the changing needs (Holloway et al., 2019; Kolakowsky-Hayner et al., 2001). The transition from acute to post-discharge care left families unprepared for the long-term responsibilities they face. While basic healthcare needs are often met, significant gaps in emotional, peer, and practical support remain.
Emotional and Financial Cost
The personal well-being of family members was identified as a significant concern in six of the 17 studies reviewed, with high levels of distress and depression reported (Fisher et al., 2021; Holloway et al., 2019; Holloway & Tasker, 2019; Marwitz et al., 2023; Paterson et al., 2001; Tverdov et al., 2016). Emotional support, such as that available through counseling services and community, peer-led support, was viewed as valuable, yet largely unavailable for families (Arango-Lasprilla et al., 2010; Finn et al., 2022; Holloway et al., 2019). The emotional burden for family members to care for their loved one following ABI was intensified by financial challenges they reported facing, which negatively impacted their mental health, suggesting the need for greater access to professional support and resources to manage these challenges (Marwitz et al., 2023; Paterson et al., 2001; Tverdov et al., 2016). Emotional and financial stresses affected caregivers' mental health, demonstrating the need for accessible mental health services and community support (Marwitz et al., 2023).
ABI Support Groups
Five out of the 17 studies emphasized support groups and community networks as highly valued by family members, as they offer emotional support and provide practical support with their loved one's rehabilitation process (Arango-Lasprilla et al., 2010; Drake et al., 2024; Holloway et al., 2019; Keenan & Joseph, 2010; Rotondi et al., 2007). Positive experiences with support groups were linked to clear communication, empathy, and inclusion in care decisions. The Heads Together Online Peer Education (HOPE) program was one noted intervention that offered the flexibility families needed, using storytelling to share experiences and hear from other families (Drake et al., 2024). The benefits of community support were observed, with positive long-term well-being outcomes for family members who continued to have access to these support groups (Rotondi et al., 2007). Support groups provide essential emotional and practical benefits to families, helping them maintain a sense of engagement throughout the recovery process and reducing feelings of isolation.
Supporting Social Connectedness
Six out of the 17 studies revealed unmet social care needs for family members, indicating that support from the community and a sense of social belonging were important yet often unmet needs (Arango-Lasprilla et al., 2010; Denham et al., 2019; Leith et al., 2004; Marwitz et al., 2023; Rotondi et al., 2007; Tverdov et al., 2016). Many families reported barriers to accessing support due to time constraints, financial challenges, and a lack of government or local authority assistance (Denham et al., 2019; Finn et al., 2022; Rotondi et al., 2007). Financial issues were often challenging for family members, impacting their ability to meet instrumental needs, such as providing transportation to their loved one, which contributed to increased levels of depression (Tverdov et al., 2016). Access to continuous professional and community resources was highlighted as essential for family members (Marwitz et al., 2023). Social care and welfare needs, including financial support and a sense of community belonging, were found to be needs broadly left unmet due to barriers to access.
Discussion
The systematic review explored the experiences of family members seeking information and support while providing care for relatives with an ABI. The findings highlight the profound and multifaceted challenges faced by families, underscoring the need for more tailored and flexible services. Rather than integrating families into existing systems, services must adapt to their unique circumstances. Five key themes emerged with families needing support and information around ABI Knowledge, particularly in the post-discharge stage after injury. Papers identified the emotional and financial support needs of families, and a desire for access to support groups, and support with improving social connectedness. The review highlighted a need for more effective support and information needs.
Interestingly, of the 17 papers identified within this review, only one explored the effectiveness of specific intervention support for families post-ABI. While other papers did exist that were excluded from this study, this highlights a distinct shortcoming in the existing literature. While Brain injury itself has received limited attention in the social care research field (Norman et al., 2023), there is an even greater gap pertaining to family and carer experiences. This highlights the invisibility of carers within this field. With many countries moving increasingly towards a model of “care in the community,” there is an urgent need for research to take more seriously the role of family carers (Skuse, 2017) and to take time to understand and address their needs.
ABI Knowledge
The review identified an important gap in the quality and consistency of information provided to ABI relatives’ family members. While families rely heavily on healthcare professionals for ABI information (Denham et al., 2019; Finn et al., 2022; Holloway & Tasker, 2019; Keenan & Joseph, 2010; Kerr et al., 2022; Kolakowsky-Hayner et al., 2001), the delivery of information is often inconsistent, leaving families feeling unsupported and anxious (Holloway et al., 2019; Holloway & Tasker, 2019; Paterson et al., 2001). Current practices fail to address the emotional and cognitive burdens families face, especially during the acute stage of ABI. A personalized approach to communication from healthcare professionals, which emphasizes appropriate timing, clarity, and consistency, may help to reduce uncertainty and empower families in their caregiving roles (Holloway et al., 2019; Paterson et al., 2001).
The Strain of Unsupported Transitions
The transition from acute to long-term care is a critical, yet under-supported period for families. The review revealed that instrumental needs, such as transportation, are particularly unmet for disadvantaged families (Denham et al., 2019; Kolakowsky-Hayner et al., 2001). Moreover, a lack of emotional support and access to peer support exacerbates stress and diminishes the quality of life for families (Kolakowsky-Hayner et al., 2001; Marwitz et al., 2023). Healthcare professionals must adopt a dynamic and empathetic approach to families’ evolving needs during this stage, offering personalized support that addresses their practical and emotional challenges over the long-term stages of care.
Emotional and financial cost: Caring for ABI relatives significantly affects family members’ health, with high levels of stress, depression, and anxiety commonly reported (Fisher et al., 2021; Holloway et al., 2019; Holloway & Tasker, 2019; Marwitz et al., 2023; Paterson et al., 2001; Tverdov et al., 2016). While services like counseling and peer support are beneficial, barriers to accessing services exist, with family members having limited funds and time to engage effectively (Arango-Lasprilla et al., 2010; Finn et al., 2022; Holloway et al., 2019; Norman et al., 2023). There is a need for more widely available support that is free and flexible in delivery to enable family members to engage despite their caregiving roles.
ABI Support Groups
Support groups offer a valuable resource for emotional and practical support. Interventions such as the HOPE program demonstrate encouraging results in fostering resilience and community among caregivers (Drake et al., 2024). Tailored support that meets diverse needs could mitigate feelings of isolation and enhance the caregiving experience. Support groups are called upon to strive to improve inclusivity and emotional services to ensure they can better address the wide-ranging needs of families (Arango-Lasprilla et al., 2010; Drake et al., 2024; Holloway et al., 2019). However, inclusivity and accessibility remain areas for improvement, with minimal numbers of family members from ethnically diverse groups accessing support groups (Rotondi et al., 2007). There is also a need to ensure that facilitators of such groups are suitably trained, enabling them to provide sensitive and appropriate support to a range of family members with different life stories and backgrounds (Holloway & Tasker, 2019; Norman et al., 2023; Odumuyiwa et al., 2019).
Supporting social connectedness: The review identified systemic inadequacies in social welfare and access to social connectedness for families of ABI survivors. Issues such as frequent reassessments for carers' benefits, inconsistent government support, and a lack of social networks place additional stress on families (Denham et al., 2019; Leith et al., 2004; Marwitz et al., 2023; Rotondi et al., 2007; Tverdov et al., 2016). Across the countries reported by the papers, there is a general lack of legislation that supports carers' rights, particularly where individuals are being cared for by family. This is further complicated when the nature of the caring responsibilities falls outside of personal care and support with activities of daily living. Further action is needed to provide stable and comprehensive financial and social support to family members who are trying to juggle supporting the families financially and caring for loved ones (Kratz et al., 2017).
This review has demonstrated gaps in the information and support provisions in current health and social care for families after brain injury. Papers have identified that support is required for families to address their lack of knowledge of ABI early on in their loved one's journey, and guidance in how to manage brain injury after the initial acute stage of injury (Bermejo-Toro et al., 2020; Kokorelias et al., 2020; Whiffin et al., 2021), and these papers clearly identify a need for emotional, financial, and social welfare support for families after ABI.
Limitations
Only papers published in English were included in this review, making the findings largely focused on the Western world. Due to the lack of data pertaining to tested interventions in the areas of support and information for families, this review was unable to provide any objective conclusions about the overall effectiveness of existing support and information services, a factor that reflects the lack of high-quality studies undertaken in this area.
Future research should address the gaps identified by exploring family experiences in larger, more diverse populations, particularly with respect to social, emotional, and financial needs. Studies need to focus on intervention design models with comprehensive data that demonstrates efficacy of approaches. Furthermore, a centralized source for clear and reliable information could help to provide more readily accessible resources for families following ABI. Improving resources for family members would help to reduce stress and promote greater well-being for caregivers and enable them to better support their loved one with a brain injury.
Conclusion
This systematic review highlights the significant challenges faced by families of ABI survivors, emphasizing the necessity of a more personalized and flexible approach to caregiving support. While programs of support and information are available, substantial gaps remain in addressing families’ information, emotional, financial, and social welfare needs. To improve outcomes for caregivers and their relatives, it is imperative that health and social care systems prioritize support and information services for families after brain injury.
Footnotes
Ethical Considerations
No ethics application was submitted for this systematic review.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
A data extraction table is available to summarize data. All data can be accessed from the corresponding author.
Appendix A: Search criteria
Concept 1—Acquired Brain Injury
Concept 2—Family
Concept 3—Information needs
Concept 4—Support needs
Information combined search
Support combined search
