Abstract
Objective
In our study, we aim to assess trends in mandibular distraction osteogenesis (MDO) management and outcomes among infants in a national database between 2012 and 2022.
Design
A cross-sectional analysis of the National Surgical Quality Improvement Program (NSQIP) pediatric database was conducted from 2012 to 2022.
Setting
Not applicable.
Patients, Participants
Children under the age of 1 undergoing MDO.
Interventions
Specific interventions were not recorded due to the nature of the study.
Main Outcome Measure(s)
Trends in the number of MDO procedures performed by otolaryngology-head and neck surgeons (OHNS) and complication rates.
Results
We identified 232 cases of MDO procedures for patients under the age of 1 year, of which 28.9% (N = 67) underwent surgery with OHNS. The proportion of MDO performed by OHNS over the study period did not exhibit a significant change in univariate Pearson correlation analysis (R = 0.426, P = .219). Non-OHNS and OHNS both demonstrated an overall complication rate of 33% (55/165 and 22/67, respectively). On multivariable regression, OHNS were more likely to treat patients with congenital lung disease (OR 5.48,95% CI 1.52-22.1, P = .011). The operative year was not associated with being treated by OHNS (P = .992).
Conclusions
No change in the proportion of MDO for patients under the age of 1 year performed by OHNS was observed over the past decade. OHNS are more likely to treat patients with congenital lung disease compared to their colleagues. Complication rates show no significant difference between non-OHNS and OHNS.
Keywords
Introduction
Pierre Robin (PR) is recognized as a clinical triad of congenital micrognathia, glossoptosis, and airway obstruction. 1 Cleft palate, while not required, has a high association rate with PR ranging from up to 90%. 1 PR affects approximately 1 in 8000 to 1 in 14 000 newborns.1,2 Described as a heterogenic condition, it can be found in isolation or as part of other syndromes. 1 Stickler syndrome, velocardiofacial syndrome (22q11.2 deletion syndrome), fetal alcohol syndrome, and Treacher Collins syndrome are among the most highly associated syndromes. 1
Untreated PR predisposes infants to respiratory obstruction, feeding problems, and failure to thrive, with respiratory obstruction most commonly due to mandibular malpositioning and subsequent tongue base obstruction. 3 Management for PR patients includes conservative approaches for mild symptomatic patients. These include prone positioning or nasopharyngeal airway. 4 If these measures fail, surgical management includes tongue-lip adhesion, mandibular distraction osteogenesis (MDO), or tracheostomy. 4 Tongue-lip adhesion has been shown to be less effective in correcting feeding difficulties compared to MDO and presents with other complications such as dehiscence.5,6 Tracheostomy, while providing a definitive airway solution, includes the risk of mucus plugging and accidental decannulation and is associated with higher morbidity compared to MDO. 6 MDO has emerged in the last 2 decades as a surgical option for PR and often is the preferred primary surgical intervention for PR, given its lower costs and better feeding outcomes than the other options mentioned.4,7 Meta-analyses have shown MDO to achieve a high success rate in the prevention of tracheostomy and in the alleviation of obstructive upper airway symptoms in children. 8
Children with craniofacial disorders are often managed with a team comprised of specialties such as audiology, genetics, orthodontia, pediatrics, otolaryngology – head and neck surgery, plastic surgery, oral and maxillofacial surgery, and speech pathology. 9 Currently, there is limited data demonstrating the proportion of fellowship-trained pediatric plastic surgeons, otolaryngology-head & neck surgeons (OHNS), or oral and maxillofacial surgeons (OMFS) performing mandibular distraction surgeries. Since 2003, the number of pediatric OHNS fellowship positions has more than tripled. 10 However, it is unclear whether OHNS has been performing more MDO procedures per year over the past decades. This study aims to understand the national landscape of infantile MDO surgeries over a 10-year period while also assessing patient factors and demographics that are associated with the surgical services that perform MDO.
Methods
We conducted a cross-sectional analysis of the National Surgical Quality Improvement Program Pediatric (NSQIP-P) database from 2012 to 2022. NSQIP-P is a deidentified database offered by the American College of Surgeons (ACS) that has collected pediatric surgical data since 2012. This national database contains information from over 150 participating institutions including patient demographics, preoperative comorbidities, intraoperative characteristics, and 30-day postoperative outcomes for pediatric surgeries across the United States. Data is collected by trained data analysts, which allows for accurate and standardized data collection. Methods of data collection have been described previously.11,12 All identifiable information was protected and de-identified, thus exempting this study from IRB approval.
Patients under the age of 1 year who underwent mandibular distraction were identified using Current Procedural Terminology (CPT) codes 20692, 20696, and 21196. Patients under the age of 1 year were selected to ensure a more uniform indication for MDO, primarily for upper airway obstruction associated with PR. In contrast, patients older than 1 year may undergo MDO for a broader range of indications, including hemifacial microsomia, revision MDO for syndromic craniofacial conditions, and obstructive sleep apnea. Given the variability in indications, medical complexity, and complication rates in this older population, patients over the age of 1 year were excluded. Patients were retained in the cohort if they had concurrent CPT codes for mandibular augmentation, reconstruction, or osteotomy including 21125, 21193, 21195, 21196, or 21198. Patients were excluded if they had CPT codes indicating procedures unrelated to primary mandibular distraction, including 20955 (harvest of autologous bone graft), 21046 (orbital reconstruction), 21070 (removal of superficial orthopedic implant), 21085 (oral surgical splint), 21121 (genioplasty), 21141, 21142, 21143, 21150, and 21155 (LeFort osteotomies), 21230 (graft of bone to the facial bones), 41150 (partial glossectomy), or 61557 (craniectomy or craniotomy). Additionally, patients with the following diagnosis codes were excluded: K09.0, M26.02, M26.03, M26.213, D16.5, S02.642A, and S02.670A.The analysis was completed by surgical case as opposed to patient, and therefore, there may be repeats of patients in the analysis should the patient have had multiple MDO procedures performed under 1 year of life.
The NSQI-P database offers the ability to identify the specialty of the surgeon performing the case from a pre-determined list that includes Pediatric Cardiothoracic Surgery, Pediatric Neurosurgery, Pediatric Orthopedic Surgery, Pediatric Otolaryngology, Pediatric Surgery, Pediatric Urology, Pediatric Plastic Surgery, Plastic Surgery, Cardiothoracic Surgery, General Surgery, Gynecology, Neurosurgery, Orthopedics, Otolaryngology, and Urology. If the surgeon does not directly identify with one of the 10 listed specialties, the closest specialty of the primary surgeon is chosen.
For our study, the specialist performing the procedure was categorized as an OHNS or non-OHNS. OHNS, within the database, was categorized into Pediatric Otolaryngology and Otolaryngology. There is no other distinction of other subspecialties within otolaryngology.
Complications analyzed in this study are from NSQI-P and included superficial incisional surgical site infections (SSI), deep incisional surgical site infections (SSI), wound disruption/dehiscence, unplanned intubations, and pneumonia.
The primary outcome of this study included the trends in the number of MDO performed by OHNS. Univariate Pearson correlation coefficients were used to quantify the correlation between the proportion of MDO procedures performed by OHNS per year and the year of operation.
Multivariable logistic regression models were used to identify predictors of being treated by an OHNS for all MDO procedures. Regression analysis was conducted to examine predictors of wound complications. All analysis was completed with R statistical software (RStudio, Inc.).
Results
We identified 232 cases of MDO for patients under the age of 1 year between 2012 and 2022, of which 40.6% (N = 67) underwent repair with OHNS. Table 1 demonstrates the characteristics of patients stratified by non-OHNS and OHNS. On univariate Pearson correlation analysis, there was not a significant change in MDO performed by OHNS over time (R = 0.426, P = .219). Figure 1 illustrates the change in the proportion of all MDO cases performed by OHNS.
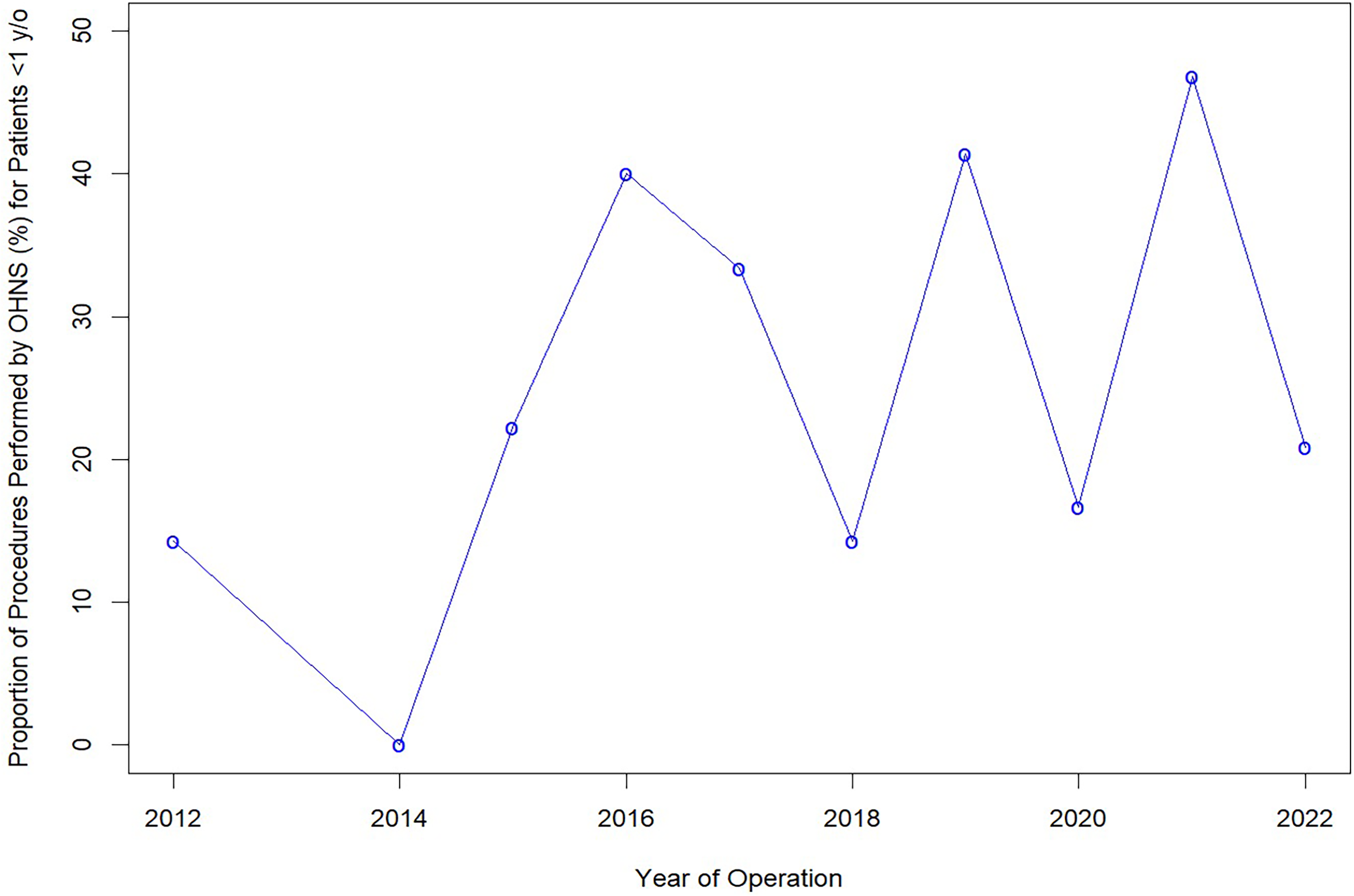
Trend in the proportion of MDO surgeries performed by OHNS over the study period. On univariate Pearson correlation analysis, there was no significant change in the proportion of MDO procedures performed by OHNS over time (R = 0.426, P = .219).
Characteristics of Patients Stratified by Non-OHNS and OHNS.
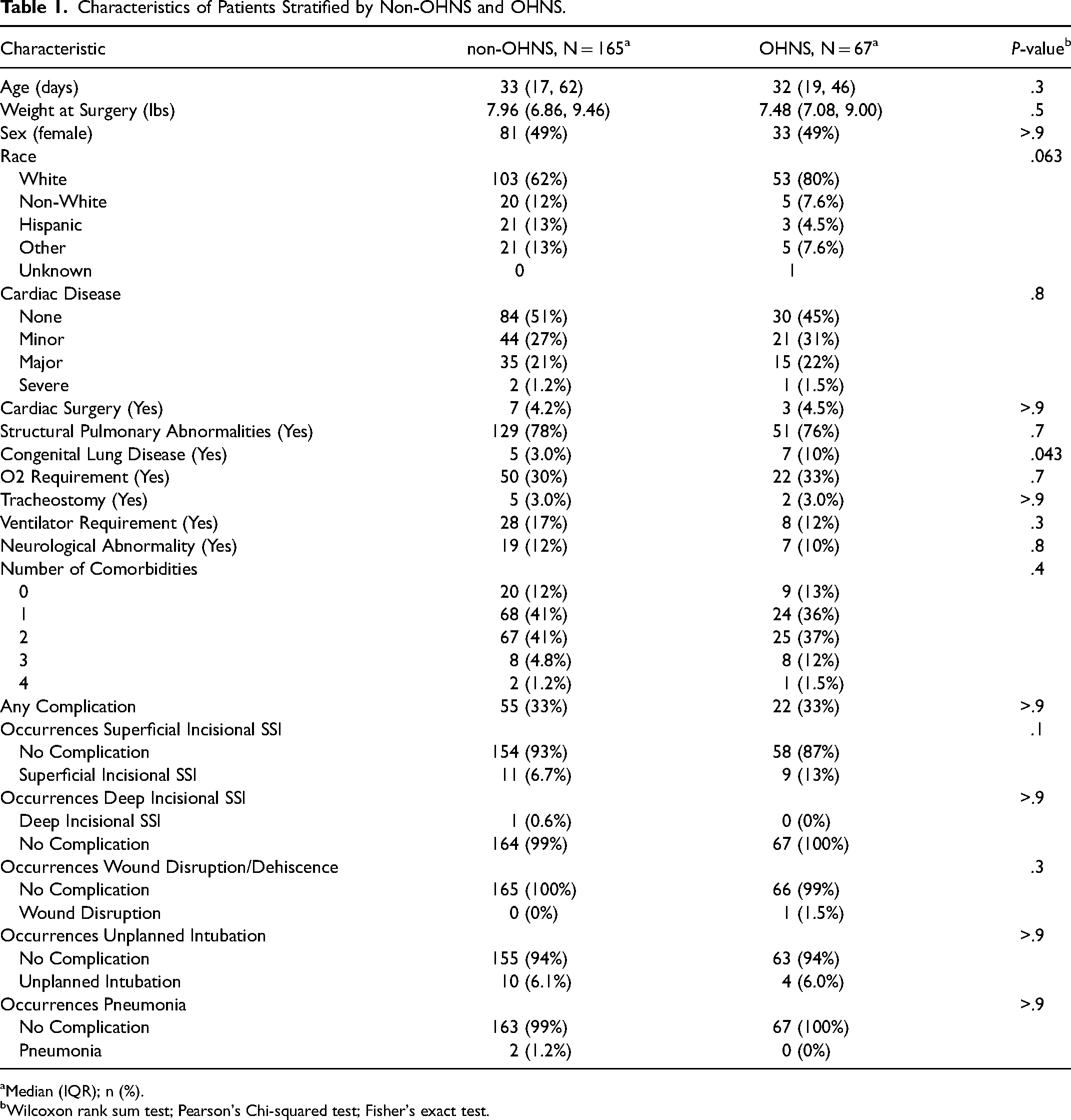
Median (IQR); n (%).
Wilcoxon rank sum test; Pearson's Chi-squared test; Fisher's exact test.
Non-OHNS and OHNS both demonstrated an overall complication rate of 33% (55/165 and 22/67, respectively). Superficial incisional SSI exhibited the highest prevalence among the different forms of wound complications for both non-OHNS and OHNS at 6.7% (11/165) and 13.4% (9/67), respectively. Other complications among non-OHNS included 0.6% deep incisional SSI (1/165), 6.1% re-intubation (10/165), and 1.2% pneumonia (2/165). Other complications among OHNS included 1.5% wound dehiscence (1/67) and 6.0% re-intubation (4/67).
OHNS demonstrated no complications from pneumonia. Multivariable regression was used to identify predictors of being operated on by OHNS. Table 2 illustrates the results of multivariable regression models. Of all patients, those with congenital lung disease (OR 5.48, 95% CI 1.52-22.1, P = .011) were more likely to be treated by OHNS. The operative year was not associated with being treated by OHNS (P = .992).
Multivariable Logistic Regression Model Predicting Patient Characteristics and Treatment by OHNS.
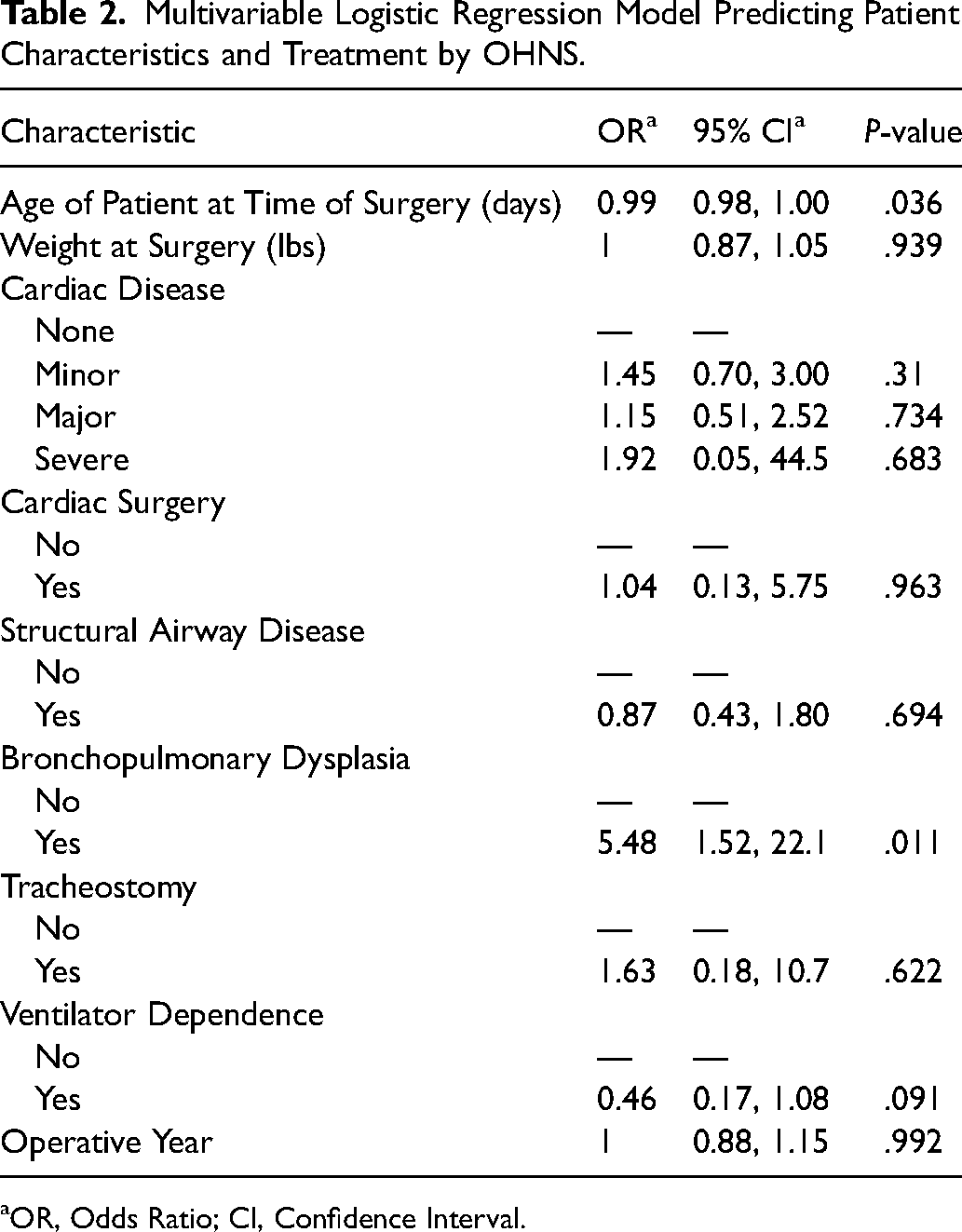
OR, Odds Ratio; CI, Confidence Interval.
Discussion
In this study, we examined trends in MDO surgeries among infants utilizing a national database. Over the 10 years from 2012 to 2022, there was no change in the proportion of MDO surgeries performed by OHNS. Non-OHNS continue to perform most mandibular distractions, with both non-OHNS and OHNS demonstrating comparable complication rates.
Our findings corroborate other studies using national databases to identify OHNS management and involvement in cleft and craniofacial procedures. Sharma et al compared plastic surgery and OHNS management in cleft lip and palate using the NSQIP database. 13 In that study, they found no statistically significant change in the proportion of cleft lip/palate repair performed over a 10-year period with no differences in complication rates between surgical specialty. 13 This is also seen in pediatric rhinoplasty, where Doval et al noted most cases were performed by plastic surgeons with comparable complication rates between specialties. 14
This study highlights a significant association with OHNS performing MDO on children with congenital lung disease. A similar trend is observed in the management of cleft lip, where Sharma et al demonstrate that OHNS are more likely to perform cleft lip and palate surgery on children with structural airway disease and major or severe cardiac conditions. 13 Despite these differences in patient characteristics between OHNS and non-OHNS, both our study and Sharma et al observed that complication rates were similar between specialties. It is not clear in the literature why there is an association with OHNS surgically managing more patients with structural airway disease. One reason could be referral patterns from the neonatal intensive care unit for children who are born premature and have airway concerns would result in an earlier consult for the pediatric OHNS team a priori to other consulting teams.15–18 Murray et al, describe how a specialized Difficult Airway Service (DAS) team composed of a pediatric anesthesiologist and nurse practitioner was established in a pediatric hospital to proactively identify and manage high-risk pediatric airways.16,17 Most of their consults come from the neonatal intensive care unit (NICU) and pediatric intensive care unit (PICU).16,17 The DAS framework is to consult the OHNS service in those children they classify with a critical airway or where surgical airway is considered a possible management approach.16,17
As specialists in upper airway management, pediatric OHNS is in a unique position to treat PR and other micrognathic/retrognathic disorders. While tracheostomy avoidance is the primary goal of MDO, feeding and swallowing difficulties are second to respiratory difficulties and can affect up to 80% of patients with mandibular micrognathia. 19 Patients with insufficient oral intake due to micrognathia are at risk for malnutrition, failure to thrive, aspiration, pneumonia, and choking and often require tube feedings. 19 Pediatric OHNS are trained to treat swallowing disorders that include structural and functional abnormalities of the upper airway or esophagus. 20 While a large majority of patients who undergo MDO ultimately have improvements in feeding issues,21,22 adequate oral intake and growth is a precursor to hospital discharge. 23 McGhee et al investigated perioperative feeding performances in infants with RS who underwent MDO and reported that it takes most patients an average of two weeks to reach full goal feeds after extubation. 23
The American Cleft Palate-Craniofacial Association (ACPA) does not specifically endorse a specialty to perform MDO surgeries. Over the past 2 decades, there has been a triple increase in the number of pediatric OHNS fellowships. 10 Moreover, it has been reported that the number of residents choosing to do fellowship after OHNS residencies has continued to grow, with over 45% of residents selecting fellowships in facial plastics or pediatric OHNS. 24 While the proportion of OHNS surgeons over the past decades performing MDO has remained constant at around 40%, this number may go up with an increased number of providers trained and capable of performing this surgery.
Referral patterns to surgeons or surgical subspecialties are influenced by numerous factors, including the specialist's clinical expertise, interactions between the patient and specialist, and the relationship between the referring physician and the specialist. 25 Institutional and leadership policies also contribute significantly to these complex patterns. Given our data, it is important that residency and fellowship programs prioritize this training. It is well understood that higher surgical volume of a specific procedure is associated with improved outcomes in otolaryngology surgeries and within other specialties.26–28 Given the increasing trends of OHNS residents who chose to undergo further subspecialty training and the top two most selected fellowships being facial plastics and pediatric OHNS, it may be beneficial for the OHNS national organizations to work towards increasing craniofacial (ie, MDO) and facial plastics surgical volume requirements to promote adequate training and enable the field to continue to grow. Residency programs, accrediting societies, and professional societies in OHNS would need to require this training or increase the number of key indicators in this realm if it is to be considered important to the field.
As the field moves toward less invasive treatment options, the pediatric OHNS will continue to play a crucial role in the management of PR, even if it is not surgical. The orthodontic airway plate (OAP) is a non-surgical alternative that is gaining attention and being adopted in the United States. 29 The OAP, like a retainer, is a custom-fabricated device composed of palatal, intrapharyngeal, and extra-oral components. 29 The OAP is thought to promote correction through forward and downward positioning of the tongue that will force the mandible and its muscular attachments forward, promoting physiologic bone remolding of the temporomandibular joint (TMJ) complex. 29 Given the pediatric OHNS's expertise in the evaluation and treatment of pediatric difficult airways, they are recognized as key personnel within the protocol of the OAP. 29 At their institution trial, Choo et al describe that patient eligibility for the OAP trial is based on clinical observations from endoscopy performed by pediatric OHNS. 29 Once in the trial, precise insertion and adjustment of the plate is realized via fiberoptic nasopharyngoscopy in collaboration with pediatric OHNS. 30 The development of the split orthodontic airway plate (S-OAP), a newer device designed to re-size periodically, 31 follows the same conventional OAP delivery protocol, necessitating the continued expertise of pediatric OHNS for placement and airway optimization. 31
Our study is subject to many limitations. Cross-sectional studies may not be ideal for studying rare diseases due to same-size constraints. Same-size constraints are also subject to sampling biases such as nonresponse bias and recall bias. Given that exposures and outcomes are measured at the same time, it is difficult to make causal inferences and associations identified may be difficult to interpret. Limitations related to the use of a national database include limited details on operative and patient-specific characteristics of each case as well as errors in reporting and physician specialty categorization. NSQIP-P does not capture important factors that affect healthcare utilization such as geographic location, surgeon availability, insurance coverage, practice type and patient referral patterns that could influence whether patients are managed by OHNS or non-OHNS. Another limitation is the inability to assess specific training pathways of non-OHNS as NSQIP-P only categorizes surgeons by general specialty. Furthermore, oral and maxillofacial surgery cannot accurately be identified by the NSQIP-P. Finally, because participation in the NSQIP is voluntary, it does not represent a population-based cohort.
Conclusion
Our study demonstrates that the proportion of pediatric OHNS performing mandibular distractions among infants has not changed over the last decade. OHNS are more likely to perform mandibular distractions on children with complex pulmonary disease. OHNS demonstrates comparable outcomes and complication rates when compared to other specialties.
Footnotes
Data Availability Statement
The datasets generated and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval and Informed Consent Statements
This study received ethical approval from IRB #240800 on May 21, 2024. This is an IRB-approved retrospective study; all patient information was de-identified, and patient consent was not required.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
