Abstract
Objective
To identify factors associated with velopharyngeal competence at 10 years of age in children with cleft palate, and examine the longitudinal development of velopharyngeal competence.
Design
Registry-based cohort study.
Setting
Regional public care university hospitals in Sweden.
Participants
A total of 507 children born with a cleft palate with or without cleft lip/alveolus.
Main Outcome Measures
Velopharyngeal competence according to speech language pathologists’ ratings corresponding to the VPC-Rate with and without consideration of intervening secondary speech-improving surgery.
Results
Children with additional conditions had significantly lower odds of velopharyngeal competence with no intervening speech-improving surgery than those without (OR 0.60, 95% CI 0.37-0.99). Children who had primary palatal surgery after 25 months of age (OR 0.23, 95% CI 0.11-0.49) or in more than 1 stage (OR 0.49, 95% CI 0.31-0.78), also had lower odds of a positive outcome, but these results may have been impacted by differences in cleft subtypes. Prevalence of velopharyngeal competence regardless of intervening surgery was 85% at age 5 years and 93% at age 10 years. For 17 children, velopharyngeal dysfunction emerged after 5 years of age.
Conclusions
Additional conditions were associated with decreased odds of velopharyngeal competence with no intervening surgery at 10 years of age. Whether primary palatal surgery performed late and in multiple stages also decreases odds of velopharyngeal competence should be investigated further. Prevalence of velopharyngeal competence increased from 5 to 10 years of age. Speech follow-up in children with cleft palate should continue until at least 10 years of age.
Introduction
The goal of primary palatal surgery in children with cleft palate with or without cleft lip (CP ± L) is to provide optimal conditions for developing velopharyngeal competence (VPC). Nevertheless, some children continue to be unable to effectively separate the oral and nasal cavities, which leads to persisting velopharyngeal dysfunction (VPD); this manifests in speech as hypernasal resonance, audible nasal air leakage, and/or reduced pressure in high-pressure consonants. Significant VPD can make speech indistinct, decrease intelligibility, and have a negative impact on the quality of life. 1 The most common treatment is secondary velopharyngeal surgery (VPD surgery). 2
Velopharyngeal Competence in Populations With Cleft Palate
In a study based on the CRANE database (data from England, Wales, and Northern Ireland), 70.8% of 5-year-old children with CP ± L had no structurally related speech difficulties and no history of speech surgery. 3 Another British study of 5-year-old children with CP ± L found that 97% had adequate velopharyngeal function, 2.6% had undergone secondary speech surgery, and 10.7% had undergone fistula repair. 4 In the multicenter randomized controlled Scandcleft trials that involved children with unilateral cleft lip and palate (UCLP), VPC was found in 35% to 61% of the participants at 5 years of age 5 and in 58% to 83% of the participants at 10 years of age. 6 Additionally, “primary competent velopharyngeal function” (defined as VPC and no secondary velopharyngeal surgery), was reported for 47% to 68% of the 10-year-olds. 6
In a systematic review that aimed to investigate the impact of age at primary surgery and surgical technique on the risk of velopharyngeal insufficiency after primary palatoplasty, Xepoleas et al. remarked that most of the included studies reported speech outcomes at a minimum age of 4 years, which they considered sufficient as it was deemed unlikely that VPD would emerge at a later age. 7 However, two separate multicenter studies reported cases of children with UCLP who were judged as having VPC at age 5 or 7 years before developing VPD at age 10 years.8,9 Analysis of the longitudinal development of VPC in other cleft subtypes and in larger cohorts would provide stronger evidence regarding minimal follow-up time.
Factors Impacting Velopharyngeal Competence
Large studies that have examined associations of patient characteristics or primary palatal surgery characteristics with the incidence of secondary VPD surgery have provided evidence both for and against significant associations.10-12 In a previous study that we conducted, we found a significantly lower risk of requiring secondary VPD surgery for children with cleft soft palate only (SP) compared with other cleft subtypes, but risk of requiring VPD surgery was not significantly associated with other cleft subtypes, gender, or additional conditions. 13 There was, however, a significantly higher risk of requiring VPD surgery for children who underwent primary palatal surgery after 18 months of age or who underwent primary palatal surgery in more than 1 stage. 13
In a meta-analysis, Sainsbury et al. aimed to identify patient factors influencing velopharyngeal function following initial cleft palate repair. 14 They found that only 30% of the included studies that reported perceptual speech assessment used a published scale, only 21% used blinded speech assessment, and many of them did not report reliability measures. 14 Nevertheless, some previous studies have investigated relationships between independent variables and symptoms of VPD in speech using reliable methodology. Butterworth et al. found that structurally related speech difficulties did not differ in relation to gender, cleft subtype, or between children with or without Robin sequence. 3 They did, however, find increasing odds of structurally related speech difficulties with increasing palatal cleft extent. 3 In a systematic review that compared outcomes after 1-stage and 2-stage palatoplasty, Cornefjord et al. 15 identified four controlled studies that reported speech outcomes in children with UCLP; one study showed better VPC outcomes in the 2-stage group at 10 years of age 6 whereas the remaining studies reported no difference between the 1- and 2-stage palatoplasty groups.5,16,17 However, this evidence was graded as having low certainty, and three of the four studies were part of the Scandcleft trials, thus investigating the same patient cohort. 15 Additionally, Klintö et al. found that 5-year-old children with cleft soft and hard palate (SHP) were less likely to have VPC compared with those with UCLP. 18 There was also higher risk of negative speech results when primary palatal surgery was completed after 25 months of age, but no significant difference in VPC outcomes based on gender was detected. 18
Cleft Palate Care in Sweden
In Sweden, approximately 175 new cases of cleft lip and/or palate (CLP) are diagnosed each year.
18
Children with CLP are treated and followed up at one of six regional CLP centers. Some of the centers perform primary palatal surgery in 1 stage, some use 2-stage surgery, and one center performs 1-stage surgery on children with SP and SHP and 2-stage surgery on bilateral cleft lip and palate (BCLP) and UCLP.
18
For children born with CLP, data are collected until they are 19 years of age and registered in the Swedish CLP Registry, including demographic information, data on surgical treatment, and outcomes related to speech and dentofacial development.
19
The CLP Registry has a high degree of coverage (94.6%) and high levels of reporting for surgical procedures (94.4%) and speech outcomes (96.4%
CLP Registry Speech Registrations
In the CLP Registry, results from speech assessments by speech and language pathologists are registered at 5, 10, 16, and 19 years of age 19 based on audio recordings of single-word naming and sentence repetition from the Swedish Articulation and Nasality Test (SVANTE) 21 as well as continuous speech. In each registration, velopharyngeal competence is rated on a three-tier scale based on all available speech material according to the VPC-Rate (VPC-R),19,22 as recommended by the International Consortium for Health Outcomes Measurement (ICHOM). 23 The tiers are 0: competent/sufficient; 1: marginally incompetent/insufficient (marginal speech symptoms indicating slight problems with velopharyngeal closure, which may be sufficient in some conditions and somewhat insufficient in others and would not usually lead to the recommendation of surgical treatment); and 2: incompetent/insufficient (significant speech symptoms which would usually lead to the recommendation of surgical treatment after further evaluation). If non-oral articulation persists throughout the speech sample, the velopharyngeal function is rated as incompetent. In addition, articulation results are reported as percentage of consonants correct and percentage of non-oral speech errors, based on phonetic transcriptions of the 59 target consonants in the SVANTE single-word naming test. 21 Parent-reported intelligibility is reported at 5 and 10 years of age using the Intelligibility in Context Scale. 24
Each speech registration is based on a perceptual evaluation by one speech and language pathologist in a clinical setting. To enable reproducible research on the speech measures in the CLP registry, intra- and inter-rater reliability have been examined for 5- and 10-year-old children in previously published studies.25-27 These analyses showed that the three-tier VPC ratings were reliable at 5 years of age, 25 but had weaker reliability at 10 years of age. 26 To facilitate the presentation of results, the VPC variable from the CLP registry has been dichotomized into a binary quality indicator of competent/marginally incompetent versus incompetent velopharyngeal function. 25 This cut point is clinically relevant, as a VPC score of 2 (incompetent velopharyngeal function) often leads to the recommendation of surgical treatment whereas a score of 0 (competent velopharyngeal function) or 1 (marginally incompetent velopharyngeal function) usually does not. This quality indicator has been found reliable at 5 and 10 years of age.25,26
Aims
The present study had two aims. The first was to analyze whether VPC at 10 years of age was associated with cleft subtype, additional conditions, age at primary soft palatal surgery, age at complete primary palatal surgery, and/or number of stages for primary palatal surgery. The second aim was to examine the longitudinal development of VPC in the population of Swedish-born children with cleft palate.
Materials and Methods
Ethical Considerations
Ethical approval was obtained from the Swedish Ethical Review Authority (reference no. 2020
Study Design and Participants
For this registry-based cohort study, data consisting of baseline information, cleft-related surgical procedures, and speech outcomes at ages 5 years (±6 months) and 10 years (±12 months) were retrieved from the CLP Registry via the Center of Registers South, Lund, Sweden. The extracted data included registrations made between 1 January 2009 and 31 October 2023 for children born from 1 January 2009 to 30 October 2014. Participants were considered eligible for the study if they were born in Sweden and had CP ± L. Participants with submucous cleft palate or a cleft not involving the palate were excluded, as were deceased individuals and those who were still within the 10-year age range but had not yet returned for follow-up. This resulted in 583 individuals in the CLP registry eligible for the study. Additionally, those who had emigrated or had no primary palate surgery registered were excluded, as well as one participant with a cleft that was detected so late that primary palatal surgery was performed after the age of 10 years. This left 563 participants for the study population. The selection of the study sample is shown in Figure 1. All data were manually examined and suspected faulty registrations were validated against medical records.
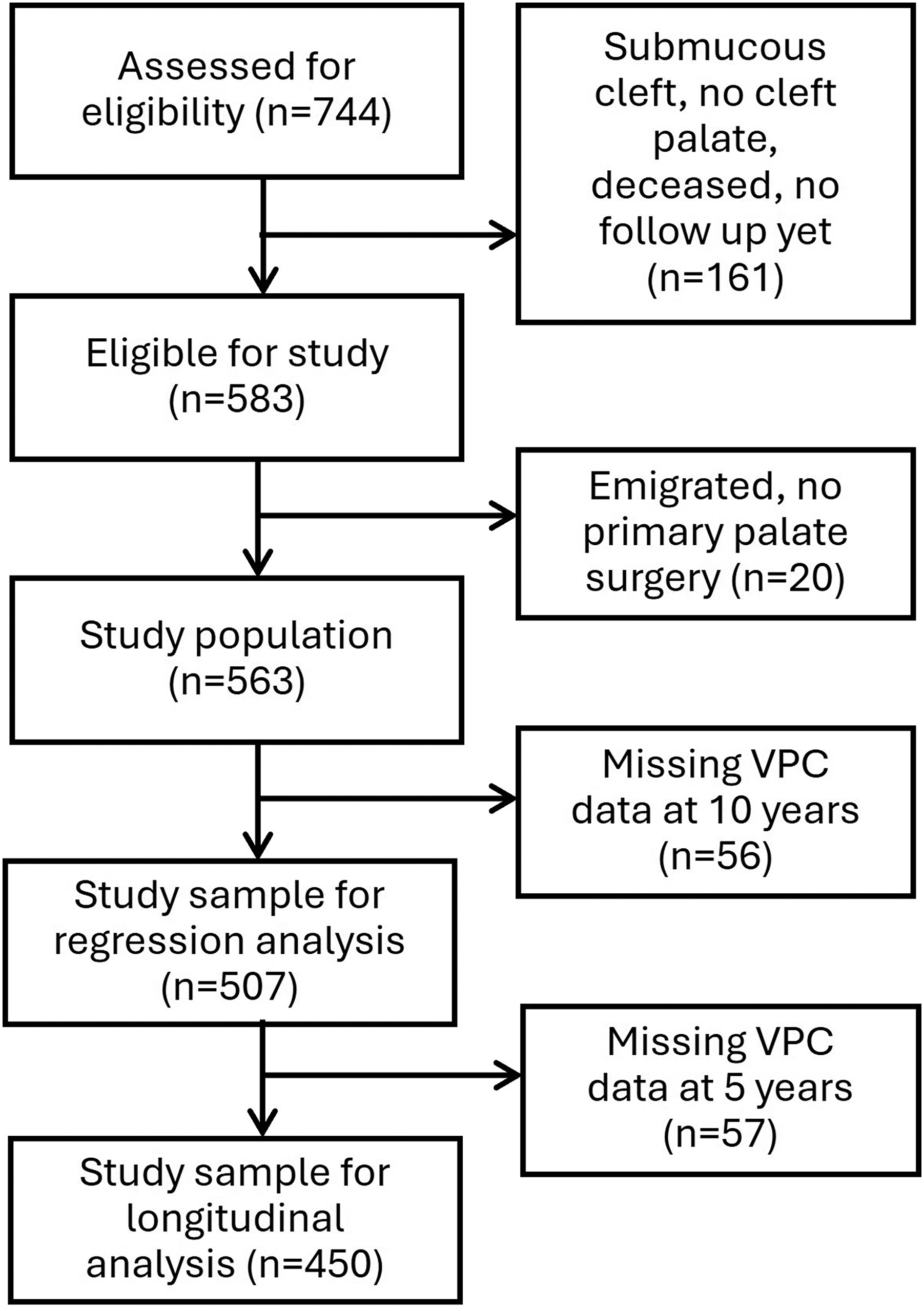
Flow chart of the study sample selection.
In the CLP Registry, if VPC could not be registered due to lack of cooperation from the child and/or limited speech, or insufficient quality of audio recordings, VPC was registered as “Not judgeable.” If VPC has not been rated for other reasons, VPC was registered as “Not evaluated.” Some participants simply had no speech registrations at certain ages for reasons unknown to us. It is likely that this was because the patient failed to attend follow-up within the specified time frame. Of the included participants, 56 were missing VPC data at 10 years of age (29 had no registered data and 27 were registered as “not evaluated” or “not judgeable”) and another 57 were missing VPC data at 5 years of age (46 had no registered data and 11 were registered as “not evaluated” or “not judgeable”).
Independent Variables
Based on the primary diagnosis for each participant, four subgroups were constructed according to cleft subtype: SP (referent category), SHP, UCLP, and BCLP. Twenty-one participants had atypical cleft diagnoses (Q36.1 Median cleft lip with Q35.5 Cleft hard palate with cleft soft palate, Q37.2 Cleft soft palate with bilateral cleft lip, and Q37.3 Cleft soft palate with unilateral cleft lip). Among these participants, clefts involving the alveolus were recoded as UCLP and clefts not involving the alveolus were recoded as SP or SHP.
In the CLP Registry, the presence of syndromes, a Robin sequence, or other malformations were registered as “yes,” “no,” or “unknown”. In the present study, those three variables were combined into the variable “additional conditions,” coded as “yes” (referent category), “no,” or “unknown.”
Participants were also divided into subgroups based on whether they had undergone primary palate surgery in 1 (referent category), 2, or 3 stages. Most of the included participants had palatal surgery in 1 stage (at 9
Based on results from previous studies, age at primary soft palatal surgery was classified as <7 months (referent category), 7 to 9 months, >9 to 13 months, or >13 months, 13 whereas age at complete primary palatal surgery was classified as <10 months, 10 to 13 months, >13 to 18 months (referent category), >18 to 25 months, or >25 months. 13 Data for the age at complete primary palatal surgery was missing for 2 of the included participants. There were no other missing data for the included participants. Characteristics of the study sample are summarized in Table 1.
Characteristics of the Study Sample, Stratified by Cleft Subtype.
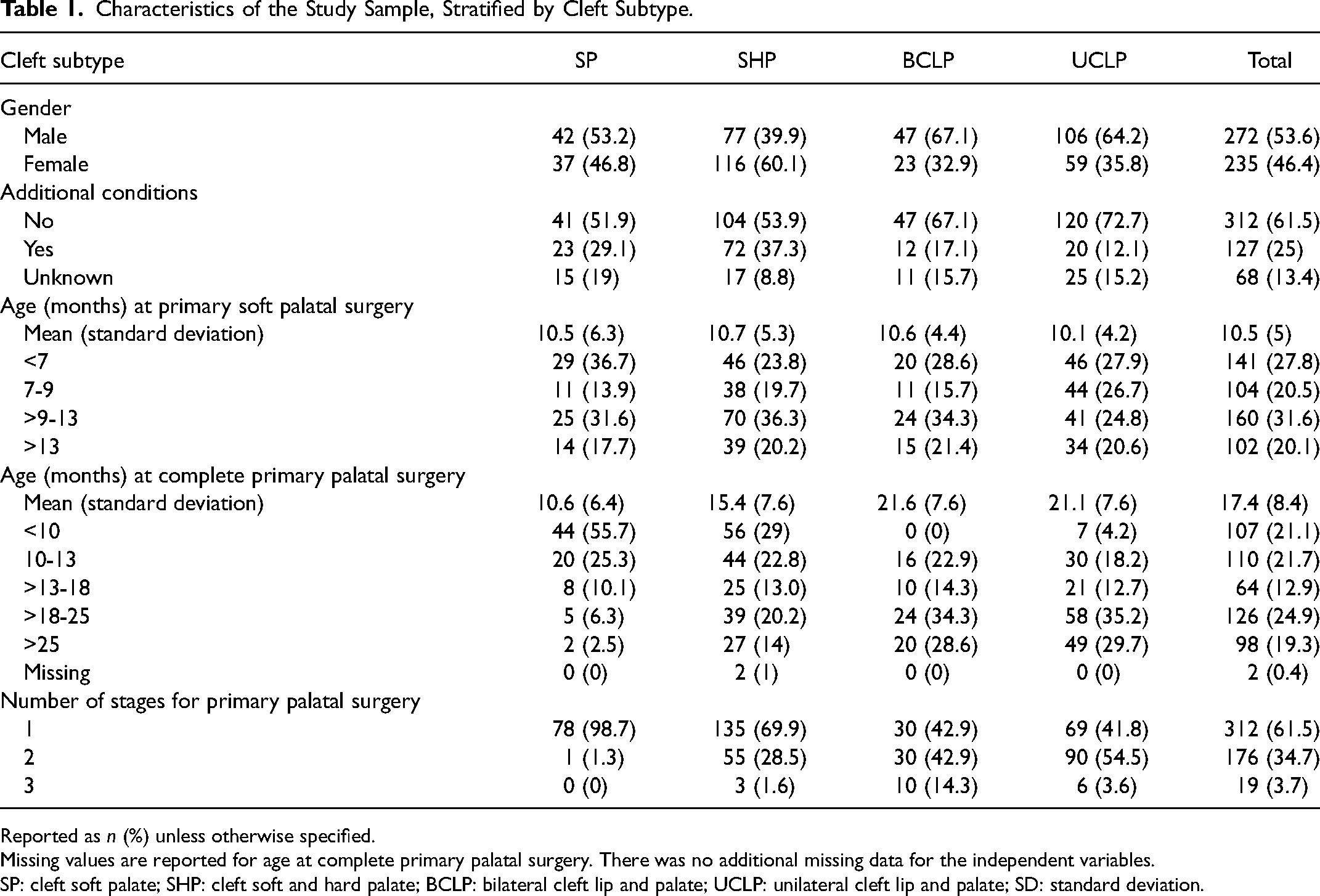
Reported as n (%) unless otherwise specified.
Missing values are reported for age at complete primary palatal surgery. There was no additional missing data for the independent variables.
SP: cleft soft palate; SHP: cleft soft and hard palate; BCLP: bilateral cleft lip and palate; UCLP: unilateral cleft lip and palate; SD: standard deviation.
Outcome Measures
For analysis, the three-tier VPC-R ratings from the CLP registry were dichotomized into the presence of VPC, defined as a competent or marginally incompetent velopharyngeal function (rating of 0 or 1), and absence of VPC, defined as an incompetent velopharyngeal function (rating of 2). As previously stated, this binary VPC variable has been found reliable for data from the CLP registry at both 5 (85% agreement 25 ) and 10 years of age (88% agreement 26 ). The outcome of primary VPC only included individuals with VPC and no intervening VPD surgery, while the outcome perceived VPC included all participants with VPC regardless of intervening VPD surgery. Since reasons for the performance of surgery are not included in the CLP Registry, we could not be certain which of the secondary procedures aimed to improve speech. We chose to define VPD surgery as palatal or pharyngeal procedures that were registered as “secondary” and performed after 3 years of age; this age limit was chosen as younger children are often not able to comply with visual evaluations of velopharyngeal function, which are a prerequisite to speech-correcting surgery in most Swedish CLP centers. Therefore, the performance of speech-correcting surgery in children younger than 3 years is unlikely. The reader is referred to Schaar Johansson et al. 13 for more information on the types of VPD surgery performed in Sweden.
Statistical Analysis
To estimate the associated effect of the independent variables cleft subtype, presence of additional conditions, age at primary soft palatal surgery, age at complete primary palatal surgery and number of stages for primary palatal surgery, and the outcome of primary VPC at 10 years of age, univariable and multivariable logistic regression analyses were used. We chose not to adjust the models for gender, since our previous study showed no significant association between gender and VPD surgery 13 and we did not have reason to expect any association between gender and VPC. Since age at primary soft palatal surgery and age at complete primary palatal surgery were both correlated with number of stages for primary palatal surgery, we included these variables in 3 separate multivariable models to avoid multicollinearity. Multivariable model 1 included cleft subtype, presence of additional conditions, and age at primary soft palatal surgery; multivariable model 2 included cleft subtype, presence of additional conditions, and age at complete primary palatal surgery; and multivariable model 3 included cleft subtype, presence of additional conditions, and number of stages for primary palatal surgery. Significance levels were set to P < .05.
To examine the longitudinal development of VPC, we plotted numbers of children with or without perceived VPC at 5 years of age who had or did not have perceived VPC at 10 years in a contingency table.
To examine the risk of selection bias on results, the characteristics of the 56 participants who were excluded from the regression analysis due to missing 10-year VPC data were compared with those who were included using the Chi-square test, as presented in Appendix 1. In the excluded group, we found that UCLP was more common and SP and SHP less common, a higher proportion had additional conditions and a lower proportion had “unknown” additional conditions, mean age at primary soft palatal surgery was lower, and the proportion that had undergone primary palatal surgery in 1 stage was higher than in the included group. The included and excluded groups did not differ significantly in terms of age at complete primary palatal surgery. The limited differences between the groups led us to consider a complete-case analysis to be valid. Statistical analysis was performed using IBM SPSS Statistics version 28.0.1.1. This study adheres to the STROBE cohort reporting guidelines. 28
Results
Associations Between Primary Velopharyngeal Competence and Independent Variables
Results of univariable and multivariable logistic regression models for primary VPC at 10 years of age are presented in Table 2. In the univariable model, the odds of primary VPC were 71% lower for participants with BCLP than for participants with SP (odds ratio (OR) = 0.29, 95% confidence interval (CI) = 0.14–0.61). The association remained similar and statistically significant in a model also including the presence of additional conditions and age at primary soft palatal surgery (OR = 0.24, 95% CI = 0.11–0.52, multivariable model 1), but changed distinctly and to below statistical significance in a model including presence of additional conditions and either age at complete primary palatal surgery or number of stages for primary palatal surgery (multivariable models 2 and 3). Odds of primary VPC were 53% lower for participants with UCLP than those with SP in a model also including additional conditions and age at primary soft palatal surgery (OR = 0.47, 95% CI = 0.23–0.94, multivariable model 1), but changed distinctly and to below statistical significance in a model including presence of additional conditions and either age at complete primary palatal surgery or number of stages for primary palatal surgery (multivariable models 2 and 3).
Results of Univariable and Multivariable Logistic Regression Analysis Modelling Associations of Independent Variables to Odds of Primary Velopharyngeal Competence (VPC) at 10 Years of Age.
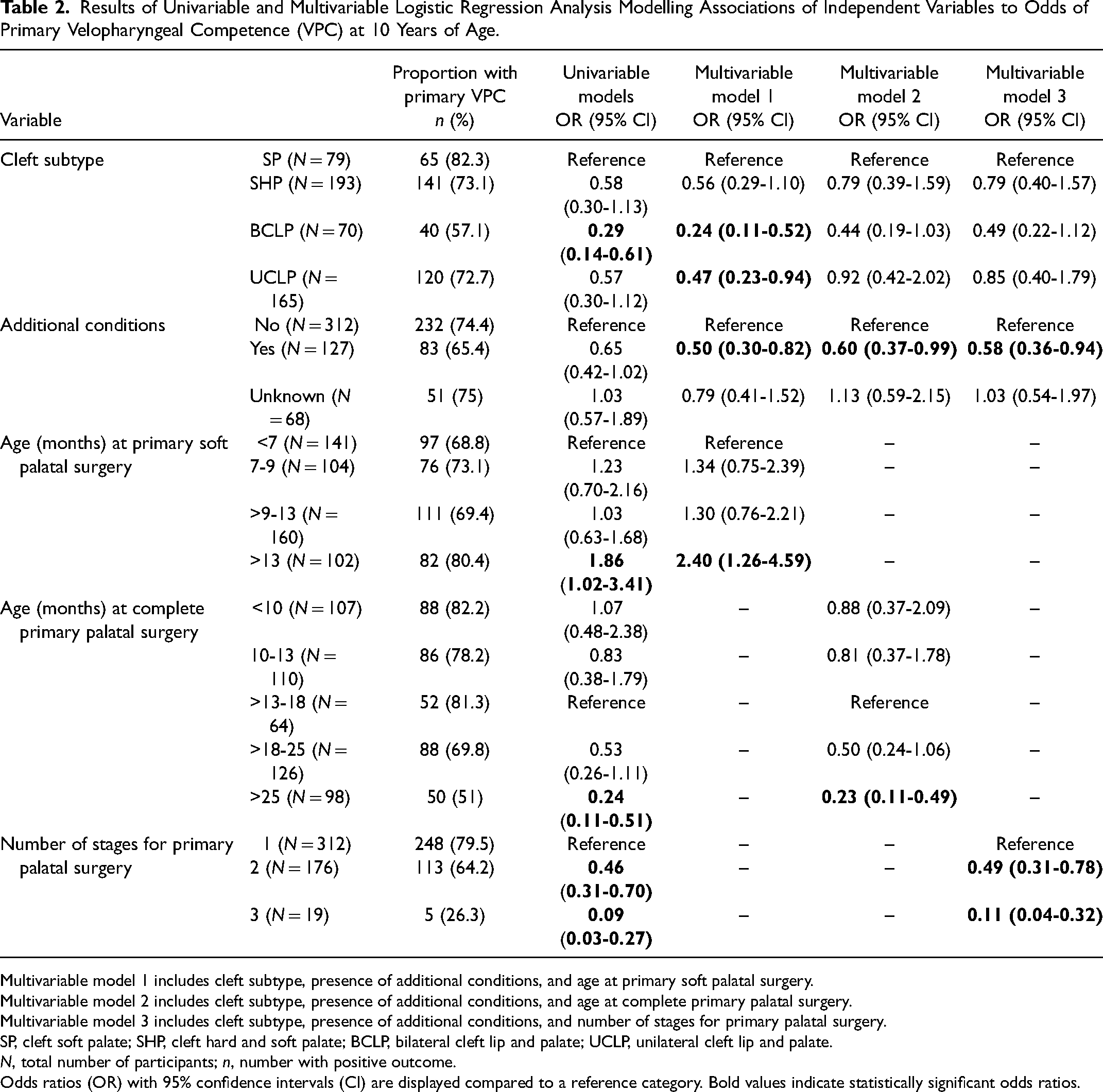
Multivariable model 1 includes cleft subtype, presence of additional conditions, and age at primary soft palatal surgery.
Multivariable model 2 includes cleft subtype, presence of additional conditions, and age at complete primary palatal surgery.
Multivariable model 3 includes cleft subtype, presence of additional conditions, and number of stages for primary palatal surgery.
SP, cleft soft palate; SHP, cleft hard and soft palate; BCLP, bilateral cleft lip and palate; UCLP, unilateral cleft lip and palate.
N, total number of participants; n, number with positive outcome.
Odds ratios (OR) with 95% confidence intervals (CI) are displayed compared to a reference category. Bold values indicate statistically significant odds ratios.
Odds of primary VPC for participants with additional conditions compared with those without additional conditions were 50% lower in a model also including cleft subtype and age at primary soft palatal surgery (OR = 0.50, 95% CI = 0.30
Unadjusted odds of primary VPC were 86% higher for participants who underwent primary soft palatal surgery after 13 months of age compared to before 7 months (OR = 1.86, 95% CI = 1.02
Unadjusted odds of primary VPC were 76% lower for those who underwent complete primary palatal surgery after 25 months of age compared to 13 to 18 months (OR = 0.24, 95% CI = 0.11
Compared to those who had undergone primary palatal surgery in 1 stage, unadjusted odds of primary VPC were 54% lower for those who had 2-stage surgery (OR = 0.46, 95% CI = 0.31
Longitudinal Development of Velopharyngeal Competence
In the longitudinal analysis, 113 participants were excluded because they were missing VPC data at 5 and/or 10 years of age. For the 450 included participants, the prevalence of perceived VPC was 85% (n = 383) at 5 years of age and 93% (n = 420) at 10 years of age. As seen in Table 3, of 383 participants who had perceived VPC at 5 years of age, 366 (96%) had the same result at age 10 whereas 17 (4.4%) did not have perceived VPC at age 10. Additionally, we found that 27 participants who had perceived VPC at both age 5 and 10 years had VPD surgery between those time points, indicating that VPD had developed after 5 years of age. Of 67 participants who did not have perceived VPC at 5 years of age, 54 (81%) had perceived VPC at 10 years of age whereas 13 (19%) did not.
Contingency Table Showing Number of Participants with Perceived Velopharyngeal Competence (VPC) at 5 and 10 Years of Age.
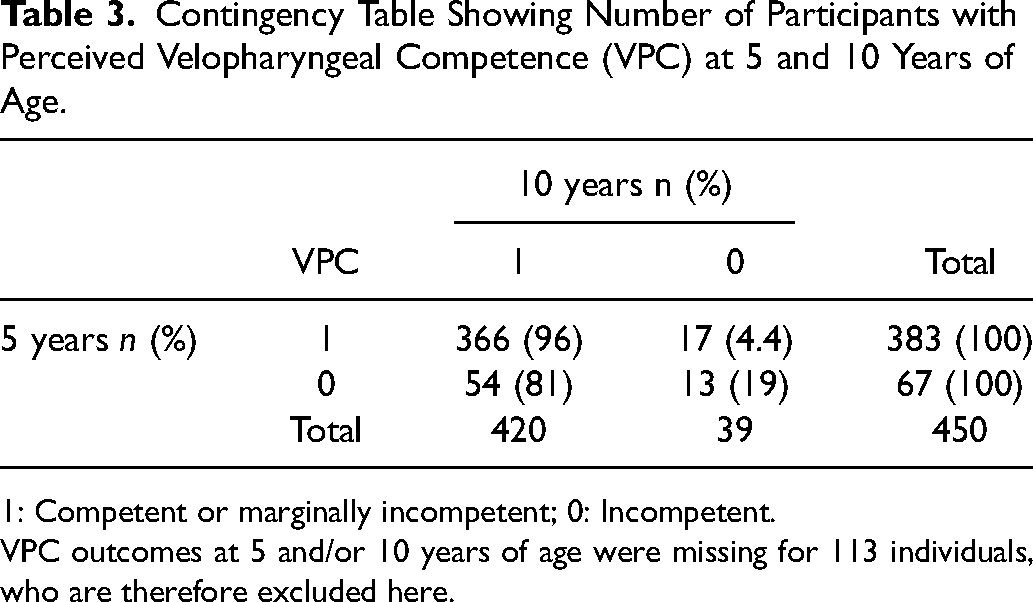
1: Competent or marginally incompetent; 0: Incompetent.
VPC outcomes at 5 and/or 10 years of age were missing for 113 individuals, who are therefore excluded here.
Discussion
The first aim of this study was to analyze the associations of VPC at 10 years of age with cleft subtype, additional conditions, age at primary soft palatal surgery, age at complete primary palatal surgery, and/or number of stages for primary palatal surgery. We found significantly decreased odds of primary VPC for participants with additional conditions and significantly increased odds for those who underwent primary soft palatal surgery after 13 months of age. We also found significantly decreased odds of primary VPC for participants who underwent complete primary palatal surgery after 25 months of age or in more than 1 stage, but distinct changes in odds ratios when including cleft subtype in the same regression models as age at complete primary palatal surgery or number of stages for primary palatal surgery indicate that outcomes may differ based on cleft subtype rather than the variations in primary palatal surgery.
Association Between Velopharyngeal Competence and Additional Conditions
We found that participants with additional conditions had around 40% lower odds of primary VPC compared with those without additional conditions. This is in agreement with a previous study by Persson et al., where a significant impact on velopharyngeal impairment was found for additional malformations in children with SP and SHP, 29 and one by Klintö et al., where the differences were similar but not statistically significant; 30 however, that study sample was quite small. In our previous study, we found that children with additional conditions and CP ± L were neither more nor less likely to have VPD surgery. 13 However, for children with additional conditions, the prevalence of VPD surgery is less likely to reflect the prevalence of VPD since a larger proportion of children with additional conditions than those without did not provide sufficient speech for VPC ratings, as indicated in Appendix 1. If VPC cannot be rated, VPD will not be discovered and there will be no reason to perform VPD surgery. Moreover, children with developmental disorders that impact their general communication abilities may not be expected to benefit from VPD surgery, which is another reason why VPD surgery may be less prevalent in this group.
Associations Between Velopharyngeal Competence and Primary Palatal Surgery
We found that the adjusted odds of primary VPC were doubled in participants who underwent primary soft palatal surgery after 13 months of age compared to before 7 months of age. Adjusted odds of primary VPC were also 77% lower for participants who underwent complete primary palatal surgery after 25 months of age compared to between 13 and 18 months of age, but it cannot be ruled out that this was due to cleft subtype rather than age at surgery. A higher risk of negative speech results has previously been found for children who had complete primary palatoplasty after the age of 25 months.
18
By contrast to the results of the present study, Willadsen et al. found a higher prevalence of primary VPC after early soft palatal closure at 3 to 4 months and late hard palatal closure at 36 months than after 2-stage soft and hard palatal closure at 12 months in the Scandcleft trials.
6
However, the prevalences of primary VPC for both groups in that study were lower than in the present study (47%
The odds of primary VPC were significantly lower for participants who underwent primary palatal surgery in more than 1 stage, but it is possible that this difference was also affected by differences in cleft subtype. In their systematic review, Cornefjord et al. found no clear advantages in speech outcomes for either 1- or 2-stage palatoplasty. 15 All of the studies included in that review focused on non-syndromic children with UCLP, and the certainty of the evidence was rated as low. 15 The referenced studies reported speech outcomes without consideration of intervening VPD surgery. 15 Although the studies referenced by Cornefjord et al. 15 showed no difference in perceived VPC based on number of stages for primary palatal surgery, the results of the present study suggest that there is reason to investigate further whether children who undergo more than one primary palatal surgery have a higher risk of requiring secondary VPD surgery to achieve that result. As a higher number of stages for primary palatal surgery usually leads to a higher age at complete primary palatal surgery, it can be difficult to isolate those two variables from each other in an observational study such as this one.
Longitudinal Development of Velopharyngeal Competence
The second aim of this study was to examine the longitudinal development of VPC in the population of Swedish children with cleft palate. We found that the proportion of participants with perceived VPC increased from 85% at age 5 years to 93% at age 10 years. The prevalence at 5 years of age was lower than in a previous study by Baillie and Sell, 4 and at both ages higher than in the Scandcleft trials.5,6 In both referenced studies, however, variations of the VPC-Sum were used as an outcome measure,4-6 whereas the present study was based on results corresponding to the VPC-Rate. 22 As previously described, the VPC-Rate is an overall rating of passive cleft speech characteristics based on all available speech material. The VPC-Sum is based on single-word speech material and combines ratings of hypernasality and frequency of passive velopharyngeal symptoms as well as non-oral errors related to VPD to a composite score. In a previous methodological study, the VPC-Sum was found to classify a higher number of cases as VPD than the VPC-Rate. 22 As for study samples, children with syndromes possibly impacting speech were excluded in both referenced studies4-6 but not in the present one. Moreover, the study by Baillie and Sell 4 had a larger number of exclusions due to missing outcome data than the present one, but made no exclusions based on native language, as in the Scandcleft project, or on immigration from another country, as in the present study. In summary, direct comparisons between these studies cannot be made due to differences regarding study cohorts and outcome measures.
While perceived VPC for most children was consistent or improved from 5 to 10 years of age, for 17 children it deteriorated. Another 27 children had VPD surgery between 5 and 10 years of age despite ratings of VPC at 5 years, which suggested that velopharyngeal function had deteriorated after the age of 5 years for them as well. The same trend has been described previously.8,9 Reasons for VPC deterioration from 5 to 10 years of age may be adenoid involution or pharynx growth, causing an increased distance between the soft palate and the posterior pharyngeal wall. Since this happens in some cases, it is important to consider in cleft care as well as clinical audits and research studies that speech should continue to be evaluated until at least 10 years of age and that speech outcomes should not be considered final at age 5.
Methodological Considerations
We chose to base the primary outcome measure not only on perceptual ratings of speech but also to consider whether or not secondary surgery had been performed. In comparing outcomes after different surgical protocols, we consider it necessary to not only look at speech results but also to include the burden of care in the form of additional interventions, as these are factors of importance for both patients and wider society. On the other hand, the prevalence of VPC based only on speech evaluations helps inform caregivers about expected outcomes for their child and may be especially relevant when comparing the impact of intrinsic patient factors, such as cleft extent or presence of additional conditions. Impact of speech therapy was not considered in the present study, as it is generally established that VPD is a structural deficit and, as such, is treated surgically rather than through speech therapy. 2
As discussed above, methodological differences may influence speech results. Furthermore, in a systematic review of the risk of velopharyngeal insufficiency after primary palatoplasty, Xepoleas et al. found that around half of the included studies did not evaluate speech at all but used the prevalence of secondary surgery as the outcome measure. 7 The difference between the prevalence of VPC and associated factors in the present study and the risk of VPD surgery and factors associated with this risk for the same cohort, as reported in our previous study, 13 confirm that the prevalence of VPD surgery alone is not a sufficient outcome measure of speech, nor is it a sufficient measure of the success of primary palatal surgery. As pointed out by Sommerlad 32 among others, it fails to identify individuals with incompetent velopharyngeal function who are not offered or who decline surgical intervention.
Previous investigations of results on VPC have often used unreliable methodologies.7,14 For perceptually judged speech results to be reproducible and valid, they should be based on standardized assessment methodology, and reports must include inter- and intra-rater reliability measures.33-35 The present study was based on retrospective registry data. Although we could not report measures of reliability for the specific study sample, the CLP registry speech data has previously been shown to be reliable,25,26 which secures reproducibility and validity of our results.
Strengths and Weaknesses
In registry studies, the selection of variables that can be included for analysis is limited. We did not have information on the surgeons’ experience or surgical skills, or which techniques they used. We also did not have data on cleft width, which has previously been found associated with the need for secondary surgery and symptoms of VPD. 36 As hearing data in the CLP Registry is incomplete for many patients, we refrained from analyzing it. These are all possible unmeasured confounders which may have influenced the outcome. On the other hand, a substantial advantage of utilizing registry data is that it gives access to a large study sample with a low risk of sampling bias. Due to the high coverage and reporting degrees of the CLP Registry, 20 the retrieved data included almost an entire national cohort of children with CLP. Thus, we consider the results generalizable to patient cohorts in other countries with a similar availability of healthcare resources and similar protocols for primary palatal surgery (i.e., 1- or 2-stage palatal closure).
The proportion of excluded participants due to no speech registrations was not higher than the drop-out level generally expected in prospective randomized multi-center studies. 37 Nevertheless, to examine the risk of selection bias due to loss to follow-up, we performed a post hoc comparison of characteristics of the 56 participants who were excluded due to missing speech results against those included (Appendix 1). The excluded participants had a higher prevalence of additional conditions, possibly because this group is more likely to be unable to provide sufficient speech for VPC ratings. Since we found lower odds of primary VPC in the presence of additional conditions, we might expect the prevalence of primary VPC at any age to be lower if those participants could have been included. On the other hand, the excluded group had a higher prevalence of cleft palate only, as opposed to cleft lip and palate. Cleft palate only was associated with higher odds of primary VPC. To summarize, the characteristics of the excluded participants might have caused selection bias if that group had been larger, but since the proportion excluded was quite small, we conclude that the risk of selection bias is low.
We chose not to exclude children with additional conditions from this study since they constitute a large proportion of the cohort with CLP (29% of the sample in this study), and it is, of course, equally important to expand the knowledge base and improve care for this group as for children without additional conditions. In a previous study comparing CLP Registry data to medical records for one of the Swedish CLP centers, the prevalence of additional diagnoses was 14.4 percentage points higher in medical records than in the registry. 38 It can be assumed that this discordance is similar in data from the other CLP centers. Knowing this, we chose to include the category of “unknown” additional conditions in our analysis rather than coding them as missing, to mitigate the effect of underreporting of additional conditions in the registry. Additional conditions were more prevalent among excluded participants and more often unknown among included participants, confirming that some of those unknowns were probably unreported cases of additional conditions. Moreover, CLP Registry data regarding the presence of syndromes or additional malformations includes a wide range of conditions with different levels of impact on communication and speech. More detailed information on those conditions would have enabled differentiation between conditions that are more or less likely to impact VPC. On the other hand, adding details to a variable will often increase the risk of incorrect or incomplete data registrations. 39 Therefore, although more detailed registry variables would provide valuable information if correctly registered, they may be less likely to have sufficient reporting degrees and reliability.
Clinical Implications
In line with several previous studies,11,13,18 the results of the present study provide added evidence that VPC without intervening VPD surgery may be less likely after late complete primary palatal surgery. VPC may also be less likely after more than one primary palatal surgery. In future studies, similar analyses performed separately for the different cleft subtypes could provide clarity as to whether cleft subtype or age at surgery/number of surgeries appears to have the most significant impact on the speech outcome.
In keeping with previous studies,8,9 we found that a small number of participants developed incompetent velopharyngeal function after the age of 5 years. It is therefore important to continue speech evaluations until at least, and preferably beyond, the age of 10 years. This also illustrates that evaluations of the effect of primary palatal surgery should not be considered final in terms of speech results before the age of 10.
Conclusions
In summary, we found that children with additional conditions had a lower likelihood of primary VPC than those without additional conditions. Primary VPC was less likely for children who had undergone complete primary palatal surgery after 25 months of age than at 13 to 18 months, and for those who underwent primary palatal surgery in more than 1 stage, but the impact of cleft subtype on these results is uncertain.
At age 10 years, 93% of Swedish children had competent or marginally incompetent velopharyngeal function. The prevalence increased from 5 to 10 years of age, most likely due to spontaneous improvement in some individuals and secondary surgical treatment in others. In some children, however, VPC at 5 years of age deteriorated to incompetent velopharyngeal function at 10 years of age. Our recommendation is therefore that follow-up speech assessments for children with CLP should continue until at least 10 years of age, and that speech outcomes after primary palatal surgery should not be considered final before 10 years of age.
Supplemental Material
sj-docx-1-cpc-10.1177_10556656251339880 - Supplemental material for Velopharyngeal Competence in Children With Cleft Palate: Related Factors and Longitudinal Development
Supplemental material, sj-docx-1-cpc-10.1177_10556656251339880 for Velopharyngeal Competence in Children With Cleft Palate: Related Factors and Longitudinal Development by Malin Schaar Johansson, Magnus Becker, Mia Stiernman and Kristina Klintö in The Cleft Palate Craniofacial Journal
Footnotes
Acknowledgments
The authors are grateful to all CLP team members who have contributed data to the CLP registry.
Consent for Publication
Not applicable.
Data Availability Statement
The datasets generated and/or analyzed during the current study are not publicly available because of ethical restrictions but are available from the corresponding author upon reasonable request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval and Informed Consent Statements
Ethical approval was obtained from the Swedish Ethical Review Authority (reference no. 2020-00227). Data access was approved by the consultation group for quality registries, care databases, and preparation in the Skåne Region (reference no. 036-22). The Ethics Review Authority of Sweden waived the requirement for informed consent because of the retrospective nature of the study. The procedure for information and consent followed the legal guidelines for participation in national quality registries in Sweden.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the Promobilia Foundation, the Sunnerdahl Disability Foundation, and the Foundation for Research in Plastic Surgery.
Stiftelsen för plastikkirurgisk forskning, Stiftelsen Sunnerdahls Handikappfond, Stiftelsen Promobilia (grant number F31/23, F21501).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
