Abstract
The reduction and cessation of vaping for young people is a global health priority, however the operationalization of guidelines into school programs is challenging. The focus of this quality improvement project was to utilize the plan-do-study-act framework and Social Cognitive Theory to support vaping cessation in Australian secondary schools. Ten school nurses led a program across 12 schools and supported 86 young people to grow knowledge and skills to reduce vaping. At baseline, most young people had self-reported that they had vaped for over a year (n = 61; 70.9%) and were aware of associated harms. Immediately post-program, 34.1% (n = 29) intended to change behavior, and at 4-week follow-up, 61% (n = 22) reported behavior change. All school staff valued and supported the program, with key benefits of professional health education delivery by a known nurse and improved health literacy, and barriers of student absences and scheduling conflicts.
Introduction
Vaping, or the use of e-cigarettes, has become a significant public health concern among adolescents due to its widespread availability and targeted marketing. The appealing flavors, attractive packaging, and the perception of vaping as a safer alternative to smoking contribute to its popularity among young people (Nguyen et al., 2019). Despite its growing use, health information about vaping remains inconsistent and often misunderstood. Many adolescents believe that vaping reduces stress and poses fewer risks compared to smoking traditional cigarettes, highlighting the urgent need for accurate communication about the risks associated with vaping (Thoonen & Jongenelis, 2023).
The presence and concentration of nicotine in vapes is concerning due to nicotine's highly addictive nature and its impact on learning, memory, and attention (Goniewicz et al., 2019). Vaping and similar product use carry a range of additional serious risks, including lung damage, physical injuries and burns, acute nicotine poisoning, and environmental pollution. Research has linked these products to adverse effects on cardiovascular health, such as elevated blood pressure and heart rate, as well as reduced lung function and interference with brain development during adolescence (Traboulsi et al., 2020). For adolescents and young people, the pathway to further health risks are clearer with those who use e-cigarettes being three times more likely to start smoking tobacco compared to non-smokers who do not use e-cigarettes (Baenziger et al., 2021).
Locally in Queensland (Australia), the School-Based Youth Health Nurses (SBYHNs) service noted a significant increase in school suspensions due to vaping. This trend, along with requests from school principals for more support, underscored the rising prevalence of vaping among high school students. Like many schools globally, Queensland schools were increasingly looking for educational strategies to address vaping issues before resorting to disciplinary measures like detentions, suspensions, and exclusions, that do not motivate adolescents to change their behavior (Hemphill et al., 2012). Overly punitive responses to vaping can lead to young people disengagement from school, heightening the risk of future substance use problems (Dovetail, 2022). Prevention initiatives are widely recognized as the most cost-effective approach to tackling public health issues, including substance use, making them a top priority (Substance Abuse and Mental Health Services Administration (US), 2016). In 2022, in the context of emerging federal legislation aiming to restrict the availability of vapes for young people (Freeman, 2025), the Australian Bureau of Statistics reported that 38% of young people aged 18–24 and 18% of those aged 15–17 had used vapes, with these figures expected to rise (Australian Bureau of Statistics, 2022). In response, the Queensland Government invested $5 million (AUD) to provide schools with access to the Blurred Minds Academy, an alcohol and drug education program. This program offered teachers educational materials linked to the curriculum for years 7 to 10 and provided education to teachers and parents/carers about vaping (Hrynyschyn et al., 2023). Students can also seek individual support from the Guidance Officer or SBYHN to quit vaping and can be referred to QUITLINE or general practice for further assistance. These governmental interventions encompass various strategies, including broad-based education and targeted clinical interventions for individuals. School-Based Youth Health Nurses recognized the need for an additional approach for young people and developed a single-session group-based program. While multi-session group programs for smoking cessation have proven effective (Mersha et al., 2023), they are often impractical in school settings due to time constraints and high dropout rates (Gould & Watters, 2015). In Australia, a pragmatic study by Gould and Watters (2015) found that the quit rate for smoking in single group sessions was comparable to that of multiple group sessions, making this a feasible approach for addressing vaping in schools.
Many young people consider quitting e-cigarettes due to health concerns, including addiction. They may also want to stop to enhance sports performance or because they feel e-cigarettes are not accepted by parents. Cost and the perception of being manipulated by the e-cigarette industry are also factors. Additionally, the lack of reliable information about e-cigarettes drives the need for credible, evidence-based guidance. School-based Youth Health Nurses are experienced in helping behavior change and can provide health-focused, evidence-based information to support young people. A 2017 systematic review (Waller et al., 2017) identified several key factors that facilitate the implementation of tobacco and substance use interventions in schools. These factors include a positive organizational climate, sufficient training, and the motivation of both teachers and students.
Adolescents face a range of complex factors when it comes to smoking and quitting, often attempting to quit without assistance. Although younger smokers express a desire to quit (Jongenelis et al., 2024), they frequently have negative attitudes toward formal cessation programs. This highlights the importance of exploring innovative and accessible approaches for this population. Combining broad educational initiatives with targeted interventions may provide a comprehensive strategy to reduce vaping among adolescents (Hanley-Jones et al., 2022)
Aims
This quality improvement project aimed to evaluate the impact and implementation of a Vaping Small Group Education Program, based on Social Cognitive Theory (SCT) (Bandura, 2013), in Australian high schools. Specifically, it sought to:
Assess whether a Vaping Small Group Education Program influenced young peoples’ vaping knowledge and self-reported behavior. Evaluate the perceived value and barriers of the Vaping Small Group Education Program from the perspectives of young people, school staff and school nurses.
Methods
Design
A non-experimental Plan, Do, Study, Act (PDSA) approach was used. The single-session health education program was first co-designed and piloted in two schools, then implemented across 12 schools over a ten-week term. It was evaluated with pre-program, post-program, and 4-week follow-up cross-sectional surveys from the perspectives of the young person participating in the program, the school staff and the school nurses leading the program.
The Standards for Quality Improvement Reporting Excellence (SQUIRE 2.0) (Ogrinc et al., 2015) guidelines were utilized to underpin the project design and reporting. This study received approval from the Children's Health Queensland Human Research Ethics Committee (Ethics application number EX/2024/QCHQ/106066). No conflicts of interest were identified, and all collected data were de-identified.
Context
Children's Health Queensland (CHQ) SBYHN service is delivered in state (government funded) high (grades 7–12) schools by Clinical Nurses in partnership with the state government Education Queensland department in Australia. As a collaboration between the state government run health and education departments, this service aims to provide brief interventions to improve young people's health and reduce risk-taking behaviors, including drug and alcohol use (Caulkins et al., 2002). In the first 28 weeks of 2024, SBYH data showed that 64% of young people seeking Alcohol, Tobacco and Other Drugs support did so for vaping. Additionally, SBYHNs across the service anecdotally reported receiving increased referrals for young people returning from suspension for vaping, prompting schools to seek alternatives to suspensions.
To prepare for the project, a needs analysis was undertaken, with consultation between SBYHN and school staff, school needs were prioritized and existing vaping support programs identified, including existing education programs within core curriculum. Consultations included discussions with school staff, local AOD organizations, and the SBYHN team. After these discussions, SBYHN nurses in ten public high schools in Southeast Queensland (within catchment from the Children's Health Queensland Health Service District) were opted in and were selected for the single-session health education program, known as the Vaping Small Group Education Program.
Participants
The Vaping Small Group Education Program was a one-time education session for young people aged 12–18, enrolled in the twelve selected schools in southeast Queensland, who were referred by schools or self-referred. These young people came from diverse socioeconomic backgrounds and were identified as vape or e-cigarette users, either through self-referral or school staff referral for vaping at school. Self-referring individuals did so as Gillick Competent, highlighting their right to make healthcare decisions when deemed competent (Griffith, 2016).
Participation was voluntary, and referrals not accepted if presented as punitive. Sessions lasted one hour, with groups of three to eight participants of similar age (12–14 or 15–18 years). Referrals were reviewed for appropriateness, and participants were organized into junior and senior groups based on .. Coordination with schools ensured consistent scheduling and accessibility for participants.
Intervention (The Vaping Small Group Education Program)
The Vaping Small Group Education Program session covered vaping risks, benefits of quitting, legality, social consequences, harm reduction, managing nicotine dependence, and support resources based on existing Queensland Health-based evidence practice guidelines (Dovetail, 2022) . The content was driven by Social Cognitive Theory (SCT), which identifies several key factors that influence an individual's readiness to quit and their ability to succeed in quitting (Bandura, 2013). This was used to develop the intervention, focusing on social support, outcome expectations, behavioral capability, and self-efficacy (Bandura, 2013).
School nurses based at the 12 participating sites received professional development and resources, including a lesson plan and a comprehensive manual. The group sessions were facilitated by the school nurse, who provided participants with information sheets and consent forms, emphasizing voluntary participation and could withdraw at any point without facing negative consequences, confidentiality, and available resources for further support.
The program's content was grounded in the theory that interventions should promote positive behavior change whilst incorporating adolescent learning styles (Bonell et al., 2015). It was designed to be interactive, encouraging activities and discussions to engage young people in active participation rather than passively receiving information (Hieftje et al., 2021).
The session began with icebreakers, followed by an interactive discussion on vaping motivations and drawbacks, using motivational interviewing and decisional balance. A four-column diagram was used on the whiteboard to help students identify and reflect on their reasons for vaping in a non-threatening way, facilitating consideration of changes to their habits and assessing their readiness for change.
Participants then explored myths and truths about vaping, using a normative education approach (East et al., 2021) . This normative education approach, recognized as best practice in vaping education effectively addressed and corrected misconceptions and beliefs regarding vaping harms, behaviors, and industry marketing strategies. The session included education in relation to nicotine and signs of dependence by use of video content as well as asking young people their own experiences. This was seen as an important inclusion given the high nicotine content of vapes and that young people are more susceptible to addiction.
Harm minimization was a key component throughout the session and young people were given information in an age-appropriate way to encourage ways to reduce harm if they continued to use vapes (Dovetail, 2022). The session concluded with opportunities to engage in activities designed to build upon skills such as relaxation, self-regulation and refusal skills as well as identifying healthier alternatives to vaping, information in relation to pharmacotherapy and how to help seek.
Measures
The Vaping Small Group Education Program was evaluated from the perspectives of the young person, the school staff and the school nurses.
Outcomes for the young people were self-reported vaping knowledge (e.g., “What do you know about vaping?” [open text response]), behaviors (e.g., “Will your vaping use change?” Options: Yes/ Undecided/ No; “How could it change?” Options: Vaping less / not dry puffing / Not vaping at school / Not re-using disposable vapes / Putting vapes out of research / Other)) and access to support (e.g., “Where could you get help for vaping?” Options: Doctor / School Nurse / Teacher / Parent/ Online).
Outcomes for school staff were the program's perceived value to young people (e.g., “In what ways did you find the program valuable?” Options Increasing health literacy, Onsite delivery by nurse known by students, Alternative to other consequences, Timely support and education, Other), identify any barriers to implementation (e.g., “What (if any) barriers did you experience?” Options Timetabling, student absence, referral process, no barriers) and determine if they wanted the program to continue.
Outcomes for SBYHN were ease of use (e.g., How easy was the lesson plan to follow? Likert scale response), confidence in advocating and negotiating with the school (e.g., How confident were you communicating with the principal to advocate for the program? Likert scale response), observed young people engagement (e.g., How engaged were the students in the group? Likert scale response), and their views on the program's continuation.
Data Collection
Student, staff and school nurse outcomes were collected via cross-sectional surveys. Student surveys were distributed via paper at the pre-phase of the education event (later imputed into Microsoft Forms®), with an electronic survey (Microsoft Forms ®) attached via email for the four-week follow-up. All responses were anonymous, however key demographic characteristics were collected at the pre-phase, for descriptive purposes only.
School staff and nurses outcomes were collected via cross-sectional electronic survey at the conclusion of the 10-week trial. School staff, primarily teachers and principals, were invited to provide feedback (maximum of two surveys per school). These surveys were not anonymous, as the school's name was required to understand which schools found value and to identify individual barriers.
Data Analysis
Data have been analyzed descriptively, appropriately to data characteristics (counts, percentages) within Microsoft Excel®. Open text fields were thematically categorized by a research assistant (LN), with double checking of categorization by a senior academic in the field of pediatric nursing (AJU).
Results
All 12 schools successfully implemented the Vaping Small Group Education Program in Term 2/Autumn (April-June) 2024, with participation from 86 young people (see Figure 1).
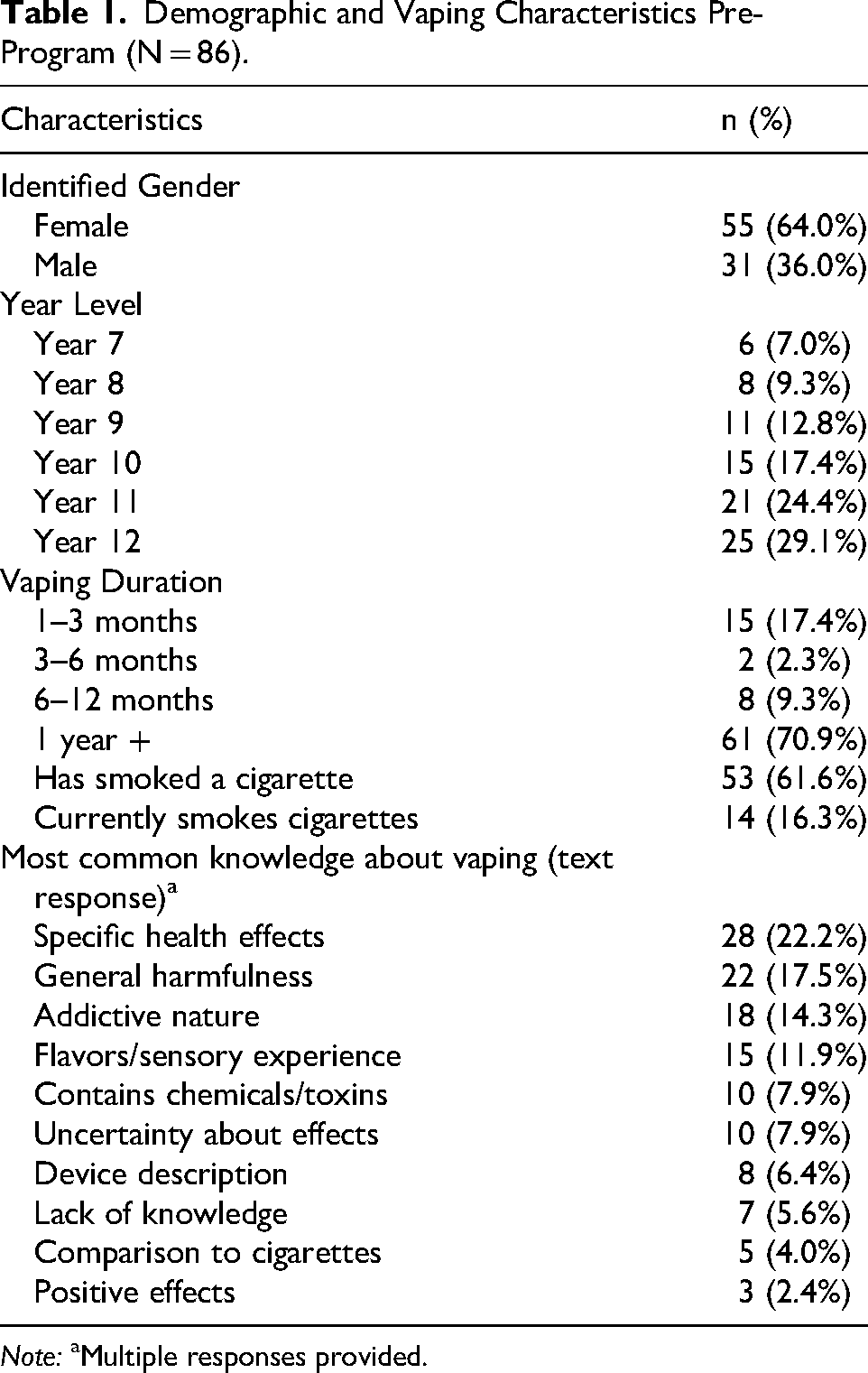
The demographic characteristics of the young people that participated in the program can be found in Table 1. Of the 86 young people, the majority identified their gender as female (n = 55; 64.0%) and ranged from Year 7 to Year 12, with the largest group in Year 12 (n = 25; 29.1%).
Demographic and Vaping Characteristics Pre- Program (N = 86).

Note: aMultiple responses provided.
Young People Vaping Knowledge and Behaviors
At baseline (pre-program), most young people reported vaping for over one year (n = 61; 70.9%). More than half had smoked a cigarette at some point (n = 53; 61.6%), though few were current smokers (n = 14; 16.3%). Most young people demonstrated awareness of vaping harms, with 22.2% (n = 28) identifying specific health risks (e.g., lung cancer respiratory complications) while others (n = 22; 17.5%) demonstrated knowledge of broader concerns about its general harmfulness (e.g., “its bad for you”). Other key knowledge areas were the addictive nature of vapes (n = 18; 14.3%; e.g., “nicotine is addictive”) and their containment of chemicals or toxins (n = 10; 7.9%; e.g., “over 200 chemicals”).
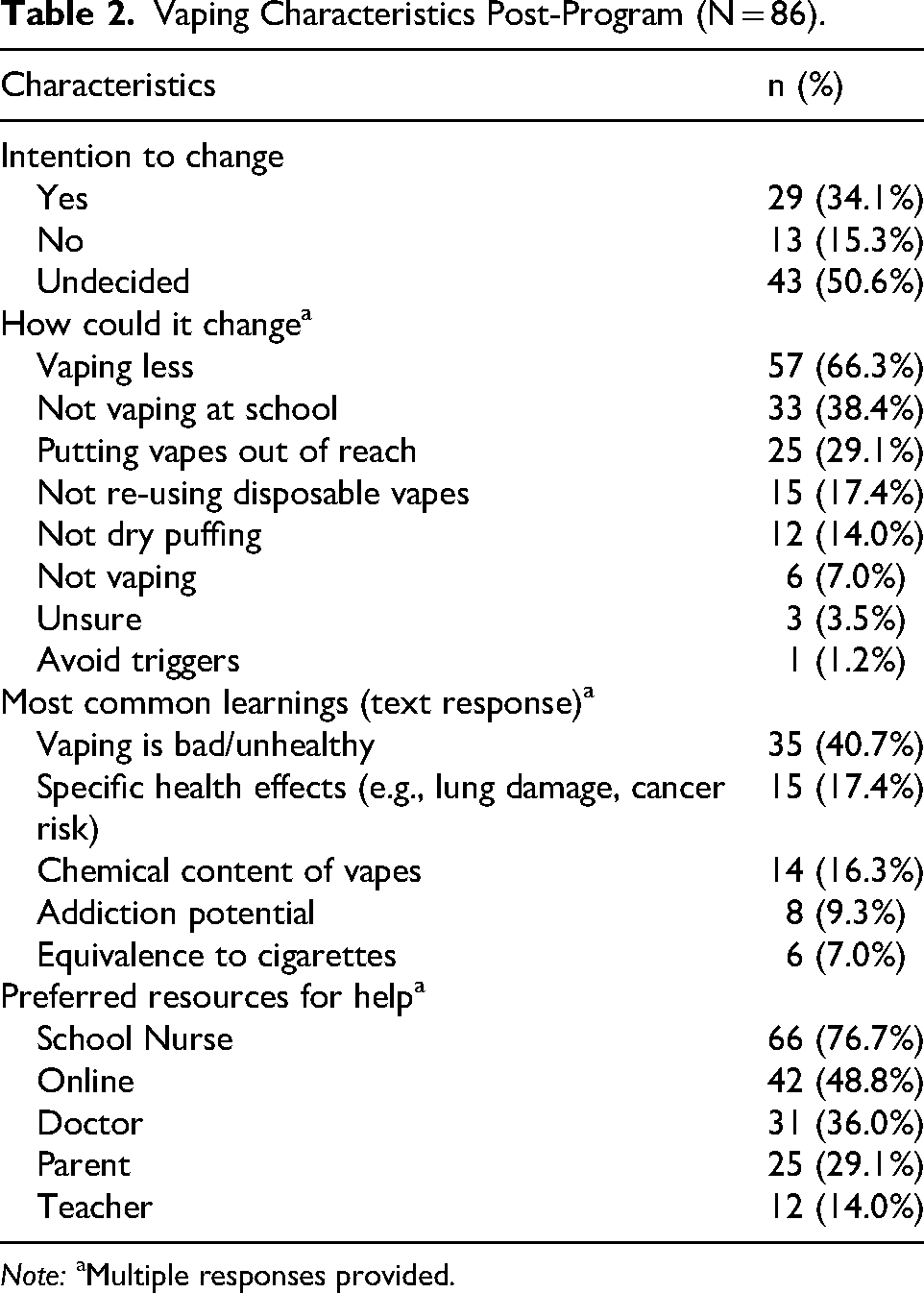
As displayed in Table 2, after the Vaping Small Group Education Program, over one third (n = 29; 34.1%) expressed an intention to change their vaping behavior, while the minority (n = 13; 15.3%) were not considering change, and half (n = 43; 50.6%) were undecided. The most common proposed behavior changes included vaping less (n = 55; 66.3%) and not vaping at school (n = 33; 38.4%). Key learnings from the session were that vaping is harmful (n = 35; 40.7%) and the specific health risks involved (n = 15; 17.4%). The preferred resources for help were the school nurse (n = 66; 76.7%) and online support (n = 42; 48.8%)
Vaping Characteristics Post-Program (N = 86).

Note: aMultiple responses provided.
At the 4-week follow-up survey, over one third of students (n = 36; 41.0%) responded to the survey, as shown in Table 3. Among these respondents, most (n = 31; 86.1%) reported that they had not been suspended since participating in the program. Additionally, most (n = 22; 61.0%) indicated a change in their vaping behavior, with reporting vaping less (n = 15; 41.7%). Furthermore, over two-thirds of the respondents (75%; n = 27) expressed interest in seeking further help, with many (n = 14; 38.9%) indicating they would seek support from the school-based nurse.
Vaping Characteristics 4 Week Follow-Up Survey (N = 36).
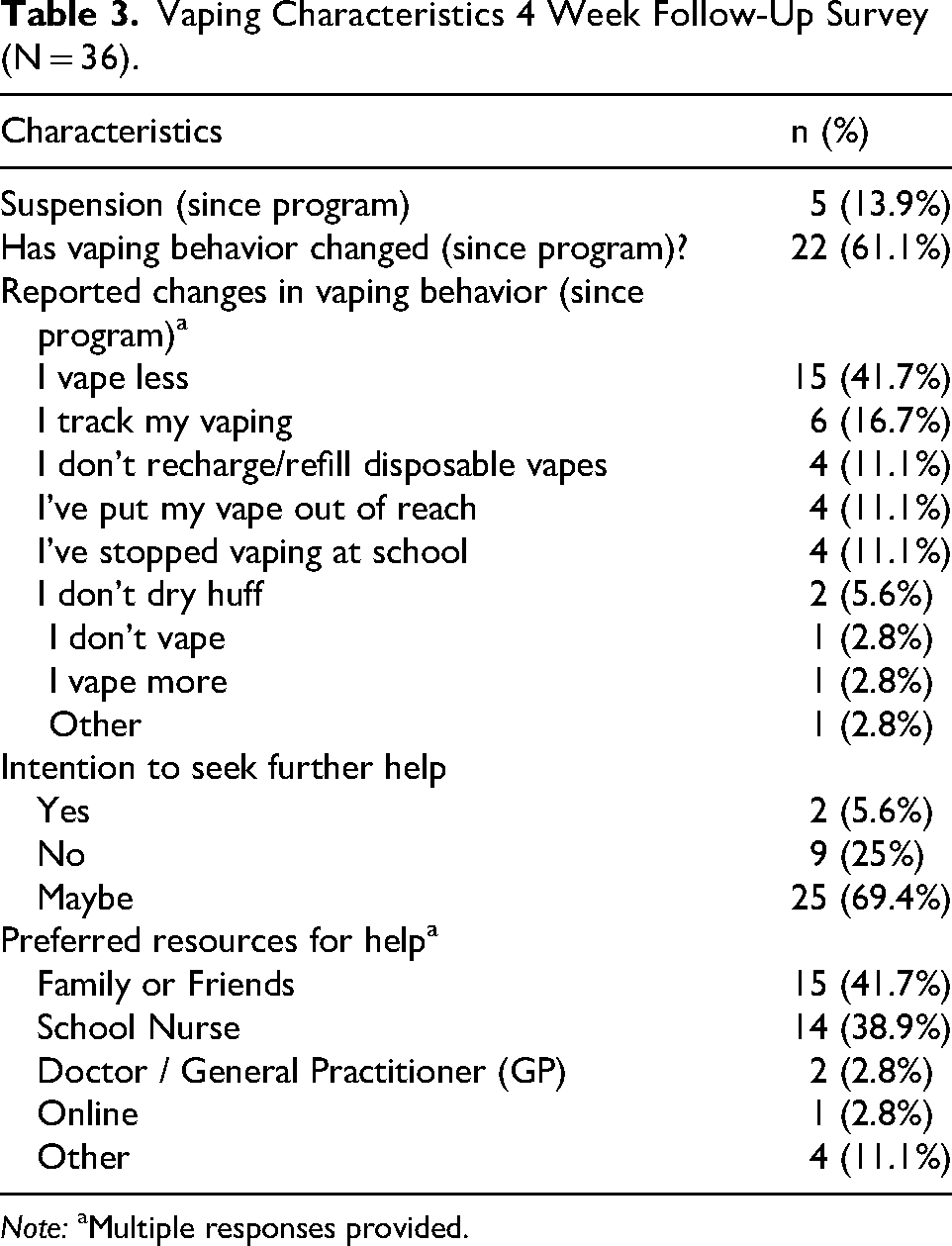
Note: aMultiple responses provided.
School Staff Perceived Value and Barriers to Program
As displayed in Table 4, at 10 weeks post program, all school staff (n = 14; 100.0%) perceived the program was valuable and supported the program continuing. The program's perceived value was attributed to health education provided by health professionals (n = 12; 85.7%), delivery onsite by a known school nurse (n = 11; 78.6%), and increased health literacy (n = 11; 78.6%). Barriers included student absences (n = 9; 64.3%) and time-tabling issues (n = 3; 21.4%).
School Staff Survey (N = 14).
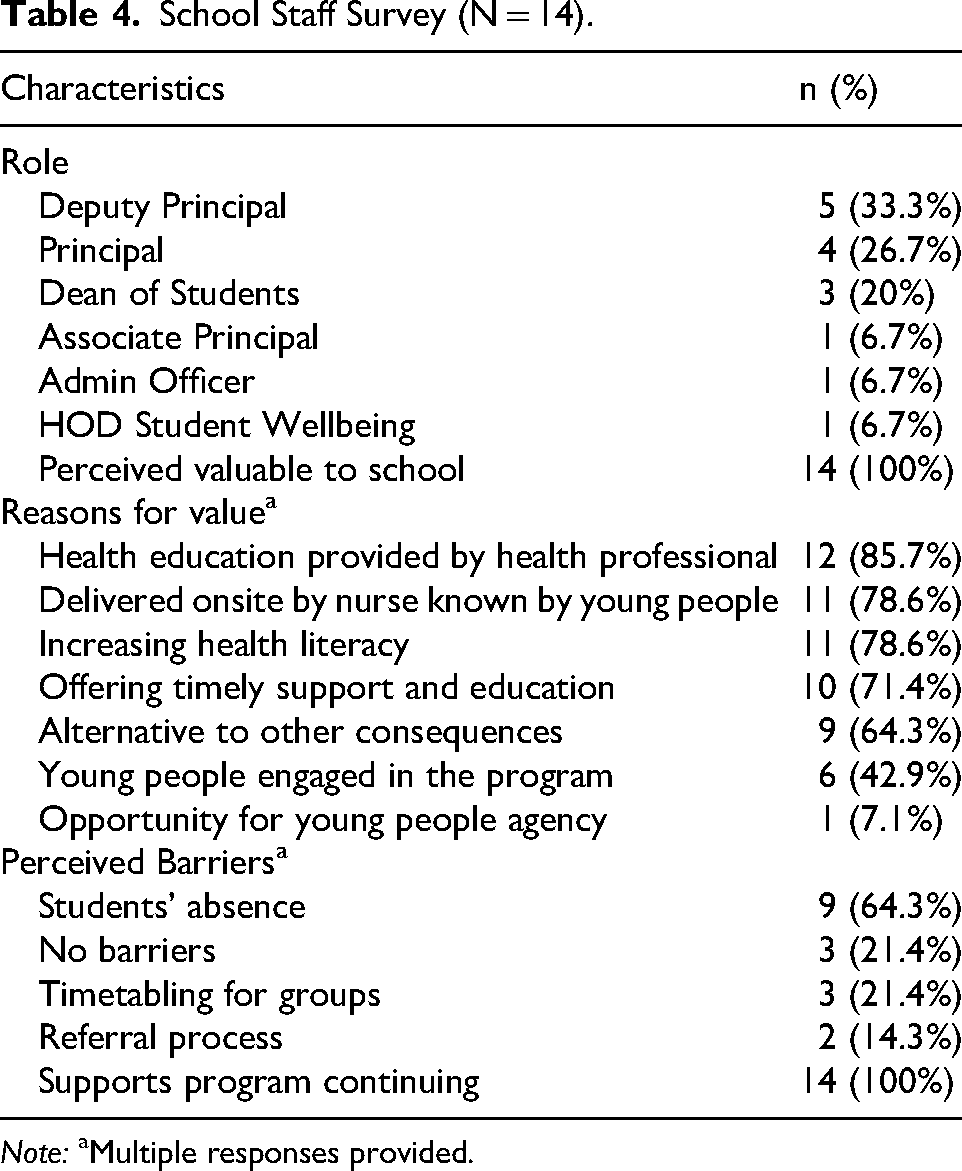
Note: aMultiple responses provided.
School Nurses Perceived Value and Barriers to Program
As displayed in Table 5, at 10 weeks post program all school nurses who responded (n = 10; 100.0%) reported having adequate education and support to implement the vaping intervention program. The majority (n = 8; 80.0%) reported feeling highly confident in advocating to principals, supported by school environments, resources, and program clarity. Student engagement varied, though most were moderately or highly engaged, and lesson plans were unanimously rated as very easy to follow. All respondents saw value in continuing the program, highlighting strengths such as evidence-based content, trusted facilitators, and strong peer dynamics. Reported barriers included limited policy alignment, student stigma or suspicion, and logistical challenges.
School Nurses Survey (N = 10).

Note: aMultiple responses provided.
Discussion
The study aimed to evaluate the short-term impact of a single-session education program delivered in schools by SBYHNs to reduce vaping use for young people. The program successfully achieved its goals by altering young peoples attitudes towards vaping, increasing health literacy among students and enhancing help-seeking behavior. Vitally, the program also successfully built trusted partnerships between young people and school nurses, with the majority of program participants highlighting they would seek further support and health information from school nurses in the future.
Key findings included an improvement in behavioral intentions by the young people, with 34.1% (n = 29) of participants post session self-reporting an intention to change their vaping behavior, with common changes being vaping less and not vaping at school. These results were echoed at a four-week follow-up, with 61% (n = 22_ reported harm minimization behavior changes, and 2.8% (n = 1) had stopped vaping entirely. These self-reported changes in vaping behaviors in young people are promising, especially in comparison to surrounding literature often reporting little to no changes over time, and even an increase in cigarette smoking (Baenziger et al., 2021; Mersha et al., 2023).
The session, designed for small groups and conducted during curriculum hours by the school nurse, was ideal for providing vaping education due to the significant time young people spend at school (Guerine, 2017) and reflects the school's commitment. The results demonstrated the school staff valued the program and supported its continuation and expansion. Student absence on days there was a scheduled groups session posed a recurring challenge. However, more flexible or strategically planned timetabling could help reduce this barrier and enhance overall participation. Positive feedback from young people, staff, and parents reinforced the program's perceived value. These results are similar to those in a recent systematic review that found that peer education improves health knowledge and reduces risky behaviors (Dodd et al., 2022). It differs from prior research as it was a single session only, targeting young people in a school community. Contextually, a recent local Queensland survey demonstrated that over 90% of parents support more e-cigarette education in secondary schools (Queensland Health, 2023). The local results of this quality improvement project, support the wider sentiments of the community expectations.
At the core of the programs curriculum was a focus on a skill-based approach. The study highlights that substance use prevention programs methods in the young person population that incorporate skills training could be more effective than traditional approaches focusing solely on changing perceptions. This aligns with broader literature, with a recent systematic review (Devine et al., 2022) confirming that programs based on social learning principles and interactive teaching strategies were more effective in reducing substance use.
Adhering to best practices in Alcohol and Other Drugs interventions is crucial (Australian Government Department of Health, 2017). Due to the specialized nature of these interventions, it is recommended that they be delivered by trained health professionals to maximize their effectiveness. The program's focus on skills training and interactive sessions delivered by SBYHNs demonstrated positive behavior changes and increased health literacy among young people. The one-time vaping education initiative achieved promising outcomes, with a third of the adolescent participants completing the four-week follow-up survey. This response rate is encouraging, given the typical challenges of maintaining engagement with this age group.
Limitations
As a quality improvement project focused in a single state in Australia, our project lacks some elements of reliability outside of the current context. Additionally, future research could incorporate elements that improve response rates and longevity of follow up (e.g., SMS-based follow up, behavior change at 6 months). In the future more detailed demographic data (e.g., indigeneity, socioeconomic status,) would provide a clearer understanding of how various groups respond to the program, enabling better-tailored interventions. This improved data collection approach would support future research to examine the potential benefit of single-session interventions across variable subgroups. However, this single intervention, pragmatic vaping education program has demonstrated clear positive value for the multiple stakeholders involved in young persons health at school.
Conclusion
Overall, the program demonstrates the value of a skills-based, interactive approach to vaping prevention in schools. The positive outcomes and feedback suggest that such programs, when delivered by SBYHNs, can positively impact students’ attitudes and behaviors towards vaping. Future evaluations should focus on improving response rates, collecting detailed demographic data, and assessing long-term sustainability to enhance the program's overall impact.
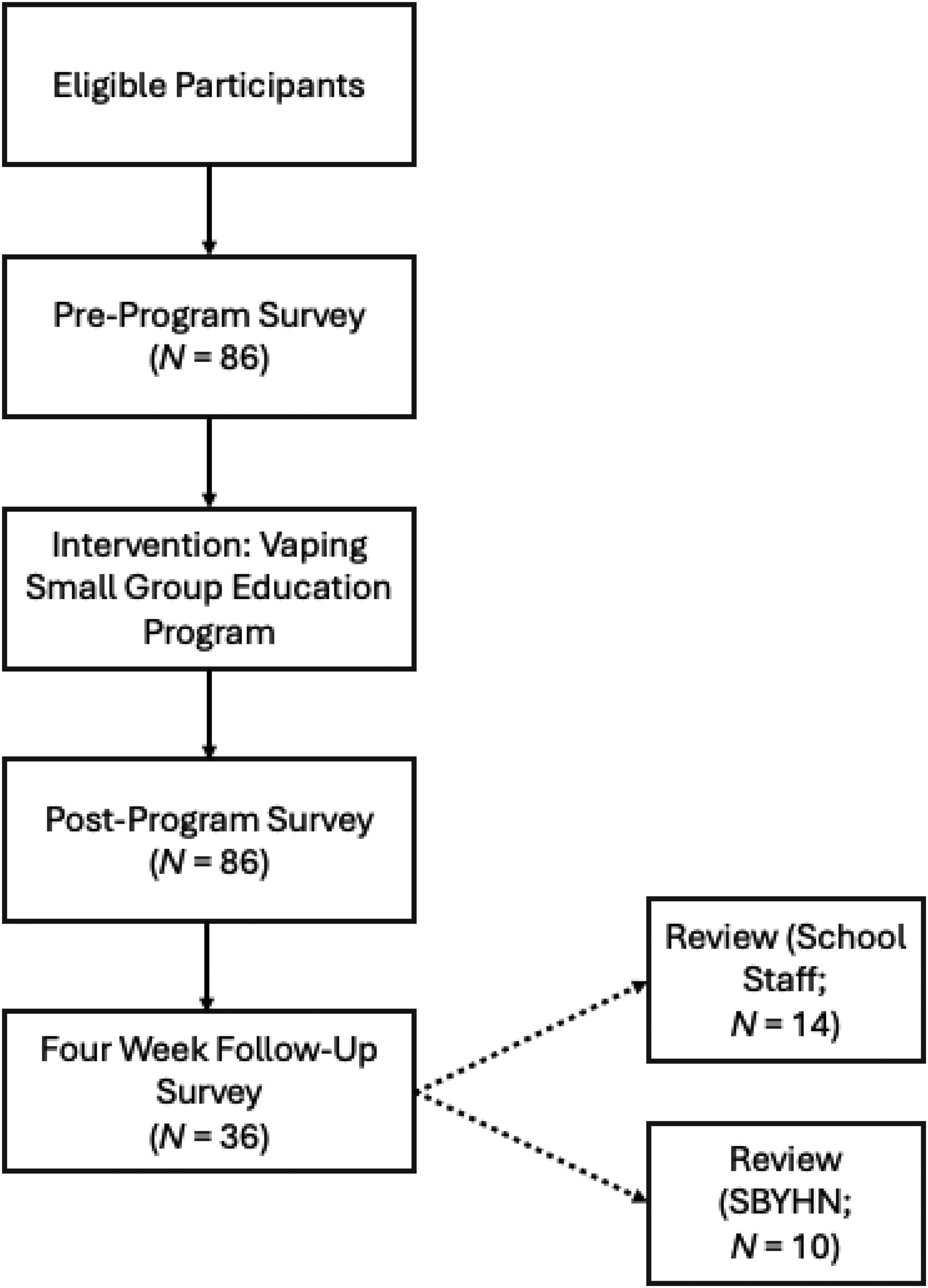
Flow Diagram (N = 86).
Footnotes
Author Contribution(s)
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
