Abstract
Social support for family members who care for a relative with dementia can mitigate caregiving burden. Yet, in that evidence points to these caretakers as often experiencing isolation and loneliness while providing dementia-related care, a need remains to better understand factors contributing to their adverse support experiences. Accordingly, this study applies sensitive interaction systems theory (SIST) to examine how caregivers’ direct versus indirect support-seeking behaviors relate to the quality of support responses they receive from a member of their social network. Associations between network support responses and caregiving burden are also investigated. Family caregivers (
More than 11 million family members in the United States care for relatives living with some form of dementia (Alzheimer's Association, 2023). In addition to providing increasing amounts of daily assistance, these family caregivers make significant care decisions for their relative (Kwak et al., 2016) while witnessing their family member's quality of life decline (Miller-Ott, 2018) and their relationship with this person drastically change (Ablitt et al., 2009). Due to the increasing dependency of one family member on another, this form of caretaking has been equated to an individual being exposed to chronic stress (Butcher et al., 2001), with the act of care shifting from a typical exchange of assistance between close relations to an inequitable burden for caregivers (Pearlin et al., 1990). Caregiving burden in this context can negatively affect family caregivers’ health (Abdollahpour et al., 2014). Moreover, while perceived social support can mitigate the negative effects of dementia care-related stress (Xu et al., 2021), these family caregivers often report having inadequate support and experiencing loneliness and isolation from friends and relatives (Kovaleva et al., 2021; Zwaanswijk et al., 2013). Deficits in support indicate a need to better understand aspects contributing to not only positive but also negative social network support experiences for these family members.
The communication tactics family caregivers use to convey their dementia caregiving support needs to members of their social network may influence the quality of responses they receive. Specifically, caregivers who directly express a need for support may provide potential helpers with greater opportunity to offer constructive assistance, leading to more positive support outcomes (Barbee & Cunningham, 1995; Derlega et al., 2003). Alternatively, caregivers’ use of indirect support seeking, which comprises ambiguous messages and behaviors, may lead others to experience uncertainty or discomfort and, in turn, provide less effective or even dismissive responses (Barbee et al., 1996; Collins & Feeney, 2000). To examine this notion, this study draws from sensitive interaction systems theory (SIST) (Barbee & Cunningham, 1995) to consider the extent to which direct versus indirect support seeking by family caregivers of people with dementia predicts the quality of support responses they receive from a person in their social network. In line with research linking social support to reduced caregiving burden (e.g., Clyburn et al., 2000; Shiba et al., 2016), this research also explores how supportive and unsupportive network responses mediate associations between family caregivers’ support elicitation strategies and their appraisals of dementia caregiving burden.
Support Seeking to Cope With Caregiving Stress
Support seeking can function as either a problem- (e.g., seeking advice) or emotion-focused (e.g., seeking comfort or distraction) coping response to stress (Carver et al., 1989). While problem-focused support seeking has been recognized as a generally adaptive reaction to stressful events (Heerde & Hemphill, 2018), eliciting emotional support can also benefit individuals when it helps them to minimize negative feelings associated with stress (Carver et al., 1989). Conversely, emotional support seeking used to vent negative feelings or pursue distraction can be a less advantageous coping strategy (Islam et al., 2022; Roth & Cohen, 1986). In the context of dementia-related family caregiving, research has been mixed regarding the effectiveness of using support seeking as a coping strategy. For instance, Cooper et al. (2008) reported that caregivers’ emotion-focused coping efforts, which included seeking emotional support, were associated with their lower anxiety, whereas their problem-focused coping strategies, including eliciting advice, predicted greater anxiety. Other research has suggested that social support seeking can contribute to reduced family caregiving burden (Chen et al., 2015) and, conversely, greater caregiver distress (Raggi et al., 2015). One implication from this research is that family caregivers’ communicative approaches used to obtain support may influence different outcomes of these efforts. To examine this idea, this study draws from SIST (Barbee & Cunningham, 1995), which offers a framework for conceptualizing social support as occurring through a process of interpersonal exchanges.
Sensitive Interaction Systems Theory
Recognizing that supportive messages develop as part of intricate social episodes (Burleson et al., 1994), SIST explains how direct and indirect support-seeking behaviors enacted by one person relate to different forms of support provision from another and ultimately lead to varying support outcomes (Barbee & Cunningham, 1995). According to the theory, support exchanges begin with one's awareness of a problem and conveyance to others that assistance is needed. This action by a support seeker, originally referred to as “support activation,” as it can occur through explicit or implicit means, is argued to set the stage for how the remaining interaction will play out (Feng & Burleson, 2006).
SIST further posits that direct support seeking, such as overtly asking for advice, resources, or reassurance, provides potential helpers greater ability to offer effective aid by clarifying an individual's particular support needs (Barbee & Cunningham, 1995). Conversely, people's attempts to indirectly elicit support, for instance, by complaining about an issue without asking for help or minimizing the seriousness of a problem, fail to provide sufficient information about a person's need while also conveying ambiguity regarding their desire for aid. Indirectly eliciting support can lead individuals, such as family or friends, to experience uncertainty or discomfort over how to help or perceive a support seeker's needs as trivial and, subsequently, offer responses that are critical or dismissive in intent (Barbee & Cunningham, 1995; Rains et al., 2020). In contexts outside of dementia family caregiving, research has substantiated associations between people's use of direct support seeking and their receiving positive responses from others (e.g., expressions of understanding and affection) as well as between indirect support seeking and negative reactions (e.g., blaming or seeming insensitive to a support seeker's needs) (Collins & Feeney, 2000; Derlega et al., 2003; Don et al., 2013; Rains et al., 2020; Williams & Mickelson, 2008).
People caring for a family member with dementia can have varying reasons to use either direct or indirect means to garner network support for issues they face with caregiving. These family caregivers may seek network support directly when they encounter greater levels of caregiving need (Dam et al., 2018) or lack knowledge about the trajectory of dementia (Laditka et al., 2013). Conversely, caregivers who anticipate greater social costs to support seeking, such as inconveniencing family or friends or experiencing a loss of their own autonomy, may be inclined to seek help more indirectly (Au et al., 2013; Dam et al., 2018). Understanding relationships between family caregivers’ support seeking and network responses is useful in demonstrating social support as a discursive process playing out between recipients and providers and resulting in more or less helpful outcomes (Burleson & MacGeorge, 2002; Feeney & Collins, 2015). Thus, this study tests the following predictions:
Support Responses and Caregiving Burden
Responses to a person's support-seeking attempts can result in positive outcomes when these actions offer beneficial problem-solving assistance or confirmation of another's feelings (Priem & Solomon, 2015; Rains et al., 2020). Alternatively, unsupportive responses can increase the likelihood of a support seeker experiencing adverse outcomes, including poor health (Derlega et al., 2003; Lee & Szinovacz, 2016). For family members providing care for a relative with dementia, perceived network support can attenuate negative impacts of caregiving stress, including reducing burden (e.g., Shiba et al., 2016; Zhang et al., 2014). This study extends this research to consider relationships between the perceived quality of network responses and caregivers’ appraisals of caregiving burden. Specifically, it is predicted that:
In testing these hypotheses, we took into account that support exchanges between individuals are shaped, in part, by interlocuters’ relationship characteristics (Barbee & Cunningham, 1995). Therefore, we considered, as potential control variables, family caregivers’ relationship satisfaction with a network member whom they sought support from about a caregiving problem as well as the extent to which that person provided caregiving assistance. We also examined care recipients’ dementia-related behavioral symptoms and caregivers’ demographic characteristics as potential control variables, in that both constructs can affect caregiving burden (Cheng, 2017; Hilgeman et al., 2009; Kahn et al., 2016) and peoples’ approaches to support-seeking and provision (Buehler et al., 2018; Wendt & Shafer, 2016).
Methods
Participants
Eligible participants were adult live-in caregivers providing care for a relative diagnosed with dementia. Family caregivers were recruited from Prolific (
Family Caregiver Demographics.
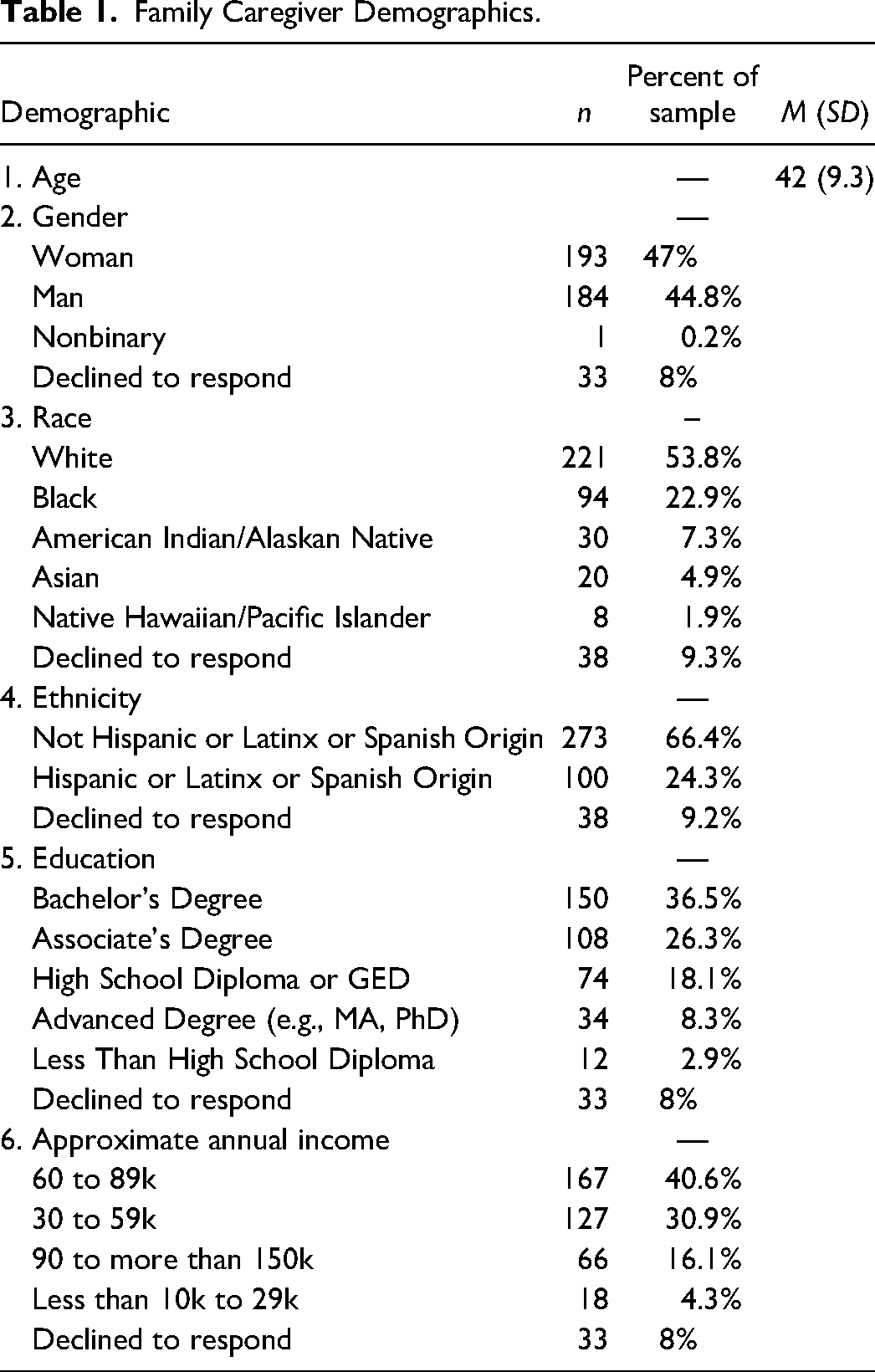
Procedure
The study survey first asked respondents to reflect on their experience as a caregiver and on someone from their social network with whom they had interacted about their caregiving struggles, regardless of whether this person had provided them helpful support. Respondents were instructed that the network member they interacted with should not be someone they knew from a formal support group or the relative they cared for. Participants were asked to indicate their relationship type with the person they interacted with and to keep this individual in mind when responding to upcoming questions. Participants reported talking about caregiving issues with the following individuals: parent (
Measures
Support Seeking
Respondents’ direct and indirect support-seeking behavior was assessed using two 5-point Likert-type scales (i.e., 1 =
Network Support Responses
To assess family caregivers’ perceptions of supportive or unsupportive responses from a social network member, we adapted items from previous research (Derlega et al., 2003; Don et al., 2013; Williams & Mickelson, 2008). Specifically, nine items were used to assess supportive responses (Cronbach’s α = 0.76,
Caregiving Burden
The Zarit Burden Interview Short Form (ZBI-SF; Bedard et al., 2001) was used to assess caregiving burden. This scale assesses caregivers’ perceptions of stress and negative experiences related to caregiving using a 5-point Likert-type scale (i.e., 1 =
Relationship Satisfaction
An adapted version of the Marital Opinion Questionnaire (Huston et al., 1986) was used to assess participants’ relationship satisfaction with the network member they had interacted with about their caregiving problems. To capture this measure as a control variable, participants responded to eight 7-point semantic differential scales providing bipolar adjectives to describe their relationship with the network member over the past 2 months (e.g., “rewarding-disappointing”, “full-empty”). These scales were averaged (Cronbach’s α = 0.82,
Help With Care
The degree to which participants received help with dementia-related care by the network member was also considered as a control variable and assessed using a single-item measure: “To what extent is the person you noted earlier in the study as having interacted with about your caregiving struggles also involved in helping with care for your relative with dementia?” Participants responded to this question using a 7-point Likert-type scale (i.e., 1 =
Care Recipient Dementia-Related Behavioral Symptoms
Participants assessed the frequency of their care recipients’ behavioral symptoms by responding to measurement items from the Revised Memory and Behavior Problems Checklist (Teri et al., 1992). This measure has been used to evaluate dementia caregiving models (Bekhet, 2023) and intervention research (Hepburn et al., 2022). For this study, participants indicated how often over the past week their care recipient demonstrated behaviors like waking family members at night, behaving aggressively, and practicing self-harm. For this control variable measure, respondents answered eight items (α = 0.78;
Demographics
Respondents answered demographic questions about their age, race, ethnicity, gender, education status, and household income.
Statistical Analysis
Correlations among all variables included in the model are presented in Table 2. The associations of interest were examined with path analyses in AMOS using a mean imputed version of the data. All exogenous variables were set to covary. Model fit was evaluated based on the model χ2 statistic, the normed χ2 value (the ratio of χ2/df), with a value < 3.0 indicating an adequate fit (Bollen, 1989; also see Crockett, 2012); Hu and Bentler (1999) have also suggested cutoff values for the comparative fit index (CFI ≥ 0.95) and the root mean-square error of approximation (RMSEA ≤ 0.08). Following Preacher and Hayes (2008), indirect associations were explored using bootstrapping, in which resampling (
Correlations Among Main Study Variables (
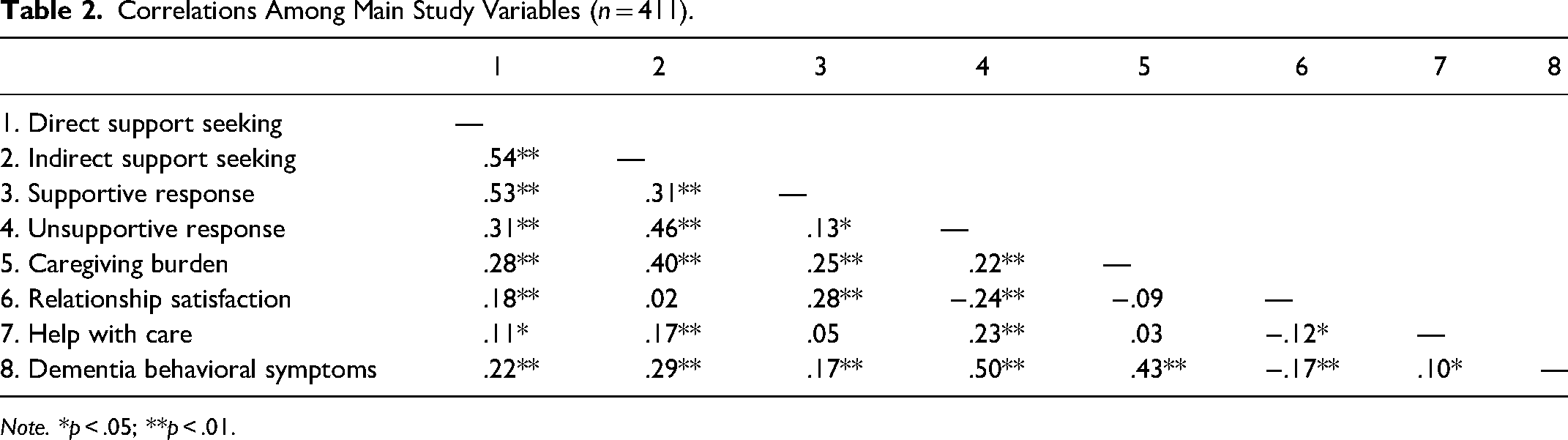
Pearson correlations, one-way analysis of variance tests, and T-tests were used to examine the extent to which the proposed control variables related to this study's dependent variables. This preliminary analysis indicated that caregivers’ relationship satisfaction with a network member, the amount of dementia care assistance this person provided to caregivers, and a care recipients’ dementia-related behavioral symptoms showed consistent main effects on the dependent variables. Consequently, these variables were included in the model as controls, while caregiver demographic characteristics were not.
Results
Results suggested an excellent model fit with χ2(1) = 0.56,
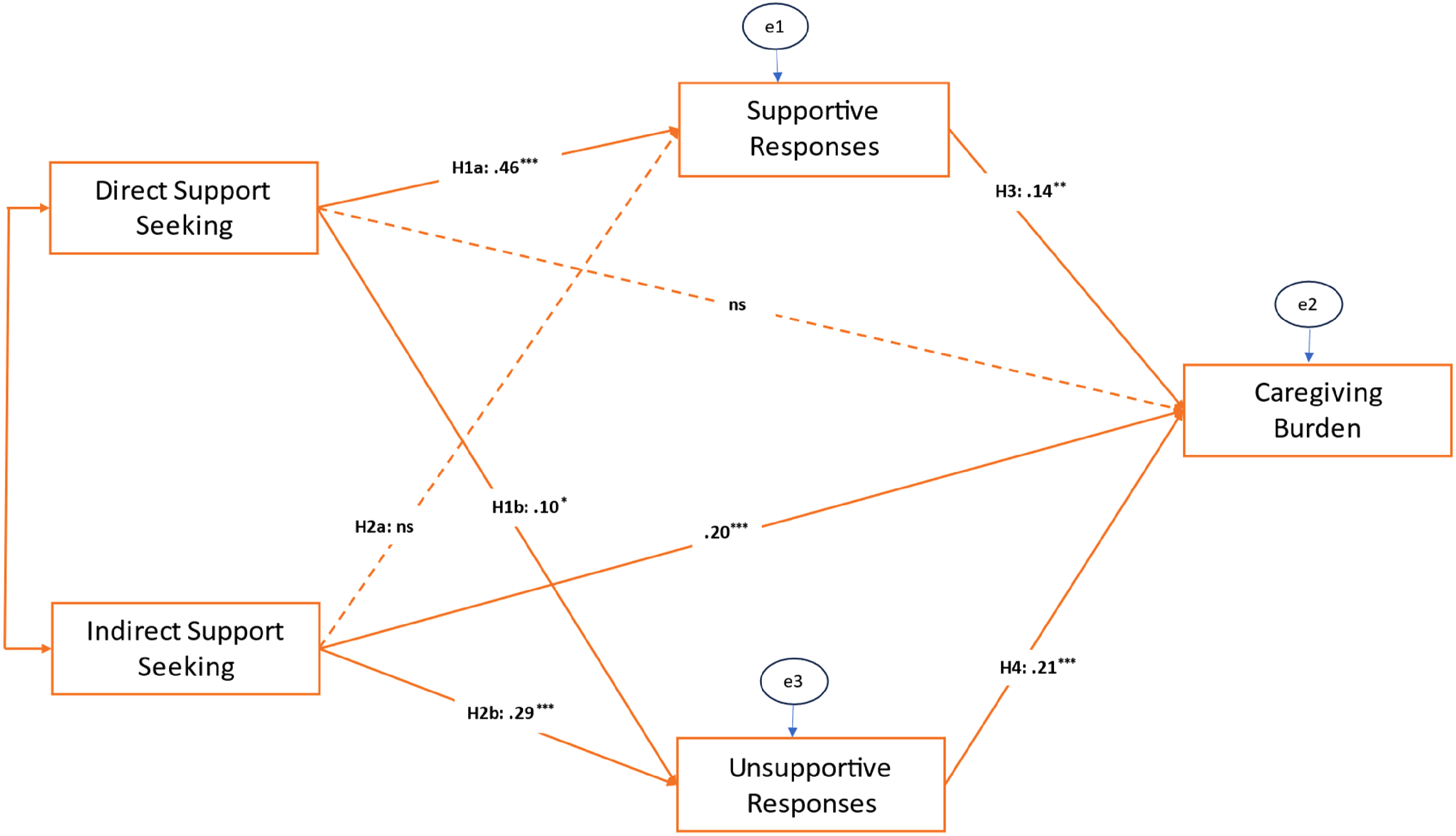
Tested model with standardized regression weights.
H2 proposed that indirect support seeking by family caregivers would predict fewer supportive responses from a network member (H2a) and greater unsupportive responses (H2b). The results revealed that while family caregivers’ indirect support seeking was unrelated to perceived supportive responses from a network member (
H3 predicted that supportive responses from a network member would be related to less caregiving burden for a family member providing dementia-related caregiving. Against expectations, results showed that supportive responses were positively related to family caregiving burden (
Indirect Effects
H5 and H6 aimed to assess whether supportive/unsupportive responses from a network member mediated the associations between direct/indirect support seeking by family caregivers and their dementia-related caregiving burden. For H5, analysis revealed that caregivers’ direct support seeking was indirectly and positively associated with the caregiving burden (
While not included as part of our main hypotheses, investigation of relationships between control variables and key study variables indicated relevant associations that we report here. First, family caregivers’ relationship satisfaction with the network member they interacted with about a caregiving problem was positively related to supportive network responses from that person (
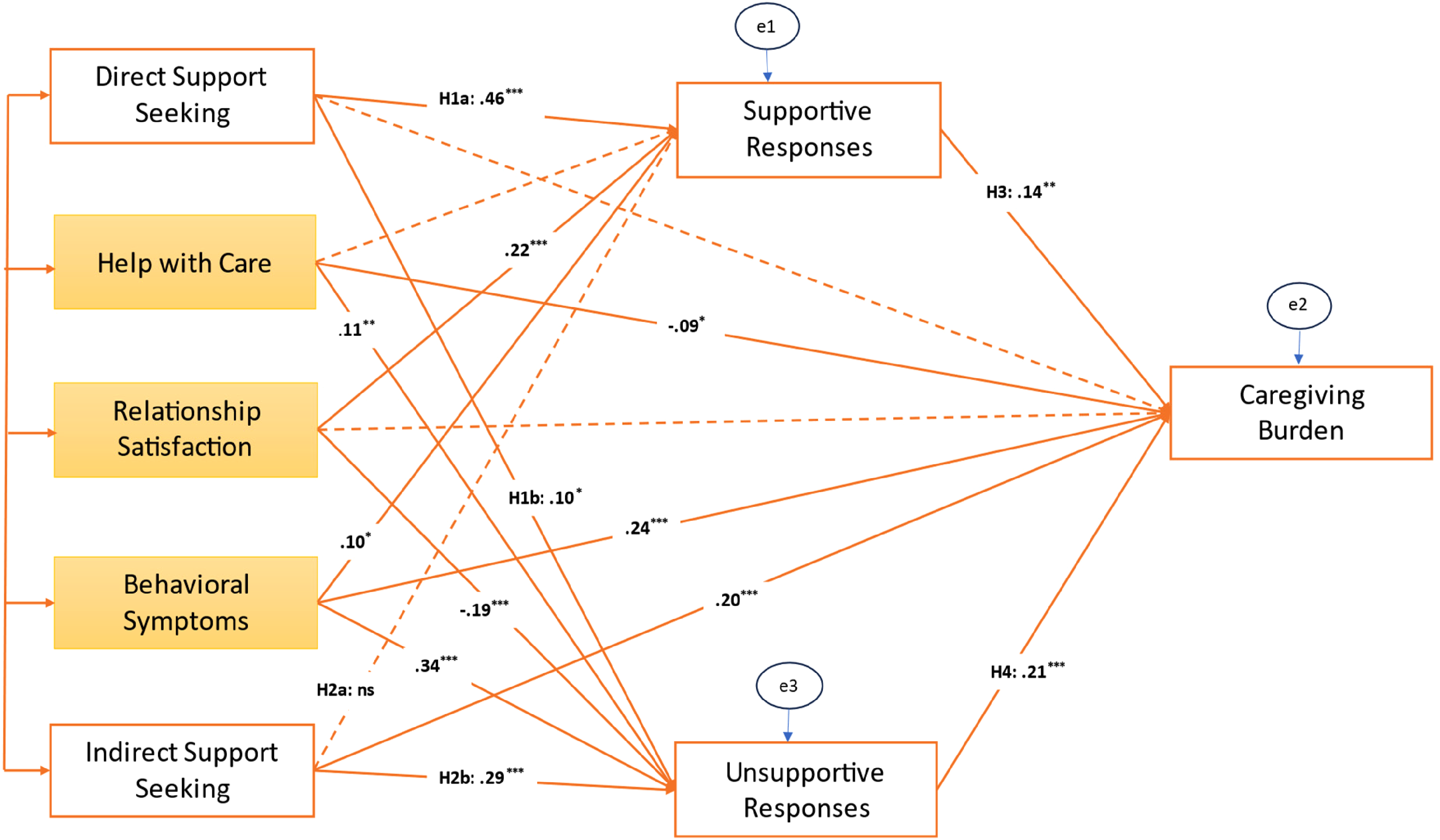
Tested model with control variables and standardized regression weights.
Discussion and Implications
Study findings reflect a key SIST principle by demonstrating ways in which dementia family caregivers actively contribute to support exchanges occurring between themselves and others in their interpersonal network. Namely, this study showed caregivers’ direct support seeking to be related to their perceptions of receiving supportive responses from a network member. Conversely, caregivers’ indirect efforts to garner aid predicted their views of receiving unsupportive network member responses. Indirect support seeking by caregivers was also associated with their experiencing greater caregiver burden as was their perceptions of receiving either supportive or unsupportive network member responses. These findings underscore the utility of helping caregivers to identify and implement strategies for effectively expressing their diverse support needs to members of their social network while also using concurrent coping strategies to manage caregiving burden.
Findings from our study align with extant research showing that practices of direct support seeking can result in more supportive reactions from others, such as expressions of understanding or affection (Derlega et al., 2003; Rains et al., 2020). Direct support seeking in the current study also predicted caregivers’ perceiving unsupportive responses from a network member, albeit to a lesser extent. Considering most caregivers in our study reflected on their support-seeking experiences from a parent or spouse (who was not the care recipient), this finding could be reflective of people in longstanding relationships reacting to direct requests for help by offering multiple and varied responses (Barbee & Cunningham, 1995; Rossetto, 2015). Moreover, family caregivers using direct support seeking and receiving beneficial help may still recall potent, negative support responses over more positively intended ones (Baumeister et al., 2001; Don et al., 2013). Finally, in addition to direct support seeking, caregivers’ relationship satisfaction with a network member predicted greater supportive and fewer unsupportive reactions from that person, which reflects the influence of relational characteristics on caregivers’ appraisals of support. Future research can benefit from investigating the influence of other relationship variables, such as partner closeness (Williams & Mickelson, 2008), on family caregivers’ perceived support quality.
Study results also mirror extant research that has demonstrated indirect support seeking, wherein people convey ambivalence over receiving support, to predict reactions like blame, criticism, or insensitivity from family or friends (Collins & Feeney, 2000; Don et al., 2013; Williams & Mickelson, 2008). While we also expected that family caregivers’ indirect tactics for eliciting dementia caregiving support would be related to their receiving fewer positive responses from others, findings indicated an insignificant relationship between these variables. As suggested earlier, participants were more likely to report supportive responses from a network member when they also experienced higher relationship satisfaction with that person, suggesting the influence of relational aspects on caregivers’ perceived support. Furthermore, it is of note that the more family caregivers received dementia caregiving assistance from a network member, the more they viewed this person's responses to their attempts to elicit aid as unsupportive. Future research can benefit from considering how caregivers’ beliefs about their dementia caregiving role as well as interpersonal variables, such as family conflict (Rote et al., 2019), shape support exchanges between primary caregivers and other network members.
Results from this study also indicated that both supportive and unsupportive network member responses to a caregiver's support-seeking efforts predicted greater caregiving burden. The association between unsupportive network reactions and burden extends research finding family caregivers to experience greater burden and lowered well-being when also receiving criticism about their caregiving (Rurka et al., 2021; Xian & Xu, 2020). The fact that supportive responses from a network member also predicted caregiving burden, as well as mediated an association between direct support seeking and burden, could be indicative of the conceptual complexity in characterizing network support. That is, some caregivers may perceive offered support from others as well-intended while still viewing it as insufficient in reducing stress. Research has shown that support, regardless of perceived intent, can be seen as less effective and even burdensome when given at inappropriate times or in an unsuitable manner (Gleason & Iida, 2015), or when it fails to meet a recipient's needs or desired level of support (McLaren & High, 2019). Future research should consider the extent to which assistance offered to family caregivers aligns with their dementia care needs and desired amount of aid (High & Crowley, 2018).
Family caregivers also reported greater burden when using indirect support seeking, with unsupportive responses from a network member partially mediating this relationship. While caregivers may rely on indirect means to gain support when they lack communication skills to effectively solicit aid (High & Scharp, 2015) or fear rejection from others (Williams & Mickelson, 2008), this approach may also lead them to experience a lowered sense of control or uncertainty (Freire et al., 2016; Kuang & Wang, 2022) over caregiving outcomes, which could contribute to higher caregiving burden. Care recipients' dementia-related behavioral symptoms, such as showing increased agitation, also predicted family caregiving burden, which aligns closely with extant research (e.g., Cheng, 2017; Raggi et al., 2015). In addition to caregiving burden, care recipients' behavioral symptoms were also related to caregivers’ perceiving more supportive and unsupportive responses from a network member. The severity of caretaking challenges faced by caregivers may lead these family members to spend more time engaging in positive as well as negative support exchanges with members of their social network (Buehler et al., 2018; Werner et al., 2014). Future research could benefit from exploring how a care recipient's dementia progression shapes ongoing shifts in caregivers’ support needs and resulting network interactions. Caregivers may also apply additional coping strategies beyond practices of support seeking to reduce burden more effectively.
Implications for Marriage and Family Counselors
This study emphasizes the role of communication in affecting family caregiver support outcomes in the context of dementia caregiving. Specifically, results from this study demonstrate how family members’ indirect support-seeking behaviors and negative support exchanges with a social network member can have an adverse effect on their dementia caregiving experiences, including contributing to greater burden. Furthermore, negative support interactions between caregivers and other family members or friends may have a greater influence on caregiving stress and burden than positive support exchanges. These results highlight the benefit of counseling efforts aimed at helping family caregivers develop effective strategies for identifying and expressing their unique and changing dementia-caregiving support needs to members in their social network. Additionally, counselors can provide impactful assistance to caregivers through education and guidance on techniques for managing ineffectual support responses from others and recognizing aspects contributing to family tension around caregiving. Finally, counseling guidance that focuses on support-seeking strategies along with a variety of additional coping strategies can be instrumental for addressing family members’ dementia-related caregiving burden.
Limitations
This research is not without limitations. First, the present study did not examine support exchanged between family caregivers and individuals from their social network as happening dyadically over time. In collecting cross-sectional data, this study was unable to indicate causal relationships between proposed variables or examine ways in which support interactions can be self-correcting when initial support activation or responses are ineffective (Barbee & Cunningham, 1995). Also, caregivers who completed this study, though having access to an online survey, may not have fully represented the family caregiver population within a dementia care context. Finally, while this study was modeled after extant research (e.g., Collins & Feeney, 2000; Don et al., 2013) in focusing on support exchanges between participants and an individual from their interpersonal network, examination of caregivers’ support seeking across multiple network members may have provided further insight into the relationships between study variables. Nonetheless, this study demonstrated social support for family members providing dementia-related care to their relatives as a rich communicative process resulting in varying caregiver outcomes.
Footnotes
Acknowledgment
The authors would like to acknowledge Amber McIlwain for editing and formatting the manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
This study (#0000243) was approved by The University of Texas at Austin Institutional Review Board, representing the first author's affiliation at the time of data collection.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
