Abstract
Cognitive behavioral therapy (CBT) is an effective treatment for child anxiety disorders. Low-intensity forms of CBT, such as guided parent-delivered CBT (GPD-CBT), have been developed to increase access; however, it is unclear why some children benefit from this treatment and others do not. This qualitative study aimed to increase understanding of parents’ experiences of GPD-CBT and what facilitates and creates barriers to good outcomes. The sample was derived from a sample of families who took part in long-term follow-up assessments (reported in). Data were analyzed using thematic analysis. Two themes containing five subthemes were developed from the data. Theme 1 described factors influencing the experience of GPD-CBT. Theme 2 described perceived outcomes in the child and wider changes within the family. The identification of facilitators and barriers to the success of GPD-CBT could inform and improve future treatment delivery.
Childhood anxiety disorders affect 6.5% of children worldwide (Polanczyk et al., 2015) and have a significant impact on children’s education, physical health, and social and family life (Essau et al., 2000; Ezpeleta et al., 2001). They also pose a risk for long-term difficulties in adulthood (Woodward & Fergusson, 2001).
Effective evidence-based treatments for childhood anxiety disorders have been developed, specifically, cognitive behavioral therapy (CBT). There is vast support for the use of CBT in treating anxiety disorders in children (James et al., 2015; Reynolds et al., 2012). Delivery of traditional CBT treatments is resource intensive and requires a lot of therapist input (Walkup et al., 2008). With the high prevalence of childhood anxiety disorders, few children affected have access to effective treatment such as CBT (Chavira et al., 2004; Essau, 2005; Merikangas et al., 2011). This means that many children who may benefit from CBT treatment are left untreated (Stallard et al., 2007).
An established way to increase access to psychological therapies is through the provision of effective low-intensity treatments (Clark et al., 2009). One brief low-intensity form of CBT is guided parent-delivered CBT (GPD-CBT) in which a therapist guides the parent to apply CBT principles in their child’s day-to-day life. This approach has been found to be similarly effective to traditional CBT treatments at treating childhood anxiety disorders (Chavira et al., 2014; Cobham, 2012; Leong et al., 2009; Lyneham & Rapee, 2006) but can be delivered with markedly reduced therapist input and fewer resources (Rapee et al., 2006; Smith et al., 2014; Thirlwall et al., 2013). The approach has also been found to be cost-effective compared to an alternative brief psychological therapy for child anxiety disorders (Creswell et al., 2017). Furthermore, long-term follow-up studies have shown that few children who recover following GPD-CBT with relapse in subsequent years (Brown et al., 2017). Thus, GPD-CBT could fit within a stepped care model where low-intensity treatments are routinely offered for mild–moderate presentations while more intensive treatments are reserved for those presenting with severe anxiety disorders and those who do not respond to low-intensity interventions (Bower & Gilbody, 2005).
Despite these promising findings, not all children benefit from a GPD-CBT approach, and predictors of child outcomes have not yet been established (Thirlwall et al., 2017). As such, it remains unclear why this treatment approach works well for some children and less so for others. This study set out to address this issue by applying qualitative methods to gain a better understanding experiences of parents who participate in GPD-CBT; in particular, to gain insights into what facilitates or creates barriers to good child outcomes from GPD-CBT in the short and longer terms. Understanding the treatment experience can help to identify predictors that enhance treatment to improve outcomes. A qualitative approach has been taken to gain an understanding of the experience of GPD-CBT for which outcome measures alone do not give insight. The findings from this study will directly influence future GPD-CBT protocols and how this is implemented in practice so that it can be used as an effective first-line treatment intervention for anxiety disorders in children.
The aim of this study was to explore the following questions:
What are the parents’ experiences of the GPD-CBT treatment intervention?
What, according to parents, facilitates the treatment?
What, from a parent’s point of view, was the outcome of the treatment and were any positive outcomes sustained?
Do parents perceive any barriers to engaging with the treatment, and, if so, how can these be minimized?
Method
Target Intervention
GPD-CBT is a brief low-intensity form of CBT. Parents are given a self-help book (Creswell & Willetts, 2012) and guided by a therapist to apply CBT principles in day-to-day life to target the child’s anxiety. The role of the therapist is to support and encourage parents to progress through the self-help book and practice the skills with their child. The therapist also supports the parents to problem solve any difficulties or barriers that may arise. The role of the parent is to work through the self-help book and implement the skills into their child’s life to support them and help them to overcome their anxiety disorder.
Procedure
One-to-one semistructured interviews were conducted with parents who had participated in GPD-CBT 39 to 61 months earlier. The interviews covered how the parents found the delivery of the CBT and what outcomes were associated with it (for the child and the wider family), what they found helpful, and any difficulties they faced. Interviews ranged from 9 to 28 minutes.
Sample
Participants were recruited from Thirlwall et al. (2013) randomized control trial. They were deemed eligible for this study if they had completed at least half of the GPD-CBT treatment sessions offered and if they had not received further treatment for any mental health condition. This allowed a focus on experiences and outcomes associated with GPD-CBT specifically. Of the 65 families that took part in follow-up assessments (see Brown et al., 2017), 39 parents consented to participate, all of whom participated in in-depth interviews.
The final sample size of 15 was determined by theoretical saturation, the point at which no new themes emerged from the data (Braun & Clarke, 2006). To ensure the detailed analysis of the full data set was feasible, no further interviews were analyzed. Formerly, it has been recommended that qualitative studies require a minimum sample size of at least 12 participants to reach data saturation (Fugard & Potts, 2015; Guest et al., 2006). Thus, a sample of 15 was deemed sufficient for the qualitative analysis of this study.
Purposive sampling was used to select the sample of 15 participants. Participant details are provided in Table 1. Purposive sampling is a nonprobability sampling method (Bryman, 2012; Robinson, 2014) in which participants are recruited based on specific characteristics, designed to provide a valid and diverse understanding of selected individuals’ experiences (Devers & Frankel, 2000). Diversity was sought first through ethnicity as this characteristic was the least diverse among the sample. The sample was then selected based on socio-economic status (11 categorized as higher/professional), marital status, educational backgrounds, and employment status of the mother and father/partner, to establish diversity among the sample. Other factors that were considered were child primary diagnosis, comorbid disorders, long-term child outcome (presence/absence of an anxiety disorder diagnosis), and the number of sessions attended, as well as child age and gender. The majority of the sample were White British (n = 13), eight males and seven females with a median age of 9 years. Anxiety disorders varied, including separation anxiety, generalized anxiety disorder (GAD), panic disorder, specific phobia, and social phobia.
Participant Characteristics.
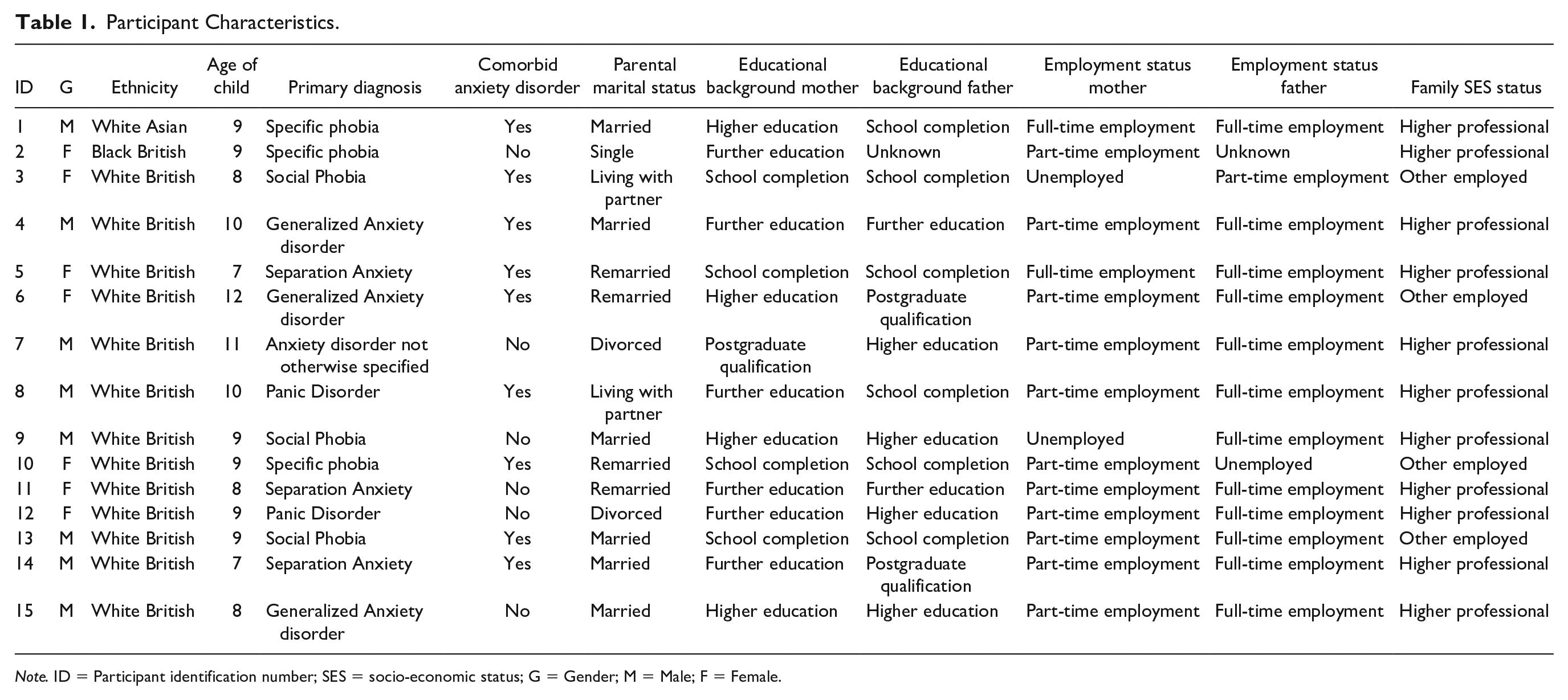
Note. ID = Participant identification number; SES = socio-economic status; G = Gender; M = Male; F = Female.
Data Analysis
The audio-recordings of the interviews were listened to several times and then transcribed verbatim and anonymised. Thematic analysis methodology was used to examine the data following Braun and Clarke (2006). This included line-by-line coding of each interview, taking an inductive approach, using NVivo software package (Version 11, Qualitative Data Analysis Software, 2015) to organize the data efficiently (Welsh, 2002). Between and within transcripts coding was used, and coding was stopped after 15 interviews, when the researcher and supervisory team were confident that theoretical saturation had been met. Codes were merged into meaningful groups (Tuckett, 2005) based on wider discussion with the research team. This was an iterative process that involved reviewing the data several times until each theme could clearly be defined to create the final two themes and five subthemes.
Patton’s (2002) criteria for defining categories was used at this stage, taking a two-level approach. First, there was consideration of whether all themes formed a clear pattern. Second, there was consideration of the validity of each of the themes to ensure that they were relevant to the transcription and reflected the interviews accurately. To do this, each subtheme was evidenced with a direct quote from the transcripts. These were discussed with the research team to ensure that each theme was clear and concise.
The verbatim transcripts were then re-read to ensure that the themes reflected the data accurately, capturing the true meaning of what was said by the participants.
Results
Two themes, collectively containing five subthemes, were developed from the data encompassing parents’ experiences of the GPD-CBT treatment intervention, as well as their perceived facilitators and barriers to the treatment, as shown in Tables 2 and 3.
Theme 1: Factors Influencing Experience of GPD-CBT.
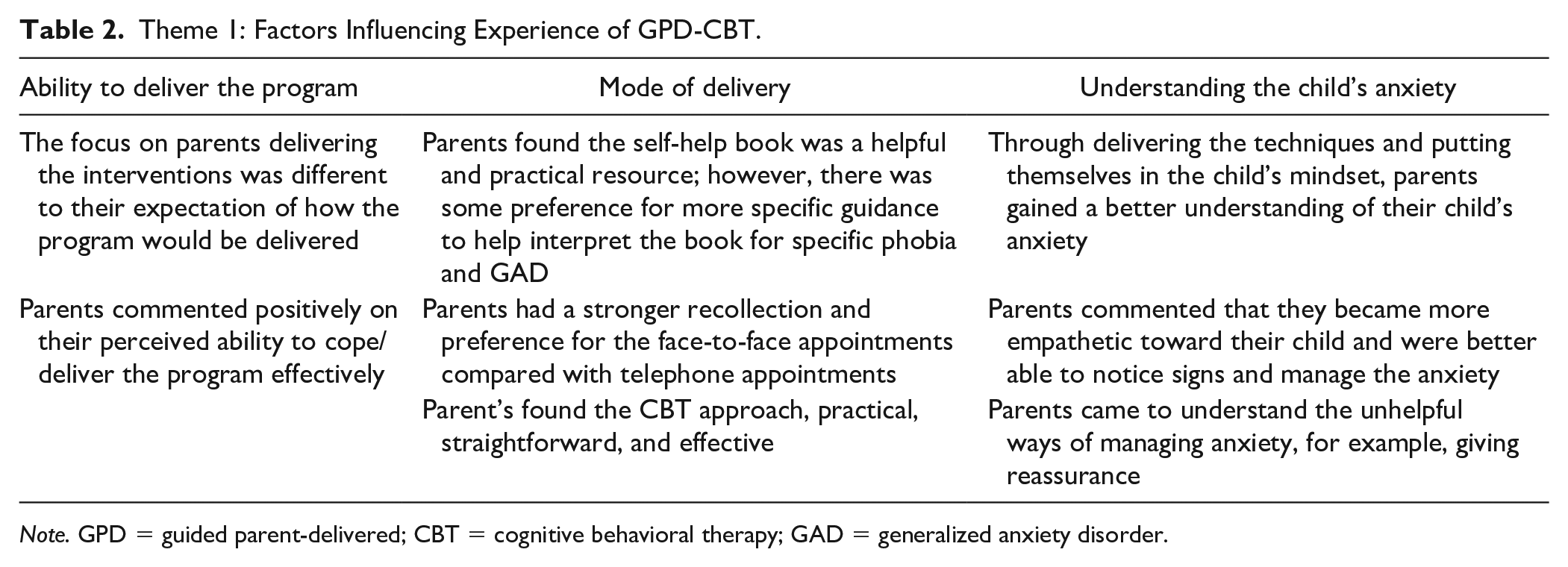
Note. GPD = guided parent-delivered; CBT = cognitive behavioral therapy; GAD = generalized anxiety disorder.
Theme 2: Perceived Outcomes.
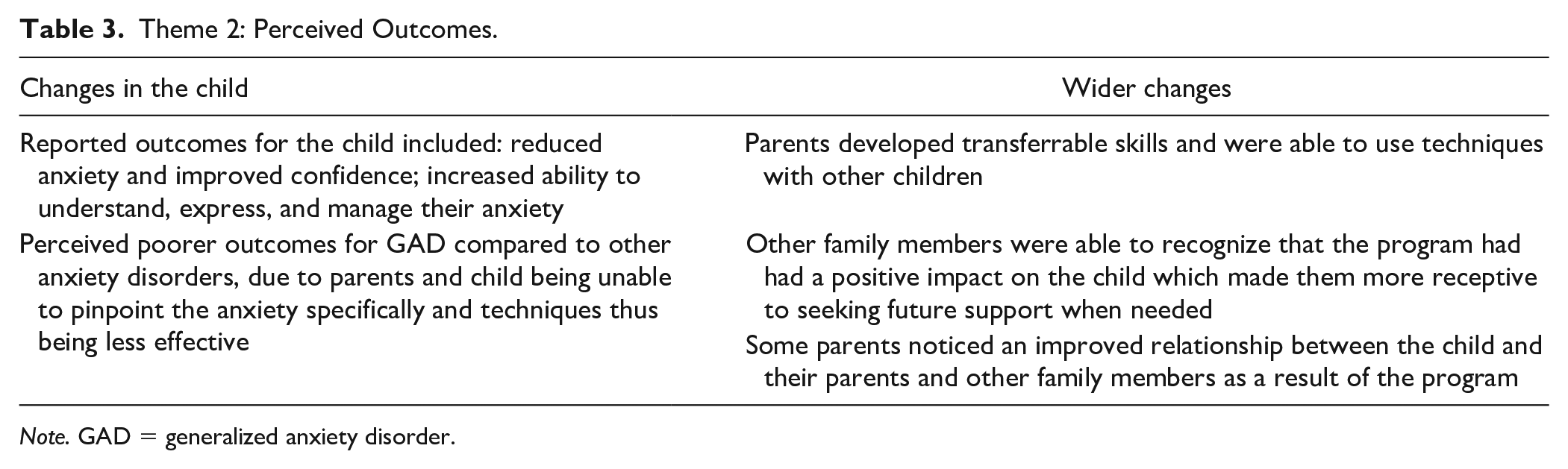
Note. GAD = generalized anxiety disorder.
Factors Influencing the Experience of GPD-CBT
Ability to deliver the program
The GPD-CBT program uses a parent-delivered approach, which several parents perceived as “incredibly important because you are the person who has got to live and to manage the situation” (Participant 13). Therefore, by taking on the role of delivering interventions, parents were educated about CBT techniques, allowing them to develop skills to manage their child’s anxiety. Parents believed this to be an important aspect, expressing that “knowledge is an important thing . . . the more you have, the more helpful you can be” (Participant 15). Furthermore, several parents found it “empowering for parents to be given the tools to come up with a solution for their children” (Participant 2). This was encouraging for parents and enabled them to develop confidence in dealing with their child’s anxiety.
However, some parents doubted their abilities to deliver the program effectively, “I did wonder sometimes whether the fact that I was doing it, did that mean that I wasn’t doing it quite right?” (Participant 8). Some parents believed they lacked the “psychological knowledge” (Participant 8) of a trained therapist. Therefore, they reported that they would have felt greater confidence if a qualified therapist was delivering the intervention: “If a therapist was doing it, you’d feel confident that they are the professional, they know exactly what they are doing” (Participant 15).
One parent felt the role of a mother and the role of a therapist should be separate because a therapist would have a greater perceived authority in delivering the treatment. She stated, “I am the mum and some of it’s not really getting in because it’s just ‘Oh mum just wants me to do this . . .’, but I think if you’ve got a therapist saying it, they might take it a bit more seriously.” (Participant 12).
A few parents expected their child’s anxiety to be treated much like a physical health problem with the assumption that “somebody should be able to sort this out . . . like you go to the doctors you’ve got a problem and someone else sorts it out” (Participant 14), and that a therapist as a professional would be able to “cure” (Participant 12) their child. Several parents expressed “being a bit surprised” (Participant 2) that they would be delivering the program and “surprised I was going to be the one that helped her through it.” (Participant 14). This led to initial hesitation and served as a barrier to their initial engagement in the program. For a few parents, this hesitation “continued for a while” (Participant 14) throughout treatment. However, in hindsight, many parents described a preference for the parent-delivered approach over a child-focused approach because it meant their child did not “become too dependent on a therapist” (Participant 11). Parents also considered the approach to be “less daunting” (Participant 14) for their child, as it did not require the child having to “learn to trust that therapist first” (Participant 1).
Practical considerations that had an impact on some parents’ abilities to deliver the program included time and the involvement of a second parent. Parents were required to attend the appointments with the therapist, read the self-help book, and translate the CBT interventions in the book to the home environment. Therefore, “finding specific time was a challenge” (Participant 4), and fitting the program around work commitments and family life was “tricky” (Participant 4) for some parents. As well as finding time to fit the program around day-to-day life, parents found it took time to get used to using the techniques because “it wasn’t what, naturally you wanted to do . . . you had to stop and think ‘No don’t say that” (Participant 14). Both the parent and child were “not used to thinking” (Participant 3) about the anxiety in the way the program encouraged, so it took some time to understand the techniques. This was initially a barrier but became less of an issue as parents began to understand the techniques and put them into “context and started thinking ‘This is how I’ve got to approach it,’ and then I was fine” (Participant 3). Some parents were concerned that if only one parent got involved in delivering the treatment this could hinder the effectiveness of treatment: the fact that [partner’s name] and I were doing it together was a really good thing. I think if you didn’t have the support of someone and you were not doing it together, I think that could be easily undermined. (Participant 2)
Mode of delivery
Parents received the self-help book along with support from a therapist through a combination of face-to-face and telephone appointments. The self-help book followed a CBT approach. According to several parents, the book was a useful and helpful resource. Parents commented that it was “very practical” (Participant 2) and “the book more than anything else” (Participant 5) was the most helpful aspect of the program. The book also included multiple techniques that were “quite specific [and] relevant to what we were going through, what [child’s name] was going through, so I found that quite helpful” (Participant 4). Parents found that they could apply the situations and techniques in the book to their own circumstances to manage their child’s difficulties with anxiety.
Parent’s commented on the techniques they learned and how they applied them to everyday life. For example, one parent said, “only a small technique but I think it was just so applicable to him [child] . . . was getting him to take responsibility for his own things” (Participant 13). Moreover, numerous parents found the techniques for testing thoughts very effective. Parents spoke of how they passed this technique to other parents who “tried it on their children and they said it’s amazing” (Participant 8).
On the contrary, a few parents found the techniques difficult to put into practice and apply to everyday life. This appeared to be particularly true for parents of children with GAD as, for example, they were unable to pinpoint particular anxious thoughts to address through the techniques. Another parent found the book focused on many different types of anxiety, whereas they wanted more explicit guidance on how to overcome a specific phobia. Therefore they “didn’t find the book helpful” (Participant 12) in supporting their child to overcome their anxiety disorder.
In terms of the level of support parents received from therapists alongside the book, parents reported that it matched their needs, describing it as, “excellent” (Participant 10), “bang on target” (Participant 3), and “just about right for us” (Participant 15). However, some parents acknowledged that “some families, depending on what they are going through, they might need more [support] or they might need less [support]” (Participant 3). This suggests that the level of support could be adapted to suit individual family needs where necessary.
Despite the passage of time, parents generally had a stronger recollection of the face-to-face support they received than the telephone support; indeed, some parents had limited or no recollection of the telephone appointments. Parents attributed this to the telephone appointments not being “specific enough” (Participant 4). However, opinions on the use of telephone appointments differed. Some parents who could recall the telephone appointments found that they “worked out really well” (Participant 6), parents could work them around a “very busy” (Participant 6) life, and they also provided “continuation without having the whole thing of going there [clinic]” (Participant 2). Subsequently, they could take the phone call while at home or work, enabling the approach to fit around family life. Others found that because the telephone appointments were brief, they only used them to ask “little questions” (Participant 3), finding more specific guidance and queries were “explained better” (Participant 3) in the face-to-face appointments. This seems to suggest that the use of face-to-face and telephone appointments should be tailored to the needs of the family.
Some parents were able to compare the CBT approach to other treatments their child had previously received, such as counseling. Parents believed the GPD-CBT provided a better outcome and was “one of the best pieces of assistance” (Participant 2) the family received. This was due to the CBT being practical, “straightforward” (Participant 13), and fitting well within the family environment. Parents found other treatments were not “as comprehensive” (Participant 15) or “just seemed to go round and round talking about stuff” (Participant 2).
Understanding the child’s anxiety
Parents found that taking on the therapist’s role was not limited to them learning techniques to support their child; it also allowed them to understand their child’s anxiety better. Parents learnt to put themselves in the child’s “mind-set and not think like an adult” (Participant 3), which gave them a better perspective of how to help their child. The understanding they developed made them more empathetic when managing their child’s anxiety. Instead of getting “really annoyed [and] shouting all the time” (Participant 12), parents were able to talk to their child to gain an understanding of the anxiety from their perspective. Furthermore, by undertaking the program parents learnt how to recognize the signs and triggers of their child’s anxiety: “Now you can kind of see it as some of the signs” (Participant 15). This skill enabled parents to recognize when their child was anxious and quickly to use effective techniques to address the anxiety before it escalated.
The majority of parents stated that the program had taught them that reassurance had a negative impact on their child’s anxiety. Before the program, parents “always thought of that [reassurance] as a good thing” (Participant 11) and would “reassure [child’s name] too much and say it’s going to be okay every time he had a problem” (Participant 6). Parents reflected “that part of the problem might have been my parenting method, in that I was always very reassuring” (Participant 11). Using different management techniques enabled parents to recognize how reassurance may have contributed to the maintenance of their child’s anxiety.
Perceived Outcomes
Changes in the child
When asked about the outcomes of the program some parents described a “big effect” (Participant 13) that led to the child being “completely different” (Participant 8) following treatment. For others positive outcomes reflected smaller or more subtle changes in the child’s symptoms. Most of the parents stated they were “extremely pleased with the outcome” (Participant 3) of the program and “without it, we wouldn’t be where we are now” (Participant 15).
Two parents did not experience positive outcomes following the program: “Unfortunately, we’re another five years down the line and it’s still a big problem” (Participant 9). Parents believed this was partly due to the particular type of anxiety their child experienced. For example, as noted above, if it was difficult for the parent and child with GAD to “pinpoint” (Participant 9) where to focus treatment.
Some parents commented on broader changes in their child following treatment; for example, enabling them to “take control and manage himself” (Participant 13). Another parent spoke of the change in how “open” (Participant 1) their child had become. This was a common theme among parents, as they believed the program “made her talk more and come out” (Participant 1), which developed the children’s abilities to express their anxieties clearly. In addition, parents noticed that the program improved their child’s confidence, which enabled them to participate in extra-curricular activities, attend social events, and stay away from home on school trips. One parent demonstrated this point when describing her daughter during the interview: She’s outgoing, she’s bubbly, she’s not shy. She is a completely different girl from what she was when she started this, to what she is now. She’s happy to go . . . for sleepovers . . . she’s just done a French trip. (Participant 3)
Other parents spoke similarly about the change in their child’s capabilities: “She started going to people’s parties and she went without me, it just completely changed” (Participant 8). Parents mentioned the change in their child’s confidence and the child’s ability to do more was a vast, positive, and unexpected outcome of the program.
Wider changes
Many parents commented that acquiring techniques to manage their child’s anxiety during the program enabled them to help their other children too: “If [sibling’s name] is anxious about something, I’ll try and get her to look at how she can look at it differently or solve the problem or think differently” (Participant 2). Parents also found that the GPD-CBT “gave us the ability to transfer the skills and use them in different situations” (Participant 2). This experience also encouraged family members to seek help for other family members when it was required: With [sibling’s name] having the same or similar anxiety problem, I don’t think he [child’s father] hesitated to get the same kind of help for her, whereas initially with [child’s name] he just thought it would go away and didn’t want help. (Participant 11)
Consequently, the program changed family members “viewpoint[s] as to how you should deal with” (Participant 11) anxiety disorders.
Some parents found that as their child’s anxiety reduced and their confidence increased, families were able to do more and go out together, thus building stronger relationships within the family. For example, before the program, one child “wouldn’t have done a lot of things because she [child] would have been feeling sick and wouldn’t want to go” (Participant 7). A few parents also noticed a positive impact on their relationship with their child, bringing them “closer together” (Participant 13) and making their relationship stronger. Parents felt that they were “certainly a bit closer than certainly we would have been” (Participant 11). Some parents attributed this to an improvement in the way they communicated with their child. For instance, one parent mentioned that now “I always make a point of asking her every day . . . about things . . . like making a point of making sure she knows that I am interested in what she says and I love her” (Participant 15).
Discussion
The themes that were developed through this qualitative study highlight parents’ broad experiences of GPD-CBT. Notably parents described being surprised at being so heavily involved in the treatment program, but often subsequently reflected on the empowerment and skills that they developed from this approach. Parents reported wide ranging benefits, both for the individual child and the wider family, in terms of symptoms and general functioning, but also family relationships. These findings add value to quantitative outcomes by highlighting the need for clinicians to be aware of the potential for initial reticence toward the treatment approach among parents, and the possible utility of normalizing this initial response for parents alongside highlighting the broader benefits of the treatment approach that parents have identified.
Where parents struggled with the approach this seemed to relate to difficulties individualizing the broad approach to their child’s particular anxiety problems. There have been few consistent predictors of treatment outcome for GPD-CBT; however, the findings add to recent reports that suggest that while children with GAD do not differ in their overall clinical outcomes from GPD-CBT compared to children with other anxiety disorders, if they have not recovered during the treatment phase they are less likely to recover in the subsequent 6 months than children with other anxiety disorders (Thirlwall et al., 2017). Together these sets of findings suggest that parents of children with GAD find it harder to apply the treatment approaches without the support of a therapist than parents of children with other forms of anxiety disorders. This may reflect it being less clear to parents how to apply an exposure-based treatment for GAD, where avoidance may be less apparent. Further development of this aspect of treatment is likely to be required. The current findings may also help explain recent reports that suggest that children with specific phobias may do less well from GPD-CBT than from more intensive face-to-face CBT, unlike children with other anxiety disorders (McKinnon et al., 2018). In this study, parents described difficulties applying the principles in the context of some specific phobias—again, perhaps, those where it may not be straightforward to develop exposure tasks (for example, vomit phobia, and injection phobias). Further development of these aspects of the treatment may be beneficial, which is in line with parents’ suggestions that the treatment might benefit from increased flexibility where more support is available for those who need it. Flexibility in how the treatment is delivered would also appear to be useful for parents who often have extremely busy lives. Views were mixed regarding the usefulness of telephone sessions, but these certainly seemed to have practical benefits for, for example, working parents. Supplementing these with online material that provides information and models treatment approaches may help parents to get the most from these remote contacts. Video-conferencing options might also be valuable to provide the depth of support that parents felt they received from face-to-face sessions, while maintaining the efficiency of the telephone sessions. Indeed, recent reports have suggested that this is a promising approach to treatment delivery (Backhaus et al., 2012). Video-conferencing might also help facilitate greater involvement of more than one parent, which parents in this study highlighted as beneficial as it can promote understanding and consistency in approach across the household.
This study ensured rigor and credibility in its reporting, first, by analyzing developing codes through “constant comparison” (Pope et al., 2000), in which developing codes were checked against previous codes, ensuring no direct overlap. As the analysis developed, earlier transcripts were re-read by the researcher to check for more subtle examples of codes during the latter stages of the coding process. Credibility was checked during the data analysis stage through extensive discussions with the supervisory team. Braun and Clarke’s (2006) guidelines for thematic analysis were closely followed throughout the data analysis process to ensure internal validity. In qualitative research, reflexivity is important, it is vital for the researcher to be conscious of how their expectations and experiences affect the research (Shaw, 2010). In this study, the analysis was led by a researcher who had not been involved in the initial treatment delivery and evaluation (Thirlwall et al., 2013) or the long-term interviews with families (Brown et al., 2017) and did not have any particular investment in the outcomes. However, it should be noted that the lead researcher did bring clinical experience in delivering guided self-help CBT interventions with adults with depression and anxiety disorders, and with that a general belief that guided CBT interventions can be successful in treating common mental health problems. Furthermore, the wider research team included others who have both developed (C.C.) and evaluated (C.C., K.T., A.B., and C.A.) the particular treatment program—and brought with them a belief in the potential value of the approach as well as a curiosity to know how to improve it further. These views were explicitly considered throughout the analysis of the parent interviews. Other methodological features that need to be considered include the sampling frame. While we sought diversity in participant characteristics and data saturation, the potential sample was limited to families who had not sought any further treatment for a mental health problem in the years that had followed GPD-CBT. As such, we were not able to examine views of those who accessed additional support, either for ongoing anxiety problems or other emerging difficulties. Furthermore, while the introduction of a new researcher to lead the qualitative analysis meant that analysis could be conducted by someone who was not directly invested in the treatment that was delivered, this brings disadvantages associated with interviews and analyses not being conducted by the same person, including less-extensive familiarity with the data and no scope to iteratively adapt interviews to specifically probe developing themes (e.g., Bryman, 2012).
The development of an in-depth understanding of parents’ perspectives provides clear implications for both how GPD-CBT is introduced to parents (e.g., recognizing potential initial reticence) and areas for improvement in treatment delivery (e.g., further developments regarding how to set up less clear-cut exposures and increased flexibility in delivery methods). Overall, the findings from this study suggest that parents experience brief parent-led CBT as an acceptable and effective treatment for childhood anxiety disorders, adding to research suggesting that it may be an appropriate first-line intervention for childhood anxiety disorders (e.g., Evans et al., 2019; Rapee et al., 2017).
Footnotes
Acknowledgements
The authors thank the participating families and the researchers and clinicians who supported the initial randomized controlled trial.
Declaration of Conflicting Interests
C.C. is the author of the book for parents that was provided to parents who received the treatment in this study, and P.C. is the series editor. Both receive royalties from sales.
Funding
The initial RCT was supported by an MRC Clinical Research Training Fellowship to K.T. C.C. is funded by an NIHR Research Professorship (NIHR-RP-2014-04-018). The views expressed are those of the authors and not necessarily those of the NHS, the NIHR, or the Department of Health.
