Abstract
Objective
This study investigated the experiences of cleft team speech-language pathologists (SLPs) in relation to continuity of care (CoC). The research aimed to understand the processes used to promote CoC, identify key barriers and facilitators, and examine how cleft team SLPs collaborate with community SLPs and parents.
Design
A qualitative study using semi-structured interviews was conducted with Australian and New Zealand cleft team SLPs. Thematic analysis was used to identify key themes.
Setting
The study focused on SLPs working within specialized multidisciplinary cleft teams in hospital settings across Australia and New Zealand, as well as their interactions with community-based SLPs and parents.
Participants: Ten specialized cleft team SLPs participated in this study. Experience in speech-language pathology ranged from 8 to 47 years (mean = 23.5 years), and their experience in cleft services ranged from 3 to 29 years (mean = 15.4 years).
Results
Six key themes were developed: (1) The Multifaceted Role of the cleft team SLP, (2) Ways We Communicate and Collaborate, (3) Our Relationships, (4) Community SLPs are Central, (5) Families are Key, and (6) The Landscape of Healthcare is Not Working.
Conclusions
This study highlights the importance of relationships in promoting CoC for children with cleft palate. While cleft team SLPs provided education and support, communication was often one-directional. A co-facilitative model, fostering shared decision-making between cleft and community SLPs, could strengthen collaboration. Parents also play a key role as advocates and active participants in therapy. Strategies such as joint sessions, structured mentoring, and intentional follow-up may enhance engagement.
Introduction
The intricate care required for children with cleft palate with or without a cleft lip (CP ± L) spans multiple disciplines, including speech-language pathology, plastic surgery, orthodontics, audiology, and psychology. 1 Speech-language pathologists (SLPs) play a pivotal role from birth to adolescence, addressing the unique challenges related to communication and feeding that arise from a cleft. Their involvement within the multidisciplinary team is essential for effectively managing these issues. 2 Many children benefit from SLP services provided by both specialized cleft team SLPs and a more local community or school-based SLP. 3
In addition to the care provided by both specialized and community SLPs, parents are crucial partners in their child's journey through cleft care and speech development. 4 They may be required to advocate for their child, assist with monitoring their overall progress, conduct therapy at home, and communicate their child's needs to the SLPs and other professionals providing services to their children. This partnership not only enhances the effectiveness of treatment, but may also empower parents to navigate the complexities of cleft speech care. Given the involvement of the different SLPs and the integral role of parents, ensuring effective communication, coordination, and collaboration among all parties is vital. This process is known as continuity of care (CoC).
CoC is an essential aspect of healthcare delivery that emphasizes the seamless, uninterrupted, and comprehensive provision of services throughout a patient's journey. 5 Three types of CoC are outlined in the literature including informational, management, and relational continuity. 6 In the context of cleft speech services, CoC is crucial given the complex and multifaceted nature of treatment required for children with cleft palate. 3 Using this framework of CoC and applying it to cleft speech services, informational continuity entails ensuring accurate and timely sharing of critical information about a child's medical history, therapy goals, and progress across specialized cleft team SLPs, community SLPs, and parents. This dimension is vital to maintaining a unified and consistent approach to care, especially when therapy transitions between providers or settings. Management continuity consists of coordinating care delivery across disciplines and settings to ensure complementary and cohesive interventions. This includes aligning therapy plans, scheduling follow-ups, and integrating input from other healthcare providers. Management continuity is crucial in preventing gaps in care that can arise from fragmented systems. Lastly, relational continuity is about building trust and long-term relationships among SLPs, parents, and other stakeholders involved in a child's care. Relational continuity fosters effective communication and collaboration, ensuring that parents feel supported and engaged in their child's therapy.
There has been limited research investigating CoC between specialized SLPs, community SLPs, and parents. 3 Despite the scarcity of literature on this topic, existing studies consistently highlight breakdowns in CoC processes between specialized cleft team SLPs and community-based SLPs. According to community SLPs, discrepancies exist between their expectations and current practices, which impacted how they effectively collaborated with specialized cleft team SLPs. 7 For example, community SLPs reported confusion regarding roles, limited support, and insufficient information-sharing, all of which negatively impacted collaborative efforts. Community SLPs also identified the need for improved collaboration with cleft team SLPs as well as assistance with the child's treatment plan. 8
Despite the pivotal role of cleft team SLPs, their perspectives and experiences on the facilitators, barriers, and nuances to CoC remain underexplored. Understanding these factors and the challenges faced by cleft team SLPs in relation to CoC including differences in expectations and resource availability, can provide valuable insights into improving service delivery. Additionally, exploring the facilitators that promote effective CoC can help identify best practices and strategies that enhance collaboration among all stakeholders, including parents and other healthcare professionals. By investigating these aspects, targeted interventions that address existing barriers and leverage strengths within the system may be developed. Ultimately, a more comprehensive understanding of the experiences and perspectives of cleft team SLPs is essential for fostering an integrated approach to cleft care that ensures consistent, high-quality support for children and their families throughout their journey.
This qualitative research aimed to explore the experiences and insights of cleft team SLPs regarding CoC for individuals with CP ± L. By capturing their perspectives, challenges, and strategies, the study seeks to address critical gaps in understanding the complexities of delivering comprehensive care in this context. It also seeks to identify barriers and facilitators to inform the development of effective solutions and best practices to enhance CoC. The research questions were as follows:
What does communication and collaboration currently look like between cleft team SLPs, community SLPs, and parents? What processes are currently being used by cleft team SLPs to ensure CoC with community SLPs, and parents? What are the barriers impacting CoC? What are the facilitators for promoting CoC?
Methods
Procedure
The study was approved by the Human Research Ethics Committee of The University of Sydney (2023/105). An invitation to participate in the study was sent via email to a special interest group comprised of Australian and New Zealand (ANZ) SLPs who were part of a cleft palate team at a tertiary facility. Informed consent was obtained before the interviews commenced and a demographic survey was completed. The interviews were conducted by the first author. Interview topics and questions were discussed across all three researchers and the interviewer had piloted the interview with the third author prior to conducting the interviews with the participants. An interview guide was created and used (see Appendix A). Throughout the interview sessions, open-ended questions were posed to explore the SLPs’ experiences, challenges, and perspectives related to CoC within cleft teams.
Participants
The study recruited SLPs based in Australia and New Zealand, who had been actively working on a cleft team for a minimum of 12 months. Purposive sampling was utilized to recruit participants who could provide insights into CoC in the context of working with children with cleft palate.
Data Collection and Analysis
Semi-structured interviews were conducted with the selected SLPs. The interviews were held via Zoom to accommodate the geographical dispersion of participants across Australia and New Zealand. The Zoom recording and transcription features were employed to capture the discussions comprehensively. Contemporaneous field notes were taken to record notable non-verbal communication. The interviews ranged between 29 and 70 min with an average duration of 44 min. The sample size for this study was determined based on the number of participants who were available and able to be recruited within the study's timeframe and criteria, out of approximately 40 eligible SLPs who worked on a multidisciplinary cleft team.
A reflexive thematic analysis approach following Braun and Clarke's (2022) methodology was used to analyze the de-identified, transcribed interviews. This systematic analysis process involved the three authors reading and re-reading the transcripts to become familiar with the data. Once this was complete, all three authors generated initial codes utilizing the qualitative analysis software, NVIVO. Once this was completed, the codes were organized into themes that captured important aspects of the data. Step four consisted of all authors reviewing the themes to ensure they accurately represented the data. The fifth step involved defining and refining the themes. Lastly, step six involved writing up the themes and their significance in relation to the research question.
Trustworthiness
Several strategies were employed to ensure the trustworthiness of this research. Member checking was conducted by offering participants the opportunity to review their interview transcripts. Of the 10 participants, 5 requested to review their transcripts, and 0 participants provided comments. Consequently, no changes were made during this process.
Researcher triangulation was used to strengthen the credibility and reliability of the data analysis. The research team were all SLPs but had diverse professional backgrounds, which reduced potential bias in coding and provided an enriched interpretation of the findings. The first author, who also conducted the interviews, is a mid-career SLP currently completing a PhD with experience working within a cleft team and in private practice. The first author had a prior professional relationship with all participants due to their joint involvement in the ANZ cleft group. This relationship was managed with reflective journaling to minimize bias. The second author was not a member of a cleft team, providing an external perspective to the analysis. This author is a senior clinical researcher with expertise in speech disorders across the lifespan and experience in both qualitative and quantitative research methodologies. The third author is also a senior researcher with experience conducting cleft-related speech-language pathology research and was previously a member of different cleft teams, adding further depth and cleft-specific insights to the analysis.
Results
Participants
Ten specialized cleft team SLPs participated in this study. Their years of experience as SLPs ranged from 8 to 47 years, with a mean of 23.5 years. The participants had worked in providing specialized speech-language pathology in the area of cleft palate for 3 to 29 years, with a mean of 15.4 years. In terms of education, the participants’ highest qualifications included seven with a specialist Bachelor's degree (which is professional entry in Australia and New Zealand), and three with higher degrees. Nine of the ten participants reported receiving instruction on how to work with patients with cleft during their university training, and three of ten had engaged in additional specialized training related to cleft care after graduation. All ten participants had prior and/or current experience working outside of a cleft team, including roles in hospital private practice, community health, and school settings.
Themes
Thematic analysis of the interviews generated 6 themes: (1) The Multifaceted Role of the Cleft Team SLP in CoC, (2) Ways We Communicate and Collaborate, (3) Our Relationships, (4) Community SLPs are Central, (5) Parents are Key, and (6) The Landscape of Healthcare is Not Working. These global themes were comprised of 17 subthemes. A summary of themes and subthemes can be seen in Figure 1.
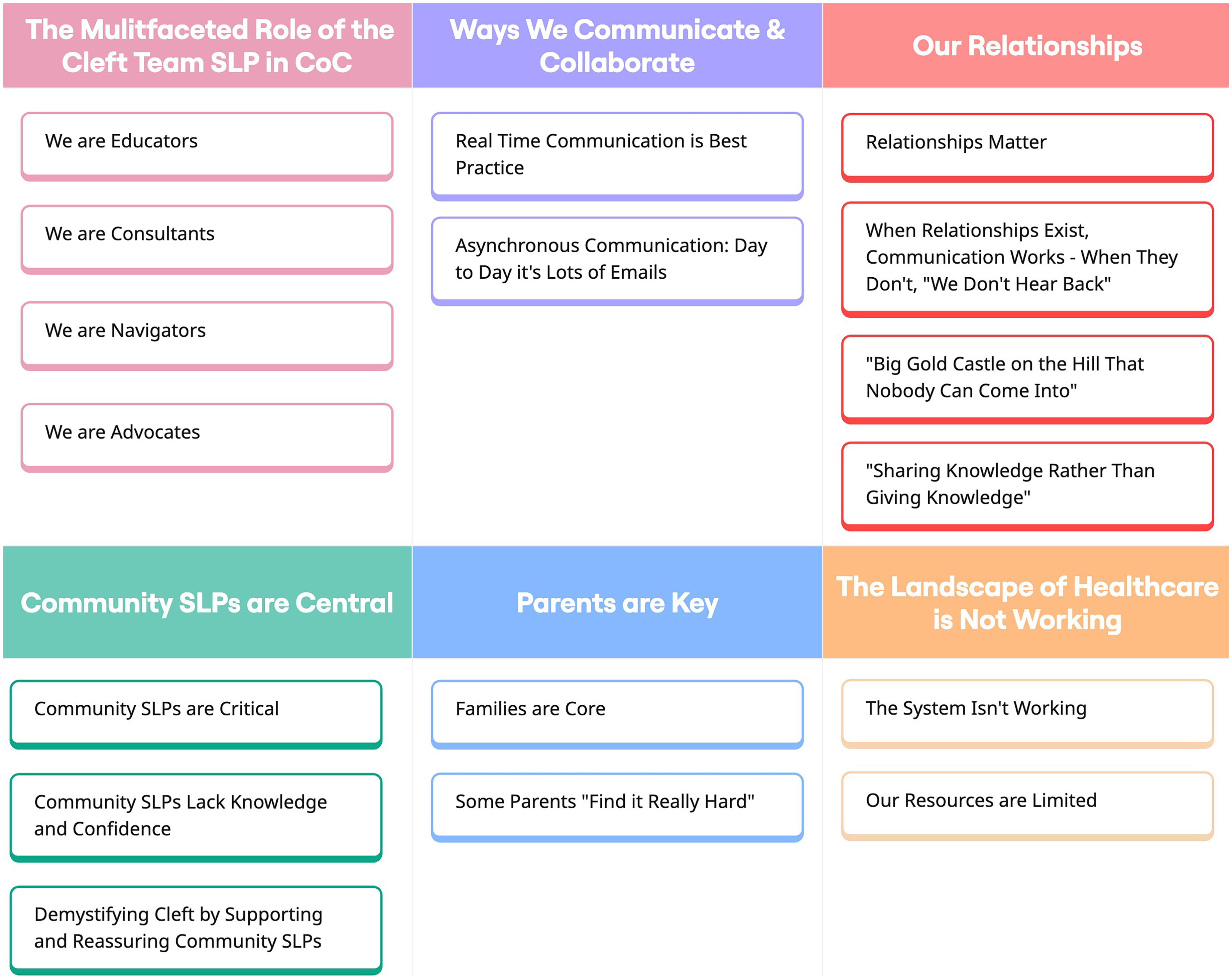
A summary of themes and subthemes.
Global Theme One: The Multifaceted Role of the Cleft Team SLP in CoC
This global theme captures the diverse and interconnected roles that cleft team SLPs undertake to facilitate CoC for children with cleft palate. Beyond direct clinical intervention, SLPs reported they have many critical roles including functioning as educators, consultants, navigators, and advocates, working collaboratively with families, community SLPs, and multidisciplinary teams.
We are Educators
SLPs believed they play a critical role as educators with parents and community SLPs. This educational responsibility was seen as central to their work and included providing professional development (PD) to community SLPs through workshops, lectures, and ongoing support. They explained that this education was aimed at enhancing the capacity of community clinicians to manage children with cleft-related speech difficulties. As P4 shared, “We also do some teaching with … the non-cleft therapists in the community.” Educational resources, such as publications on therapy techniques, were also provided as P10 stated, “I don’t just talk to them… but I will send them the publication on the therapy techniques.” Their reported aim was to provide clinicians with the knowledge and support needed to manage cleft-related speech issues, explaining that introducing cleft speech principles can make others feel more comfortable reaching out for further advice, “Letting them know who we are and giving them a bit of an introduction to cleft speech and therapy principles can make them feel comfortable contacting us” (P6).
SLPs also described their role as educators for parents, working to build their understanding of their child's condition, development, and the journey ahead. They explained that education begins early in many services, starting at birth and continuing as the child develops. P1 shared, “We have it (parent education) at birth, we have parent education at 6 months, and then we have ongoing contact.” Simplifying complex information for parents was also identified with P5 explaining, “You educate them a little bit phonetically and about how speech sounds are made, and then you take them into how do your kids make speech sounds.” Respondents also provided structured educational opportunities for parents, such as workshops. P5 shared, “I’m just starting to run some parent workshops.”
We are Consultants
SLPs described their role as primarily consultative, operating both as external consultants, who provide guidance and mentorship to community SLPs and parents, and internal consultants, who play a key role in decision-making within the multidisciplinary cleft team.
External Consultants
As external consultants, SLPs offered specialized expertise to support community clinicians in delivering therapy, rather than acting as the primary treating clinician. P9 explained, “I feel like a lot of other people… view that we’re the main clinician in the child's care when really… our service here is very consultative, and we don’t have that much capacity to see children regularly or ongoing.” This consultative role was closely tied to processes that aimed to ensure COC, as cleft team SLPs provided guidance to help local therapists manage cleft-related speech issues effectively. They also reported they often acted as mentors or informal supervisors, sharing their expertise to try to build the confidence and skills of local clinicians. As P8 described, their role was “almost like a bit of a mentor coach, (an) informal supervision arrangement.” Another SLP highlighted the importance of their advisory role, saying, “My role has largely been an advisory role, so I advise speech therapists out in the field” (P5). This process included offering tailored advice on therapy strategies, troubleshooting challenges, and sharing specialized knowledge that might not otherwise be available in the local setting. “I think it's really having that maybe extra level of knowledge and experience to have a bit more of a consultative role and to help guide community therapists and parents,” P9 explained.
Internal Consultants
Internally, SLPs perceived themselves as integral to hospital-based discussions regarding intervention planning, particularly in guiding surgical decision-making within the multidisciplinary cleft care team at the hospital. They explained that their involvement is key in determining appropriate interventions at different stages of care. As P9 stated, “I think that's a big part of our role… helping with decision making around intervention at different time points.” They saw their role as particularly significant in guiding decisions related to surgical interventions. P9 highlighted this role by explaining, “I find, in our hospital anyway, they (surgeons) are relying hugely on us to guide them around decision making for surgical intervention for secondary speech surgery.”
We are Navigators
SLPs described themselves as navigators, guiding families, and coordinating care, and ensuring COC between families, community SLPs, and other professionals involved in the cleft care journey. Communication with parents was a key aspect of this navigational role, with SLPs describing they often served as the primary point of contact for families for the multidisciplinary team. P3 explained, “We find we speak to a lot of that coordination. And part of that is because of that relationship we have. Parents speak to us, and they open up about other things.” This relationship facilitated a sense of trust and support, enabling cleft team SLPs to act as liaisons between families and the wider care team. The respondents mentioned they also assist in navigating complex systems such as the (Australian) National Disability Insurance Scheme (NDIS). As P7 explained, “A lot of that has been NDIS… Helping manage with NDIS and helping them navigate these kinds of really tricky pathways.”
We are Advocates
Many SLPs saw advocacy as integral to their role, ensuring that children with cleft palate receive the care and support they need, even in complex situations. This advocacy often required effective communication and collaboration with and between families, community SLPs, and multidisciplinary teams, aligning with processes that promote CoC. P9 highlighted this role, stating, “I think that's a big part of our role… advocacy, and helping to steer or making helping with decision making around intervention at different time points.” This advocacy included working closely with families to ensure their voices were heard and that the child's best interests were prioritized. P6 highlighted, “Are they getting the right kind of therapy or not, and then trying to, in a politically correct way, help the parents advocate for… improving the focus of therapy.” SLPs also found themselves in a position where they needed to advocate for children whose families may not be fully engaged in their care. P6 explained, “If families are not engaged… but the child does need help, then looking at how can we advocate for that child.” In these situations, SLPs reported seeking alternative ways to support the child, such as through school-based therapies or through other agencies.
In addition to working with families, SLPs also reported advocating for children within multidisciplinary teams. They saw themselves as pivotal in raising concerns and communicating with the team and family, particularly when coordinating care across different providers. As P3 stated, “I think we are pivotal in raising concerns to the whole team, first of all to our whole team, and to the family too if they then have other providers.” This advocacy aimed to ensure that all aspects of the child's care, from speech to hearing and beyond, are addressed in a coordinated way. “I think we kind of reach across (the team) a little bit…with the hearing and everything else and try and keep everything in place to advocate for these kids” (P7).
Global Theme Two: Ways we Communicate and Collaborate
Respondents used a variety of communication methods to collaborate with community SLPs and parents, ensuring CoC. These methods included both real-time communication, such as phone and video calls, and asynchronous communication, such as emails and written reports.
Real-Time Communication is “Best Practice”
Real-time communication, including phone calls, video calls, and face-to-face meetings, was valued for its immediacy and ability to foster collaborative discussions. SLPs used phone and video calls to discuss assessment findings, treatment plans, and shared goals. P5 explained, “I either do phone call or a zoom call or they come in and see me with the patient.” These direct interactions allowed for immediate clarification, problem-solving, and relationship-building. For more complex cleft-related speech issues, real-time collaboration was seen as particularly beneficial. SLPs reported facilitating joint sessions where community SLPs attended therapy or assessment appointments, either in person or remotely. P8 highlighted the importance of this approach: “Having them joining in via Teams for a joint session… that's… best practice for some of that complex cleft speech… errors.” However, coordinating schedules for real-time communication could be challenging. SLPs acknowledged that time constraints and conflicting commitments sometimes made it difficult to arrange phone calls or joint sessions, particularly when community SLPs had busy caseloads or worked in different time zones.
Asynchronous Communication: “Day-to-Day It's Lots of Emails”
Due to scheduling difficulties, emails and written reports were often the default mode of communication between cleft and community SLPs. These asynchronous methods provided flexibility and ensured that all clinicians had access to the same clinical information. P8 acknowledged this reality: “All that other stuff I’ve talked about takes time and it takes everyone's diaries lining up. To be honest, it probably looks day-to-day like lots of emails.”
SLPs highlighted the importance of sharing written reports with community clinicians to ensure that therapy recommendations were clear and accessible. P2 explained, “If it's a child that we’re reviewing as part of routine… processes, I would always be sending a copy of my correspondence or report… sent to the family and cc’ing the community speech pathologist.” Recognizing that written reports alone might be insufficient for complex cases, cleft team SLPs sometimes reported taking a proactive approach to follow-up communication. P2 described their method, saying, “If there's additional complexity and I really would like to discuss that, I’ll usually follow that (the report) up with a phone call or an email to that child's (community) speech pathologist.” This ensured that any areas of uncertainty or concern could be addressed collaboratively.
To further facilitate communication, many SLPs provided direct contact details to parents and encouraged local SLPs to reach out when needed. P2 shared, “I’ll often say to parents, here's my card. If your speech pathologist has any questions, please, please get them to give me a call or email me.”
Global Theme Three: Our Relationships
Relationships Matter
In their work with children with cleft palate, SLPs consistently emphasized the importance of fostering strong, respectful relationships. They worked to create a “non-threatening” environment, where they could share knowledge without appearing to assert authority. P2 explained, “Usually once you’ve broken those walls down and you’re non-threatening in sharing of your knowledge, people (community SLPs) are usually really happy to collaborate.” SLPs explained that relationships with community SLPs and families should be built on trust and mutual respect, where all parties felt free to discuss successes as well as difficulties. P8 noted, “I need to make a connection with this family before they take on anything I say.” Once these relationships were established, respondents said that openness and honesty flourished. P2 shared, “And once you build that relationship, people are quite happy to be… fairly candid… So, it's just about building the relationship where you feel comfortable to make mistakes together and to learn together.” This sense of mutual learning and support helped to create a collaborative environment where both SLPs and families could work towards the child's progress without fear of judgment.
When Relationships Exist, Collaboration Works – When They Don’t, “We Don’t Hear Back”
SLPs recognized that effective communication with community SLPs was essential for CoC, and when strong relationships existed, communication tended to be two-way and collaborative. Many described positive experiences where community SLPs reached out regularly to discuss cases, ask questions, and share progress. These successful exchanges often occurred with community SLPs who managed a higher volume of cleft cases and felt more comfortable contacting specialists: “They probably have contacted a few times and know that it's not so scary once they do.” When these relationships were in place, the communication was two-way, collaborative, and helped ensure everyone—including the family—was on the same page.
However, when relationships were not well established, SLPs frequently reported communication breakdown. Many expressed frustrations at the lack of follow-up, despite their efforts to provide handovers and support. P4 noted, “We very rarely hear back from them, which is a big frustration. So it tends to be one way.” This issue was particularly evident with private therapists, as opposed to those who worked in public health, who might be constrained by time pressures or the demands of a fee-for-service model. P7 explained, “I think I’m less likely to hear back from private (therapists). I don't know the reason. P3 described their efforts, stating, “For them to actually share back is hard and I’m working hard at that… By communicating outwards, I’m hoping I get inwards.”
“Big Gold Castle on the Hill That Nobody Can Come Into”
A barrier to CoC identified by cleft-team SLPs was the perception that specialized cleft services were often viewed as being in a “big gold castle on the hill” (P8). This perception represented a divide between cleft team SLPs and community SLPs, which appeared to impact effective collaboration. P8 captured this sentiment, explaining, “There's this perception that (hospital) is this big gold castle on the hill that nobody can come into, that's not approachable. And I think if you do call us, we’re gonna tell you you’re doing a bad job or you’re not skilled enough to be doing the job.” The SLPs perception was that this belief discouraged community SLPs from reaching out for support, creating a barrier that made it difficult to ensure consistent and collaborative care for children with cleft palate.
SLPs recognized that this traditional medical model where specialists are seen as the sole experts, was not conducive to building strong, collaborative relationships. P3 rejected this approach, stating, “We take this medical model of ‘we're an expert, come to me and I shall lay hands.’ No, we can't do that anymore for so many reasons..”
The perception of a hierarchical dynamic also impacted families, who respondents thought sometimes saw hospital-based cleft teams as superior to their local therapists. P2 explained, “I think it's really important that families understand and respect what their local speech pathologist is giving… there can be that ‘Oh, they’re the experts at the hospital and they know better, and my speechie is just implementing.’” This mindset appeared to undermine the crucial role and skillset of community SLPs in delivering therapy and supporting families.
“Sharing Knowledge Rather Than Giving Knowledge”
SLPs advocated for a collaborative approach to knowledge exchange, emphasizing the importance of “sharing knowledge rather than giving knowledge” (P8). This perspective highlighted the idea that knowledge transfer should be two-way and highlights that community SLPs and parents also bring valuable knowledge to the team. They consistently mentioned avoiding presenting themselves as the “experts” who held all the answers and instead emphasized a “partnership.” P2 emphasized this, “that sort of concept that the hospital is the experts and actually letting the families know we're very much a partnership, in partnership with their local clinician.”
Global Theme Three: Community SLPs are Central
Community SLPs are Critical
Community SLPs were also recognized as pivotal in ensuring CoC for children with cleft palate. Respondents said they saw community SLPs as integral members of the care team, often having more consistent and long-term interactions with the child and their family. P9 explained, “I think they’re (community clinicians) probably one of the two most important people in their cleft team along with their parents… because they’re going to have that degree of frequency that the tertiary cleft team are not going to have.” SLPs acknowledged that community therapists provided essential support between specialized cleft team visits, often managing the bulk of day-to-day therapy. P4 elaborated, “I think that they, in the end, are more important than us. If they get it together with the child and with the parent, they’re a very significant person in that child's life, trying to improve their speech.” P7 stated, “Decisions are made on that child's progress in therapy,” highlighting how community SLPs’ observations and feedback informed the overall care plan and surgical decisions.
Community SLPs were seen as essential for maintaining CoC through regular therapy and following through with recommendations from cleft team SLPs. P8 described the process, saying, “We’ll see kids for therapy for diagnostic purposes to see what's their capacity like, stimulability-wise… Often that then involves going back to a local therapist to have that repetition and that practice and then coming back to us.” This collaborative approach ensured that children received consistent therapy and that their progress was monitored and supported across different settings.
Community SLPs Lack Knowledge and Confidence
SLPs highlighted a barrier to CoC: the perception of limited knowledge and experience in some community SLPs in managing cleft-related speech issues. While acknowledging that some community therapists were highly skilled, participants noted that these clinicians were “few and far between.” P3 reflected on this disparity, explaining, “We have some very talented long-term cleft specialists in the community, but as I said, they are few and far between.” This inconsistency in expertise created challenges for ensuring consistent and effective care for children with cleft palate.
Respondents went onto describe they perceived many community SLPs as not feeling confident addressing cleft-related issues, even when they had the necessary skills. P7 remarked, “They do have the therapy, they do have the knowledge. They’re not quite sure where to start or what to do, but they actually do know what they're doing.” SLPs also observed that while some community therapists were open to collaboration, more experienced clinicians sometimes hesitated to seek support. P3 explained, “The more experienced the therapist is, the less likely they are to actually want to go, ‘Hey, I’m doing this, it's not really working,’” This reported reluctance to ask for guidance or engage in collaborative problem-solving may pose as a barrier to effective communication and collaboration.
Despite their importance, respondents recognized they perceived that community SLPs sometimes felt disconnected from the broader cleft team. P10 reflected, “I don’t think they feel as though they’re part of the team. But they are critical to the team.” This perceived disconnect was identified as a barrier to CoC, and cleft team SLPs stressed the need to actively include and support community therapists in the care process. Facilitating communication through regular contact, joint sessions, and sharing resources were seen as ways to bridge this gap and reinforce their role as key team members. P6 explained, “We’re all a part of that team. I don’t see anyone as being any more important… the plastic surgeon is as important in that team as the community speechie.”
Demystifying Cleft by Supporting and Reassuring Community SLPs
SLPs saw an essential part of their role as breaking down the complexities of cleft speech therapy to make it more accessible to community speech therapists. They recognized that the unique challenges of cleft speech could feel daunting to clinicians without specialized training. P5 explained, “Unless you work in the field, you don't understand quite the quantity and complexity of the speech that we have to work with.” To address this, SLPs focused on “demystifying” (P8) cleft care, as they shared strategies and insights that made cleft-related speech goals achievable for community therapists.
For cleft team SLPs, empowering community clinicians was about building confidence and breaking down perceived barriers. P9 reflected on her own early experiences, recalling the uncertainty she once felt: “I remember feeling like that myself thinking, I have no idea… but I think when you can break it down… it makes it a lot easier for them.” By guiding therapists through specific cleft techniques and reinforcing that these were extensions of skills they already had, SLPs helped to reinforce the idea that cleft therapy was not “rocket science” (P2). P7 shared that their goal was “just going through it and showing them what they do know, and how you've done this a hundred times but we're just targeting this instead.” They acknowledged that this capacity-building was essential to providing consistent cleft care in the community. As P3 stated, “While I'm not going to say anyone can do it, I think with our support we need anyone to do it, because that's our capacity building.”
Global Theme Five: Parents are Key
Families are Core
SLPs emphasized the core role parents had in the care and management of children with cleft palate, describing them as integral to every step of the care process including holding critical information, facilitating interventions, and driving decision-making. P6 illustrated this by describing a conceptual framework: “The picture that I always use is like a circular picture. We have the child and their family in the middle of a wheel and the whole team around them.” P2 echoed this sentiment, stating, “I would like to think of the team as the child and the family are the core people at the centre and the heart of what we do.” Parents were described as the ongoing holders of information, maintaining continuity across years of therapy, surgical procedures, and interactions with various specialists. P1 noted, “They’re like the ongoing person that is holding all the information… they’ve been there since the beginning….” This continuity was seen as essential, particularly in cases where children were not yet able to take on that responsibility themselves. Parents were viewed as the primary point of connection, bridging gaps between the child, the multidisciplinary team, and community services.
Empowering parents and supporting their involvement were described as essential processes for promoting CoC and overcoming barriers. P3 stated, “Ideally, I would want parents to be liaising with us and being a true partner in that care. And knowing that the door is always open.” Respondents emphasized the importance of facilitating parents’ understanding and engagement, ensuring they had the tools and confidence to act as advocates and collaborators. P7 summarized, “I think the parents are just absolutely key in every step that happens. And we just need to help ensure they’ve got the support and the understanding to… come into those situations and those decisions with what they need.”
SLPs also emphasized the pivotal role of parents as both decision-makers and therapists in their child's care. SLPs viewed parents as integral to the success of speech therapy itself, emphasizing the importance of their active involvement in home practice and the generalization of therapy outcomes to daily life. P3 explained, “Parents are ultimately their child's therapist. We are merely the people with the expertise to go, try this.”
Some Parents “Find it Really Hard”
Collaboration reportedly broke down when families struggled to process the complexity of cleft care. Some parents arrived at appointments without fully understanding their purpose or the role of the cleft team SLP. P8 explained, “You've got families that kind of come in, don't really know why they're there. Don't really know what your job is.” This lack of understanding apparently led to misinterpretations, with parents finding it difficult understand the complexities. P8 shared, “They find it really hard to process that… pulling apart speech versus VPD versus language versus hearing versus all of that,” which often required SLPs to provide repeated explanations and additional guidance: “You feel like you're constantly having to over explain what you're doing and why” (P8). For these families, SLPs acknowledged the importance of breaking down information clearly and supporting parents in managing the many elements of cleft care.
SLPs noted that parents often relied heavily on clinicians for guidance, with some deferring decisions to the “experts.” P9 reflected on this dynamic, sharing, “mum has said on every single occasion… ‘You’re the experts, whatever you say.’ And you know, really, I kind of want to say, well, actually, you know your child the best… you need to feel like you’re making a decision in this, too”. This sentiment underscored the need for cleft team SLPs to empower parents to feel as though they are an integral team member.
The burden of care also played a significant role in the quality of communication and collaboration. For parents juggling work, after-school care, and other responsibilities, engaging in therapy and supporting home practice was challenging. P3 empathized with these families, stating, “They get home, the kids in after school care, they meet their kids at 6 o'clock at night, when are they meant to do therapy?” P5 acknowledged this tension, stating, “Parents have got limitations in that they have other kids at home. They have other roles to play, and sometimes being the therapist as well as a parent can be really… detrimental on their relationship.” SLPs acknowledged that not all families were able to take on an advocacy role due to various barriers. Some parents lacked the confidence, time, or knowledge to advocate effectively. P6 noted, “Not all families are going to be able to advocate for their child and, you know, have that level of interest or time to spend.”
Global Theme Six: The Landscape of Healthcare is Not Working
SLPs described a healthcare system across Australia and New Zealand that was often disjointed, inconsistent, and difficult to navigate. A combination of structural issues, funding models, and workforce limitations contributed to gaps in service delivery, leading to fragmented care and limited collaboration.
The System Isn’t Working
Respondents identified significant barriers to CoC due to issues within the current healthcare and funding models, particularly with the NDIS in Australia. Many SLPs noted that the NDIS model, while beneficial in increasing access to services, often appeared to lead to fragmented care and reduced parental involvement. P8 explained, “I know that NDIS has changed things for the better, but it's also made it really challenging for some of these families. They just go and see somebody, the first person they can get into, not necessarily the person that's got the best skill set for them.” This lack of specialist care in community settings was reported to create gaps in service quality and effectiveness.
The structure of NDIS funding was also seen as undermining the perceived value of therapy. SLPs reported that they perceived when families did not have to pay directly for therapy, their engagement decreased. P10 observed, “The parents who pay for something, value it.” This diminished sense of ownership led to challenges in achieving therapeutic outcomes. P2 added, “Parents often aren't present for the therapy… they’ll come into (the cleft) review and say, ‘Oh, are you still seeing that lady? What are you working on with her? (to their child)’” This lack of involvement appeared to hinder collaboration.
SLPs found that public health SLPs were generally easier to collaborate with compared to private therapists. P10 noted, “The community health therapists are easy to deal with… they are committed to helping.” This perceived commitment appeared to translate into more effective collaboration. In contrast, private therapists were perceived as harder to contact, because their time was billable, which discouraged collaboration. As P3 explained, “Private therapists are possibly some of the hardest to contact because parents are paying from their own pocket.” This financial structure sometimes created barriers to collaboration, as private therapists faced competing demands on their time and resources, possibly making it more challenging to engage in open and frequent communication.
Our Resources are Limited
SLPs identified numerous systemic challenges within the current healthcare landscape that hindered CoC for children with cleft palate. One major barrier was geographical distance, which limited access to specialist services. As P5 noted, “Because we’re spread out, we don’t have a lot of (children) who can travel to us for speech therapy.” The vast geographical areas meant that many children worked with local therapists for intervention. Another participant highlighted the difficulty, stating, “In the country region they have to go to the country therapists for intervention because… (the state) is huge” (P1).
Staffing shortages and limited resources further compounded these challenges. P1 explained, “if we were to be implementing gold standard evidence-based practice, we would need a lot more staff. I think at this stage we rely on our community services to provide that.” The lack of capacity to deliver ideal services, such as language programs for toddlers, was a significant barrier. Another participant expressed frustration at these limitations, saying, “There's not enough hours in the day… issues with staffing, (P5)” while another described their service as being “pulled in lots of different directions” (P9). These constraints made it difficult for SLPs to engage in hands-on therapy, collaboration, and follow-up care as frequently as needed. P10 explained, “With the two days a week we have, we can’t do enough therapy, and that impacts our ability to provide ongoing support and advice.”
The challenge of coordinating care across different organizations was another obstacle. As P1 pointed out, “You can’t co-provide (air quotes) from two health organisations at the same time.” This organizational divide made it difficult to provide joint therapy or mentorship to community SLPs. Furthermore, the logistics of arranging time for communication were problematic, with P2 stating, “The biggest challenge to all of this obviously is time and finding mutual time.” These barriers may disrupt the flow of information and delayed timely interventions, impacting CoC. P2 elaborated, “If your speech pathologist has any questions, please, please get them to give me a call or email me. But the reality is, it's hard to find time that matches up.”
Discussion
This study explored the experiences of specialist cleft team SLPs in their communication and collaboration with community SLPs and parents. The cleft team SLPs described multiple ways in which they communicate and collaborate to maintain CoC, as well as the barriers and facilitators that influence these processes. The findings align with Haggerty and colleagues’ framework for CoC encompassing informational continuity, focusing on communication and knowledge-sharing; management continuity, relating to coordinated service provision and role clarity; and relational continuity, which emphasizes trust, professional rapport, and relationships between cleft teams, community SLPs and families. 6
Informational and Relational Continuity: Building Relationships Beyond Broadcasting
Effective CoC relies not only on the seamless transfer of information but also on the strength of relationships that support collaboration. Informational continuity ensures that critical knowledge about a child's care is consistently shared between professionals and families, while relational continuity fosters trust, mutual respect, and long-term partnerships that enhance the quality and consistency of care. Both elements are essential in cleft speech therapy, as they enable community SLPs, cleft teams, and families to work together effectively. However, findings from this study suggest that while cleft team SLPs were committed to sharing information, communication often remained one-directional, highlighting an opportunity to strengthen engagement through more reciprocal and interactive approaches. Respondents consistently highlighted the importance of strong relationships in ensuring CoC for children with cleft palate. They emphasized that effective partnerships with community SLPs and families facilitated trust, collaboration, and knowledge-sharing, ultimately benefiting the child's therapy journey. While cleft team SLPs recognized that “relationships matter” and reported they were committed to sharing information and supporting community clinicians, the data suggested that much of this communication was one-directional, with a focus on providing reports, email, and educational resources. There was less discussion on how ongoing, two-way communication and collaboration were actively fostered over time. This highlights an opportunity to strengthen engagement by exploring more interactive and reciprocal approaches to relationship-building.
While respondents frequently reported providing education and resources to community clinicians, there was little discussion on whether they actively sought feedback from these therapists about what support they needed or how they preferred to engage in collaboration. Instead, communication was often structured around reports and professional development, which, while valuable, may not have encouraged true partnership-building. The focus on knowledge dissemination over reciprocal exchange may have reinforced the reported hierarchical dynamic, where cleft team SLPs were positioned as the experts “giving” knowledge rather than collaborating on equal footing. While respondents spoke about wanting to integrate community SLPs more seamlessly into the care pathway, there was little mention of direct efforts to understand how these clinicians worked, what barriers they faced, or what type of support they needed. Without mechanisms for soliciting feedback and adapting their support accordingly, cleft team SLPs risked reinforcing the very divide they sought to overcome.
Cleft team SLPs also recognized the power of language in shaping professional relationships. Simple shifts in how emails, reports, and letters are worded could foster a more welcoming and collaborative tone. Instead of passive phrases like “Please contact me if needed,” stronger invitations such as “I’d love to discuss this case with you—please let me know a time that works” could encourage more reciprocal communication. These small but intentional adjustments could help reposition interactions as collaborative exchanges rather than top-down directives, fostering more engagement from community clinicians.
Moving forward, more intentional efforts could be explored to build relationships beyond information-sharing in order to facilitate collaboration. Strategies such as joint sessions, structured follow-up after reports, regular case discussions, and shifting language in communications to invite more engagement could create more sustainable, two-way partnerships. Without deliberate relationship-building efforts, the risk remains that cleft team SLPs will continue to broadcast information rather than cultivate lasting, collaborative connections that promote CoC. By expanding their approaches to communication and collaboration, cleft team SLPs could bridge the gaps in CoC and strengthen the partnerships that underpin high-quality care for children with cleft palate.
Management Continuity: Moving Beyond the Consultative Model
Management continuity refers to the coordination of care and service delivery across multiple providers to ensure that interventions are aligned and consistent. Cleft team SLPs have traditionally operated within a consultative model, providing advice, assessments, and recommendations to community SLPs who then implement therapy. While this model ensures that children with cleft palate receive specialized input, it can also reinforce a hierarchical dynamic, where community SLPs may feel they are simply receiving directives rather than being active partners in care. Many respondents expressed frustration over the lack of response from community SLPs, but the data suggested that limited two-way engagement may have contributed to these challenges.
Moving beyond a purely consultative role requires shifting towards a collaborative partnership model, where cleft team and community SLPs co-design treatment plans, share decision-making, and engage in structured mentoring. Grames et al.'s collaborative treatment model offers an innovative approach, promoting joint goal-setting, knowledge-sharing, and ongoing case discussions rather than isolated consultations. Implementing peer mentoring programs and co-treatment opportunities would allow cleft team SLPs to work alongside community clinicians, supporting skill development and ensuring therapy remains consistent across settings. 9 By redefining their role as facilitators of shared care, rather than just consultants, cleft team SLPs can foster stronger, more sustainable partnerships. This shift would not only enhance CoC but also empower community clinicians to feel more confident and engaged in cleft therapy, ultimately improving outcomes for children with cleft palate. Ultimately, this research should inform policy, practice, and education in cleft care, emphasizing the importance of cohesive care for improved patient outcomes and quality of life.
Limitations
A limitation of this study is its focus on specialist cleft team SLPs working within established cleft services in Australia and New Zealand. The findings may not fully capture the experiences of cleft team SLPs in other healthcare systems or resource-limited settings, including low and middle-income countries. Additionally, the participants in this study were highly experienced clinicians which may limit the applicability to less experienced clinicians in the same or similar settings. Finally, there is the potential influence of pre-existing professional relationships between the researchers and the participants which was managed through the inclusion of researchers without these relationships and through reflexive practice as described in the method.
Conclusion
This study explored the experiences of cleft team SLPs in communicating and collaborating with community SLPs and parents to facilitate CoC for children with cleft palate. Respondents consistently emphasized the importance of relationships in ensuring effective care, recognizing that strong partnerships facilitated trust, collaboration, and knowledge sharing. While cleft team SLPs demonstrated a strong commitment to education and supporting families and community clinicians, their engagement often took the form of information dissemination rather than interactive, two-way relationship-building. Although some community SLPs actively sought guidance and maintained open lines of communication, cleft team SLPs expressed frustration at the lack of engagement from others, suggesting that communication gaps persisted.
Despite these challenges, cleft team SLPs remained dedicated to fostering collaboration and enhancing the capacity of community clinicians through education and knowledge-sharing. Moving forward, a shift towards a co-facilitative role rather than a purely consultative model may strengthen relationships and improve CoC. Rather than positioning themselves as the primary experts directing care, cleft team SLPs could work alongside community clinicians in a more interactive, shared capacity, encouraging reciprocal learning and collaborative problem-solving. Strategies such as joint sessions, interdisciplinary meetings, structured mentoring, and more intentional follow-up processes could help foster this approach. Additionally, cleft team SLPs may benefit from refining the way they frame communication—using language that encourages reciprocal dialogue and ensures that community clinicians and parents feel empowered to contribute to the care process.
Further research is needed to explore the perspectives of community SLPs and parents to gain a more comprehensive understanding of their experiences and expectations in CoC within cleft speech pathology services. Ultimately, fostering a culture of shared learning, mutual respect, and equal partnership between cleft team and community SLPs, alongside active parental involvement, will be essential in improving CoC for children with cleft palate.
Supplemental Material
sj-docx-1-cpc-10.1177_10556656251348297 - Supplemental material for Experiences of Cleft Team Speech-Language Pathologists in Continuity of Care: Building Relationships Beyond Broadcasting
Supplemental material, sj-docx-1-cpc-10.1177_10556656251348297 for Experiences of Cleft Team Speech-Language Pathologists in Continuity of Care: Building Relationships Beyond Broadcasting by Mikaela Bow, Patricia McCabe and Alison Purcell in The Cleft Palate Craniofacial Journal
Footnotes
Acknowledgments
A huge thank you to Dr. Rebecca Sutherland for jumping in and helping get this paper over the line. Your support, insights, and fresh perspective in the final stages made all the difference.
Data Availability
The data that supports the findings of this study is available in the supplemental material.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was approved by the Human Research Ethics Committee of The University of Sydney (2023/105).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written informed consent for publication was obtained from all participants included in this study.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
