Abstract
This study examines existing Swedish population data to investigate the evolving role of men in providing informal care for older adults, challenging the persistent stereotype of men’s limited participation. Our findings consistently show that men in Sweden are active and significant participants in a wide range of caregiving tasks. This involvement is profoundly shaped by the Swedish welfare state and cultural emphasis on gender equality, rather than solely by individual caring masculinities. We argue that the high involvement of Swedish men is a normatively supported outcome of a specific welfare structure. By critically questioning frameworks like caring masculinities and feminist ethics of care, which can inadvertently exclude men’s perspectives, we call for a re-evaluation of how male caregiving is theorized and measured globally. Recognizing these gendered patterns within their societal context is crucial for developing inclusive and equitable policies that support all caregivers.
“Traditional masculinity” and “traditional femininity”, hence traditional gender roles, are defined as enduring characteristics, behaviors, and interests that have been conventionally associated with either men or women (Constantinople, 1973). These roles are shaped by strong societal beliefs about what is appropriate for each gender across all aspects of life, including household labor, careers, and personal relationships (e.g., women as caregivers and men as breadwinners) (Coltrane, 1998). This societal framework often assumes men are less likely to be caregivers and that that women are primary caregivers (cf. Björk, 2015; Campbell & Martin-Matthews, 2000; Lyonette & Yardley, 2003; Watt et al., 2014). This assumption is pervasive in the literature and is often linked to factors such as family-oriented welfare solutions, lack of support systems, or traditional gender roles (cf. Goto et al., 2023; Sharma et al., 2016). However, the Swedish context presents a unique case since it has been described as a prime example of a country having a Social Democratic Welfare Regime characterized with universal social rights and a high level of public welfare services (Esping-Andersen, 1990). This includes municipal childcare, disability care and eldercare enabling both women and men to participate in the workforce. Furthermore, Sweden has high levels of employment among women and a well-developed parental insurance.
While traditional structure reinforces the idea of men as breadwinners and women as primary caregivers, being a breadwinner often correlates with reduced opportunities for direct caregiving, this does not equate to a lack of willingness to provide care. Contributing financially can itself be considered a form of informal caregiving (Li & Song, 2019). Caregiving encompasses both formal (paid) and informal (unpaid) support provided by family, friends, or neighbors (Li & Song, 2019). Notably, informal care extends beyond familial relationships, including care provided by non-relatives (Ekwall et al., 2004; Tennstedt et al., 1993). In this context, informal care refers to unpaid support or assistance provided regularly outside of formal care settings, such as caregiving not compensated by The Swedish Social Insurance Agency (Försäkringskassan).
Despite Swedish policies promoting equal parental leave, women continue to undertake a disproportionate share of childcare responsibilities (Statistics Sweden, 2022; Swedish Social Insurance Agency, 2020). However, this gender disparity in childcare does not automatically extend to informal care for older adults. While women remain overrepresented in formal caregiving roles, with nursing assistants being predominantly female (91% women, 9% men) in 2019 (Statistics Sweden, 2021), the pattern in informal care is different. Contrary to expectations, data from 1992 onwards demonstrates a relatively equal distribution of informal care provided by Swedish women and men. We will focus exclusively on Sweden to discuss trends of gender patterns of informal caregiving with a focus on men as caregivers.
Aims
The aim of this study is to investigate the prevalence, characteristics and gender dynamics of informal caregiving in Sweden, focusing on following research questions: • How common is informal caregiving among men in Sweden? • How do the time commitment and intensity of caregiving differ between male and female caregivers? • Are there any differences in the types of informal care tasks undertaken by men and women?
Earlier Research on Gender Aspects in Informal Care
While it is essential to avoid reductive and stereotypical notions of gender, ignoring its influence would result in an incomplete picture. As Tolhurst and Weicht (2023) point out the complexity of caregiving experiences cannot be fully understood without considering the role of gender. Several scholars have highlighted a bias towards women in caregiving research (cf. Wallroth 2016). Studies often focus on the female experience, particularly unpaid care work (Sandberg et al., 2009). This is because caring is constructed as a feminine trait, associated with maternal and nurturing qualities (Ungerson, 2000). Fromme et al. (2005) argue that research frequently compares men’s caregiving to women’s, neglecting men’s own needs and experiences. Henz (2009) suggests that limited definitions of caregiving activities often overlook men’s contributions, thus, studies employing broader caregiving definitions (Ekwall et al., 2004; Lee et al., 1993; Spitze & Logan, 1990; Stoller, 1990) provide a more balanced picture. McDonnell and Ryan (2013), for example, show how gender differences in the caregiver burden can be observed but conclude that there still is a lack of research on the needs and experiences of male carers. However, informal caregiving is influenced not only by gender but also by factors such as care obligations and life stage (Finch & Mason, 1990, 1993; Parker & Lawton, 1994; Ungerson, 1987; Wallroth, 2016). Houde (2002) emphasizes the need for more research specifically focused on male caregivers and their experiences within caregiving relationships. Thus, gender analyses play a central role in caregiving research, typically focusing on women and how gender norms of femininity influence their caregiving behaviors, while overlooking similar considerations for men. Wallroth (2016) calls this a hegemony of care referring to caregiving literature tends to exclude men’s perspectives on caregiving. These analyses seldom delve into the norms of masculinity and the challenges or opportunities they present for men’s caregiving roles. In this article, we argue that adopting a gender-conscious perspective on caregiving necessitates an understanding of how gender norms can impact both men and women in their caregiving roles.
Masculine Norms and Caregiving With Femininity
When examining men’s caregiving, it is crucial to consider the influence of masculine norms alongside the association of caregiving with femininity. This implies that there exists an idealized image of the caregiver that everyone, particularly men, may struggle to fulfil (Wallroth, 2016). Drawing on a constructivist conception of gender and masculinity, Tolhurst and Weicht (2023) explore how gender influences caregiving relationships. They argue that contemporary society values rationalism and economic productivity, while devaluing unpaid care work. This can be particularly challenging for men, as traditional masculinity is often associated with strength and independence, rather than vulnerability and caregiving. These societal norms can lead men to feel conflicted or inadequate when taking on caregiving roles, as they may not align with dominant notions of masculinity (Buchbinder, 2010).
Hanlon (2012) outlines two broad perceptions of men’s caring practices in respect of gender equality. The first perspective is optimistic about progressive change, and the other is more pessimistic about men’s will to change. Many optimistic perceptions of men’s caring practice support the view that women continue to carry the greatest burden of caring labor. However, in the optimistic perspective a gradual generational shift among men is highlighted. Optimistic perspectives also tend to emphasize particular groups of men such as older male caregivers. In the pessimistic perspectives the highlight is instead on men’s continuing power and privilege, and on the fact that men will only undertake caring when there are no women able to do it for them.
There’s a surge of interest in “caring masculinities” (Elliott, 2016; Hanlon, 2012; Scambor et al., 2014). Elliott (2016) and Hunter et al. (2017) have highlighted the need to challenge traditional gender norms and expectations to accommodate men in caregiving roles. By actively engaging in caregiving, men can redefine their gender roles and challenge societal stereotypes. Elliott (2016) proposes a unique framework for understanding care, emphasizing practice over emotion. She argues that men can cultivate nurturing feelings by “doing care work,” ultimately leading to positive changes in gender roles. Similarly, the concept of “caring masculinities” has been explored by researchers (Scambor et al., 2014) to highlight the idea that men can embrace new forms of care that challenge traditional roles. This signifies potential progress towards greater male involvement in achieving gender equality in various national contexts.
The Development of the Swedish Welfare State
Even though Sweden has been described as an extensive welfare state, it has undergone significant changes in recent decades, including policy cutbacks and shifts in priorities, especially regarding elderly care by for example reduced availability to residential care and stricter needs assessments for home help care (Szebehely & Meagher, 2018). Since the 1980s, ideological shifts, cutbacks, market orientation, and an increased emphasis on informal care have led to a renewed focus on the responsibility of families. In the 1970s and 1980s, the welfare state increased, and informal caregiving was characterized, in politics and research, as a complement to public welfare services (Davey et al., 2007; Edebalk, 2022; Sand, 2022; Szebehely & Ulmanen, 2012). During the 1990s, there were cutbacks of social care services for older people and other age groups. These changes in the welfare state have changed the view of the importance of informal caregiving, and now there is a consensus in politics and research that public welfare services are a complement to informal caregiving.
Informal caregiving has been “re-discovered” by the Swedish state, and since 2009, municipalities are legally obliged to offer support for an informal caregiver who provides care for someone with chronic illness, an older person, or a person with functional disabilities (SFS (2009:549), Chapter 5, Section 10). Alftberg (2022) describes this phenomenon as “refamilization,” which refers to a greater dependence on the family due to reduced access to formal care and welfare (Ulmanen & Szebehely, 2015). Finish researchers (cf. Jolanki, 2015; Jukhila et al., 2017) notice a form of “responsibilization”, where individuals are held responsible for tasks that previously fell under the purview of the welfare state. This trend has also been observed by researchers in Sweden, who have noted a growing societal expectation that next of kin should take on a greater responsibility for older family members, with less emphasis on voluntariness (Alftberg, 2022; Szebehely & Meagher, 2018; Takter, 2017; Ulmanen & Szebehely, 2015; Wallroth & Ågren, 2023).
Method
Methods Used in Included Population Studies
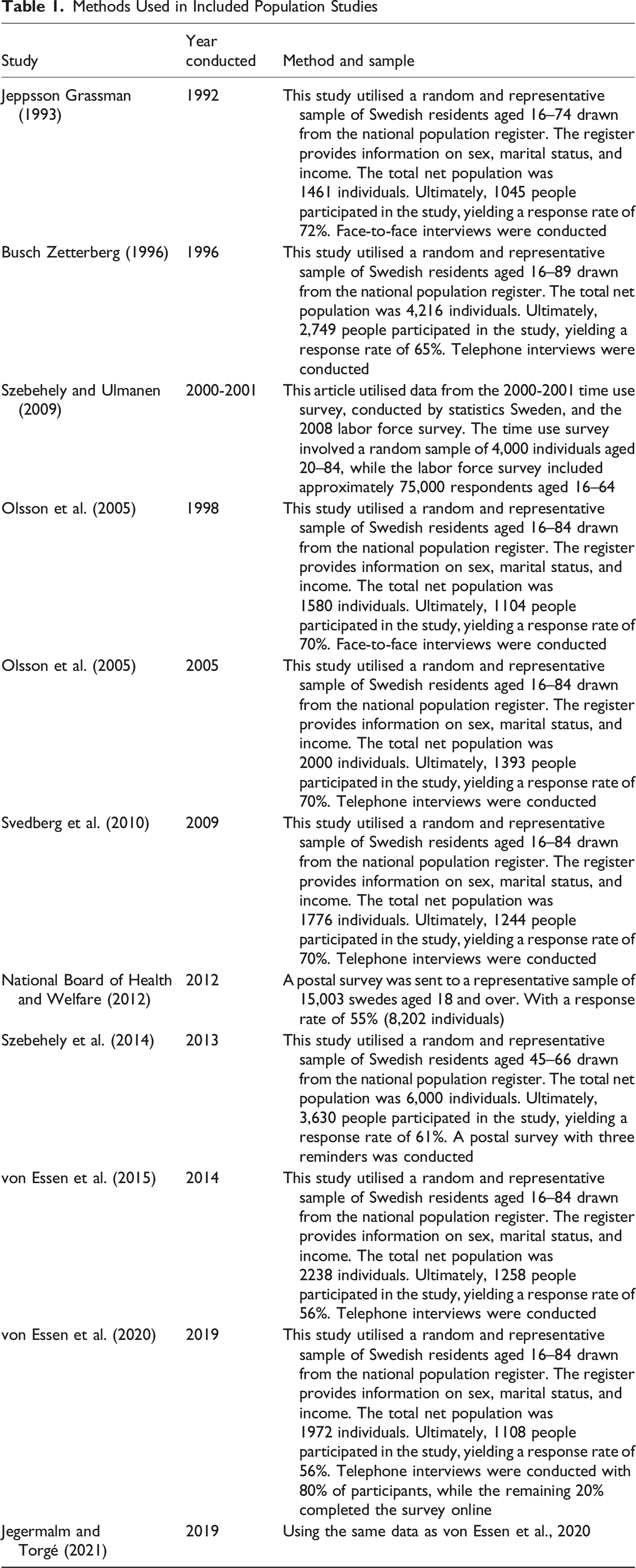
Ethical Considerations
Our analysis specifically focused on identifying gender differences or similarities in the results of the studies we used. As such, we did not conduct our own ethical review. The data analyzed in this study were derived from previously conducted studies that underwent ethical reviews according to the standards in place at the time of their original data collection. Given that the requirements for ethical review have evolved over time, and that the earliest studies included in our analysis were conducted under the ethical guidelines of their respective eras, we have assumed that the ethical considerations pertinent to those studies were adequately addressed at the time.
How Common is Informal Caregiving Among Men in Sweden?
A fundamental question in this article revolves around what previous research has shown about the scope and direction of informal caregiving in Sweden, with a focus on men as caregivers. Answers to questions about the extent of informal caregiving depend on how the questions are posed, it makes a difference whether one asks the giver or receiver of informal caregiving and how one defines what constitutes as caregiving. We can speak of a broad definition that includes both “lighter” tasks and “heavier” tasks (such as housework, personal care, and transport, or whether they kept an eye on someone), or a narrower definition that only includes personal care (such as dressing, bathing, feeding, using the toilet and helping with medication). One distinction that has been used in several studies asks the informal caregiver if the recipient of care has special care needs, in terms of the help was being given to someone who was old, sick, had a disability or “in need of special care in the form of personal and physical care”. Some researchers differentiate between whether one is assisting someone not living in the same household or someone within the household who is old, sick, having a disability or “in need of special care in the form of personal and physical care”. Informal caregiving definitions vary by research tradition. Nursing and social care research often define it as long-term personal and physical care for close next of kin, highlighting the strain on social services (Jegermalm, 2003, 2005; Sundström et al., 2002; Szebehely & Trydegård, 2007). Civil society research uses a broader definition, including help outside organizational frameworks, extending to informal social connections and community groups. This wider scope allows for analysis of “active citizenship” beyond formal volunteering (Henriksen et al., 2008; Hinterlong, 2008; Jeppsson Grassman & Svedberg, 2007; Musick & Wilson, 2007; Putnam, 2000).
Swedish Studies on Caregiving Outside and Within One’s Own Household
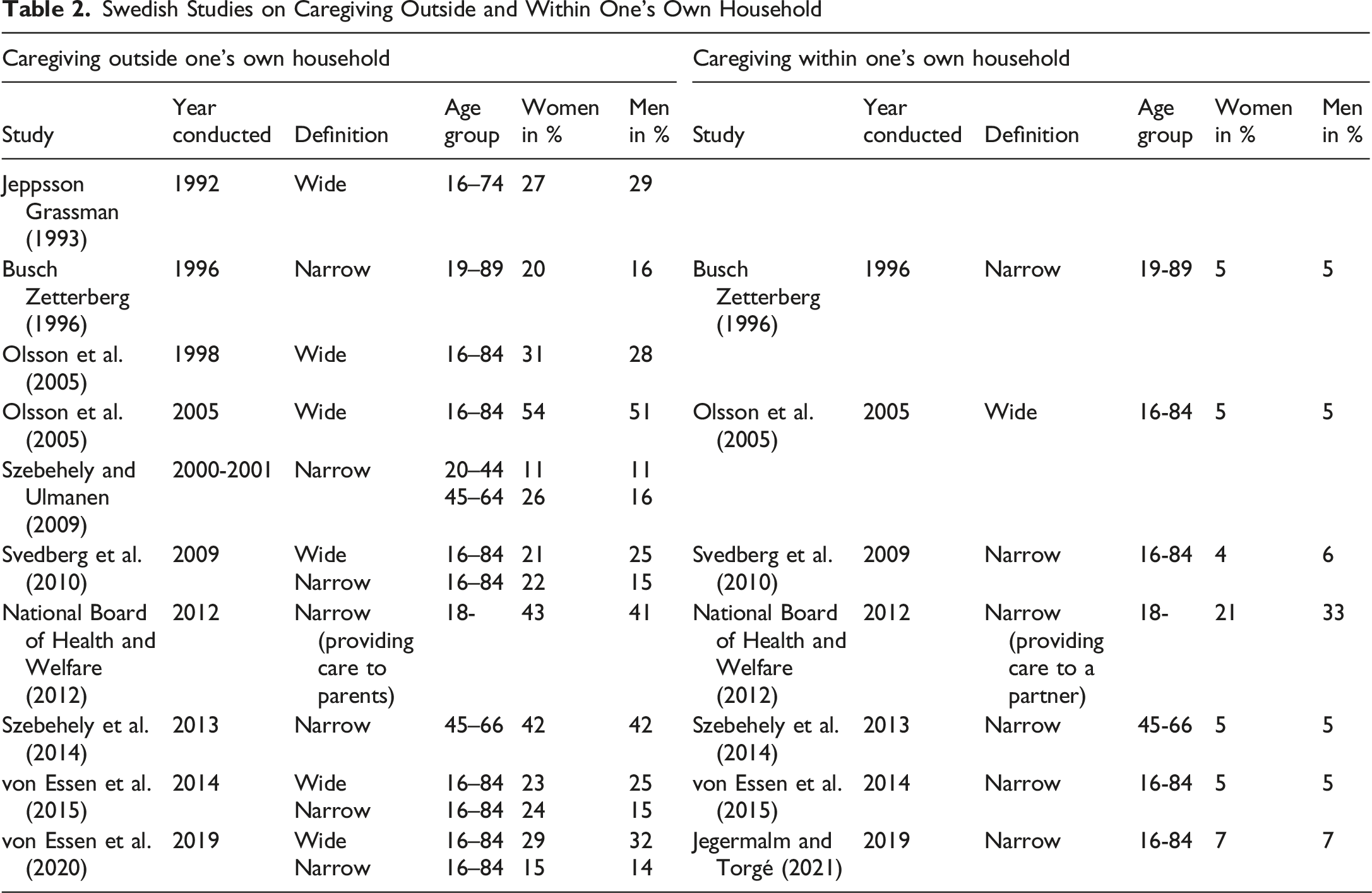
1992–1998
Table 2 shows three studies conducted in the 1990s. A pioneering survey conducted in 1992 by Marie Cederschiöld University (formerly Ersta Sköndal UC) marked the first inclusion of questions about informal caregiving in a representative Swedish population sample. The study employed a broad definition of care encompassing transportation, shopping, household chores, nursing, and other forms of support. Results indicated that 28% of Swedes engaged in such activities, with equal participation rates between men and women.
Another study during this period was conducted by Busch Zetterberg, (1996). In this study a relatively narrow definition of care was used asking if the respondent provided care for someone who was sick, disabled or an older person with care needs. The results indicated that around 23% of women and 20% of men were informal caregivers. The third study from 1998 used the same definition of care as the study from 1992 and showed about the same results as the 1992 study.
The studies conducted in 1992 and in 1998 by Marie Cederschiöld University have been repeated four times in 2005, in 2009, in 2014 and in 2019, as shown in Table 2. The studies contain comparable data from 1992. The filter question used in the 1992 and 1998 surveys was: “This survey is about the extent to which people help other people with things like housework, transport, gardening, personal care or other help. Do you give such help regularly to relatives with whom you do not live with, as well as neighbors, friends or co-workers?” From the 2005 study and onward two examples of caregiving tasks were added, keeping company or keeping an eye on someone (Olsson et al., 2005).
All three studies conducted in the 1990s showed that informal caregiving is common (20%–30%) both among women and men, regardless of whether a wide or narrow definition of care were used. One study (Busch Zetterberg, 1996), studying informal caregiving for someone in the same household showed that 5% of both men and women were caregivers. Thus, the findings from the early 1990s studies consistently demonstrate that informal caregiving is prevalent among both Swedish women and men. Despite variations in care definitions, the research indicates that approximately 20–30% of the population provided unpaid care to individuals outside their household. These early studies laid the groundwork for subsequent research, establishing a benchmark for understanding the scope and nature of informal caregiving in Sweden.
2000–2010
Szebehely and Ulmanen’s (2009) study utilized data from the 2000–2001 Time Use Survey (Tidsanvändningsundersökningen), conducted by Statistics Sweden, and the 2008 Labor Force Survey (Arbetskraftsundersökningen). The study employed a narrow definition of care, inquiring about assistance provided to non-household members with tasks such as grocery shopping, cleaning, laundry, and childcare (excluded from analysis). Among the 3,553 respondents answering this question (Szebehely & Ulmanen, 2009), women aged 45–64 were more likely to provide care (26%) than men (16%). It is important to note that the question’s focus on traditionally female-associated tasks may influence these results.
Studies conducted by Marie Cederschiöld University in 2005 (Olsson et al., 2005) and 2009 (Svedberg et al., 2010) revealed a significant increase in informal caregiving compared to the 1990s. The 2005 study reported a peak in caregiving rates, with over 50% of both women and men providing care. While a modified filter question may partly explain this rise, the data indicate a substantial growth in caregiving activities. The 2009, 2014, and 2019 studies employed a two-step approach to identify caregivers. Participants were first asked about providing regular assistance to non-household members, and subsequently about the care recipient’s specific needs. This yielded two caregiver groups: those assisting individuals without specific care needs and those caring for people with disabilities, illnesses, or advanced age. Notably, men were more likely to provide general assistance, while women were more involved in care for individuals with specific needs. Consistent with previous research (Busch Zetterberg, 1996), both the 2005 and 2009 studies yield, with minor deviations, that both women and men provided care to a spouse or partner within their household.
The studies from the years 2000–2010, using a wide definition of care, indicates an increase in the prevalence of informal caregiving, both among women and men. From around 30% to about 45% of the Swedish population (women and men) identifying themselves as carers. While the prevalence of caregiving within households remained relatively stable, care provided to individuals outside the household experienced significant growth.
2012–2019
In early 2012, the Swedish National Board of Health and Welfare (Socialstyrelsen) commissioned Statistics Sweden to conduct a population study, exploring the prevalence of caregiving within the Swedish population. The initial survey question inquired about providing regular care, help, or support to someone due to illness, disability, or old age. Over one-fifth (24%, or 1,964 individuals) reported providing such care regularly. A follow-up question narrowed the focus to caregivers who provided support more than once a month. This resulted in a group of 1,513 individuals (18% of the initial sample). Women (20%) were slightly more likely to be caregivers in this category than men (16%). It is important to note that the study did not distinguish between care provided within or outside the caregiver’s household. Thus, in Table 1 we have included the number of women and men answering that they provided care for a parent or to a husband/wife thus assuming that partners are living together, and adult children do not liv together with their parents.
The National Board of Health and Welfare (2012) study found that most care recipients (60%) lived in their own homes, separate from the caregiver. This suggests that a significant portion of caregivers provide support remotely. Parents were the most common care recipients, with nearly half of caregivers (48%) reporting helping a parent. This trend held true across most age groups but became more pronounced with age. Around 50% of caregivers aged 18–29 helped a parent. This figure rose to 68% for those aged 45–64. Men were more likely to provide spousal care (33%) compared to women (21%). One possible explanation could be that this speaks to men’s difficulties asking and accepting help. This difference was further amplified by age. Only 10% of respondents aged 45–64 reported providing care to a spouse or partner. In the 65–80 age group, this figure rose to 33%. Among those 81 years of age and older, a significant 77% helped their spouse or partner. When looking at those who provide care daily, there was no difference at all between men and women.
Data from 2013 (Szebehely et al., 2014) come from a survey conducted by the Institute of Social Work at the University of Stockholm, where 3630 people aged 45–66 years responded to questions on caregiving for people outside their own household (see Szebehely et al., 2014). The study used a wide definition of care, and the results showed that 42% of both women and men reported that they were carers. The two studies from 2014 and 2019 conducted by the Marie Cederschiöld University indicates that it is somewhat more common among men to provide informal help to someone without care needs. While in the 2014 study it was more common among women to help someone with care needs, the 2019 data indicated that this informal caregiving had become about equally common for both men and women. Possibly this convergence in informal care provision could, at least in part, be attributed to a reduction in social services provided due to stricter needs assessment.
In sum, the studies presented in Table 2 show that the prevalence of informal caregiving differs over time and is also dependent on whether the studies have used a narrow or wide definition to identify the carers. The studies show that it is common among men to identify as informal caregivers in all studies even though there are differences. In the studies using a narrow definition of care there are usually more common among women, but the difference is about 1%–10% mostly within a 5% margin. Five of the studies asked specifically if the caregiving was within one’s own household. In four of them, around 5% of both women and men responded that they provide care for someone in their household, and in one study, the percentage was 7%.
How Do the Time Commitment and Intensity of Caregiving Differ Between Male and Female Caregivers?
In Jeppsson Grassman’s (1993) study, few questions were also asked about the extent of informal caregiving to someone outside their own household. As previously mentioned, the results showed that 28% of Swedes performed such work, with men and women equally likely to participate. However, women performed on average almost twice as many hours of help per month as men.
Svedberg et al.’s (2010) study demonstrates that 5% of the population helps someone in their own household with special care needs, a consistent finding across both the 2005 (Olsson et al., 2005) and 2009 studies (Svedberg et al., 2010). However, the 2009 study (Svedberg et al., 2010) reveals a significant increase in the number of hours, from an average of 67 h per month to just over 91 h. Although Svedberg et al. (2010) showed that men provided slightly more informal care within their own households, a substantial disparity exists in the extent of their efforts: 36 h on average for men compared to 153 h for women. For those helping outside their household, men were more likely to assist those without special care needs, providing slightly more hours (Svedberg et al., 2010).
The Szebehely et al. (2014) study found that female caregivers dedicate more time to helping, averaging 5.4 h per week compared to 3.8 h per week for male informal caregivers. This gender difference stems partly from more women than men providing daily care, but primarily from women who provide daily care offering more hours of help than their male counterparts. Among those providing daily care, women contribute 19.1 h of care per week compared to 12.7 h for men.
In the von Essen et al. (2015) study, the research team compared the results of studies conducted and analyzed by the research group at Marie Cederschiöld University. The average number of hours per month for those providing regular care to someone they do not live with, within the 16–74 age group, was as follows: 1992 (women 15, men 9, total 12), 1998 (women 13, men 11, total 12), 2005 (women 14, men 9, total 11), 2009 (both women and men 17, total 17), and 2014 (women 16, men 12, total 14). A slight increase in hours is observed, from 12 h in the first two studies (1992, 1998) to 14 h in the 2014 study, with a peak of 17 h in the 2009 study. The results demonstrate that women consistently performed more hours on average per month than men in four out of the five studies. In the 2014 study, women provided an average of four more hours of informal care per month than men.
The von Essen et al. (2020) study does not clearly reveal significant gender differences measured over time. However, for those helping someone outside their own household with special care needs, a decrease is observed, from just over 20% in the 2005 study (Olsson et al., 2005) to around 15% in the two most recent studies (Svedberg et al., 2010; Von Essen et al., 2015). While women constituted a majority of caregivers in this group during the 2005–2014 period (approximately 55%), the 2019 study showed a more equitable distribution, with women and men providing care with similar frequency and for approximately the same number of hours.
The studies demonstrate that both men and women provide informal care, but in most instances, women report more hours of informal care per month than men. Men tend to provide slightly more care than women to people outside their own households who do not have special care needs. However, a trend towards increased male participation in informal care is evident, particularly in recent studies.
Are There Any Differences in the Types of Informal Care Tasks Undertaken by Men and Women?
Research suggests that men often express caregiving through a distinct set of masculine behaviors, emphasizing practical tasks, technical skills, and taking control (Anjos et al., 2012; Björk, 2015; Campbell & Carroll, 2007; Milligan & Morbey, 2016; Spendelow et al., 2017). This aligns with findings by Jeppsson Grassman (2001) who identified a difference, with women providing more personal care and men taking on tasks like repairs and transportation. Further supporting this, Jegermalm et al. (2014) compiled quantitative studies indicating men gravitate towards practical help like shopping and supervision, while women tend to focus on personal care. One question that becomes evident is what care is and what it consists of. Wærness (1983, 1996) defines care as doing something for someone who cannot perform the task themselves or would have great difficulty doing so. What care consists of can be understood through Horowitz’s (1985) division of caregiving efforts. Horowitz (1985) categorizes caregiving into: emotional support (socializing, comfort, advice, availability); provision of services (personal care, medical tasks, household chores, transport, shopping, administration); mediation with organizations (authorities, healthcare); financial support; and cohabitation (living together to provide care).
Caregiving Tasks
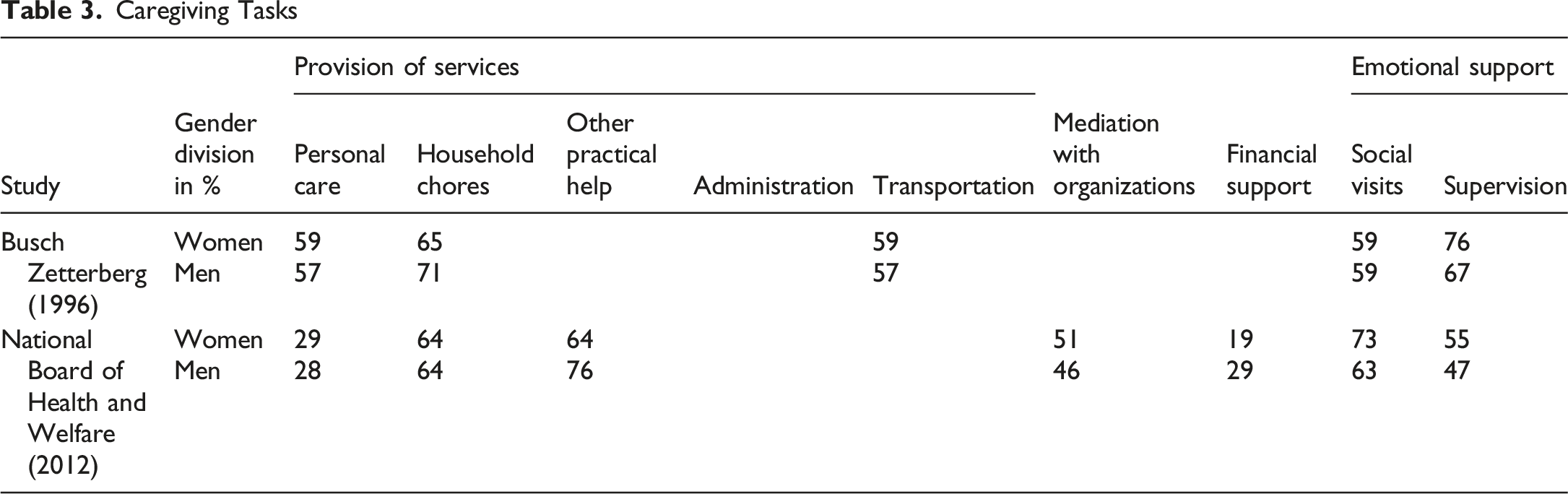

The early study by Busch and Zetterberg (1996) found no significant gender differences in informal care tasks, except that a slightly higher proportion of women reported providing supervision (women 76%, men 67%) and a slightly higher proportion of men reported performing household chores such as cooking, laundry, cleaning, gardening, and home maintenance, as well as accompanying individuals to hospital appointments. However, it is important to note that in Busch and Zetterberg (1996), household chores were not distinguished from other forms of practical assistance; therefore, these categories were combined. The National Board of Health and Welfare (2012) showed that the most common form of care was socializing, which was reported by 73% of women and 63% of men. The same study showed that 63% of women and 64% of men helped with chores such as shopping, cleaning, laundry, and cooking. When it comes to personal care, 29% of women and 28% of men reported that they helped with such things. According to this study, the differences between men and women when it comes to things that can be seen as more traditionally feminine tasks were thus not particularly large. There was a slightly larger difference between the question of other practical help, where 64% of women and 76% of men reported that they provided such care. Men also provided financial support to a greater extent (29% compared to 19% of women).
Discussion
This study aimed to investigate the prevalence, characteristics, and gender dynamics of informal caregiving in Sweden, addressing the following research questions:
How common is informal caregiving among men in Sweden? How do time commitment and caregiving intensity differ between male and female caregivers? What are the differences in the types of informal care tasks undertaken by men and women?
We have approached these questions with a gender-aware and masculinity-informed perspective, aiming to understand how gender norms influence both men and women in their caregiving roles, alongside the impact of the welfare state context. Our analysis of existing population studies shows challenges of defining and measuring caregiving. Definitions of informal care varies in impacting prevalence, estimates and caregiver characteristics. Some studies adopt broad definitions encompassing a wide range of support activities, while others focus narrowly on personal care. These differing definitions significantly influence the identification of caregivers. Furthermore, the distinction between care provided within and outside the household is crucial for understanding caregiving roles and responsibilities. Studies indicate that a substantial portion of the Swedish population, both men and women, engages in informal caregiving. It is important to acknowledge that how caregiving is defined and measured can significantly influence observed gender differences. Moreover, gender norms and societal expectations shape how individuals perceive and perform caregiving roles. While both men and women engage in a wide range of caregiving activities, including personal care, household chores, and emotional support, there may be some differences in the specific tasks performed. Nonetheless, Swedish men demonstrate significant involvement in informal caregiving to older adults.
When connecting this to Hanlon’s (2012) perceptions of men’s caring practices in respect of gender equality, it becomes clear that Swedish men are involved in informal caregiving. This suggests that the optimistic view holds true, and it is no longer certain that women will continue to bear the greatest burden of caregiving labor—at least when it comes to informal care. As Wallroth (2016) concluded this involvement is not simply a matter of men filling a gap when female caregivers are absent. However, the studies we used do not tell us anything about how men and women interact regarding informal care at an individual level. Different cultural norms likely influence the willingness of men and women to respond to questions about caregiving. Understanding the high prevalence of male involvement in informal care in Sweden requires consideration of several factors. The Swedish welfare state, with its extensive elderly care, disability care and childcare, and the demand for both women and men to work full-time, coupled with a strong commitment to gender equality—a commitment that is quite radical in many other countries—likely contributes to men’s high involvement in informal care in Sweden. It also contributes to a breakdown of masculine norms that emphasize the breadwinner role.
Thus, informal caregiving by men in Sweden can be viewed through both a linguistic and an empirical lens. It is important to consider the limitations of these studies in Tables 2 and 3 and the potential influence of gender norms on caregiving behaviors. For example, while there may be variations in the specific tasks performed by men and women in caregiving roles, these differences should be understood within the broader context of gender norms and empirical evidence. However, it is important to acknowledge a potential limitation: studies may not capture the full extent of care provided by caregivers, as they often rely on self-reported data about specific tasks.
A common suggestion in caregiving literature is that men tend to overreport their caregiving (cf. Björk, 2015; Campbell & Martin-Matthews, 2000; Lyonette & Yardley, 2003; Watt et al., 2014). However, perhaps it is time to consider the possibility of underreporting, as men may not be as accustomed to associating their actions with caregiving. Men may be more likely to report practical tasks, while women may be more inclined to emphasize emotional support and personal care. One explanation for men’s potential underreporting of caregiving, particularly in the form of socializing, could be the emphasis on practical tasks. Gender norms often position women as more emotionally oriented and men as more practically inclined. Thus, it may be easier for men in quantitative studies to recognize and tick the box for practical help (cf. Jegermalm, 2006) than to call it socializing. For men, it may also be easier to socialize over a task while women may see socializing as the central thing and the task as a part of socializing. This thus has to do with gender norms but also how studies are designed. Winqvist (1999) also criticizes this division of emotional support, arguing that it is not always possible to separate emotional support from other tasks. For example, family members may show and provide emotional support by helping practically. Thus, as societal norms evolve, men begin to understand that the “help” they provide is indeed care. They start to adopt and understand a “care language” that was previously more associated with women. In this way, they also begin to identify themselves as caregivers. On the other hand, there’s an argument that women may be underrepresented as caregivers because their caregiving roles are so deeply ingrained that they may downplay them, as they are seen as part of their traditional roles. Szebehely and Ulmanen (2012) suggest that: “There are likely systematic differences between women and men in their perceptions of what constitutes providing care; differences that probably mean that women underestimate their contributions while men overestimate theirs” (p. 20, author’s translation). Another explanation is that researchers are increasingly highlighting findings that deviate from the assumption that only women provide care. However, men’s contributions to informal care in Sweden are no longer as easily dismissed as overexaggeration or as a different type of, less demanding, care.
Recent research on “caring masculinities” (Elliott, 2016; Hanlon, 2012; Scambor et al., 2014) emphasizes the need to challenge traditional gender norms to accommodate men in caregiving roles (Elliott, 2016; Hunter et al., 2017). Elliott (2016) argues that men can cultivate nurturing feelings through “doing care work” (p. 255), ultimately redefining their gender roles. This aligns with Scambor et al. (2014), who observe a growing trend of caring masculinities in Europe, suggesting potential progress towards greater gender equality.
However, some questions need to be addressed to nuance the debate of “caring masculinities”. The first one is that a conceptualization of “caring masculinity” builds on the assumption that men have not been involved in caregiving before. The second one is that “caring masculinities” gives the impression that men who provides care are a certain kind of man even a new type of man. The third one is that conceptualization of caring masculinity gives the impression that only men can choose to provide care, but women cannot. The fourth one is that there is an assumption that men’s less involvement in care is because their privilege position in society and women’s involvement in care is seen as a burden. These assumptions overlook what may be the main cause: a research bias where men’s caregiving has not been given the same attention as women’s. We lack sufficient knowledge about men’s care. Their voices have not been amplified to the same extent as women, and when they are heard, they are often interpreted from a feminist ethics norm. The concept of “caring masculinities” can inadvertently reinforce the very binary it seeks to dismantle. By labelling men who provide care as a distinct category, it risks implying that caring is somehow “natural” for women but “unnatural” for men. This reinforces the notion of a feminine essence tied to caregiving. However, as Wallroth (2016) argues, caregiving is not a preordained feminine trait, but a human capacity. Another key consideration is as we have already argued how we define “caregiving” itself.
While Tolhurst and Weicht (2023) rightly emphasize the importance of gender in understanding caregiving experiences, it is crucial to acknowledge the limitations of a solely gender-based perspective. An overemphasis on gender norms can inadvertently reinforce stereotypes and overshadow other significant factors influencing caregiving roles and experiences. As Olsson et al. (2005) highlight, informal caregivers exhibit significant diversity in their motivations, experiences, and the nature of the care they provide. Recognizing this diversity is essential for a comprehensive understanding of caregiving dynamics. For instance, occasionally driving a neighbor’s child to soccer/football practice differs significantly from the daily, multi-hour commitment required to care for an elderly parent with significant needs. Another way of exploring the spectrum of informal caring we find in Jegermalm and Torgé (2021) study. Using data from a nationally representative survey of caregivers in the Swedish population they describe three different caregiver profiles and analyze them in relation to their panorama of care, that is, the extent to which caring is shared with other formal and informal co-carers. The profile of “Co-habitant Family Carer” includes caregivers who provide care to someone living in the same household with special care needs. They are typically older, often married, and provide a significant amount of care, including personal care, housework, and companionship. The profile of “Care Network” consists of caregivers who provide care to someone outside their household with specific care needs. They are often older and provide a mix of care, including personal care, housework, and companionship. They rely on a combination of formal and informal support. The profile of “Helpful Fellowman” includes caregivers who provide care to someone outside their household without specific care needs. They are typically younger and provide less intensive care, such as keeping company and assisting with practical tasks. They rely less on formal support but have a strong social network. What also can be interesting to point out is that a slight majority of caregivers in all three profiles are men (Jegermalm & Torgé, 2021). Overall, our examination of existing population studies in Sweden challenges traditional gender stereotypes but also questioning theoretical perspectives such as caring masculinities and feminist ethics of care, demonstrating that men in Sweden are increasingly involved in caregiving roles.
Conclusion
Men in Sweden actively participate in informal caregiving for older adults. This is consistently evident across various studies and time periods. The Swedish welfare state and cultural emphasis on gender equality contribute to men’s involvement. Both men and women engage in a wide range of caregiving tasks, including personal care, household chores, and emotional support. While some gendered differences exist, both genders contribute significantly. Gender norms, societal expectations, the presence or absence of adequate public welfare services and individual circumstances significantly shape caregiving roles. Moreover, these factors also influence how we empirically study caregiving. Researchers may inadvertently focus on women as the primary informants while neglecting the perspectives of male caregivers. Thus, research methodologies and interpretations can be inadvertently shaped by prevailing gender norms and expectations, potentially leading to biased findings or an incomplete understanding of the complexities of informal caregiving. Focusing solely on women as primary caregivers can lead to an incomplete understanding of caregiving, potentially overlooking the vulnerabilities and experiences of men in caregiving roles.
It is important to acknowledge that both men and women can be informal caregivers. When we emphases differences between men and women in caregiving, we may inadvertently miss opportunities for shared caregiving responsibilities and a more equitable distribution of care work. Focusing solely on gender disparities in caregiving may oversimplify a complex issue. Both men and women contribute to caregiving in diverse ways, and a more nuanced understanding requires considering a range of factors beyond gender. By recognizing these gendered patterns in caregiving within their broader societal context, we can work towards developing more inclusive and equitable policies and support systems for all caregivers.
While existing literature documents men’s involvement in care, this study makes a novel contribution by providing a gender-aware and masculinity-informed analysis grounded in the unique Swedish welfare state context. By focusing on Sweden, which has shown a relatively equal distribution of informal care between men and women since 1992, the study counters the widespread assumption that women inevitably carry the greatest burden of informal caregiving. By critically questioning theories like caring masculinities and feminist ethics of care, we argue that these frameworks can inadvertently reinforce gender binaries and exclude men’s perspectives, instead proposing that male involvement is significantly shaped by several reasons and circumstances but mostly by a country’s welfare policies. We also bring attention to how the definition and measurement of caregiving, and the very language of care, can be biased. This is potentially leading to the underreporting of care by men. In essence, the study’s novelty is the argument that men’s high involvement in care of older adults in Sweden results from a synthesis of the welfare system and societal gender norms. Their participation is thus a normatively supported outcome of a specific welfare structure, not merely an individual choice or a caring masculinity. This perspective requires a re-evaluation of how we theorize and measure male caregiving globally. Providing informal care in Sweden is not just a women’s issue because viewing it solely as such risks cementing care work as an exclusive female burden, obscuring the fact that caregiving is a fundamental human capacity shaped by welfare policy and societal norms, and effectively ignoring both the existing contributions and the immense potential for male engagement.
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
